* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Congenital absence of pericardium revisited
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Coronary artery disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Myocardial infarction wikipedia , lookup
Atrial septal defect wikipedia , lookup
Congenital heart defect wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
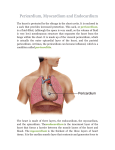
The International Journal of Cardiovascular Imaging 18: 67–73, 2002. Ó 2002 Kluwer Academic Publishers. Printed in the Netherlands. 67 Congenital absence of pericardium revisited Yang Faridah & Paul R. Julsrud Department of Radiology, Mayo Clinic, 200 First Street Southwest, Rochester, 55905 MN, USA Received 29 May 2001; accepted in revised form 16 July 2001 Key words: congenital, magnetic resonance imaging, pericardium Abstract Although much have been published regarding congenital absence of pericardium, it is essential that this anomaly, like an old friend, be revisited from time to time. Review of this anomaly with emphasis on its embryological process is discussed. Furthermore, with the advances in magnetic resonance imaging, absence of pericardium can now be diagnosed with ease and the radiological findings of this condition are reviewed as well. Introduction Congenital defects of the pericardium are a relatively rare anomaly that was first described in 1559 by Columbus [1]. Following this, there were still reservations about the true existence of this condition and it was not until 1778 when Baillie [2] gave a detailed description of a case that all doubts were laid to rest. Since then numerous cases and studies have been published. A review of this anomaly with regards to its classification and epidemiology, embryology, clinical features and radiological features is presented here with the aid of a case report, to illustrate the radiological findings and technical aspects of magnetic resonance imaging (MRI). Classification and epidemiology Pericardial defects have generally been classified as being complete or partial. In the majority of cases these pericardial defects, both complete and partial types, affect the left side of pericardium rather than the right. Complete absence of the left pericardium is the most common defect accounting for 76% of all pericardial defects in one large series [3]. Right sided and bilateral partial absences of the pericar- dium are extremely rare [4]. Seventy seven percent of all types of pericardial defect occur in males [3]. Embryology During the first week of development, irregular cavities are formed in the mesodermal substance of the embryo. These cavities enlarge and coalesce to form the primitive pericardial, peritoneal and pleural cavities (Figure 1). By the fourth week, a wedge of mesoderm, has begun to grow and interposed itself between the primitive pericardial and peritoneal cavities. This is the septum transversum and it contains the developing liver and termination of the umbilical and vitelline veins (Figure 2). This separation however is not complete, as there exist pericardio–peritoneal canals bilaterally, just medial to the common cardinal veins (ducts of Cuvier) (Figure 1). The lung buds grow and protrudes into these canals, which fold about them forming the pleural sacs (Figures 2 and 3). At the end of the fourth week, twofolds begin to grow out from the ducts of Cuvier, on each side, the ventral fold forming the pleuropericardial membrane while the dorsal fold forms the pleuroperitoneal membrane (Figures 2 and 3). 68 Figure 1. Diagrammatic representation of a fetus in early development in the sagittal plane showing formation of the pericardial, pleural and peritoneal cavities. Curved arrow represents the position of the pericardio–peritoneal canal which lies medial to the bilateral ducts of Cuvier. PC1 – pericardial cavity; PC2 – peritoneal cavity; PC3 – pleural cavity; PPM1 – pleuropericardial membrane; PPM2 – pleuroperitoneal membrane; ST – septum transversum; * – common cardinal vein (duct of Cuvier); ACV – anterior cardinal vein; PCV – posterior cardinal vein; PN – phrenic nerve. By the fifth week, these membranes reach and fuse with the medial wall of the pleuroperitoneal canal on each side of the lung bud, separating the pericardial and pleural cavities from the peritoneal cavity (Figure 3). The pleuropericardial membrane obliterates the pleuropericardial opening while the pleuroperitoneal membrane obliterates the pleuroperitoneal opening. Each lung extends anteriorly to the front of the heart. The complete separation of the pericardial cavity from the pleural cavity takes place when the pleuropericardial membrane unites with the root of lung (Figure 3). Figure 2. Diagrammatic representation of a fetus at fourth week of development in the sagittal plane showing the formation of the septum transversum and the eventual division of the pleuropericardial and pleuroperitoneal membranes. PC1 – pericardial cavity; PC2 – peritoneal cavity; PC3 – pleural cavity; PPM1 – pleuropericardial membrane; PPM2 – pleuroperitoneal membrane; ST – septum transversum; * – common cardinal vein (duct of Cuvier); ACV – anterior cardinal vein; PCV – posterior cardinal vein; PN – phrenic nerve. Failure of the pleuropericardial membranes to close completely on one or both sides will result in pericardial deficiencies. It is generally accepted that defects in the pericardium are due to the persistence of the pleuropericardial foramen, but there are differing opinions on the causative factor that prevents this closure: (a) Perna (1909) [5] proposed the current generally accepted theory that the arrested closure of the pleuropericardial membrane is due to the premature atrophy of the left duct of Cuvier. In normal development, the right duct of Cuvier develops into the superior vena cava. As the left brachiocephalic vein forms, the left duct of Cuvier atrophies with its distal portion persist- 69 Figure 3. Diagrammatic representation of a developing fetus from fourth to sixth week of gestation in the axial plane. A. Normal development of the pericardium. B. Proposed abnormal development resulting in absence of the left pericardium as hypothesized by Perna. a – aorta; aldc – atretic left duct of Cuvier; es – esophagus; da – dorsal aorta; dc – duct of Cuvier; h – heart; ivc – inferior vena cava; l – lung; lb – lung bud; nt – notochord; pp – parietal pericardium; ppl – parietal pleura; ppm1 – pleuropericardial membrane; vp – visceral pericardium; vpl – visceral pleura. ing as the coronary sinus. The early obliteration of the duct diminishes the blood supply to the growing pleuropericardial membrane resulting in a defect in the left pericardium. This theory explains why the majority of these defects involve the left pericardium (Figure 3). (b) An alternative hypothesis postulates that the heart enlarges and stretches the enveloping pericardium during development [6]. It is thought that the pleuropericardial foramen has to close before the heart enlarges. Failure of the membrane to grow and fuse in time would result in a persistent defect. This can affect the whole membrane in total or either the pericardial or pleural membrane in isolation. The size of the defect would depend on the rate of growth of the heart and the enveloping mem- brane. This theory would explain the preponderance of the defect to the left, as the heart is a left-sided structure. It would also explain the rare circumstance of right-sided defect and total absence of pericardium depending on which membrane is affected. The types of defect, either total or partial absence, is also explained by this. Cases in which there is absence of pericardium but with an intact pleural membrane can be attributed to this as well [7]. Clinical features Most patients are asymptomatic and the discovery of this defect is incidental. The most common symptom of complete absence of pericardium is 70 vague chest pain occurring in up to 33% of patients [8, 9]. Dyspnea, dizziness and syncope have also been reported [10]. Marked displacement of the apical impulse into the mid-axillary line is seen in patients with complete absence of pericardium. The heart appears enlarged in approximately 50% of cases, which may be partially due to the slight rotation of the heart into the left chest [3, 11]. This coupled with the presence of a strong and displaced apical impulse, tends to give the impression of an enlarged heart on physical examination and on chest radiograph when no actual enlargement is present [12]. Cardiac murmurs are not specific to the condition. When present, an ejection systolic murmur is heard most often in the second left intercostal space or along the sternal border. Sinus bradycardia is not an uncommon finding [4, 10]. Electrocardiograpy (ECG) changes are commonly seen in cases of complete left pericardial defect and consist of right axis deviation, incomplete right bundle branch block pattern and leftward displacement of the transitional zone in precordial leads. Patients with partial defect of the pericardium are more at risk of morbidity than those with complete defects, as herniation of the heart through a partial defect may occur resulting in Figure 4. Posteroanterior chest radiograph reveals slight rotation of the heart into the left chest and a prominent aortopulmonary notch. 71 strangulation of the heart and death. Conversely, the physical examination and ECG in patients with partial defect are usually normal [13]. Associated cardiac anomalies are seen in 30% of all pericardial defect cases, both complete and partial. These anomalies include atrial septal defect, patent ductus arteriosus, bicuspid aortic valve, bronchogenic cyst, pulmonary sequestration and diaphragmatic hernia [4]. Radiological features Complete absence of pericardium gives a distinctive radiographic picture on a chest radiograph. There is rotation of the heart into the left chest with the right cardiac border projected over the midline. The contour of the left cardiac border is prominent with accentuation of the convexities of the aortic knob, the main pulmonary artery and the left ventricle. The space between the aorta and the main pulmonary artery may appear widened due to the presence of aerated lung between these two vessels. This also results in sharp demarcation of the pulmonary artery. The inferior cardiac border is elongated and flatten and there is commonly interposition of lung between the dome of the left hemidiaphragm and the inferior cardiac border. The trachea and esophagus remain as midline structures [4]. Leftward rotation of the heart is also Figure 5. Coronal T1-weighted spin-echo image demonstrates complete absence of the left pericardium with a prominent aortopulmonary notch. Note the presence of lung between the base of the heart and left diaphragm. 72 seen in atrial septal defect, mitral valve disease and pulmonary valvular stenosis, which may mimic absence of pericardium radiographically [11]. Baim et al. (1980) first described the computed tomography (CT) findings of complete absence of pericardium. Prominence of the main pulmonary artery and interposition of the left lung between the great vessels was described [9]. Vesely and Julsrud (1989) further described tethering of the right pericardium to the anterior chest wall by sternopericardial ligaments as a radiographic sign seen on axial computed tomography [14]. MRI findings of complete pericardial defect were presented by Gutierrez et al. in 1985 [15]. MRI coronal sections through the heart demonstrated actual absence of the pericardium. There was leftward displacement of the heart, a bulging pulmonary artery and herniation of lung between the base of the heart and the left diaphragm [15]. Partial cardiac defect usually presents with a normal chest radiograph. Occasionally, a prominent bulge along the left side of the cardiac silhouette in the vicinity of the left atrial appendage maybe seen [8, 16]. Herniation of the heart through the partial defect can be appreciated, forming an indentation on the heart or a myocardial crease on CT or MRI [17, 18]. Figure 6. Axial T1-weighted spin-echo image illustrates prominence of the main pulmonary artery with extension of the lung between the pulmonary artery and aorta. Presence of the sternopericardial ligament is clearly depicted (arrow). 73 Case report A 59-year-old male presented with shortness of breath for 5 months and investigations to assess his cardiac status were performed. Chest radiograph was reported as normal. On echocardiogram, his left ventricle was found to be displaced to the left axilla. Although actual pericardium cannot be visualized, the abnormal position of the heart raised the suspicion of absent pericardium. Subsequent MRI confirmed the diagnosis. Retrospective analysis of the chest radiograph reveals slight rotation of the heart to the left and a prominent aortopulmonary notch (Figure 4). The MRI demonstrated complete absence of the left side of pericardial sac (Figures 5 and 6). There was difficulty in cardiac gating using chest leads, as the signal from this was bizarre and unreadable. Switching to peripheral leads for cardiac gating solved this problem. On MRI, there is rotation of the heart into the left chest with prominence of the right ventricular outflow tract (Figure 5). There is presence of sternopericardial ligament tethering the heart and great vessels to the sternum (Figure 6). The lung extends in between the pulmonary artery and ascending aorta. There is a tongue of lung extending between the heart and left hemidiaphragm (Figure 5). Discussion Gutierrez et al. [15] predicted that MRI would become the preferred technique for the definitive diagnosis of absence pericardium due to its capability to image in any plane. We believe this prediction was correct. The presence of other congenital anomalies can also be observed as both morphological and functional imaging may be performed with MRI. Thus, we consider MRI with its unique ability to display anatomy of the heart, including pericar- dium, to be the diagnostic tool of choice for evaluating pericardial defects. References 1. Columbus MR. De re anatomica. Vol. XV, 1559: 265. 2. Baillie M. On the want of a pericardium in the human body. Tr Soc Improve M Chir Knowl 1793; 1: 91. 3. Southworth H, Stevenson CS. Congenital defects of the pericardium. Arch Intern Med 1938; 61: 223–240. 4. Tabakin BS, Hanson JS, Tampas JP, Caldwell EJ. Congenital absence of the left pericardium. Am J Roentgen 1965; 94: 122–128. 5. Perna G. Sopra un arresto di sviluppo della sierosa pericardica nell’ uomo. Anat Anz 1909; 35: 323. 6. Sunderland S, Wright-Smith RJ. Congenital pericardial defects. Br Heart J 1944; 6: 167–175. 7. Moore RL. Congenital deficiency of the pericardium. Arch Surg 1925; 11: 765–777. 8. Glover LB, Barcia A, Reeves TJ. Congenital absence of pericardium. Am J Roentgen 1969; 106: 542–549. 9. Baim RS, McDonald IL, Wise DJ, Lenkei SC. Computed tomography of absent left pericardium. Radiology 1980; 135: 127–128. 10. Nasser WK. Congenital absence of the left pericardium. Am J Cardiol 1970; 26: 466–470. 11. Schad N, Stark P. The radiological features of cardiac rotation: a pictorial essay. J Thorac Imaging 1992; 7(3): 81–87. 12. Ellis K, Leeds NE. Congenital deficiencies in the parietalpericardium. Am J Roentgen 1959; 82: 125–137. 13. Morgan JR, Rogers AK. Congenital absence of the left pericardium. Ann Intern Med 1971; 74: 370–376. 14. Vesely T, Julsrud P. Congenital absence of the pericardium and its relationship to the ligamentum arteriosum. Surg Radiol Anat 1989; 11: 171–175. 15. Gutierrez FR, Shackelford GD, McKnight RC, Levitt RG, Hartmann A. Diagnosis of congenital absence of left pericardium by MR imaging. J Comput Assist Tomogr 1985; 9: 551–553. 16. Pernot C, Hoeffel JC, Henry M. Radiologic patterns of congenital malformations of the pericardium. Radiol Clin 1975; 44: 505–511. 17. Lau KW, Ding ZP. Partial pericardial defect. Circulation 1998; 97(19): 1992. 18. Gassner I, Judmaier W, Fink C, et al. Diagnosis of congenital pericardial defects, including a pathognomic sign for dangerous apical ventricular herniation, on magnetic resonance imaging. Br Heart J 1995; 74: 60–66.