* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Online Appendix for the following JACC article TITLE: Evidence
Remote ischemic conditioning wikipedia , lookup
Coronary artery disease wikipedia , lookup
Myocardial infarction wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Marfan syndrome wikipedia , lookup
Turner syndrome wikipedia , lookup
Aortic stenosis wikipedia , lookup
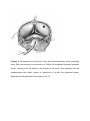
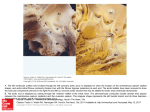
Online Appendix for the following JACC article TITLE: Evidence, Lack of Evidence, Controversy, and Debate in the Provision and Performance of the Surgery of Acute Type A Aortic Dissection AUTHORS: Robert S. Bonser, A. M, Ranasinghe, M. Loubani, J. W. Evans, N. M. A. Thalji, J. Bachet, T. Carrel, M. Czerny, R. <Di Bartolomeo, M. Grabenwöger, L. Lonn, C.-A. Mestres, M. Schepens, E. Weigang APPENDIX Supplementary eFigures eFigure 1: The time dependency of mortality risk of patients admitted to hospital (alive) with acute aortic dissection according to dissection sub-type and treatment allocation (A= type A dissection and B= type B dissection). Reproduced, with permission, from Hagan et al. (1). eFigure 2: Resuspension of the aortic valve after acute dissection of the ascending aorta. Each commissure is anchored by a Teflon felt pledgeted horizontal mattress suture, suturing from the inside to the outside of the aorta. This technique can be supplemented with fabric inserts or adhesives to re-affix the dissected layers. Reproduced with permission from Arom et al. (2). eFigure 3: Cumulative probability bar charts for Group A (supracoronary anastomosis) and Group B (composite aortic root replacement for outcomes with respect to (a) proximal reoperation and (b) distal reoperation. There is a trend towards lower proximal reoperation rates in Group B patients. Thirteen distal aortic procedures were performed in 10 group A patients and 10 procedures in five group B patients. Reproduced with permission from Halstead et al. (3). eFigure 4: Actuarial survival curves demonstrating survival in patients undergoing repair of type A aortic dissection with profound hypothermic circulatory arrest (PHCA) and without (non-PHCA) for (A) the entire study group (n= 307) and (B) a propensity score matched subset (n= 152). There was no statistically significant difference in outcomes noted between the two techniques. Reproduced with permission from Lai et al. (4). Supplementary eTables ECG finding Percentage incidence Normal 19% Sinus rhythm 91% Atrial fibrillation 5% Other rhythm 4% Left ventricular hypertrophy 29% Right bundle branch block 7% Left bundle branch block 2% Left anterior hemiblock 8% Low voltage 5% Old Q waves 5% Nonspecific ST-T abnormalities 59% ACS-like profile 26% STEMI 4% Non-STEMI 21% ST depression 1% ST elevation and T wave 7% abnormalities 13% T wave ≥2mm in ≥2 contiguous leads eTable 1: ECG findings in acute Type A aortic dissection. Over 25% of presenting patients have an ECG compatible with an acute coronary syndrome, most often compatible with a non-ST elevation myocardial infarction (NSTEMI). Modified and reproduced with permission from Biagini et al. (5). Immer Geirsson Girdauskas Cumulative Number of patients 227 221 276 724 Overall incidence MPS (%) 33 27 34 31 Cardiac (%) 4 7 15 9 CNS (%) 14 9 14 13 Limb (%) 15 13 12 13 Visceral (%) 2 1 3 2 Renal (%) 4 4 Not reported 4 Number of MPS(%) Not reported Single 64 81 73 Double 27 13 20 Triple 5 5 5 Quadruple 3 4 4 eTable 2: The incidence of malperfusion syndrome (MPS) in patients presenting with acute type A aortic dissection. Data adapted from studies by Immer, Geirsson and Girdauskas(6–8). Cannulation site Advantages Disadvantages Femoral artery Ease of access Retrograde flow Size Pressurization of false lumen Adequate flow rates Proximal embolization Axillary/subclavian artery Reports of reduced More time consuming mortality and stroke rates Brachial plexus injury Aortic cannulation Speed of cannulation Identification of true lumen Ventricular apex Adequacy of flow Direct Antegrade flow Ventricular injury Direct cannulation of true lumen eTable 3: The potential advantages and disadvantages of the different cannulation sites utilized in acute type A aortic dissection REFERENCES 1 Hagan PG, Nienaber CA, Isselbacher EM, et al. The International Registry of Acute Aortic Dissection (IRAD): new insights into an old disease. JAMA 2000;283:897–903. 2. Arom KV, Grover FL. Adult cardiac surgery during the first 50 years of the Southern Thoracic Surgical Association. Ann Thorac Surg 2003;76:S17–46. 3. Halstead JC, Spielvogel D, Meier DM, et al. Composite aortic root replacement in acute type A dissection: time to rethink the indications? Eur J Cardiothorac Surg 2005;27:626–32. 4. Lai DT, Robbins RC, Mitchell RS, et al. Does profound hypothermic circulatory arrest improve survival in patients with acute type A aortic dissection? Circulation 2002;106 Suppl 1:I218–28. 5. Biagini E, Lofegio C, Ferlito M, et al. Frequency, determinants and clinical relevance of acute coronary syndrome-like electrocardiographic changes in patients with acute aortic syndrome. Am J Cardiol 2007;100:1013–9. 6. Immer FF, Grobety V, Lauten A, Carrel TP. Does malperfusion syndrome affect early and mid-term outcome in patients suffering from acute type A aortic dissection? Interact CardioVasc Thorac Surg 2006;5:187–90. 7. Girdauskas E, Kuntze T, Borger MA, Falk V, Mohr F-W. Surgical risk of preoperative malperfusion in acute type A aortic dissection. J Thorac Cardiovasc Surg 2009;138:1363–9. 8. Geirsson A, Szeto WY, Pochettino A, et al. Significance of malperfusion syndromes prior to contemporary surgical repair for acute type A dissection: outcomes and need for additional revascularizations. Eur J Cardiothorac Surg 2007;32:255–62.