* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Chapter 20
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Artificial heart valve wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Electrocardiography wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Jatene procedure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
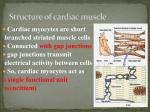
Chapter 20 Cardiovascular System The Heart THE HEART As the nervous system connects entire body with its network for the purpose of communication, the circulatory system and its circulating matter, blood, connect the entire body and the heart must pump the blood. In a simpler organism, diffusion may have sufficed to transport nutrients and oxygen throughout the organisms, but in a more complex organism, the gases and nutrients need to be transported through a specialized system and disposed. In fact, in the early stage of embryonic development of humans, and in many other higher organisms, the beating of the heart is the first observable organ activity. The heart that continuously beats about 70 times a minutes throughout your life-time and performs a tremendous amount of work. It beats 100,000 times a day. (How many times in your life-time?) Pumps about 8,000 liter of blood a day. Can you change the rate of heart beat? Cardiovascular overview Functions of the Heart • Generating blood pressure • Routing blood – Heart separates pulmonary and systemic circulations • Ensuring one-way blood flow – Heart valves ensure one-way flow • Regulating blood supply – Changes in contraction rate and force match blood delivery to changing metabolic needs Anatomy and histology Heart Skeleton • Consists of plate of fibrous connective tissue between atria and ventricles • Fibrous rings around valves to support • Serves as electrical insulation between atria and ventricles • Provides site for muscle attachment Blood Flow Through Heart 2. Route of blood flow through the heart Study Seeley’s Fig. 20.10 flow of blood through the heart chambers. The heart is divided into the left and right chambers. The deoxygenated blood from tissues pass through the right chambers and oxygenated blood from the lungs pass through the left chambers. In order for the blood to pass through these chambers, both arteria contract at about the same time and both ventricles contract at about the same time. A sequence of events to flow blood through the heart depends on the change in pressure inside the chambers and two sets of valves which prevent the back flow of blood. Phases of cardiac cycles For example from the perspectives of the blood flow: Fig. 20-16. (1) Blood enters the right atrium because pressure in the superior/inferior vena cava is higher than that in the right atrium. The pulmonary semilunar valve stay closed. (2) The blood flow into the right atrium, which is in a relaxed state after contraction. (3) The right atrium contacts (atrial systole) and pushes through remaining blood into the right ventricle. Tricuspid valve open. (4) Upon contraction of the right ventricle, (systole) the pressure inside forces the tricuspid valve to close, but the pulmonary semilunar valve to open, allowing the blood to flow out into the pulmonary trunk then to pulmonary arteries. (5) Blood in the lung capillaries releases carbon dioxide and picks up oxygen. (6) Blood returning from the lungs through the pulmonary veins (note that these are veins, but carry oxygenated blood), and fill up the left atrium. The bicuspid valve is opened. (7) The contraction of left atrium (while aortic semilunar valve closed) completes the transfer of blood to the left ventricle. Contraction of the left ventricle forces the bicuspid valve to close and blood gushes out through the now opened aortic semilunar valve.. This is a powerful push. Note that contraction of the both ventricles take place at the same time, as do the atria. Also note the thickness of ventricular walls. Cardiac muscles (1) Cardiac muscle cells are less ordered than skeletal muscle cells. (2) They are branched and each cell has one or two nuclei. Sarcomeres are still evident i.e. some striation, but T tubules are not extennsive. (3) Cells are surrounded with connective tissue and intercalated disks connect cardiac muscle cells. (4) Slow and prolonged contraction of cardiac muscle cells allow Ca++ to move in and out the myofibrils. (5) Desmosomes hold the cells together and gap junctions connect them for easy transmission of action potentials. (6) Well vasculated for aerobic respiration for steady and enough oxygen supply for mitochondrial activities. (7) Cardiac muscle cells, which are under continuous steady contraction/relaxation cycles, glucose, fatty a acids and lactic acid to produce ATP. Conducting system Conducting System of Heart b. The conducting system (Fig. 20-12,13) Unlike skeletal muscle, cardiac muscle can contract spontaneously -automaticity. The sequence of rhythmic contraction, the atria to the ventricles, is regulated by nodal cells, that determines the rate of contraction, and conducting cells, which distribute the contractile stimuli. i.Nodal cells: The pace maker nodal cells spontaneously depolarize at 70 - 80 times a minute. The pace maker cells in the right atrium near at the entrance of the superior vena cava is the sinoatrial node (SA node) and regulates the heart beat. ii. node. Conducting cells: The signal for contraction starts with the SA (1)The action potential from the SA node spreads along the wall of the atrium to the atrioventricular (AV) node. (2)The action potential from the AV node spreads along the atrioventricular (AV) bundle into the interventricular septum. (3)The AV bundles are divided into right and left branches. (4)These bundles are connected to the Purkinje fibers of the ventricular wall and stimulate both right and left entricular muscle cells Although the cardiac muscles are capable of contracting spontaneously, the frequency of contraction is regulated by the generation of action potentials by the pace maker SA node. While the action potential from the SA node induce contraction of the atrium, its spread to the AV node takes 0.04 second. Further, the spread of the action potential within the AV node is slow. Thus all together 0.11 seconds of delay is caused before ventricular contraction takes place. That makes total of 0.15 seconds. Electrical properties i. Action potentials The electrical properties, thus ionic distributions, of cardiac muscles are similar to those of the neurons and skeletal muscle cells. The difference of action potentials between skeletal muscle or neuron and cardiac muscle lies in the special role of voltage-gated Ca++ slow channels in cardiac muscle. (Fig. 20-15) Also note the roles of voltage gated Na+ and K+(small contribution) channels. The initial fast depolarization by the voltage gated Na+ channels (opened) is followed by the opening of voltage-gated Ca++ slow channels. Presence of the opened voltage-gated Ca++ slow channels extends the partial repolarization phase (plateau phase) thus prolong duration of the action potential up to 500 msec until the Ca++ channels begin to close. Thus there will be a long contraction period, hence a long refractory period. Autorhythmicity of cardiac muscle (Fig. 20-12) SA Node Action Potential ii. Autorhythmicity of cardiac muscle (Fig. 20-12) The SA node has a significantly large number of voltageregulated Ca++ slow channels (slow channels). Gated K+ channels are present and behave opposite to Ca++ channels with relatively small contribution. The slow channels spontaneously open and let Ca++ into the cell to generate a local membrane potential. When more slow channels are opened, there will be a complete depolarization - the action potential. The resting potential is reestablished by closing the Ca++ slow channels and opening the K-channels. The process will repeat, thus autorhythmic generation of action potentials. The action potential spreads out through the local cardiac muscle fibers and reaches the AV node to depolarize it. The SA node appears to have the largest number of Ca++ slow channels, thus more frequent cycles (70 - 80 bpm). While the AV node can beat at the rate of 40 - 60 bpm and usually let the SA node to dictate the frequency. iii. Refractory period Although contraction of cardiac muscle is initiated similar to that of skeletal muscle by depolarization and subsequent distribution of action potentials in the sarcolemma, there are two important differences between the two types of muscles. (1) In cardiac muscles the entire cycle of an action potential in sacrolemma takes up to 250 -300 msec and is about 30 times longer than that in a sacrolemma of skeletal muscle. Adding to this is a relatively long refractory period of cardiac muscle cell, thus making only up to 200 contractions per minute is possible. (2) We have seen that summation of contraction is possible in skeletal muscle fibers, but it is not possible in cardiac muscle cells. Thus no summation or tetanic contraction can take place. This is an important protective mechanism for the heart. iv. Electrocardiogram Electrocardiogram • Action potentials through myocardium during cardiac cycle produces electric currents than can be measured • Pattern – P wave • Atria depolarization – QRS complex • Ventricle depolarization • Atria repolarization – T wave: • Ventricle repolarization The sequential depolarization of muscle cells may be recorded and the result is called an electrocardiogram (ECG or EKG). Fig. 20-14. (Three electrode system, left and right wrists and left lower leg.) The P wave: The depolarization of the atria. After 100 msec the atria begin to contract. The QRS complex: The depolarization of the ventricles. Contraction is after the R wave. The T wave: Ventricular repolarization. Cardiac arrhythmia etc. Seeley’s Fig. 20.17. Cardiac Arrhythmias • Tachycardia: Heart rate in excess of 100bpm • Bradycardia: Heart rate less than 60 bpm • Sinus arrhythmia: Heart rate varies 5% during respiratory cycle and up to 30% during deep respiration • Premature atrial contractions: Occasional shortened intervals between one contraction and succeeding, frequently occurs in healthy people Alterations in Electrocardiogram Cardiac Cycle • Heart is two pumps that work together, right and left half • Repetitive contraction (systole) and relaxation (diastole) of heart chambers • Blood moves through circulatory system from areas of higher to lower pressure. – Contraction of heart produces the pressure Cardiac Cycle Heart Sounds • First heart sound or “lubb” – Atrioventricular valves and surrounding fluid vibrations as valves close at beginning of ventricular systole • Second heart sound or “dupp” – Results from closure of aortic and pulmonary semilunar valves at beginning of ventricular diastole, lasts longer • Third heart sound (occasional) – Caused by turbulent blood flow into ventricles and detected near end of first one-third of diastole Location of Heart Valves 4. Heart dynamics The amount of blood ejected from a ventricle during a single hear beat is the stroke volume (SV). Instead of measuring the blood volume after a single stroke, the amounts of blood pumped in one minute is more often used as the cardiac output (CO). Cardiac output(CO) = Stroke volume(SV) X Heart rate(HR) Fig. 20-17, 18 summarize all the events. Use them to review the events. a. Factors controlling cardiac output (Fig. 20-20, 21) Baroreceptor and Chemoreceptor Reflexes a. Factors controlling cardiac output Both intrinsic and extrinsic factors regulate the heart rate. i. Intrinsic regulation The amount of blood flow affect the cardiac muscles and stretches the SA node. ii. Extrinsic regulation Both parasympathetic and sympathetic nerves can regulate heart beat. Parasympathetic stimulation decreases heart rate. Sympathetic stimulation increases heart rate. Epinephrine and norepinephrine released by sympathetic stimulation increase heart rate. Heart Homeostasis • Effect of blood pressure – Baroreceptors monitor blood pressure • Effect of pH, carbon dioxide, oxygen – Chemoreceptors monitor • Effect of extracellular ion concentration – Increase or decrease in extracellular K+ decreases heart rate • Effect of body temperature – Heart rate increases when body temperature increases, heart rate decreases when body temperature decreases Baroreceptor Reflex Chemoreceptor Reflex-pH Effects of Aging on the Heart • Gradual changes in heart function, minor under resting condition, more significant during exercise • Hypertrophy of left ventricle • Maximum heart rate decreases • Increased tendency for valves to function abnormally and arrhythmias to occur • Increased oxygen consumption required to pump same amount of blood