* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download respiratory system
Embryonic stem cell wikipedia , lookup
Cell culture wikipedia , lookup
Chimera (genetics) wikipedia , lookup
Artificial cell wikipedia , lookup
Neuronal lineage marker wikipedia , lookup
Induced pluripotent stem cell wikipedia , lookup
Microbial cooperation wikipedia , lookup
Hematopoietic stem cell wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
State switching wikipedia , lookup
Cell theory wikipedia , lookup
Regeneration in humans wikipedia , lookup
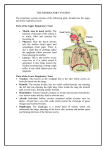
Anatomy and Human Biology 2214 September 28, 2009 M. Hall RESPIRATORY SYSTEM After studying this lecture you should be able to: List the tubules that make up the Conducting and Respiratory portions of the respiratory system. Recognise and describe the cellular components of respiratory epithelium. Understand the functions of respiratory epithelium Understand the function of the conchae Describe the components of the true vocal cord. Where is it located? Recognise and describe the cellular components of olfactory epithelium. Where is it located? Distinguish between these two epithelia. Recognise and understand the function of the epiglottis Distinguish between a bronchus, bronchiole, respiratory bronchiole, alveolar duct and alveolar sac. List all the components that make up the interalveolar septum and the alveolar membrane, and distinguish between the two. Distinguish between type I and type II alveolar cells. Understand the functions of these two cells. Describe the two separate blood supplies to the lungs and understand their functions. The respiratory system includes the lungs and a system of tubes that link the sites of gas exchange with the external environment. It is customary to divide the respiratory system into two principal regions: (1) Conducting Portion nasal cavity nasopharynx larynx trachea bronchi bronchioles terminal bronchioles (2) Respiratory Portion respiratory bronchioles alveolar ducts alveoli - it is here that O2 and CO2 are exchanged between inspired air and blood--the principal function of the lungs. 1 Nasal cavity Nasopharynx Oropharynx Larynx Trachea Structures of the Respiratory System Br B Tb/Rb AD A Lung Diaphragm The conducting portion serves two main functions: 1) to provide a conduit through which air can travel to and from the lungs, 2) to condition the inspired air. 1) In order to ensure that the airways remain open, a combination of cartilage, elastic fibers and smooth muscle provide the conducting portion with a rigid structural support as well as flexibility and extensibility. 2) Before it enters the lungs, inspired air is cleansed, moistened and warmed. To carry out these functions, the mucosa of the conducting portions is lined by a specialized respiratory epithelium, and there are numerous mucous and serous glands, as well as a rich superficial vascular network in the lamina propria. As the air enters the nose, hairs serve to remove coarse particles of dust, etc. Once the air reaches the nasal fossae, particulate and gaseous impurities are trapped in a layer of mucous. This mucous, in conjunction with serous secretions, serves to moisten the incoming air, which protects the delicate alveolar lining from dessication. In addition, the incoming air is warmed by a rich, superficial vascular network. Respiratory Epithelium Most of the conducting portion is lined by a pseudostratified, columnar ciliated epithelium Respiratory Epithelium containing a rich population of goblet cells. This respiratory epithelium continues from the nasal fossae, through the nasopharynx, larynx, trachea, bronchi and larger bronchioles, unchanged except for a gradual decrease in the number of goblet cells. However, the 2 ciliated cells continue all the way into the respiratory bronchioles--these serve to prevent mucous from accumulating in the respiratory portion of the system. The beating of the cilia in an anterior direction serves to move the mucous toward the oral cavity, where it is either swallowed or expectorated. Were this not to occur, we would drown in our saliva. Respiratory epithelium consists of 5 cell types, although only 3 are easily visible under the light microscope: viz: the ciliated columnar cells, mucous goblet cells, and basal cells (which give rise to the other cell types by division and differentiation). Other cell types are brush cells (which contain many microvilli) which have afferent nerve endings on their basal surface, and are considered to be sensory receptors, and small granule cells. Underlying the respiratory epithelium is a lamina propria which contains hyaline cartilage, serous and mucous glands and a rich vascular bed. The former two components decrease in frequency as one passes down the conducting passages. There is a change in the epithelium at the level of the terminal and respiratory bronchioles--there is a loss of goblet cells, and the pseudostratified epithelium changes to a simple columnar/cuboidal (terminal bronchioles) and then to a simple cuboidal epithelium (respiratory bronchioles). Let’s now look at some of the individual portions of this respiratory system starting at the nose and traveling down to the smallest units, the alveolar sacs. Nasal Cavity: The two nasal cavities are separated by a septum. Each cavity is divided into 2 parts: a vestibule, and the internal nasal fossa. The vestibule is the short chamber just internal to the external nasal orifice. It is continuous with the skin of the face and is lined by stratified squamous epithelium which undergoes a transition to typical respiratory epithelium before entering the fossa. The medial wall of the fossa is smooth, but the lateral wall is uneven due to the presence of 3 bony, shelflike projections known as conchae (turbinate bones). The middle and lower conchae are covered by typical respiratory epithelium, while the upper concha is covered by a specialized olfactory epithelium. The narrowed passages formed by the conchae improve the conditioning of the inspired air by increasing the surface area of respiratory epithelium, and by creating turbulence in the air flow, resulting in increased contact with the mucous layer. The rich venous networks in the lamina propria of the respiratory epithelium are capable of becoming greatly engorged with blood. The rich and complexly organized vascular system of the fossae thus results in the efficient warming of the inspired air. Swell bodies are venous plexuses in the lamina propria of conchae. One side swells every 20-30 min, thus directing air through the other nasal fossa 3 and allowing the delicate respiratory epithelium to recover from dehydration. Allergic reactions also cause engorgement of swell bodies, thus restricting air flow. The paranasal sinuses are large airspaces within the frontal, ethmoid, and sphenoid bones and in the maxilla. They open into the nasal cavity. They are covered by typical respiratory epithelium with underlying glands. Coordinated ciliary activity moves the secretions of the sinuses to the nasal cavities. Thus, in its passage through the nasal cavity, air is cleaned, warmed and moistened in preparation for its passage down the trachea to the lungs. Olfactory Epithelium is found only lining a small area of the roof of the nasal cavity and the upper portions of the nasal septum and superior concha. This pseudostratified columnar epithelium with microvilli is modified to serve as a receptor for smell and contains the olfactory cells, which are actually bipolar neurons. The apical surface of the olfactory cells possesses long cilia, which lie parallel to the surface of the epithelium in the fluid secretions of the Bowmans glands Olfactory epithelium These cilia contain receptors for odiferous substances. Excitation of the receptors stimulates cAMP production in the cell, which eventually results in the generation of a receptor potential. The base of the bipolar neuron gives rise to a long axonal process which enters the underlying connective tissue and joins axons of other bipolar olfactory neurons, to form the olfactory nerves (unmyelinated). Two other cell types found in the olfactory epithelium are columnar sustentacular cells with microvilli (probably a metabolically active supportive cell), and basal cells, which are stem cells that can replace both the olfactory cells and the sustentacular cells. The underlying lamina propria contains numerous glands called Bowmans’ glands. These branched, tubuloaveolar glands empty their secretions via ducts onto the olfactory surface. Odoriferous molecules (odorants) dissolve in these secretions, and are then able to stimulate the receptors on the cilia of the olfactory cells. 80% of our sense of taste is due to our sense of smell. When we chew something, the odoriferous molecules that are released stimulate the taste buds, but also the olfactory cells, which can create a much more complex sensation than do the taste receptors. [Taste receptors detect only 5 flavors: sweet, sour, salty, bitter, unami (savory)]. This is why, when your nose is blocked, your sense of taste is greatly diminshed. The olfactory epithelium ends abruptly at a boundary with respiratory epithelium. Pharynx. The pharynx serves both the respiratory and digestive systems as a passageway for air and food. The pharynx communicates anteriorly with the nasal and oral cavities, and are called the nasopharynx and the oropharynx. The nasopharynx is lined with 4 respiratory epithelium, while the oropharynx is surfaced by non-keratinized, stratified squamous epithelium as it is continually abraded by food. Larynx. The larynx is an irregular tube that connects the pharynx to the trachea. It has a cartilaginous framework which serves to maintain an open airway. It serves as the organ of phonation. The epiglottis is a leaflike cartilage which projects from the rim of the larynx and extends into the pharynx. It prevents food from entering the trachea. The epiglottis has a lingual and a laryngeal surface. The entire lingual surface and the apical portion of the laryngeal side are covered with a stratified squamous epithelium, as it is constantly abraded by the passage of food. Larynx Larynx in X-section Larynx Toward the base of the epiglottis, on the laryngeal side, the epithelium undergoes a transition to a typical respiratory epithelium (pseudostratified columnar ciliated with goblet cells). As you know, the epiglottis is comprised of elastic cartilage which allows it to bend easily, thus closing off the larynx during swallowing. Below the epiglottis, the mucosa forms 2 pairs of folds that extend into the lumen of the larynx. The upper pair are the false vocal cords, while the lower pair are the true vocal cords. These are quite easy to distinguish, as the false vocal cords are covered by typical respiratory epithelium with numerous serous glands in the lamina propria, while the true cords are covered by stratified squamous epithelium beneath which is the vocal ligament and bundles of skeletal muscle, the vocalis muscle. This muscle regulates the tension of the fold and its ligaments. When air is made to pass through the larynx, the vocal cords are made to vibrate by the passing air. The vibrations are altered by altering the tension placed on the cords by the vocalis muscle. This change in the vibrations produces sounds of different pitch. Trachea Connecting the larynx to the bronchi is a thin walled tube, the trachea. It extends from the larynx to about the middle of the thorax. This is still part of the conducting system, and like most of the airways, is lined by typical respiratory epithelium. The trachea is lined with 16-20 C-shaped rings of hyaline cartilage, which serve to keep the trachea open. At the posterior, open end of the C, a fibroelastic cartilage and a bundle of smooth muscle (trachealis muscle) bind to the periochondrium. This arrangement allows for expansion and contraction of the lumen and is also used in the cough reflex. 5 Nasal cavity Nasopharynx Oropharynx Larynx Trachea Trachea and Esophagus The Trachea Br B Tb/Rb AD A Lung Diaphragm Bronchial Tree. The bronchial tree stretches from the primary bronchi to the smallest respiratory bronchioles. This bifurcating airway is largely lined with respiratory epithelium, although there are changes in the complexity of this epithelium as we reach down to the smaller bronchioles. The trachea bifurcates into 2 primary bronchi, which enter the lungs at the hilum. Shortly thereafter, the primary bronchi divide to give rise to 3 secondary bronchi in the right lung, and 2 in the left lung. The secondary bronchi divide repeatedly, giving rise to numerous smaller bronchi. The histological features of these bronchi are similar to those of the trachea except that the C-shaped rings of cartilage are replaced by irregular rings, and then by plates of cartilage. Thus, as long as cartilage is present, the airway is classified as a bronchus (large or small). After the bronchi lose their cartilage they are classified as bronchioles. Each bronchiole enters a pulmonary lobule where it branches to form terminal bronchioles. It is here that we start to see major changes in the respiratory epithelium. Bronchioles and terminal bronchioles contain no glands or cartilage and few or no goblet cells. Additionally, the epithelium is reduced to a simple columnar or even cuboidal epithelium, with ciliated cells. Terminal bronchioles also contain specialized secretory cells called Clara cells. These non-ciliated cells secrete a surface active agent (glycosaminoglycan) which probably serves to protect the delicate bronchiolar lining. They also function as stem cells and function in the replacement of ciliated cells. They are also thought to act in the detoxification of harmful substances inhaled into the lungs, through the cytochrome P450 system. An additional feature at this level of the airways is an increased amount of smooth muscle which is wrapped around the bronchiole in criss-crossing bundles. Additionally, the lamina propria contains large numbers of elastic fibers. Thus, the diameter of these airways can change due to contraction of the smooth muscle bundles. Contraction of the smooth muscle of the bronchioles is responsible for the symptoms associated with Asthma—difficulty inhaling and exhaling. 6 Terminal bronchioles are the last portion of a bronchiole, as it leads into a respiratory bronchiole. These are very short, and not easily distinguished. Each terminal bronchiole subdivides into 2 or more respiratory bronchioles that serve as regions of transition between the conducting and respiratory portions of the respiratory system. The mucosa is identical to that of the terminal bronchioles with a simple, ciliated, cuboidal epithelium and Clara cells. A distinguishing feature of respiratory bronchioles is the presence of scattered alveoli budding from the walls of the tubules. The number of alveoli increases distally, until eventually the wall consists only of alveoli and the tube is now called an alveolar duct. Smooth muscle is still present in the columns between adjacent alveoli, but disappears at the distal ends of alveolar ducts. At the termination of the alveolar duct, clusters (3 or 5) of alveoli share a common opening to the alveolar duct. Such a cluster of alveoli is referred to as an alveolar sac. Each alveolar sac may contain many alveoli. The openings of the alveolar sacs and alveoli are surrounded by elastic and reticular fibers. The elastic fibers allow the alveoli to expand upon inspiration and to passively contract upon expiration, while the reticular fibers prevent overdistension of the alveoli, which would cause damage to the delicate capillaries and alveolar septa. Alveoli. The alveoli are the small air sacs with thin walls which allow for the rapid diffusion of gases between the air space and the blood. They are the terminal portions of the bronchial tree and are responsible for the spongy structure of the lungs. The structure 7 of the alveolar walls is specialized for enhancing diffusion between the internal and external environments. Each wall is a partition, or septum, between 2 adjacent alveoli, and is called an interalveolar septum. An interalveolar septum consists of 2 thin squamous epithelial layers between which lie capillaries, elastic and collagen fibers, macrophages and fibroblasts. The capillary network in the septum is the richest in the body, and the extreme thinness of the septum between the capillary lumen and the alveolus allows for the ready exchange of 02 and C02. In order to allow for the free flow of air between the alveoli, the septa are perforated by the alveolar pores Kohn. The interalveolar septum is comprised of 5 main cell types, and can be thought of as a "sandwich" 1. Type I cells which covers 97% of the alveolar surface and comprise the “bread” of the septal sandwich. Tight junctions between these cells contribute towards the blood-air barrier. The main role of this cell is to provide a very thin barrier that is readily permeable to gases. 2. Endothelial cells of the capillaries are extremely thin and comprise the “filling” of the septal sandwich. These are continuous capillaries without fenestrations. In both these types of cells (type I and endothelial), the nucleus and organelles are clustered in order to allow the remaining areas of the cell, across which diffusion of gases occurs, to become extremely thin. These two cell types form a "septal sandwich" which is composed of two type I cells (the bread) and one capillary endothelial cell (the filling). However, the alveolar membrane, across which O2 and CO2 must diffuse, is less than half the thickness of the interalveolar septum, since it consists only of i) the thin cytoplasm of the type I cell, ii) the fused basal laminae of the type I cell and the capillary endothelial cell, and iii) the thin cytoplasm of the capillary endothelial cell. 3. Type II Cells (Great Alveolar Cells) are found located at septal junctions, and bulge slightly into the airspace of the alveolus. Although these cells are as numerous as the type I cells, they cover only 3% of the alveolar surface. These cells are responsible for the synthesis and secretion of pulmonary surfactant, a phospholipid, protein and glycosaminoglycan-rich secretion that spreads over the apical surface of the entire alveolus, providing an extracellular coating that lowers the surface tension of the alveolus. 8 This surfactant facilitates the expansion and contraction of the alveoli. Surfactant is continuously removed by macrophages and replaced by type II cells. (Hyaline membrane disease in newborns is due to insufficient surfactant production, so that the alveoli have difficulty in expanding. Emphysema results from destruction of the alveolar wall, with subsequent reduction in the respiratory portion of the lungs. It is clearly associated with smoking and air pollution). 4. Alveolar macrophages: Chronic inflammation is rare in the lungs due to the presence of macrophages (dust cells) found both within the alveolar septum and on the surface of the alveolar wall. These macrophages scavenge dust and other particles which find their way into the alveoli. They may then be passed up the bronchial tree by the cilia and swallowed; others remain in the connective tissue of the septum and scavenge along the capillary wall. 5. Other cells found within the alveolar septum include fibroblasts, mast cells, brush cells and ‘dust cells’, which are macrophages that are filled up with dust particles, and may remain in the lung for many years. The lungs of smokers and coal miners are filled with such dust cells, and look pretty gross! Pulmonary Blood Supply. Circulation to the lungs includes both nutrient (systemic) and functional (pulmonary) vessels. The functional circulation (i.e. blood to be “treated”) is represented by pulmonary arteries and veins. (Remember, pulmonary arteries carry C02-rich blood, while pulmonary veins carry 02-rich blood). The pulmonary circulation branches and accompanies the bronchial tree. At the level of the respiratory bronchioles/alveolar ducts, the branches of the pulmonary artery form a capillary network which courses in the interalveolar septa between all alveoli. The lung has the most extensive capillary network in the body. Venules which arise from this capillary network enter the interlobular septa (connective tissue septa), and after leaving the lobule, follow the bronchial tree towards the hilum. These venules carry oxygenated blood. The nutrient supply to the lungs is provided by the bronchial arteries which are smaller than the pulmonary vessels. These convey blood to the larger masses of connective tissue of the lung. The arteries extend as far as the respiratory bronchioles, at which point they anastomose with the pulmonary artery and capillaries. Thus, most of the blood entering the lungs via the bronchial arteries leaves by the pulmonary veins (bronchial veins drain only the upper region of the lungs). The lungs, like all other organs are drained by lymphatic vessels. 9 Pleura. The surface of the lung is covered by a serous membrane. It consists of two layers parietal and visceral which are continuous at the region of the hilum. Both layers of the pleura are covered by mesothelial cells which delimit a cavity which is thus lined by these mesothelial cells. In the healthy state, this pleural cavity contains only a film of liquid that allows the smooth sliding of one surface over the other during respiratory movements. In certain pathological states (pleurisy), the pleural cavity can become filled with fluid which is derived from blood plasma by exudation. 10