* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Heart Failure
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Electrocardiography wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart arrhythmia wikipedia , lookup
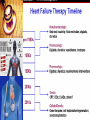
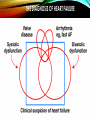
HEART FAILURE Mary Alt, APRN, MSN, CCRN Cardiovascular Institute • Definition • Treatment over time • Causes • Incidence • Risk factors • Risk stratification • Prevention • Conclusion/Future direction QUIZ 1) Initial evaluation of heart failure should include all but the following: a)echocardiogram b)heart catheterization c)clinical presentation d)Lab data 2) Heart failure patients are at a higher risk for sudden cardiac death ? True or False 3)The main underlying cause of fatal arrhythmias is a) Long QTS, Brugada syndrome, congenital problems b) Cardiomyopathy c) Coronary Disease d) Electrolyte Abnormalities 4 )Patients with an Acute MI and low ef (<35%) qualify immediately for ICD? True or False 4 HEART FAILURE-A SYNDROME Heart failure is a constellation of symptoms and signs produced by a complex circulatory and neuro-hormonal response to cardiac dysfunction Heart failure is a complex clinical syndrome that can results from any structural or functional cardiac disorder that impairs the ability of the ventricle to fill with or eject blood. HEART FAILURE~ A LOOK AT THE PAST THE DIAGNOSIS OF HEART FAILURE ECHOCARDIOGRAPHIC EVALUATION OF CHF • LV function (EF),chamber size,wall motion • Segmental dysfunctioncoronary disease • MS-severity, valve area • AS- valve gradient, valve area • AR/MR severity • TR- RV systolic pressure = PA pressure • RV function • R/O IHSS, HCM • R/O Pericardial Disease • R/O rare causes e.g. myxoma, infiltrative disorders- restrictive cardiomyopathy • Diastolic function • Hyperdynamic states 10 CLINICAL CLASSIFICATIONS • Systolic: • Impaired ability of the heart to contract • Weakened muscle, enlarged heart size • Inability of heart to empty • Left ventricular ejection fraction (LVEF) < 40–45% • Diastolic: • inability of the heart to relax is impaired • Stiff, thickened myocardial wall but normal size • Inability of heart to fill • LVEF 45% 11 CLINICAL CLASSIFICATIONS • Acute • sudden onset with associated signs and symptoms • Chronic • secondary to slow structural changes occurring in the stressed myocardium • Acute Decompensated • sudden exacerbation or onset of symptoms in chronic heart failure 12 CLINICAL CLASSIFICATIONS Heart Failure is a Symptomatic Disorder New York Heart Association-Functional Classification Class I: No abnormal symptoms with activity Class II: Symptoms with normal activity Class III: Marked limitation due to symptoms with less than ordinary activity Class IV: Symptoms at rest and severe limitations in functional activity 13 CLINICAL CLASSIFICATIONS Heart Failure is a Progressive Disorder ACC/AHA Stages of HF Stage A--Presence of risk factors for heart failure Stage B--Presence of structural heart disease but no Symptoms Stage C--Presence of structural heart disease along with signs and symptoms Stage D--Presence of structural heart diseases and advanced signs and symptoms SEVERITY OF HEART FAILURE AND MODES OF DEATH 12% 26% 64% 24% 59% 15% 33% NYHA Class II n = 103 56% 11 % NYHA Class IV n = 27 NYHA Class III n = 103 CHF Other Sudden Death SCD RATES IN CHF PATIENTS WITH LV DYSFUNCTION Control Group Mortality % 50 Total Mortality Sudden Death 44 42 41 39.7 40 30 20 20 19 17 15 11 9 10 7 6 8 4 0 CHF-STAT GESICA SOLVD V-HeFT I MERIT-HF CIBIS-II CARVEDILOL-US 45 months 13 months 41.4 months 27 months 12 months 16 months 6 months Total Mortality ~15-40%; SCD accounts for ~50% of the total deaths % Sudden Cardiac Deaths RELATION OF LVEF TO RISK OF SCA 8 7.5% 7 6 5.1% 5 4 2.8% 3 2 1.4% 1 0 0-30% 31-40% 41-50% LVEF > 50% Note: 56.5% of all SCA victims had an LVEF < 30% SCA RELATIONSHIP TO HF • Patients with HF are overall at 6-9 times higher risk for SCD than general population • As HF progresses, pump failure (rather than SCA) becomes relatively more likely as the cause of death Heart Disease and Stroke Statistics—2005 Update. AHA. www. americanheart.org SCD IN HEART FAILURE Despite improvements in medical therapy, symptomatic HF still confers a 20-25% risk of premature death in the first 2.5 years after diagnosis.1,2 50% of these premature deaths are SCD CORONARY HEART DISEASE Coronary heart disease and its consequences account for the majority of sudden cardiac deaths. 5% Other* 15% Nonischemic Cardiomyopathy 80% Coronary Heart Disease *ion-channel abnormalities, valvular or congenital heart disease, other causes MYOCARDIAL INFARCTION • Prior myocardial infarctions are identified in as many as 50-75% of SCA victims. • Therapeutic innovations in the last decade* have improved initial survival in patients with reduced ejection fraction and may have altered the epidemiology of post-MI risk. *including early and aggressive revascularization and effective pharmacologic therapy 2006 ACC/AHA/ESC GUIDELINES FOR THE MANAGEMENT OF VENTRICULAR ARRHYTHMIAS: PRIMARY PREVENTION OF SCD ICD Class I Recommendations: • Patients with ischemic cardiomyopathy who are at least 40 days post-MI with an LVEF ≤ 35% and NYHA functional class II or III • Patients with NYHA Class II-III, LVEF ≤ 30 - 35%, non-ischemic cardiomyopathy • Patients who are at high risk of SCA due to genetic disorders such as long QT syndrome, Brugada syndrome, hypertrophic cardiomyopathy and arrhythmogenic right ventricular dysplagia (ARVD). ICD Class II Recommendation: • Ischemic and non-ischemic patients with NYHA functional class I, LVEF ≤ 30-35% Zipes, DP, et al. 2006 ACC/AHA/ESC Practice Guidelines 5. Circulation. 2006;114;385-484 PRIMARY PREVENTION ADVANCED HEART DISEASE SECONDARY PREVENTION AFTER SCA ...patients who have already experienced a life-threatening ventricular tachyarrhythmia event... SCD TREATMENT OPTIONS AED & 911 EMS Response The success of community-based resuscitation is low, with a median survival of 6.4% in communities with defibrillatorequipped EMS.22 Implantable Defibrillators Limitations • Medicare Waiting Periods • Potential Scheduling Delays • “Not Covered” Indications such as NYHA Class IV patients SCA RESUSCITATION SUCCESS VS. TIME* Chance of success reduced 100 90 7-10% each minute 80 70 60 % Success *Non-linear 50 40 30 20 10 0 1 2 3 4 5 6 Time (minutes) Cummins RO. Annals Emerg Med. 1989;18:1269-1275. 7 8 9 SCD TREATMENT OPTIONS Wearable Defibrillator • Non-invasive • No Clinical intervention required • Reduces Time to Treatment (< 60 Secs) • 98% First Shock Success Rate • 92% Survival to ER • Covered During ICD “Waiting Periods” • Post MI – 40 Days • Post PCI/CABG – 90 Days • NICM/DCM – 90 – 270 Days LIFEVEST SYSTEM ECG Electrodes • Dry & nonadhesive • 4 electrodes providing 2 channels of monitoring Self-Gelling Defibrillation Electrodes Response Buttons Monitor • 1.8 lbs. • 150 joule biphasic shock • Stores ECG, daily use, etc. LIFEVEST BY THE NUMBERS • Over 50,000 patients have worn the LifeVest • Currently Saving a Patient every 2 Days • 700 Patients have been saved by the LifeVest • 98% first shock success rate • 92% shocked event survival (conscious to ER arrival or stayed at home) • Average duration of use is 2 to 3 months • Median daily use is 94% (22.4 hours/day) LIFE VEST QUICK REFERENCE GUIDE Sustained VT (> 30 Seconds) - or - Low EF (35% or less) - or - with Previous MI or NICM/DCM ICD Explant CONCLUSIONS • Pharmacologic and device therapies are effective in preventing SCD and overall mortality in high risk post-MI and HF patients: – Beta-blockers – ACE inhibitors – Aldosterone Receptor Blockade Drugs (HF) – ICD therapy • Prophylactic use of ICD therapy prevents SCD and saves lives in patients with CAD and LV dysfunction, who are also on optimal pharmacologic therapies. QUIZ 1) Initial evaluation of heart failure should include all but the following: a)echocardiogram b) heart cath c)clinical presentation d)Lab data 2) Heart failure patients are at a higher risk for sudden cardiac death ? True or False 3)The main underlying cause of fatal arrhythmias is a) Long QTS, Brugada synd, congenital problems b) Cardiomyopathy c) Coronary Disease d) Electrolyte Abnormalities 4 )Patients with an Acute MI and low ef (<35%) qualify immediately for ICD? True or False Thank you