* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Protocol for dealing with suspected anthrax in Ireland
Survey
Document related concepts
Transcript
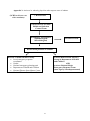
Protocol for dealing with suspected anthrax in Ireland Immediate steps to be taken in the event of the discovery of a suspect package Call Gardai (999 or 112). Gardai to tightly seal off site and to carry out preliminary investigation If suspicious, Gardai to contact -Army -Fire and Ambulance Services and -Directors of Public Health Fire and ambulance services (decontamination units) to carry out decontamination of exposed individuals on site using mobile units. Army to carry out decontamination of environment if required. Army will arrange transport of all clinical and environmental specimens to Public Health Laboratory in Cherry Orchard Hospital. Director of Public Health to get a list of exposed individuals, to ensure that the correct clinical specimens are taken and to ensure that appropriate chemoprophylaxis is given. 2 1. Description of Agent/ Syndrome a. Aetiology Anthrax is an acute infectious disease caused by Bacillus anthracis, a spore forming, gram-positive bacillus. Associated disease occurs most frequently in animals which acquire spores through ingestion of contaminated soil. Humans can become infected through skin contact, ingestion, or inhalation of B. anthracis spores from infected animals or animal products or through bioterrorism. Person-to-person transmission of inhalational disease does not occur. Direct exposure to vesicle secretions of cutaneous anthrax lesions may result in secondary cutaneous infection. b. Clinical features Human anthrax infection can occur in three forms: pulmonary, cutaneous, or gastrointestinal, depending on the route of exposure. Of these forms, pulmonary anthrax is associated with bioterrorism exposure to aerosolised spores. Clinical features for each form of anthrax include: Pulmonary Non-specific prodrome of flu-like symptoms follows inhalation of infectious spores. Possible brief interim improvement. Two to four days after initial symptoms, abrupt onset of respiratory failure and hemodynamic collapse, possibly accompanied by thoracic edema and a widened mediastinum on chest radiograph suggestive of mediastinal lymphadenopathy and hemorrhagic mediastinitis. Gram-positive bacilli on blood culture, usually after the first two or three days of illness. Treatable in early prodromal stage. Mortality remains extremely high despite antibiotic treatment if it is initiated after onset of respiratory symptoms. Cutaneous Local skin involvement after direct contact with spores or bacilli. Commonly seen on the head, forearms or hands. Localized itching, followed by a papular lesion that turns vesicular, and within 2-6 days develops into a depressed black eschar. Usually non-fatal if treated with antibiotics. Gastro-intestinal Abdominal pain, nausea, vomiting, and fever following ingestion of contaminated food,usually meat. Bloody diarrhoea, hematemesis. Gram-positive bacilli on blood culture, usually after the first two or three days of illness. Usually fatal after progression to toxemia and sepsis. c. Modes of transmission The spore form of B. anthracis is durable. As a bioterrorism agent, it could be delivered as an aerosol. The modes of transmission for anthrax include: Inhalation of spores. 3 Cutaneous contact with spores or spore-contaminated materials. Ingestion of contaminated food. d. Incubation period The incubation period following exposure to B. anthracis ranges from 1 day to 8 weeks (average 5 days), depending on the exposure route and dose: 2-60 days following pulmonary exposure. 1-7 days following cutaneous exposure. 1-7 days following ingestion. e. Period of communicability Transmission of anthrax infections from person to person is unlikely. Airborne transmission does not occur, but direct contact with skin lesions may result in cutaneous infection. 2. Preventive Measures Vaccination against anthrax is not recommended for the general public to prevent disease. 3. Infection control practices for management of patients with anthrax Standard precautions are used for the care of patients with anthrax. (Standard precautions include the routine use of gloves for contact with nonintact skin, including rashes and skin lesions). Patient placement Private room placement for patients with anthrax is not necessary. Airborne transmission of anthrax does not occur. Skin lesions may be infectious, but this requires direct skin contact. Patient transport Standard precautions should be used for transport and movement of patients with B. anthracis infections. Cleaning, disinfection, and sterilisation of equipment and environment Principles of standard precautions should be generally applied for the management of patient-care equipment and for environmental control. Hypochlorite is the disinfectant of first choice with hydrogen peroxide, peracetic acid or glutaraldehyde as alternatives. Spores require steam sterilisation, autoclaving or burning to effectively disinfect. Fumigation and chemical disinfection can be used for valuable equipment. Post-mortem care Standard precautions should be used for post-mortem care. (Standard precautions include wearing appropriate personal protective equipment, including masks and eye protection, when generation of aerosols or splatter of body fluids is anticipated).Full post mortems however are not recommended in cases of anthrax. 4 4. Post Exposure Management a. Decontamination of patients (To be carried out by the fire brigade and ambulance services) The risk for re-aerosolization of B. anthracis spores appears to be extremely low in settings where spores were released intentionally. In situations where the threat of gross exposure to B. anthracis spores exists, cleansing of skin and potentially contaminated fomites (e.g. clothing or environmental surfaces) may be considered to reduce the risk for cutaneous and gastrointestinal forms of disease. The plan for decontaminating patients exposed to anthrax may include the following: Instructing patients to remove contaminated clothing and possessions and store in labeled, plastic bags. Handling clothing minimally to avoid agitation. Instructing patients to shower thoroughly with soap and water (and providing assistance if necessary). Instructing attending personnel regarding Standard Precautions and wearing appropriate barriers (e.g. gloves, gown and surgical masks) when handling contaminated clothing or other contaminated fomites. Decontaminating environmental surfaces using an approved sporicidal/germicidal agent or 0.5% hypochlorite solution (one part household bleach added to nine parts water). The emergency services (fire brigade and ambulance services) will provide mobile decontamination units. Emergency staff should avoid close contact with exposed persons until they have been decontaminated. b. Prophylaxis and post-exposure immunisation All patients with suspected anthrax exposure should be commenced immediately on chemoprophylaxis. Prophylaxis should continue until B. anthracis exposure has been excluded. If exposure is confirmed, prophylaxis should continue for 8 weeks. During this period, no special precautions are required for exposed persons. However they should receive an anthrax information sheet and be instructed to seek medical attention immediately in the event of any suspicious symptoms developing. Table 1. Recommended post-exposure prophylaxis after exposure to Bacillus anthracis Antimicrobial agent Adults Children Oral fluoroquinolones Ciprofloxacin 500mg bd 20-30mg per kg of body mass daily, divided into two doses – as a guide 10kg: 125mg bd 20kg: 250mg bd 30kg: 375mg bd 40kg: as for adult If fluoroquinolones are not available or are contraindicated Doxycycline 100mg bd 5mg per kg body mass per day divided into two doses Paediatric use of fluoroquinolones and tetracyclines can be associated with adverse effects that must be weighed against the risk of developing a lethal disease. 5 If B.anthracis exposure is confirmed, the organism must be tested for penicillin susceptibility. If susceptible, exposed children may be treated with oral amoxycillin 40mg per kg of body mass per day divided with doses 8 hourly (not to exceed 500mg, three times daily). (c) Treatment The treatment for anthrax is shown below in Table 2. Table 2: Recommended treatment for inhalation and ingestion anthrax Initial Therapy Optional therapy if strain is proven susceptible Duration Adults Ciprofloxacin 400mg iv every 12hr (change to oral 500 mg bd when appropriate) Penicillin G. 4 million iU iv every 4hr (change to oral therapy when appropriate) 8 weeks Children* Ciprofloxacin 20-30mg/kg per day iv divided into 2 daily doses, not to exceed 1g per day Age <12y: penicillin G 50,000 iu/kg iv every 6hr Age 12y: penicillin G 4million iu iv every 4hr (change to oral therapy when appropriate) 8 weeks Pregnancy Same as for non pregnant adult *Ciprofloxacin is not licensed for use in children or pregnant women. Change to oral therapy when considered appropriate. Note that cephalosporins are ineffective for the treatment of anthrax. Treatment of cutaneous anthrax is with oral Ciprofloxacin 500mg bd for 7 days. This can be changed to penicillin if the organism is found to be sensitive. Contacts of cases There is no need to provide antibiotic prophylaxis or immunisation to contacts of patients unless there is concern that they were also exposed to the initial release. (d) Environmental decontamination (To be carried out by the army) The greatest risk to human health following a release of anthrax spores occurs during the period in which anthrax spores remain airborne, called primary aerosolisation. The duration and scale of the infectious risk depends on the duration for which spores remain airborne and the distance they travel before they fall to the ground. This depends on meteorological conditions and aerobiological properties of the dispersed aerosol. The aerosol is likely to be fully dispersed within hours to 1 day at most, well before the first symptomatic cases would be seen. An exposed zone will be defined according to the time and place of release in order to identify all persons exposed to primary aerosolisation. The area surrounding the site of release will remain designated as an exposed zone until sufficient time has elapsed and the risk of infection has subsided. Once the spores have settled, although they remain infectious for long periods, the risk to human health is much lower. 6 Decontamination of small areas may be achieved with 0.5% hypochlorite solution (one part household bleach added to nine parts water). The room in which the package and other areas of the building deemed to be contaminated should remain tightly sealed until results from the suspicious substance are known. If they are positive further advice in decontamination will be provided. If this advice is not deemed feasible, decontamination of the exposed zone may be achieved as described above. Protection of frontline workers This includes all emergency staff involved in management at the scene of a release, as well as those involved in treating patients with anthrax. Protective clothing The exposed zone presents a high risk of infection, and anyone entering it should wear full protective equipment including high-efficacy air filter masks conferring full biological protection. Healthcare workers will not normally be asked to enter this zone. It is possible, however, that they may be called to treat casualties, for example if an explosive device has accompanied the release of biological agent. In this case the appropriate protective clothing should be worn. Exposed persons will normally be moved from the exposed zone, through decontamination, and into a holding area for medical assessment and administration of prophylactic treatment. Those involved in decontamination, and others who have who have any contact with contaminated clothing and fomites should observe standard l Precautions - gloves, masks, gowns, eye protection and hand washing. Emergency staff who attend exposed persons after decontamination has been completed do not need to take any special precautions. For healthcare workers involved in the management of hospitalised patients with all forms of anthrax, standard precautions provide sufficient protection, and mortuary staff should use similar barrier protection. More sophisticated countermeasures for airborne protection such as high-efficacy air filter masks airborne protection are not required. Antibiotic prophylaxis and immunisation Healthcare workers entering the exposed zone should be offered antibiotic prophylaxis as in Table 1. Prophylactic treatment may also be considered for frontline workers involved in other activities including: Handling exposed persons. Management of patients or disposal of bodies infected with anthrax. Decisions about who should receive prophylaxis should be taken on an individual basis according to duration and degree of potential exposure, and taking into account the availability and side effects of prophylactic treatments. 7 5. Laboratory Support and Confirmation B anthracis is a hazard group 3 pathogen. All laboratory procedures should be performed in a Containment Level 3 laboratory using a Class 1 microbiology safety cabinet by experienced medical laboratory scientists. Diagnosis of anthrax is confirmed by aerobic culture performed in a CL-3 laboratory. Use of standard precautions (gloves, masks, gowns, eye protection and hand washing) in the laboratory reduces the risk of cutaneous anthrax to zero. Samples to be taken from humans negative). Nasal swabs (laboratory diagnosis is easier if these are sent dry since this prevents growth of other organisms and facilitates detection of anthrax spores). Swabs from cutaneous lesions. ALL HUMAN SAMPLES SHOULD BE SENT TO THE PUBLIC HEALTH LAB IN CHERRY ORCHARD HOSPITAL. Samples to be taken from the environment Samples should be taken from any material (soil, dust, clothing, swabbing etc) present in the environmental area thought to have been exposed to the release of anthrax spores, or soiled by exudates from humans. ALL ENVIRONMENTAL SAMPLES SHOULD BE SENT TO THE PUBLIC HEALTH LAB IN CHERRY ORCHARD HOSPITAL WHO WILL SEND THEM ON TO THE UK. Post mortem specimens Samples may be taken from dead humans to assist diagnosis, including: Blood (approx 10ml) from a vein Swabs of haemorrhagic exudate from orifices. Swabs or sample of other body fluids if appropriate. However full post-mortems are discouraged if anthrax is suspected because of the risk of releasing anthrax spores present in body fluids, drips etc. Procedure Phone laboratory to inform them that samples are on their way (01)6206175 office hours/ (01)6264702 out of hours To accompany sample -Put code on sample (BAB/number of sample) -Brief details of incident -Name of doctor in charge -Contact telephone number of doctor in charge 8 Appendix 1: Adapted from CDC Health Advisory document HOW TO HANDLE ANTHRAX AND OTHER BIOLOGICAL AGENT THREATS Many facilities in the USA have received anthrax threat letters. Most were empty envelopes; some have contained powdery substances. The purpose of these guidelines is to recommend procedures for handling such incidents. DO NOT PANIC 1. Anthrax organisms can cause infection in the skin, gastrointestinal system, or the lungs. To do, so the organism must be rubbed into abraded skin, swallowed, or inhaled as a fine, aerosolized mist. Disease can be prevented after exposure to the anthrax spores by early treatment with the appropriate antibiotics. Anthrax is not spread from one person to another person. 2. For anthrax to be effective as a covert agent, it must be aerosolized into very small particles. This is difficult to do, and requires a great deal of technical skill and special equipment. If these small particles are inhaled, life-threatening lung infection can occur, but prompt recognition and treatment are effective. SUSPICIOUS UNOPENED LETTER OR PACKAGE MARKED WITH THREATENING MESSAGE SUCH AS “ANTHRAX”: 1. Do not shake or empty the contents of any suspicious envelope or package. 2. PLACE the envelope or package in a plastic bag or some other type of container to prevent leakage of contents. 3. If you do not have any container, then COVER the envelope or package with anything (e.g., clothing, paper, trash can, etc.) and do not remove this cover. 4. Then LEAVE the room and CLOSE the door, or section off the area to prevent others from entering (i.e., keep others away). 5. WASH your hands with soap and water to prevent spreading any powder to your face. 6. What to do next… If you are at HOME, then report the incident to the Gardai. If you are at WORK, then report the incident to the Gardai, and notify your building security official or an available supervisor. 7. LIST all people who were in the room or area when this suspicious letter or package was recognized. Give this list to both the local public health authorities and the gardai for follow-up investigations and advice. 9 ENVELOPE WITH POWDER AND POWDER SPILLS OUT ONTO SURFACE: 1. DO NOT try to CLEAN UP the powder. COVER the spilled contents immediately with anything (e.g., clothing, paper, trash can, etc.) and do not remove this cover! 2. Then LEAVE the room and CLOSE the door, or section off the area to prevent others from entering (i.e., keep others away). 3. WASH your hands with soap and water to prevent spreading any powder to your face. 4. What to do next… If you are at HOME, then report the incident to the Gardai. If you are at WORK, then report the incident to the Gardai, and notify your building security official or an available supervisor. 5. REMOVE heavily contaminated clothing as soon as possible and place in a plastic bag, or some other container that can be sealed. This clothing bag should be given to the emergency responders for proper handling. 6. SHOWER with soap and water as soon as possible. Do Not Use Bleach Or Other Disinfectant On Your Skin. 7. If possible, list all people who were in the room or area, especially those who had actual contact with the powder. Give this list to both the local public health authorities so that proper instructions can be given for medical follow-up, and to the Gardai for further investigation. QUESTION OF ROOM CONTAMINATION BY AEROSOLIZATION: For example: small device triggered, warning that air handling system is contaminated, or warning that a biological agent released in a public space. 1. Turn off local fans or ventilation units in the area. 2. LEAVE area immediately. 3. CLOSE the door, or section off the area to prevent others from entering (i.e., keep others away). 4. What to do next… - If you are at HOME, then dial “999” to report the incident to Gardai. If you are at WORK, then dial “999” to report the incident to Gardai and notify your building security official or an available supervisor. 5. SHUT down air handling system in the building, if possible. 10 6. If possible, list all people who were in the room or area. Give this list to both the local public health authorities so that proper instructions can be given for medical followup, and to law enforcement officials for further investigation. HOW TO IDENTIFY SUSPICIOUS PACKAGES AND LETTERS Some characteristics of suspicious packages and letters include the following… Excessive postage Handwritten or poorly typed addresses Incorrect titles Title, but no name Misspellings of common words Oily stains, discolorations or odour No return address Excessive weight Lopsided or uneven envelope Protruding wires or aluminum foil Excessive security material such as masking tape, string, etc. Visual distractions Ticking sound Marked with restrictive endorsements, such as “Personal” or “Confidential” Shows a city or state in the postmark that does not match the return address 11 Appendix 2: Summary of steps to be taken if a case of anthrax is suspected by a medical practitioner in a health care institution 1. Notify case or suspected case to Director of Public Health 2. Patient to be commenced on oral ciprofloxacin as per protocol. 3. Clinical samples to be taken including blood cultures and nasal swab. 4. Standard precautions to be used include the routine use of gloves for contact with non-intact skin, including rashes and skin lesions. 5. Private room placement for patients with anthrax is not necessary. 6. Standard precautions should be used for transport and movement of patients with suspected anthrax infection and for the management of patient-care equipment and for environmental control. 12 Appendix 3: Action to be taken by physician who suspects case of anthrax (NCHD to discuss case with consultant) ? Bioterrorism Notify Director of Public Health and Infection Control Team Preliminary investigation (epidemiological/ microbiological) Not Bioterrorism Bioterrorism probable or definite Director of Public Health to notify Local emergency response coordinator Gardai National emergency planning unit Department of Health and Children National Disease Surveillance Centre National Disease Surveillance Centre Activate Bioterrorism Advisory Group in Department of Health and Children AND Activate National Major Emergency Response Team (inter-agency/ interdepartmental) 13 Appendix 4: Summary of steps to be taken if a case of anthrax is notified to a Director of Public Health Establish local group with public health, environmental health and microbiological representation to oversee epidemiological investigation. Commence epidemiological investigation. (Health Board CEOs to make arrangements for appropriate 24 hour cover). Director of Public Health to contact Department of Health and Children and National Disease Surveillance Centre immediately bioterrorist attack is suspected. Notify Directors of Public Health in other health board areas. Allocate extra public health staff to affected area. Provide information to A&E departments, laboratories, GPs and other clinicians. Liaise with communication director. Provide regular information to public via media, telephone helplines, website etc. Bioterrorism plan should be integrated with local emergency planning In the event that the suspect package contains anthrax, an information leaflet should be circulated to all exposed persons with advice on actions to be taken in the event of developing suspicious symptoms. 14 Contacts Dr Brian O’Herlihy Director of Public Health Eastern Regional Health Authority Steevens Hospital Dublin 8 Dr Orlaith O’Reilly Director of Public Health South Eastern Health Board Head Office Lacken Dublin Road Kilkenny Dr Declan McKeown Director of Public Health Western Health Board Merlin Park Galway Dr Rosaleen Corcoran Director of Public Health North Eastern Health Board Kells Co. Meath Dr Pat Doorley Director of Public Health Midland Health Board Arden Road Tullamore Co. Offaly Dr Sean Denyer Director of Public Health North Western Health Board Manorhamilton Co. Leitrim Dr Kevin Kelleher Director of Public Health Mid Western Health Board 31-33 Catherine Street Limerick Dr Elizabeth Keane Director of Public Health Southern Health Board Sarsfield House Sarsfield Road Wilton Cork Tel: 01-635 2170 Fax: 01-671 0606 Email [email protected] Tel: 056 51702 Fax: 056 70842 [email protected] Tel: 091 751131 Fax: 091 758 283 [email protected] Tel: 046 49145 Fax:046 72325 [email protected] Tel: 0506 21868 Fax: 0506 51760 [email protected] Tel: 072 55123 Fax: 072 55627 [email protected] Tel: 061 316655 Fax: 061 316870 [email protected] Tel: 021 346060 Fax: 021 346063 [email protected] 15 Dr. Darina O’Flanagan Director National Disease Surveillance Centre Sir Patrick Dun’s Hospital Lower Grand Canal St Dublin 2 Dr John Devlin Tel: 01-6617346 Fax: 01-6617347 [email protected] Tel: 01-6354249 Deputy Chief Medical Officer Deot of Health and Children Dublin 2 Professor William Hall Director Virus Reference Laboratory Belfield Dublin 4 Cherry Orchard Hospital David Sexton Defence forces Fire and ambulance services Tel: 01-7061354 Fax: 01-2697611 [email protected] Tel: 01-6206175 (office hours) 01-6264702 (out of hours) Tel – 01-8042624 Pager 2003110 Tel – 999 or 112 16