* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Sexology - Doctors.am
History of homosexuality wikipedia , lookup
Sexual objectification wikipedia , lookup
Hookup culture wikipedia , lookup
Sexual assault wikipedia , lookup
Adolescent sexuality wikipedia , lookup
Incest taboo wikipedia , lookup
Human sexual activity wikipedia , lookup
Sexual racism wikipedia , lookup
Erotic plasticity wikipedia , lookup
Sexuality after spinal cord injury wikipedia , lookup
Sexual fluidity wikipedia , lookup
Human male sexuality wikipedia , lookup
Sexual abstinence wikipedia , lookup
Age of consent wikipedia , lookup
Sex and sexuality in speculative fiction wikipedia , lookup
Heterosexuality wikipedia , lookup
Ages of consent in South America wikipedia , lookup
Sexual selection wikipedia , lookup
Sex in advertising wikipedia , lookup
Penile plethysmograph wikipedia , lookup
Sexological testing wikipedia , lookup
Sexual reproduction wikipedia , lookup
Ego-dystonic sexual orientation wikipedia , lookup
Sexual addiction wikipedia , lookup
Sexual stimulation wikipedia , lookup
Female promiscuity wikipedia , lookup
Sexual dysfunction wikipedia , lookup
Sexual ethics wikipedia , lookup
History of human sexuality wikipedia , lookup
Slut-shaming wikipedia , lookup
Rochdale child sex abuse ring wikipedia , lookup
Lesbian sexual practices wikipedia , lookup
Human female sexuality wikipedia , lookup
Yerevan State Medical University after M. Heratsi
Department of Sexology
Nersisyan N.R, Azatyan R.E.
Clinical Sexology
Handout on Clinical Sexology
for foreign students of general medicine faculty
2008
Yerevan State Medical University after M.Heratsi
Department of Sexology
Nersisyan N.R, Azatyan R.E.
Clinical Sexology
Handout on Clinical Sexology for foreign students of
general medicine faculty
Yerevan, YSMU,
2008
UDS 616.89-008.442(07)
This handout is adopted by the Methodical
Commission of Foreign Students of the YSMU
Recenzent: Narimanyan Z. Michail
Chairman of department Family Medicine of YSMU
Recenzent: Gasparyan Kh.
Chairman of department Medical Psychology
Edited by prof. Hakobyan E. Aram
ISBN 978-99941-40-77-0
©Nersisyan N., Azatya R.
ºñ¨³ÝÇ Ø. лñ³óáõ ³Ýí³Ý å»ï³Ï³Ý µÅßÏ³Ï³Ý Ñ³Ù³Éë³ñ³Ý
ê»ùëáÉá·Ç³ÛÇ ³ÙµÇáÝ
Ü»ñëÇëÛ³Ý Ü.è.,²½³ïÛ³Ý è.¾.
ÎÈÆÜÆÎ²Î²Ü êºøêàÈà¶Æ²
àõëáõÙÝ³Ï³Ý Ó»éݳñÏ
ÎÉÇÝÇÏ³Ï³Ý ë»ùëáÉá·Ç³ÛÇ Ó»éݳñÏ
ÀݹѳÝáõñ µÅßÏáõÃÛ³Ý ý³ÏáõÉï»ïÇ
ûï³ñ»ñÏñ³óÇ áõë³ÝáÕÝ»ñÇ Ñ³Ù³ñ
ºñ¨³ÝÇ Ø.лñ³óáõ ³Ýí³Ý
å»ï³Ï³Ý µÅßÏ³Ï³Ý Ñ³Ù³Éë³ñ³ÝÇ Ññ³ï³ñ³ÏáõÃÛáõÝ
2008
Preface
4
Preface
The book has been written on the foreign students’ advice and the
aim of the book is to be of concrete assistance to future physicians, as
they deal with the day-to-day concerns of their patients in sexual matters.
The first chapters of the book discuss the psychosexual
development and male/female sexual manifestations, the other chapters
are devoted to classification of sexual disorders. The book centers on
etiology, differential diagnosis, and clinical description of sexual
dysfunctions, and consequently, it suggests effective methods of
treatment. It also covers evaluation of sexual disorders, paraphilias and
briefly some aspects of male reproductive function. The book mainly
contains factual information and, therefore, provides a very thoroughly
and carefully organized introduction to the whole of clinical sexology. It
does not restrict to clinical and therapeutic aspects, but it also includes
psychological, biological and sociological contributions. The last part of
the book presents tests related to each subject covered in the book.
The book is initially intended for medical students, and it also can
be meant for sexologists, psychologists, psychiatrists, psychotherapists,
sociologists and for the other specialists.
We welcome any comment, well-founded criticism, and
recommendation on the practical value of this book so that we can strive
to come even closer to realization of that objective in succeeding
editions.
Acknowledgments
Acknowledgments
We are gratefully acknowledged to everyone associated
with production of this book. We would like to express our most
sincere gratitude to members of department of sexology and Special
thanks to Hakobyan S.V.,Vardanyan G.V., Grigoryan A.D., and as
consultant Davtyan R.M. We would also like to extend our special
thanks to Bisharyan M.N. from department of foreign languages at
YSMU.
5
CONTENTS
6
CONTENTS
Preface ........................................................................................................................... 4
Acknowledgments...................................................................................................... 5
CONTENTS .................................................................................................................... 6
Chapter 1 The subject of clinical sexology and its methodological
approaches ................................................................................................................... 8
Paradigms in sexology .......................................................... 9
Chapter 2 Psychosexual development through the life cycle ................. 11
Prenatal influences .................................................................................................. 13
Parapuberty (1 to 7 Years) .................................................................................. 15
Infancy (Birth to 15 Months) ............................................... 15
Toddlerhood (15 Months to 3 Years) .................................... 16
Preschool Period (3 to 7 Years) ............................................ 17
Prepuberty (7 to 11 Years) .................................................................................. 19
Puberty (11 to 16 Years) ...................................................................................... 20
Transitional period to mature sexuality (17 to 25 Years) ........................ 23
Mature sexuality (25 to 55 Years) .................................................................... 23
Involution (55 to 70 Years) ................................................................................. 26
Sexual constitution
27
Chapter 3 Sexual response cycle ...................................................................... 33
The desire phase ...................................................................................................... 36
Anatomy........................................................................... 37
Physiological mechanisms ................................................... 38
Disorders of desire phase ................................................... 40
The excitement phase ............................................................................................ 40
Male excitement - Erection .................................................. 40
Female excitement............................................................. 43
Disorders of excitement phase ............................................ 45
The orgasm phase ................................................................................................... 46
Disorders of the orgasm phase ............................................ 49
Chapter 4 Sexual disorders ................................................................................. 51
Classification of sexual disorders ....................................................................... 51
Disorders of sexual desire .................................................................................... 57
Female sexual arousal disorder.......................................................................... 69
Female orgasmic disorder .................................................................................... 77
Vaginismus ................................................................................................................. 83
Male orgasmic disorder ......................................................................................... 85
Male erectile dysfunction ...................................................................................... 93
Ejaculatory Pain Due to Muscle Spasm of the Male Genitals ................ 101
CONTENTS
7
Sexual Phobias and Avoidance ......................................................................... 102
Chapter 5 Paraphilias ........................................................................................... 104
Chapter 6 Gender identity disorders .............................................................. 111
Childhood .................................................................................................................. 112
Chapter 7 Ego-dystonic homosexuality ........................................................ 121
Varieties of homosexual expression ............................................................... 123
Preferential or obligatory homosexuality ............................. 123
Pseudohomosexuality ....................................................... 124
Situational homosexuality ................................................. 125
Exploitative homosexuality................................................ 125
Enforced homosexuality .................................................... 125
Chapter 8 Evaluation of sexual disorders ..................................................... 127
Chapter 9 Treatment of sexual disorders ..................................................... 134
Psychotherapy of sexual disorders ................................................................. 134
1.
Hypnosis .............................................................. 134
2.
Adlerian therapy .................................................... 134
3.
Behavior therapy ................................................... 135
4.
Existential therapy ................................................. 136
5.
Gestalt therapy ..................................................... 136
6.
Person-centered therapy ........................................ 136
8.
Psychoanalytic therapy ........................................... 137
9.
Rational-emotive and Cognitive-behavioral Therapy ... 138
10.
Male reproductive function ...................................... 138
11.
Transactional Analysis ............................................ 143
12.
Sex therapy .......................................................... 144
Pharmacological therapy of sexual disorders.............................................. 144
Tests ........................................................................................................................... 146
Keys ............................................................................................................................ 156
References ................................................................................................................ 157
The subject of clinical sexology and its methodological approaches
8
Chapter 1
The subject of clinical sexology and its
methodological approaches
Clinical sexology is a medical discipline which studies
behavioral, personal and emotional aspects of sexual
functioning and develops methods of diagnosis, treatment and
prevention of sexual disorders.
At the beginning of development of sexology it is
considered that the cause of sexual disorders is the presence of
any basic disease (endocrine, urological, psychiatric), and
patients were treated by the specialist who was competent in
treatment of these diseases.
But very often sexual
dysfunction presents itself, e. without any coexisting basic
disease. Furthermore, more resistant and hard-to-cure sexual
disorders were observed at those patients whose thorough
urological, endocrine, neurological and psychiatric examination
did not find out any aberration. On the contrary, during serious
illnesses, both somatic and mental, complete sexual health
might be observed.
Both in our country and abroad, doctors undoubtedly
confirm that sexuality is the integration of several dimensionssomatic, emotional, intellectual, social and ethical. In order to
sexual health could be maintained complex and integrated
interactions of different functional systems are required.
To summarize methodological approaches in sexology
three of them could be mentioned:
1. Monodisciplinary approach - is limited to a service of
only one expert: urologist, gynecologist, endocrinologist,
neurologist, psychiatrist, clinical psychologist, marriage and
family therapist, sociologist. Several aspects of sexual health
are viewed separately.
2. Multidisciplinary approach - Various specialists work
together to understand and treat patients referred to medical
center with a wide variety of sexual problems. Those of them
trained to do psychotherapy do the initial interviewing and the
The subject of clinical sexology and its methodological approaches
9
majority of the therapy. Clinical psychologists administer
objective and projective tests. Medical specialists do physical
exams, obtain necessary lab tests, and participate in the
formulation and planning stages of therapy.
3. Interdisciplinary or integrated approach – tries to
integrate all (physiologic, psychological and social) aspects of
sexual functioning. Sexology stands apart as separate clinical
discipline and develops own system of scientific categories and
understanding of sexual disorders.
Paradigms in sexology
According to three methodological approaches in sexology
there are three paradigms that try to explain sexual functioning
and pathogenesis of sexual dysfunctions.
Mechanical paradigm associates all sexual dysfunctions
with local changes in genitalia.
Encyclopedic paradigm follows to the multidisciplinary
methodological approach.
Systemic paradigm tries to integrate all aspects of
sexuality.
The representatives of the first paradigm consider that
sexual dysfunctions are consequence of urological lesion (for
example: urethritis, prostatitis or colliculitis) and therapeutic
approach was reduced to the treatment of these focuses,
supposing mechanical recovery of the sexual function. The
influence of this paradigm is obvious in practice of such medical
specialties
as
urology,
venereology
and
gynecology.
Prescription of antibacterial drugs in an irrational amounts after
diagnosis of inflammatory process does not bring to the
recovery of sexual function and the patient leaves the medical
institution with the same complaints he had before.
Development of experimental endocrinology and chemistry
of hormones makes all-powerfulness capacity of hormones to
dominate in medical thinking. The experts with endocrine bias
were considered as advanced ones in the field. As a result all
variety of sexual difficulties and dysfunctions started to be
interpreted by qualitative and quantitative changes of sexual
and other hormones.
The subject of clinical sexology and its methodological approaches
10
In our practice there are a great number of such visitors
that for a long time were cured unreasonably by androgens for
recovery of their sexual potency, though the true cause of
disorder was the congestive process in the small pelvis, caused
by “neurosis of failure expectation”. In these cases hormonal
treatment is not only inefficient, but also full of danger of total
disappearance of erections.
The second – encyclopedic paradigm is characterized by
the prevalence of multidisciplinary methodological approach of
sexology. Sexual disorders are analyzed by several points of
view. Many groups of factors are taken into account at once
(urological, neurological, endocrine, and psychic) together with
socio-psychological, cultural and other factors.
The
greatest
achievement
of
multidisciplinary
methodology is parametrical surveys which were carried out
both in Russia and in the USA. In the USA these surveys were
carried out by Kinsey (1948-1953). He collected numerous
data and found out average rates on the basis of specially
developed questionnaires. Further the data obtained by the
scientist became a basis for development of clinical sexology
not only as a branch of medicine, but also as a separate
science which also includes other aspects of public life.
The third – systemic paradigm and interdisciplinary model
of clinical sexology in Russia developed by G.S. Vasilchenko,
on the basis of theory of functional systems of Anokhin (1975)
and a concept of phases and components of a copulative cycle
developed by himself. It allows defining specific discrete forms
of sexual disorders and developing treatment corresponding to
these forms.
There is also another model that gives systemic
framework of sexual functioning developed by D. M. Schnarch.
It is called quantum model. It offers an alternative to the
widespread tendency to conceptualize sexual dysfunctions as
separate “diseases”. The quantum model also avoids the
tendency to dichotomize the causes of sexual dysfunctions into
“organic” and “psychogenic” categories, as commonly occurs in
urology, gynecology, and psychiatry texts.
Psychosexual development through the life cycle
11
Chapter 2
Psychosexual development through
the life cycle
Psychosexual development is the continuing process by
which each person becomes the sexual being he or she is. At
any point in life, it represents the cumulative effects of many
forces, and it is one facet of psychological and maturational
development that is constantly being directed and shaped by
three forces simultaneously. One force is biological, including
hormonal, physiological and anatomical influences, innate
maturational timetables. A second is cultural, including social
learning in the family and influences outside the family. A third
force is intrapsychic, including normal developmental conflicts;
unconscious fantasies, conflicts and attitudes; and the
influences of all earlier experiences and emotions that help
determine how one approaches and copes with each new
biological , cultural and intrapsychic event.
The normal development of systems of a higher
organizational level depends on the successful development of
early related systems. Therefore, disruption of an early criticalperiod phenomenon impairs the successful acquisition of
certain later systems.
According to Vasilchenko G. S. the development of
sexuality comprises of the following phases:
1. Prenatal phase-include the period of time from the
conception up to the delivery. At this time brain structures of
sexuality and gonads are differentiated.
2. Parapuberty (1 to 7 Years). The chief developmental
event of this period is learning core sexual identity-the sense of
being male or female. There are two stages of this process:
first children become aware of their sexual identity and
consider themselves either boys or girls. Then increased
curiosity to explore anatomical differences between two sexes
enforces admitted identity.
Psychosexual development through the life cycle
12
3. Prepuberty (7 to 13 Years). At this period the sex he or
she belongs to is fixed. Socialization in sex roles takes place
during this period corresponding to the core sexual identity.
Again two steps can be distinguished-one is the choosing the
ideal prototype of masculinity and femininity and the other is
practicing chosen stereotypes of appropriate behavior in plays.
4. Puberty (13 to 16 Years). The main psychosexual event
in this period is the formation of psychosexual orientation.
While the former two phases proceed in a relatively quiet
background, this period is marked by blooming of endocrine
system, especially the activity of gonads increases and the
level of sex hormones become higher. This triggers the bodily
changes and emerging of secondary sexual characteristics. In
general, the sexual orientation develops in tree smoothly
following stages, two of which accomplish at this period. It is
necessary to highlight that the end of each stages marks with
learned experience on the basis of previously stated position.
These two stages are (1) the platonic libido stage that begins
with platonic fantasies and thoughts, and ensuring after by
platonic communications, and (2) the erotic libido stageevolving from erotic dreams to erotic contacts, such as hugging
and kissing
5. Transitional period to mature sexuality (16 to 25
Years). The last stage of forming of sexual orientation takes
place. This is the sexual libido stage. Sexual fantasies enhance
with sexual intercourse scenes, person has his or her first
sexual intercourse, and the sexual life with its excesses and
abstinences is being established.
6. Mature sexuality (25 to 55 Years). During this period
all the tree psychosexual development phases are over. Sexual
identity, sexual socialization and sexual orientation are
somehow formed and person who has a stabile sexual life
enters in certain physiologic rhythm called conditional
physiologic rhythm (CPR).
7. Involution (55 to 70 Years). At this period the sexual
activity decreases, interest in sex lowers. The reverse dynamic
of libido evolution is observed up to the platonic libido phase.
Psychosexual development through the life cycle
13
Prenatal influences
The presence of normal sex chromosomes (XX or XY)
determines whether the undifferentiated gonadal analogs
develop, respectively, into tests or ovaries. In the XY embryo,
testes begin to develop and to produce androgens at a fetal
age of about six weeks. In the XX embryo, ovaries begin to
develop somewhat later.
Sexual development begins at about six weeks and
depends upon the presence or absence of fetal testicular
androgens. The external genitalia of both sexes form from the
same embryological tissue. In the presence of fetal androgens,
the genital tubercle enlarges and becomes a penis. The
urogenital folds fuse, enclosing the urethra along the underside
of the penis. The labioscrotal swellings fuse at the midline to
form the scrotum. At the same time, the Wolffian ducts will
begin to form the vas deferens, seminal vesicles and
ejaculatory ducts. A separate fetal testicular substance called
antimullerian factor, reduces the Mullerian ducts to vestigial
remnants.
External male genital morphology is complete and
irreversible by the end of the 14th week.
In the absence of androgen, the genital tubercle becomes
a clitoris. The urogenital groove remains open as the vaginal
introitus. The urogenital folds remain in place as the labia
minora; labioscrotal swellings remain unfused and enlarged to
form the labia majora. The Mullerian ducts form the fallopian
tubes the uterus and the major part of the vagina. The cause
of the Wolffian duct to become vestigial is not known. Female
genital morphology, like male morphology, is complete and
irreversible by the 14th week.
Psychosexual development through the life cycle
14
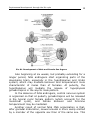
Pic. 01 Development of Male and Female Sex Organs
Also beginning at six weeks, but probably extending for a
longer period, fetal androgens start organizing parts of the
developing brain, especially in the hypothalamus and limbic
system, which may mediate behavior and temperament more
characteristic of males than of females. At puberty, the
hypothalamus will mediate the release of hypophyseal
gonadotropins in the acyclic male pattern.
In the absence of fetal androgens, central nervous system
is organized so that at puberty gonadotropins will be released
in the typical cyclic female pattern (which accounts for the
menstrual cycle), and female behavior and feminine
temperament may be mediated.
Another result of normal fetal CNS organization is that,
after gonadal maturation, sexual arousal is more easily elicited
by a member of the opposite sex than of the same sex. This
Psychosexual development through the life cycle
15
constitutes an innate heterosexual bias. However, this bias can
be overridden by a variety of postnatal emotional and learning
experiences.
It seems that nature is predisposed to differentiate a
female, unless effective fetal androgens cause male
dimorphism. If there are no fetal gonads of either sex, as in
Turner’s
syndrome
(chromosomes
45,
XO),
female
morphological and feminine temperamental differentiation
occur. They also occur if fetal testes are present and
functioning but the androgen is not effectively used by the
tissues, as in animal experiments with antiandrogens and in
the human androgen insensitivity syndrome. If there are
excessive levels of virilizing androgens in a chromosomal and
gonadal female, as in congenital hyperadrenocorticism, male
morphological and masculine temperamental differentiation
occur.
Parapuberty (1 to 7 Years)
This period of time can be divided into tree pieces:
infancy, toddlerhood and preschool period.
Infancy (Birth to 15 Months)
Learning core sexual identity- the sense of being male or
female-is the chief event of this period. It determined mostly
by brain structures differentiated in prenatal period. Some
microsocial factors also play a role. Parents not only handle
male and female newborns differently, they tolerate and elicit
different behaviors from them. From the time an infant is
named, a constant stream of cues teaches it that it is male or
female.
Other sexual experiences of infancy are derived from
having a male or female body. The mostly invisible and internal
female sex organs create more vague and diffuse sensations.
In contrast, the more external, visible male organs provide
more localizable sensations. These differences of body
conceptions lay early bases for the different sexual self-
Psychosexual development through the life cycle
16
concepts, body images, sexual attitudes and vulnerabilities felt
by female and male.
Another sexual aspect of infancy is learning to accept
one’s own and others’ bodies as good, pleasureful, and
trustworthy or as bad, unpleasant, and dangerous. This
learning results largely from the manner of mothering-the
quality and quantity of touching, holding, and fondling and of
physical warmth or its lack. A sense of one’s body as good or
bad also arises from parental responses to genital behavior.
The capacity to form bonds with others is strongly influenced in
early infancy as well, because of the interactions that produce
trust of physical closeness.
Infancy is probably the optimal period for achieving trust
and enjoyment of physical closeness, as well as the capacity to
form healthy and loving bonds, and for acquiring one’s coresexual identity. This latter development may continue into
early toddlerhood, but core-sexual identity is usually
irreversible by age 1, 5 to 2 years.
Toddlerhood (15 Months to 3 Years)
The chief developmental events of this period are the
recognition of body autonomy and learning to balance control
of oneself with acceptance of social controls. During this time,
most children become aware of anatomical sex differences.
Normally this awareness is not traumatic, but it really
stimulates enormous curiosity. Circumstances expose many
toddlers to the events of pregnancy and birth, to which they
also respond with great curiosity.
Along with increased drive to explore one’s body and
physical environment, there is increased genital exploration,
purposeful masturbation, and sex play with others. Toilet
training has sexual implications because of proximity of sexual
sensations to eliminatory functions. There is always the danger
of learning an inappropriate association between “dirty” bowel
functions and sexual sensations; this is a greater emotional
hazard for girls than for boys. And as the toddler struggles with
the inner conflict between wanting control of his own bowel
action and the requirement to relinquish at least part of it, he
Psychosexual development through the life cycle
17
may generalize this conflict to feeling that he also does not
have an autonomous right to sexual sensations.
Socialization in sex roles increases at this time. Social
interaction exposes him to role models, chiefly within the
family. Which sex he or she belongs to is already fixed; what it
means to be that sex is the new horizon. Toddlers begin to
identify with and imitate the same-sex parent; some temporary
periods of cross-sex identification are normal, but persistent
cross-sex identification is not.
A toddler is encouraged and rewarded for behavior that
his parents consider sex-appropriate and ridiculed or punished
for deviations. Destructively rigid sex-role stereotyping, when
present, begins its damaging constriction by toddlerhood, but
the child probably has no awareness of it. Toddlers are affected
by evidence within the family of how one or the other sex is
valued, as reflected in parents’ attitudes toward one another,
and by any differential treatment of siblings and other relatives
according to sex. A toddler can begin to develop a deep-seated
repudiation of his own or the opposite sex if he senses
consistent overt or covert disparagement of males or females.
Toddlerhood is the optimal period of language readiness;
during these years, children must learn effective verbal
communication or carry a major handicap through life.
Toddlers’ sexual curiosity is not only physical and visual but
verbal and cognitive. Accurate words are necessary to normal
ego development. Without clear verbal concepts, one cannot
bring order to one’s world or categorize one’s experiences
realistically.
Preschool Period (3 to 7 Years)
Some subtle but important maturational changes in sexual
physiology mark this period. The sensory nerves to the penis
and clitoris become fully myelinated by about 3 to 3, 5 years of
age, allowing for more discrete and intense erotic sensation.
There is also probably a slight increase in androgen production
in both sexes. Because androgen is largely responsible for
erotic desire in both sexes and for sensitizing the clitoris and
penis to respond sexually to tactile stimulation, this rise
Psychosexual development through the life cycle
18
enhances the child’s sexual drive. These factors cause
increasing genital eroticism, with an even greater increase in
masturbatory activity than in toddlerhood. The most important
change is that masturbation is now goal-directed with
heterosexual fantasies. It is inevitable for the child to wish to
gratify his desires with the opposite-sex person he loves mostusually the parent. This is a manifestation of the Oedipus
complex, and it occurs largely outside awareness or in dreams
and disguised masturbatory fantasies. But there is no
substantial doubt that it occurs, and most parents can recall
such seemingly naïve comments as, “when Daddy dies and I
grow up, I’m going to marry Mommy”.
These wishes produce fear and conflict. If the child wants
to displace or destroy the parent, he fears that the bigger,
stronger parental rival will be angry and destroy him. In a
child’s logic, the punishment would fit the crime; the result is
fearful fantasies that his or her sexuality will be destroyed. At
the same time, the child loves the rival parent deeply and feels
guilty over Oedipal impulses.
A child’s sexual anatomy affects the kinds of fears and
dangers he imagines. A boy’s penis is external and vulnerable;
this invites fear of it being cut off, and he may regard female
anatomy as proof of that possibility. A girl may believe that in
the past her mother deprived her of a penis as punishment for
her sexuality.
The child’s fantasies cannot be sustained in the face of the
fact that the “rival” parent remains loving and accepting and
does not reinforce the fears. And the parents’ continued
preference for one another in intimacy, a new arrival, a harsh
punishment at the hands of beloved parent, and the physical
impossibility of replacing the parent cannot forever be denied.
So reality with its painful disappointments as well as fear
divests the fantasy of much of its unconscious power and
forces renunciation of the wish. The Oedipus-complex becomes
extinguished by its lack of success, the result of its inherent
impossibility.
The Oedipal phase ends with the child
beginning to accept and strive for a definitive identification with
the parent of the same sex.
Psychosexual development through the life cycle
19
Healthy parental response is crucial to successful
resolution of Oedipal conflict, and parents can unwittingly fall
short. It may be difficult for a father to be both patient and
firm with a persistently intrusive and provocative son,
especially when he does not know what the behavior means
unconsciously. If he is unreasonably angry or punitive in
return, the boy may attribute it to rivalrous retaliation, and this
reinforces his fearful fantasies. If there is dissension between
the parents, either one may turn to the child out of spite or
value the child’s love more than the spouse’s, making the
fantasized rivalry real. Oedipal feelings exist in parents, too;
many a parent is shocked and horrified to discover erotic
stirrings in response to childish imitations of coquetry or
wooing. Frequently such a parent, more often the father,
withdraws out of guilt and ends all physical affection and
warmth, nonverbally teaching the child that heterosexual
feelings are bad.
What is needed is an openly welcoming attitude toward
the child’s budding heterosexual interests. In such families,
there is no reason to be jealous of the child or to fear one’s
own responses. The child also should be shown gently but
firmly that the parents’ physical intimacies are reserved for one
another and that, while the child’s sexuality is accepted, it
must be deferred and eventually directed toward a different
partner.
The successful resolution of complex Oedipal processes is
essential for psychosexual development. This is the stage when
the child first feels, and experiments in fantasy with,
heterosexual urges; it is probably the optimal period for the
acceptance and fixing of heterosexual preference. Although the
child must defer and redirect his urges, he must achieve and
retain a firm sense of their basic goodness and acceptability,
his right to them, and his right to their ultimate gratification.
Prepuberty (7 to 11 Years)
This period has often been referred to as sexual latency,
because of Freud’s belief that there is then an organic
Psychosexual development through the life cycle
20
diminution of sexual energy. Studies and investigation have not
support this view. There is a steady increase in the incidence of
sexual activity among children during these years.
One ego-development task that occurs in this period is
consolidating sex-appropriate sex-role preference. This started
in infancy with the beginning of core sexual identity, continued
during toddlerhood as the child experimented with the samesex and cross-sex identifications, and finally settled on
identification with the same-sex parent at the resolution of
Oedipal conflicts. Now the child, by attending school, is thrust
into the larger society. It is probably in these early school
years that socialization is most intense and most strongly
determines role preference. Sex-roles in the family may have
been unusual; now the child learns more of how the sexes are
treated and what is expected of them in the world outside
home. Pathogenic family attitudes can be ameliorated,
although early learning can be very refractory; family
expectations can be so powerful that a child has difficulty
learning or accepting different or broader sex-role definitions.
On the other hand, a warm and loving family can often insulate
a child from the effects of a larger social milieu that adheres
rigidly to overly restrictive sex-role stereotypes and is less
tolerant of normal but divergent interests and attitudes.
The basic acceptance of satisfaction with one’s sex rolethe social expression and consequences of being male or
female- are most influenced during this period.
Sex play, if not suppressed, begins in early toddlerhood,
and it continues in the school years. But solitary or mutual
masturbation, visual or tactile curiosity about others’ bodies,
and imitations of adult sexual activities are almost universally
disapproved of or punished in this society.
Puberty (11 to 16 Years)
Puberty is the biological surge of maturation that results
in reproductive capacity and adult appearance. Its midpoint is
somewhat arbitrarily defined as menarche in girls and the
capacity for seminal emission in boys.
Psychosexual development through the life cycle
21
Puberty occurs about two years earlier in girls than boys,
and all the body changes may take from one and one-half to
four years. Usually at about 9 to 11 years of age, the ovaries
produce the sex hormone, estrogen, in increasing amounts;
this increase initiates breast and uterine development and the
fat distribution that results in typical female body contours.
Females also produce male hormones (androgens) which are
responsible for the development of pubic and axillary hair and
increased growth of the clitoris and labia majora. Androgen is
also responsible for erotic desire and the intensity o genital
sensation in both sexes. At about the middle of puberty
(average, 12 to 12.5 years), the hypothalamus has begun its
cyclic regulation of sex hormones, and menarche occurs.
Testicles begin to enlarge at about age 12 and start
producing increasing amounts of testosterone about a year
later. This initiates growth of the penis, pubic hair, and
prostate; deepens the voice; and causes characteristic male
musculature and bone growth. The ability to ejaculate semen
with viable sperm, the equivalent of first menstruation in
females, usually is achieved shortly before age 14.
Adolescence is marked by increasing emotional lability,
irritability, and unpredictable shifts from striking maturity to
regressive behavior. This turbulence is probably caused by the
rising production of sex hormones, which influences behavior
before any major physical signs appear; therefore, the
youngster has nothing concrete to which to attribute these
puzzling feelings. Even when external changes have begun, the
youngster still feels more like a child than an adult, has not yet
moved into the adolescent social world, and often conveys a
sense of being at odds with him and the word.
Masturbation increases, primarily among boys, and
homoerotic play becomes the most frequent form of sexual
exploration with others. For the vast majority of youngsters,
such homoerotic activity is a developmental way station to
heterosexuality. The rising tides of sex hormones press for
gratification at a time when most youngsters’ egos are not yet
ready to cope with the emotional risk of heterosexual
interaction; they often find it easier to explore their changing
Psychosexual development through the life cycle
22
bodies and stronger sex drives with their more familiar samesex peers.
Normal puberty can occur as much as two and one-half
years earlier or later than the average. However, markedly
early or late puberty can cause serious emotional distress,
even lasting problems of sexual self-confidence.
There is a recrudescence of oedipal feelings; often they
are stronger and more consciously disturbing than in childhood.
It is not uncommon for early adolescents to have conscious
fantasies and undisguised dreams of sexual activity with a
parent.
Both the intensity and potential reality of these feelings
help precipitate one of the major tasks of adolescence. This
task entails a shift from the parent as primary love object to a
nonfamilial heterosexual peer. The early adolescent’s first
expression of this is often crude distancing from the parents,
especially the opposite-sex parent, by turning away and by
derogation; this is a way of denying attraction and associated
conflict.
By the end of early adolescence, youngsters should have
accomplished the resolution of their dependency and
reawakened Oedipal conflicts with parents enough to move into
the mainstream of adolescent socialization and to begin
heterosexual pairing. And they should have gained enough
familiarity with, and security about, their own and other’s
bodies to begin turning their attention more to the
partnerships.
Masturbation remains the most common sexual outlet
throughout adolescence, even for many of those with coital
experiences. This is more true for boys.
A few adolescents begin coitus by 12 or 13. Our society is
more accepting of sexual activity in males than in females.
Thus, the age at which male adolescents begin various sexual
activities is lower then that of female adolescents.
Adolescent sexual experience is natural and, regardless of
much that has been written about the dangers of coitus to
adolescent ego development, there is no evidence that
heterosexual coitus per se is damaging. The matter is that the
Psychosexual development through the life cycle
23
younger or less mature adolescents are, the less likely are they
to think of such consequences as pregnancy and sexually
transmitted disease.
Abstract thought is not normally fully possible until about
age 14; until this level of “formal operations” is reached, one
cannot understand involvement and commitment, anticipate
inexperienced consequences, or plan for the future. Those
whose sexual interactions remain self-centered reveal a delay
of both emotional and cognitive maturation.
Transitional period to mature sexuality
(17 to 25 Years)
Adolescence is thought of as a time of exploration, but,
because of the greater opportunities afforded most young
adults, many of them engage in even more sexual
experimentation. On the other hand, because the intrapsychic
progress from adolescence to adulthood entails the
crystallization of identity, values, and interests, other young
adults will have experimented sufficiently during adolescence
and found what they like sexually, and their current
experimentation therefore is diminished.
There is greater incidence of premarital coitus now among
women, so that there is now much less difference between the
sexes than in the past.
A characteristic of healthy adult sexuality is the capacity
to focus both tender and sexual love on the same person (not
necessarily only one person in an individual’s lifetime). Both
the successful resolution of adolescent development and the
early adult experience in sexual relationships are important for
the achievement of such fusion, a capacity that is necessary
before genuine, lasting commitment to a partner is possible.
Mature sexuality (25 to 55 Years)
Marriage and parenthood are only two of various ways
that individuals of the 25 to 40 age period deal with the sexual
issues. There is no implication that marriage is either the only
Psychosexual development through the life cycle
24
appropriate or the healthiest way to manage adult sexuality.
Married persons and parents are not by definition healthier
than unmarried childless people. Some of the continued
development possible within marriage is also possible in
unmarried partnerships, but marriage and parenthood are
qualitatively different from nonmarriage and childlessness.
Marriage legally commits couples to try to develop their
sexuality cooperatively rather than as individuals. Marriage also
provides an opportunity for resolving remnants of unconscious
sexual guilt related to parental disapproval. Girl friends and boy
friends are just that, but a husband or wife has a role earlier
held by a parent. A spouse’s enjoyment of sex play, coitus and
variety of sexual expression can promote guilt-free sexual
pleasure. The intimacy possible in marriage, the daily
experiencing of one another’s fluctuating moods and
physiological changes can dispel the anxiety-producing mystery
of the opposite sex.
Parenthood is a potent force in resolving remaining
unconscious sexual conflicts and in further development.
Pregnancy awakens new levels of a woman’s identification with
her own mother. For her husband, it evokes similar
identification with both father and mother, since in his primary
identification with mother he internalized some of her nurturing
qualities. Pregnancy begins to trigger a woman’s maternalism
and enormously expands her awareness and acceptance of her
previously vague internal sexuality; now there are contents
and sensations to define it in a new way.
Childbirth turns husbands and wives into parents and even
more powerfully precipitates identification with their own
parents. The woman gains functional equality with her mother,
the man sexual parity with his father. These identifications
carry the seeds both of growth and regression or disorder.
Becoming a parent may awaken unresolved Oedipal conflicts in
a destructive way; sexual activity may be inhibited if the
spouse is unconsciously identified with the sexually tabooed
parent.
Parents also identify with their child and continue to do so
as the child grows. In each developmental stage, the child
Psychosexual development through the life cycle
25
reawakens in the parent the emotions, the developmental
tasks, and any residual conflicts from that stage in their own
lives. Of course, the parent meets each recrudescence not as a
child coping with a stage for the first time but with an adult’s
ego development, able to repair maladaptations and achieve
greater health.
A child’s increased sexual activity during the Oedipal stage
forces many parents to re-evaluate attitudes toward their
children’s and their own rights to sexual expression, such as
the right to masturbation. A man whose father was physically
undemonstrative and avoided him, perhaps fearing homosexual
taint in such behavior with a son, may discover how natural
such father-son affection is and lose some of his own anxiety
about affection among men.
Adolescence is often especially trying for parents. Parents,
who have enough ego flexibility to hear their adolescent
children’s questions and challenges, and to consider them with
respect and intellectual honesty, will benefit as much as their
youngsters. They will find that their previously unquestioned
values have been opened to the possibility of alternatives, and
their own sexual identities may be richer for it.
Replacement by the young is inevitable for all people and
painful for many. It is not true that all parents of adolescents
have begun to lose their vigor and sexual attractiveness and
capacity; many are in their sexual prime. But it is true that
they have fewer remaining years of peak sexuality and
reproductive potential than their adolescent children. True
replacement does not take place during these years, but the
issue starts to become conscious. This can cause severe
distress in psychosexually immature parents and in those
whose adult sexuality has been less than fulfilling. However,
the growing sexual independence of one’s children can permit
greater sexual freedom and enjoyment. Many parents gain
more free time and privacy than they have had since their first
child was born. If they have made good use of their
relationship, they know so much more about sex and about
each other’s sexuality that feverishly active adolescents seem
like fumbling novices. The reassessments of attitudes and the
Psychosexual development through the life cycle
26
changes in life-style that accompany one’s children’s
adolescence can bring major achievements in psychosexual
development.
Involution (55 to 70 Years)
This period entail biological changes that make it
improbable for most persons to maintain the level of sexual
functioning and to have the same emotional responses as in
young adulthood.
Our culture has been, and largely continues to be, as
antisexual toward older people as toward the young.
Traditionally active sexuality is considered to be acceptable
only in married people of reproductive age. The result is that
relatively little normal psychosexual development has been
acknowledged or studied in the older population.
Diminished fertility and menopause force a woman to
think about her sexuality differently. This can be a very difficult
time, often of severe depression or even psychosis, especially
for women who had emotional conflicts about childbearing or
child rearing, whose childbearing potential or desire was
unfulfilled, or whose self-esteem was exaggeratedly linked to
maternal capacity. Hormonal changes can lead to unpleasant
physical symptoms, and then to gradual vaginal changes that
may impair sexual responsiveness and pleasure.
There are no male biological changes comparable to
menopause. Neither a man’s sexual function nor his fertility is
lost or even declines sharply because of age alone. Paternity
has been documented into the 80’s and 90’s, and while almost
all authorities report a gradual decline of circulating
testosterone in later life, there is not an inevitable correlation
with a diminished capacity for paternity. However, some men
become depressed or panicky in middle life over their imagined
loss of sexual vigor and hurl themselves into ill considered
sexual adventures or new marriages as a means of
reassurance.
The biological changes of middle life in women are a major
impulse toward further psychosexual development. For women
Psychosexual development through the life cycle
27
whose values have precluded the use of contraception,
menopause offers the first opportunity for sex without fear of
pregnancy and may bring a great increase in enjoyment. Since
these changes typically coincide with the end of preoccupation
with active parenting, they allow new leisure for parents to
enjoy one another and, for the woman, the possibility of a new
or resumed career. The enhanced self-esteem that
accompanies a continued sense of personal and social
contribution is an antidote to depression and therefore to
sexual decline.
In the absence of specific disease, male erectile capacity is
never lost as a consequence of age alone. Sexual arousal and
achievement of orgasm may. However, take longer, there are
longer refractory periods after orgasm, and ejaculation is less
forceful and may not occur on every coital occasion. Unless a
man misinterprets theses changes as decreased virility, they
can carry more advantages then disadvantages.
One of the most dramatic examples of psychosexual
development that sometimes occurs in middle life is that which
follows the dissolution of a marriage that has been sexually
unsatisfactory. Many couples maintain a sexually and
interpersonally unhappy marriage out of the conviction that
their children will benefit from an broken home. Often these
are mismatched people who have tried unsuccessfully to make
their relationship gratifying and are capable of previously
unattained levels of sexuality with other partners. When their
children are no longer dependent, they may wisely separate or
divorce and make developmental gains with new partners that
transform their many remaining years.
Sexual constitution
In the sexual practice ''sexual constitution'' is aggregate
of steady biological properties, which are under the influence of
hereditary factors, condition of development at prenatal period
and early ontogenesis. It limits diapason of individual sexual
needs and defines individual resistibility to pathogenic factors
particularly considered with sexual sphere.
Psychosexual development through the life cycle
28
Table 1
Definition of female sexual constitution
Constitution
Vectors
1. The age of sexual
libido arising
2. The age of first
ejaculation
3. Trochanter index
(height/legs length ratio)
weak
17 and
later
19 and
later
< 1.85
middle
strong
16
15
14
13
12
11
10
17-18
16
15
14
13
12
11
1.86-1.89
1.90-1.91
1.92-1.94
1.95-1.96
1.99
2.0
1.971.98
9 and
earlier
10 and
earlier
> 2.0
Inclination
4. Pubic hairy
spar
Feminine
for
se hair
type
feminine
Masculine type with
Masculine type
hypertrichosis
type
5. Maximal excesses
6.Conditional physiologic
rhythm (CPR)
7. The absolute age of
CPR standing
0
2
3
4
5
6
7
8
-
honeymoon
1
2-3
4-5
6-10
11-19
20-29
-
before22
23-26
27-31
32-36
3740
41-45
46-50
9 and
more
30 and
more
51 and
more
Psychosexual development through the Definition
life cycle
of male sexual constitution
29
Table 2
Vector
Constitution
Weak
The age of
menarche
17
and later
16
15
14
Regularity
Amenorrhea
or rare
menstrual
cycle
Prolonged
menstrual
cycle
disturbance,
without some
kind of
external
factors'
influences
Menstrual cycle
disturbance only
due to external
psycho-emotional
or somatic factors
Rare and
episodic
disturb
ance of
menstrual
cycle
The age of
first
pregnancy
in regular
sexual life
_
10 years and
more
3-9 years
1-2 years
I Menstrual
function
II
Reproductive
function
Middle
Strong
13
12
11
10
Regularly
3-6
month
1-3
month
Even with using
of
contraceptives
9 and earlier
Menstrual
function
disturbance
_
Psychosexual development through the life cycle
30
-
Grave
pathology of
pregnancy
with abortion
Threat abortion,
grave toxicosis
Toxicoses
with mild
course
III Trochanter index
1.88
1.89-1.93
1.94-1.96
1.97-1.98
IV Axillary and pubic hairy
A0P0
A1P1
A2P2
V. The age of arising
erotic libido
≥17
15-16
14
Course of
pregnancy
First orgasm
Normal course
1.99
Female type A3P3
2.0
Bent
for
male
type
2.012.02
2.032.04
Bent for male
type
Male type
with
hypertrichosis
13
12
11
10
9
8
and earlier
Absolute age
-
≥35
31-34
26-30
21-25
18-20
15-17
12-14
11 and earlier
After regular
sexual
activity
-
10
years
3-9
years
1-2 years
6-11
month
2-5
month
1
month
After
CPR
Before sexual
life
Absolute age
-
40
35
30
25
20
19
18-16
15 and
earlier
After regular
sexual
activity
-
10-15
years
5-9
years
3-4 years
1-2
years
6-11
month
2-5
month
1
month
After first sex
intercourse
VI Orgasm
50-100%
Psychosexual development through the life cycle
31
Sexual manifestations
There are some sexual manifestations, each of them
occurs at the definite period of life. The same sexual
manifestation is commented differently at the different periods
of the age. For instance, masturbation and night pollution takes
place in the puberty, excesses and abstinence-in the
transitional period, conditional physiological rhythm-in the
mature sexuality, abstinences in the period of involution.
Masturbation: There are different types and forms of
masturbation, each of which has its specific meaning in
sexology.
1.
frustrational pseudomasturbation
2.
early prepubertal
3.
Masturbation of youth hypersexual period
4.
Compensator
5.
perseverator-obsessive
6.
imitative
The type of masturbation which takes place in the puberty
considers as a substitute to ease physiological discomfort
created by the consequence of the impossibility to have
intercourse.
Here we stop on the description of the other types of
masturbation, as clinically they are cases of great importance.
Vasilchenko distinguishes these types of masturbation.
Frustrational
pseudomasturbation
is
a
type
of
masturbation accompanied with neither ejaculation nor
orgasm.
Early prepubertal masturbation reveals before arising of
sexual libido. A characteristic measure is the dissociation
between the ejaculation and orgasm, orgasm without
ejaculation or the vice versa. Usually this disappears within the
sexual maturity.
Substitute masturbation reveals in the transitional period
to mature sexuality, when there isn’t opportunity to have a
sexual intercourse (abstinence period).
Psychosexual development through the life cycle
32
Pereseverator obsessive masturbation: characterized by
obsession. If the above mentioned types of masturbation
vanish after some years or give way to another type, then this
one goes on and even after the marriage. In the hardest cases
it happens without erection, sexual desire and orgasm. The
patient isn't able to rein the demand of masturbation and does
not understand why he/she does it when he/she doesn’t have
any need for it.
Imitative masturbation is not on own initiative and isn’t
realized alone, only in group of adolescence of the same age.
Frustrational and imitated masturbations are considered
to be pseudomusturbations that demand not medical but
breeding treatments. Adult hypersexual and compensator types
of masturbations are physiological. Obsessive masturbation is
pathological and demands medical treatments against to the
causes of it. Prepubertal masturbation can be just a type of
imitation but also it can be result of early beginning sexual
activity related to nervous system’s residual organic
pathogenesis.
Sexual excess - all intercourses with ejaculation in a day.
It is specifically masculine phenomenon. It's essentially
connected with the sexual constitution.
Conditional physiological rhythm- is a masculine
phenomenon, frequency of intercourses according to biological
needs, and depends on sexual constitution. CPR takes place at
the period of mature sexuality.
Sexual abstinence is absence of sexual intercourses. This
can be partial with masturbation or night pollution and total
without any sexual manifestation.
Night pollution is also a masculine phenomenon,
involuntary ejaculation during the sleep. Usually it is the first
sexual manifestation that takes place at the beginning of the
puberty and accompanied with erotic and sexual dreams.
Sexual response cycle
33
Chapter 3
Sexual response cycle
Throughout history the human sexual response was seen
monistically, as a single event that passed from lust to
excitement and was climaxed by the orgasm. All the sexual
dysfunctions were also perceived as though they were a single
clinical entity. No distinction was made between premature
ejaculation or impotence or lack of libido or sexual avoidance.
All males who could not perform or enjoy sexual intercourse
were termed impotent, while all women with sexual difficulties
were labeled frigid.
It followed that treatment was also undifferentiated.
Since all sexually dysfunctional patients carried the same
diagnosis, they also received the same therapy. At the same
time, the etiology of sexual pathology was not clearly
understood and so the nature of treatment was empirical. Not
surprisingly, treatment for sexual problems was not very
successful.
The old monistic view of the human sexual response thus
impeded advances in the field. Progress in understanding
human sexuality required the separation of the component
parts from the undifferentiated mass.
Gradually, it was recognized that the sexual response is
not an indivisible entity, vulnerable to a single pathogen,
subject to only one disorder, and amenable to a single
treatment regimen. On the contrary, the human sexual
response is composed of three separate but interlocking phases
which are each vulnerable to disruption in a specific manner by
multiple physical and psychic pathogens, and which produce a
variety of disorders that are responsible to specific and rational
treatment strategies.
Before the three phases could be accurately discriminated,
it was necessary to obtain a clear description of the physiology
of the sexual response of men and women. It was Masters and
Johnson who first had the courage and good sense to regard
Sexual response cycle
34
the human sexual response as a natural biologic function and
who observed male and female sexual behavior accurately
under the same kinds of laboratory conditions which serve the
study of other biological systems such as digestive and
respiratory physiology. Their work yielded the first clear and
accurate description of the human sexual response. Masters
and Johnson divided the sexual response into four well-known
stages: excitement, plateau, orgasm and resolution.
Masters and Johnson scheme describes only the genital
Pic. 02 Sexual excitement during the time
phases of the sexual response-excitement phase and orgasm
phase. Plateau phase refer to different degree of the
excitement phase and resolution merely refers to the absence
of sexual arousal. Therefore, the biphasic concept represented
a significant theoretical advance in the field which led to
important clinical development. The understanding of the
sexual response and its dysfunctions was completed and
clinical data were sufficiently accounted for after recognition of
a third, a central phase, the phase of sexual desire.
The three phases are physiologically related but discrete.
They are interconnected but governed by separate
neurophysiologic systems. Sexual desire is an appetite or drive
which is produced by the activation of a specific neural system
in the brain, while the excitement and orgasm phases involve
Sexual response cycle
35
the genital organs. In both males and females the excitement
phase is produced by the reflex vasodilatation of genital blood
vessels. By contrast, orgasm essentially consists of reflex
contractions of certain genital muscles. These two genital
reflexes are served by separate reflex centers in the lower
spinal cord.
Male-Female differences in the sexual response
cycle. Typically, a young man in the resting phase can be
aroused quickly, strives for rapid increase in pleasure and
wants intensely to move quickly through plateau to orgasm.
His sexual focus is sharp and strong and he approaches orgasm
with rapid heavy breathing and pelvic thrusting. Orgasm is
usually explosive and brief, often with local noises, an end of
thrusting, retraction of the pelvis and brief loss of awareness.
Then he rapidly loses sexual interest and returns to the resting
state.
In some women resolution occurs quickly. Some may
return to the plateau and then to additional orgasms. For other
women, perhaps a majority in our society, excitement builds
more slowly, the plateau is prolonged and orgasm is less
dramatic. For still other women, orgasm seems not to be a
climax but a passing over to a more relaxed state, with little
movement or noise, followed by slow resolution. What they
describe as orgasm is not subjectively or objectively much
different from a plateau experience, but afterward they feel
release of tension, a sense of completion and a desire to talk,
rest, cuddle or sleep, all of which suggests that orgasm has
occurred. For a number of women, perhaps 10 to 30 per cent,
orgasm never or rarely occurs. For many others, it is
intermittently absent.
Erection of nipples is an early sign of arousal in females
and occurs in about half of all males. Vasocongestion enlarges
the female breasts and areolae during the excitement and
plateau phases, especially in nulliparas and women who have
not nursed. The breasts and areolae quickly return to normal
size during resolution.
During sexual response, 70 to 75 per cent of women and
about 25 per cent of men show sex flush a brush or rash-like
Sexual response cycle
36
vasocongestion across the chest, breasts, back and neck. It
develops during the transition from excitement to plateau, is
most evident at orgasm and disappears quickly during
resolution.
The desire phase
The neurophysiologic and neuroanatomic bases for sexual
desire have not yet been delineated with the same degree of
accuracy as other drives, such as hunger, thirst and the need
to sleep. Current concepts regarding the biology of the sexual
appetite are based on relatively few experimental studies,
inferred from clinical evidence, and drawn by analogy from our
general knowledge of brain functioning and of the
neurophysiology of the other biological drives.
The sex drive is basically similar to the other drives in that
it: 1) depends on the activity of a specific anatomical structure
in the brain; 2) contains centers that enhance the drive in
balance with centers that inhibit it; 3) is also served by two
specific neurotransmitters-an inhibitory and an excitatory one;
and 4) has extensive connections with other parts of the brain
which allow the sex drive to be influenced by and integrated
into the individual’s total life experience.
Sexual desire or libido is experienced as specific
sensations which move the individual to seek out, or become
receptive to, sexual experiences. These sensations are
produced by the physical activation of a specific neural system
in the brain. When this system is active, a person is “horny”,
he may feel genital sensations, or he may feel vaguely sexy,
interested in sex, open to sex, or even just restless. These
sensations cease after sexual gratification, i.e., orgasm. When
this system is inactive or under the influence of inhibitory
forces, a person has no interest in erotic matters; he “lose his
appetite” for sex and becomes “asexual.”
Sexual response cycle
37
Anatomy
The sex center of the brain consists of a network of neural
centers and circuits. These are known to be located within the
limbic system, with important nuclei in the hypothalamus and
in the preoptic region. The limbic system is an archaic system
which governs and organizes the behavior that ensures not
only individual survival but also the reproduction of the species.
Towards those ends it contains the neural apparatus that
generates and regulates emotion and motivation. The limbic
system exists even in primitive vertebrates, and has remained
essentially unchanged even in man. However, it has been
integrated into our complex brains so that it often seems to
have disappeared. Yet it is very much alive and influential and
comprises the biological substrate of our complex sexual
experience.
The sexual system has extensive neural connections with
other parts of the brain. All of these pathways have not as yet
been located precisely, but much of the structure, function and
connections of the sexual system can be inferred from
behavior. Because of pleasurable quality of sexuality, it may be
inferred that the sexual circuits have intimate connections with
the pleasure centers of the brain, and release a chemical for
which receptor sites exist in the pleasure circuits. But sexual
desire must also be anatomically and chemically connected
with the pain centers, for if a sexual object or stimulation
produces pain- i.e., is experienced as dangerous or destructiveit will cease to evoke desire. In other words, pain has the
capability of inhibiting sexual desire, since our brain is
organized so that pain has priority over pleasure, which makes
sense from an evolutionary perspective.
Behavioral observations also suggest that the sex circuits
are extensively interconnected with those parts of the brain
that analyze complex experience and also with the memory
storage and retrieval systems. There is evidence that sexual
desire is highly sensitive to experimental factors which
determine and shape, in large measure, the objects and
activities which will and will not evoke our desires.
Sexual response cycle
38
It may be speculated that neural connections exist
between the central sex centers and the spinal reflex centers
that govern genital functioning. Input from the higher centers
can enhance or diminish the genital reflexes. Thus, when libido
is high, when a person feels sexy and sensuous, erection and
lubrication are full and rapid, and orgasm is easily achieved. In
fact, erection and even orgasm may at times be achieved
purely on the basis of external stimuli and fantasy without any
physical stimulation of the genitals. But the opposite is also
true. When desire is absent and the sexual experience is flat
and joyless, the threshold for the genital reflexes is much
higher. When one is not turned on it can take “forever” and the
physical stimulus must be intense before the genitals will
function.
Physiological mechanisms
Information regarding the physiologic mechanisms, the
electric and chemical events which govern the sexual system,
is just beginning to be accumulated, and the information is still
too fragmentary to build a coherent conceptual structure.
In the natural state, libido and the sex circuits are
governed by biological rhythms as well as by the availability of
an attractive partner. Animals whose reproductive behavior is
regulated by an estrus cycle are more subject to biological
rhythms than man is. For example, female animals whose
sexual receptivity is governed by the estrus cycle display a
total absence of sexual desire and avoid sex except during
periods of “heat,” are controlled by hormones. In infrahuman
females, both sexual attractiveness and sexual receptivity
depend on estrogen. The central action of estrogen on the
brain makes them receptive, while the peripheral action makes
them attractive. Specifically, estrogen causes the vaginal cells
of some species of animals to manufacture pheromones which
release sexual desire in the male. In human females, does not
enhance sexual desire and its role in female attractiveness
remains controversial. But humans, too, fluctuate to some
extent in their sexual desire on a biological basis. The biological
sex rhythms of humans are probably mediated by sex
Sexual response cycle
39
hormones via their influence on the sex centers of the
mammalian brain.
The role of testosterone in human sexuality seems clearer.
It is the “libido hormone” for both genders. In the absence of
testosterone, there is little sexual desire in both males and
females in all species studied so far, including humans.
Presumably this effect is due to the crucial role testosterone
plays in the functioning of the sex centers of both genders,
although the mechanism of this action is not clearly understood
as yet.
Recent evidence indicates that luteinizing hormonereleasing factor (LH-RF), may enhance sexual desire even in
the absence of testosterone or when testosterone is ineffective.
It has been speculated that the sex hormones,
testosterone and perhaps LH-SF, influence sexual behavior by
some interaction with the neurotransmitters which are the
mediators of neural impulses within the sexual circuits.
Evidence suggests that serotonin acts as an inhibitor, and
dopamine as a stimulant, to the sexual centers of the brain.
Neurophysiologic studies have shown that the two genders
have similar neurological bases for sex. For example, both
genders require testosterone for activation. However, there
seem to be major gender differences in the stimuli that evoke
desire. Desire in male animals is normally aroused by the
smell, sight and other sensory cues provided by a receptive
female, by a female in “heat,”, while desire in receptive
females is evoked by the presence of a sexually active,
courting male.
Slightly different spectrum of factors seems to be
associated with inhibition of the sexual desire of males and of
females. For example, while both men and women may be
“turned off” if they are angry at their partner, this is more
often true of women. The majority of women seem to lose their
desire for a partner towards whom they feel hostile. This is also
true of some men, but less frequently, and more males than
females can experience intense desire for a partner with whom
they are angry.
Sexual response cycle
40
Disorders of desire phase
Hypoactive sexual desire and inhibition of sexual desire
(ISD) are common syndromes of males and females. The
hypoactive individual is asexual; he behaves as though his
sexual circuits have been “shut down.” He loses interest in
sexual matters, will not pursue sexual gratification, and if a
sexual situation presents itself, is not moved to avail himself of
the opportunity. It may be speculated that hypoactivity of
sexual desire can result from the lack of activity of the sexual
centers or from their active inhibition.
Inhibition is often selective in that the genital functioning
of men and women with sexual anorexia may be maintained.
These individuals may be able to experience erection or
lubrication-swelling and orgasm, but in a mechanical manner,
without much pleasure.
The excitement phase
In both men and women the physiologic signs of sexual
excitement are produced by the reflex vasodilatation of the
genital blood vessels. During sexual arousal two centers in the
spinal cord, one at S2, S3, and S4 and one at T11, T12, L1, and L2,
become activated and cause the arterioles which invest the
genitals to dilate. This vasodilatation causes these organs to
become swollen and distended and changes their shape to
adapt them to their function. The reflex dilatation occurs in
both genders. However, because of anatomic differences in the
male and female genitals, this swelling takes different forms
and so produces changes which are different but
complementary. The penis becomes hard and enlarged to
penetrate the vagina and the vagina balloons and becomes wet
to accommodate the penis.
Male excitement - Erection
In the male, the cavernous spaces of the corpora
cavernosi of the penis fill with blood and distend the penis
against its tough, rigid outer sheath. This changes the flaccid,
Sexual response cycle
41
soft penis into a hard and erect organ capable of penetrating
the vagina. The penis is maintained hard and erect by a high
pressure hydraulic which uses blood as its fluid.
Erection is attained and maintained by a complex
physiologic system which produces an increased flow of blood
to the penis while at the same time decreasing the flow of
blood out of the penis. This increases the amount of blood and
traps it inside the penis at a relatively high pressure.
The increased amount of blood is shunted into the
cavernous sinuses which distend, thus enlarging the penis.
Pic. 03 Male Excitement
Pic. 04 Cross-section cut of penis
Sexual response cycle
42
The enlargement is contained by the tough fascia which
encases the penile cylinder. The pressure of the increased
blood against this sheath hardens the penis and makes it erect.
The increased penile flow during excitement is known to be
caused by a dilatation of the penile arteries. This is brought
about by parasympathetic impulses from the erection centers
which cause the muscles in the arterial walls to relax.
Pic. 06 cGMP dependent mechanism of erection beginnings
The mechanism responsible for decreasing penile outflow
is not yet entirely clear. Some hypotheses hold that it is caused
by reflex constriction of the penile veins. An alternate
hypothesis suggests that special penile valves control the
outflow, while still another postulates that the outflow and also
the shunting of blood to the cavernous sinuses are controlled
by “polsters” or small smooth muscle structures located only on
the penile blood vessels walls.
The erectile response is primarily a parasympathetic one,
although surgical and pharmacological evidence suggests that
some sympathetic components is also required for potency,
possibly by controlling outflow of erectile blood. However, it is
well-known clinically that an intense sympathetic response,
such as that produced by fear and anxiety, can instantly drain
Sexual response cycle
43
the penis of extra blood and so cause a psychogenic loss of
erection.
Female excitement
In the female, the excitement phase is also produced by
reflex vasodilatation of the genital organs. Within 10 to 30
seconds after excitement starts, the vaginal walls begin a
sweating-like process (transudation). The transudate is clear,
slightly slippery, nonoily and has a distinctive odor and taste.
This fluid seems to have at least three functions: It lubricates
penile movement in the vagina, it neutralizes the usually acidic
vaginal environment and its moisture aids sperm survival. In
some women, especially after menopause, there is too little
lubrication for comfortable coitus. This reduced wetting does
not necessarily reflect lack of erotic interest or poor sexual
technique, any more than copious fluids always indicate intense
interest and pleasure.
As excitement increases, the inner portion of the vaginal
barrel begins to balloon; a space greater than is necessary for
the penis is thereby created and perhaps provides a receptacle
where semen van collect. Increasing vasocongestion turns the
vagina from its normal pink color to red. The inner portion of
the evagina continues to balloon, a process called tenting.
Meanwhile, the outer third narrows and tightens; it is now
called the orgasmic platform.
Changes in the labia majora and minora during the
excitement are affected by parity. In nulliparous women,
myotonia makes the labia majora become flatter and thinner
during arousal, and they remain so throughout plateau and
orgasm. In women who have had children, the labia have
developed an axtensive vascular network, which becomes
congested dueing sexual response, the labia swell two to three
times in size. In all women, the labia minora normally double
or triple in size and become reddish purple.
It is believed that, like male erection, the physiologic
concomitants of female excitement, lubrication and swelling,
which are produced by local vasodilatory reflexes, are governed
Sexual response cycle
44
primarily by the parasympathetic nervous system, which
controls the vasodilatation of blood vessels.
Pic. 07 Female Excitement
Erection in the male is governed by two spinal reflex
centers, involving thoracic and lumbar segments, and one at
the sacral level. Clinical evidence from spinal cord accident
victims suggests that the upper center responds to psychic
stimuli, while the lower one is stimulated by tactile input from
the genitals. The lower reflex center can function without any
higher input or outflow. This accounts for the well-known
clinical fact that patients whose spinal cord has been
transected above the erection centers can have erections by
tactile stimulation of the genitals, on a reflex basis, even when
sensation is lost below the level of injury.
Under normal circumstances the excitement reflex centers
receive input from the brain and provide outflow to the brain.
These connections provide the biological basis by which
excitement can be enhanced or inhibited, the pleasurable
sensations augmented or blocked by experiential factors.
Sexual response cycle
45
Pic. 08 Female plateau
The neural apparatus that governs the female excitement
phase has not yet been delineated precisely. It may be
speculated, in view of the analogous embryologic development
of the reproductive and nervous systems of the two genders
that the spinal reflex centers as well as the higher neural
connections are analogous in males and females.
Disorders of excitement phase
Disorders of the male excitement phase are called erectile
dysfunctions. This consists of difficulties in attaining or
maintaining an erection. This may occur with or without
associated disturbances of libido or ejaculation.
Female excitement disorders are marked by difficulty with
lubrication and swelling during love-making.
The complex physiology of male erection and the need to
create a temporary high blood pressure system make this
phase of the male sexual response the most vulnerable to
biological factors, as well as to anxiety. It follows that erectile
dysfunction is a highly prevalent sexual disorder. By contrast,
dysfunction of the female excitement phase, i.e., the isolated
Sexual response cycle
46
inhibition of lubrication and swelling, is a relatively uncommon
clinical syndrome, except as the result of such local physiologic
factors as estrogen deficiency with senile vaginitis. Excitement
phase dysfunction of females can exist as a discrete syndrome,
but the painful and uncomfortable experience of coitus with a
dry and nondistended vagina can cause a secondary inhibition
of desire and/or avoidance of sex.
The orgasm phase
The orgasm phase of the sexual response is, like
excitement, a genital reflex that is governed by spinal neural
centers. Sensory impulses which trigger orgasm enter the
spinal cord in the pudendal nerve at the sacral level, and the
efferent outflow is from T11 to L2. The spinal reflex centers for
orgasm are in close anatomic proximity to those which govern
bladder and anal control. For this reason, in injuries to the
lower cord, orgasm, urinary and defecatory control may all be
impaired. Orgasm does not, as does excitement, involve a
vascular reflex but consists in both males and female of reflex
contractions of certain genital muscles.
The male orgasm is made up of two independent but
coordinated reflexes which make up its two subphases:
emission and ejaculation.
Emission consists of the reflex contraction of the smooth
muscles which are contained in the walls of the internal male
reproductive organs: the tubuli epididymides, the vas deferens,
the seminal vesicles and the prostate gland. This contraction
deposits a bolus of seminal fluid into the posterior urethra. The
internal vesical sphincter snaps shut, placing the seminal bolus
into an enclosed space. This emission response is not
pleasurable; it is reported to be perceived as a slight
physiologic signal which has been called the “sensation of
ejaculatory inevitability” by masters and Johnson.
In the healthy male, emission is followed a split second
later by rhythmic, .8 per second contractions of the striated
muscles which are located at the base of the penis, the ishio
and bulbo cavernosi muscles. The effect of these contractions
Sexual response cycle
47
is to propel the seminal fluid out of the penis in a series of
squirts. These contractions are accompanied by the typical
pleasurable orgastic sensations.
Pic. 09 Male Orgasm
Female orgasm is strictly analogous to the second phase
of male orgasm. There is, of course, no emission phase in the
female. During orgasm, tenting continues and the orgasmic
platform contracts, first strongly and rhythmically, then more
weakly and at longer intervals. Rhythmic contraction occurs at
the rate of 8 per second, just as during the ejaculatory part of
the male orgasm. Orgasmic contractions may continue far
longer than in men. The woman’s awareness of orgasm
usually, although not always, corresponds with these
contractions; longer more intense contractions are felt as a
longer, more intense orgasm. For many reasons- e. g.,
prolonged excitement without orgasm-vasocongestion may
remain after sexual activity; this chronic pelvic congestion can
cause severe pelvic discomfort and emotional frustration.
Sexual response cycle
48
Pic. 10 Female Orgasm
Emission in the male is governed by the sympathetic
nervous system. During emission, stimulation of the alpha
adrenergic receptors of the smooth muscles of the male
reproductive organs is causing them to contract.
The neural connections which control the second part of
the male, as well as the female, orgasm, which consists of
contractions of striated muscles, are probably controlled by a
different reflex center which has not yet been identified.
The reflex center for orgasm in males is located in the
sacral spinal cord, near the centers that govern defecation and
urination reflexes. It is believed that the female orgasm center
is similarly located. Spinal cord victims can have the physical
component of orgasm and so father children. This can occur as
a result of local stimulation of the genitals, as long as this
center is intact, even if they experience no sensation. But
under ordinary circumstances, the orgasm center receives
input from the brain, and also contributes its output to the
higher centers.
Sexual response cycle
49
Pic. 11 Female Resolution
These connections between the spinal orgasm centers and
the higher brain provide the physiologic apparatus for learned
inhibition of orgasm. Orgasm, unlike erection, which is not
subject to voluntary control, can be, and under normal
circumstances is, under the individual’s voluntary control. This
means that there are probably neural circuits that connect the
orgasm center to voluntary motor and conscious perception
areas of the brain. It may also be speculated that orgasm has
close connections with the pleasure center of the brain. It is
this connection which under normal circumstances makes the
experience of orgasm so pleasurable.
Disorders of the orgasm phase
Clinical syndromes produced by disorders of the orgasm
phase include: premature ejaculation, retarded ejaculation, and
its female analogue, orgastic dysfunction of females. Orgasm
inhibitions of both males and females fall along a spectrum of
severity from total anorgasmia to mild situational difficulties in
reaching a climax. An interesting subvariety of retarded
ejaculation is a syndrome of partial retardation. Such patients
have a normal emission response, but the second phase
Sexual response cycle
50
ejaculation is selectively inhibited. Clinically these men
experience “seepage” of semen but no orgastic squirting and
no ejaculatory pleasure. Return to the flaccid state is
commonly delayed in these patients.
Classification of sexual disorders
51
Chapter 4
Sexual disorders
Classification of sexual disorders
There are several sources to classify sexual disorders. The
major one is Diagnostic and Statistical Manual of Mental
Disorders-IV (DSM-IV; American Psychiatric Association,
1994). The other source that is used by many physicians and
mainly agrees with DSM-IV is the International Classification of
Diseases (ICD-10; World Health Organization, 1992).
DSM-IV describes the following sexual disorders:
Sexual dysfunctions:
1. Sexual desire disorders
2. Sexual arousal disorders
3. Orgasmic disorders
4. Sexual pain disorders
5. Sexual dysfunctions related to a general medical condition
6. Substance-induced sexual dysfunction
Paraphilias:
1. Exhibitionism
2. Fetishism
3. Frotteurism
4. Pedophilia
5. Sexual masochism
6. Sexual sadism
7. Transvestic Fetishism
8. Voyeurism
Gender Identity Disorders:
1. Transsexualism
2. Gender identity disorders of childhood
3. Other gender identity disorders of adolescence or adult life
Other Sexual Disorders:
Sexual disorders not elsewhere classified
Classification of sexual disorders
52
Sexual desire disorders are defined by decreased
interest in sexual interaction. Hypoactive Sexual Desire
Disorder (302.71) is manifested by persistently deficient or
absent sexual fantasy and desire for sexual activity. Sexual
Aversion Disorder (302.79) is a more extreme condition in
which there is persistent aversion to and avoidance of all
genital sexual contacts with another person.
Sexual arousal disorders involve dysfunction of the
lubrication-swelling stage of sexual response and are divided
along gender lines. Female Sexual Arousal Disorder (302.72) is
diagnosed when a woman manifests a persistent inability to
maintain an adequate lubrication-swelling response in the
presence of adequate stimulation. Male Erectile Disorder
(302.72), commonly called impotence, is the persistent
inability to maintain an adequate erection until completion of
the sexual activity. Both of these disorders involve the blood
flow response mediated by the parasympathetic nervous
system and are thus vulnerable to medications that affect the
autonomic nervous system.
Orgasmic disorders include Female Orgasmic Disorder
(302.73), formerly called anorgasmia or inhibited female
orgasm, is marked by a persistent delay in or absence of
orgasm following an adequate excitement phase. Thus a
woman suffering from this syndrome is able to become
aroused, to lubricate and feel excited, but is unable to reach
orgasm in spite of adequate stimulation. Male Orgasmic
Disorder (302.74) was formerly called retarded ejaculation, a
term which is preferable as it is descriptive of the problem. A
persistent delay in or absence of orgasm following an adequate
excitement phase is the signifier of this disorder. Premature
Ejaculation (302.75) is the inability to have a reasonable
amount of control over the ejaculatory reflex. A man suffering
from prematurity often reaches orgasm with minimal
stimulation, usually before he wants it or is ready.
Premature ejaculation has sometimes been diagnosed
based on the length of time a man could delay orgasm, and
sometimes by the degree of satisfaction the man’s partner
experiences through sexual interaction. Neither of these
Classification of sexual disorders
53
definitions is satisfactory, as they do not focus on the basis of
the problem-control. Most men learn how to control the onset
of orgasm by varying the amount of stimulation they are
obtaining. In essence, most men learn how to regulate their
excitement level, maintaining their arousal below the point of
ejaculatory inevitability (that moment when the orgasm reflex
begins).
Sexual pain disorders include Dyspareunia (302.76),
which refers to recurrent genital pain with sexual intercourse in
a man or a woman. This is one diagnostic category that always
requires a complete medical examination. Vaginismus (306.51)
is the persistent involuntary spasm of the circumvaginal
muscles when attempting penetration. It is most often noticed
when intercourse is attempted, but sometimes is apparent
during gynecological examinations.
Sometimes a woman who is not aroused, and
consequently is not lubricated, will complain of painful
intercourse. A careful and complete sexual history will help
differentiate cases of Female Arousal Disorder from
dyspareunia and Vaginismus.
Sexual dysfunction due to a general medical
condition is a particularly important category of sexual
problems. As the name implies, this diagnosis is made when
history, physical examination, or laboratory tests indicate that
the sexual dysfunction is fully explained by the direct
physiological effects of a general medical condition. All of the
symptoms found in the specific sexual disorders can be caused
by a general medical condition; thus you can not rule out the
possibility of a physical cause of sexual dysfunction based only
on the presenting sexual symptoms. Most sexual disorders
caused by a general medical illness are generalized, and
usually the sexual symptoms are concurrent with the onset or
exacerbation of the illness.
Substance-induced
sexual
dysfunction
is
unfortunately all too common. To make the diagnosis, history,
physical examination, or laboratory findings must indicate that
the sexual dysfunction is fully explained by the substance use
and either (1) the symptoms developed during, or within a
Classification of sexual disorders
54
month of, substance intoxication, or (2) medication use is
etiologically related to the disturbance.
Paraphilias, commonly referred to as sexual perversions,
include eight forms of recurrent, intense, sexually arousing
fantasies, urges, or actions involving either (1) nonhuman
objects, (2) the suffering or humiliation of self or another
person, or (3) sexual interaction with children or nonconsenting
persons.
To make a diagnosis of a paraphilia, the sexually arousing
fantasy or action must have been present for at least a period
of six months and, like all sexual disorders, must cause
personal or interpersonal difficulty. Many perverse sexual
actions involve behaviors that are intrusive, and illegal, and
thus patients with paraphilias are sometimes mandated to be
evaluated by the court. The brief description of paraphilias
according to DSM-IV:
Exhibitionism (302.4), exposure of one’s genitals to an
unsuspecting stranger
Fetishism (302.81), use of nonliving objects for sexual
gratification
Frotteurism (302.89), touching or rubbing against a
nonconsenting person
Pedophilia (302.2), sexual activity with a prepubescent
child or children
Sexual masochism (302.83), sexual arousal by being
humiliated, beaten, bound, or otherwise made to suffer
Sexual sadism (302.84), sexual arousal by causing
physical or psychological suffering
Transvestic Fetishism (302.3), heterosexual male
aroused by cross dressing
Voyeurism (302.4), sexual arousal at watching an
unsuspecting person who is naked, undressing, or
having sex
Gender Identity Disorders are characterized by the
individual’s feeling of discomfort and inappropriateness about
his or her anatomic sex and by persistent behaviors generally
Classification of sexual disorders
55
associated with the other sex. Gender identity is a personal
awareness of one’s sex (male, female, or ambivalent) or of
one’s feelings of masculinity and femininity, it is the inner
sense of masculinity or femininity. Core gender identity is a
sense of maleness or femaleness. Gender role behavior is the
outward expression of this personal awareness. Disturbances in
gender identity and rolebehavior are severe disturbances, to be
distinguished from feelings of inadequacy generated by
thoughts that one is not living up to the concept of gender role
behavior. Some feelings of inadequacy about masculinity and
femininity are ubiquitous in childhood and adolescence, and
remnants of these doubts are found in almost every adult.
Transsexualism is an overriding feeling “of discomfort with
one’s anatomic sex and a constant desire to be rid of one’s
genitals and become a member of the opposite sex. The
diagnosis is made only if the disturbance has been continuous
for at least two years; is not symptomatic of another mental
disorder, such as schizophrenia, and is not associated with
physical intersex or genetic abnormality.”
The differential
diagnosis must be made among true Transsexualism,
transvestism, crossdressing and homosexuality.
Sexual dysfunctions may be overt or covert, lifelong or
immediate, intrapsychic or interpersonal, and some of them
may be traced to significant medical or psychiatric factors. In
addition, the dysfunctions may be generalized or situational.
Overt Sexual Disorders. “Overt” may refer to (1)
patient’s knowledge, (2) presenting complaint, or (3) revelation
of the sexual disorder in the course of history-taking in which
the presenting complaint was nonsexual.
The most overt situation occurs when the patient is fully
aware of the sexual disorder, and presents it as his chief
complaint. The sexual disorder is less overt when the patient,
although fully aware of it, seeks help for another real or
imaginary condition. For example, a patient may complain of
depression but will reveal his impotence during the course of
the interview. Sometimes the disorder is fully known to the
patient, but he denies its importance. Denial as a defense
Classification of sexual disorders
56
mechanism may cause the patient to withhold information or to
make light of it.
When the symptom or syndrome is overt, the physician’s
task is somewhat easier because he does not have to overcome
the patient’s resistance in order to uncover the connection
between the presenting complaint and the underlying sexual
disorder, and point out the connections to the patient.
Covert Sexual Disorders. A “covert” sexual disorders is
one in which the disorder is not connected in the patient’s mind
with other symptoms he presents. Symptoms may include
fatigue, headache, backache, gastrointestinal disturbances,
menstrual irregularities or dysmenorrheal. Identifying and
labeling the unconscious connection between symptom and
sexual frustration becomes the task of the therapist.
Lifelong and Acquired Sexual Disorders. If the sexual
disorder follows a period of normal functioning, it is said to
have been acquired. The man who develops impotence after he
has been able to have satisfactory erections and coitus has
“acquired” impotence or, as it is sometimes called, “secondary”
impotence. If he has never had an erection sufficient for
penetration, he has lifelong or “primary” impotence. The
differentiation is important in the diagnostic evaluation of the
etiology of the disorder.
Generalized and Situational Sexual Disorders. If a
disorder, is situational (i.e., occurring only in certain situations
or only with certain partners), one can be certain that the
problem is psychogenic (unless limited to association with
alcohol or drugs). If the disorder occurs in all situations (i.e., is
“generalized”), it may be psychogenic, biogenic or a
combination of the two. The most typical situation is one in
which the sexual dysfunction is restricted to the marriage. In
this case the physician has to examine the nature of the
marital relationship.
Intrapsychic or Interpersonal Factors. Since anxiety
or other negative emotions responsible for sexual disorder or
dysfunction are intrapsychic, one might say that all sexual
dysfunctions have an intrapsychic component. Differentiation
between intrapsychic and interpersonal in this context means
Classification of sexual disorders
57
that the dominant etiology can be traced to either intrapsychic
or interpersonal factors. If negative associations to sex create
retarded ejaculation in relationships prior to a man’s marriage,
clearly the etiology is primarily intrapsychic. On the other
hand, if there is a period of good functioning which later
deteriorates because of marital conflict, the situation clearly is
primarily an interpersonal one, although, as has just been
stated, it has to have its intrapsychic components.
Medical and Psychiatric Causes. Some sexual
dysfunctions may be attributable to physical illness, for
example erectile dysfunction stemming from diabetes. Some
may be primarily due to a psychiatric disorder such as
inhibition of sexual desire as a consequence of depression.
Disorders of sexual desire
Definition and description
The DSM-IV describes the common desire problems as (1)
Hypoactive Sexual Desire Disorder (302.71), deficiency or
absence of sexual fantasies and desire for sexual activity that
causes marked distress or interpersonal difficulty, not caused
by a general medical condition; and (2) Sexual Aversion
Disorder (302.79), aversion to and active avoidance of genital
sexual contact with a sexual partner that causes marked
distress or interpersonal difficulty, not caused by a general
medical condition.
Diagnosis
Reliable and valid norms of human sexual behavior are not
yet available and in the final analysis the diagnosis of ISD is
made by comparing the patient’s experience with a sense of
what the normal range of sexual desire is. This is based on
deduction rather than on the kinds of direct scientific
observation and measurement which are available for the
genital responses. Thus, concepts of the normal parameters of
the sexual drive of men and women are inferred from various
statistical surveys of the frequency of intercourse and orgasm,
as well as from diverse clinical observations and from personal
experience.
Classification of sexual disorders
58
The typical clinical versions of this problem are the selfdiagnosed patient, the patient identified by a partner, and the
couple in which both partners wish they had stronger mutual
desire.
In each of these presenting complaints, there is
recognition that sexual desire is not what it might be, what it
should be, what it used to be, or what it is with different
partner. The identified patient is often considered (by self or
partner) inhibited specifically in contrast with the partner or
with his or her own past functioning. Thus, there is relativity to
this evaluation.
The diagnosis of HSD rests in part on a comparison of the
patient’s sexual history with the norm. In the healthy
individual, some form of sexual appetite is present throughout
life no matter what his cultural origins are. As with any human
trait, e.g., height, intelligence, etc., the intensity of the sex
drive varies widely, and in some cases, it may be difficult to
determine what is pathologic and what is a normal variation. In
other words, some normal persons apparently have such a low
sex drive that their experience overlaps that of persons
suffering from pathologic HSD.
Sexual appetite changes in intensity with age and takes a
gender-specific course of development. Infants seem to already
have some capacity for erotic feelings. These are evoked when
their genitals are stimulated. When a tiny clitoris or penis is
touched in the course of bathing and dressing, the infant
expresses pleasure by smiling and cooing. Children, if they are
not stopped, will masturbate and later play sexual games which
may entail looking at and touching each other’s genitals. We
tend to forget or repress much of these early sexual fantasies
and experiences but some memory is normally retained. And
when during a psychosexual evaluation the patient remembers
no prepubescent erotic feelings or sex play or fantasies, one
can assume a certain amount of early sexual inhibition or
repression.
There is a substantial increase in sexual desire at puberty.
This is probably correlated both with the maturation of the
cerebral circuits which govern sexual expression and with the
Classification of sexual disorders
59
increase in testosterone which is produced by the gonads at
this time and which activates these circuits.
After puberty sexual development takes a different course
in the two genders. In the male sexual desire seems to peak
around 17 years and then slowly declines. The normal
adolescent male is intensely interested in sex, is easily
aroused, and in the absence of a partner will masturbate, while
conjuring up erotic fantasies, with frequencies varying from
several times a day to several times a week. If there is no
sexual outlet he will experience frustration. This phenomenon
is so predictable that if the sexual history of a male reveals no
adolescent increase in sexual desire as reflected in
masturbation and/or fantasy and/or actual intercourse, one
may suspect a problem in psychosexual development.
The intensity of the male sex drive diminishes gradually
after adolescence. At middle age he still desires sex, but often
can go without sexual outlets for longer periods of time without
experiencing frustration. Throughout his life, however, his
sexual desire can be aroused under exciting circumstances.
Female also experience increase in libido at puberty.
However, this appears less intense than that of adolescent
males. Girls seem more easily discouraged from sexual
expression than boys. Thus, the absence of adolescent
masturbation in a female psychosexual history does not carry
the same clinical significance of severe sexual repression as it
does in the male. The female sex drive does not decline after
adolescence, but slowly increases and peaks somewhere
around the age 40. Then female sexual desire is more variable
than that of males. While women have a greater orgastic
potential, their sexuality is also more easily suppressed.
Throughout his life the normal person experiences
spontaneous sexual desire, and also has the capacity to be
aroused by an attractive partner. When the sex drive is high,
the person will experience spontaneous desire and will be
aroused by a wide range of stimuli. As desire diminishes, the
range of stimuli that will evoke the sexual appetite narrows,
and more intense psychic and physical stimulation is required
to produce a response.
Classification of sexual disorders
60
Factors apart from age also affect the sexual appetite.
Physical health and mood are important determinants in
reproductive behavior. Both genders experience an increase in
sexual appetite when in love and both genders experience a
decrease in sexual desire when they are under stress.
Clinical description
The person with low sexual desire will not feel “horny” or
interested in sex. He will not be moved to seek out sexual
activity, nor will he fantasize about sex. Also, in contrast to
normal experience, sexual desire evoked by stimulation of the
genitals will be absent or greatly reduced. The reflexes may, in
fact, work if stimulation is permitted; i.e., the person may have
an erection or lubricate and/or have an orgasm. But this
experience is not really satisfying in the presence of low desire
state pleasure is fleeting, perhaps just before orgasm, and is
limited to and localized in the genitals. Patients describe such
experiences as similar to eating a meal when one is not really
hungry. In situations which would normally arouse their sexual
desire, inhibited patients will report an absence of feeling or
even negative sensations of irritation, tension, anger, anxiety
and /or disgust.
Clinical Variants of ISD
Disorders of sexual desire can be described as primary or
secondary and can exist globally or situationally. Primary HSD
is a rare condition which is marked by a lifelong history of
asexuality. The patient is devoid of sexual interest to the
extent that he does not even masturbate. Primary HSD is
characteristic of constitutionally low sex drive and certain
disease states, as well as of severe psychopathologic states
such as schizophrenia and chronic depression. Persons whose
libido is severely repressed on the basis of neurotic conflict
may also present an asexual picture.
Secondary HSD, in which there is a loss of sex drive after
a history of normal sexual development, is much more
common than primary inhibition. Secondary loss of libido may
be produced by a variety of physical factors and is also seen
after psychological crises such as marriage, the birth of
children, a traumatic rejection or object loss, anger at or
Classification of sexual disorders
61
disillusionment with a partner, or nonsexually related stress
such as a job loss or an accident.
When there is a global loss of sex drive, the person ceases
to desire or be interested in sex at all. He experiences no erotic
wishes, fantasies or thoughts and, if male, may even cease to
have morning erections. Global or total loss of libido is typically
associated with depressive states, severe stress and physical
causes.
The most common clinical variant is situational HSD. This
is the typical picture found in psychogenic inhibited sexual
desire. Characteristically, the person feels desire only in
situations that are psychically “safe.” It is usually the most
appropriate and most desirable partner who represents the
“psychic danger” that results in the inhibition of desire. Thus a
man may feel desire for and be sexually active with prostitutes
or strangers or a woman who treats him sadistically or women
of a lower social class. But his sex drive becomes inhibited with
his intelligent and attractive girlfriend with whom he would like
to be intimately and tenderly connected.
Also typical of the situational ISD group is the woman who
feels very erotic during the many years of her precoital
experiences. She felt desire and erotic pleasure during
“petting,” but she loses sexual interest after she has engaged
in coitus, or after marriage, or after childbirth, i.e., in situations
which on a symbolic and unconscious level represent danger.
Differential diagnosis
The cardinal sign of ISD is a low frequency of sexual
activity. However, this alone only denotes hypoactivity, which
must, for clinical purposes, first be differentiated from sexual
avoidance. In this condition, the frequency of sexual activity
can also be low, but because of fear of sex and not because
desire is diminished. Once it has been established that libido is
indeed low, then an etiologic diagnosis must be made.
Physiologic and primary psychiatric etiologies must be
differentiated from psychogenic ISD and, finally, pathological
lack of desire must be differentiated from those normal states
where desire is appropriately inhibited or not generated.
Classification of sexual disorders
62
Differentiation from orgasm and excitement phase
disorders: One of the most important consequences of the
separation of desire phase dysfunctions from excitement and
orgasm dysfunctions is that it enables the clinician to sort out
this patient population from those suffering from disturbances
of the genital phases. Patients who complain of orgasm and
excitement phase dysfunctions but who retain normal desire
generally have an excellent prognosis when they are treated by
sex therapy, but patients who have little or no sexual desire do
not respond as well to these methods and require different
treatment strategies.
Sexual Avoidance: Low frequency or absence of sexual
contact may also be a sign of sexual avoidance on the part of
one or both of the partners. When sex arouses intense anxiety,
a pattern of phobic avoidance can develop, regardless of
whether desire is present or not. This is an important
diagnostic point, because if sexual avoidance complicates the
clinical picture of any of the dysfunctions, e.g., Vaginismus as
well as ISD, this avoidance presents a clear obstacle to therapy
and must be treated and resolved first.
Normal Asexuality: Asexuality is certainly not always
abnormal. It has already been mentioned that some persons’
sexual appetite falls on the low side of the normal distribution
on the basis of constitutional determinants. Such persons are
not bothered by the infrequency of their need for sex unless
external circumstances exert pressure. Such pressure includes
a partner with a relatively higher sexual drive as well as the
high sexual expectations currently in vogue in our society.
Finally, despite current propaganda to the contrary, it is
not appropriate to find all potential sexual partners or
situations attractive. Frequently the evaluation of a couple who
complain of loss of sexual desire reveals that there is no real
basis for attraction. The partners do not like each other-or
her/his hygiene is so poor as to be repulsive-or there is a
significant discrepancy in intellectual capacity, etc. the
irrationality of these situations lies in the fact that persons
think they should be attracted, should feel desire when it
makes no sense.
Classification of sexual disorders
63
The etiology of desire phase disorders
Sexual desire is governed by multiple biological and
experiential determinants; consequently, a wide variety of
physical and psychological factors can disturb its functioning.
An understanding of the physiology of sexual desire is
basic to the understanding of its disorders. Sexual desire is a
drive that serves the biologic function of species survival. It
instills a strong erotic hunger that prods us to engage in
species specific behavior that leads to reproduction. It moves
us to find a mate, to court, to seduce, to excite, to impregnate,
to be impregnated.
The neural organization that governs libido is similar to
that which produces hunger, thirst and the urge to sleep. Like
these other drives, it is served by its own specific network of
centers and circuits. The behavioral correlate of neural activity
in these centers is the experience of sexual desire. In the
absence of such activity there is no libido.
Like the other drives, sexual desire is organized so that it
is kept in balance by inhibitory and activating mechanisms.
When the inhibitory centers dominate, sexual desire is
diminished; an increase of sexual desire is experienced when
the circuits are under the influence of the activating centers.
The centers have extensive anatomical connections to other
parts of the brain, and by virtue of these connections, sexual
desire can be enhanced and inhibited by a number of internal
and external forces.
The sex centers and sexual appetite are responsive to
hormones, specifically testosterone and LH-RF. Without an
adequate hormonal environment they cannot operate and libido
vanishes. Also, external stimuli such as the aroma, sight,
sound and touch that indicate that an attractive partner is at
hand-influence the state of desire profoundly.
The connections of the sex centers to the parts of the
brain that process and store experience make sexual desire
highly sensitive to the past. The suppression of sexual desire
can be acquired. We learn to inhibit desire in situations that
carry negative contingencies, and learn to allow desire to
emerge in “safe” contexts. In fact, desire is the product of a
Classification of sexual disorders
64
biologically rooted substrate that is shaped indirection and
intensity by events of the past.
Also important from a clinical vantage is the fact that the
sex centers are profoundly influenced by emotion. The negative
emotions that serve individual survival and motivate us to
avoid and defend against danger-fear and anger-have priority
over the urge to reproduce. This hierarchy has clear survival
value. But this adaptive mechanism can go awry if the
“dangers” are not accurately perceived. If an individual reacts
to fantasy dangers, if he reacts with alarm to fears that have
no basis in reality, his sex drive will become inhibited just as
surely as if there was a real tiger in his bed. That is the
psychophysiologic basis of the inhibition of sexual desire.
Physiologic causes of HSD
Depression
Depression is perhaps the most common physiologic cause
of HSD. Depression is marked by a diathesis of vegetative
symptoms which includes sleep, eating and libido disturbances.
It may be speculated that during a depressed state the activity
of the centers and circuits that serve such vital function as
eating and sex is diminished. The loss of sexual appetite may
be an early symptom of depressive states and may appear
even before the patient’s mood becomes perceptibly sad.
Characteristically, during depression erection and orgasm are
not impaired at all or not to the same extent as is libido. Again,
sexual therapy is not an appropriate treatment modality when
loss of libido is secondary to depression. The underlying
depression should be treated first by appropriate means which
may include medication and/or psychotherapy. Often, but not
always, sexual desire returns spontaneously when the
depression lifts.
Stress
Severe stress, such as is experienced on the battlefield, or
during a traumatic divorce, or after a job loss or forced
retirement, is often associated with a loss of sexual interest.
Clinical observations suggest that crisis and stress are also
Classification of sexual disorders
65
associated with a physiologic depression of the sexual
apparatus.
Drugs
The sex centers depend for their proper functioning on a
delicate balance of the neurotransmitters serotonin and
dopamine, on a specific matrix of sex and pituitary hormones,
and probably on yet undiscovered chemical ingredients as well.
Anything that upsets these balances, which tinkers with the
recipe, may result in a malfunctioning of the centers and so
depress libido.
While the specific mechanisms of action are not clear in all
cases, clinical evidence suggests that some drugs may produce
a diminution of sexual desire; these include narcotics, high
doses of sedatives and alcohol, certain centrally acting
antihypertensive agents such as those, for example, which
contain reserpine and methyl dopa, and drugs which
antagonize the action of testosterone.
Hormones
Because the activity of the sex centers depends on
testosterone, insufficient levels of this hormone or its
physiologic unavailability may produce a diminution of sexual
interest in both males and females. This can result from any
condition or drug or psychic state which impairs the production
of androgens by the testes, ovaries and adrenals. Common
factors in testosterone deficiency include the aging process,
prolonged stress, surgical removal or disease of the
testosterone-producing glands, and hormones and medication,
such as provera and estrogen which antagonize the action of
testosterone. A low testosterone level should always be ruled
out when the evaluation points to a possible organic etiology
for HSD. Recent evidence suggests that increased levels of the
hormone prolactin may play some role in libido problems.
Medical Illness
Any medical illness or surgical procedure which disturbs
the anatomy or physiology of the brain’s sex centers such as,
for example, renal dialysis, can be associated with low libido
states. Such conditions are rather rare, but they do play a role
in some cases and should not be neglected. Also, some
Classification of sexual disorders
66
medical, urological and gynecological disorders cause sexual
activity to lose its pleasurable aspect or to become
uncomfortable and even painful. Under such circumstances a
secondary loss of interest and /or sexual avoidance may occur.
Psychological causes of ISD
When a patient’s sexual drive is constitutionally low, or he
is deficient in testosterone, or he is depressed, i.e., when the
sex centers are hypoactive on a physiologic basis, sexual
appetite is low because it is not generated. But in ISD libido is
diminished because it is actively, albeit unconsciously and
involuntarily, suppressed on the basis of psychological conflict.
In clinical practice psychogenic disturbances of libido are more
prevalent than those that are secondary to physiologic factors.
Some patients are so strongly defended against their
sexual desire that they will actively avoid any situations which
may evoke it. Such patients will not read erotic literature or
look at erotic pictures. They will not discuss sexual topics and
may even experience discomfort when a conversation or joke
has sexual overtones. They may avoid socializing with a
potential sexual partner and will go out of their way to avoid
physical contact. Other patients have learned to control their
sexual appetite so well they don’t need to avoid stimuli which
would ordinary evoke it. They are able to suppress erotic
appetite in the face of the most tantalizing stimulation.
The “Turn Off” Mechanism
Most of patients tend to suppress their desire by evoking
negative thoughts or by allowing spontaneously emerging
negative thoughts to intrude when they have a sexual
opportunity. They have learned to put themselves into negative
emotional states, by selectively focusing their attention on a
perception or thought or by retrieving some memory or
allowing an association to emerge that carries a negative
emotional valence. In this manner they make themselves
angry, fearful or distracted, and so tap into the natural
physiologic inhibitory mechanisms which suppress sexual
desire when this is appropriate and in the person’s best
interest. In other words, sexual desire is normally inhibited
Classification of sexual disorders
67
when the individual is in danger or in an emergency. In
physiologic terms the sex circuits are blocked by the activity of
the fear and “anger” circuits. Some patients have learned to
activate these emergency circuits, evoking or permitting
upsetting thoughts, and in this manner suppressing their
sexual desire.
A variety of evoked images, associations or perceptions
are “selected” for their ability to serve as a “turn off”
mechanism-there is no specificity in the content of these
negatives. A patient will focus his/her attention selectively on
one of the partner’s unattractive physical features-his pot belly,
her unkempt hair, her fat thighs, the odor of his breath, or his
genitals etc.-in the service of shutting down the sex centers. Or
the memory of the partner’s unacceptable behavior or past
injustices may be employed. Other persons choose sexual
times to retrieve memories of non-erotic situations to control
their erotic mood. Work, children and money are commonly
used “turn offs.”
It may be speculated that in patients who suffer from
global ISD, all erotic feelings cause anxiety and evoke the
attendant defenses against this. All sexual situations evoke
negative thoughts and associations. When the desire inhibition
is situational, only specific situations evoke sexual conflict and
cause the patient to tap into the “turn off” mechanism.
Such negative thoughts serve the opposite purpose as
sexual fantasies, which are used to enhance the sexual desire
and serve to diminish the anxieties that turn off desire. Erotic
imagery buffers the sex circuits and protects them from the
negative input which may shut them down. The negative focus
described above does the exact opposite. It “opens the switch”
which will suppress the sex centers.
The person who is conflict-free about sex mentally does
the opposite of the inhibited one, in the sense that he does not
allow negative feelings or thoughts or distractions to intrude
upon his sexual pleasure.
Some persons have a very narrow range of requirements
for sexual pleasure. Only partners with very specific
characteristics “turn them on.” This is adaptive if they are with
Classification of sexual disorders
68
such a desired partner, but if they never seem to find the right
one, the clinician should be alert to the possibility that they are
inhibiting themselves in the service of a hidden sexual conflict.
Others can respond to a wide variety of partners; they are
much more accepting, finding and relating to the partner’s
positive attributes so that they are able to enjoy the
relationship.
The conflicts which cause the patient to be conflicted
about wanting sex-seem to be multiple.
On a deeper level, any and all of the countless reasons
which make sex dangerous or undesirable to that individual
may be operative. There seems to be no specific content, no
special unconscious conflict or fantasy or developmental
disturbance that produces this symptom. A variety of
intrapsychic as well as interactional factors may contribute to
the development of desire inhibition, although ultimately it is
always fear or anger, most often but not always beyond the
patient’s awareness, which makes desire undesirable. These
underlying causes can be organized qualitatively, i.e.,
according to the depth or intensity of the underlying conflict.
Mild Sources of Anxiety
o performance anxiety,
o the anticipation of lack of pleasure in the act,
o mild residual gilt about sex and pleasure.
“Mid-level” Sources of Anxiety
o Unconscious Fear of Success and Intimacy
o Power struggles
o anger at contractual disappointments
Deep Sources of Anxiety
o unconscious fears of injury and/or castration
Treatment of desire dysfunctions
In the simplest terms, the objectives of treatment are to
modify the patient’s tendency to inhibit his erotic impulses, and
to allow these feelings to emerge naturally and without effort
as they will in the healthy, conflict-free person. The patient
must learn not to fight his natural tendency to “turn on.”
Classification of sexual disorders
69
To implement this objective a combination of experiential
tasks and psychotherapeutic sessions is employed.
In the psychosexual therapy of desire phase disorders,
behavioral
experiences
are
employed
together
with
psychotherapeutic exploration of resistances.
ISD patients will seldom improve unless they gain some
measure of insight into underlying conflicts, into why they do
not want sex, and so therapeutic exploration of emotional
conflicts with the aim of fostering insight becomes the primary
treatment modality.
HYPERACTIVE SEXUAL DESIRE
Excessive sexual desire is so rare as to constitute a clinical
curiosity when it is a primary symptom. An abnormally intense
sexual appetite in females has been termed “nymphomania”
and the corresponding condition in the male is “Don Juanism.”
Primary hyperactive sexual desire must be differentiated
from those high levels of sexual activity that are components of
manic and hypomanic states.
Compulsive and obsessive sexual states must also be
differentiated from true excessive sexual desire. Sexual
obsessions are highly prevalent. Many patients are constantly
preoccupied with their sexuality and may masturbate to
orgasm ten times a day or more. However, careful evaluation
reveals that these patients really do not experience an
excessive or constant desire for sex. Rather they are highly
anxious and tense and seek to relieve their discomfort with
sexual activity. In all compulsive states, anxiety rises when the
compulsive act is prevented. And, indeed, these patients
experience a flood of anxiety when they are not engaging in
physical stimulation or in seduction. Sexual activity used in the
service of tension relief is a compulsion and not truly
overactive sexual desire.
Female sexual arousal disorder
Though its actual prevalence is not known, female sexual
arousal disorder (FSAD) is believed to affect a significant
Classification of sexual disorders
70
proportion of women in all age groups. Epidemiological survey
conducted in 1994 in USA shows that 19% of women between
the ages of 18 and 59 reported lubrication difficulties. Some
authors surveyed 100 “normal” couples, finding that 48% of
women reported “difficulty getting excited” and 33% reported
difficulty “maintaining excitement.” However, despite the
frequent difficulty in regard to sexual excitement/arousal, 86%
of these women rated their sexual relations as “very satisfying”
or “moderately satisfying”. This discrepancy may be attributed
to the fact that intercourse may occur even though a women is
minimally aroused while males require a sufficient rigid
erection for intercourse to occur. In this regard, despite the
48% and 33% of women reporting difficulty getting excited and
maintaining excitement, only 15% of the husbands thought
their wives had this problem. In postmenopausal women, the
rate of lubrication problems is even higher, reaching 44% in
one study.
Definition and diagnostic issues
Female sexual arousal disorder specifically refers to the
arousal phase of the sexual response cycle. Criteria for FSAD
according to the fourth edition of Diagnostic and Statistical
Manual of Mental Disorders (DSM-IV; American Psychiatric
Association, 1994) are following:
A. Persistent or recurrent inability to attain, or to maintain
until completion of the sexual activity, an adequate
lubrication-swelling response of sexual excitement.
B. The
disturbance
causes
marked
distress
or
interpersonal difficulty
C. The sexual dysfunction is not caused by a general
medical condition or by direct physiological effects of a
substance.
The essential criteria of a deficient physiological response
agree with the International Classification of Diseases (ICD-10;
World Health Organization, 1992).
Clinical description
Women who meet the criteria for this syndrome feel the
desire for sex and like lovemaking. Frequently they can have
orgasms, especially when stimulated intensely with a vibrator.
Classification of sexual disorders
71
However, they remain dry when they are stimulated in a
manner which would be adequate for most women. Penetration
without normal lubrication and swelling can result in painful
and uncomfortable intercourse. This may result in secondary
problems such as dyspareunia, Vaginismus, and loss of sexual
desire. Partners of such patients often feel rejected and upset
by what they take to be a personal sexual rejection or evidence
that they are poor lovers.
Differential diagnosis
Like the male, the female’s lubrication-swelling response is
mediated by the autonomic nervous system, principally by its
parasympathetic divisions. This mechanism is ultimately under
the control of the cortex; therefore, theoretically female
excitement should be as sensitive to emotional factors as male
excitement. In actual fact, however, the psychogenic form of
this disorder is uncommon. Apparently, a woman with sexual
conflicts is more likely to lose her interest in sex or to develop
orgasm difficulties than to become inhibited in the excitement
phase. Most women who have a normal desire for sex and can
reach orgasm but fail to lubricate are menopausal.
The vasocongestive phase of the female sexual response
cycle is much more resistant to illness and drugs than male
erection, because it involves simpler anatomic structures and
does not depend on a complex hemodynamic high pressure
system in the genitals. The increased pelvic vascularity which
marks the female excitement phase merely causes a
transudate to seep through the vaginal wall.
The only factor that makes female excitement vulnerable
to physical stressors at all is that for proper vasocongestion
and lubrication the vagina must be supplied with adequate
levels of estrogen. When estrogen is deficient the vaginal
endothelium which transmits the fluid and its underlying
network of blood vessels tend to atrophy. The most common
cause of estrogen deficiency is menopause, due to the natural
aging process or to the surgical removal of the ovaries.
Although the senile ovary and the adrenal gland continue to
make small amounts of estrogen in posmenopausal women, in
most cases this is not sufficient to support the lubrication
Classification of sexual disorders
72
function of the vagina. Therefore, all postmenopausal women,
especially if they do not have regular intercourse, are likely to
suffer from deficient vaginal lubrication.
Estrogen
deficiency
is
easily
diagnosed.
Normal
menstruation is presumptive evidence of an adequate estrogen
level and all patients who complain about vaginal dryness
should be asked about the regularity and quality of their
menses. In addition, all patients with this complaint should
have a vaginal examination, which will reveal a dry and pale
vaginal mucosa. Estrogen has a marked effect on the cells that
line the vagina, and a microscopic examination of the patient’s
vaginal smear that has been specially stained will give a rapid,
but not highly reliable, indication of whether estrogen is
deficient. Advanced laboratory techniques for the measure of
estradiol levels in the blood are now available for a much more
reliable measure of estrogen.
The evaluator should inquire about any health problems
that could be contributing to the sexual dysfunction. Although
the following theoretically can interfere with the female
excitement phase by causing a longer arousal time and, in
some instances, by decreasing vaginal lubrication, it should be
noted that they are, with rare exception, not the primary
clinical complaint of excitement phase disturbance.
Neurogenic disorders: disorders affecting the sex centers
of the brain include head trauma or CVA (Cerebrovascular
Accident). This may decrease excitement phase by direct injury
to the sex centers and/or injury to the limbic system or parietal
lobe. Hypothalamic lesions or chraniopharingoma result in the
same from pressure on the cerebral structures, while
chromophobe adenoma decreases excitement not only by
pressure on the sex center and limbic system, but also by
elevating the prolactin level. Psychomotor epilepsy may
diminish female excitement phase by disturbance of the limbic
system.
Disorders affecting the lower neural structures associated
with genital reflexes include the following: neurological
conditions may cause diminished or even absent excitement
phase due to patchy lesions in the spinal cord which interfere
Classification of sexual disorders
73
with genital reflexes. Those which are most frequently
responsible for such sexual difficulties are multiple sclerosis
and alcoholic neuropathy. In fact, sexual difficulties are
sometimes among the first manifestations of multiple sclerosis,
with variable complaints such as diminished lubrication,
diminished or absent clitoral sensitivity, and dyspareunia, all of
which interfere with arousal. Patches of demyelinization in the
spinal cord are responsible. Other disorders affecting the spinal
cord, and possibly associated with decreased or absent arousal
phase, are tabes dorsalis, amyotrophic lateral sclerosis,
syringomyelia, myelitis, and severe malnutrition and vitamin
deficiencies.
Alcoholic neuropathy and herniated lumbar disc lead to
diminished or absent phase by virtue of injury to somatic and
autonomic nerves concerned with genital reflexes, as does
primary autonomic degeneration (Shay-Drager syndrome).
Traumatic injuries to the spinal cord resulting in
paraplegia preclude sexual excitement since no sensations are
perceived. The sensory pathways are interrupted and
sympathetic fibers may also be disrupted.
Vascular problems may result in diminished or absent
excitement phase because of thrombotic injury and occlusion of
pelvic blood vessels. The arousal phase is diminished in many
patients suffering from coronary disease or severe
hypertension. The reasons are probably predominantly
psychological-including depression and anxiety about sudden
death. Antihypertensive and beta adrenergic blocking drugs or
possibly diseased pelvic blood vessels may contribute to
diminished excitement on an organic basis.
Endocrine and metabolic disorders: the following are most
likely to impair the orgasm and desire phases rather than
excitement; the effect on excitement is secondary. Diabetes
mellitus may be associated with diminished or absent
excitement due to neuropathy of the sensory nerves of the
clitoris. Testosterone deficiency states in females result in
diminished lubrication and interference with the functioning of
the sex centers, which require testosterone. In addition, neural
transmission and cellular response of the genitals may be
Classification of sexual disorders
74
impaired. Thyroid deficiency states may interfere with arousal
by mechanisms not clearly understood. Other endocrine
disorders, such as Adison’s disease, Cushing’s syndrome,
acromegaly and hypopituitarism may all diminish excitement
because of various endocrine deficiencies which affect the
sexual circuits of the brain or the cellular response of genitals.
Other medical disorders which may diminish female
excitement include liver disease, due to insufficient conjugation
of estrogen and resulting neutralization of androgens. Such
sexual dysfunction may also result from kidney diseases.
A small number of young menstruating women do
complain about vaginal dryness on a psychogenic basis. In
some cases, this syndrome is clearly related to fear or conflict
about intercourse or to poor lovemaking techniques that do not
provide sufficient time and stimulation for an adequate
response. But the clinical experience with these rare
syndromes has been spare and a specific set of immediate
psychological antecedents has not yet been revealed for this
disorder.
It is also necessary to determine whether sexual
symptoms are secondary to a psychiatric disorder such as an
affective disorder, or an anxiety disorder. A few screening
questions that may be helpful are as follows: has substance
abuse or mental illness ever been a problem? Has the woman
ever received psychiatric treatment or been hospitalized for
psychiatric reasons? Has she ever taken psychiatric
medications? Has she ever experienced depression, phobias, or
panic attacks?
If a psychiatric disorder appears to be present, the
diagnosis and treatment should be clarified. It is important to
know whether any medications could be contributing to the
sexual dysfunction. It is also informative to know which came
first, the sexual symptoms or the psychiatric problems, and
whether extreme stressors are present. As always, the patient
should also be asked about suicidality. Patients with severe
psychiatric illnesses may be too fragile to tolerate psychosexual
therapy or otherwise unable to benefit from it.
Classification of sexual disorders
75
The etiology of excitement phase disorders
The excitement phase in females is accompanied by reflex
vasodilatation with generalized swelling of the labia and the
tissues surrounding the vagina, resulting in heightened labial
coloring and increases lubrication or wetness, the latter
transudes from the vessels in the vaginal barrel. Arteriolar
dilation is caused by activation of two centers in the spinal
cord, one at S2, S3, and S4, and the other at T11, L1, and L2.
As with the male, excitement can be enhanced or inhibited by
signals from the brain, which are in turn influenced by previous
experiences.
Estrogen plays the dominant role in vaginal lubrication. Its
physiologic, cyclic effect
upon cervical secretions is well
known, that is, increased wetness during the midcyclic
ovulatory phase and diminished secretions postovulatory,
coincident with progesterone (anti-estrogen) release and
diminished estrogen production.
Estrogen also affects vaginal lubrication directly by
enhancing the vascular bed beneath the epithelium, which
results in improved lubrication. This effect upon the vaginal
mucosa is not dependent upon ovulation and continues as long
as sufficient estrogen is produced by the ovaries. Although
estrogen production by the ovaries diminishes and eventually
ceases
beyond
the
menopause,
estrogen
levels
in
postmenopausal women can continue to be substantial, due
primarily
to
the
peripheral
conversion
of
adrenal
androstendione to estrone and, to a much lesser extent, of
testosterone to estradiol. However, with increasing age such
adrenal contribution to estrogen production becomes
inadequate to sustain secondary sex tissues such as the
vaginal mucosa and, indeed, even adjacent tissues such as the
urethra and trigone
Although excitement phase dysfunction in females can
exist as a separate syndrome, the discomfort of intercourse
with a dry vagina can easily lead to secondary inhibition of
sexual desire, if not complete avoidance. In essence, then,
female excitement phase disorders are due chiefly to
impairment of the vasocongestive excitement phase response,
Classification of sexual disorders
76
associated primarily with diminished or inhibited estrogen
production. It should be emphasized that in the premenopausal
woman such disorders are relatively uncommon.
Estrogen Deficiency States
Atrophic vulvo-vaginitis. This condition is by far the most
common gynecological cause of excitement phase dysfunction
that cause genital discomfort during the postmenopausal years.
Gynecological examination reveals that the introitus is dry
and often reddened. There may be less muscle tone and fascial
strength (inelasticity) of introital and vaginal supports. The
vaginal mucous membrane exhibits various degrees of dryness
and thinning, sometimes to the point of minute mucosal
hemorrhages.
Laboratory findings will usually show the following: in the
absence of other causes of vaginitis, the wet smear of vaginal
secretions shows mainly parabasal cells. Blood levels of
estrogen are low, while FSH and LH are typically elevated.
Aside from physiological postmenopausal estrogen
deficiency, other conditions which would produce atrophic
vulvo-vaginitis include:
Oophorectomy, particularly in younger women whose
ovaries are still producing significant amounts of
estrogen. The mechanism is, of course, by removal of
the chief source of estrogen supply (“surgical
menopause”)
Radical pelvic surgery (as for cervical cancer), since it
includes oophorectomy and also interferes with the
parasympathetic and sympathetic sensory pathways
To a lesser but sometimes significant degree, vaginal
dryness may be induced by progesterone compounds such as
medroxyprogesterone, which act as anti-estrogens and also
anti-androgens. This would include certain oral contraceptives
containing a high progestin ratio (hypoestrogenic). In such
instances the gynecological examination reveals a noticeable
vaginal dryness but no thinning of the mucosa or petechial
spots, as in atrophic states. The vaginal smear reveals a
preponderance of intermediate cells, rather than cornified or
parabasal.
Classification of sexual disorders
77
Treatment of arousal dysfunctions
The treatment of FSAD may be carried out individually
with the patient alone or in conjoint sessions with the patient
and her partner, or through a combination of the two. In
patients with impaired sexual arousal, treatment may proceed
along medical or counseling sex therapy lines or with both in
combination. Medical treatments are rarely considered for
premenopausal women. Menopausal patients who are estrogen
deficient and have impaired arousal and dyspareunia are often
given hormone replacement therapy alone without specific
counseling. This approach although it improves lubrication and
discomfort, is often inadequate for the treatment of sexual
dysfunction. The most effective approach for these cases would
be specific sex therapy counseling for arousal deficiency, in
addition to hormonal or other medical treatment.
For patients with impaired sexual arousal that is
psychogenic, the range of cognitive-behavioral sex therapy
techniques may be employed. These techniques are integrated
with psychodinamically oriented psychotherapy when deeper
emotional issues and resistances to treatment become
apparent.
Female orgasmic disorder
Orgasm phase disorders are highly prevalent. Among
patients under 40, inhibition of the female orgasm and
premature ejaculation in males are possibly the most common
sexual complaints seen in clinical practice.
Definition and diagnostic criteria
DSM-III describes the following diagnostic criteria for
Impaired Female Orgasm when this is due to psychological
inhibition: “Recurrent and persistent inhibition of the female
orgasm as manifested by a delay in or absence of orgasm
following a normal sexual excitement phase during sexual
activity that is judged by the clinician to be adequate in focus,
intensity, and duration”
Classification of sexual disorders
78
Patients in this diagnostic category are not “frigid” in any
sense of that outdated term. They may be loving, care about
men, be interested in sex, and have the capacity for erotic
pleasure. During loveplay, they may feel sexual excitement and
may lubricate. In other words, the desire and excitement
phases of the sexual response are intact and their chief
complaint is only that orgasm is difficult or impossible to
achieve.
The female orgasm threshold is distributed along a
continuum.
1. At one extreme are those rare women who can have an
orgasm without any physical contact with the clitoral
area, merely by engaging in erotic fantasies, kissing or
stimulation of the breasts.
2. Then there are the approximately 20 to 30% who are
able to achieve orgasm through coitus alone without
direct clitoral stimulation.
3. Next on the continuum are women who can climax
together with their partner but only if coitus is
“assisted” by clitoral stimulation.
4. Women who fall into the next segment of the
distribution cannot reach orgasm in the presence of a
partner, even if they receive clitoral stimulation. They
can, however, stimulate themselves to orgasm when
they are alone and employing erotic fantasies.
5. At the pathological extreme of the orgasm threshold
continuum are the totally anorgasmic women who have
never had an orgasm at all. These constitute
approximately 8% of the U> S> female population
(Fisher, 1973).
The demarcation between normalcy and pathology is a
matter of some controversy. There is little disagreement that
the last two response patterns are clearly pathological and that
treatment should be recommended for such patients and those
with situational anorgasmia who reach climax only in certain
circumstances or with certain partners and not with other
desired partners. Some psychoanalytically oriented clinicians
feel that all women who cannot reach a climax on penetration
Classification of sexual disorders
79
unless by additional clitoral stimulation are abnormal and in
need of treatment, even if they are orgastic with a partner.
However, it is the consensus of current professional opinion
that such a response pattern constitutes a normal variation of
the female sexual response (DSM-III, 1980), and some
therapists with a feminists orientation feel that such women
should never be treated (Hite, 1976).
It has been clinical experience that some coitally
anorgasmic women can acquire a coital orgastic response and
should be given the opportunity for treatment, while it makes
no sense to treat others. The distinction between who should
be offered a trial of treatment and who should be reassured
should be made during the evaluation.
The reaction of women and their partners to this
dysfunction varies widely. In contrast to males, who are always
distressed when sexual excitement does not lead to
ejaculation, some women are perfectly content about not
having orgasms and do not seem to suffer from tension or
discomfort after sexual stimulation. In some cases this is
denial, but there are women who simply find sex gratifying
even if they do not experience a climax. This is not necessarily
a sign of pathological passivity. The person’s point of view
should be respected and that such women should not be
pressured into treatment by husbands or by well meaning
therapists. However, other anorgasmic women are desperate
about their situation, sometimes to the point of obsession.
They complain of tension, physical pelvic discomfort, and anger
at their partner when the sex act always ends with a climax for
him but never for her.
Sometimes the partner is more upset about his mate’s
orgasm problem than she is. The spouse may infers also some
deficiency on his part. This is especially likely if a man
misperceives female orgasm as a man’s responsibility,
something a man “gives” to a woman.
Partner reaction is always an important diagnostic issue
because, even though he may not have caused the patient’s
problem, his negative or pressuring response may create an
Classification of sexual disorders
80
obstacle to her cure, while his cooperation and support are
invaluable for the success of sex therapy.
Primary anorgasmia-never having experienced orgasm by
any means-is not uncommon. Secondary anorgasmia-the onset
of anorgasmia in a woman who has been orgasmic in
masturbation and coitus-is not uncommon, but the diagnosis is
usually secondary to inhibition of desire, even though the
inhibition of orgasm may have occurred first.
The differential diagnosis and etiology
Actually, only a few drugs and illnesses impair orgasm in
women and this syndrome is usually psychogenic.
Over half the women who complain of orgasm problems
have a situational pattern, being able to have orgasm when
they masturbate but not with a partner. It is not necessary to
pursue physical causes in such cases. But for women who have
no orgasms at all, medical causes must be ruled out.
In otherwise healthy women, these include use of MAO
inhibitors (antidepressants) and the alpha adrenergic blocking
agents (used to treat hypertension), true phimosis of the
clitoris, and very rare congenital abnormalities.
Neurological degenerative diseases or injuries or tumors
that destroy the spinal centers and nerves that mediate the
orgasm reflex, severe damage to the genital organs (as in
radical pelvic surgery for cancer), and advanced diabetes,
which may injure the sensory nerve endings of the clitoris, can
also produce an absence or delay of orgasm. But women with
these conditions tend to be ill and have other medical signs or
symptoms.
The history of all totally anorgasmic women should include
questions to rule out these drugs and diseases. A physical
examination is also required to insure that the patient does not
have one of the rare anatomic abnormalities of the genitals
that can cause orgasm problems in women.
The risks of organicity are so low in the primary form of
this syndrome that, when the medical history rules out the
specific illnesses and drugs and patient’s genitals are normal, a
trial of sex therapy without any further medical workup is safe.
However, when a previously orgastic woman loses her capacity
Classification of sexual disorders
81
to climax, especially in the absence of a psychological crisis,
there is a strong possibility that she has a medical problem,
and the diseases and drugs that can cause orgasm impairment
must be carefully ruled out, because serious and treatable
illness, including diabetes, multiple sclerosis, spinal cord
tumors and degenerative diseases, may otherwise be missed.
The most common immediate psychological mechanism
instrumental in the inhibition of the female orgasm is obsessive
self-observation during lovemaking, which will effectively
interfere with the release of the orgasm reflex.
Another common simple cause is that the patient is not
obtaining sufficient clitoral stimulation. This can happen when
the couple has the unrealistic expectation that she should
climax merely in response to rapid penile penetration without
much foreplay and without clitoral contact. In other cases a
woman will not let her partner know what she wants because
of shame and insecurity.
Some anorgastic women are unable to fantasize or to use
sexual imagery. Some report obsessive phenomena, that
unwelcome thoughts or meaningless phrases or parts of songs,
etc., enter their minds during sex. Others feel only neutral or
even irritating sensations when the clitoris is touched and/or
they are simply not aroused by clitoral stimulation. It may be
speculated that these women have erected perceptual defenses
against erotic sensations and are afraid of letting themselves
go in sexual abandonment (fear of the loss of control that
occurs at climax and fear of closeness or fusion with the
partner).
Inability or unwillingness to communicate with the partner
is associated with anorgasmia.
The patient’s deeper
intrapsychic problems in her relationship with her partner are
inferred from her family and psychosexual history and from the
assessment of the couple’s relationship. Conflicts due to strict
childhood prohibitions against masturbation and other forms of
sexual expression are often found in the histories of women
with sexual problems. Most of these women did not masturbate
in adolescence. A significant number had hostile or distant
Classification of sexual disorders
82
relationships with their mothers, who did not encourage their
emerging sexuality.
Unconscious neurotic processes (oedipal conflicts), which
cause the woman to develop a “father transference” towards
her current partner, with attendant defenses against sexuality,
are given a prominent place in the psychoanalytic literature on
female sexual problems. In fact, overly close or ambivalent
relationships with fathers are seen in some (but not all) women
with sexual and relationship problems. Pleasure inhibitions and
ambivalence about closeness and commitment to a man are
often noted when reviewing these patient’s relationships with
the men in their current life. Some women with sexual
problems are competitive with all men and may experience
fear, ambivalence, and mistrust towards their current partner.
This often comes from a sense of outrage at what is perceived
by the woman as unfair advantages accorded to men in our
culture. An overcontrolling and compulsive personality style
which makes it difficult for the patient to “let go” is commonly
found among anorgastic women.
Treatment and prognosis
Treatment must be aimed at correcting fears and
misconceptions. It must also help a woman increase her
assertiveness and sexual initiative, and support her in realizing
that her sexual activity is for her own enjoyment as much as
her partner’s. Progressive exercises in masturbation and in sex
play with her partner may help her to become more familiar
with her desires and sexual responses and to achieve
satisfaction.
Orgasm inhibition of women has an excellent prognosis
with sex therapy. Almost all totally anorgastic women can learn
to have orgasms, even when the symptom is associated with
deeper intrapsychic and relationship problems. Whether the
woman will be able to have orgasms with her partner is not as
easily predictable, since this depends on the nature of the
couple’s system, and may require more complex conjoint
therapy.
Classification of sexual disorders
83
Vaginismus
Diagnostic criteria and clinical features
According to DSM-III, vaginismus is defined as follows:
“There is a history of recurrent and persistent involuntary
spasm of the musculature of the outer third of the vagina that
interferes with coutus”. It is usually evident at the start of a
marriage, precluding consummation.
Ordinarily, when woman is sexually aroused, the vaginal
muscles relax and the introitus opens. But in vaginismic women
the muscles snap together so tightly that penetration may be
impossible. When the vaginal muscle spasm is somewhat less
severe, entry may be forcibly attained but the experience is
painful for the woman. The patient has no voluntary control
over her response, and on a conscious level vaginismic patients
are often extremely distressed by there inability to have
intercourse and children.
It is interesting to note that while some patients with this
disorder also have other sexual problems, many have normal
sexual desire, lubricate, and are orgasmic. It is only
penetration which is difficult, painful, or impossible.
In most cases, the vaginal muscles go into spasm in
response to any attempt at vaginal penetration, so that the
patient has great difficulty in undergoing a pelvic examination.
A few patients have a specific vaginismus which only occurs
during coital attempts and not at other attempts at vaginal
penetrations. These patients can be examined without difficulty
and this situational pattern rules out organic obstruction.
The differential diagnosis
Those patients who find vaginal penetration difficult in all
situations must first have a vaginal examination to rule out
organic obstruction and to establish that the vaginal muscles
are in fact in spasm.
The examiner can palpate the vaginal muscles and confirm
that they are tightly closed. Patients with vaginismus may feel
pain when examiner’s finger are first introduced, but if the
examiner retains the examining finger in the vagina while she
quietly reassures or distracts the patient, the vaginal muscles
Classification of sexual disorders
84
of vaginismic patients will usually relax within 10 to 60
seconds. The patient then begins to feel comfortable with the
speculum or the examiner’s finger inside her vagina. She has
been confronted with the important fact that there is no
structural abnormality and that the block was only due to her
muscle spasm, which will diminish if she does not panic.
If the vaginal muscles are found to be tight, the next
diagnostic question is whether the cause of the spasm is
psychogenic or physical, because both can result in muscle
spasm. Any gynecological disorder that makes sex painful can
evoke a conditioned guarding response and vaginismus.
Endometriosis, PID, vaginitis, herpes, birth and surgical injuries
of the genitals are among the many painful medical disorders
which can result in this syndrome.
For this reason, if the patient complains of pain during the
vaginal examination, apart from that produced by the spastic
vaginal muscle, a thorough gynecological evaluation is in order
to insure that no treatable or dangerous gynecological
conditions are missed.
Behavioral
analysis
shows
that
the
immediate
psychological cause of vaginismus is a reflex involuntary spasm
of the muscles that guard the vaginal introitus. At times the
patient’s sexual history reveals a specific precipitating trauma,
such as incest or rape or a painful attempt at intercourse.
Some have or have had a painful gynecological condition.
Others are guilty and conflicted about sex. In many cases,
however, the patient remembers nothing that could explain her
symptom.
Analysis of the intrapsychic dynamics and of the couple’s
system shows that the underlying psychological causes range
from the trivial to the serious. Vaginismus may occur as an
isolated symptom in a basically healthy woman who is in a
good relationship. Other vaginismic patients have severe
neurotic conflicts about sex. Some are ambivalent about their
marriage and/or about pregnancy or motherhood. Some are
passive-aggressively punishing their husbands. Some have a
panic disorder.
Classification of sexual disorders
85
When evaluating the vaginismic patient it is important to
gauge the severity of the underlying emotional problem,
because this will determine how difficult treatment will be. In
the more complex cases the symbolic meaning of the symptom
and/or the role that the closed vagina plays in the relationship
should be assessed, so that the therapist knows what
psychological issues will have to be confronted during the
psychodynamic aspects of treatment.
Many vaginismic patients develop a secondary phobic
avoidance of vaginal penetration. This must be analyzed so it
can be treated before the vaginal spasm, for one can hardly
expect a patient to proceed with vaginal dilation if she panics
at any approach to her vagina.
Treatment and prognosis
Regardless of the severity of the associated emotional
problems, the symptom of vaginismus has an excellent
prognosis with treatment that includes progressive vaginal
dilation. Although patients with more complex problems may
resist during therapy, it is the rare vaginismic woman whose
symptom cannot be cured with brief, direct, behavioral
treatment.
Male orgasmic disorder
There are three types of ejaculatory symptoms which may
be either psychogenic or organic: absent or delayed (retarded)
ejaculation, absence of orgastic sensation or partially retarded
ejaculation, and rapid (premature) ejaculation. “Dry” orgasm is
caused by retrograde ejaculation or by anejaculatory orgasm,
which are always due to organic causes.
Male orgasmic disorder (302.74) was formerly called
retarded ejaculation. This ambiguity in diagnostic label refers
to what is primarily stressed out-not ejaculating or not being
coitally orgasmic. In some cases retarded ejaculation is seen
because his partner wants to be impregnated and couple seeks
treatment because the retarded ejaculation creates frustration
over the consequent infertility. However, in actual practice,
retarded ejaculation refers to male coital anorgasmia and
Classification of sexual disorders
86
treatment strategies are directed at the inability to have
specifically coital orgasms. Some men with this condition are
proud of maintaining erection for a long time and repeatedly
satisfying partners. Yet, clinical experience shows that this
creates problems in relationships because man’s partner takes
it as a personal rejection.
Definition and diagnostic criteria
DSM-IV describes the following criteria for male orgasmic
disorder: “Recurrent and persistent delay in or absence of
orgasm following an adequate excitement phase”.
The diagnosis of retarded or absent ejaculation is not
based on how long it takes to reach orgasm. The duration of all
phases of the sexual response cycle varies among individuals
and from one occasion to another. Many people vary the
amount of time at any stage of the sexual response for their
own satisfaction or their partners’. Retarded or inhibited
ejaculation exists when a man wishes to pass from the plateau
stage to ejaculation but cannot. With increased striving for
ejaculation, his distress increases, ejaculation becomes more
difficult, and pleasure diminishes. If ejaculation does occur, it is
relatively unsatisfying. Men with this condition usually do not
have the same problem with masturbation but do have it with
genital contact with partners.
Differential diagnosis
The
differential
diagnosis
between
organic
and
psychogenic RE is simple in the majority of cases. Most
retarded ejaculators below the age of 50 can climax without
difficulty on masturbation and organic factors do not have to be
considered in these cases. In older men, the ejaculatory delay
often occurs in all situations; then medical causes must be
ruled out.
Ejaculation may be delayed or blocked by any physiologic
stressors that impair the sex drive, including testosterone
deficiencies, depression, and drugs which depress the central
nervous system, such as alcohol, sedatives, and narcotics.
The aging process, which increases the refractory period
of the male orgasm, alpha adrenergic blocking drugs and also
thioridazine are virtually the only organic causes which
Classification of sexual disorders
87
selectively impair the orgasm phase of the male sexual
response cycle and produce no other sexual or medical
disabilities.
Primary RE is usually psychogenic, secondary ejaculation
problems carry a significant risk of organicity. When a man
whose orgasms have previously been normal complains of
delayed ejaculations, unless this is clearly the product of the
normal aging process, a thorough medical history and
neurological workup is requires because serious neurological
disease states may be associated with this symptom.
Surgical and traumatic injuries, tumors, disease of the
spinal cord and of the pelvic nerves that mediate ejaculation,
and advanced diabetes which injures the peripheral nerves can
certainly cause ejaculatory difficulties. However, in such cases
the patient either has a history of radical pelvic or abdominal
surgery or spinal cord injury or will probably have other
neurological signs and symptoms. These are likely to affect the
motor and sensory functions of the lower extremities. And,
since the spinal cord centers which control these reflexes are in
close proximity, impairment of urinary and/or bowel control is
often seen together with ejaculatory symptoms that are caused
by neurological impairment.
When a patient complains that he experience normal
orgastic sensations but no fluid emerges from his penis,
anejaculatory orgasm must be differentiated from retrograde
ejaculation. This differential is not difficult, since the two
syndromes are produced by different states and drugs. The
most common cause of retrograde ejaculation is transurethral
prostatectomy. Anejaculatory orgasm is caused by the failure
to produce semen or by a blockage of the tubus which conduct
semen from the testicles to the urethra. Vasectomy is currently
the most common cause of anejaculatory orgasm.
The differential diagnosis between these two syndromes is
made by examining a post orgasm urinary specimen under the
microscope. Sperm cells will have entered the bladder and will
be found in the urine of men with retrograde ejaculation, while
the urine of anejaculatory patients will contain no sperm.
Classification of sexual disorders
88
Etiology
The etiology of retarded or inhibited ejaculation remains
controversial, but it often involves internal conflicts over coitus
and ejaculation that the man finds unacceptable. Often the
problem is lifelong, but it sometimes develops after a traumatic
incident (such as discovering a partner’s infidelity), after the
onset of represses or suppressed anger toward the wife
following a period of good sexual functioning.
The most common immediate psychological antecedent
that blocks ejaculatory release is the same as in female orgasm
inhibition-obsessive self-observation. The patient obsessively
wonders: “Will I come? When will I come? IS she getting tired?
Is she really enjoying this? IS she making love to me because
she has to?” he is free of theses obsessions when he
masturbates and immerses himself in his sexual fantasies, and
therefore has no trouble ejaculating in that situation.
Deeper psychological problems include all the neurotic
conflicts about sex and all the relationship difficulties that have
been implicated in the other sexual disorders of males.
Ambivalence and rage towards women, which derive from
unresolved childhood problems with mother, are particularly
prevalent in this group. Fears of intimacy, commitment and
pleasure are also common and related to the same dynamics.
Exploration of the patient’s feelings towards women and a
detailed analysis of his relationship with his mother, as well as
with his current partner, often reveal neurotic processes that
must be dealt with in treatment. Retarded ejaculators are
frequently very angry at their current wives and lovers and
involved in sadomasochistic system with them. They “hold
back” their orgasms along with their rage. A rigid, compulsive,
and overcontrolling personality with difficulty in handling anger
is often seen in this patient population.
Treatment
Treating retarded ejaculation is usually very difficult, and
success may be followed by relapse. Sometimes the emotional
dynamics of the couple are involved with the relapse, so
treatment requires cooperation and motivation by both
partners. Progressive behavioral therapy is used over a period
Classification of sexual disorders
89
of weeks; vigorous manual stimulation to orgasm by the
partner is followed by vigorous manual stimulation and
insertion just as ejaculation is about to occur.
Premature Ejaculation (PE) (302.75) is the most
common sexual problem for men. Almost all men ejaculate
rapidly in their first-partner sexual experiences. Such response,
with or without distress, is normal in adolescence; this is not
PE, as control has not yet been learned-something that will
come with experience, i.e. with time many men are able to
teach themselves how to achieve control that is gratifying and
satisfactory. However, ejaculatory control is elusive for many
men, and their sexual experience becomes defined by it. The
figures vary by author, with the range being between 30% and
75%. Obtaining an accurate figure of incidence is complicated
by the lack of agreement as to definition. Many men who have
PE may develop a secondary erectile disorder and may
therefore present to the clinician with a different chief
complaint.
Definition and diagnostic criteria
DSM-IV defines premature ejaculation as follows:
A. Persistent or recurrent ejaculation with minimal
sexual stimulation before, on or shortly after
penetration and before the person wishes it. The
clinician must take into account factors that affect
duration of the excitement phase, such as age,
novelty of the sexual partner or situation, and recent
frequency of sexual activity.
B. The disturbance causes
marked distress
or
interpersonal difficulty.
C. The premature ejaculation is not due exclusively to
the direct effects of a substance
Defining this condition has always been a source of
controversy. Vasilchenko finds that ejaculation is premature if
it occurs within 60 seconds after penetration or by 20 penile
thrusts. He defines this condition as ejaculatio praecox
absoluta-EPA. Masters and Johnson (1970) diagnosed
premature ejaculation (PE) when the male would have an
Classification of sexual disorders
90
orgasm before his partner more than 50% of the time, i.e.
when a man cannot control his ejaculation after vaginal
penetration so that a fully orgasmic partner fails to reach
orgasm at least half the time. The DSM-IV definition quoted
above depends on a person’s subjective sense of regulation,
not on limits of time, thrusts or even personal satisfaction. This
seems more practical, since some men and their partners are
not distressed by rapid ejaculation. They are able to develop
mutually enjoyable lovemaking patterns despite lacking
control. Men who ask for help feel sexual dissatisfaction
because ejaculation occurs before the individual wishes it. This
often (though not always) has an impact on the individual’s
partner, resulting in distress or interpersonal difficulty. The
individual feels a reinforced sense of shame, dread,
humiliation, and inadequacy with painful consequences. The
partner initially maybe confused and may feel responsible, but
the more usual response in a partner who has some sexual
understanding is to feel frustrated, impatient, and angry. This
in turn is perceived by the individual, which only intensifies his
anxiety and distress and distorts even further the nature of the
sexual experience.
Most cases of PE are primary, in that the condition has
always existed. In the rare cases on which it is secondary, it is
usually associated with a specific psychosexual stress. Long,
enforced sexual abstinence may produce rapid ejaculation
when sexual activity is resumed; most men rapidly regain
voluntary control, but, in some, PE apparently becomes
established with increasing anxiety. All men with PE experience
anxiety, which is central to the dysfunction. The initiation of
sexual activity is viewed by both partners with apprehension,
and completion of sexual activity is associated with a
decreasing level of satisfaction. As a secondary phenomenon,
sexual desire becomes inhibited, and in some men, erectile
capacity is also impaired. They may develop a secondary
pattern of sexual avoidance.
Etiology
There have been many attempts to explain the cause or
causes of PE. The sexual status examination of premature
Classification of sexual disorders
91
ejaculators indicates that they are frequently not aware of the
state of their sexual excitement or of their level of tension.
These patients may obsessively focus on trying to control their
ejaculation. Their excitement rises rapidly and they are not
conscious of the sensations premonitory to orgasm. It has been
postulated that this perceptual failure is the key to this
syndrome.
Sensory awareness is necessary for acquiring
control of all voluntary reflexes, including ejaculation. On a
deeper level, many premature ejaculators are conflicted about
sexual gratification and pleasure and seem to suppress or deny
their erotic sensations when these become “too” intensely
pleasurable or last “too” long. The premature ejaculator’s
perceptual defenses thus interfere with this learning process.
Unconscious intrapsychic conflict seems to appear less
often in PE than inmost sexual dysfunctions. PE is often
isolated symptom, and no other psychological problem can be
detected on the evaluation. In such cases the syndrome can be
conceptualized as a sexual learning disability. In other cases,
prematurity is associated with deeper psychological problems
and difficulties in the marital relationship. It has been
postulated that premature ejaculators are hostile to women
and that their symptom serves the unconscious purpose of
depriving their partner of pleasure. Another view has been that
PE is an expression of castration anxiety. The vagina is seen as
frightening and dangerous, and the PE serves to “get the penis
out of their” as rapidly as possible. Clinical evidence shows that
psychological problems of these patients are not specific. One
finds loving and kind as well as hostile men in this population;
the partners also vary from loving to demanding. For this
reason, the psychodynamics and relationship system of each
patient must be carefully and individually evaluated.
Differential diagnosis
The excellent response of this syndrome to psychotherapy
indicates that primary prematurity is rarely organic. However,
there are some congenital conditions of the urinary tract and
spinal cord which can cause ejaculatory control difficulties on a
physical basis. The most common of these is spina bifida. Such
conditions are extraordinarily rare and tend to be associated
Classification of sexual disorders
92
with other signs and symptoms of medical and neurological
disability.
Therefore, when a healthy young man who has a negative
medical history complains that he has always come too rapidly,
a syndrome of lobuli paracentralis should be ruled out. This
syndrome is triggered by the affected cortical centers that are
responsible for regulation of urogenital functioning. The
syndrome marked by PE, nocturnal enuresis, pollakiuria and
premature puberty. Neurologic symptoms are associated with
integrating in the process of pyramid innervation.
Secondary prematurity is much more likely to be caused
by an underlying medical disorder, especially when the loss of
control is not associated with significant stress or a change in
the patient’s sexual relationship. A frequent case of late
occurring PE is organic erectile dysfunction. The man, who is
progressively becoming impotent for a medical reason may
“learn” to ejaculate rapidly before he loses his tenuous
erection. Some surgical procedures and spinal cord disorders
can cause secondary PE by impairing the nerves and neural
center that govern the ejaculatory reflex. Therefore, when a
man who had enjoyed good control complains that he is now
coming rapidly, it is mandatory that he receive a careful
Neurologic or urologic evaluation.
Treatment and prognosis
Ejaculation is a matter of control. Not surprisingly, the
most common method for treating PE is the behavioral
approach. PE has an excellent prognosis with sex therapy that
uses either the “squeeze” or the “stop-start” methods. The
symptom can often be cured with these behavioral measures,
even if it serves unconscious defensive functions. However,
when prematurity plays a role in the patient’s intrapsychic
dynamics and/or the couple’s neurotic system, treatment is
likely to be more complex. In such cases rapid improvement in
sexual adequacy is apt to evoke anxiety and resistances to
treatment that require psychotherapeutic interventions.
Surprisingly, the SSRI medications, such as Prozac, Paxil,
and Zoloft, whose negative side effects include decreased
sexual desire and less intense orgasm, can be a good
Classification of sexual disorders
93
treatment for PE. Phosphodyesteras inhibitors help a man
sustain his erection even after the orgasmic release, making
these medications also helpful in assisting men with PE.
Male erectile dysfunction
Erections difficulties are found in all ages. They become
more common with age. While any problem with sex is
upsetting to a man, nothing generates as much concern,
anxiety, shame and even terror as an inability to get or
maintain erections. This can make a man feel less of a man.
The primary meaning of impotence, the term traditionally
applied to erection difficulties, is “a lack of power, strength and
vigor”-the negation of all that is considered to be masculine.
Sexual excitement in both males and females is caused by
reflex vasodilatation and congestion of the genital organs. This
influx of blood changes them from the quiescent state and
prepares them for their reproductive functioning. The
excitement phase in males marked by penile erection and in
females by vaginal lubrication and swelling.
Definition
Erectile Dysfunction (ED) or Inhibited Sexual Excitement
in the male is defined in the DSM-IV as “Recurrent and
persistent inhibition of sexual excitement during sexual
activity, manifested by partial or complete failure to attain or
maintain erection until completion of the sexual act”. This
definition assumes that sexual desire is present, that the
environment is suitable. This definition includes the rare cases
of male erectile difficulty during masturbation.
Most patients with ED find kissing, touching and even
genital contact pleasurable, but the arousal component of
these behaviors is blocked either continuously or intermittently.
If this blocking occurs frequently, it can lead to diminished
desire, in which case inhibited sexual desire is a secondary
diagnosis. Some of these men develop a secondary avoidance
of sex, so that it may look as though they are completely
asexual.
Classification of sexual disorders
94
ED is always obvious and causes concern, even though its
occasional occurrence is a natural part of most men’s
experience. The outcome depends on how a man interprets it.
Most men accept it enough to be able to go on to further
sexual experiences unimpeded. Their partners are usually even
less concerned. However, some men, after even one episode of
impotence, approach sexual activity with dread and monitor
their performance. This fear may well be confirmed: the man’s
attention shifts from his pleasure to the degree of his penis’
tumescence or flaccidity. Treatment must focus on eliminating
spectatoring and the underlying anxiety.
Careful and meticulous questioning is often necessary to
elicit the precise and detailed information about the specific
circumstances under which the erectile difficulty appears that is
needed to differentiate between organic and psychologically
impotent men. Some patients have morning erections, or can
masturbate without difficulty when they are alone, but are
impotent with a partner. Some complain they cannot attain an
erection. Others lose it-when they take their clothes off, or are
about to penetrate, or are inside the vagina or when there is a
demand for performance, or when they are with certain types
of women, or in an intimate or committed situation. Still others
complain that their erections are not completely firm. The
partner’s reports are frequently helpful in clarifying these
important diagnostic issues.
Women vary greatly in their reaction to their partner’s ED.
Some are marvelously supportive and convey to the man the
massage that he is important to her-not his erect penis. Such
loving attitudes rule out partner pressure as an etiological
factor. At the other extreme are partners who are sexually
demanding and critical and carry on when their man does not
perform to their satisfaction. Some women insist on
penetration as their only means of gratification, or object to
their partner’s use of erotica, or do not wish to stimulate his
genitals. The pressure created for a man when he knows that
his partner expects him to attain an erection rapidly and
maintain it until she is satisfied heightens his performance
anxiety and is likely to create or aggravate his potency
Classification of sexual disorders
95
problems. Sometimes partner may be supportive, but he may
be so consumed with self-loathing that he can’t accept what
she offers. Many men distance themselves from their partners
after such “failures” and engage in orgies of self-flagellation.
Etiology
The highly complex erectile system depends on the
integrity of the delicate penile anatomy, the pelvic blood
vessels and nerves, the correct balance of neurotransmitters
in the brain, a functional autonomic nervous system, an
adequate hormonal environment, and last but not least, a calm
and erotically focused psyche. It is not wonder that erection is
the most vulnerable part of the male sexual response and that
impotence can be caused by a variety of drugs and disease
states and emotional stressors.
Psychological factors play a role in almost all cases of ED,
whether primarily organic or psychogenic. The patient who is
partially impotent because of a mild circulatory deficiency
frequently reacts to his diminished erectile capacity with panic,
thereby worsening the physical disability. For this reason, the
psychological aspects of the problem should be evaluated in all
cases of erectile difficulty, even when the problem is clearly
organic.
Here is an outline of the issues that should be considered
while evaluating a patient with erectile dysfunction:
I. Psychogenically caused erectile dysfunction
A. Anxiety
There are many presentations of anxiety, from performance
issues to insecurity about a man’s sense of masculinity.
B. Depression
Depression is one of the most common causes of impotence.
Sometimes the sexual dysfunction is the presenting symptom
of a man who denies his emotion and says he is not depressed.
C. Unconscious sexual conflict
II. Organically caused erectile dysfunction
A. Disease of or injury to the nervous system
1.
The brain-strokes, tumor, trauma, Parkinson’s
disease, dementia, surgery
Classification of sexual disorders
96
2.
Spinal cord-trauma, tumor, surgery, multiple
sclerosis
3.
Prostate and rectal surgery, trauma
B.
Disease of or injury to the circulatory system
1.
Arteries-arteriosclerosis, diabetes, hypertension,
trauma, aneurism, surgery
2.
Veins-venous leaks, incompetent veins
3.
Blood-severe anemia, sickle-cell anemia
C.
Disease of the endocrine system
1.
Hyperprolactinemia
The hormone prolactin, which controls the production of
milk in a nursing mother, is usually present only in minimal
amounts in the male. One of its secondary effects is to diminish
sexual interest and arousal. Tumors of the pituitary gland can
cause an abnormal increase in the production of prolactin,
leading to impotence in man.
2.
Hypergonadotropic hypogonadism: testicular
The testicles manufacture androgens, which are necessary
for sexual desire and function. When the testis do not function
properly, as sometimes happens after mumps, trauma, or
abnormalities of fetal development, the pituitary sends out
more gonadotropic hormone to try to “turn on” the
underfunctioning testes. Blood tests diagnose this condition.
3.
Hypogonadotropic hypogonadism: pituitary
Like the aforementioned condition, this disease is marked
by insufficient androgens in the man’s system. This time it is
caused by a malfunctioning pituitary gland, so that the
gonadotropic hormones that “turn on” the testes are low or
absent. Again, blood tests are necessary to make this
diagnosis.
4.
Thyroid disease
Thyroxin, the major hormone produced by the thyroid
gland, regulates the metabolic rate of the entire body. Both
too little (hypothyroidism) and too much (hyperthyroidism)
can lead to impotence. Physical examination and blood tests
are the means to diagnosis.
5.
Adrenal disease
Classification of sexual disorders
97
The hormones of the adrenal gland-steroids and
adrenaline-regulate a wide variety of bodily functions. Again,
too much or too little can cause erectile problems.
D.
Local conditions
1.
Peyronie’s disease-fibrosis of penis, which can
cause the penis to bend to one side or other
2.
Phimosis- a condition in which the foreskin is
contracted and cannot be retracted.
E.
Drugs
There are a variety of medications and street drugs that
can lead to erectile problems. The most common are
antidepressants, antihypertensives, antiandrogens, estrogen,
cimetidine, marijuana, and cocaine.
Alcohol and smoking tobacco are risk factors to ED. Social
drinking or having “just a few drinks to relax” may inflame
desire but kill erections. Long-term alcoholism-which can
destroy testicular cells, lower testosterone production, and
increase the production of female hormones-has serious
negative effects on penises and sexual desire. Smoking
contributes to the hardening and clogging of arteries, including
the ones that supply blood to the penis. Smokers have far
more potency problems than nonsmokers.
Most patients have more than one factor causing their
erectile dysfunction. In a man with diabetes, for example,
vascular, neural, and psychological factors may combine to
cause erectile dysfunction.
In most cases, the currently operating immediate
psychological cause of psychogenic ED is performance anxiety.
An examination of the patient’s mental processes when he
attempts to make love will reveal this mechanism: “I wonder if
it will work,” or “I’m afraid I might not be able to have an
erection,” or “I don’t think I can keep this erection until she
comes,” etc. Because of his obsessive concern about his
erections, he is very likely to experience difficulty. The focus on
performance to the exclusion of pleasure is threatening and,
since the erectile response is very sensitive to emotion, the
physiologic concomitants of the patient’s performance anxiety
Classification of sexual disorders
98
will trigger the reflexes that drain the penis of the extra blood
required for erection.
Sometimes performance anxiety is “pure” and the
psychological assessment of the couple reveals that the patient
is free of emotional problems and that his relationship is good.
In other cases the symptom serves as a defense against
unconscious sexual conflict or plays a dynamic role in
relationship difficulties. Such issues must be detected during
the evaluation. The psychopathology of the impotent patient is
not specifically different from that of men with other sexual
symptoms. Psychoanalytic theory postulates that unresolved
oedipal problems and “castration anxiety” play a role in male
sexual disorders and it is not uncommon to see evidence of
ambivalence towards women and excessive sexual fears in
impotent men.
“Oedipal” problems are recognized by investigating the
patient’s family dynamics and also by analyzing his adult
sexual relationships. Was he overly close to or ambivalent
toward his mother? Is he still too involved with her? Does he
make “mothers” out of his current lovers or does he phobically
avoid women who remind him of his mother? Is he overly
competitive with or fearful of other men? Is his anxiety about
sex excessive and impervious to realistic reassurance? The
evaluation of impotent men frequently reveals that they are
ambivalent about or openly hostile towards women and that
they are still overly involved with their mothers.
Many men with erectile difficulties have received negative
messages about sexual pleasure. For this reason, it is
important to assess the attitudes about sex and pleasure that
prevailed in the patient’s family of origin.
Partner’s aggressive sexual demands and critical attitudes
play a causal role in impotence. An aggressive, nonsupportive
partner who uses sex as a pawn in the marital struggle is often
the critical element in impotence and the success of treatment
may depend on the improvement of the partner’s attitudes.
Therefore, the assessment of the couple’s sexual system and of
the partner’s emotional characteristics is important in the
evaluation of men with erectile problems.
Classification of sexual disorders
99
Diagnosis and differential diagnosis
Since the physical manifestations of psychogenic and
organic impotence are identical, unless the symptom is clearly
situational, organic factors must always be investigated and
ruled out during the evaluation.
In men under the age of 40, psychogenic impotence is
more common, while in older men there is a higher risk of
organicity because of the greater incidence of circulatory
problems and diabetes, as well as the more common usage of
medications with sexual side-effects. So, the fact that erectile
dysfunction increases progressively with age does not mean
that it is an inevitable consequence of aging: other age-related
conditions increase the likelihood of its occurrence.
Essentially, the diagnostic procedure consists of
systematically ruling out the few disease states, such as
diabetes and testosterone deficiency, that are known to cause
obvious neurogenic, vasculogenic, and endocrine problems- a
complex, costly, and far from precise procedure.
Actually only a small proportion of impotent patients
require a complete urological workup. A skillful examiner who
is knowledgeable about sexual medicine can probably rule out
organicity in over 90% of psychologically impotent patients on
the basis of the interview alone, simply by establishing that the
difficulty fluctuates with the patient’s emotional state. Patients
whose erectile impairment has an organic basis do not have full
erection at any time, while men whose problem is psychogenic
may experience erectile difficulty only under emotionally
demanding circumstances. For this reason impotent patients
must be carefully questioned about spontaneous erections,
erections on masturbation, as well as a.m. and nocturnal
erections. If the patient or his partner recalls normal erections
that are undiminished in quality and firm enough for
penetration in any circumstance, organic factors do not have to
be investigated further.
Treatment and prognosis
Maltifactorial nature of erectile dysfunction requires a
multidisciplinary approach to its management.
Classification of sexual disorders
100
If there are physical problems influencing the patient’s
sexual function, there are a variety of treatment options that
can be used in conjunction with psychotherapy.
Oral medication. There are several oral medications that
operate to increase the likelihood of obtaining and maintaining
an erection. They operate in slightly different ways, but
basically they all function to increase the blood flow into the
cavernous areas of the penis and to retard outflow. Success
with these agents is variable. They include yohimbine, alpha 2
blockers,
trazodone,
vasodilan,
L-arginin,
and
phosphodyesteras type V inhibitors (sildenafil citrate [Viagra],
tadalafil [Cialis], vardenafil hydrochloride [Levitra]).
The agents of the latest group specifically inhibit
phosphodiesterase type V, the class of enzymes that are
responsible for the breakdown of cGMP. The type V isoform is
expressed in reproductive tissues and the lung. Inhibition of
the breakdown of cGMP enhances the vasodilatory action of NO
in the corpus cavernosum and in the pulmonary vasculature.
Nowadays sildenafil citrate is approved for treatment of
pulmonary hypertension and does not prescribed to ED patients
due to its severe adverse effects. Phosphodiesterase type V
inhibitors are contraindicated in patients taking nitrates,
because a sharp blood-pressure drop might occur, resulting in
a heart attack.
Patients whose ED is the product of mild performance
anxieties growing out of a lack of sexual confidence and
partner pressure that is only due to ignorance and not a
product of rooted hostility have an excellent and rapid response
to sex therapy. Those whose symptoms reflect profound
psychopathology and marital difficulties are, of course, more
difficult to treat. It is important to assess the severity of the
underlying problems during the evaluation in order to be able
to give the patient a realistic estimate of his prognosis.
Classification of sexual disorders
101
Ejaculatory Pain Due to Muscle Spasm of
the Male Genitals
This rather rare syndrome is analogous to vaginismus in
the sense that it is caused by a painful and involuntary spasm
of the muscles of the reproductive and sexual organs. In the
male the cremasteric muscles and/or the smooth muscles of
the internal male reproductive organs and/or the perineal
muscles react with painful spasm as the man ejaculates or
immediately thereafter. Patients typically experience a sharp
cramp-like pain immediately upon ejaculation. this may be mild
but can be excruciating and disabling. The pain is experienced
in the perineum and in the shaft of the penis. It may be
transient or last for hours ad even days. The physical
examination between episodes is normal and may also be
normal while the patient is in pain. Sometimes, however, the
scrotum is red, swollen, tender and tense during an attack.
Patients tend to be extremely distressed by this symptom
and develop a fear of and avoidance of orgasm, which creates
an intense conflict when they feel sexual tension. Some
patients always experience the pain whenever they ejaculate,
on masturbation as well as with a partner. In other cases the
symptom is situational and is experienced only when they are
ambivalent about ejaculating.
Differential Diagnosis
Organic disorders, such as prostatitis, epididymitis,
vesiculitis, diseases of the urethra and referred pain from other
areas can theoretically cause ejaculatory pain, and evidence of
these should be pursued during the medical history. Actually,
organic ejaculatory pain is rare, but must nevertheless always
be ruled out as it can be associated with dangerous disease
states including penile cancer. The diagnosis of ejaculatory
muscle spasm is made by the typical history of pain, by
exclusion of organic causes, and by a trial of sexual therapy.
There is some evidence to suggest that the painful
ejaculation syndrome lies on a continuum of ejaculatory
inhibition which results from ambivalence about orgasm. At one
Classification of sexual disorders
102
extreme is retarded ejaculation, then partially retarded
ejaculation, next is the syndrome of functional ejaculatory pain,
while the orgastic experience of the least conflicted men merely
lacks gratification and pleasure. This syndrome may explain
some of those puzzling cases of ejaculatory pain that remain
undiagnosed and unimproved after repeated urological
examinations.
Sexual Phobias and Avoidance
The avoidance of sex because of irrational fears and
phobias is not, strictly speaking, a sexual disorder, because
there may be nothing wrong with the phobic patient’s sexual
response. For this reason it is not included in DSM under the
psychosexual disorders. However, sexual phobias are discussed
here because these disabling syndromes are very common
among patients with sexual complaints and are frequently
amenable to sex therapy. Actually, some elements of sexual
avoidance is present in almost all sexual disorders, but it is the
essential feature of sexual phobias.
The detection and analysis of a phobic component in any
sexual problem are important aspects of the evaluation,
because the patient’s avoidance of sex must be resolved before
the other aspects of the difficulty can be treated.
According to DSM-IV, sexual phobias are classified under
the term “Psychosexual Disorder Not Elsewhere Classified.”
Diagnostic Criteria and Clinical Features
The essential feature of a sexual phobia is the persistent
and irrational fear of and compelling desire to avoid sexual
feelings and/or experiences. The fear is recognized by the
individual as excessive and unreasonable.
Phobic patients may avoid sex altogether or their anxiety
and avoidance may be confined to specific aspects of sex:
sexual failure, the genitals, sexual secretions and odors, sexual
fantasies,
various
erotic
activities
such
as
kissing,
masturbation, orgasm, undressing before the partner, seeing
the partner nude, pregnancy, etc.
Classification of sexual disorders
103
Fear and avoidance of sex are often highly distressing and
may seriously interfere with the development of a normal sex
life, romantic attachments, and marriage. The social and
emotional life of such patients may become progressively
constricted as a result of their avoidance of sexual situations.
Some patients with sexual phobias remain virgins all their
lives; many do not marry and some become socially isolated.
Other phobic patients manage to marry despite their phobias,
but their lives are never easy. During the evaluation it is
important to gain an understanding of the emotional damage
which has resulted from the patient’s phobic avoidance of sex,
as this usually requires additional therapeutic intervention.
When the phobic person is “trapped” into a situation
where sex can no longer be avoided on the pain of losing a
valued partner or feeling guilt about frustrating a beloved one,
the experience is extremely unpleasant. Phobic patients report
that they feel panic or revulsion and sometimes rage during
sex. A common experience is trying “to get it over with as
quickly as possible.”
Some partners of phobic patients are amazingly
understanding, patient, and protective. Others are furious and
threatened and try to manipulate and pressure the phobic
patient for sex. The partner’s reaction is a significant variable
in planning therapy and in estimating the prognosis, because
the cooperation of a gentle, nonpressuring partner is extremely
helpful in treatment.
Sexual phobias must be differentiated from other kinds of
problems which result in sexual avoidance. Some patients with
ISD avoid sex because it gives them no pleasure. Others with
anxiety about their sexual performance are afraid to face the
humiliation and frustration of failure. Still other patients avoid
intercourse because it is physically painful or uncomfortable,
while some deliberately withhold sex to punish their partner.
Again, the differential diagnosis between these different causes
of low sexual frequency is important because in each entirely
different treatment approaches are required.
Paraphilias
104
Chapter 5
Paraphilias
The word paraphilia describes a variety of sexually intense
experiences that differ from the standard pattern. Formed by
the prefix para (meaning “beside” or “alongside of”) and philia
(“love”), a paraphilia then was originally conceived of as a
sexual act or fantasy lying “alongside” or “outside” the normal
experience of love.
The most recent Diagnostic and Statistical Manual (DSMIV) considers a paraphilia to have basic characteristics:
1. An intense, recurrent sexual experience existing for at
least six months that involves fantasy, urges, or behavior.
2. A particular object of the sexual experience-nonhuman
things, individuals who suffer or are humiliated, children
or other nonconsenting persons.
3. A particular result of the sexual experience-clinically
significant distress or significant impairment in social,
occupational, or other important areas of function.
The DSM-IV classifies perversions into eight categories:
1. Exhibitionism. The exhibitionist is usually thought of as a
man who exposes his genitals to a stranger. It is unusual
for an exhibitionist to do more than show himself and
perhaps masturbate. Most men anticipate the viewer’s
shocked response, though some imagine that the
surprised woman will find them sexually desirable. In
general, exhibitionists are younger men who began their
activity prior to the age of eighteen.
2. Fetishism. Fetishism is the preference for nonliving objects
as the exclusive means of attaining sexual excitement.
The fetishist prefers the fetish rather than the human
being associated with it. Such behavior is “safe” in that it
avoids the dangers of a real human experience. Not all
fetishists require the fetish for gratification, but without it
sexual excitement tends to be much less intense. The
most common fetish is an article of clothing. Minor
Paraphilias
3.
4.
5.
6.
105
fetishistic behavior should not be considered aberrant;
however, when the fetishistic behavior becomes acute,
relationship problems occur and normal sexual relations
tend to be avoided. There is evidence that in some
fetishists a biogenic factor is present, namely, abnormal
electrical activity in the temporal lobes indicative of
temporal lobe epilepsy.
Pedophilia. Pedophilia is a preference for repetitive sexual
activity with prepubertal children. Twice as many
pedophiles prefer opposite-sex children. Heterosexually
oriented
males
prefer
8to
10-year-old
girls.
Homosexually oriented males prefer a partner 10 to 13
years of age. Adults who have no sexual preference
choose children under age 8. Incestuous pedophilia is
found in only 15 per cent of cases. On the other hand, the
victim is a total stranger to the pedophile in only 10 per
cent of cases. While in general the pedophiles are males,
it is well known that there are women who have sexual
relations with young boys. However, they are almost
never charged with the crime of pedophilia. Mothers are
occasionally involved in incest with their preadolescent
daughters, as well as sons.
Masochism. True sexual masochism involves sexual
excitement generated by one’s own humiliation, pain, or
suffering. It can involve being spanked, whipped, tied up,
or made to say humiliating things. Sexual asphyxiation, a
form of masochism that involves becoming oxygen
deprived-often by a rope around the neck-is a particularly
dangerous form of sexual arousal that leads to a number
of deaths.
Sadism. Sadism exists in a spectrum from mild fantasies
of dominance all the way to lust murder. The sadist is
more likely to be a man, is likely to have known about his
predilection as an adolescent or young adult, and is likely
to maintain this form of sexual interest for many years.
Transvestic fetishism. A man who wears women’s clothes
because he believes he is a woman in a man’s body is a
transsexual. A man who wears women’s clothes because
Paraphilias
106
he gets sexually aroused while doing it is a Transvestic
fetishist. This disorder is limited to males, most of whom
are heterosexual, though some may report homosexual
experiences.
Their
preferred
sexual
release
is
masturbation, and their desire is stimulated by the clothes
they wear. A gender identity disorder (transsexualism)
may appear in these individuals depending on their degree
of satisfaction with their maleness.
7. Voyeurism. A voyeur is someone who seeks out situations
where he can secretly observe another person undressing,
naked, or engaging in sexual activity. The voyeur
masturbates while peeking, or afterwards while the
memory is still fresh. Interest in sexual looking begins in
early adolescence and to some extent is normal. It
becomes a paraphilia when it persists, becomes an
individual’s main form of sexual gratification, and causes
him distress or leads to social problems, the most
common of which is getting caught.
Other Parafilias. This category includes rare types of
nonstandard sexual behavior, such as zoophilia in which sexual
excitement is produced by the act or fantasy of engaging in
sexual activity with animals. Animals are the preferred form of
sexual outlet, even when other forms are available. Coprophilia
(the love of feces), frotteurism (sexual excitement produced by
by rubbing against an unsuspecting stranger), klismaphilia
(autoeroticism produced by a self-administered enema),
mysophilia (sexual excitement created by filthy surroundings),
necrophilia (sexual excitement produced by sexual activity with
a corpse), telephone scatalogia (obscene telephone calls) and
urophilia (sexual excitement produced by urination on a victim)
are other types of nonstandard sexual behavior.
Not all persons who exhibit paraphiliac behavior are
distressed. Many come to the physician’s attention because the
behavior distresses the spouse, usually the wife (paraphiliac
disorders affect males far more frequently than females), or
because the behavior has become a criminal offense and the
Paraphilias
107
patient a “sex offender”, who is referred by some agency of the
criminal justice system.
Within the range of paraphiliac behavior, paraphiliacs are
a heterogenous group engaging in diverse sexual activity. Their
degree of psychopathology varies from mild to severe and the
degree of danger to the public ranges from nonexistent to
grave. Moreover, there is no direct correlation between any of
the paraphilias and character structure or personality trait.
These are also heterogeneous and very diverse.
The primary-care physician has only to retain his
equanimity and detached concern long enough to obtain a
reasonably accurate history that will enable him to make an
appropriate referral to a psychiatrist.
The primary-care physician should empasize to the patient
the inherent dangers of the paraphiliac behavior, both legal and
social, and stresses the importance of psychiatric care. The
physician should be considerate and compassionate while
indicating willingness to continue medical care during and after
psychiatric treatment.
Understanding the psychodynamics of perversion
Sigmund Freud’s View of Perversion
Freud thought a perversion was the “inverse of a
neurosis.” To understand his vision, we must understand
neurosis. A neurotic symptom is the result of a compromise
between a wish and the anxiety that the wish generates. The
symptom, for example impotence, serves to hide knowledge
and expression of a forbidden thought or action. We can say
that the symptom expresses the wish and fear simultaneously,
and does this while keeping both out of the awareness of the
individual with the symptom. Thus, a neurotic symptom is the
mixing together of a wish and a fear. It is a displaced, often
symbolized expression of a forbidden sexual or aggressive
wish.
In a perversion this situation is reversed. Instead of
feeling threatened by the open expression of forbidden desires,
the perverse individual clings to them, is excited by them, and
wishes to enact them. Instead of the disgust or anxiety most of
us would feel when confronted with the fantasy of being sexual
Paraphilias
108
with a child, the pedophile finds the notion arousing. Thus, the
perverse individual enacts a forbidden sexual wish in fantasy
and perhaps realty.
In a healthy individual, anxiety functions as a signal that
some desires are unacceptable because they will cause trouble
either in realty or in the inner world of prohibitions against
incestuous, rapacious desire. The signal is recognized, and
behavior is inhibited, rerouted. Defenses come into play to
manage the impulse. Healthy defenses allow the energy behind
the impulse to be used in socially acceptable, positive ways.
In the neurotic, defenses also come into play, but they are
less adequate to the task. Instead of rerouting behavior into
positive channels, a neurotic symptom appears. The man who
(unconsciously) wants women to admire his erect penis is
unable to speak in public. The woman who (unconsciously)
desires to seduce the thirteen-year-old boy who lives next door
is unable to go over and borrow a cup of sugar.
Freud noticed that children naturally enjoy and do many of
the things we think of as perverse. However, as the child grows
up and matures he leaves behind “polymorphous perverse”
sexuality and replaces it with adult, genital sexuality. The
perverse individual is neither concerned with giving speeches
nor unable to borrow sugar.
The perverse sexual act serves to protect an individual
from the anxieties involved in separating and individuating. In
a sense, Freud was suggesting that perverse patients are
desperately holding on to sexualized, childhood ways of
experiencing and feeling and are unable to grow up and face
the realities of adult sexual life.
Robert Stoller’s Model of Perverse Sexual Excitement
Stoller considers that a particular kind of hostility drives all
forms of sexually exciting fantasy. The more hostility, the more
perverse the fantasy or action. Stoller wrote: “...hostility, overt
or hidden, is what generates and enhances sexual excitement,
and its absence leads to sexual indifference and boredom. This
dominance of hostility in eroticism attempts to undo childhood
traumas and frustrations that threaten the development of
masculinity and femininity (gender indentity). The same sort of
Paraphilias
109
dynamics, though in different mixes and degrees, is found in
almost everyone, those labeled perverse and those not so
labeled.”
What does this mean? It means there is a spectrum of
childhood trauma ranging from minor and unavoidable to
severe and unusual sexual, physical, and emotional abuse. It
means that when the child experiences these traumas as aimed
at his or her developing sexual self, the child attempts to cope
with the threat by the creation of fantasy stories that are
sexualized. The themes of these stories eventually coalesce to
form a core masturbation fantasy, which becomes the center
around which adult sexual experiences are organized.
Many victims of child abuse are so overwhelmed that they
avoid sexual experience all together, but some are pervesely
drawn to it. It is a well-Known fact that individuals who
sexually abuse have often been sexually abused. If they have
not been sexually or physically molested, they have been
subjected to repeated hostile, humiliating emotional abuse that
was experienced as an attack on their gender identity.
Perverse sexual fantasy and action are attempts to change
the past in order to prove to the individual that he is no longer
the small, powerless, frightened little person that he once was.
Treatment and Prognosis
Treatment of the paraphilias should not be undertaken by
a nonpsychiatric physician. All cases should be referred to a
psychiatrist. Patients with paraphilias are difficult to treat, and
the results of therapy are often disappointing. Seldom do
patients seek treatment on their own. More often they are
referred by their wives or by the courts. Occasionally they
request treatment because of threat of legal action or of
divorce. The prognosis is much more optimistic if the patient’s
concern about his deviant behavior is sufficient to cause him to
seek help on his own., If motivation is not inadequate, the
patient will skip therapy sessions, avoid “homework”
assignments, resist revealing his fantasies or dreams, and use
passive-aggressive maneuvers with the therapist, such as
arriving late, forgetting sessions and diverting the attention of
the therapist to irrelevant issues.
Paraphilias
110
The principal objectives of any therapy are to increase
heterosexual
responsiveness
and
decrease
paraphiliac
behavior. Within this framework, the therapist attempts to help
the patient establish a rewarding sexual relationship and to
improve sexual functioning within that relationship. The
therapist usually tries to help the patient control his
undesirable sexual behavior rather than to reduce his interest
in it. If this proves to be impossible, the therapist helps the
patient adapt to his deviant role.
Gender identity disorders
111
Chapter 6
Gender identity disorders
The fourth edition of the Diagnostic and Statistical Manual
of Mental Disorders has five criteria that must be met before a
diagnosis of gender identity disorder can be given:
1. There must be evidence of strong and persistent crossgender identification.
2. This cross-gender identification must not merely be a
desire for any perceived cultural advantages of being the
other sex.
3. There must also be evidence of persistent discomfort
about one's assigned sex or a sense of inappropriateness
in the gender role of that sex.
4. The individual must not have a concurrent physical
intersex condition (e.g., androgen insensitivity syndrome
or congenital adrenal hyperplasia).
5. There must be evidence of clinically significant distress
or impairment in social, occupational, or other important
areas of functioning.
The current edition of the ICD-10 (International Statistical
Classification of Diseases and Related Health Problems) has
five different diagnoses for gender identity disorder:
transsexualism, Dual-role Transvestism, Gender Identity
Disorder of Childhood, Other Gender Identity Disorders, and
Gender Identity Disorder Unspecified.
Transsexualism has the following criteria:
The desire to live and be accepted as a member of the
opposite sex, usually accompanied by the wish to make
his or her body as congruent as possible with the
preferred sex through surgery and hormone treatment.
The transsexual identity has been present persistently
for at least two years.
The disorder is not a symptom of another mental
disorder or a chromosomal abnormality.
Gender identity disorders
112
Dual-role transvestism has the following criteria:
The individual wears clothes of the opposite sex in order
to experience temporary membership in the opposite
sex.
There is no sexual motivation for the cross-dressing.
The individual has no desire for a permanent change to
the opposite sex.
Gender Identity Disorder of Childhood has essentially
four criteria, which may be summarized as:
The individual is persistently and intensely distressed
about being a girl/boy, and desires (or claims) to be of
the opposite gender.
The individual is preoccupied with the clothing, roles or
anatomy of the opposite sex/gender, or rejects the
clothing, roles, or anatomy of his/her birth sex/gender.
The individual has not yet reached puberty.
The disorder must have been present for at least 6
months.
The remaining two classifications have no specific criteria.
This chapter discusses gender identity problems in terms of
age-related developmental stages, because this approach
seems to be of most practical value to physicians. At each
stage beyond infancy, problems representing normal
developmental conflicts are differentiated from those
considered pathological.
Childhood
During infancy (birth to 18 months) core gender
identity is already being learned. The most severe gender
identity disorder, transsexualism, is already manifests in this
period. This early onset has led to speculation that a disorder
of fetal sex hormone is etiologically significant in
transsexualism. In any event, physicians not consulted about
transsexualism at this early stage.
Some organic and intersex conditions that often cause
sexual identity problems later in life are evident at birth, but
Gender identity disorders
113
only those that produce ambiguous or anomalous external
genitalia usually are recognized.
The ambiguous genitalia in girls are enlarged clitoris with
or without some degree of labial fusion. This is noticed in
infants with hyperadrenocorticism or whose mothers were
exposed to androgenic substances in the first trimester.
Ambiguous genitalia in male are microphallus and hypospadias
or epispadias. Extremely rare is the condition of true
hermaphroditism. Definitive medical or surgical intervention
can be undertaken ad completed immediately for some of
these
problems,
such
as
progestin-induced
female
pseudohermaphroditism. Crucial decisions affecting sexual
identity must be made immediately after birth to prevent
sexual identity problems. This process often involves complex
determinations of chromosomal, gonadal, hormonal and
anatomical sex, and sometimes delicate decisions about the
appropriate sex of assignment and rearing.
During toddlerhood and preschool period (1 ½ years
through 5 years), many aspects of normal development can
become the basis of sexual identity problems. The first object
of identification for both boys and girls is a mothering female;
it is entirely normal for children of this age to show both samesex and cross-sex identification. As they explore their
identities, they magically assume that they can be whichever
sex they wish. Intermittent (but not predominant or preferred)
cross-sex identification or behavior in boys and girls does not
indicate sexual identity problems.
If parents or other important adults misinterpret such
manifestations, however problems may ensue. For example, a
father who sees his son playing with dolls or wanting to wear
an apron and help mother cook may think he is effeminate or
potential homosexual. The father may withdraw and reject,
ridicule and disturb the boy’s masculine development by
becoming unavailable as a role model and by convincing the
child that he must, indeed, be unmasculine. Such conflicts can
be induced by either parent in children of either sex, although
in this culture, at least, cross gender behavior is usually more
censured in boys than in girls by parents of both sexes, and
Gender identity disorders
114
fathers tend to be more concerned with clear sex differentiation
than mothers.
Both envy and fear of the opposite sex occur normally in
preschool children. Girls may envy male genitals as something
they do not have and may fear them as potentially damaging.
Boys may fear female genitals as something to confirm the
possibility of castration and may envy females’ capacity for
creativity and their dominance in the world of the toddler.
These normal internal struggles can become pathological, with
the child rejecting his or her own sex, when parents and other
adults fail to value the sexes equally.
During this period, Oedipal conflicts are most intense. The
conflict caused by fear of the fantasized retaliation by the
“rival” same-sex parent may cause the unconscious wish to
submit to that rival as a love object to retain his love and
appease him. Also, some parents render heterosexuality
genuinely unattractive or fearsome through their relationship
with one another or with the child. Obligatory or preferential
homosexuality may sometimes have such a background.
Organic conditions, such as genital malformations, begin
to produce subjectively perceived sex identity problems in this
period. During these years, most children become clearly
aware of anatomic sex differences. Body image formation,
especially with respect to the genitals, is a major component of
sexual identity. Toddlers begin to compare themselves with
others. More important, those whose genitals remains
ambiguous may continue to suffer from ambiguous gender
identity messages in their rearing by parents, older siblings and
others.
Any delay in correcting remediable conditions should be
discouraged. However, correction carries risks of its own.
Whether surgery is performed mainly to prevent further
emotional damage due to genital ambiguity , or whether it is
medically unavoidable, as in some cases of second – or laterstage repair of hypospadias, careful psychological counseling
and follow-up for the child are imperative.
Precocious puberty, whether idiopathic or organic, can
occur even before age 5. Cases with specific pathology demand
Gender identity disorders
115
immediate treatment. When treated early enough, these
conditions need not cause a child serious sexual identity
problem unless the reactions of others make the child believe
he is sexually abnormal. Even conditions that virilize as well as
cause
precocious
puberty
in
girls,
such
as
hyperadrenocorticism, need not disturb normal core gender
identity if the girls are treated early and raised unambiguously.
A possible parallel has been noted in boys exposed to excessive
levels of female hormones in utero. They are less aggressive,
less assertive and less athletic than controls.
Disturbances in core gender identity become set and
behaviorally obvious during this period. Transsexuals already
are firmly set in their cross-sex behavior and preferences.
These children cross-dress whenever possible, they hate and
avoid all activities and interests of their own biological sex and
they are interested only in those of the opposite sex. Boys are
extremely feminine in appearance and behavior, girls are very
masculine. These children are already aware of intense gender
dysphoria. Their parents either foster their cross-gender
identity or make no effective efforts to interfere with it.
Disturbances in sex-appropriate behavior are a separate
entity, both clinically and conceptually. The younger the child,
the more difficult it is to distinguish such disturbances from
those of core gender identity, and to differentiate disturbances
from normal variations. Cross-sex role preference may reflect
not problems of core gender identity or sexual orientation, but
a child’s observation of, or belief that there is, preferential
treatment of the opposite sex or denigration of his own sex
within the family. Sometimes the same-sex parent or, less
frequently, an older sibling or other important relative displays
behavior or a personality that makes him or her unacceptable
to the child as someone with whom to identify. Parents,
siblings or other relatives may systematically negate and
demean the child’s sex-appropriate behavior.
Cross-sex interests and behavior-effeminacy in boys and
tomboyism in girls-is common in sexual identity problems
observed during this period. These are temporary or
intermittent in normal children. When persistent (especially
Gender identity disorders
116
effeminacy in boys), they announce significant conflict. By age
5, a boy who consistently prefers to play with dolls and girls
and is indifferent to trucks, fire engines and strenuous noisy
play with other boys is probably expressing a sexual identity
problem.
During the period of early school years (6 years to
puberty) there is increased interaction with the environment
during this time, when the child in moving out of the parental
cocoon into the wider world of peers and teachers. This process
heightens the possibility that masculine and feminine
stereotypes may distort atypical but normal interests and
attitudes onto conflicted or pathological sexual identity. School
children can be very cruel, and they may place a normal but
studious boy who is not interested in sports in the same
category as effeminate boys who have serious sexual identity
conflicts. Some athletic coaches even exceed children in
shattering the sense of masculinity in normal boys if they are
not as competitive as the coaches expect them to be.
Tomboyism is not as stigmatized as effeminacy, but girls too
can be made to doubt their femininity if they deviate from the
stereotypes of the community.
Toward the latter part of this period, homoerotic play
begins to increase. For the vast majority of youngsters this is
not prognostic of homosexuality and they are seldom disturbed
about it. However, the parents may be horrified and, by their
actions and attitudes, may convince the child he is abnormal.
They often seek medical advice, although they may find it
difficult to accept even the most knowledgeable reassurance
that such play is usually just part of growing up.
When visible body or genital abnormalities have been
repaired or may not be fully correctable, they become
particularly troublesome to a child because of the emotional
and ego development characteristics of latency. Body and
genital comparison is ubiquitous in the showers and toilets of
schools-perhaps less so among girls than among boys, but this
difference is diminishing. Children with uncorrected conditions
respond intensely to their own perceptions of their pathology,
as well as to the real or imagined reactions of others.
Gender identity disorders
117
Girls whose mothers were exposed to androgenic
substances during the sixth to twelfth week of pregnancy and
who developed progestin-induced hermaphroditism constitute
one group of children who have no active organic pathology,
but who, in this period, show behavioral consequences of fetal
androgenization. Even if this condition is recognized at birth,
the anomalous genitalia immediately repaired and the girls
assigned and reared unambiguously as females, they show
more tomboyism than average. However, there is no
disturbance of core gender identity or, so far as is known, of
later sexual orientation. There is the same possibility of
analogous behavioral shifts in fatally estrogenized boys.
Transsexualism is evident in this age period to anyone
who pays attention to the child. Typically, the child’s crossgender identity has been fostered at home; now the child
confronts the full community and for the first time feels the
weight of social disapproval and rejection. This makes the child
miserable without modifying his inappropriate identity in the
least. It is usually in this period that true transsexuals first
come to medical attention because the parents also cannot
ignore the pressure from others, the diagnosis of
transsexualism in females at this age is often less clear than
that in males because of society’s greater tolerance of crosssex preferences in girls.
Persistent effeminacy and tomboyism are common in
sexual identity problems that appear in childhood. In a
comparative study of markedly effeminate boys and their
families and of a control group of noneffeminate boys and
families, it had been found that the early life experiences of the
effeminates include:
1. Parental fostering of, or unconcern about, effeminate
behavior during the earliest years.
2. Lack of psychological separation from the mother,
caused in part by excessive holding of the baby.
3. Maternal overprotection and inhibition of rough-tumble
play with other boys.
4. Greater availability of female than male companions and
playmates in the early years.
Gender identity disorders
118
5. Actual or emotional unavailability of a consistent adult
male role model.
6. Strong paternal rejection of the young boy.
7. Unusual physical beauty, which may influence adults to
treat the boy as a girl.
There is expert consensus that markedly effeminate boys
are at higher risk of developing one of these-three gender
identity
disorders:
transsexualism,
transvestism,
and
homosexuality.
Preadolescence
and
adolescence
Normal
developmental behavior in this period that most likely gives
rise to sexual identity problems is homoerotic play. Mutual
masturbation is the most common homoerotic act of both
sexes, but any homosexual behavior, e. g., fellatio,
cunnilingus, may occur normally at this phase.
Puberty and early adolescence bring to light several
organic and intersex conditions that usually are not evident in
childhood. Turner’s syndrome is finally diagnosed because of
the complete absence of puberty. Exogenous estrogen will
produce the external physical changes of puberty and feminine
appearance. These girls need serious, repeated reassurance
that their sexual function can be entirely normal and that they
can be mothers by adoption.
Failure to menstruate, even though other pubertal
changes have taken place, can have many causes; one is
vaginal agenesis. In some girls, this is a relatively simple
consequence of incomplete Mullerian ducts development, and
the girl has normal ovaries, tubes and uterus; in others there is
faulty development of the other internal sex organs as well.
Whether reproductive capacity can be established depends on
many factors, but vaginal agenesis is relatively simple in terms
of healthy sexual identity. These patients have been reared as
girls and, in the absence of sexually pathogenic influences,
have a normal female core gender identity, heterosexual
orientation and feminine sex role preferences. Vaginoplasty is
usually safe and successful and permits full sexual function,
includig orgasm.
Gender identity disorders
119
A more striking intersex condition that is sometimes
revealed when menarcheal failure and vaginal agenesis are
investigated is the androgen insensitivity (testicular feminizing)
syndrome. In the fully developed form of this familial disorder,
the body cells of a genotypic male are completely insensitive to
androgen. Because of cellular insensitivity to androgen, the
external genitaliadifferentiate as female, the normal result of a
lack of fetal androgen during the sixth to fourteenth weeks, the
infant is born with normal looking female external genitalia and
is assigned and reared as a girl. There are no ovaries or other
female reproductive organs, and abdominal testes produce
normal amounts of androgens. At puberty the estrogen
normally produced by the testes and the adrenal glands cause
breast growth and other female body characteristics-a
phenotypically normal looking pubescent girl.
Only laparotomy prompted by lack of a vagina reveals the
absence of other female structures and the presence of testes.
Although medically dramatic, this condition causes few major
problems of sexual identity. The patient will be infertile and will
require vaginoplasty with administration of exogenous
estrogens after the testes are removed. However, normal
female sexual identity has already occurred, and if the patient
can be helped to resolve the emotional trauma of discovering
her lack of reproductive potential, sexual identity problems
generally do not occur.
Because body preoccupation is painfully intense in early
adolescence, anomalous genitalia or atypical secondary sex
characteristics can cause not only sexual identity problems but
even psychotic depression and suicide. That is why in cases of
true hermaphroditism, all organs of the sex opposite to the sex
of rearing should be surgically extirpated, so that the physician
can honestly assure the adolescent that no contradictory sex
organs exist.
The gender dysphoria of transsexualism reaches a peak of
painful intensity in early adolescence. Adult body configuration
and genitalia intensify the rejection of what the individual
considers to be the ''wrong'' anatomy. Adult sex drive coupled
with the impossibility of functioning as members of the sex to
Gender identity disorders
120
which they feel they ''really'' belong are deeply frustrating
realities that transsexuals cannot deny. Some early-adolescent
boys surreptitiously obtain and use estrogens to effect body
changes. Some already begin to press for sex-reassignment
surgery. Request for sex reassignment surgery increase in late
adolescence and are sometimes desperate.
Delayed or absent puberty caused by organic pathology,
especially in boys, is commonly not discovered until late teens.
The etiology varies, it is often untreatable and it sometimes is
life compromising. As in other conditions not evident in
childhood, normal rearing can protect the child from major
disorders of sexual identity, but not from the trauma to his
sense of male adequacy caused by failure to achieve puberty or
to look like or function sexually as a man. Of course any
treatable condition should be treated immediately, but
diagnosis and treatment of delayed sexual maturation is highly
complex and still experimental.
Therapy
Education and explanation often remain the physician's
most helpful tools in treating sexual identity problems. Helping
the child or adolescent and the adults in his life to understand
what is happening, and why, often makes therapy unnecessary
if the problem has not yet become internalized or fixed. The
younger the child, the more necessary it is to involve the entire
family in therapie for a sexual identity problem.
The principle of earliest intervention is axiomatic in
medicine and nowhere more so than in intersex conditions.
Because many components of sexual identity are fixed or most
strongly influenced early in life, the sooner that ambiguities can
be resolved, especially in the parent's minds, and decisions
made about sexual assignment and rearing, the more troublefree will be the development of the child's sexual identity.
Ego-dystonic homosexuality
121
Chapter 7
Ego-dystonic homosexuality
Egodystonic sexual orientation is an egodystonic condition.
The World Health Organization lists egodystonic sexual
orientation in the ICD-10, under "Psychological and behavioral
disorders associated with sexual development and orientation".
The WHO describes it thus:
The gender identity or sexual preference (heterosexual,
homosexual, bisexual, or prepubertal) is not in doubt, but the
individual wishes it were different because of associated
psychological and behavioral disorders, and may seek
treatment in order to change it. (F66.1)
The WHO applies the following note to the entirety of part
F66: "Sexual orientation by itself is not to be regarded as a
disorder."
Ego-dystonic homosexuality was included in the American
Psychiatric Association's DSM-III but it was removed from
DSM-III-R in 1987, because "almost all people who are
homosexual first go through a phase in which their
homosexuality is ego-dystonic". But psychically distressing
("ego-dystonic") homosexuality appears in DSM-IV. Under
"Sexual Disorder Not Otherwise Specified," there is the
diagnosis "Persistent and marked distress about sexual
orientation". This category includes distressing homosexuality
and distressing heterosexuality.6 DSM-IV doesn't use "egodystonic" to name distressing homosexuality; indeed, it doesn't
even use "homosexuality" to name it.
Probably 1 to 3 per cent of female, and 3 to 6 per cent of
male, adults are predominately or exclusively homosexual, and
perhaps as many as 33 per cent of all people will have had
some kind of homosexual activity during their lives.
Available evidence indicates that the biologically normal
newborn infant probably has an innate neuropsychological and
neuroendocrinological bias toward an eventual heterosexual
orientation. If this point of view is accurate, it means that, in
Ego-dystonic homosexuality
122
the absence of biological abnormality, various kinds of
unnatural influences are necessary to disrupt heterosexual
orientation permanently.
Probably adult homosexuality can result from many
different influences-some known, some speculated, some still
unknown. One possibility is that there is an alteration or
aberration in the fetal hormonal influences that organize the
embryonic central nervous system for ultimate heterosexual
arousal and responsivety. The altered developmental biology
could reverse that bias or diminish or neutralize its strength.
Although there is no direct empirical evidence for this as a
basis of homosexuality in man, experimental evidence on
primates and other mammals, and clinical evidence from
studies on human endocrinopathies and genetic disorders
suggest that some such altered biology during fetal
development may play a significant role in some or all gender
role and orientation deviation.
A known cause of homosexuality in some adults is
unconscious conflict arising from postnatal rearing influences
that make heterosexuality unappealing or unattainable. The
causes and psychodynamics of such conflicts are varied. There
is no doubt that such conflicts are etiologic in homosexual
psychiatric patients who are unhappy with their homosexuality.
It is not known whether or what extent they are etiologic in the
much larger nonpatient homosexual population, although
several researchers typical conflicts in nonpatient research
population also. If aberrant fetal biology plays no role, fairly
powerful and chronic influences are probably necessary to
deflect the innate heterosexual bias. If fetal biology is aberrant,
a child may have less resistance to relatively minor pathogenic
experiences of the sort that might also be found in the histories
of many heterosexuals. Homosexuality that arises from
interpersonal ad intrapsychic conflict may be considered an
adaptive response to the psychological repudiation or
avoidance of heterosexuality.
There are many social learning theories that explain
preferential adult homosexuality on the basis of various
Ego-dystonic homosexuality
123
postnatal learning and socializing influences and that minimize
the importance of unconscious conflict. But as general
explanation, these theories lack credibility because of the onesided position they take in the nature/nurture interaction,
neither extreme of which is scientifically tenable.
Homosexuality does not necessarily imply diminished
function in other areas of life or even an impoverished sex life.
There are more homosexuals who feel satisfied and are
productive or creative in all walks of life than homosexuals who
cannot function effectively because of emotional conflict over
their sex orientation.
If aberrant fetal biological development is found to be the
basis of some homosexuality, such cases could possibly be
considered one of the sexual anomalies. Perhaps only that
unknown proportion of cases of homosexuality that are
traceable to identifiable interpersonal and intrapsychic
disturbances of psychosexual development can be assumed to
follow the medical psychiatric model of illness. Even in these
cases, determining what to do about the problem is the sole
right and choice of the individual, except in specific instances of
misuse against others. A broad range of homosexual persons
and homosexual behaviors, perhaps a majority, probably fall
outside such a model of illness and reflect a wide variety of
motives, origins, and individual and cultural meanings.
Varieties of homosexual expression
Preferential or obligatory homosexuality
– elicits the most interest and is subject to the most bias and
misunderstanding, even though only minority of persons who
have ever had any homosexual experiences fall into this
category.
These people can respond erotically only to members of
the same sex, or they are more readily and pleasurably
aroused by members of the same sex even when opposite sex
partners are available and willing.
Ego-dystonic homosexuality
124
Developmental homoerotic activity is homosexual in terms
of object choice, but it is usually not prognostic of adult
homosexuality. It may occur at any or all immature
developmental stages in both boys and girls, Kinsey found that
33 per cent of women and 50 per cent of men recalled
preadolescent or adolescent homoerotic play.
Pseudohomosexuality
– has been described primarily in males but complementary
motivation may operate in females. The primary conflicts of
pseudohmosexuals concern dependency and power, which they
associate respectively with femininity and masculinity. If they
perceive themselves as week or inadequate compared to other
men, they unconsciously assume that they are nonmasculine,
which equals feminine, which equals homosexual.
The most common symptom of this condition is
pseudohomosexual anxiety or panic, often when the man finds
himself in an all-male environment or when some life situation,
such as rejection by a sex partner or losing out to another man
in the competitive job market, is perceived as a blow to
masculine self-esteem. Sometimes these men may act out
these conflicts in occasional homosexual behavior, either to
test out their perceptions of themselves or in passive
resignation to what they perceive as their fate.
These experiences are usually not satisfying and are often
severely
anxiety-producing.
But
pseudohomosexuality
sometimes develops into a pattern of exclusive behavior
through restricted learning and socialization and through the
absence of emotional freedom to explore heterosexuality.
The childhoods of these men may have been characterized by
passivity and isolation from peers, but few remember wishing
to be girls or feeling early erotic attraction to males.
Pseudohomosexuality is a risk for people of either sex
whose developmental conflicts gave them an inadequate sense
of masculinity or femininity.
Ego-dystonic homosexuality
125
Situational homosexuality
– is that which occurs among preferential heterosexuals in
enforced single-sex envirenment, such as some armed forces
assignments. Usually these people revert later to their
heterosexual patterns and no problem is presented to the
physician
unless
the
experience
precipitates
a
pseudohomosexual panic.
Exploitative homosexuality
– is that in which people with physical and social power, as in
an inmate subculture, force weaker or more submissive people
to be sexual objects, usually through anal intercourse but also
through fellatio. While there may be unconscious sexual
identity conflicts in the exploiters, these are essentially acts of
violence in which the penis is used as a weapon or symbol of
dominance, as in heterosexual rape. Sexual exploitation
motivated by power, dominance and underlying rage also
occurs in women’s prisons. Male exploiters typically do not
consider themselves homosexual and would rarely seek
therapy for a sexual conflict.
Enforced homosexuality
– is the complement of exploitative homosexuality. While there
is a general and probably accurate consensus that primarily
erotic homosexual preference cannot be induced in anyone in
the absence of pre-existing sexual orientation conflicts, there is
one report of preferential homosexuals who claim never to
have had homosexual tendencies before being forced in prison
to be regular sexual objects.
Treatment
More professionals consider treatment in appropriate for
homosexuals who are content with their preference. However,
some homosexuals are very distressed about their homosexual
feelings and seek treatment with the aim of acquiring the
capacity to love a woman, to experience heterosexual
gratification, and to enjoy a normal family life. Many clinicians
Ego-dystonic homosexuality
126
consider these persons eminently deserving of a trial of
treatment.
The published data on shift in orientation among
homosexuals of both sexes after psychoanalysis or
psychoanalytically-oriented psychotherapy are remarkably
consistent: about one-third or more of those patients who wish
to change and who remain in treatment become exclusively
heterosexual, and about one-third more become bisexual or
preferentially heterosexual. A somewhat higher reversal rate
has been reported with the use of psychoanalytic group
therapy in groups composed entirely of homosexuals.
Evaluation of sexual disorders
127
Chapter 8
Evaluation of sexual disorders
The first step in the treatment of sexual disorders is a
thorough evaluation. The physician must clarify the chief
complaint, establish an accurate diagnosis and determine the
etiology of the problem. The latter requires two kinds of data:
the differential diagnosis between organic and psychological
causes and an analysis of the psychological elements of the
problem.
Not all patients whose chief complaint is of a sexual nature
should undergo an immediate evaluation and assessment of
their sexual lives. Sometimes sexual problem is in fact a sign of
a serious mental disorder. Patients with psychosis, mania, and
borderline conflicts may present with sexual symptom. That is
why it is important to evaluate entire person when looking at
sexual issues. When a major psychiatric illness is suspected, it
is vital to address it before limiting attention to sexual issues.
An important early step in the evaluation of every sexual
complaint is to take a thorough drug and alcohol history.
Although alcohol is the most commonly abused substance that
interferes with sexual performance, most of the “street drugs”
(cocaine, heroin, amphetamines, sedatives) can have a
deleterious effect on sexual performance. Further, there are a
variety of legitimately prescribed medications that influence
sexual physiology.
Here are some of these medicaments (Table 1):
Conditions that suggest that a patient’s sexual disorder is
not substance related-even though the patient may be using a
potentially problematic drug-include symptoms whose onset
precedes the use of the drug, symptoms that persist over a
month after completely stopping use of the drug, and a prior
history of sexual dysfunction while not using the substance in
question.
Evaluation of sexual disorders
128
Table 1
Drug name
Paroxietine (Paxil)
Perphenazine (Trilafon)
Phenelzine (Nardil)
Prazosin (Minipress)
Propranolol (Inderal)
Protriptyline (Vivactil)
Ranitidine (Zantac)
Reserpine
Sertraline (Zoloft)
Spironolactone (Aldactone)
Sulfasalazine (Azulfidine)
Tamoxifen (Nolvadex)
Testosterone
Thiazide diuretics
Thioridazine
Thiothixene
Trazodone (Desyrel)
Potential effect
Decreased desire; delayed or no
orgasm
Decreased or no ejaculation
Impotence; retarded or no
ejaculation; delayed or no
orgasm; priapism
Impotence; priapism
Loss of desire; impotence
Loss of desire; impotence;
painful ejaculation
Loss of desire; impotence
Decreased desire; impotence;
decreased or no ejaculation
Decreased desire; retarded or no
orgasm
Decreased desire; impotence
Impotence
Priapism
Priapism
Impotence
Impotence; retrograde, painful,
or no ejaculation; priapism,
anorgasmia
Spontaneous ejaculations;
impotence; priapism
Priapism; clitoral priapism;
increased desire; retrograde or
no ejaculation; anorgasmia
The following lists of the main areas of inquiry in a sexual
evaluation cover all the bases.
Basic information
Nature and development of the sexual difficulty
Evaluation of sexual disorders
129
Emotional reaction to the problem
Understanding of its genesis
Attempts to resolve it
Psychiatric history
Previous illness, therapy, hospitalization
Previous psychological testing
Physical health
Medical history, illnesses, disabilities
Medicines taken
Drug and alcohol use
Motivation for treatment
History specific to couples
How they met, what attracted them to each other
Initial sexual experience together
Changes in the nature of their sexual experience, wanted
or unwanted, over the course of the relationship
Method of and satisfaction with birth control
What can not be talked about in the relationship
Sexual history
Family, cultural, religious background concerning sex
Early sex play, education
Discovery of arousal
Initial shared experiences, same and opposite sex
Abuse, sexual or physical
Adolescence
Dating
Sexual experiences: petting, mutual orgasm, intercourse
Body image, eating disorders
Masturbation
How often, how done
Fantasies
Other sexual partners
Before present relationship (if any)
During present relationship (if any)
Feelings about sex not already discussed
Evaluation of sexual disorders
130
Likes and dislikes
Wishes and fears
What is important about sex
Orgasm
Closeness
Verbal, nonverbal communication
Feelings about partner(s) not already discussed
Once the basic information has been gathered, it is time to
consider medical examination and psychological testing. A
medical examination should be done in the vast majority of
sexual dysfunction cases regardless of the general state of the
patient’s health. There are variety of medical conditions, from
diabetes to sickle-cell anemia, that can cause alteration of
sexual function, and it is only through a thorough medical
examination that some of them can be diagnosed. Medical
illness can influence each and every stage of sexual function.
One of most serious errors is to overlook a medical condition
that causes a sexual disorder. Not only would any psychological
treatment the patient receives be limited in its effect, but there
is also the possibility that an unrecognized illness would
progress and cause irreversible harm to the patient in a
situation where it could have been diagnosed and treated.
There are two important clues that would suggest that a
medical condition might be causally related to a sexual
dysfunction. First is a temporal association between the onset
or exacerbation of an illness and the appearance or
exacerbation of a sexual dysfunction. Second is an alteration in
sexual function that goes against usual physiological function,
as when a twenty-year-old man develops impotence without
any stressors that might argue for psychological etiology.
Some sexual disorders are more likely to be caused by
medical conditions than others. For example, pain with sexual
interaction is a symptom that especially requires a complete
physical examination. Vaginismus can also be related to variety
of physical abnormalities of the female genitourinary tract.
Withdrawal from alcohol or opioids is known to be related to
Evaluation of sexual disorders
131
the sudden appearance of premature ejaculation. Other sexual
disorders frequently associated with organic causes are
impotence, low or absent libido, secondary anorgasmia in
males and females, seconadary retarded ejaculation.
Illness and drugs must be carefully ruled out when evaluating
patients, especially those over the age of 40, with complaint
that carry a high risk of organicity.
If the symptom is clearly situational, psychogenecity is
established and, conversely, drugs and illness are ruled out as
causative factors.
Since sexual symptoms frequently result from interplay
between organic and psychological factors, an attempt must be
made to sort out the relative contributions of each. Organic
disease can occur in people with previous psychological
problems and their anxious response to even mild organic
deficiencies will complicate the clinical picture enormously.
Therefore, for the management and rehabilitation of patients
with organic or partial organic problems, the assessment of
psychological reactions is extremely important. The partners
responses and attitudes are of equal importance in determining
the ultimate clinical picture and must be carefully noted during
the evaluation.
Psychological testing is very helpful in the evaluation of
patients with sexual symptoms. This is particularly true for
those individuals with dual diagnoses, personality disorders,
potentially factitious disorders, and the paraphilias. The
personality structure of such patients is often complicated, and
it is consequently difficult to evaluate their capacity to engage
in therapy. Psychological testing can help sort out the degree
of psychopathology, the motivation to get better, and the
nature of hidden conflicts. Further, psych testing is useful with
those individuals who have difficulty communicating verbally
because of depression, shyness, or anxiety.
When making diagnosis of a sexual problem, it is
important to remember that notions of what is sexually
“normal” vary from culture to culture and family to family.
Socioeconomic, educational, and religious background strongly
Evaluation of sexual disorders
132
influence an individual’s notions of sexual deviance, standards
of performance, and gender role behavior. Sexual mores
change from generation to generation.
Sexual symptoms can appear in a variety of situations. As
we have already mentioned, sexual apathy and even anhedonia
(lack of any pleasurable feelings) can accompany severe
depression. Inappropriate sexual behavior can be seen in acute
manic episodes. When making a diagnosis of a sexual disorder,
you must first determine that the sexual symptoms are not
better accounted for as an aspect of another psychiatric
disorder. Furthermore, for a problem to classify as a
diagnosable sexual dysfunction it must cause marked distress
or interpersonal difficulty. Thus individual who tells you that he
is not at all interested in sex and is perfectly content with his
celibate, abstinent state, does not have a diagnosable disorder
of desire.
Formal DSM diagnoses are only the first step in
understanding the nature of a problem. An understanding of
patients with sexual difficulties should include a formulation of
the psychodynamics of each individual and a description of the
nature of the relationship between the partners. We must try to
understand not only how the disorder got to be the way it is
but also what function it serves in the psychic and
interpersonal economy of the patient, what other conflicts and
problems trouble the patient, and the ways in which the patient
habitually solves or fails to solve problems both in the inner
and the outer worlds.
Male infertility
Causes of male infertility are divided into three main
groups:
1. Pre-testicular
2. Testicular
3. Post-testicular
1. Pre-testicular – disorders of hypothalamuses and hypophysis
(congenital or occurred): Hypogonadotropic hypogonadism,
prolactinome, isolated deficiency of FSH, isolated deficiency of
Evaluation of sexual disorders
133
LH etc. This disorders result in impairment of spermatogenesis
regulation.
2. Testicular - two types are distinguished:
a) Chromosomal (Kline Felter syndrome Noonan syndrome,
digenesis of gonads, y-chromosome mycrodeletion syndrome)
b) No chromosomal (varicocele, hydrocele, cryptorchysm,
trauma of testis, orchitis, Sertoli-cell-only syndrome,
chemiotherapy, radiotherapy). These disorders result in the
impairment of spermatozoa production.
3. Post-testicular
common
disorders,
urinogenital
inflammatory processes, being passed on from infections (STI)
and immunological impairments. These disorders lead to
disturbance of motility of spermatozoa and seminal duct
opturation.
Treatment of sexual disorders
134
Chapter 9
Treatment of sexual disorders
Treatment of sexual disorders should be directed to their
causes, including deep seated sexual conflicts developed during
psychosexual development. It is necessary to take into account
that sexual inferiority affects the psyche of person, and vicious
circle is formed which deepens the pathological process.
Interpersonal relations between sexual partners worsen and
conflict situations become more frequent.
All this proves that the psychotherapy plays a central role
in correction of sexual disorders. If necessary psychotherapy
combines with other forms of treatment: pharmacotherapy,
physiotherapy. The important part of treatment is the
elimination of bad habits: alcohol abuse, smoking, formation of
a normal dietary ration, normalization of sleep. It is desirable
to distract patient’s compulsive thoughts about own sexual
inferiority towards other essential interests, mental and
physical job.
Psychotherapy of sexual disorders
Following forms of psychotherapy are common in treating
sexual dysfunctions:
1. Hypnosis
The purpose of the hypnosis is to expose the patient to
conforming suggestion during a hypnotic sleep.
2. Adlerian therapy
Adlerian Therapy is a growth model. It stresses a positive
view of human nature and that we are in control of our own
fate and not a victim to it. We start at an early age in creating
our own unique style of life and that style stays relatively
constant through the remained of our life. We are motivated by
Treatment of sexual disorders
135
our setting of goals; how we deal with the tasks we face in
life, and our social interest. The therapist will gather as much
family history as he could. He will get an idea of the clients'
past performance. These data will be used in setting goals for
the client. This will help make certain the goal is not to low or
high, and that the client has the means to reach it. The goal of
Adlerian therapy is to challenge and encourage the clients'
premises and goals. To encourage goals that are useful
socially, and to help them feel equal. These goals include any
component of life, parenting skills, marital skills, ending
substance-abuse, and most anything else. The therapist will
focus on and examine the clients' lifestyle and the therapist will
try to form a mutual respect and trust for each other. They will
then mutually set goals and the therapist will provided
encouragement to the client in reaching their goals. The
therapist may also assign homework, setup contracts between
them and the client, and make suggestions on how the client
can reach their goals.
3. Behavior therapy
Behavior therapy is always undergoing refinement and
uses learning to overcome specific behavioral problems. In this
type of therapy it is believed that behaviors are learned, that
we are a product of our environment. Focus will be on present
and overt behavior. In this type of therapy it is believed that
reinforcement and imitation teaches normal behavior and that
abnormal behavior is a direct result of defective learning.
Therapy will be based on learning theory. The therapy will
include a treatment plan, the goals of the treatment will be laid
out up front, and the outcome expected from the therapy will
be set right up front too. To eliminate unwanted behaviors you
need to learn new behaviors. This may include assertion,
behavioral
rehearsal, coaching,
cognitive
restructuring,
desensitization,
modeling,
reinforcement,
relaxation
methods, self-management, or new social skills. Both client
and therapist need to take an active role in learning the more
desired behavior.
Treatment of sexual disorders
136
4. Existential therapy
Focuses on freedom of choice in shaping one's own
life. Teaches one is responsible to shape his / her own life and
a need for self-determination and self-awareness. The
uniqueness of each individual forms his / her own unique
personality, starting from infancy. Existential therapy focuses
on the present and on the future. The therapist try's to help
the client see they are free and to see the possibilities for their
future. They will challenge the client to recognize that he / she
themselves were responsible for the events in their life. This
type of therapy is well suited in helping the client to make good
choices or in dealing with life.
5. Gestalt therapy
Gestalt therapy integrates the body and mind factors, by
stressing awareness and integration. Integration of behaving,
feelings, and thinking is the main goal in Gestalt therapy.
Client's are viewed as having the ability to recognize how
earlier life influences may have changed their life's. The client
is made aware of personal responsibility, how to avoid
problems, to finish unfinished matters, to experience thing in a
positive light, and in the awareness of now. It is up to the
therapist to help lead the client to awareness of moment by
moment experiencing of life. Then to challenge the client to
accept the responsibility of taking care of themselves rather
then excepting others to do it. The therapist may use
confrontation, dream analysis, dialogue with polarities, or role
playing to reach their goals. This may include treatment of
crisis intervention, marital / family therapy, problem in
children's behavior, psychosomatic disorders, or the training of
mental health professionals.
6. Person-centered therapy
Person-centered therapy gives more responsibility to the
client in their own treatment and views humans in a positive
manner. Founded by Carl Rogers in the 1940's. Rogers had
Treatment of sexual disorders
137
great faith that we could and would work out our own
problems. The therapist will move the client towards self
awareness, helping the client to experience previously denied
feelings. They will teach the client to trust in themselves and to
use this trust to find their direction in life. The person-centered
therapist makes the client aware of their problems and then
guilds them to a means of resolve them. The therapist and
client must have faith that the client can and will find selfdirection. The therapy focus on the here and how. They
motivate the client in experiencing and expressing feelings. The
person-centered therapist believes that good mental health is a
balance between the ideal self and real self. This is where the
problem lies, the result of difference between what we are and
what we wish to be causes maladjusted behavior.
7. Psychoanalytic therapy
Psychotherapy focuses on the unconscious and believes it
influences human behavior. It is believed that a person is
driven by aggressive and sexual impulses. It focuses mainly on
the first six years of human life and how the events of this time
period determine later personality. Repressed conflicts from
childhood lead to personality problems later in life. Anxiety is a
direct result of the repression of conflicts. Psychotherapist
believes that the unconscious motives along with unresolved
conflicts lead to maladapted behavior. They believe that to
develop a normal personality, a person successful go through
five psychosexual stages:
Oral - Birth to 1 year: Sucking.
Anal - 1 to 3 years: Holding and releasing urine and
feces.
Phallic - 3 to 6 years: Pleasure in genital stimulation.
Latency - 6 to 11 years: Sexual instincts develop.
Genital - Adolescence: Sexual impulses return.
Inadequate resolution of any of these stages leads to
flawed personality development. The client with the therapist
help will make repressed conflicts conscious, making the
Treatment of sexual disorders
138
unconscious conscious. Making these conflicts conscious to the
client will help them in working through them, awareness.
Psychotherapy is not useful in clients that are selfcentered, impulsive, or severely psychotic. The therapist should
have extensive training and expense. The therapist when
working with minorities should focus on the client’s family
dynamics. Treatment will be long term.
8. Rational-emotive and Cognitive-behavioral
Therapy
Rational-emotive therapy is a highly action-oriented and
deals with the client's cognitive and moral state. This therapy
stresses the client’s ability of thinking on their own and in their
ability to change. The rational-emotive therapist believes that
we are born with the ability of rational thinking but that my fall
victim to irrational thinking. They stress the clients ability to
think, in making good judgments, and in taking action. The
therapist will use directed therapy. The therapist believes that
a neurosis is a result of irrational behavior and irrational
thinking. The
Rational-emotive
and
Cognitive-behavioral
therapist believe the clients problems are rooted in childhood
and in their belief system, that was formed in childhood.
Therapy will include method is solving and dealing with
emotional or behavior problems. The therapist will help the
client to eliminate any self-defeating outlooks they may have
and to view life in a rational way. The therapist will never have
a personal relationship with the client. The therapist will think
of the client as a student and themselves as the teacher.
Male reproductive function Access
Throughout spermatogenesis multiplication, maturation
and differentiation of germ cells results in the formation of the
male gamete. The understanding of spermatogenesis needs
detailed information about the organization of the germinal
epithelium, the structure and function of different types of
germ cells, endocrine and paracrine cells and mechanisms,
Treatment of sexual disorders
intratesticular
and
spermatogenesis.
139
extratesticular
regulation
of
Introduction
Starting from a self-renewing stem cell pool, male germ
cells develop in the seminiferous tubules of the testes
throughout life from puberty to old age. The complete process
of germ cell development is called spermatogenesis. The
products of spermatogenesis are the mature male gametes,
namely the spermatozoa. Spermatogenesis depends on
intratesticular
and
extratesticular
hormonal
regulatory
processes and functions of the intertubular microvasculature,
the Leydig cells and other cellular components of the
intertubular space.
Organization of the testis
The human testes are two organs of the shape of
rotation ellipsoids with diameters of 2.5 × 4 cm engulfed by a
capsule (tunica albuginea) of strong connective tissue. Thin
septula testis divide the parenchyma of the testis in about 370
conical lobules. The lobules consist of the seminiferous tubules
and intertubular tissue, containing groups of endocrine Leydig
cells and additional cellular elements. The seminiferous tubules
are coiled loops . Their both ends open into the spaces of the
rete testis . The fluid secreted by the seminiferous tubules is
collected in the rete testis and delivered to the excurrent ductal
system of the epididymis.
Structure of the seminiferous tubule
The seminiferous tubule consists of the germinal
epithelium and the peritubular tissue.The germinal epithelium
consists of cells that include different developmental stages of
germ cells, namely spermatogonia, primary and secondary
spermatocytes and spermatids. These are located within
invaginations of Sertoli cells. The prismatic Sertoli cells are
connected by specialized zones of tight junctions of cellular
membranes separating the germinal epithelium . Sertoli cells,
Treatment of sexual disorders
140
investigated in histological sections, exhibit increasing amounts
of lipid droplets in correlation to advanced age being an
indicator of the "biological clock" of the testis.
Further functions are attributed to Sertoli cells: 1.
Sustentacular and nutritive functions for the germ cells. 2.
Organization of the delivery of mature spermatids into the
tubular lumen (spermiation). 3. Production of endocrine and
paracrine substances for the regulation of spermatogenesis. 4.
Secretion of androgen binding protein (ABP) for the
maintenance of epithelia of the excurrent duct system. 5.
Interaction with the intertubular endocrine Leydig cells.
Spermatogenesis
Spermatogenesis is the process by which a complex,
interdependent population of germ cells produces spermatozoa.
Spermatogenesis begins at puberty after a long preparatory
period of "prespermatogenesis" in the fetus and the infant.
Three major stages can be distinguished:
spermatogoniogenesis, maturation of spermatocytes
and spermiogenesis, which is the cytodifferentiation of
spermatids.
Spermatogonia multiplicate continuously in successive
Mitoses in to spermatocyt. Spermatocytes divide in meiosis to
spermatids. Mature spermatids are released from the serminal
epithelium and the free cells are called spermatozoa. The
delivery of mature spermatids from the germinal epithelium is
managed by the Sertoli cells .
Components of the intertubular space
The intertubular space of the human testis contains the
microvasculature, the endocrine Leydig cells, nerve fibres,
macrophages, fibroblasts, further connective tissue cells and
lymph vessels.
Leydig cellsare prominent cells of the intertubular
space. They constitute groups surrounding the capillaries.
Leydig cells produce and secrete among others androgens, the
male sex hormone, the most well known of which is
Treatment of sexual disorders
141
testosterone. Testosterone activates the hypophyseal-testicular
axis, the masculinization of the brain and sexual behaviuor, the
initiation, processing and maintenance of spermatogenesis, the
differentiation of the male genital organs and secondary sex
characteristics.
Recent investigations elucidated that the Leydig cells
possess neuroendocrine properties in addition to their
endocrine functions. There is evidence that Leydig cells express
serotonin, different antigens characteristic for nerve cells as
well as neurohormones, neuropeptides and numerous growth
factors and their receptors.
Kinetics of spermatogenesis
Spermatogenesis commences during puberty and
continues throughout life and until old age because of the
inexhaustible stem cell reservoir. An abundance of germ cells
are developed and delivered from the seminiferous tubules.
The process of spermatogenesis is highly organized:
Spermatogonia divide continuously, in part remaining
spermatogonia, in part giving rise to spermatogenesis.
Originating from dividing spermatogonia, cell groups migrate
from the basal to the adluminal position of the germinal
epithelium. Cell groups of different development are met in a
section of a seminiferous tubule and contribute to the typical
aspect of the germinal epithelium. Six of these typical aspects
were described in the human testis as "stages of
spermatogenesis".
The development of an A type spermatogonium up to
mature spermatids requires 4,6 cycles, e.g. 74 days. The
mature spermatids delivered from the germinal epithelium as
spermatozoa are transported through the epididymal duct
system during additional 12 days. Therefore, 86 days at the
minimum must be calculated for a complete spermatogenetic
cycle from spermatogonium to mature spermatozoa.
Spermatozoa with their unique shape are suitable for
the transport to the female gamete. For this reason the nucleus
of the spermatozoon is condensed, covered by an acrosome for
Treatment of sexual disorders
142
establishing contact to the female gamete and connected with
a flagellum for progressive motility.
The diameter of the head of spermatozoon is 4–5 μm,
the diameter of the flagellum is of 1–2 μm and the length of
the spermatozoon measures 60 μm. Spermatozoa acquire their
competence of motility during the transport throughout the
epididymal ducts. Only 25% of the germ cells reach the
ejaculate and more than half of them are malformed.
Therefore, only 12% of the spermatogenetic potential is
available for reproduction.
Regulation of spermatogenesis
The process of spermatogenesis in the seminiferous
tubules is maintained by different internal and external
influences. The Leydig cells in the intertubular space secrete
testosterone and additional neuroendocrine substances and
growth factors. These hormones, transmitters and growth
factors are directed to neighbouring Leydig cells, to blood
vessels, to the lamina propria of the seminiferous tubules and
to Sertoli cells. They are involved in maintenance of the trophic
of Sertoli cells and the cells of peritubular tissue; they influence
the contractility of myofibroblasts and in that way regulate the
peristaltic movements of seminiferous tubules and the
transport of spermatozoa. They also contribute to the
regulation of blood flow in the intertubular microvasculature.
The local regulation of spermatogenesis in the testis requires
the well known extratesticular stimuli provided by the
hypothalamus
and
hypophysis.
Pulsatile
secretion
of
gonadotropin releasing hormone (GnRH) of the hypothalamus
initiates the release of luteinizing hormone (LH) of the
hypophysis. As a result of this stimulus Leydig cells produce
testosterone. Testosterone influences not only spermatogenesis
in the seminiferous tubules of the testis but is also distributed
throughout the body and provides feedback to the hypophysis
related to the secretory activity of Leydig cells. Stimulation of
Sertoli cells by the pituitary follicle stimulating hormone (FSH)
Treatment of sexual disorders
143
is necessary for the maturation of germ cells. The Sertoli cells
itself
Secrete inhibin in the feedback mechanism directed to
the hypophysis. The extratesticular influences are a necessary
basis for the function of intratesticular regulations.
Disturbances of spermatogenesis
Proliferation and differentiation of the male germ cells
and the intratesticular and extratesticular mechanisms of
regulation of spermatogenesis can be disturbed at every level.
This may occur as a result of environmental influences or may
be due to diseases that directly or indirectly affect
spermatogenesis. In addition, different nutrive substances,
therapeutics, drugs, hormones and their metabolites, different
toxic substances or x-radiation may reduce or destroy
spermatogenesis. Finally, also a rather simple noxe as
increased temperature reduces the spermatogenetic activity of
the testis. Under these negative influences the testis answer
rather monotonuous by reduction of spermatogenesis. This
may be expressed in the reduced number of mature
spermatids,
in
malformation
of
spermatids,
missing
spermiation, disturbance of meiosis, arrest of spermatogenesis
at the stage of primary spermatocytes, reduced multiplication
or apoptosis of spermatogonia. If spermatogonia survive then
spermatogenesis may be rescued. Otherwise spermatogenesis
ceases and shadows of seminiferous tubules remain.
9. Transactional Analysis
Transactional analysis focus on the clients cognitive and
behavior functioning. The therapist helps the client evaluate
their past decisions and how those decisions affect their
present life. They believe self-defeating behavior and feelings
can be overcome by an awareness of them.The therapist
believes that the clients personality is made up of the parent,
adult, and child. They believe that it is important for the client
Treatment of sexual disorders
144
to examine past decisions to help their make new and better
decisions.
10. Sex therapy
The sex-therapy combines methods of behavioral
psychotherapy, psychodynamic analysis and interpersonal
attitudes.
Pharmacological therapy of sexual
disorders
Pharmacotherapy has a large appliance in treatment of
sexual disorders both in men and in female. CNS stimulators,
psychotropic drugs, biogenic stimulators, prostaglandins,
vitamin therapy, immunomodulators, local anesthetics,
hormonal preparations such as gonadotropins, androgens and
their synthetic analogues, anabolic steroids and specialized
sexological drugs are used. The choice of medicine at sexual
disorders is linked to the cause of disease, its duration, age of
the patient, presence of concomitant somatic or psychic
diseases, etc. According to this all medicinal treatment can be
etiological, pathogenetic or somatic.
In the treatment of sexual disorders sanatorium-and-spa
treatment plays the great role. The physiotherapeutic
treatment:
the
electrophototherapy,
taking
baths,
fangotherapy, therapeutic massage, exercise therapy have
salutary effect on organism particularly on the nervous, psychic
and sexual systems. Acupuncture is also efficient.
It is wrong to neglect methods of non-traditional medicine.
Erectorotherapy is used in erectile dysfunction (outer
prothetics), therapy by local negative pressure are often used.
In the case of ineffective conservative therapy of an erection’s
disorder resort to surgical methods which, as a rule, have three
directions:
1. Revascularization of cavernous bodies of the penis,
2. Decrease of venous flow of cavernous bodies
Treatment of sexual disorders
145
3. Endoprosthesis
replacement
of
the
penis
(endofaloprosthesis):
The results of treatment of sexual disorders are
satisfactory in the case when the complex of regulating and
therapeutic methods is used including also the partner.
Tests
146
Tests
1. The stage of sexual libido defined as
a) forming sexual identity
b) striving for being in the focus attention
c) striving for erotic contacts such as hugging and kissing
d) forming sexual fantasies enhance with sexual intercourse scenes
2. Criteria of definition males’ sexual constitution is without
a) index of trochanter
b) maximal excesses
c) the age of first masturbation
d) becoming pubic hairy
e) the age of first ejaculation
3. The type of Obsessive-Compulsive masturbation define as
a) obsessive character
b) beginning before arising sexual libido
c) beginning after the period of mature sexuality
d) manipulations on sexual organs which arise erection
4. Sort out three methodological approaches of sexology by order of priority
a) monodisciplinary
b) multidisciplinary
c) interdisciplinary
a) a,b,c
b) c,a,b
c) c,b,a
5. Particularity of sexual organs’ blood vessels
a) one a. dorsales penis is accompanied by two vv. dorsales penis
b) one v. dorsales penis is accompanied by two aa. dorsales penis
c) small smooth structures (pollsters) located only on the penile vessels
walls
6. The main male desire’s hormone is
a) prolactine
b) estrogens
c) testosterone
d) thyroxine
Tests
7. Which is typical for dispareunia
a) sensation of itching
b) sensation of burning
c) recurrent and persistent pain feeling during sexual intercourse
d) spasm of the musculature of the outer third of the vagina
e) insufficient lubrication
8. Contractions of the striated muscles are
a) 0.8 per second
b) 0.6 per second
c) 0.3 per second
9. The organic causes of erection dysfunction are without
a) diabetes Mellitus
b) hypogonadismus
c) alcohol polineuropathia
d) asthenisation
10. Which of followed disorders can’t be cause of retrograde ejaculation
a) diabetes Mellitus
b) the state after prostatectomy
c) mental disorders
11. The brain center’s of ejaculation are
a) frontals lobes
b) temporally lobes
c) paracentral lobes
12. Ejaculation before emission called
a) ejaculation preccox
b) ejaculation ante portas
c) ejaculation tarda
13. When is chlorethile blockade using
a) retrograde ejaculation
b) premature ejaculation
c) syndrome of unejaculation
147
Tests
14. Man who exposes his genitals to a strangers called
a) voyeurism
b) exhitionism
c) fetishism
15. What is the fetishism
a) preference for sexual activity with animals
b) preference for nonliving objects of opposite sex
c) a man who wears opposite sex’s clothes
d) man who exposes his genitals to a strangers
e) preference for repetitive sexual activity with prepubertal children
16. The age of menstrual cycle of the middle constitutions’ women
a) before 11 year
b) 12-14 years
c) 14-16 years
d) 16-18 years
17. What is the oligozoospermia
a) absence of spermatozoa
b) akinesia of spermatozoa
c) high level of degenerative spermatozoa
d) hypokinesia of spermatozoa
e) low concentration
18. Transsexualism is
a) inhibition of sexual desire
b) disorder of sexual orientation
c) disorder of sexual identity
d) transformation of socialization in sex roles
19. Sort out sexual response cycles’ phases by order of priority
a) plateau
b) excitement
c) orgasm
d) resolution
a) a,c,b,d b) a,b,c,d c) b,a,c,d
148
Tests
20. During the lubrication:
a) the vaginal walls begin a sweating like process transudation
b) turns the vagina from its normal pink color to red
c) develops orgasmic platform
d) occurs rhythmic contraction
a) a,b,c
b) a,b
c) a,d
d) b,d
21. The stage of platonic libido is characterized
a) forming sexual identity
b) striving for being in the focus attention
c) striving for erotic contacts such as hugging and kissing
d) forming sexual fantasies enhance with sexual intercourse scenes
22. According to the progress Female orgasm is without
a) transitory
b) delayed
c) clitoral
23. Involuntary election is:
a) developing immediately during sexual organ's stimulation
b) developing within sleep
c) morning erection
d) developing immediately during sexual organ's stimulation with
participation of brain centers
a) a,b,c,d b) b,c,d
c) b,c
24. Emission consists of the reflex contraction of
a) prostate glands and tubuli epididymides
b) vas deferens and the seminal vesicles
c) small pelvic muscles
25. At the period of puberty is the formation of
a) socialization in sex roles
b) psychosexual orientation
c) sexual life with its excesses and abstinences
d) sexual identity
e) physiologic rhythm called conditional physiologic rhythm (CPR)
149
Tests
150
26. The stage of sexual orientation forming takes place
a) in puberty
b) in the period of mature sexuality
c) in Prepuberty
d) in Transitional period to mature sexuality
27. Psychogenically caused erectile dysfunction is
a) anxiety
b) spinal cord-trauma
c) depression
d) unconscious sexual conflict
a) a,b
b) a,c,d
c) b,c,d
d) a,b,c
28. The criteria of female sexual constitution are the following besides
a) the age of first menstruation
b) trochanter index
c) pubic hair
d) the age of first sexual intercourse
e) the age of forming erotic libido
29. Exhibicionism is
a) touching or rubbing against a nonconsenting person
b) usе of nonliving objects for sexual gratification
c) expose of one's genitals to an unsuspecting stranger
d) sexual arousal at watching an unsuspecting person who is naked or
having sex.
30. The lower level of spermatozoa in sperm is
a) 100million/ml
b) 50million/ml
c) 20 million /ml
d) 80 million /ml
31. The criteria of transsexualism are the following besides
a) the desire to live and be accepted as a member of opposite sex, usually
accompanied by the wish to make his or her body as congruent as
possible with the preferred sex
Tests
151
b) the transsexual identity has been present persistently for at least two
years
c) the disorder is not a symptom of another mental disorder
d) expose of one's genitals to an unsuspecting stranger
32. Organically caused erectile dysfunction is following besides
a) the brain-strokes, trauma, dementia
b) anxiety
c) spinal cord-trauma
d) arteries-arteriosclerosis, diabetes
e) hyperprolactinemia
33. At the period of prepuberty is the formation of
a) sexual identity
b) socialization in sex roles
c) sexual orientation
34. At the period of puberty masturbation called
a) obsessive
b) masturbation due to frustration
c) vicarial masturbation
d) masturbation is determined by hypersexual period
35. Transvestic Fetishism is
a) heterosexual male aroused by cross dressing
b) expose of one's genitals to an unsuspecting stranger
c) us of nonliving objects for sexual gratification
d) sexual arousal at watching an unsuspecting person who is naked or
having sex
36. The following group of medication can be cause of erectile dysfunction
besides
a) neuroleptic medication
b) sedative medication
c) antihypertensive medication
d) antibacterial medication
Tests
37.
a)
b)
c)
d)
152
Sexual pain disorders are
dyspareunia
premature ejaculation
erectile dysfunction
vaginismus
a) a,b
b) a,d
c) b,c
d) c,d
38. Criteria for female sexual arousal disorder according to DSM-IV are
following besides
a) persistent or recurrent inability to attain, or to maintain adequate
lubrication-swelling
b) the disturbance cause marked distress or interpersonal difficulty
c) deficiency or absence of sexual fantasies and desire for sexual activity
d) it is not caused by a general medical condition
39. The vaginismus is
a) ejaculation, immediately after coitus
b) recurrent and persistent involuntary spasm of the musculature of the
outer third of the vagina that interferes with coitus
c) recurrent genital pain with sexual intercourse in a man or a woman
40. Teratospermia is
a) absence of spermatozoa
b) akinesia of spermatozoa
c) high level of degenerative spermatozoa
d) low concentration of spermatozoa
41. The main manifestations of male sexuality are the following besides
a) libido
b) erection
c) erogenous reactivity
d) ejaculation
e) orgasm
42. The main manifestations of female sexuality are the following besides
a) libido
b) erogenous reactivity
c) lubrication
Tests
d) orgiastic platform
e) orgasm
a) d
b) c,d
153
c) a,b
d) d
43. Sexual manifestations according to age differences
a) Prepuberty
1) sexual orientation
b) Puberty
2) excesses
c) Transitional period
3) socialization in sex roles
d) Mature sexuality
4) CPR
44. Spinal center of erection
a) Th2-th4
b) L2-L4
c) S2-S4
d) Th12-L4
45. Spinal center of ejaculation
a) L1-L3
b) L4-L5
c) Th1-Th2
d) Th11-L5
46. The vesicular mechanism of the erection
a) increasing penile flow
b) decreasing penile outflow
c) contraction of small smooth structures located only on the penile blood
vessels walls
a) a,c
b) b,c
c) a,b,c
d) c
47. The libido is:
a) The penis distends and becomes rigid
b) Specific sensations which move the individual to seek out sexual
experiences
c) Emissia of sperma
48. Female sexual desire's hormone is
a) prolactine
b) estrogen
c) testosterone
d) thiroxin
Tests
154
49. What is the ejaculation ante portas
a) becomes after 20 friction
b) more than 20 friction, but before partner having orgasm
c) less than 50 friction
d) before introitus
e) before 5 min
a) b,e
b) a
c) c
d) e
50. Forming genetical sex
a) 7-10 weeks of embryonal period
b) 10-12 weeks of embryonal period
c) conception
d) puberty
e) 12-20 weeks of embryional period
51. The male of middle constitution has the first ejaculation
a) before 10 year
b) 11-13 years
c) 13-15 years
d) 15-17 years
e) above 18 year
52. The female orgasmic manifestation is
a) erogenous reactivity
b) ejaculation
c) lubrication
d) libido
a) b
b) d
c) no one d) c
53. During orgasm
a) female Orgasmic contraction is longer (20-30 sec) than male's
b) some females are capable of multiple orgasm without refractor period
c) force of the contraction is diminished
d) male orgasmic contraction is longer (20-30 sec) than female's
e) force of the contraction is increased
a) a,b,c,d,e b) a,b,c
c) a,b,e
d) b,c,d
54. Bartholin' s glands are located
a) major vulvar lipes
Tests
155
b) minor vulvar lipes
c) urinary
d) vagina
55. Orgasm is
a) the climax of pleasurable sensations
b) the penis distends and becomes rigid
c) specific sensations which move the individual to seek out sexual
experiences
d) emissia of sperma
56. Parapuberty is characterized
a) socialization in sex roles
b) forming psychosexual orientation
c) first sexual intercourse, with excesses and abstinences
d) forming sexual identity
e) forming certain physiologic rhythm (CPR)
57. Vicarial masturbation is characterized
a) obsessive
b) premature onset, before arising sexual libido
c) later onset, at the transitional period to mature sexuality
d) after onset libido, during puberty
e) activity on sexual organs which accompanied with erection
58. The stage of puberty is characterized
a) forming psychosexual orientation
b) forming sexual identity
c) socialization in sex roles
59. The transitional period to mature sexuality is characterized the following
besides
a) sexual excesses
b) socialization in sex roles
c) sexual abstinences
d) the realization of the sexual libido
60. The erectile response is primarily
a) parasympathetic one
b) sympathetic one
Tests
156
Keys
1. d
11. c
21. b
31. d
41. c
49. d
59. b
2. d
12. b
22. c
32. b
42. d
50. c
60. a
3. a
4. a 5. b
13. b 14. b 15. c
23. c 24. b 25. b
33. b 34. d 35. c
43. a-3, b-1, c-2, d-4
51. c 52. c 53. b
6. c
16. b
26. a
36. d
44. c
54. a
7. c
17. e
27. b
37. b
45. d
55. a
8. a
18. c
28. d
38. d
46. c
56. d
9. d
19. c
29. c
39. b
47. b
57. c
10. c
20. a
30. c
40. c
48. c
58. a
References
157
References
1. Հ ակ ո բ յ ան Ա.Է ., Նե ր ս ի ս յ ան Ն.Ռ., «Կլ ի ն ի կ ակ ան
Սե ք ս ո լ ո գ ի ա», Եր և ան 2006
2. Васильченко Г.С., “Общая сексопатология” Руководство
для врачей, Москва: Медицина 2005
3. Васильченко Г.С. “Сексология. Справочник”, Москва:
Медицина 1990
4. Гери Ф. Келли, “Основы современной сексологии”, СaнктПетербург 2002
5. Кратохвил С., “Психотерапия семейно-сексуальных
дисгармоний’, Москва: Медицина 1991
6. Кон И.С., “Сексология”, Москва: Академия 2004
7. Кришталь В.В., Григорян С.Р., “Сексология”, Москва: ПерСе
2002
8. Masters William H., Virginia E. Johnson and Robert C.
Kolodny, “Human Sexuality”, New York: HarperCollins 1998
9. Kaplan H.S., “The new sex therapy”, New York: Quadrangle
1995
10. John H. Harvey, Amy Wenzel, Susan Sprecher, “The
Handbook of Sexuality in Close Relationships”, Place of
Publication: Mahwah, NJ 2004
11. Bergin A.E., & Garfield S.L., “Handbook of psychotherapy and
behavior change”, New York 1994
12. Myra J., “Hard Sex”, Gender and Science Department of
sociology: Kingston, Ontario, Canada 2004
13. Alcira Mariam Alizade, “Feminine Sensuality”, London 1999
14. Janice W. Lee, “Gender Roles”, New York 2005
15. Tony Ward, D. Richard Laws, Stephen M. Hundson,
“Thousand”, Oaks-London-New Delhi 2003
16. Judith Halberstam, “Female Masculinity”, London 1998.