* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 5HT - wmshp
Sexual dysfunction wikipedia , lookup
Anxiety disorder wikipedia , lookup
Bipolar II disorder wikipedia , lookup
Selective mutism wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
Antipsychotic wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Postpartum depression wikipedia , lookup
Behavioral theories of depression wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Major depressive disorder wikipedia , lookup
Biology of depression wikipedia , lookup
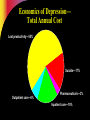
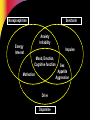
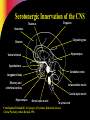
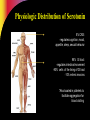
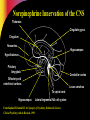
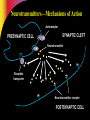
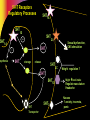
Pharmacotherapy of Depression Jerry Overman, Pharm.D., BCPP Clinical Pharmacy Specialist, Mental Health (NIMH) NIH Clinical Center Pharmacy Department WMSHP and DC-CCP Spring Meeting May 10, 2014 9:00 AM Jerry Overman, Pharm.D., BCPP – has no financial interest or relationships to disclose Objectives Define major depressive disorder and list the core symptoms of the illness Identify the various mechanisms and theories proposed for the pathogenesis of depression List the medication classes used to treat depression Discuss the pharmacology of the various classes of antidepressants and how these mechanisms relate to both efficacy and tolerability Epidemiology of Depression Lifetime prevalence of a major depressive episode: 17% – Male: 13% – Female: 21% Trends – Age at onset: Younger – Incidence: Increasing Weissman MM, et al. JAMA. 2011;276:293-299. Depression and Suicide Up to 15% of patients with major depressive disorder requiring hospitalization commit suicide Depression Guideline Panel. AHCPR publication 93-0550. Additional Risk Factors for Suicide Hopelessness Male gender White race Advanced age History of attempts Medical illnesses Substance abuse (self or family) Psychotic symptoms Living alone Insomnia Anxiety Depression Guideline Panel. AHCPR publication 93-0550. Suicides/100,000 person-years Pharmacotherapy Reduces Risk of Suicide 300 250 259 Treated Untreated 200 150 141 100 50 0 Isacsson G, et al. J Affect Disord. 1996;41:1-8. DSM-5 Criteria for Major Depressive Episode ≥5 symptoms present during same 2– week period Change from previous functioning Functional impairment and/or distress Symptoms not due to another cause DSM-5. Washington, DC: American Psychiatric Association. 2013. DSM-5 Criteria for Major Depressive Episode 5 Symptoms in the same 2-week period Sleep: Insomnia or hypersomnia Interest: Anhedonia - loss of interest or pleasure Guilt: Feelings of worthlessness Energy: Fatigue Concentration: Diminished ability to think or make decisions Appetite: Weight change Psychomotor: Psychomotor retardation or agitation Suicide: Recurrent thoughts of death * Must include 1 of these DSM-5. Washington, DC: American Psychiatric Association. 2013. Common Presenting Somatic Complaints “Tired all the time”, “blahs” Headache, Pain Malaise Vague abdominal or joint pains Disturbed sleep Sexual or relationship problems DSM-5. Washington, DC: American Psychiatric Association. 2014. Psychological Symptoms Hopelessness Low self esteem Denial, discounting, or explaining away stigmatized feelings Impaired memory, difficulty concentrating DSM-5. Washington, DC: American Psychiatric Association. 2013. Depression Guideline Panel. AHCPR publication 93-0550. Continuum of Depression and Anxiety Major depressive disorder Comorbid depression and anxiety Anxiety disorders Outcomes of Treatments of Major Depressive Disorder Dropout Nonresponse/response w/residual symptoms Response – Incomplete remission – Complete remission Recovery Acute Recovery in Major Depression HAM-D score 7 Patient asymptomatic – No longer meets criteria for depression – Minimal or no symptoms Psychosocial and occupational functioning restored Rush AJ, et al. Psychiatr Ann. 1995;25:704. Consequences of Failing to Achieve Recovery Greater risk of relapse Continued psychosocial limitations Continued impairments at work Worsens prognosis of other medical disorders Increased utilization of medical services Sustained elevation of suicide and substance abuse risks Response and Remission Remission Relapse Increased severity Euthymia Symptoms Recurrence Relapse Response Syndrome Treatment Phases Acute (6–12 wk) Time Kupfer DJ. J Clin Psychiatry. 1991;52(suppl 5):28-34. Continuation Maintenance (4–9 mo) (1 yr) Economics of Depression— Total Annual Cost Lost productivity—55% Suicide—17% Outpatient care—6% Pharmaceuticals—3% Inpatient care—19% Profile of the Ideal Antidepressant Rapid Onset of Action Once Daily Dosing Activity in a Range of Disorders Cost Effective Ideal Antidepressant Safety in Overdose No Drug Interaction Minimal Side Effects New Mechanisms Various effects on: – Serotonin (5HT) – Dopamine (DA) – Norepinephrine (NE) – Gamma amino butyric acid (GABA) – NMDA Glutamate (N-Methyl-D Aspartate) Tachykinins – NK1, NK2, NK3 Corticotropin releasing factor Glucocorticoid receptor antagonists Neuropeptide Y Brain Derived Neurotrophic Factor (BDNF) Cannabinoid receptors Ascending Aminergic System Cortex Selective manipulation of these aminergic transmitters has been the common denominator for all currently marketed antidepressants These same systems are implicated in anxiety DA Midbrain NE 5-HT Brain Stem Serotonin Norepinephrine Anxiety Irritability Energy Interest Impulse Mood, Emotion, Cognitive function Sex Appetite Aggression Motivation Drive Dopamine Serotonergic Innervation of the CNS Thalamus Cingulum Neocortex Cingulate gyrus Striatum Hippocampus Ventral striatum Hypothalamus Cerebellar cortex Amygdaloid body Olfactory and entorhinal cortices Intracerebellar nuclei Caudal raphe nuclei Hippocampus Dorsal raphe nuclei To spinal cord From Kaplan HI, Sadok BJ. In: Synopsis of Psychiatry, Behavioral Sciences, Clinical Psychiatry, 6th ed. Revised. 1991. Physiologic Distribution of Serotonin 5% CNS: -regulates cognition, mood, appetite, sleep, sexual behavior 95% GI tract: -regulates intestinal movement -90% cells of the lining of GI tract -10% enteric neurons *Also located in platelets to facilitate aggregation for blood clotting Types of Receptors (5-HT1-7) Receptor Function 1A, 1B , 1D, 1E, 1F Anxiety, aggression, sexual behavior, appetite, vasoconstriction 2A, 2B, 2C 2A: inhibits dopamine release; mediates anxiety, agitation, hallucinations, sexual behavior, weight gain/loss 2B: Smooth muscle (GI tract), cardiovascular function 2C: inhibits dopamine and norepinephrine release; mediates appetite, anxiety, mood, GI motility, sexual behavior, thermoregulation, weight gain/loss 3 Chemoreceptor trigger zone, emesis, GI/bowel motility, nausea, memory 4 Cardiac repolarization (seizure susceptibility), respiration, gastric emptying, oesophageal peristalsis, appetite, anxiety 5A, 5B Locomotion, anxiety, sleep, cognition, thermoregulation, respiration, mood, memory 6 7 Norepinephrine Innervation of the CNS Thalamus Cingulate gyrus Cingulum Neocortex Hippocampus Hypothalamus Pituitary Amygdala Cerebellar cortex Olfactory and entorhinal cortices Locus ceruleus To spinal cord Hippocampus Lateral tegmental NA cell system From Kaplan HI, Sadok BJ. In: Synopsis of Psychiatry, Behavioral Sciences, Clinical Psychiatry, 6th ed. Revised. 1991. Neurotransmitters—Mechanisms of Action Autoreceptor PRESYNAPTIC CELL SYNAPTIC CLEFT Neurotransmitter Reuptake transporter Neurotransmitter receptor POSTSYNAPTIC CELL 5-HT Receptors Regulatory Processes 5HT1A 5HT 1D 5HT 5HT1A synthesis 2A Sexual dysfunction, CNS stimulation 5HT 5HT storage release 5HT 2C Weight regulation ? 5HT 5HT1D 5HT Transporter 5HT3 Might food intake Regulate vasculature Headache Nausea ? anxiety, insomnia, panic Pharmacologic Effects of Antidepressants Reduce depression Psychomotor activation Antiparkinsonian effects Sedation/drowsiness Hypotension Weight gain H1 block Blurred vision Dry mouth Constipation Sinus tachyardia Urinary retention Cognitive dysfunction ACh block Alpha2 block DA reuptake inhibition Antidepressant Alpha1 block 5HT reuptake inhibition Reduce depression Antianxiety effects GI disturbances Sexual dysfunction NE reuptake inhibition Anxiety Postural hypotension Dizziness Reflex tachycardia Memory dysfunction Reduce depression Tremors Tachycardia Erectile/ejaculatory dysfunction The Evolution of Antidepressants 1950s MAOIs 1960s Tricyclics 1970s Older heterocyclics 1980s 1990s SSRIs Newer dual reuptake inhibitors Selective dopamine reuptake inhibitors Mixed Receptor Effects Brief history of MAOI’s Monoamine oxidase inhibitors first observed to have mood elevating properties (1950’s) Limited prescribing – Acute hypertension reported from ingestion of dietary tyramine “cheese reaction” – Interactions with other medications – Introduction of the newer antidepressants Continued efforts have been made to develop MAOI’s that do not require restriction of dietary tyramine – One strategy has been to exploit the existence of multiple isoenzymes of MAO (MAOA and MAOB) Monoamine Oxidase Inhibitor Antidepressants Type Selectivity Agent Brand Irreversible Nonselective Phenelzine Nardil Tranylcypromine Parnate Isocarboxazid Marplan Reversible MAO-A selective Clorgyline MAO-B selective Selegiline MAO-B selective Moclobemide Brofaramine Toloxatone Befloxatone Eldepryl Monoamine Oxidase Inhibitors Drugs Brand Name Dosage Range (mg) Isocarboxazid Marplan 20-60 Phenelzine Nardil 45-90 Tranylcypromine Parnate 20-60 Selegeline patch Emsam 6-12 The Evolution of Antidepressants 1950s MAOIs 1960s Tricyclics 1970s Older heterocyclics 1980s 1990s SSRIs Newer dual reuptake inhibitors Selective dopamine reuptake inhibitors Mixed Receptor Effects Tricyclic Antidepressants Amitriptyline (Elavil) Nortriptyline (Pamelor ) Imipramine(Tofranil ) Desipramine (Norpramin ) Clomipramine (Anafranil ) Amoxapine(Asendin ) Doxepin (Sinequan ) Maprotiline (Ludiomil) Protriptyline (Vivactil) Trimipramine (Surmontil) Pharmacologic Effects of TCA’s Sedation/drowsiness Hypotension Weight gain H1 block Blurred vision Dry mouth Constipation Sinus tachyardia Urinary retention Cognitive dysfunction ACh block Antidepressant Alpha1 block Postural hypotension Dizziness Reflex tachycardia Memory dysfunction 5HT reuptake inhibition Reduce depression Antianxiety effects GI disturbances Sexual dysfunction NE reuptake inhibition Reduce depression Tremors Tachycardia Erectile/ejaculatory dysfunction The Evolution of Antidepressants 1950s MAOIs 1960s Tricyclics 1970s Older heterocyclics 1980s 1990s SSRIs Newer dual reuptake inhibitors Selective dopamine reuptake inhibitors Mixed Receptor Effects Selective Serotonin Reuptake Inhibitors Drugs Starting Maximum Range Fluoxetine 10 (QAM) 80 20-40 Paroxetine 10 (QHS) 50 20-40 Citalopram 10 40* 20-40 Escitalopram 5 20 10-20 Fluvoxamine 50 300 (BID) 100-300 Sertraline 25 200 50-200 * http://www.fda.gov/Safety/MedWatch/SafetyInformation/SafetyAlertsforHumanMedicalProducts/ucm297624.htm?source=govdelivery 1.) The antidepressant effects of the drugs are known to be limited to the s-isomer 2.) The difference between the effects of citalopram and escitalopram on the QT interval presumably means that the QT effects are not specific to the s-isomer http://www.fda.gov/Drugs/DrugSafety/ucm297391.htm FDA Recommendations re; Citalopram Not recommended at doses greater than 40mg due to prolongation of QTc interval Not recommended for use in patients with congenital long QT syndrome, bradycardia, hypokalemia, hypomagnesemia, recent acute MI or uncompensated heart failure Not recommended in patients who are taking other drugs that prolong QTc The max recommended dose is 20mg per day for patients with hepatic impairment, patients > 60 years of age, patients who are CYP 2C19 poor metabolizers and patients who are taking another CYP219 inhibitor; these factors can lead to increased blood levels of citalopram, increasing the risk of QTc prolongation and Torsades de Pointes http://www.fda.gov/Drugs/DrugSafety/ucm297391.htm The Evolution of Antidepressants 1950s MAOIs 1960s Tricyclics 1970s Older heterocyclics 1980s 1990s SSRIs Newer dual reuptake inhibitors Selective dopamine reuptake inhibitors Mixed Receptor Effects Serotonin and Norepinephrine Reuptake Inhibitors Drugs Starting Maximum Range Venlafaxine (Effexor) 25 375 150-375 BID/TID Venlafaxine (Effexor XR) 37.5 225 75-225 QD Duloxetine (Cymbalta) 10 60 20-60 QD/BID Desvenlafaxine (Pristiq) 50 100 50-100 QD Levomilnacipran ER (Fetzima) 20 120 40 – 120 QD The Evolution of Antidepressants 1950s MAOIs 1960s Tricyclics 1970s Older heterocyclics 1980s 1990s SSRIs Newer dual reuptake inhibitors Selective dopamine reuptake inhibitors Mixed Receptor Effects Dopamine and Norepinephrine Reuptake Inhibitors Drugs Starting Maximum Range Bupropion 100mgBID 450mg(3-4 divided) 300-400 150mgQD 200mgBID 300-400 150mgQD 450mgQD 300-400 150mgQD 300mg For 7-12wks Wellbutrin Bupropion WellbutrinSR Bupropion WellbutrinXL Bupropion Zyban The Evolution of Antidepressants 1950s MAOIs 1960s Tricyclics 1970s Older heterocyclics 1980s 1990s SSRIs Newer dual reuptake inhibitors Selective dopamine reuptake inhibitors Mixed Receptor Effects Mixed Receptor Effects SRI, 5HT2 antagonist – Trazodone (Desyrel, Oleptro) – Nefazodone Noradrenergic (alpha 2), 5HT2, 5HT3 antagonist – Mirtazapine (Remeron) SRI, 5HT1 partial agonist – Vilazodone (Viibryd) SRI, 5HT1a agonist, 5HT1b partial agonist, 5HT3/7 antagonist – Vortioxetine (Brintellix) Some Augmentation Strategies Lithium Thyroid Supplementation Atypical Antipsychotics Buspirone Modafanil Lamotrigine Stimulants ……………………… Discontinuation Syndrome Withdrawal Syndrome – Can occur with most antidepressants – Symptoms: dizziness, nausea, paresthesias, anxiety/insomnia – Onset 36-72 hours – Duration 3-7 days Summary Depression is a biologically based illness that responds to antidepressant therapy in the majority of patients Appropriate choice of antidepressant therapy should be based on past response, patient characteristics and adverse event profile Appropriate trial length and dosage is important when evaluating response to antidepressants Questions?