* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Ch. 24 – The Digestive System
Survey
Document related concepts
Transcript
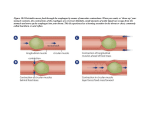
Ch. 24 – The Digestive System • The overall idea is to obtain nutrients from the environment • There are 2 general types of digestive organs involved: – 1. Parts of the digestive tract (= a long muscular tube from the mouth to the anus) • This is a.k.a. the gastrointestinal (GI) tract or alimentary canal • It’s made up of the oral cavity (mouth), pharynx (throat), esophagus, stomach, small intestine, and large intestine • Food passes through these – 2. Accessory organs = the teeth, tongue, salivary glands, liver, gallbladder, and pancreas • Food does not pass through these Fig. 24-1, p. 882 The general functions of the digestive system • 1. Ingestion = eating • 2. Mechanical processing (e.g. by the teeth and stomach) = crushing, shearing, and mixing – This increases the surface area on food particles for attack by enzymes – Smaller pieces are easier to move • 3. Digestion = chemical breakdown (usually by enzymes) – Proteins → amino acids – Triglycerides → glycerol + fatty acids – Polysaccharides → monosaccharides • 4. Secretion of water, acids, enzymes, buffers, and ions • 5. Absorption of nutrients across the digestive tract epithelium, and eventually into the blood • 6. Excretion = the removal of waste (via defecation) Fig. 24-1, p. 882 1 An overview of specific digestive organ functions Fig. 24-1, p. 882 The peritoneum and mesenteries • • We first learned about the parietal peritoneum, visceral peritoneum (serosa), and peritoneal cavity in BIOL& 242 Mesenteries = double sheets of peritoneal membrane that connect the parietal peritoneum to the visceral peritoneum – Function: stabilize and provide a route for N.A.V.a.L to the abdominopelvic organs Fig. 24-2bd, p. 884 2 The general histology of the GI tract • Most parts of the tube have most (if not all) of these features • Additional details are found in the textbook and on p. 24 of the Lab Manual Lumen (interior) Exterior Fig. 24-3, p. 885 Fig. 24-4, p. 887 The movement of digestive materials • The muscular layers of the GI tract have gap junctions between cells and pacesetter cells that spontaneously depolarize – They can also be stimulated autonomically by the CNS and ENS (see the next slide) • Peristalsis = waves of rhythmic contractions that propel the bolus (= a soft compacted mass of digestive materials) forward through the tract • Segmentation (not shown here) = irregular contractions in the intestines that mix/churn/fragment the bolus 3 The regulation of digestive activities These short reflexes are part of the enteric nervous system (ENS), the lesser known third division of the ANS E.g. prostaglandins and histamine Fig. 24-5, p. 888 E.g. gastrin, secretin, etc. We’ll discuss some of the main ones later in the chapter. The oral (buccal) cavity and tongue • • The oral (buccal) cavity (mouth) is lined by the oral mucosa, which has a protective stratified squamous epithelium (some parts of it are keratinized) Functions of the tongue include: – – – – Mechanical processing and manipulation of food for chewing and swallowing Sensation (taste, touch, and temperature) Secretion of mucins (= mucus glycoproteins) Secretion of lingual lipase, which initiates the digestion of fats Fig. 24-6, p. 889 4 Fig. 24-7, p. 891 • • • • Salivary glands There are 3 pairs: parotid, sublingual, and submandibular Functions of saliva: moisten and lubricate food, rinse/flush the mouth, dissolve chemicals for taste bud stimulation, initiate the chemical digestion of complex carbos (by salivary amylase) Composition: saliva is 99.4% water; the rest is solutes, including ions, salivary amylase, buffers (so pH ~ 7.0), waste products, IgA antibodies, lysozyme, and mucus (which helps with the lubrication of food) Secretion is stimulated by: – – – – Parasympathetic activity The smell, sight, or sound of food Food in the mouth, the taste of food, and chewing Stomach or small intestine irritation (in order to dilute, rinse, or buffer the unpleasant stimulus) • Periodontal ligament = – Dense connective tissue (CT) that, along with cementum, anchors the tooth in its alveolus (bony tooth socket) Teeth • Function: mechanical processing – Mastication = chewing • Tooth composition: – Dentin = the bulk of a tooth • It’s similar to bone (but it’s acellular) – The pulp cavity within the crown • Contains pulp (= N.A.V.a.L.), which exits via the root canal and apical foramen – Enamel (the hardest biologicallymade substance) • = crystalline calcium phosphate • Covers and protects the dentin of the crown Fig. 24-8a, p. 892 5 Fig. 24-9, p. 894 Types of teeth • Deciduous (primary) teeth = 20; typically appear between 6-24 months of age – Per quadrant: 2 incisors, 1 cuspid (canine), and 2 molars • Permanent (secondary) teeth = 32; most appear between 6-12 years of age – Per quadrant: 2 incisors, 1 cuspid (canine), 2 bicuspids (premolars), and 3 molars Fig. 24-8b, p. 892 • • • = a common passageway for solid food, liquids, and air Has underlying skeletal muscle for swallowing Has 3 regions: The pharynx (throat) – 1. The nasopharynx (respiratory only) – superior to the uvula of the soft palate – 2. The oropharynx (respiratory and digestive) – from the uvula to the base of the tongue (or tip of the epiglottis) – 3. The laryngopharynx (respiratory and digestive) – from the base of the tongue to the junction of the esophagus and larynx • The oropharynx and laryngopharynx are lined and protected by a protective stratified squamous epithelium Fig. 24-6a, p. 889 6 The esophagus Fig. 24-10, p. 895 • • = a hollow muscular tube that functions to transport solid food and liquids from the pharynx to the stomach Histology notes: – The mucosa includes a protective stratified squamous epithelium – The submucosa contains esophageal (mucous) glands for lubrication of the bolus • The mucosa and submucosa are folded when the esophagus is empty, allowing for expansion during swallowing – The muscularis externa contains a mixture of skeletal muscle and smooth muscle – Adventitia (not serosa) = fibrous CT for attachment Swallowing (deglutition) • The entire process takes ~ 9 seconds for a typical bolus • It consists of 3 phases: – 1. The buccal phase – the tongue moves the bolus from the oral cavity to the oropharynx, and the soft palate and uvula move upward (to seal off the nasopharynx) – 2. The pharyngeal phase – the bolus stimulates receptors in the posterior oropharynx, which triggers the swallowing reflex: • The larynx moves up, the epiglottis folds over and covers the superior opening of the larynx (directing the bolus toward the esophagus), and there is inhibition of the respiratory centers (breathing stops for less than a second) – 3. The esophageal phase – peristalsis pushes the bolus toward the stomach Fig. 24-11, p. 896 7 Stomach terminology • Fundus = the dome-shaped region superior to the esophageal opening • Body = the main central region • Pylorus = the region that connects with the duodenum via the pyloric sphincter (a sphincter is a circular muscular valve) • Rugae = folds of mucosa that allow the stomach to stretch • Chyme = a viscous, acidic, soupy mix of partially digested food and gastric juice Fig. 24-12b, p. 898 Functions of the stomach • • • • Temporary storage of ingested food Mechanical processing Chemical digestion via acid and enzymes Production of intrinsic factor = a glycoprotein needed for the intestinal absorption of vitamin B12 Fig. 24-12a, p. 898 8 Note that the: • • Mucosa is folded into gastric pits that open into deeper gastric glands Muscularis externa has 3 layers of smooth muscle Histology of the stomach lining – An inner oblique layer is present in addition to the circular and longitudinal layers Fig. 24-13a, p. 899 The stomach mucosa • Gastric pits and glands contain the following cells (which together secrete gastric juice that mixes with ingested food to form chyme): Under the ‘scope in lab: Parietal cells = “fried eggs”; central round nucleus Chief cells = not “fried eggs”; grainy; in clusters with nuclei toward the outer edge of the cluster; more numerous in the deeper region of the gastric glands – Parietal cells secrete HCl (hydrochloric acid) and intrinsic factor – Chief cells secrete the inactive proenzyme pepsinogen… • Which is converted by HCl to the active enzyme pepsin, which begins protein digestion – Mucous cells secrete an alkaline mucus (to protect the stomach’s epithelium from the HCl) – G cells secrete gastrin (a hormone), which: • ↑ Stomach motility • ↑ The secretion of gastric juice Fig. 24-13b, p. 899 9 HCl secretion by parietal cells • • Keeps the stomach contents at a pH of about 1.5-2.0 Functions: – – – – Kill most microbes Denature the proteins (including enzymes) in food Help break down plant materials and the CT in meat Help convert inactive pepsinogen to active pepsin Fig. 24-14, p. 900 Regulation of gastric activity • Gastric acid and enzyme secretion can be controlled/regulated by: – 1. The CNS – 2. Short reflexes via the stomach wall • These are part of the enteric nervous system (ENS) – 3. Hormones secreted by the GI tract • There are 3 specific phases of gastric secretion: – 1. The cephalic phase – 2. The gastric phase – 3. The intestinal phase On the next two slides, for each phase, note the differences with respect to the stimulus (what causes the phase to begin), some of the key responses, and the overall function 10 The 3 phases of gastric secretion (continued on the next slide…) Fig. 24-15, p. 902 Fig. 24-15, p. 903 The 3 phases of gastric secretion Additional notes: • (continued from the previous slide) • CCK, GIP, and secretin also target the pancreas; CCK also targets the gallbladder; secretin also targets the liver (more details later) There are also two central gastric reflexes (described above) that stimulate activity of the small intestine 11 Digestion and absorption in the stomach Digestion • The digestion of carbohydrates and lipids (by salivary amylase and lingual lipase, respectively) continues until the pH of the stomach contents falls below 4.5 • The digestion of proteins by pepsin begins – This is the preliminary digestion of proteins (small polypeptides and peptides)…further breakdown into individual amino acids will be completed in the small intestine Absorption • No nutrient absorption occurs in the stomach, but there is some absorption of alcohol, aspirin, and other lipid-soluble drugs The small intestine • • Is the site of most of the chemical digestion and nutrient absorption that occurs in the GI tract Has 3 segments: – 1. Duodenum – has duodenal (Brunner’s or submucosal) glands in the submucosa that secrete an alkaline mucus to help neutralize incoming chyme – 2. Jejunum – 3. Ileum – has many Peyer’s patches (lymphoid tissue) that protect the small intestine from the large intestine’s resident bacteria • It connects to the cecum of the large intestine at the ileocecal valve (not shown here) Fig. 24-16, p. 904 12 Small intestine histology • The wall of the small intestine is modified to increase surface area for secretion and absorption; there are 3 levels of folding: – 1. Circular folds (plicae circulares) = relatively large (macroscopic), transverse, permanent folds • These folds contain submucosa (which is useful for lab slides) – 2. Intestinal villi = fingerlike projections of mucosa • They contain lacteals (= lymphatic capillaries), which absorb fatty acids, and transport them as chylomicrons (lipid + protein) to the blood via the lymphatic system Fig. 24-17ab, p. 905 Small intestine histology – 3. Microvilli = microscopic projections of the epithelial plasma (cell) membrane (they’re so tiny that they’re barely visible in this figure) Fig. 24-17cd, p. 905 • They form the brush border and contain brush border (digestive) enzymes • Thanks to the circular folds, villi, and microvilli, the total increase in surface area (for digestion and absorption) compared to the wall of a simple, unfolded tube with smooth walls is 600X! (~ 2200 ft2 total) 13 • Intestinal glands Are a.k.a. intestinal crypts or crypts of Lieberkuhn, and contain… – Mucous cells that, like duodenal glands, secrete an alkaline mucus to help neutralize incoming chyme – Stem cells that replace the epithelial cells that are shed into the lumen – Enteroendocrine cells that secrete gastrin, GIP, secretin, and CCK • Intestinal juice consists of water (due to osmosis from the mucosa to the relatively concentrated chyme in the lumen), plus the secretions from the intestinal glands Fig. 24-17b, p. 905 Fig. 24-18a, p. 908 The pancreas • • Is a mixed gland; i.e., it has both exocrine and endocrine functions Exocrine ducts: – The pancreatic duct (duct of Wirsung) joins the common bile duct and empties into the duodenum at the duodenal papilla – In 3-10% of the population, the pancreatic duct branches to form the accessory pancreatic duct (duct of Santorini), which also empties into the duodenum 14 Pancreatic histology • 1. The exocrine portion = acini and ducts (= ~ 99% of the pancreas) – The acini secrete digestive enzymes – Duct cells secrete water and buffers (which help neutralize chyme) Fig. 24-18b, p. 908 • Pancreatic juice = an alkaline mixture of the enzymes, H20, and buffers • 2. The endocrine portion = pancreatic islets (islets of Langerhans) – These secrete (mostly) the hormones glucagon and insulin More on pancreatic juice • Its secretion is controlled by the vagus nerve (CN X) as well as duodenal hormones (which are released when chyme enters the duodenum), especially… – Secretin, which targets pancreatic duct cells to secrete water and buffers – Cholecystokinin (CCK), which targets pancreatic acini to secrete pancreatic enzymes • Its enzymes include (see Table 24-1 for much more FYI detail)… – – – – Pancreatic alpha-amylase (a carbohydrase) Pancreatic lipase Nucleases Proteolytic enzymes (= proteases and peptidases) • These are secreted as inactive proenzymes (to protect the cells of the pancreas itself) – E.g. trypsinogen, chymotrypsinogen, procarboxypeptidase, and proelastase are converted into active trypsin, chymotrypsin, carboxypeptidase, and elastase, respectively 15 The liver • = the largest visceral organ in the body • Has 4 lobes (the right and left are the largest ones) • The falciform ligament separates the right and left lobes • The round ligament = a thickening in the falciform ligament that is the remnant of the fetal umbilical vein Fig. 24-19, p. 910 • • The liver is divided by CT into roughly six-sided lobules Portal areas (portal or hepatic triads) at the corners of each lobule contain branches of the: Liver histology – 1. Hepatic portal vein – 2. Hepatic artery proper – 3. Bile ducts • Hepatocytes (= liver cells) surround sinusoids (= large leaky capillaries) – Arterial and portal blood empties into the sinusoids – The sinusoids empty into the central veins • Kupffer cells = fixed macrophages… – Which phagocytize worn out RBCs, bacteria, debris, etc. • Hepatocytes secrete bile into the bile duct system (part of which is shown here in green), which carries bile out of and away from the liver Fig. 24-20ab, p. 911 16 Some functions of the liver It has over 200 functions! Here are just a few… 1. Metabolic regulation – Carbohydrate metabolism (e.g. glycogenolysis, gluconeogenesis, and conversion into lipids) – Lipid metabolism (regulation of blood levels of triglycerides, fatty acids, and cholesterol) – Amino acid metabolism (e.g. protein synthesis and conversion into lipids or glucose) – Waste removal (e.g. conversion of ammonia → less harmful urea) – Vitamin storage (B12 and fat-soluble vitamins A, D, E, and K) – Mineral storage (iron) – Drug inactivation 2. Hematological regulation – – – – Phagocytosis and antigen presentation (by Kupffer cells) Synthesis of plasma proteins Removal of circulating hormones and antibodies Removal (or storage) of toxins 3. The synthesis and secretion of bile (see the next slide for the functions of bile) Bile • Contains: – Mostly water, and minor amounts of cholesterol, bile salts (derived from cholesterol), pigments (bilirubin), and ions • Functions: – The emulsification of fats • Bile salts have hydrophilic and hydrophobic ends, so they surround large fat globules and break them into small lipid droplets in a watery environment – This increases the surface area for digestion by lipases, and aids absorption – The excretion of bilirubin • Remember (see Ch. 19), bilirubin is a pigment derived from the heme of hemoglobin • The bilirubin in bile is ultimately converted to urobilins and stercobilins, which are eliminated in feces • Note: > 90% of the bile salts in bile are reabsorbed (mostly by the ileum) for recycling back to the liver 17 The gallbladder Fig. 24-21, p. 912 Functions: • • • 1. Bile storage 2. Bile modification – via the reabsorption of water, concentrating the bile 3. Bile release – the presence of chyme in the duodenum (especially if the chyme is lipid-rich) causes the release of CCK, which causes the hepatopancreatic sphincter (sphincter of Oddi) to relax and the gallbladder to contract The main actions of the major digestive tract hormones Fig. 24-23, p. 916 18 The large intestine • • Consists of the cecum, colon, and rectum Connects with the ileum of the small intestine via the ileocecal valve (which is a sphincter) Fig. 24-24a, p. 918 • • • • Histology of the large intestine No villi are present, and no digestive enzymes are produced The mucous (goblet) cells of the intestinal glands (crypts) produce mucus for lubrication Lymphoid nodules are present in the mucosa and submucosa The outer, longitudinal layer of the muscularis externa has been reduced to 3 distinct bands called taeniae coli; the muscle tone of these bands creates haustra (= pouches) Fig. 24-25, p. 919 19 Physiology of the large intestine • Functions of the large intestine include: – Absorption of: • Water (forming feces) • Ions (electrolytes) • Vitamins produced by normal resident bacteria (e.g. vitamin K, biotin, and vitamin B5) • Bile salts • Certain organic waste products and bacterial toxins – Storage of feces prior to defecation • Movements of the large intestine include: – Peristalsis (which is typically slow) – Segmentation movements (= haustral churning) – Mass movements = powerful peristalsis a few times a day • The stimulus = the stretch of the stomach or duodenum • These move feces from the transverse colon onward into the rectum – Defecation (see the next slide) The defecation reflex • • • Fig. 24-26 p. 921 The internal anal sphincter is made of smooth muscle (involuntary) The external anal sphincter is made of skeletal muscle (voluntary) The distal anal canal is lined by a protective stratified squamous epithelium Fig. 24-24c, p. 918 20 Carbohydrate digestion and absorption • Amylases break down complex carbohydrates into trisaccharides and disaccharides • Brush border enzymes break down trisaccharides and disaccharides into monosaccharides (simple sugars), such as glucose and fructose • Monosaccharides are absorbed via facilitated diffusion and Na+linked cotransport Fig. 24-27, p. 923 Lipid digestion and absorption • • • • • Bile salts in the small intestine emulsify fats (triglycerides) Lipases break down triglycerides into monoglycerides and fatty acids Bile salts interact with monoglycerides and fatty acids to form tiny micelles, which aid absorption (via simple diffusion) Monoglycerides and fatty acids are reassembled into triglycerides and coated with proteins to form chylomicrons Chylomicrons are secreted via exocytosis and diffuse into lacteals Fig. 24-27, p. 923 21 Protein digestion and absorption • Is complex and time-consuming • Each protease targets specific types of peptide bonds and breaks down polypeptides into smaller peptides • Peptidases (including brush border enzymes) break down small peptides into individual amino acids • The mechanism of amino acid absorption is similar to that of monosaccharides (refer back 2 slides) Fig. 24-27, p. 923 The secretion and absorption of water • Fun fact: you lose only ~ 2% of the total water in the GI tract to the feces! – Total water ingested + secretions = 9200 mL – Water lost in feces = 150 mL • Most absorption of water occurs in the small intestine • Water is absorbed osmotically following the absorption of solutes (e.g. nutrients and ions) – See Table 24-2 for more FYI info on the absorption of vitamins and ions Fig. 24-28, p. 926 22