* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Tissues - Sinoe Medical Association
Survey
Document related concepts
Embryonic stem cell wikipedia , lookup
Artificial cell wikipedia , lookup
Nerve guidance conduit wikipedia , lookup
Cellular differentiation wikipedia , lookup
Hematopoietic stem cell wikipedia , lookup
Chimera (genetics) wikipedia , lookup
Microbial cooperation wikipedia , lookup
Cell culture wikipedia , lookup
State switching wikipedia , lookup
Neuronal lineage marker wikipedia , lookup
List of types of proteins wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
Human embryogenesis wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Cell theory wikipedia , lookup
Transcript
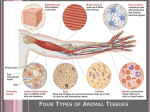
The cell and tissue Tissues : Danil Hammoudi.MD I. Histology – The study of tissues 4 basic tissue types • Epithelial • Connective • Muscle • Nervous Groups of cells similar in structure and function II. Epithelial tissue A. Two major types 1. covering and lining epithelium 2. glandular epithelium • exocrine – outside of the body • endocrine – into the bloodstream B.Epithelial Tissue Cellularity – composed almost entirely of cells. closely packed cells – continuous sheets Special contacts – form continuous sheets held together by tight junctions and desmosomes Polarity – apical and basal surfaces Supported by connective tissue – reticular and basal laminae 1 The cell and tissue Avascular but innervated – contains no blood vessels but supplied by nerve fibers Regenerative – rapidly replaces lost cells by cell division Attached to adjacent connective tissue by basement membrane. Derivation: Ectoderm, mesoderm, and endoderm can all give rise to epithelia • Cells are contiguous; arranged in sheets • Epithelium has little extracellular space • Basal surface on basement membrane • Cells are polarized • Membrane of apical surface is specialized HIGH MITOTIC ACTIVITY C: Where do we find Epithelial Tissue? • Covering body surfaces – Epidermis – Epithelium • Lining body cavities – Mesothelium - body cavities – Endothelium - cardiovascular system • Forming parenchyma of glands D. Functions mechanical Protection dehydration chemicals (acids) enzymes pathogens Nutrients Absorption Gasses Ions (salt) Mucus Secretion enzymes/proteins lipds/steroid hormones salts water (sweat) nutrients (male/femal reproductive). touch Sensation heat/cold pain taste smell pressure 2 The cell and tissue lactation Contraction (myoepithelial cells) perspiration salivation ions Transport antibodies nutrients Epithelium Functions mechanical, chemical, bacterial Protection Secretion sweat/wax/mucus/saliva/milk/hormone water, metabolites, debris/waste absorption Exchange /filtering Transport Sensory reception Reproduction O2, CO2 through capillary walls mucus, sperm etc (using cilia) smell (olfaction), taste (gustation) not mitotic duplication) cells of gonads produce gametes E. Covering and lining epithelia 1. classified based on number of layers - simple = single - stratified = “layered” - pseudostratified 2. classified based on cell shape [SEE DETAILS BELOW] - squamous = flat“scale” - cuboidal - columnar - transitional 3 The cell and tissue Classification of Epithelia Squamous, cuboidal, or columnar Surface view, Simple Squamous Epithelium 4 The cell and tissue cross section, simple squamous and simple cuboidal epithelium longitudinal section, simple cuboidal epithelium 5 The cell and tissue simple cuboidal epithelium on a free surface simple cuboidal epithelium (kidney tubules in oblique section) 6 The cell and tissue simple cuboidal epithelium (kidney tubules in cross section) simple columnar epithelium (intestinal lining) pseudostratfied columnar epithelium (lining the trachea) 7 The cell and tissue nonkeratinized stratified squamous epithelium 8 The cell and tissue keratinized stratified squamous epithelium (skin) 9 The cell and tissue Surface epithelia: continuous sheet of one or more cellular layers number cell layers • simple: all cells touch basal lamina • simple proper: all cells also reach free surface • • pseudostratified: basal cells fail to reach free surface stratified (layered): surfaces subject to wear • keratinized • nonkeratinized (mucous membranes) parakeratinized (papillae of tongue) • transitional: in urinary tract; dome-shaped cells at free surface shape of cells Outermost layer of stratified epithelium: looked at section perpendicular to surface; generally reflected in shape of nuclei • squamous (flat; scale-like): endothelium, mesothelium and peritoneum (pleural and pericardial cavity), lining alveoli 10 The cell and tissue • cuboidal: spherical nuclei; typically located in center of cell but displaced basally in exocrine cells; frequently described as low (verging of squamous), medium, or high cuboidal (verging on columnar). • columnar: elongate; cigar-shaped nuclei surface specializations • surface (luminal) specializations: • cilia and flagella expecially pseudostratified and columnar epithelia • microvilli (= brush border (proximal convoluted tubule) also called striated border (small intestine); 0.5 to 1.0 micro meters; as many as 3000 per apical surface; microfilaments in core of microvilli attached to electron-dense material at tip • stereocilia appear branched due to fixation artifact; in male reproductive tract (e.g., epididymis); facilitate absorptive processes Apical surface specializations: • Cilia: large - individuals can be seen by light microscopy motile organelle found predominately on respiratory epithelium internal framework of microtubules in a 9+2 arrangement insert into basal bodies at their base consisting of a centriole and supporting material. Cilia are 0.25 um thick and 10 to 200 um long. They can be seen individually with a (good) light microscope. • Microvilli: surface protrusions too small and close together to be seen individually, instead a brush border is seen at the apical surface of cells. increase surface area in adsorptive cells formed from a core of 20-30 bundled actin filaments Microvilli are 0.08 um wide and 0.5 to 1.0 um tall. They cannot be individually seen with a light microscope (which is limited to obervation of structures about 0.2 um in diameter). • Stereocillia: an elongated form of microvilli found in the cells of the epididymis and hair cells of the inner hear. These are NOT true cilia 11 The cell and tissue Cilia =C, CM = cell membrane, BB= basal bodym Cy= cytosol Microvilli with actin filaments 12 The cell and tissue Lateral specializations (junctions and patterns of folding): intercellular surfaces specializations • • junctional complex (always paired on opposing surfaces): combination zonula occludens, zonula adherens desmosomes occluding junctions = tight junctions: collar; sealing strands (fine matching ridges); stitch membranes together • fascia occludens: discontinuous strips of tight junctions between endothelial cells (except in brain) • zonula occludens: tight junctions form continuous circumferential band • adhering junctions: anchorage of cytoskeleton and binding cite between cells (also in cardiac and visceral muscle) • zonula adherens = belt desmosomes: circumferential; beneath zonula occludens; terminal web: fine meshwork of microfilaments joined to zonula adherens desmosomes (circumferential and spot adhering junctions) also called macula adherens: patches; beneath zonula adherens; transmembrane 13 The cell and tissue linkers: cadherins (calcium dependent cellular adhering proteins); (midway across intercellular space); : unique desmoplakin (desmogleins) between cells; tonofilaments (intermediate filaments) coalesce at plaque within cell intermediate filaments inserted into electron-dense plaque = prickles of spiny layer of epidermis • communicating junctions = gap or nexus junctions: contain hundreds of tiny pores (< 2 nanometers) through connexon complex (of 6 transmembrane proteins); permitting passage chemical messages (cations; nutrients); pore closes in presence of increased calcium ion (also in cardiac and visceral muscle) • Basal specialization • • folding: ion transport • hemidesmosome: resemble desmosome but do not occur in pairs; integrins: receptors for laminin and collagen type IV. The basal lamina is present at the basal surface of all epithelial cell layers and forms a limiting barrier between connective and epithelial tissues. Also plays a role in regulating the passage of macromolecules between connective tissues and the lumen of epithelial bound cavities. The basal lamina is composed of a central, dense lamina densa, sometimes flanked on one or both surfaces by a lighter lamina lucida. • • Major components of the basal lamina: 1. Collagen (type IV) 2. Glycoproteins (laminin) 3. Proteoglycans (heparan sulfate) • • Attachment to underlying lamina propria is made by fibrils of collagen type VII and microfibrills. The underlying connective tissue may sometimes secrete a reticular lamina composed of reticular fibrils adjacent to the basal lamina. 14 The cell and tissue Trachea Types and location Simple squamous: Selective diffusion, absorption or secretion; pavement epithelium Simple cuboidal: Lines small ducts and tubules; excretory, secretory or absorptive; ; nuclear chromatin dispersed; nucleoli prominent; bm. Highly absorptive surfaces (sm. intestine); secretory surfaces (stomach); lining gall bladder (absorbs water); nuclei may be basal; microvilli Simple columnar: Simpl e columnar ciliated: 200 to 300 cilia per cell; female reproductive tract; nuclei apically distributed; includes secretory, nonciliated cells (with basal nuclei) Pseudostratified columnar ciliated: Nuclei disposed at different levels; basal cells do not extend to surface; larger airways of respiratory system = respiratory epithelium (mammals); mucociliary escalator. Resists abrasion; moistened by glandular secretions; but poorly adapted to withstand desiccation; oral cavity, pharynx, esophagus, anal canal, uterine cervix, vagina surface of skin (epidermis); cells keratinize; accumulate keratin Stratified squamous (mucous variety) Stratified squamous keratinizing: Stratified cuboidal Transitional only 2 to 3 cell layers; lining large excretory ducts of exocrine glands (salivary gland); not absorptive urinary tract (mammals); accommodates stretching and toxicity of urine; surface cells larger, pale-staining, scalloped surface outline; luminal surface appears 15 The cell and tissue thickened; may be binucleate; large, round, prominent nucleoli A. Squamous • • 1. Simple • • • • • 2. Stratified Mesothelium found on the outer surface of gut and most other visceral structures. This example is from the ileum. Mesothelium (peritoneum) - spread preparation giving a surface view; "cementing" lines stained with silver. lining of Bowman's capsule in the nephron of the kidney. The endothelium that lines the blood vessels may be seen on almost any slide of sectioned tissue, , skin, soft palate;, lip. Vagina (non-keratinizing). Upper esophagus (non-keratinizing). Human skin (keratinizing). B. Cuboidal • • 1. Simple • • Ovary. Kidney. See the proximal and distal convoluted tubules of the nephron and the collecting tubules. Note the brush border (microvilli) of the cells of the proximal convoluted tubule. Lining of some ducts, such as the sweat glands of the skin. Seminiferous tubules of the testis. C. Columnar 1. Simple 2. Stratified D. Pseudostratified E. Transitional F. Non-surface • • • • Gall bladder. Inner surface of the small intestine Glands of the stomach and small intestine. Rare; soft palate, pharynx, larynx, anus and the large ducts of glands (e.g., salivary, pancreas) • • • nose, trachea and large bronchi - note ciliated cells. epididymis - note the stereocilia. Fetal skull, xs. Note lining of nasal passages. • lining of ureter and renal pelvis. • Urinary bladder. • • cuboidal cells of the liver. Note that the Leydig cells are external to the seminiferous tubules. Islets of Langerhans of the pancreas. • Classification of Covering Epithelia Characteristic: Types: # of layers simple 16 The cell and tissue pseudostratified stratified cell shape squamous cuboidal columnar apical specialization ciliated keratinizing Epithelial cells are classified by the following three factors: • • • shape Stratification Specializations Classification of Epithelia Simple or stratified Shape • Squamous: Squamous cells are flat cells with an irregular flattened shape • • . The one-cell layer of simple squamous epithelium that forms the alveoli of the respiratory membrane, and the endothelium of capillaries, and is a minimal barrier to diffusion. Places where squamous cells can be found include 17 The cell and tissue o • • the alveoli of the lungs, the filtration tubules of the kidneys, and the major cavities of the body. These cells are relatively inactive metabolically, and are associated with the diffusion of water, electrolytes, and other substances. Cuboidal: o As the name suggests, these cells have a shape similar to a cube, meaning its width is the same size as its height. o The nuclei of these cells are usually located in the center. Columnar': o These cells are taller than they are wide. o Simple columnar epithelium is made up of a single layer of cells that are longer than they are wide. o The nucleus is also closer to the base of the cell. o The small intestine is a tubular organ lined with this type of tissue. o Unicellular glands called goblet cells are scattered throughout the simple columnar epithelial cells and secrete mucus. o The free surface of the columnar cell has tiny hairlike projections called microvilli. '''' == HI ==''''They increase the surface area for absorption. • Transitional: o This is a specialized type of epithelium found lining organs that can stretch, such as the urothelium that lines the bladder and ureter of mammals. o Since the cells can slide over each other, the appearance of this epithelium depends on whether the organ is distended or contracted: if distended, it appears as if there are only a few layers; when contracted, it appears as if there are several layers. Stratification • Simple: There is a single layer of cells. • • Stratified: o More than one layer of cells. o The superficial layer is used to classify the layer. o Only one layer touches the basal lamina. o Stratified cells can usually withstand large amounts of stress. Pseudostratified with cilia: o This is used mainly in one type of classification (pseudostratified columnar epithelium). o There is only a single layer of cells, but the position of the nuclei gives the impression that it is stratified. o If a specimen looks stratified, but you can identify cilia, the specimen is 18 The cell and tissue pseudostratified ciliated epithelium since stratified epithelium cannot have cilia. 19 The cell and tissue 20 The cell and tissue Specializations • Keratinized cells contain keratin (a cytoskeletal protein). While keratinized epithelium occurs mainly in the skin, it is also found in the mouth and nose, providing a tough, 21 The cell and tissue impermeable barrier. • Ciliated cells have apical plasma membrane extensions composed of microtubules capable of beating rhythmically to move mucus or other substances through a duct. Cilia are common in the respiratory system and the lining of the oviduct. Simple Epithelium: simple squamous: lining of blood vessels, mesothelium of body cavity simple cuboidal: lining of small ducts found in kidney, salivary glands simple columnar: lining of gall bladder,small intestine simple columnar ciliated: female reproductive tract. Stratified Epithelium stratified squamous keratinising: found at dry surfaces (skin) stratified squamous non-keratinising: moist surfaces, oral cavity,anus,vagina stratified cuboidal epithelium: sweat glands, ovarian follicles stratified columnar epithelium: rare- found lining large ducts in salivary glands, sweat glands and pancreas. Pseudostratified Epithelium Neuroepithelia: Myoepithelial cells: transitional epithelium: lines urinary tract: characterized by dome like cells (undistended) or flattened cells when stretched. Pseudostratified columnar ciliated epithelium: lining of respiratory tract. Cells of epithelial origin which are specialized for a sensory function (taste buds). are found in glandular tissues (sweat,mammary and salivary) that are specialized for contraction. 22 The cell and tissue II/ Parenchymous epithelia = glandular epithelia A gland is one or more cells that makes and secretes an aqueous fluid Classified by: Site of product release – endocrine or exocrine Relative number of cells forming the gland – unicellular or multicellular • • (primarily secretory); separated from connective tissue by basal lamina; Function: to make macromolecules for export. Type of secreted macromolecules: • • • • • Proteins (insulin of the pancreas) Lipids (steroid hormones) Carbohydrates (salivary glands) All of the above (mammary glands) Salts (sweat glands) 23 The cell and tissue Goblet Cell Generally formed by down growth of surface epithelium into underlying connective tissue. • Exocrine : retain connection with surface o Single cell glands o goblet cells: PAS (periodic acid Schiff: carbohydrates stain red) positive; secrete mucus; scattered among cells of simple epithelium (respiratory and gastrointestinal tracts); mucigen granules (mixture of neutral and acidic proteoglycans; form viscid mucus. o multicellular glands o serous glands: secretion watery and rich in protein o o o mucous glands: secretion mucus; poor in protein o seromucous glands: intermediate o 8 types distinguished by morphology of secretory portion o (tubular [coiled versus straight] o acinar [simple versus compound]) o and branching versus straight excretory portions (which may also secrete bicarbonate) simple tubular: large intestine: single, straight; lined by goblet (mucous) cells simple coiled tubular: sweat glands; terminal secretory portion lined by simple cuboidal epithelium; followed by nonsecretory (excretory) duct lined by stratified cuboidal epithelium 24 The cell and tissue o o o o o o o simple branched tubular: stomach; secretory portions converge into unbranched duct (wider diameter); lined by mucus-secreting cells. simple acinar: rounded secretory unit; pockets in epithelial surface; secretory cells (e.g., mucus-secreting glands of penile urethra) simple branched acinar: several acini emptying into single excretory duct (stratified epithelium); sebaceous gland compound branched tubular: = duct branched; secretory portions tubular and branched; duodenal (Brunner's) glands compound acinar: secretory units are acinar and drain into branched ducts; pancreas; branched excretory ducts of increasing diameter lined by simple cuboidal epithelium compound tubulo-acinar: 3 types secretory units: branched tubular; branched acinar (serous cells); branched tubular (mucous cells) with acinar end pieces ([serous] demilunes); submandibular salivary gland myoepithelial cells: sometimes embedded in basement membrane; may aid secretion of acinus glands o striated ducts: striations due to mitochondria lined up along folds of basal membrane; transport Na and bicarbonate; cells high cuboidal to columnar o intercalated ducts come between acini or acini and striated ducts; cells low cuboidal Mechanism of secretion o merocrine (eccrine): exocytosis (e.g., proteins) o apocrine: discharge free, unbroken, membrane-bound vesicles; lipid secretory products (breast) and some sweat glands o holocrine: discharge whole cell; sebaceous glands (sebum) method of discharge: (for exocrine) Merocrine Apocrine Holocrine exocytosis (most common) products still membrane-bound entire cell secreted - breaks up 25 The cell and tissue where products are secreted: • endocrine: internally via tissue fluids • secretions are "hormones" • exocrine: via duct to epithelial surface • (NB pancreas is both exo- and endo-) 26 The cell and tissue Endocrine or ductless (hormones) lose connection with surface or formed without duct; surrounded by basement membrane; secretions enter circulatory system o clumps o cords follicular: thyroid 27 The cell and tissue Classification of Glandular Tissues: • • Unicellular: goblet cells Multicellular glands: arise by proliferation of a covering epithelium followed by invasion of the underlying connective tissue and further differentiation. Types of Multicellular glands: o Exocrine: glands connecting with surface epithelium via tubular ducts lined with epithelial cells. Classification of exocrine glands by shape: Tubular glands: Acinar glands: Tubuloacinar glands: simple tubular simple coiled tubular simple branched tubular compound tubular simple acinar simple branched acinar compound acinar tubuloacinar compound tubuloacinar Classification of exocrine glands by method of secretion: Merocrine: Holocrine: Apocrine: o Pancreas) secretory products leave cell via exocytosis sebaceous) secreted products is accompanied by loss of whole cells mammary) portions of apical cytoplasm are shed with secreted products. Endocrine: glands which lose their attachment too the surface during development. Secreted products are picked up and transported by blood vessels. Endocrine glands can take the form of: cellular cords in which groups of cells secrete their products into surrounded by blood vessels follicles in which secretor cells line a a follicle or cavity filled with secreted material (thyroid). Basement membranes (bm; epithelia) = external lamina (of muscle & nerve) 3 layers in em first two produced by epithelia: o contain collagen type IV, laminin (binds CAM); entactin (binds laminin to type IV collagen) lamina lucid o 10 to 50 micro-meters; abuts parenchymal cells; lamina densa 20 to 300 micro-meters; intermediate 28 The cell and tissue lamina fibroreticularis merges with CT type III; binds fibronectin. glycosaminoglycans heparan sulphate: PAS positive o collagen type IV o glycoproteins fibronectin (produced by fibroblasts) not produced by fibroblasts laminin entactin o Endocrine Glands Ductless glands that produce hormones Secretions include amino acids, proteins, glycoproteins, and steroids Exocrine Glands More numerous than endocrine glands Secrete their products onto body surfaces (skin) or into body cavities Examples include mucous, sweat, oil, and salivary glands The only important unicellular gland is the goblet cell Multicellular exocrine glands are composed of a duct and secretory unit A. Exocrine Glands 1. Simple tubular Human skin, Find the deep-lying tubular secretory units of the sweat glands and the simple (unbranched) ducts that carry the secretory product. Note that the secretory units are coiled and stain less intensely than the cells of the duct which form two layers. Locate the nuclei of the basally located myoepithelial cells. 2. Serous secretory units Tongue. Locate the serous von Ebner's glands and their ducts within and under the circumvallate papillae of the tongue. 29 The cell and tissue Note the cytoplasmic basophilia, due to large amounts of rough endoplasmic reticulum and free ribosomes, and the rounded nuclei. Located nearby are mucus secreting glands . Parotid glands. Locate the numerous serous acini of this gland. Sublingual gland. Locate the mucous secretory units of this mixed gland. They are characterized by a flattened, disc-like nucleus that is pushed against the 3. Mucous basal surface of the cell and reduced cytoplasmic basophilia. Serous components secretory units are also present, either as serous acini or as crescent shaped caps on the mucous acini called serous demilunes. Note the connective tissue septa and associated ducts and blood vessels. Submandibular (Submaxillary) gland. Locate the mixed secretory units consisting of a serous demilune capping a 4. Mixed secretory mucous acinus. units Also find the numerous serous cells organized as serous acini. Note the connective tissue septa and associated ducts and blood vessels. Human skin, Locate the sebaceous glands of the hair follicles. 5. Holocrine glands These are the only holocrine glands in the body. They are so called because the entire cell dies and bursts (Gr., holos, all) in order to release the fatty secretory product called sebum. B. Endocrine Glands In this endocrine gland the secreting cells are organized into follicles for storing their products. 1. Thyroid gland Locate the following: secretory cells, colloid-containing follicles, connective tissue capsule and trabeculae, blood vessels and capillaries. In this gland the secretory cells are organized into cords of varying morphology, depending on their location within the gland. 2. Adrenal gland Locate the following: secretory cells, connective tissue capsule, blood vessels, and capillaries (by the location of endothelial cell or connective tissue cell nuclei). Human pineal, 3. Pineal gland Note the capsule, connective tissue trabeculae, and large amounts of basophilic brain sand. C. Mixed Exocrine-Endocrine Gland (Compound Gland) Locate: exocrine serous acinar secretory units, endocrine islet cells, exocrine ducts, blood vessels and capillaries, and connective tissue (capsule, interlobular septa and interlobar septa). 1. Pancreas reveal the zymogen granules and the location of the Golgi apparatus in the exocrine cells of the pancreas. cells. Epidermal Glands Epidermal structures lying within dermis: Sebaceous glands: (alveolar, holocrine) • • • secrete an oil sebum into hair follicle, or on to skin surface (lips/eyes/genitals) oil protects against drying, and bacteria secreting cells die so gland is holocrine 30 The cell and tissue Sweat glands: (coiled tubular, all merocrine)[you will see them with the skin] i) merocrine: secrete hypotonic solution (mostly NaCl+ammonia, urea, lactic acid etc) via duct to skin surface. • • many on palms/soles, also on hairy skin (humans), but not around lips/genitals sweat cools by evaporation. Glands activated by heat, and emotional stress ii) apocrine: secrete sweat + scent into hair follicles, in genitals/armpits (BO!) • activity may indicate sexual maturity Mammary glands: (alveolar, merocrine) • • modified sweat glands + adipose tissue secrete milk (proteins/lactose/fat/etc) via raised nipple. Control:oxytocin/prolactin Mammary glands 31 The cell and tissue III. Connective tissues A. Structural features 1. widely spaced cells with abundant intercellular material called matrix. o major cell type - fibroblast o secretes matrix o immature, “sprout” o active cell “bud” • • • • • • Loose Connective (Areolar) Dense Fibrous (white fibrous) Hyaline Cartilage (Elastic & Fibrocartilage (no microscope work)) Adipose Bone (compact) Cross Section= CS Blood 2. matrix contains protein fibers embedded in amorphous ground substance. o o o collagen – “ropes” elastic – “rubber bands” c.t. fibers reticular – “hairnet” 3. highly vascular (except tendons and cartilage) 4. good nerve supply 32 The cell and tissue B. Functions o o Support Packing o Defense (inflammation, barrier to infection: note some pathogenic organisms produce hyaluronidase) o Transport (enclose vascular tissue) o Repair (wound repair) o o Storage (lipids, water, electrolytes) Energy storage (adipose – “fat”) GENERAL FEATURES OF CONNECTIVE TISSUES A. Functions: The functions of connective tissues, determined chiefly by their mechanical prop erties, include the binding together, compartmentalization , support, and physical and immu nologic protection of other tissues and organs, as well as storage B. Types: The connective tissues described in this chapter (III) are loose and dense collagenous connective tissue (connective tissue proper), reticular connective tissue, elastic connective tissue, and mucous connective tissue. Adipose tissue, cartilage, and bone are specialized con nective tissues. Blood, often considered a highly specialized type of connective tissue C. Three Fundamental Components: Connective tissue types differ in microscopic appear ance, but all consist of cells, fibers, and ground substance. Connective tissue types and subtypes are classified according to the amounts, types, and proportions of these components. D. Extracellular Matrix: The fibers and ground substance constitute the extracellular matrix. Connective tissues contain abundant matrix, which largely determines their mechanical proper ties. The fibers are of 2 types, collagen and elastic. The ground substance, in which the fibers and cells are embedded, is composed mainly of glycosaminoglycans (GAGs) dissolved in tissue fluid, Matrix viscosity and rigidity are determined by the amount and types of GAGs, the association of GAGs with core proteins to form proteoglycans, GAG-fiber associations, and GAGGAG associations. Fiber and ground substance components are synthesized and secreted by connective tissue cells (mainly fibroblasts), and the fibers are assembled in the extracellular space. E. Embryonic Origin: All connective tissue cell types derive from embryonic mesenchyme. Mesenchyme derives from embryonic mesoderm, except head mesenchyme, which derives from the neural crest (mesectoderm). 33 The cell and tissue Composition I. Ground Substance: Amorphous transparent and homogeneous gel matrix. A. Glycosaminoglycans: Polysaccharide component of ground substance. Composed of repeating disaccharide units (a hexosamine and a uronic acid) existing either as a single chain or linked to a core protein. • • Hyaluronic acid: A single, long chain of disaccharide units, usually glucuronic acid or iduronic acid linked to D-glucosamine or D-galactosamine. Found in synovial fluid, cartilage, vitreous humor. Proteoglycans: Molecules composed of disaccharide chains linked to a core protein molecule. They differ on the basis of the composition of sugars making up the disaccharide repeat unit. o o o o o • chondroitin sulfate: Cartilage, bone,cornea,skin,aorta,notochord. heparan sulfate: Aorta,lung,liver,basal lamina. dermatan sulfate: skin,tendon, aorta keratan sulfate: cornea,cartilage. Proteoglycan aggregates: Enormous molecules created by linking proteoglycans to a hyaluronic acid core by linker proteins. B. Glycoproteins:Fibronectin: A dimeric molecule with paired epitopes binding cell surface receptors, hyaluronic acid, heparin and collagen. Plays a role in cell-cell and cell-substrate attachments. Cancer cells do not synthesize fibronectin. Laminin: Found in basil lamina where it mediates epithelial cell adhesion to collagen. Chondronectin: Found in cartilage where it mediates attachment of chondrocytes to collagen (Type II). II. Protein Fibers: A. Collagen: Most abundant protein of the human body (30% of dry weight). Type I: Most abundant and widespread collagen. Type II: Found mostly in hyaline and elastic cartilage Type III: Makes up the collagenous component of reticular fibers. Type IV: Found in basal lamina underlying epithelial cells. Type VII: Connects the basal lamina to underlying lamina propria. Collagen Synthesis 1. Synthesis of collagen monomer (pre-procollagen) into RER. 34 The cell and tissue 2. Hydroxylation of proline and lysine while in RER. 3. Glycosylation of hydroxylysine (variable) and assembly into procollagen (triple helix) moleculer complex. 4. Export of procollagen. 5. Digestion of amino and carboxyl terminal domains by procollagen peptidase to form tropocollagen. 6. Fibril assembly and subsequent stabilization by lysyl oxidase. B. Reticular Fibers: Extremely thin fibers, mostly composed of collagen III, forming a reticular (mesh-like) network. Stained with silver salts or PAS staining. Support many cellularized organs such as glands, lymph nodes and the liver. C. Elastic fibers: Thin fibers or fenstrated sheets of elastin giving elastic properties to tissues which must return to their initial shape after deformation (lung,skin,bladder). o Elastic fibers develop by a three step pathway, first being generated as fine oxytalin fibers composed of fibrillin. o Elastin is added, forming elaunin fibers, and finally o Further addition of elastin and microfibrils generates mature elastic fibers. Connective Tissue Cells 35 The cell and tissue o Fibroblasts: Most common connective tissue cell type. Responsible for the synthesis collagen and glycosaminoglycans. Also involved in wound contraction and repair. o Fibrocyte: a mature or dormant fibroblast which can revert to fibroblast form when wounding occurs. Characterized by elongated "spindle" shape. o Macrophages: Large, long-lived phagocytotic cells whose major function is to ingest and destroy particulate matter. Characterized by an eccentric, lobed nucleus and granular cytoplasm. Major function is the injection of particulate material such as cellular debris. o Mast cells: Large cells with an extensive cytoplasm filled with large granules. These granules contain heparin , histamine and other compounds which are released during immune responses and cause tissue inflammation. o Plasma cells: Small cells responsible for antibody synthesis, characterized by an enlarged granular nucleus and basophilic cytoplasm. o Adipose cells: connective tissue cells specialized for fat storage. White adipose tissues contains cells consisting of a single large non-membrane bound lipid droplet and a displaced nucleus. Brown adipose tissue (also multilocular adipose tissue) is found in immature and hibernating mammals; its cells contain multiple membrane bound lipid vesicles. A white adipocyte has a single large lipid droplet; a brown adipocyte has many small droplets. Distribution: 1. Subcutaneous fat (hypodermis) is the layer of white adipose tissue found just beneath the skin except in the eyelids, penis, scrotum, and most of the external ear. (There is some fat in the earlobe.) In infants, it forms a thermal insulating layer of uniform thickness covering the entire body and is termed the panniculus adiposus, In adults it becomes thicker or thinner in selected areas, depending upon the person's age, sex, and dietary habits. Where it thins, it takes on the appearance of areolar tissue. In males, the fat layer thickens over the nape of the neck, deltoids (shoulders), triceps brachii (back of the upper arm), lumbosacral region (lower back), and buttocks. In females, additional fat is deposited in the breasts, buttocks, and hips and over the anterior aspect of the thighs. 2. Intraabdominal fat. Fat deposits of variable size surround blood and lymphatic vessels in the omentum and mesenteries suspended in the abdominal cavity. Additional accumulations occur in retroperitoneal areas, such as around the kidneys. 3. Other locations. Other prominent accumulations of fat are found within the eye orbits, surrounding major joints leg. knees), and forming pads in the palms and soles. Connective Tissue Cells ·fibro- 36 The cell and tissue · cells of fibrous connective tissues · elongated in direction of fibres chondro· cells of cartilage · often spherical or oval osteo· cells of bone · variable shape suffix denotes function/age of cell -blast cells create (build up) matrix -cyte cells maintain it -clast cells break it down (remodelling) eg fibroblast, chondrocyte, osteoclast Fibrous Connective Tissues Top Loose (areolar: L. small open space): • • • • • whitish, sticky: stretchy in all directions fine mesh of collagen/elastin/reticular fibres, with fluid-filled spaces cells include fibroblasts, macrophages forms loose packing, anchors skin, supports basement membranes, nerves can blend in with dense tissue or fat Dense (white): • • • • high proportion of large collagen/elastin fibres, so high tensile strength/elasticity cells mostly elongated fibroblasts Dense regular: fibres in 1 main direction eg tendon, ligaments, vocal cords Dense irregular: fibres in random mesh (or alternating layers with 1 direction in each) eg fascia, dermis, organ capsules 37 The cell and tissue Fibroblasts (large oval nucleus, large nucleolus, collagen-secreting) and fibrocytes (no collagen production) Chondroblasts (metabolically active, large nuclei and prominent nucleoli, L= lacuna= space due to fixation. Chondrocytes (smaller, dense nuclei, less cytoplasm, low activity) 38 The cell and tissue Loose (areolar) connective tissue: underlies basement membranes. Black lines label the cell nuclei (blue blob), broad collagen fibre (purple) and elastic fibre Dense regular collagenous connective tissue: elongated cell nuclei are shown. Special Connective Tissues o Adipose tissue (contains adipocytes): · cells store lipid (fat) for energy/heat regulation, and to cushion organs. Sparse matrix of reticular fibres. · white: large polygonal cells filled with one lipid drop; nucleus etc squashed against membrane; many mitochondria · brown: multiple lipid vesicles; nucleus unsquashed; brown pigments in many mitochondria; lot in 39 The cell and tissue armpits/shoulders o Reticular tissue: · fine r. fibres attached to r. cells. Also, dendritic cells, and blood/lymph cells · provides framework of lymph tissues, bone marrow and liver o Hemopoietic blood-forming tissue: · most in red bone marrow (yellow = fat) IV. Epithelial membrane = epithelium + c.t. (areolar) A. Mucous membranes (mucosa) 1. line cavities exposed to the exterior 2. epitheliumsecretes mucus 3. c.t. layer is called – lamina propria B. Serous membranes (serosa) 1. line cavities not exposed to the outside 2. epithelium forms a bag that secretes and contains small amounts of watery fluid 3. locations o pleura (2) – lungs o pericardium – heart o peritoneum – abdominopelvic cavity C. Cutaneous membrane = skin V. Muscle tissue [we will them in detail] VI. Nervous tissue [we will see this in detail] VII. Neuromuscular junction (NMJ) [we will see this in details] Epithelial Cells Specialized for Transport: [just a reading] 1. Ion-transporting cells. o o o o Some epitheiial cells are specialized for transcellular transport; ie. they can pump ions across their entire thickness, apex to base. Sheets of such cells form active barriers that control ion and waterconcentrations in body compartments. Tight junc tions are often found between the cells and appear to restrict backflow. Iontransporting cells typically have highly infolded basal plasma membranes that interdigitate with numerous mitochondria. Commonly, the ion pump is specific for sodium tie, it is Na/K+-ATPase), and chloride ions and water follow the sodium ion flow passively. 40 The cell and tissue o o Some ion-transporting epithelia exploit this mechanism to concentrate other solutes by moving water from one compartment to another. Important ion-transporting epithelia are found in the kidney tubules. the stnated ducts of the salivary glands, the gallbladder, the choroid plexus and the ciliary body of the eye. 2. Cells that transport by pinocytosis. o Epithelial cells specialized for pinocytosis have tight junctions and abundant pinocytotic o o vesicles. The vesicles transport substances across the cell from the luminal surface to the basal surface or vice versa. The best example is the endo thelial cells lining the blood vessels, where transcellular transport is rapid (2-3 minutes). Epithelial Cells Specialized for Absorption: Specialized absorptive cells lining the digestive tract (especially the small intestine) have numerous microvilli on their apical surfaces to increase the exposed area. Small nutrient molecules diffuse into the microvilli, and contraction of the microfilaments shortens the microvilli, bringing the nutrients into the cytoplasm. Other nutrients are pinocytosed between microvilli. Absorptive cells with similar specializations occur in the proximal tubules of the kidney. C. Epithelial Cells Specialized for Secretion: 1. Protein-secreting cells. Cells that synthesize proteins for segregation and secretion have abundant basophilic RER, a well-developed Golgi complex, and, frequently, an accumula tion of secretory granules in the cell apex. Proteins secreted by epithelial cells include the digestive enzymes, produced by pancreatic acinar cells and the chief cells of the stomach: serum albumin, produced by liver hepatocytes; and protein hormones leg, parathyroid hor mone, produced by the chief cells of the parathyroid gland). 2. Polypeptide-secreting cells. Secreted polypeptides have fewer amino acids than the secreted proteins just mentioned. Polypeptide-secreting cells have a small amount of RER, a supranuclear Golgi complex, and an accumulation of 100- to 400-nm secretory granules in their bases. These APUD cells (amine precursor uptake and decarboxylation) charac teristically concentrate important bioactive amines such as epinephrine, norepinephrine, and serotonin in their cytoplasm. They may absorb these amines from the bloodstream or synthe size them from amino acid precursors by means of amino acid decarboxylases, also found in high concentrations in these cells. Most APUD cells are unicellular glands scattered among other epithelial cells. They are believed to derive mainly from the embryonic neural crest. The number, variety, and wide distribution of cells with these characteristics has generated the concept of the diffuse neuroendocrine system (DNES~ DNES is becoming the pre ferred designation, but DNES and APUD refer to the same polypeptide-secreting cells. Some APUD polypeptides have paracrine effects on neighboring cells; others are released into the bloodstream and have endocrine effects on distant cells. Some important APUD polypeptides are glucagon, from pancreatic islet A cells: insulin. from pancreatic islet B cells; gastrin. from the stomach, small intestine, and pancreatic islet G cells; and somatostatin, from the stomach, small intestine, and pancreatic islet D cells. Tumors composed of APUD cells are called apudomas. 3. Mucous cells occur as unicellular, sheet, or solid glands. Histologic features include a light staining, foamy appearance caused by numerous large mucus-containing vesicles concen trated near the cell apex; PAS-positive staining from an abundance of oligosaccharide resi dues, predominantly acidophilic staining with H&E; a large supranuclear Golgi complex with distinctive glycosyltransferases (V.B.Z.a); and 41 The cell and tissue nuclei and sparse RER in the base of the cell. 4. Serous cells have characteristics of protein-secreting cells. They are usually smaller, darker staining, and more basophilic than mucus-secreting cells. Serous cells include pancreatic acinar cells and secretory cells of the parotid salivary glands. 5. Steroid-secreting cells. Endocrine cells specialized to secrete steroid hormones are polygo nal or rounded, with a central nucleus and pale-staining, acidophilic cytoplasm that often contains numerous lipid droplets. Their abundant SER contains enzymes for cholesterol synthesis and for converting steroid hormone precursors (eg, progesterone) into specific hormones leg, androgens, estrogens, and progesterone). Their mitochondria typically have tubular rather than shelflike cristae and contain enzymes that convert cholesterol to progesterone. Steroid hormones include testosterone, produced by interstitial cells of the testes: estrogen, from follicle cells of the ovaries; progesterone, from granulosa lutein cells of the corpus iuteum; and cortisone and aldosterone, from cells of the adrenal cortex. Loose Connective: Areolar 42 The cell and tissue ADIPOSE: Dense Regular Collagenous Connective 43 The cell and tissue Elastic Cartilage Adipose and Hyaline Cartilage 44 The cell and tissue 45 The cell and tissue A. General Connective Tissues - Comments Areolar connective tissue - intestinal mesentery. 1. Loose Mesentery. Mast cells, macrophages. 46 The cell and tissue 2. Dense Irregular 3. Dense Regular dermis of skin and connective tissue of the digestive tract. Elastic ligament. Tendons. B. Specialized Connective Tissues - Comments Elastic ligament. Elastic fibers appear as wavy, refractile lines embedded in a dense regular connective tissue. 1. Elastic wall of blood vessel - elastic fibers appear as refractile lines, best seen by stopping down the condensor diaphragm. Occurs abundantly; here can be seen around periphery of lymph nodes. H&E and Azure. 2. Adipose adipose tissue under the skin. White and brown adipose tissue White adipose tissue. 3. Reticular human lymph node showing reticular fibers as a fine black network. 4. Mucous Umbilical cord. C. Cells of the connective tissues Cell 1. Fibroblasts 2. Macrophages Comments Umbilical cord. Loose connective tissue. Liver, stained to show phagocytosis by macrophages. Mesentery. Macrophages can be visualized because they have phagocytized particles of India Ink. Don't confuse the black ink particles with the purple-stained granules of mast cells. Umbilical cord. About half of the connective tissue cells are macrophages, but they are difficult to distinguish from fibroblasts. 3. Mast cells Look for oval-shaped cells whose cytoplasm is filled 47 The cell and tissue with basophilic or metachromatic staining granules. 4. White fat cells Can be seen around the periphery of lymph nodes and under the skin 5. Eosinophils Best seen in the connective tissue of the villi of the small intestine, as well as in c.t. of oral cavity, esophagus, stomach and colon. 6. Plasma cells Can be found in loose connective tissue throughout the body, including the soft palate , the mammary gland , the intestines . 7. Lymphocytes Well seen in the connective tissue of the soft palate and of the small and large intestine. 8. Granulocytes Well seen in the blood vessels and connective tissue of the soft palate and of the small and large intestine. Seen in the co 48 The cell and tissue 49 The cell and tissue 50 The cell and tissue 51 The cell and tissue 52 The cell and tissue 53 The cell and tissue 54 The cell and tissue 55 The cell and tissue 56 The cell and tissue Content Review 1. All epithelia exhibit cellularity, polarity, attachment to underlying connective tissue, avascularity, innervation, and high regeneration capacity. 2. The basal lamina contains collagen fibers, as well as both protein and carbohydrate macromolecules that are secreted by the cells of the epithelium. Cells in the connective tissue underlying the epithelium secrete the reticular amina, which contains protein fibers and both protein and carbohydrate macromolecules. These laminae form the basement membrane, which strengthens the attachment and forms a molecular barrier between the epithelium and the connective tissue layers. 3. (a) Simple columnar epithelium lines the stomach lumen; (b) stratified squamous epithelium lines the oral cavity; (c) transitional epithelium lines the urinary bladder; and (d) simple squamous epithelium lines the tiny air sacs of the lungs. 4. (1) Merocrine secretion occurs when small secretory vesicles move to the apical surface of the cell and release their contents by exocytosis. (2) Holocrine secretion occurs when cells fill with an accumulated product and then the entire cell disintegrates, releasing both product and cell fragments. (3) Apocrine secretion occurs when the apical region of the cell pinches off, releasing some cellular fragments and product. 5. All connective tissues share a similar structural plan that includes (1) specific cells that produce (2) protein fibers to strengthen and support the connective tissue, and (3) a packing material called ground substance, within which the cells and protein fibers reside. Together the protein fibers and ground substance form an extracellular matrix. 6. In dense regular connective tissue, collagen fibers are packed tightly and aligned parallel to applied forces. In dense irregular connective tissue, collagen fibers form a scattered meshwork in which individual bundles of fibers extend in all directions. 7. Hyaline cartilage is found in the nose, trachea, larynx (voice box), costal cartilage (the cartilage attached to the ribs), particular ends of long bones, and the fetal skeleton. Hyaline cartilage functions primarily to support soft tissue; it also forms most of the fetal skeleton and thus functions as a model for future bone growth. Fibrocartilage resists compression and is a good shock absorber. It is found in the intervertebral discs, the pubic symphysis, and the menisci of the knee joint. Elastic cartilage is extremely resilient and flexible. It is found within the epiglottis and in the external ear. 8. The four types of body membranes are mucous membranes, which line body passageways, as in the digestive, respiratory, reproductive, and urinary systems; serous membranes, which line body cavities (the parietal layer) and cover organs (the visceral layer); a cutaneous membrane, commonly called the skin and composed of epidermis and dermis; and a synovial membrane, which lines some joints of the skeletal system. 9. Intercalated discs are strong gap junctions between neighboring cardiac muscle cells. They permit the rapid transport of an electrical stimulus (muscle impulse) through many cardiac muscle cells at once, allowing the entire muscle wall to contract as a unit. 10. Skeletal muscle tissue is composed of long, cylindrical, thin muscle cells that often have more than one nucleus. Skeletal muscle cells are striated, attached to the skeleton, and voluntary. Cardiac muscle tissue is confined to the heart wall; its cells are often shorter than skeletal muscle cells, but they are striated like skeletal muscle cells. Cardiac muscle cells are usually branched, and they contain only one or two centrally located nuclei. Cardiac muscle cells are connected by intercalated discs, which are strong gap junctions between the cells. Smooth muscle tissue lacks striations and is involuntary. Smooth muscle is sometimes called visceral muscle because it is found in the walls of most viscera (organs), such as the stomach, urinary bladder, and blood vessels. Its contraction helps propel material. 1. 2. 3. 4. 5. Regeneration ensures the continued repair and renewal of the epithelium. Basal lamina is produced by secretions of the epithelial cells. Reticular lamina is produced by secretions of the cells in the underlying connective tissue. The tight junction (zonula occludens) ensures that epithelial cells act as “gatekeepers.” Desmosomes provide resistance to mechanical stress at a single point. Epithelial tissues are classified according to the number of cell layers and the shape of the 57 The cell and tissue 6. 7. 8. 9. 10. 11. 12. 13. 14. 15. 16. 17. 18. 19. 20. 21. 22. 23. 24. cell at the apical surface. A simple squamous epithelium is the thinnest and occurs in areas where maximum filtration and diffusion are needed. A pseudostratified epithelium looks multilayered, or stratified, because the cells’ nuclei are distributed at different levels between the apical and basal surfaces. However, although all of these epithelial cells are attached to the basement membrane, some of the cells do not reach its apical surface. A transitional epithelium exhibits a variable appearance, depending on whether it is relaxed or stretched (distended). This epithelium lines the urinary bladder, an organ that changes shape as it fills with urine. Secretions of endocrine glands are called hormones. Exocrine glands originate from an invagination of epithelium that burrows into the deeper connective tissues. These glands maintain their contact with the epithelial surface through a duct. Multicellular exocrine glands contain both a secretory portion and a conducting portion. Because each secretory cell is destroyed during holocrine secretion, the ruptured, dead cells are replaced by regeneration. Extracellular matrix is a nonliving material produced by and surrounding connective tissue cells. Protein fibers and ground substance are the components of the extracellular matrix. Connective tissue functions include physical protection, support and structural framework, binding of structures, storage, transport, and immune protection. The three categories of connective tissue are connective tissue proper, supporting connective tissue, and fluid connective tissue. Collagen fibers, elastic fibers, and reticular fibers make up connective tissue proper. Loose connective tissue has a scattered distribution of fibers that are in relatively low concentration; its primary is ground substance. Dense connective tissue has extensively distributed fibers, which are its primary component. Ground substance is sparse in dense connective tissue. The two forms of bone tissue are spongy bone and compact bone. Mucous membranes function in absorption, protection, and secretion. The parietal layer of a serous membrane lines the body cavity, and the visceral layer covers organs. Skeletal muscle tissue has long, cylindrical, multinucleated cells with obvious striations. Intercalated discs facilitate rapid transmission of impulses for cardiac muscle contraction. We do not have voluntary control over smooth muscle. Glial cells are the supporting cells in nervous tissue. 58