* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The Advanced Cardiovascular Life Support Guidelines
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Jatene procedure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Electrocardiography wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Transcript
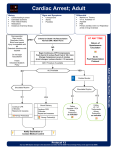
January 2013 • Volume 27 • Number 1 Lesson 2 The Advanced Cardiovascular Life Support Guidelines Sharon E. Mace, MD, FACEP, FAAP ■Objectives On completion of this lesson, you should be able to: 1. Describe the treatment of adult patients in cardiac arrest recommended in the 2010 American Heart Association (AHA) basic life support guidelines. 2. Explain the appropriate management of patients based on the AHA’s new adult advanced cardiovascular life support algorithms, including drug therapy. 3. Discuss the rationale for “handsonly” cardiopulmonary resuscitation. 4. Explain the appropriate electrical therapy for various dysrhythmias, including ventricular fibrillation, ventricular tachycardia, atrial fibrillation, atrial flutter, and others. 5. Describe the key principles in post–cardiac arrest management, including hypothermia, titration of supplemental oxygen (to avoid hyperoxemia), and use of quantitative capnography. 6. Communicate the principles of systems of care for patients with ST-segment elevation myocardial infarction. ■From the EM Model 3.0 Cardiovascular Disorders 3.1 Cardiopulmonary Arrest The cornerstone of resuscitation in patients of any age is high-quality cardiopulmonary resuscitation (CPR), with an emphasis on chest compressions. This lesson will summarize the key points in the American Heart Association’s (AHA’s) guidelines for advanced cardiovascular life support (ACLS), including electrical therapy, pharmacology, airway, and postresuscitation care, while reiterating the essentials of basic life support (BLS) that provide the foundation for ACLS. Case Presentations ■ Case One Paramedics are called to the home of a 65-year-old woman. She had been sitting on the porch talking with her neighbors when she became unresponsive. The neighbor gently placed her on the firm surface of the porch and found her unresponsive with gasping respirations. One of the neighbors began performing “handsonly” CPR, while his wife called 911. The neighbor began chest compressions within 10 seconds of recognizing the arrest. His compression rate was at least 100/ minute. He completed a complete cycle of 30 compressions in less than 18 seconds. His compression depth was at least 2 inches (5 mm). He allowed for complete chest recoil after each chest compression. When the paramedics arrived, the monitor defibrillator showed ventricular fibrillation (VF), so one shock was given at 200 J because this was a biphasic defibrillator and the manufacturer’s recommended dose was unknown. Chest compressions were continued for 2 minutes, and an intravenous line was placed. The monitor still indicated VF, so another shock was given. Chest compressions were continued for 2 minutes, during which time 1 mg of epinephrine was administered via the intravenous line. The monitor rhythm was still VF, so another shock was given. Chest compressions were resumed, and a 300-mg IV bolus of amiodarone was administered. Without interrupting CPR (eg, chest compressions), paramedics intubated the patient on the way to the hospital. On arrival in the emergency department, waveform capnography was applied and indicated that the endotracheal (ET) tube was in appropriate position with good CPR/chest compressions in progress. The monitor revealed asystole, so epinephrine, 1 mg IV, was given since it had been 3 minutes since the last dose. Reversible causes of her arrest were considered: she was intubated with the ET tube in good position, on 100% Fio2, and arterial blood gas was drawn to check for acidosis and hypoxia. A normal saline (NS) bolus was administered to treat hypovolemia. The breath sounds were equal bilaterally, and there was no tracheal deviation or jugular venous distention, so a tension pneumothorax was ruled out. A bedside echocardiogram showed absent wall motion consistent with 11 Critical Decisions in Emergency Medicine Critical Decisions • How have the American Heart Association’s (AHA’s) basic life support guidelines changed when compared to the previous guidelines? • What is “hands-only” CPR, and what is the science behind this recommendation? • What are the differences regarding the new airway and breathing recommendations compared to previous recommendations? • What are the new pharmacology recommendations in the ACLS protocols? • What suggestions have been made regarding postresuscitation care? • What do the AHA guidelines recommend regarding devices and CPR techniques? • What do the AHA guidelines recommend regarding systems of care? • What are the new guidelines for electrical therapy? a myocardial infarction, and her cardiac enzymes were elevated. She had return of spontaneous circulation (ROSC). ■ Case Two A 45-year-old man presents with chest pain that began 1 hour ago. He has no allergies and is on no medications; his past medical history is negative. Vital signs are blood pressure 120/80, pulse rate 80 and regular, respiratory rate 20, and pulse oximetry 99% on room air. The nurse asks if she should put the patient on oxygen and give morphine for his pain. The physician asks the nurse to get an ECG; start an intravenous line; draw blood, including cardiac enzymes; and place the patient on a monitor. Supplemental oxygen is not started because the patient has a normal pulse oxygen saturation. Aspirin, 325 mg, and a sublingual nitroglycerin are ordered for his chest pain instead of the morphine because the physician recalls a study in a large registry showing increased mortality rates with morphine use. The patient’s initial ECG is unremarkable. His chest pain resolves, but enzymes are positive, so the physician calls for a cardiology consultation. A short time later, the patient again complains of chest pain, and he has become pale and sweaty and is now confused. His blood pressure is 65/35 and heart rate is 30. The monitor shows a complete heart block. The 12 physician immediately gives atropine, 0.5 mg IV bolus, and asks the nurse to prepare an epinephrine infusion. The patient is still hypotensive and bradycardic so a second dose of atropine is given 3 minutes after the first dose; an epinephrine infusion is started at 5 mcg/minute, and preparations are made for transcutaneous pacing. ■ Case Three A 50-year-old woman presents with palpitations. Her past medical history is negative. She is on no medications and has no allergies. Vital signs are blood pressure 130/80, pulse rate 180, respiratory rate 16, and pulse oxygen saturation 97% on room air. She is placed on a monitor, and an intravenous line is started. Her ECG shows a wide QRS (≥12 seconds) and indicates that her tachycardia is regular and monomorphic, so adenosine, 6 mg rapid IV push, is given. Her heart rate and blood pressure remain unchanged, so adenosine, 12 mg rapid IV push, is administered. There is no response, so the physician asks the nurse to see what antiarrhythmic infusions are available, and a cardiology consultation is requested. The nurse reports that sotalol (dose 100 mg or 1.5 mg/kg up to 100 mg over 5 minutes), procainamide (20-50 mg/ min), and amiodarone (150 mg over 10 minutes) are immediately available from the department’s automated medication dispensing system. Because of concern for heart failure and because the patient’s QT is prolonged, procainamide is not given. The prolonged QT also makes sotalol a poor choice. Amiodarone, 150 mg over 10 minutes, is given. Unfortunately, she does not respond but instead becomes unresponsive, with a blood pressure of 65/35. Synchronized cardioversion at 100 J is attempted because the patient’s rhythm is wide-complex regular. CRITICAL DECISION How have the AHA’s basic life support guidelines changed compared to the previous guidelines? The 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular care stress the importance of high-quality CPR with a focus on high-quality chest compressions. Thus, there is a fundamental shift from the previous airway-breathing-chest compressions, or A-B-C, to chest compressionsairway-breathing, C-A-B.1-5 With this new focus, there is a change in the sequence of steps in basic life support. The current recommended sequence is, first check responsiveness and breathing, next call for help and get the automatic external defibrillator (AED), then check the pulse and give chest compressions. After chest compressions, open the airway and give two rescue breaths, then resume January 2013 • Volume 27 • Number 1 compressions. In the new 2010 guidelines, chest compressions come before the two rescue breaths1-5 (Table 1, Figure 1). Science Behind the New Guidelines: C-A-B versus A-B-C The rationale for the new BLS guidelines includes the fact that the overwhelming number of cardiac arrests occur in adults and the highest cardiac arrest survival rates in all patients occur with a witnessed arrest and with ventricular fibrillation (VF) or pulseless ventricular tachycardia (VT) as the initial rhythm. Chest compressions and early defibrillation are the key initial elements of BLS in these patients. The goal of C-A-B is to begin chest compression as soon as possible. With A-B-C, chest compressions not only occur later in the BLS sequence but also are frequently delayed further while the rescuer attends to the airway (retrieving a barrier device or other airway/ventilation equipment and while opening the airway and giving rescue breaths). However, even with the change to C-A-B, there should only be a minimal delay in ventilation: specifically, the time needed to deliver the first cycle of 30 chest compressions for one rescuer (about 18 seconds). Unfortunately, most out-of-hospital cardiac arrest victims do not receive any bystander CPR. Several factors may contribute to this low rate of bystander CPR. Chest compressions are easier to perform than opening the airway and delivering rescue breaths. Starting with the easier procedures (eg, chest compressions instead of airway) may encourage more bystanders to initiate CPR. CRITICAL DECISION What is “hands-only” CPR, and what is the science behind this recommendation? For those who are not trained in CPR, the new guidelines allow the untrained bystander to provide “hands-only” (or “compressiononly”) CPR for the adult with sudden collapse.6,7 The bystander rescuer should continue hands-only CPR until an AED is ready for use or until other rescuers can assume care of the collapsed victim. If the trained lay rescuer can perform rescue breathing, the ratio remains 30 compressions to two breaths (the same as in the 2005 guidelines). Science Behind the New “HandsOnly” CPR There are several reasons for “hands-only” CPR. Survival rates for cardiac arrest from a cardiac etiology are similar whether “hands-only” CPR or CPR with compressions and rescue breaths is done. “Hands-only” CPR is easier for an untrained rescuer to perform. It is also easier for an emergency medical dispatcher to provide instructions for “hands-only” CPR. If the rescuer is hesitant about starting CPR because of a concern about potential transmission of an infection or potential contact with secretions or vomitus, hands-only CPR should allay this fear. It should be noted, however, that if the trained rescuer is able, he/she should perform both compressions and ventilations. Chest Compressions The new parameters for adult chest compressions are: depth at least 2 inches (5 cm) (the 2005 compression depth for adults was 1½ to 2 inches) and compression rate “at least 100/ minute” (compared with the previous of “about 100/minute”). The goal is to “push hard and push fast” and to begin compressions within 10 seconds of recognizing the arrest. The 2010 recommendation is that chest compressions should be completed in less than 18 seconds; the 2005 guidelines recommended they be done in less than 23 seconds. Deeper and faster compressions are essential in order to generate the pressure needed to perfuse the coronary and cerebral arteries. Table 1. Summary of 2010 BLS recommendations Order of CPR CPR sequence “Look-listen-feel” Check for breathing Ratio for 1-rescuer CPR for all patients Initiation of CPR Compression depths (adults) Compression rate (adults) Chest compressions completed 2010 Guidelines Chest compressions first Chest compressions-airway-breathing (C-A-B) Omitted as a distinct step in BLS 2005 Guidelines Airway first Airway-breathing-circulation (A-B-C) Part of step 1, occurs when rescuer checks for responsiveness 30 compressions:2 breaths “Look-listen-feel” occurred after opening airway Occurs after opening airway; is a separate, distinct step 30 compressions:2 breaths Within 10 seconds of recognition of arrest At least 2 inches (5 cm) At least 100/minute Within 18 seconds 1½ to 2 inches About 100/minute Within 23 seconds 13 Critical Decisions in Emergency Medicine Figure 1. Adult cardiac arrest algorithm. From: Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S736. Used with permission from the American Heart Association. 14 January 2013 • Volume 27 • Number 1 CRITICAL DECISION What are the differences regarding the new airway and breathing recommendations compared to the previous recommendations? With the prior BLS guidelines, airway and breathing came before chest compressions; now this is reversed. Previously, “look, listen, and feel” was a distinct step in the BLS sequence that occurred after opening the airway. Now “look, listen, and feel” is deleted as a step in BLS and instead has become part of step 1. Step 1 is to check breathing when you check responsiveness as a part of the first action in the BLS sequence.1-4 With the advanced airway protocols, cricoid pressure (Sellick maneuver) is an option and is no longer mandatory and end-tidal carbon dioxide monitoring is recommended in adults not only to confirm appropriate ET tube placement but also to monitor CPR quality and detect ROSC.8,9 for this.8-10 Aspiration can occur even if the Sellick maneuver is used. It is difficult to teach and to learn the correct application of the Sellick maneuver. Indeed, studies have shown that cricoid pressure is frequently misapplied even by trained health care providers.10 There have been multiple reports of cricoid pressure actually impeding passage of the ET tube during intubation.10 Science Behind the Guidelines: Airway Cricoid pressure during intubation/ventilation is no longer routine.8,9 There are many reasons Table 2. Electrical therapy Synchronized Cardioversion Atrial fibrillation (initial) Atrial flutter (initial) Ventricular tachycardia stable monomorphic (initial) Defibrillation (unsynchronized shock) Sequence: Dose: Ventricular fibrillation (VF) or pulseless ventricular tachycardia Pediatric defibrillation Ventricular fibrillation (for in-hospital monitored patients with sudden cardiac arrest) AEDs Chain of survival Use in hospitals Infants Defibrillation with implantable cardioverter-defibrillator AED pad placement 2010 Guidelines 2005 Guidelines 200 J monophasic 120 – 200 J biphasic 50 J (monophasic or biphasic) 100 J (monophasic or biphasic) 100 – 200 J monophasic 1-shock sequence Escalating doses for second and subsequent shocks 200 J (monophasic) Biphasic (use manufacturers recommended energy dose, 120 – 200 J) 2-4 J/kg initial ≥4 J/kg subsequent (consider higher doses) Maximum is 10 J/kg or adult dose For inhospital sudden cardiac arrest, in monitored patients the time from VF to shock delivery should be <3 minutes 3-shock sequence Fixed doses for second and subsequent shocks Integration of AEDs into chain of survival for public places Consider use of AEDs in hospitals May be used in infants if manual defibrillator is not available Consider plading pads or paddles directly over implanted device so pad or paddle placement does not delay defibrillation May use any of four pad positions: anterolateral (sternal-apical) is reasonable default, anteroposterior, anterior left infrascapular, anterior right infrascapular 2 J/kg initial 4 J/kg subsequent (monophasic or biphasic) No recommendations Position the pad at least 1 inch (2.5 cm) away from the device 1 position, anterolateral (sternal-apical) 15 Critical Decisions in Emergency Medicine CRITICAL DECISION What are the new guidelines for electrical therapy? There are many changes to the recommendations for electrical therapy11 (Table 2). There is now a 1-shock instead of a 3-shock protocol for unsynchronized shocks for defibrillation, and escalating energy doses are recommended for the second and subsequent shocks. The 2005 guidelines called for fixed doses for the second and subsequent shocks. In synchronized cardioversion, the initial dose for patients in atrial fibrillation now depends on whether the defibrillator is monophasic (200 J) or biphasic (120-200 J); for atrial flutter the recommended initial dose is 50 J, and for stable monomorphic VT the recommended dose is 100 J. For VF, the defibrillation dose now depends on the defibrillator manufacturer’s recommended dose and on whether the device is monophasic (200 J) or biphasic (120200 J). For pediatric defibrillation, higher doses are in the current guidelines. Previously, 2 J/kg was the initial recommended dose, with 4 J/kg recommended for subsequent doses, whether the device was monophasic or biphasic. The new guidelines are 2 to 4 J/kg for the initial dose, and 4 J/kg or more for subsequent doses, with higher doses considered with a maximum of 10 J/kg or the adult dose. For defibrillation in a patient who has an automated implantable cardioverter defibrillator (AICD), the prior guidelines suggested positioning the pad at least 1 inch (2.5 cm) away from the device. In order to try to prevent any delay in beginning chest compressions, it is now acceptable to place pads or paddles directly over implanted devices. There are changes to guidelines for AED use, as well. AEDs should be integrated into the chain of survival in public places. Their use should be considered in hospitals. AEDs can now be used in infants (age <1 year) if a manual defibrillator is not available. There are four acceptable pad positions now, instead of just one: anterolateral, anteroposterior, anterior-left infrascapular, and anterior-right infrascapular (Table 2). CRITICAL DECISION What are the new pharmacology recommendations for the ACLS protocols? The 2010 guidelines list fewer indications than in the past for the use of lidocaine, magnesium, calcium, bicarbonate, and atropine8,9 (Table 3). Atropine is no longer recommended for routine use in pulseless electrical activity/ asystole, but it is still included in the bradycardia algorithm. Lidocaine and magnesium are no longer routinely recommended for use in VF/pulseless VT. Magnesium is indicated with documented hypomagnesemia and torsade de pointes. Neither calcium nor bicarbonate is recommended for routine use in cardiac arrest except under certain circumstances. Calcium is indicated for hypocalcemia, hyperkalemia, hypermagnesemia, and calcium channel blocker overdose. Sodium bicarbonate can be used for hyperkalemia or sodium Table 3. Pharmacology and adult ACLS algorithms: 2010 Guidelines Rhythm VT cardiac arrest (Figure 1) Drug Epinephrine Amiodarone Vasopressin Pulseless electrical activity (PEA) asystole Epinephrine Bradycardia (Figure 3) Tachycardia (stable, regular rhythm) (Figure 2) Stable wide QRS tachycardia (Figure 2) Vasopressin Atropine Dopamine infusion Epinephrine infusion Adenosine Amiodarone Procainamide Sotalol 16 Dose 1 mg IV/IO every 3-5 min 300 mg IV/IO first dose; 150 mg IV/IO second dose 40 units IV/IO (can replace first or second dose of epinephrine) 1 mg IV/IO every 3-5 min 40 units, can replace first or second dose of epinephrine 0.5 mg bolus IV, repeated every 3 minutes (maximum 3 mg) 2-10 mcg/kg/min 2-10 mcg/min 6 mg rapid IV push followed with normal saline flush, second dose 12 mg if needed 150 mg IV over 10 minutes, repeat as needed if VT recurs, follow by maintenance infusion of 1 mg/min for first 6 hours) 20-50 mg/kg until arrhythmia suppressed, hypotension ensues, QRS duration increases >50%, or maximum dose of 17 mg/kg given Avoid if prolonged QT or CHF, maintenance infusion 1-4 mg/min 100 mg (1.5 mg/kg) over 5 minutes; avoid if prolonged QT January 2013 • Volume 27 • Number 1 channel blocker toxicity. There is also a caution not to routinely use amiodarone and procainamide simultaneously. Previously recommend only for suspected regular narrow complex reentry supraventricular tachycardia, adenosine is now recommended for the initial diagnosis and treatment of stable, undifferentiated regular monomorphic wide complex tachycardia. However, adenosine should not be used for irregular widecomplex tachycardia because it can precipitate VF (Figure 2). The 2010 guidelines allow chronotropic drug infusions as an alternative to pacing. The previous guidelines recommended that they be given only after atropine and if transcutaneous pacing failed (Figure 3). CRITICAL DECISION What suggestions have been made regarding postresuscitation care? Post–cardiac arrest care requires a “comprehensive, structured, integrated, multidisciplinary system of care that includes cardiopulmonary and neurologic support.” Favorable outcomes have been reported with percutaneous coronary interventions (PCI) in adult patients resuscitated from cardiac arrest.12,13 Thus, cardiac catheterization should be considered in post–cardiac arrest protocols, and coma is not a contraindication. Coronary angiography may be indicated after ROSC in patients whose arrest is likely due to ischemic cardiac disease, even in Pearls • Use out-of-hospital 12-lead ECGs to reduce time to reperfusion with fibrinolytic therapy. • Use a 1-shock instead of a 3-shock sequence for ventricular fibrillation (VF). • Use escalating instead of fixed doses for the second and subsequent shocks. • Omit atropine from the advanced cardiovascular life support (ACLS) cardiac arrest algorithm. • Use morphine with caution in patients with unstable angina/non-STEMI. • Use quantitative waveform capnography for monitoring CPR quality and detecting ROSC based on end-tidal carbon dioxide values. • Include AEDs in the adult chain-of-survival system for public places, and consider their use in the hospital. Pitfalls • Failing to provide high-quality, basic CPR, especially high-quality chest compressions, which are the foundation for ACLS. • Focusing on ventilation instead of high-quality chest compressions. • Relying on drugs and devices while minimizing the importance of chest compressions and BLS measures. • Failing to titrate the use of supplemental oxygen in postresuscitation care. • Failing to use morphine with caution and using morphine as a first-line drug (instead of nitrates) for patients with ACS. • Failing to implement comprehensive care for patients after cardiac arrest with STEMI or suspected ACS, which may include PCI. • Failing to institute systems of care for patients with STEMI in order to improve outcome for STEMI patients. the absence of a STEMI because the ECG can be insensitive or even misleading following cardiac arrest. Recommendations new to the 2010 guidelines are to transfer patients to a facility with a comprehensive post–cardiac arrest treatment system of care, identify/treat reversible causes including acute coronary syndrome (which may include PCI), control temperature to optimize neurologic recovery, and anticipate, treat, and prevent multiple organ dysfunction (which includes avoiding excessive ventilation and hyperoxia and considering hypothermia). CRITICAL DECISION What do the AHA guidelines recommend regarding devices and techniques? The precordial thump may be used for patients with witnessed, monitored, unstable VT if a defibrillator is not immediately ready for use14 (Table 4). Continuous waveform capnography should be used for intubated patients in the periarrest period and is useful for confirming ET tube placement in adults, monitoring CPR quality, and detecting ROSC in adults based on end-tidal carbon dioxide. CPR techniques have been designed to increase perfusion during resuscitation from cardiac arrest and to increase survival. In certain situations when used by well-trained providers, some alternative CPR techniques may improve hemodynamics/short-term survival, but not long-term survival.6 Furthermore, these alternative CPR techniques generally require additional equipment, training, and personnel and often can only be used in a specific setting.6 “To date, no CPR device has consistently been shown to be superior to standard conventional (manual) CPR for outof-hospital BLS, and no device other than a defibrillator has consistently improved long-term survival for outof-hospital cardiac arrest.”6 17 Critical Decisions in Emergency Medicine Table 4. CPR techniques and devices Continuous waveform capnography Precordial thump CPR devices impedance threshold device Load-distributing band CPR (auto-pulse) New 2010 Guidelines Recommended for intubated patients in peri-arrest period In adults, confirms ET tube placement, detects ROSC, and monitors CPR quality Consider if: witnessed, monitored unstable VT if defibrillator is not immediately ready for use Improved ROSC/short-term survival but no improvement in long-term survival No improvement in 4-hour survival Worse neurologic outcome when used Figure 2. Adult tachycardia algorithm. From: Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S751. Used with permission from the American Heart Association. 18 January 2013 • Volume 27 • Number 1 CRITICAL DECISIONS What do the AHA guidelines recommend regarding systems of care? Optimal management of STEMI care requires integration of community, EMS, physician, and hospital resources in a well-organized, coordinated, system-wide approach to care. Components of such a systemic approach to care can involve public awareness/education regarding the symptoms of acute coronary syndrome (ACS), dispatch instructions, EMS protocols, out-ofhospital 12-lead ECGs, emergency department and hospital programs, and intrafacility systems of care and interfacility transfer agreements, where appropriate. Out-of-hospital ECGs can reduce the time to PCI and streamline triage to specific hospitals when PCI is the therapy of choice. Positive outcomes have occurred in adults resuscitated from cardiac arrest who have undergone PCI. Emergency angiography with revascularization of the infarct-related artery in patients with out-of-hospital cardiac arrest is one of the 2010 recommendations. The following should be noted: 1) the ECG may be insensitive or misleading after cardiac arrest, 2) coronary angiography after ROSC in patients with arrest of presumed cardiac etiology may be reasonable, even in the absence of a clearly defined STEMI, and 3) coma is frequently seen after outof-hospital cardiac arrest and is not a contraindication to immediate angiography and PCI. artery is recommended in patients with out-of-hospital cardiac arrest from VF. A stent was placed in the cardiac catheterization lab, and the patient woke up after the procedure, did well, and was discharged home 4 days later, neurologically intact. ■ Case Two The 45-year-old patient with complete heart block was sent to the cardiac ICU. A pacemaker was inserted. The patient did well and was sent home 3 days later with the diagnosis of complete heart block, status post-pacemaker placement, and non-STEMI. ■ Case Three After the synchronized cardioversion, the tachycardic patient with a widened QRS awakened. Her heart rate was 84, and blood pressure was 130/80; she was responding appropriately to verbal stimuli. The cardiologist arrived and noted that the patient had been scheduled for a cardiac ablation in 2 weeks for recurrent supraventricular tachycardia. She was admitted to the cardiac ICU, and a successful ablation was done. She was discharged home in sinus rhythm 1 day later. Summary Although airway and breathing are still important, the emphasis in the 2010 AHA guidelines is on Figure 3. Adult bradycardia algorithm. From: Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S749. Used with permission from the American Heart Association. Case Resolutions ■ Case One In the case of the woman who had a witnessed arrest and received immediate by-stander CPR, although she was comatose and had a nondiagnostic ECG, she was taken to the cardiac catheterization laboratory for emergent angiography. According to the ACLS guidelines, emergent angiography with prompt revascularization of the infarct-related 19 Critical Decisions in Emergency Medicine high-quality CPR—especially highquality chest compressions. A major change is from airway-breathingchest compressions (A-B-C) to chest compressions-airway-breathing (C-A-B); chest compressions should be started before attention to airway and breathing. Recommendations for electrical therapy have been modified and include a 1-shock protocol versus 3-shock sequence for VF. Some of the changes in pharmacology include elimination of atropine from the PEA/ asystole algorithm and elimination of lidocaine from the VF/pulseless VT algorithm. There are also new sections on post–cardiac arrest care and stroke care that focus on organized systems of care with a goal of improving functional outcome. References 1. Field JM, Hazinski MF, Sayre MR, et al. Part 1: Executive Summary 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S640-S656. 2. Tavers AH, Rea TD, Bobrow BJ, et al. Part 4: CPR Overview: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S676-S684. 3. Berg RA, Hemphill R, Abella BS, et al. Part 5: adult basic life support: 2010 American Heart Association Guidelines for Cardiovascular Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S685-S705. 4. Berg MD, Schexnayder SM, Chameides L, et al. Part 13: pediatric basic life support: 2010 American Heart Association Guidelines for Cardiovascular Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S862-S875. 5. Mace SE. Essentials of pediatric basic and advanced cardiac life support. In: Fuchs S, Yamamoto L, eds. APLS: The Pediatric Emergency Medicine Resource. 5th ed. Elk Grove Village, IL, Dallas, TX: American Academy of Pediatrics, American College of Emergency Physicians; 2011. 6. Field JM, Hazinski MF, Sayre MR, et al. Part 1: executive summary: 2010 American Heart Association Guidelines for CPR/ECC. Circulation. 2010;122:S639. 7. Science Update: Guidelines CPR/ECC 2010. American Heart Association Guidelines CPR/ECC 2010 Instructor Conference, Chicago, IL November 12, 2010. 8. Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S729-S767. 9. Kleinman ME, Chameides L, Schexnayder SM, et al. Part 14: pediatric advanced life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122:S876-S908. 10. Mace SE. Challenges and advances in intubation: airway evaluation and controversies with intubation. Emerg Med Clin North Am. 2008;26(4):977-1000, ix. 11. Link MS, Atkins DL, Passman RS, et al. Part 6: electrical therapies: automatic external defibrillators, defibrillation, cardioversion, and pacing: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S706-S719. 20 12. Peberdy MA, Callaway CW, Neumar RW, et al. Part 9: post–cardiac arrest care: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122:S768-S876. 13. O’Connor RE, Brady W, Brooks SC, et al. Part 10: acute coronary syndromes: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S787-S817. 14. Cave DM, Gazmuri RJ, Otto CW, et al. Part 7: CPR techniques and devices: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S720-S728.