* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Daily Report 09-14-2016
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Pericardial heart valves wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Electrocardiography wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiac surgery wikipedia , lookup
Transcript
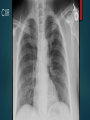
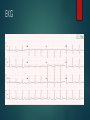
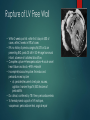
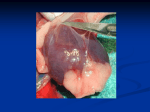
Daily Report September 14, 2016 MARIN MCCUTCHEON, PGY-2 OLIVE VIEW MEDICAL CENTER 43 yo F who presents with chest pain Discussion: HPI HPI Sharp pinching pain and pressure in left chest Onset in am while at work (cleaning houses) Constant Worse with deep inspiration Improved with Nitro Does not radiate Associated with dyspnea, worse with lying down and better when sitting up DOE with pinching sensation in chest Reports angiography at OSH, adherent to all meds including clopidogrel Sxs are similar to MI but not as intense PMH/PSH CKD stage II 2/2 PCKD HTN No surgeries Medications Clopidogrel 75mg daily Atorvastatin 40mg nightly MTP 25mg PO BID ASA 81mg daily HCTZ 12.5mg daily Losartan 25mg PO BID Discussion: Differential Physical Exam VS: 36.7 HR 69 BP 157/94 RR 18 100% on RA Gen: NAD HEENT: NCAT, PERRLA, EOMI, OP clear CV: RRR, nl S1 S2 no MRG Lungs: CTAB, no WRR Abd: soft NTND, +BS, no guarding Ext: WWP, trace edema BLE, +2 distal pulses Neuro: A+Ox4, CN 2-12 intact, motor 5/5 throughout, sensation grossly intact Discussion: Orders Labs WBC 12.4 / Hgb 12.9 / Plt 195 Na 138 / K 3.0 / 103 / 28 / BUN 18/ Cr 0.88 Trop <0.010 x 3 ESR 16 CXR EKG TTE Summary: 1. Left ventricle: Systolic function is normal. The estimated ejection fraction is 60-65%. Wall motion is normal; there are no regional wall motion abnormalities. 2. No significant valvular disease. 3. Pulmonary arteries: Systolic pressure is mildly increased, estimated to be 37 mm Hg. Discussion: Post-MI complication MKSAP Question An 82-year-old man was admitted to the coronary care unit (CCU) 48 hours ago after a late presentation with anterior ST-elevation myocardial infarction. The patient underwent coronary angiography and was found to have an occluded proximal left anterior descending coronary artery but did not undergo an attempt at revascularization at the time of coronary angiography because of his late presentation and symptomatic improvement. Today, he felt faint and lost consciousness while visiting with his family in the CCU. On physical examination, blood pressure is 72/54 mm Hg and pulse rate is 108/min. Cardiac examination shows tachycardia with a normal S1 and S2, new holosystolic murmur heard best at the left lower sternal border that radiates to the apex, and a right ventricular heave Which of the following is the most appropriate management? A) Emergency cardiac surgery B) Emergency pericardiocentesis C) Percutaneous coronary intervention to left anterior descending artery D) Right heart catheterization and dopamine infusion Medical Optimization Continued ASA, clopidogrel, atorvastatin, losartan Discontinued HCTZ Increased metoprolol Started isosorbide dinitrate Started Colchicine Exercise Treadmill Test Clinically positive stress test with no evidence of ischemia Good cardiovascular condition for age and gender Abnormal clinical response to exercise as patient developed chest pressure during exertion Normal exercise electrocardiogram Myocardial Infarction Complications Mechanical Complications Conduction Abnormalities Pericardial Complications Time Course of Complications Hours – days: conduction abnormalities 1-3 days: Peri-infarction pericarditis Days: Pericardial effusion Days – 2 weeks: Rupture of LV, IV septum Weeks – Months: Postcardiac Injury Syndrome Mechanical Complications Rupture of LV free wall Rupture of interventricular septum Acute Mitral Regurgitation Rupture of LV Free Wall • Within 2 weeks post-MI: within first 5 days in 50% of cases, within 2 weeks in 90% of cases • RFs: no history of previous angina/MI, STE or Qs on presenting EKG, peak CK-MB > 150 large transmural infarct, absence of collateral blood flow • Complete rupture hemopericardium acute onset heart failure and shock PEA death • Incomplete/subacute rupture: thrombus and pericardium seal rupture • s/s: persistent/recurrent chest pain, nausea, agitation, transient hypoTN, EKG features of pericardititis • Dx: clinical, confirmed by TTE if time, pericardiocentesis • Tx: hemodynamic support w IVF, inotropes, vasopressors; pericardiocentesis, surgical repair Rupture of Interventricular Septum Usually 3-5 days after MI (1 day – 2 weeks) RFs: 1V disease (esp wraparound LAD), large infarction, poor septal collateral circulation, no previous MI Most: inf 1/3 of septum supplied by RCA Some: LAD extends past LV apex wraps around to supply inferior septum ant MI 2/2 LAD lesion decreased collaterals to septum and larger septal infarction STE in inf leads S/S: hemodynamic compromise Dx: PA catheter, TTE with Doppler Tx: afterload reduction, inotropes, diuretics, surgery Acute Mitral Regurgitation 2/2 ischemic papillary muscle displacement (dysfunction), LV dilatation/aneurysm, papillary muscle rupture S/S: hemodynamic compromise, new systolic murmur Dx: TTE flail segment of MV, TEE Tx: afterload reduction (nitrates, nitroprusside, diuretics), surgery Conduction Abnormalities Inferior MI: sinus bradycardia, First degree AV block, Second degree AV block Mobitz type 1 Anterior MI: first degree AV block, Second degree Mobitz type II, Third degree AV block Pericardial Complications Early infarct-associated pericarditis (Peri-infarction pericarditis) Pericardial effusion (+/- tamponade) Postcardiac Injury Syndrome (Dressler’s syndrome) Peri-infarction pericarditis Early cx days after MI, self-limited S/S: pericardial friction rub, pleuritic chest pain Dx: clinical, EKG with ST segments remaining elevated and upright T waves Evaluation: TTE to assess for pericardial effusion if effusion > 10mm thick increased risk of free wall rupture or already with subacute rupture that is contained Importance: a/w larger infarct risk stratification Tx: supportive, ASA+Colchine, avoid NSAIDs/glucocorticoids Pericardial Effusion Usually small, rarely with tamponade physiology Occurs within days can take months for resorption S/S: usually asx Dx: TTE Importance: a/w higher morbidity/mortality larger infarct Tx: supportive Postcardiac Injury Syndrome (PCIS) Can occur after MI, cardiac surgery, PE Late cx weeks – months after MI s/s: pleuritic CP, pericardial friction rub, fever, leukocytosis, pericardial/pleural effusion Pathogenesis: immunologic: myocardial injury release of cardiac Ags Ab formation immune complexes deposit onto pericardium, pleura, lungs inflammatory response Dx: clinical, ↑ESR, EKG Tx: NSAIDs, Colchine, steroids if refractory Colchicine in Addition to Conventional Therapy for Acute Pericarditis: Results of the COlchicine for acute PEricarditis (COPE) Trial 2005 Inclusion criteria: acute pericarditis of idiopathic, viral, and autoimmune causes, including postpericardiotomy syndromes and connective tissue diseases Acute pericarditis, 2+ of the following: typical chest pain, pericardial friction rub, and widespread ST-segment elevation on the ECG ASA or ASA+Colchine ASA 800 mg PO q6-8h x 7 -10 days with taper over 3 - 4 weeks (group I) ASA at the same dose + colchicine 1.0 - 2.0 mg x 1 day, then 0.5 - 1.0 mg daily x 3 months (group II) primary end point: recurrence rate recurrent pain + 1 or more: fever, pericardial friction rub, ECG changes, pericardial effusion on TTE, elevations in the WBC, ESR, or CRP Results of COPE trial 2873 patient-months of follow-up Higher recurrence rate in patients treated only by aspirin (group I) v. patients treated with colchicine plus conventional treatment (group II), (33.3% versus 11.7%; P=0.009) Group II with longer symptom-free interval (22.9±10.3 versus 17.2±12.3 months; P=0.007). References Khan, A. H. (1992), The postcardiac injury syndromes. Clin Cardiol, 15: 67–72. LeWinter, M et al. Pericardial complications of myocardial infarction. Up To Date, accessed 9/13/2016. Massimo Imazio, et al. Colchicine in Addition to Conventional Therapy for Acute Pericarditis. Circulation. 2005;112:2012-2016