* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Types of Blood Vessels
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac surgery wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Myocardial infarction wikipedia , lookup
Artificial heart valve wikipedia , lookup
Jatene procedure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
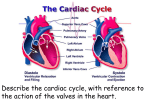
Types of Blood Vessels ARTERIES Arterioles capillaries Venules VEINS Structure of Blood Vessels • Tunica Intima: thin innermost layer of endothelium • Tunica Media: middle layer of smooth muscle; thickest layer • Tunica Externa: outermost layer; fibrous Structure of Blood Vessels • Capillaries – Only have tunica intima to easily let things in and out • What passes into and out of the capillaries?? – CO2/O2, nutrients/waste Trace Pathway Through Heart As Class • Right Atrium • Right Atrium Animation of Blood Flow • http://www.biologyinmotion.com/cardio/cvsy stem.swf Blood Flowing Through the Heart Re‐Label ALL parts (including valves) Refresh your memory… • In order to push blood OUT of the heart what part(s) of the heart contract(s)? – ventricles • Do the contractions occur simultaneously or at separate times? – simultaneously Vocab Differences • Atrioventricular (AV) valves = tricupsid & mitral (bicupsid) valves • Semilunar (SV) valves= pulmonary & aortic valves Heart Sounds • Heart beat sounds like Lub dup – Lub • AV valves close after atrial systole – Dup • Closing of semilunar valves after ventricular systole – Pause • Refilling of chambers Cardiac Cycle (heart beat) = alternate periods of: Diastole: muscle relaxed; chambers filling; blood flowing passively Systole: muscle contract; chambers empty; signal for blood to move in appropriate direction What makes gas exchange in the capillaries? • Pressure • Things move from a __________ pressure to ___________ pressure. Pressure Presence • Pressure within heart chambers will cause valves to open & close like a door opening & closing CARDIAC CYCLE 4 Step Process to Lub/Dub 4 steps to Cardiac Cycle 1. 2. 3. 4. Atrial Diastole Atrial Systole Ventricular Systole Ventricular Diastole 1. Atrial Diastole • • • • Atria RELAXED SV valves= CLOSED AV valves= OPEN Blood flow from veins INTO heart (atria) 2. Atrial Systole • • • • Atria CONTRACT SV valves= CLOSED AV vales= OPEN Blood moves into ventricle 3. Ventricular Systole • Ventricle CONTRACT • AV valves = CLOSE (LUB) • Because AV valves close… – Volume decreased – Pressure increase • Causes SV valves to OPEN. Blood flow into artery 4. Ventricular Diastole • Ventricle RELAX • SV valves CLOSE (DUP) • AV valves OPEN • Restart process Atrial Diastole Atrial Systole Ventricular Systole Ventricular Diastole Contract/Relax Relax Contract Contract Relax AV valve (open/close) open open close Open SV valve (open/close) close close open Close Blood flow to… Into atria Into ventricle Into artery Capillaries, to veins The Cardiac Cycle http://bcs.whfreeman.com/thelifewire/conte nt/chp49/49020.html ON A PIECE OF PAPER… • Place the following events of the cardiac cycle in order & then put the #s of what occurs at each A. Atrial Diastole B. Ventricular systole C. Atrial systole D. Ventricular diastole 1. 2. 3. 4. 5. 6. SV valves close SV valves open AV valves close AV valves open Dup Lub • What purpose do the valves serve? Cardiac Cycle & Heart Sounds 1) Atrial Diastole: blood flowing into atria 2) Atrial Systole: blood flowing into ventricles 3) Ventricular systole: ventricles contract, atria diastole/relax 1) AV valves close: prevent backflow (Lub) 4) Ventricular diastole: atria filling, ventricles relaxing 1) SV valves close: prevent backflow (Dup) Animations • http://library.med.utah.edu/kw/pharm/hyper _heart1.html • http://msjensen.cehd.umn.edu/1135/links/An imations/Flash/0028‐swf_the_cardiac_cy.swf • http://www.azisoft.com/Cardiovascular_Syste m.swf Controlling the heart • Nodal System – The Pacemaker – Special tissue that is a cross between muscle and nervous tissue that controls heart contractions • Three parts: 1. Sinoatrial node 2. Atrioventricular node 3. Atrioventricular bundles Nodal System • Sinoatrial Node – Located in the right atrium – starts each heart beat • Atrioventricular Node – Located at junction between atria and ventricles Nodal System • Atrioventricular Bundles – Branch off from the AV node and trigger ventricular contraction SA Node starts impulse AV Node triggered Atria Contract PAUSE Impulse travels through AV Bundlesbundles Ventricles Contract Cardiac Cycle During what phase do the AV valves close? ‐ Ventricular Systole During what phase do the SV valves open? ‐Ventricular Diastole During what phase do the SV valves close? ‐Ventricular Diastole Where are the SA & AV nodes? Combining Cardiac Cycle & Nodes Place these events in order during a heart beat: 1. Atria fill with blood 2. SV valves close 3. AV valves close 4. SA node receives signal 5. Atrioventricular Bundles receive impulse 6. Ventricles contract (systole) Correct Order • 4, 1, 5, 6, 3, 2 ECG Video • http://www.youtube.com/watch?v=nK0_28q6 WoM Electrocardiogram (ECG) • Recording of electrical changes that occur in heart tissue during one heart beat (or cardiac cycle) • Electrodes are placed on skin & wires are connected to a machine that responds to weak electrical changes. ECG Pattern • Several waves – P wave: depolarize atria by SA node – QRS complex: depolarization of ventricle by AV node to AV bundles (larger electrical change b/c ventricular walls are thicker than atria) • Atria repolarizing at same time – T wave: after contraction of ventricle, repolarization of ventricles Label what happens at each wave Animation: Cardiac Cycle w/ ECG • http://library.med.utah.edu/kw/pharm/hyper _heart1.html Heart Rate • Controlled by SA node – Impulses sent from medulla oblongata which receives sensory impulses & relays motor impulse back to the heart. – Impulses from cerebrum or hypothalamus can influence rate • Decrease heart rate after you faint • Increase heart rate b/c of anxiety Heart Rate • Also affected by temperature & ions – High body temperature (fever) increased rate – Low body temperature decreased rate – K+ & Ca++ if too much or too little Circulation Physiology • Vital Signs – Pulse – Blood Pressure Pulse • Expansion and contraction of arteries • Pressure Points (aka pulse points) – Locations on the body where the arteries are close to the surface and are easily felt Pressure Points Acupuncture • Eastern medicine– not western medically proven to work. – Needles in pressure points to find chi/balance of body’s force Blood Pressure • Pressure blood exerts on the walls of blood vessels Blood Pressure Gradient Blood Vessel Pressure Aorta Arterioles Systolic: 120 Diastolic: 90 Systolic: 110 Diastolic: 80 65 Capillaries 15 Venules 5 Veins 1 Venae Cavae 0 Arteries Factors Affecting Blood Pressure • Neural Factors – Nerves can cause blood vessels to constrict • Renal Factors (Kidneys) – Changes the amount of water in blood which changes blood volume which changes pressure • Temperature – Coldness causes blood vessels to constrict – Heat causes them to dilate Factors Affecting Blood Pressure • Chemicals – Drugs (including alcohol) alter heart rate and can cause blood vessels to dilate or constrict • Diet – Salts, saturated fats, and cholesterol can lead to high blood pressure Blood Pressure • Hypotension – Low blood pressure (< 100 mmHg) – Most commonly caused by blood loss • Hypertension – High blood pressure (> 140/90) – Long‐term effects: strains heart and damages blood vessels • http://www.youtube.com/watch?v=HNuPWdfj Doc (how veins work) • http://www.youtube.com/watch?v=Nb4jpp‐ GGUs&feature=fvst (blood pressure) • http://www.youtube.com/watch?v=tAmLbclS ucQ (high blood pressure) • http://www.youtube.com/watch?v=02tpzvme N_I (new method to lower bp) BP Article • http://www.nhlbi.nih.gov/health/dci/Diseases /Hbp/HBP_WhatIs.html How does one measure the strength of a heart? Cardiac Output • Cardiac Output (CO) – Amount of blood pumped out by each side of the heart in 1 minute (ml/min) • Stroke Volume (SV) – Volume of blood pumped out by a ventricle with each heart beat (ml/beat) • Heart Rate (HR) – Number of beats per minute (bpm) Cardiac Output • Equation • CO = HR x SV • Example: Average heart rate is 70 bpm and the average stroke volume is 70 ml/beat. What is the average cardiac output? • If a person has a larger heart, how would this affect his/her cardiac output? To increase cardiac output… • Increase heart rate – When might your body do this? • Increase stroke volume – How might your body do this? Composition of Blood I. Functions 1. Transports nutrients, oxygen, wastes, hormones 2. Maintains stability of fluid between tissues 3. Distributes heat What is blood made of? 1. Solid (formed elements) 55% A. Red blood cells B. White blood cells C. Platelets 2. Liquids 45% D. Plasma A. Red Blood Cells aka erythrocytes • Shape: biconcave disc (like a lifesaver or donut) • How the shape helps the RBC to function: – Increase surface area through which gases diffuse Sickle‐cell Anemia • Mutation causes hemoglobin to crystalize when O2 is not present • Bends the RBCs into sickle shape • Blocks circulation in small blood vessels • Results in joint pain, organ damage • FYI: 1 copy of mutationÆ immunity from malaria; 2 copies of mutation Æ sickle cell disease B. White Blood Cells aka leukocytes • Five types • Function: protect against disease – Produce proteins (antibodies) that destroy foreign particles. – Phagocytize (eat) bacterial cells. C. Platelets • Aka thrombocytes • Structure: – Not complete cells – Come from large cells in bone marrow that fragment • Function: – Controls blood loss from broken blood vessels – Initaite blood clots D. Plasma • Water, amino acids, proteins, carbohydrates, lipids, vitamins, hormones, electrolytes, cellular waste.