* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiology Review: Heart Failure and Valve Disease April 20, 2007
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Artificial heart valve wikipedia , lookup
Cardiac surgery wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Coronary artery disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Myocardial infarction wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Aortic stenosis wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
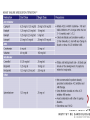
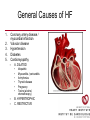
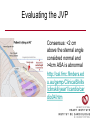
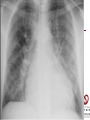
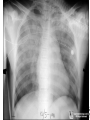
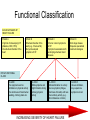
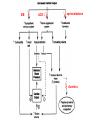
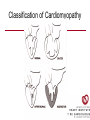
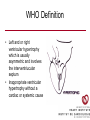
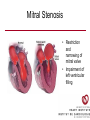
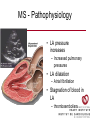
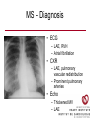
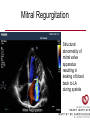
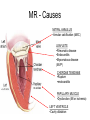
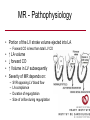
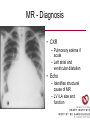
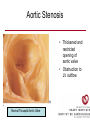
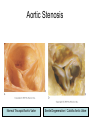
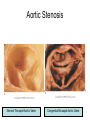
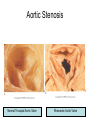
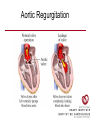
Cardiology Review: Heart Failure and Valve Disease April 7, 2010 Dr. Nisha D’Mello Assistant Professor Medicine University of Ottawa Heart Institute Outline • Heart Failure – Causes – Symptoms – Treatments • Cardiomyopathies • Approach to valve disease – Mitral stenosis and regurgitation – Aortic stenosis and regurgitation Define Heart Failure Definition • Condition where the heart cannot pump an adequate supply of blood at normal filling pressures to meet the metabolic needs of the body • HF is a complex syndrome in which abnormal heart function results in – clinical symptoms and signs of • low cardiac output and/or • pulmonary or systemic congestion Increased contractility Normal A Heart Failure Hypotension Stroke volume (cardiac output) Pathophysiology of Heart Failure B C Pulmonary congestion Left ventricular end diastolic pressure (volume) Cardiomyopathy • Characterized by ventricular – Dilatation – Hypertrophy • Frank Starling: CO = SV x HR • Laplace: Tension = Press x rad/ 2 x thick WHAT CAUSES HEART FAILURE? Classification of Heart Failure Causes • Multiple ways to consider classification: – Etiologic – Systolic vs. Diastolic – Right vs. Left General Causes of HF 1. 2. 3. 4. 5. Coronary artery disease / myocardial infarction Valvular disease Hypertension Diabetes Cardiomyopathy – A. DILATED • • • • • • – – Idiopathic Myocarditis / pericarditis Arrhythmias Thyroid disease Pregnancy Toxins (alcohol, chemotherapy) B. HYPERTROPHIC C. RESTRICTIVE Mechanisms and Causes of HF Impaired Contractility Myocardial infarction Transient ischemia Chronic volume overload MR/AR Dilated cardiomyopathy Increased Afterload AS Uncontrolled HTN Systolic Dysfunction Left Sided HF Diastolic Dysfunction Obstruction of LV filling MS Pericardial constriction or tamponade Impaired ventricular relaxation LVH Hypertrophic cardiomyopathy Restrictive cardiomyopathy Transient ischemia Mechanisms and Causes of HF Cardiac Causes Left sided HF Pulmonary stenosis Right ventricular infarction Right Sided HF Pulmonary Vascular Disease Pulmonary emobolism Pulmonary HTN Right ventricular infarction Parenchymal pulmonary disease COPD Interstitial lung disease Chronic infections Adult respiratory distress syndrome The Heart Failure Continuum poor prognosis average 1-year mortality rate of 33% HOW DO YOU DIAGNOSE HEART FAILURE ? Diagnosis of HF • Constellation of symptoms and signs • CXR • Echocardiogram – MUGA – Serum BNP testing Symptoms and Signs of HF Increased filling pressures Congestion Poor Cardiac Output Poor Perfusion Assessing Perfusion • Symptoms – Fatigue – Confusion – Dyspnea • Signs – – – – – – Hypotension Tachycardia Cool extremities Altered mental status Rising creatinine Liver enzyme abnormalities Congestion • Left-Sided – Symptoms • Dyspnea • Orthopnea • Paroxysmal nocturnal dyspnea – Signs • • • • • S3 gallop Displaced apex MR Pulmonary rales Loud P2 • Right-Sided – Symptoms • • • • Peripheral edema Abdominal bloating Nausea Anorexia Signs • • • • Elevated JVP Hepatomegaly Ascites Edema Evaluating the JVP • Consensus: <2 cm above the sternal angle considred normal and >4cm ASA is abnormal • http://cal.fmc.flinders.ed u.au/gemp/ClinicalSkills /clinskil/year1/cardio/car dio04.htm Diagnosis of HF • Constellation of symptoms and signs • CXR • Echocardiogram – MUGA – Serum BNP testing Pulmonary Edema • General Considerations – Increase in the fluid in the lung – Generally, divided into cardiogenic and non-cardiogenic categories. • Pathophysiology – Fluid first accumulates in and around the capillaries in the interlobular septa (typically at a wedge pressure of about 15 mm Hg) – Further accumulation occurs in the interstitial tissues of the lungs – Finally, with increasing fluid, the alveoli fill with edema fluid (typically wedge pressure is 25 mm Hg or more) Cardiogenic vs. Noncardiogenic pulmonary edema • Cardiogenic pulmonary edema – Heart failure • Coronary artery disease with left ventricular failure. • Cardiomyopathy • Obstructing valvular lesions -for example – Fluid overload -- for example, kidney failure. • Non-cardiogenic pulmonary edema -- due to changes in capillary permeability – LUNG • • • • Smoke inhalation Near-drowning Overwhelming aspiration Acute Respiratory Distress Syndrome (ARDS) • Acute lung re-expansion • High altitude pulmonary edema – CAPILLARY • Overwhelming sepsis • Disseminated intravascular coagulopathy (DIC) CXR Findings of Pulmonary Edema cardiogenic pulmonary edema • • • • Kerley B lines (septal lines) – Seen at the lung bases, usually no more than 1 mm thick and 1 cm long, perpendicular to the pleural surface Pleural effusions – Usually bilateral, frequently the right side being larger than the left – If unilateral, more often on the right Fluid in the fissures – Thickening of the major or minor fissure Peribronchial cuffing – Visualization of small doughnut-shaped rings representing fluid in thickened bronchial walls • Non-cardiogenic pulmonary edema – Bilateral, peripheral air space disease with air bronchograms or central bat-wing pattern – Kerley B lines and pleural effusions are uncommon – – Typically occurs 48 hours or more after the initial insult – Stabilizes at around five days and may take weeks to completely clear Diagnosis of HF • Constellation of symptoms and signs • CXR • Echocardiogram – MUGA – Serum BNP testing SO YOUR PATIENT HAS HEART FAILURE… WHAT NOW? Functional Classification ACC/AHA STAGES OF HEART FAILURE STAGE A •High risk for developing HF (diabetes, CKD, HTN) •No structural disorder of the heart STAGE B •Structural disorder of the heart (e.g.. Previous MI) •Not yet developed symptoms of HF STAGE C •Past or current symptoms of HF •Symptoms associated with underlying structural heart disease STAGE D •End stage disease •Requires specialized treatment strategies NYHA FUNCTIONAL CLASS CLASS I •No symptoms and no limitations in physical activity •No shortness of breath when walking, climbing stairs etc. CLASS II •Mild symptoms and slight limitation during ordinary physical activity CLASS III •Marked limitation in activity due to symptoms (fatigue, shortness of breath) with less than ordinary activity (e.g.. Short distances or ADL’s) INCREASING SEVERITY OF HEART FAILURE CLASS IV •Severe limitation, may experience symptoms at rest HOW DO YOU TREAT HEART FAILURE? Goals of Therapy • 1. Identify and Treat the Underlying Cause – Cardiac cath if necessary • • • • 2. Eliminate the acute precipitant 3. Manage HF symptoms 4. Slow progression of LV disease 5. Improve long-term survival Precipitants of HF • Increased metabolic demands – Fever, anemia, infection, tachycardia, hyperthyroidism, pregnancy • Increased circulating volume – Excessive salt or fluid in diet – Renal failure • Increased afterload – Hypertension – PE • Impaired contractility – Negative inotropes – Ischemia • Failure to take medications Progression of underlying disease BB ACE I sprionolactone diuretics Management • 1. Education – Fluid and salt restriction – Daily weights – Avoid precipitants • 2. Diuretics if volume overloaded • 3. Neurohormonal modulation – ACE-I – bB – spironolactone • 4. Devices – CRT – ICD • 5. Referral for cardiac transplantation Who needs an ACE-I? • All HF patients with LVEF <40% should be treated with an ACEI and a beta-blocker, unless a specific contraindication exists CONSENSUS Trial . N Engl J Med 1987;316:1429-35. SOLVD Investigators. N Engl J Med 1991;325:293-302. Flather MD et al. Lancet 2000;355:1575-81. These trials form the basis of ACE-I use in HF with LVEF < 40% and/or post-MI with reduced LVEF and/or HF Who needs a bB? • All HF patients with LVEF 40% (use clinically proven beta- blocker) • In stabilized HF patients with NYHA Class IV symptoms MERIT-HF Study Group. Lancet 1999;353:2001-7. CIBIS II Investigators. Lancet 1999;353:9-13. Packer M et al. Circulation 2002;106:2194-9. Other Drugs ? • Nitrates • Digoxin • Spironolactone Management Strategy Education Severe symptoms: refer to specialist, ER or HF clinic Risk factor reduction Fluid/salt regimen If EF>40%: treat cause (HTN) If EF<40% ACE I +Beta blocker intolerant Prescribe ARB Consider nitrates Titrate to target doses If QRS>120, consider CRT If EF<30% consider ICD Clinically stable •Add ARB NYHA III •Digoxin or nitrates •Combo diuretics •spironolactone Continue therapy Class IIIb-IV Can J Cardiol 2007; 23 CARDIOMYOPATHY Classification of Cardiomyopathy Dilated Cardiomyopathy • CAD is the most common cause of systolic dysfunction • Idiopathic (50%) • Familial • Substance abuse • What are the other nonischemic causes of a dilated cardiomyopathy? • • • • • • • Myocarditis Infiltrative disease Peripartum HIV Chemotherapy Electrolyte imbalance Nutritional: thiamine,scurvy WHO Definition • Left and or right ventricular hypertrophy which is usually asymmetric and involves the interventriucular septum • Inappropriate ventricular hypertrophy without a cardiac or systemic cause Restrictive CM • What are some causes of restrictive CM? • • • • • Amyloidosis Sarcoidosis Hemochromatosis Chemotherapy Endomyocardial fibrosis Valvular Disease Mitral Stenosis • Restriction and narrowing of mitral valve • Impairment of left ventricular filling Mitral Stenosis - Causes • Rheumatic Fever (>90% cases) – 50% patients will have known history – Average 20 years prior to clinical symptoms • Congenital stenosis of MV • Extensive calcification • endocarditis MS - Pathophysiology • LA pressure increases – Increased pulmonary pressures • LA dilatation – Atrial fibrillation • Stagnation of blood in LA – thromboembolism MS - Clinical Presentation • Natural history variable • 10 year survival (symptoms) – 50-60% • Early onset – Dyspnea and reduced exercise capacity • Advanced – – – – SOB at rest Pulmonary congestion (orthopnea, PND etc) Pulmonary HTN (RHF) Hoarseness from laryngeal nerve compression MS - Examination 1. Loud S1 – From calcification of mitral valve 2. Opening snap – Sudden tensing of chordae and stenotic leaflets on valve opening 3. Diastolic murmur – Low frequency – Severity relates to duration MS - Diagnosis • ECG – LAE, RVH – Atrial fibrillation • CXR – LAE, pulmonary vascular redistribution – Prominent pulmonary arteries • Echo – Thickened MV – LAE MS - Treatment • Percutaneous balloon valvuloplasty • Surgical repair • Antibiotics at time of risk • Diuretics for vascular congestion • Decrease HR if AF • anticoagulation Mitral Regurgitation • Structural abnormality of mitral valve apparatus resulting in leaking of blood back to LA during systole MR - Causes MITRAL ANNULUS •Annular calcification (MAC) LEAFLETS •Rheumatic disease •Endocarditis •Myxomatous disease (MVP) CHORDAE TENDINAE •Rupture •endocarditis PAPILLARY MUSCLE •Dysfunction (MI or ischemia) LEFT VENTRICLE •Cavity dilatation MR - Pathophysiology • Portion of the LV stroke volume ejected into LA – Forward CO is less than total LV CO • • • • ↑ LA volume ↓ forward CO ↑ Volume in LV subsequently Severity of MR depends on: – – – – SVR opposing LV blood flow LA compliance Duration of regurgitation Size of orifice during regurgitation MR – Clinical Presentation • Chronic – Fatigue – If LV contractile dysfunction – heart failure • Acute – Pulmonary edema – hypotension MR - Examination 1. Murmur – Pansystolic murmur heard at apex 2. S3 – Reflects increased volume returning to LV in early diastole 3. LV displacement – If LV enlargement present MR - Diagnosis • CXR – Pulmonary edema if acute – Left atrial and ventricular dilatation • Echo – Identifies structural cause of MR – LV /LA size and function MR - Treatment • Acute MR – Reduce the resistance to forward flow (Vasodilators) – Relieve pulmonary edema (Diuretics) • Chronic – Operative repair once symptoms develop or LV starts to dilate Aortic Stenosis • Thickened and restricted opening of aortic valve • Obstruction to LV outflow Normal Tricuspid Aortic Valve Aortic Stenosis Normal Tricuspid Aortic Valve Senile Degenerative / Calcific Aortic Valve Aortic Stenosis Normal Tricuspid Aortic Valve Congenital Bicuspid Aortic Valve Aortic Stenosis Normal Tricuspid Aortic Valve Rheumatic Aortic Valve AS - Pathophysiology • Blood flow across the AV is impeded • Once AVA ↓ 50%: – Significant LV pressure needed to drive blood into aorta – Results in LV hypertrophy – ↓ LV compliance (Stiffer LV) => Increased end diastolic pressure AS – Clinical Presentation • Angina – Imbalance b/w myocardial oxygen supply and demand • Syncope – Peripheral vasodilation with inability to augment CO with exercise • HF – Increased LAP from high LVEDP – Contractile dysfunction if longstanding pressure overload Symptom Median survival Angina 5 yrs Syncope 3 years HF 2 years AS -Exam 1. Carotid pulse – Weakend (parvus) and delayed (tardus) due to LV obstruction 2. Murmur – Late peaking systolic ejection murmur 3. S4 – Atrial contraction into stiff LV AS - Treatment • Only effective treatment for severe symptomatic disease is surgical correction • What if asymptomatic? – 20% of patients will progress over 20 years if mild disease only Aortic Regurgitation AR - Causes • Abnormalities of valve leaflets – Congenital (bicuspid valves) – Endocarditis – Rheumatic • Dilatation of aortic root – Aortic aneursym – Aortic dissection – syphilis AR - Pathophysiology • Severity of AR – Size of regurgitant orifice – Pressure gradient across valve in diastole – Duration of diastole • Acute – LV noncompliant – LVEDP rises quickly – pulmonary edema • Chronic – Chronic volume/pressure overload – Dilates – well compensated AR – Clinical Manifestations • SOB on exertion • Fatigue • Decreased exercise tolerance AR - Examination • Murmur – Blowing diastolic along LSB • Widened pulse pressure Name Description Bisferins Double impulse Corrigans Marked distention and collapse deMusset Head bobbing Duroziez To and fro murmur Hill Greater popliteal SBP Muller Uvula pulsations Quincke Nail bed pulsation Traube Pistol shot femoral art AR - Treatment • Asymptomatic disease progresses very slowly • Surgery if: – Symptoms – Impaired LV function • Death occurs within 4 years after angina or 2 years after HF Summary Slide • Heart Failure – Understand causes of systolic and diastolic HF – Awareness of the presentation of left vs. right HF – Know treatment priniciples • Valve Disease – Identify the most common causes of 4 common valve lesions – Remember clinical presentations – Surgery treatment of choice any time symptoms present or LV dysfunction Cardiology Review: Heart Failure and Valve Disease April 7, 2010 Dr. Nisha D’Mello Assistant Professor Medicine University of Ottawa Heart Institute