* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Preoperative Alcohol Septal Ablation for Hypertrophic Obstructive
Coronary artery disease wikipedia , lookup
Echocardiography wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Atrial septal defect wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
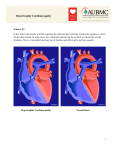
Case Report HOCM and Pheochromocytoma Acta Cardiol Sin 2010;26:189-92 Preoperative Alcohol Septal Ablation for Hypertrophic Obstructive Cardiomyopathy before Surgical Resection of Pheochromocytoma: The First Medical Report Jia-Feng Chang,1 Chih-Ming Lin,2 Chi-Hung Huang,1 Ching-Ling Lin,3 Shih-Hung Huang4 and Chih-Hui Chin1 A 50-year-old woman was admitted to the hospital because of chest pain accompanied with cold sweating, palpitation and extremely high blood pressure. Transthoracic echocardiography (TTE) revealed systolic anterior motion of mitral valve, with peak velocity crossing the left ventricular outflow tract (LVOT) about 4.9 m/s and severe mitral regurgitation (MR). The study for secondary hypertension revealed high urine vanillylmandelic acid (82.57 mg/24 hrs) and norepinephrine (916.5 ug/24 hrs). A huge pheochromocytoma was found by abdominal computed tomography and magnetic resonance imaging. During the hospitalization, her blood pressure could fluctuate from 188/122 mmHg to 89/46 mmHg, depending on fluid challenge, within three hours with chest pain and cold sweating. Thus, we decided to apply alcohol septal ablation therapy to provide a more stable hemodynamic status for tumor resection. TTE was done one week post alcohol septal ablation and showed the peak velocity crossing the LVOT declined to 2.3 m/s and only mild MR. Subsequently, the patient successfully received surgical resection and was discharged under long-term outpatient clinic follow-up. Key Words: Alcohol septal ablation · Hypertrophic obstructive cardiomyopathy · Pheochromocytoma CASE REPORT tum thickness was 17 mm and posterior wall thickness was 12 mm) with systolic anterior motion of the anterior mitral valve. The peak velocity cross left ventricular outflow tract (LVOT) was 2.0 m/s at that time. Her baseline blood pressure had been well-controlled around 130/80 mmHg without significant discomfort in the past years. Nevertheless, she suffered from intermittent high blood pressure above 220/110 mmHg with dizziness and had had several episodes of non-admitted patient emergency department service since the age of forty-eight. Two weeks prior to this admission, chest pain, headache, and palpitation developed in addition to high blood pressure. Subsequently, the patient received cardiac catheterization under the first impression of acute coronary syndrome, which showed patent coronary artery and hypertrophic obstructive cardiomyopathy. Transthoracic echocardiography (TTE) revealed systolic anterior motion of mitral valve with peak velocity crossing the LVOT of A 50-year-old woman was admitted to the hospital because of chest pain accompanied with cold sweating, palpitation and extremely high blood pressure. The patient had previously been diagnosed with essential hypertension and started on antihypertensive treatment when she was thirty-nine years old. Five years later, her two-dimensional transthoracic echocardiography revealed hypertrophic obstructive cardiomyopathy (sep- Received: October 7, 2009 Accepted: March 25, 2010 1 Division of Cardiology; 2Division of Urology; 3Division of Endocrine; 4 Pathology, Cathay General Hospital, Taipei, Taiwan. Address correspondence and reprint requests to: Dr. Chih-Hui Chin, Division of Cardiology, Department of Medicine, Cathay General Hospital, No. 280, Section 4, Jen-Ai Road, Taipei 106, Taiwan. Tel: 886-2-2708-2121 ext. 3118; Fax: 886-2-2932-4969; E-mail: [email protected] 189 Acta Cardiol Sin 2010;26:189-92 Jia-Feng Chang et al. hrs). The physical examination found a huge abdominal mass. When touching the abdominal mass, the patient felt palpitation, headache and sweating. The blood pressure was extremely increased from 128/86 mmHg to 220/130 mmHg, and heart rate was increased from 78 bpm to 116 bpm. Under the impression of pheochromocytoma, a series of imaging studies were done. The abdominal computed tomography demonstrated a welldefined mass of size about 7.4 ´ 7.0 ´ 5.4 cm with calcification, central necrosis and heterogeneous density at the right retroperitoneum. The abdominal magnetic resonance imaging also displayed a right retroperitoneal tumor, 7.6 ´ 7.6 ´ 5.9 cm in size with central necrosis (Figure 2A). Since all the laboratory and imaging studies were compatible with the diagnosis of pheochromocytoma, surgical intervention was recommended. During the hospitalization, the patient’s blood pressure could fluctuate from 188/122 mmHg to 89/46 mmHg depend- about 4.9 m/s (Figures 1A and B). Septum thickness was 22 mm, posterior wall thickness was 14 mm, left ventricular ejection fraction was 68% and mitral regurgitation (MR) was severe. Because of extremely high blood pressure, study for secondary hypertension was done. On the day of admission, the patient had severe chest pain that was accompanied by cold sweating and palpitation. The pulse was 95 beats per minute, blood pressure 262/143 mmHg, respiratory rate 20 breaths per minute, and temperature 35.3 °C. Electrocardiography presented sinus rhythm, left ventricular hypertrophy and ST segment depression with T-wave inversion in leads II, III, aVF, and V3 through V6. Chest radiography showed no abnormalities except cardiomegaly. The values of creatinine, sodium, potassium and cardiac enzyme were within normal range. The study for secondary hypertension revealed high urine vanillylmandelic acid (82.57 mg/24 hrs) and norepinephrine (916.5 ug/24 A B C D Figure 1. Transthoracic echocardiography (TTE) revealed systolic anterior motion of mitral valve (A) with peak velocity cross left ventricular outflow tract (LVOT) about 4.9 m/s (B). One week after alcohol septal ablation, systolic anterior motion of mitral valve was much better (C) and peak velocity cross LVOT declined to 2.3 m/s (D). Acta Cardiol Sin 2010;26:189-92 190 HOCM and Pheochromocytoma A B Figure 2. (A) The abdominal magnetic resonance imaging displayed a right retroperitoneal tumor, 7.6 ´ 7.6 ´ 5.9 cm in size with central necrosis. (B) Pathology revealed that tumor cells possess mildly to moderately pleomorphic nuclei and abundant finely granular eosinophilic or amphophilic cytoplasm with nucleolation and few mitotic activity, H&E, x400. ization, myxoid change and cystic change were noted. In immunohistochemical study, the tumor cells are positive for synaptophysin, chromogranin and CD56, and focally positive for S-100 protein. Taking the histopathological picture and the results of immunostain together, it is a paraganglioma. All of the three dissected lymph nodes revealed no evidence of metastasis. ing on fluid challenge within three hours with chest pain and cold sweating. Thus, we decided to apply for alcohol septal ablation therapy to provide a more stable hemodynamic status for tumor resection. On the fourth hospital day, percutaneous transluminal septal myocardial ablation therapy was performed smoothly. Before the procedure, left ventricular pressure was 205/7 mmHg, aortic pressure was 115/72 mmHg, and heart rate was 84 bpm. After procedure, left ventricular pressure was 203/12 mmHg, aortic pressure was 173/104 mmHg and heart rate was 88 bpm. The pressure gradient crossing the left ventricular outflow tract decreased from 90 mmHg to 30 mmHg immediately. The peak creatine kinase and creatine kinase MB were 926 U/liter and 238.8 ng/ml post alcohol septal ablation, respectively. TTE was done one week post alcohol septal ablation and showed the peak velocity crossing the LVOT declined to 2.3 m/s and systolic anterior motion of mitral valve was better then pre-ablation (Figures 1C and D). Subsequently, she successfully received surgical resection and discharged under long-term outpatient clinic follow-up. After postoperative 8 months, echocardiography was repeated and the data showed that septum thickness was 15 mm, posterior wall thickness was 12 mm, peak velocity crossing the LVOT was 1.9 m/s, left ventricular ejection fraction was 62% and MR was mild. The pathology revealed that tumor cells possess mildly to moderately pleomorphic nuclei and abundant finely granular eosinophilic or amphophilic cytoplasm with nucleolation and little mitotic activity (Figure 2B). Focal hemorrhage, hyalin- DISCUSSION Hypertrophic obstructive cardiomyopathy (HOCM) is characterized by asymmetric left ventricular hypertrophy and dynamic LVOT obstruction, which can impair blood flow into and out from left ventricle, leading to progressive heart failure and sudden death in some patients. 1,2 The overall probability of death related to hypertrophic cardiomyopathy was significantly greater among patients with outflow tract obstruction than among those without obstruction.3 Studies report higher perioperative risk of inhospital mortality and myocardial infarction associated with noncardiac surgery in patients with hypertrophic cardiomyopathy. 4 Accordingly, patients with HOCM undergoing elective procedures may require more careful preoperative assessment, careful planning in anesthesia and perioperative monitoring to minimize morbidity and mortality. Also perioperative morbidity and mortality in patients with pheochromocytoma were 23.6% and 2.4%, respectively.5 There is a paucity of reports about complications of pheochro191 Acta Cardiol Sin 2010;26:189-92 Jia-Feng Chang et al. REFERENCES mocytoma associated with clinical and echocardiographic features simulating HOCM. 6,7 Both pheochromocytoma and HOCM can lead to perioperative morbidity and mortality, therefore, patients who suffer from both diseases are at especially high risk for surgery. According to preoperative assessment of the patient, the peak velocity crossing the LVOT by was up to 4.9 m/s, with severe MR. Her clinical paroxysmal blood pressure fluctuation was stressful and made us hesitate to administer the preoperative medicine of alfa-adrenergic blockade. As a result, we decided to perform alcohol septal ablation therapy for relative hemodynamic stability. After the septal myocardial ablation, there was neither hypotension nor complication. Therefore, alcohol septal ablation of HOCM in such condition may be one of the options. Systemic hypertension due to pheochromocytoma may be associated with left ventricular hypertrophy that is often concentric and symmetric.8-10 However, a few cases simulating HOCM revealed asymmetric septal hypertrophy, systolic anterior motion of mitral valve, MR and dynamic LVOT obstruction. 5 Huddle et al. found only partial regression of abnormal septum and posterior wall thickness in patients with pheochromocytoma simulating asymmetric septal hypertrophy. The present case also showed asymmetric septal hypertrophy and partial regression of abnormal septum and posterior wall thickness after successful removal of pheochromocytoma. Acta Cardiol Sin 2010;26:189-92 1. Wigle ED, Rakowski H, Kimball BP, et al. Hypertrophic cardiomyopathy: clinical spectrum and treatment. Circulation 1995; 92:1680. 2. Maron BJ. Hypertrophic cardiomyopathy: a systematic review. JAMA 2002;287:1308. 3. Maron MS, Olivotto I, Betocchi S, et al. Effect of left ventricular outflow tract obstructionon clinical outcome in hypertrophic cardiomyopathy. N Engl J Med 2003;348:295-303. 4. Hreybe H, Zahid M, Sonel A, et al. Noncardiac surgery and the risk of death and other cardiovascular events in patients with hypertrophic cardiomyopathy. Clin Cardiol 2006;29:65-8. 5. Plouin PF, Duclos JM, Soppelsa F, et al. Factors associated with perioperative morbidity and mortality in patients withpheochromocytoma: analysis of 165 operations at a single center. J Clin Endocrinol Metab 2001;86:1480-6. 6. Huddle KR, Kalliatakis B, Skoularigis J. Pheochromocytoma associated with clinical and echocardiographic features simulating hypertrophic obstructive cardiomyopathy. Chest 1996;109:1394-7. 7. Kassim TA, Clarke DD, Mai VQ, et al. Catecholamine-induced cardiomyopathy. Endocr Pract 2008;14:1137-49. 8. Mardini MK. Echocardiographic findings in pheochromocytoma. Chest 1982;81:394-5. 9. Yang YN, Chuang YC, Yin WH, et al. Catecholamine-induced cardiomyopathy secondary to pheochromocytoma mimicking fulminant acute myocarditis. Acta Cardiol Sin 2007;23:125-30. 10. Lin CT, Rim R, Lin TK, et al. Hypertrophyic cardiomyopathy associated with midventricular obstruction and apical aneurysm. Acta Cardiol Sin 2008;24:221-5. 192