* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The Tissue Level of Organization
Embryonic stem cell wikipedia , lookup
Cell culture wikipedia , lookup
Microbial cooperation wikipedia , lookup
Stem-cell therapy wikipedia , lookup
Chimera (genetics) wikipedia , lookup
Artificial cell wikipedia , lookup
State switching wikipedia , lookup
List of types of proteins wikipedia , lookup
Nerve guidance conduit wikipedia , lookup
Hematopoietic stem cell wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Neuronal lineage marker wikipedia , lookup
Human embryogenesis wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
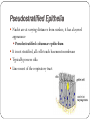
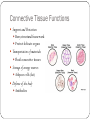
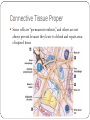
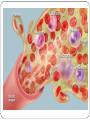
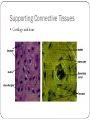
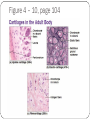
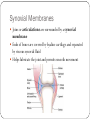
The Tissue Level of Organization Chapter 4 Four Basic Tissue Types Epithelial 2. Connective 3. Muscle 4. neural 1. Epithelial Tissue Includes epithelia and glands Epithelia – layers of cells that cover internal or external surfaces Glands – secreting cells derived from epithelia Important characteristics: Cells bound closely together A free (apical) surface exposed to the environment or to some internal chamber or passageway Attachment to underlying connective tissue By a basement membrane Epithelial cells that are damaged or lost at the exposed surface are continuously replaced Functions of Epithelia Provide physical protection 1. Protect exposed and internal surfaces Control permeability 3. Provide sensation 2. detect changes in the environment and relay the information to the nervous system Produce specialized secretions 4. Gland cells Glandular epithelium Exocrine – secretions discharged onto the surface of the epithelium Endocrine – secretions into the surrounding tissues and blood (hormones) Intercellular Connections Must remain firmly attached to a basement membrane and each other Tight junction Lipid layers of adjacent cell membranes are tightly bound together by interlocking membrane proteins Gap junction Two cells are held together by embedded membrane proteins. Form a narrow passageway to let small molecules and ions to pass through Desmosome Cell membranes of two cells are locked together by intercellular cement and by membrane proteins connected to a network of intermediate filaments The Epithelial Surface Have specialized structures that distinguish them from other body cells Many that line internal passageways have microvilli on their exposed surface Increases surface area about 20 times A cell with a ciliated surface has about 250 cilia that beat in a coordinated fashion to move materials across the surface of the cell Example: the respiratory tract The Basement Membrane A network of protein fibers Lies between the epithelium and underlying connective tissues Is a place of attachment for epithelial cells Provides strength and resists distortion Is a barrier between underlying connective tissues and the epithelium Epithelial Renewal and Repair Epithelium must continually repair and renew itself Are lost or destroyed by chemical or physical wear and tear Stem cells Unspecialized cells Found deep in the epithelium near the basement membrane Continuously divide to replace dead or damaged cells in the epithelium Classifying Epithelia Two types of layering: Simple 2. Stratified 1. Three Cell Shapes: Squamous 2. Cuboidal 3. Columnar 1. Table 4 – 1 page 93 Cell Layers Simple epithelium Single layer of cells covering the basement membrane Line ventral body cavities, heart chambers and blood vessels Where secretions or absorption occurs – thinness reduces diffusion time Stratified epithelium Has several layers of cells over the basement membrane Provides more protection Found in areas subject to more mechanical or chemical stress Cell Shape Squamous epithelium 1. Cells are thin and flat Looks like fried eggs laid side by side Cuboidal epithelium 2. Hexagonal boxes in 3D view, but in sectional view look like boxes Columnar epithelium 3. Also hexagonal but taller and more slender Nuclei are crowded in a narrow band close to basement membrane Simple Squamous Epithelia Found in protected regions where absorption takes place or where a slippery surface reduces friction Simple Cuboidal Epithelium Provides limited protection Secrete enzymes and buffers in the pancreas and salivary glands Involved in the production of urine Simple Columnar Provides some protection and allow for absorption and secretion Lines the stomach, intestinal tract and many excretory ducts Pseudostratified Epithelia Nuclei are at varying distances from surface, it has a layered appearance Pseudostratified columnar epithelium It is not stratified, all cells touch basement membrane Typically possess cilia Lines most of the respiratory tract Transitional and Stratified Transitional epithelium Withstands considerable stretching Lines ureters and urinary bladder Stratified squamous epithelium Found where mechanical stresses are severe Surface of the skin, lining of mouth, tongue and esophogus Figure 4 – 4 and 4 – 5, pgs. 95&96 Glandular Epithelia Produce exocrine or endocrine secretions Exocrine Discharge products through a duct onto some internal or external surface Can be characterized as unicellular glands (goblet cells) or multicellular glands (secretory sheet) Endocrine (hormones) Produced by ductless glands and released into blood or tissues Mode of Secretion Each glandular cell releases secretions by one of three mechanisms: 1. Merocrine secretion Apocrine secretion 2. 3. Most common mode of secretion Product released in vesicles by exocytosis Mucus Involves loss of both cytoplasm and secretory product Outermost portion of cytoplasm becomes packed with secretory vesicles and is the shed Holocrine secretion Entire sell becomes packed with secretions and then bursts apart and dies Sebaceous glands Modes of Secretion Type of Secretion Exocrine glands can be categorized as serous, mucous or mixed Serous Glands Watery solution containing enzymes Mucous glands Secrete mucins that form a thick, slippery mucus Mixed glands Contain both serous and mucous glands together Connective Tissues All have three basic components: Specialized cells 2. Protein fibers 3. Fluid known as ground substance 1. Protein fibers and ground substance form the matrix that surrounds the cells Accounts for most of the volume of connective tissue Connective Tissue Functions Support and Protection Bony structural framework Protect delicate organs Transportation of materials Fluid connective tissues Storage of energy reserves Adipose cells (fat) Defense of the body Antibodies Classifying Connective Tissues Connective tissue proper 1. Many types of cells and matrix fibers in a ground substance Tissue under skin, fatty tissue, and tendons and ligaments Fluid connective tissues 2. Distinct cells in a watery ground substance with dissolved proteins Blood and lymph Supporting connective tissues 3. Matrix of dense ground substance and closely packed fibers Cartilage and bone Connective Tissue Proper Some cells are “permanent residents,” and others are not always present because they leave to defend and repair areas of injured tissue The Cell Population Fibroblasts – most abundant cells Produce and maintain connective tissue fibers and ground substance Macrophages – “big eater” cells Phagocytize damaged cells or pathogens Mobilize immune system Fat cells – adipocytes Large droplet of lipid that pushes nucleus and organelles to one side of the cell Mast cells – found near blood vessels release chemicals to begin body’s defensive activities after an injury or infection Antibodies, white blood cells and stem cells Connective Tissue Fibers Collagen fibers 1. Long, straight and unbranched Strong and flexible, most common Elastic fibers – contain protein elastin 2. After stretching return to original length Reticular fibers – least common 3. Commonly form a branching, interwoven framework in various organs Ground Substance Fills spaces between cells and surrounds fibers Clear, colorless and has consistency of maple syrup Slows movement of bacteria and other pathogens Loose Connective Tissue Areolar tissue Contains all cells and fibers found in connective tissue proper Extensive blood supply Forms a layer that separates the skin from underlying muscles Provides padding and allowing movement Adipose Tissue; Figure 4 – 9 pg. 102 Loose connective tissue containing large numbers of fat cells Provides more padding and shock absorption for body Insulation and energy storage Dense connective tissue Mostly collagen fibers Two types: dense regular and dense irregular Dense regular connective tissue Collagen fibers packed tightly, parallel to one another Tendons – attach muscle to bone Ligaments – attach bone to bone; often contain elastic fibers Dense irregular connective tissue Interwoven network of collagen fibers Provides support to areas subjected to stresses from many directions Fluid Connective Tissues Blood and lymph Proteins dissolved in watery matrix do not form fibers Watery matrix is plasma in blood Red blood cell – makes up ½ of volume of blood Transport oxygen White blood cell – component of immune system Platelets – cell fragments that function in blood clotting Lymph forms as interstitial fluid enters small passageways, or lymphatic vessels Cells of immune system monitor the composition of lymph Supporting Connective Tissues Cartilage and bone Cartilage Matrix of a firm gel with embedded fibers Chondrocytes – only cells found in matrix Live in small pockets called lacunae Avascular – limits repair capabilities Perichondrium Structure that separates cartilage from surrounding tissues TYPES OF CARTILAGE Hyaline cartilage – most common 1. Closely packed collagen fibers Tough but flexible Connects ribs to sternum, supports respiratory tract, and covers opposing bone surfaces Elastic cartilage – numerous elastic fibers 2. Elastic flap of ear and epiglottis Fibrocartilage – little ground substance, lots of collagen 3. Extremely durable and tough Spinal column, between pubic bones and pelvis and in a few joints Resist compression, absorb shocks and prevent damaging bone – bone contact Figure 4 – 10, page 104 Bone (osseous tissue) Lacunae contain osteocytes (bone cells) and surround blood vessels Canaliculi Branching network within bony matrix Periosteum Covering of bone that has outer fibrous and inner cellular layers Table 4 – 3 page 105 Membranes Form barriers or cover and protect structures and tissues Four types: Mucous membranes 2. Serous membranes 3. Cutaneous membranes 4. Synovial membranes 1. Mucous Membranes aka mucosae, line cavities that communicate with exterior Kept moist at all times Most lined by simple epithelia Also simple columnar, stratified squamous and transitional squamous Line the digestive, respiratory, reproductive and urinary tracts Serous Membranes Line the sealed, internal subdivisions of the ventral body cavity Three kinds: Pleura – covering the lungs 2. Peritoneum – lines organs of abdominal cavities 3. Pericardium – covers the heart 1. Has parietal and visceral portions Friction is reduced by water, serous fluid The Cutaneous Membrane Skin Covers surface of the body Thick, relatively waterproof, and usually dry Synovial Membranes Joins or articulations are surrounded by a synovial membrane Ends of bones are covered by hyaline cartilage and separated by viscous synovial fluid Helps lubricate the joint and permits smooth movement Muscle Tissue Specialized for contraction Involves interaction between filaments of myosin and actin Three types in the body: Cardiac 2. Skeletal 3. Smooth 1. Skeletal Muscle Tissue Contains large, multinucleated cells Are usually called muscle fibers Produced through division of stem cells Partial repairs can occur after injury Marked by a series of bands called striations Nervous system provides voluntary control over its activities Striated voluntary muscle Cardiac Muscle Tissue Only found in the heart Cells are interconnected at intercalated discs Specialized attachment sites containing gap junctions and desmosomes Very limited ability to repair itself Do NOT rely on nerve activity Specialized cells called pacemaker cells establish a regular rate of contraction striated involuntary muscle Smooth Muscle Tissue Walls of blood vessels, around hollow organs, and in layers around the respiratory, circulatory, digestive and reproductive tracts No striations Cells are able to divide Regenerate after injury Nonstriated involuntary muscle Neural Tissue Specialized for conduction of electrical impulses from one region of the body to another Two types of cells: Neurons – communicate through electrical events that affect their cell membranes Neuroglia - provide physical support for neural tissue, maintain the chemical composition of the tissue fluids, supply nutrients to neurons and defend the tissue from infection Neurons Longest cells in your body (up to 39 in.) Cannot divide – very limited ability to repair themselves Contain three parts: Cell body – w/ large nucleus 2. Dendrites – numerous branching projections 3. Axon – long and slender part, communicate with other cells 1. End at synaptic terminals Tissue Injuries and Repair Inflammation – area is isolated from healthy tissue while damaged cells are cleaned up. Swelling, warmth, redness and pain Regeneration – second phase of following injury Fibroblasts produce dense network of collagen fibers known as scar tissue or fibrous tissue Over time, scar tissue is remodeled and resumes normal appearance Is more successful in some tissues than others Permanent replacement of normal tissues is called fibrosis