* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Device Closure for Ventricular Septal Defect After Myocardial Infarction
Electrocardiography wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Cardiac surgery wikipedia , lookup
Coronary artery disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
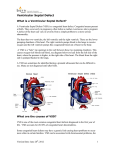
COVER STORY Device Closure for Ventricular Septal Defect After Myocardial Infarction An overview of the potential use of transcatheter options to treat anatomically suitable patients with postmyocardial infarction VSD. BY NIKOLAOS KAKOUROS, BSC, MBBS, MRCP, AND STEPHEN J.D. BRECKER, MD, FRCP, FESC, FACC A (LAD) coronary artery that supplies both the anterior and inferior apical septum, with extensive myocardial damage and poor septal collateral blood supply are at increased risk of developing septal rupture.9-12 There is a higher incidence of triple-vessel disease in autopsy series, but this may reflect bias due to these patients being less likely to survive the septal rupture event.13 (Courtesy of AGA Medical Corporation.) cquired ventricular septal defect (VSD) is one of the three major mechanical complications of acute myocardial infarction (AMI), the other two being acute mitral regurgitation and rupture of the ventricular free wall. Although ventricular septal rupture was described on autopsy as early as 1847, its clinical correlation with AMI was not established until almost 100 years later.1 In the era before thrombolysis, VSD was not an infrequent complication of AMI, occurring in as many as 1% to 3% of patients.2-5 With the advent of early reperfusion strategies and adjunct medical therapy, the incidence of this complication has significantly decreased to < 1% of cases (0.2% in the Global Utilization of Streptokinase and Tissue Plasminogen Activator for Occluded Coronary Arteries-I [GUSTO-I] trial)6 but remains associated with a high morbidity and mortality. Data on the impact of primary percutaneous coronary intervention (PPCI) on the incidence of VSD are limited, but a study of 1,321 patients by Yip et al suggested a significant impact on the incidence of this complication (0.23% with PPCI vs 3% with no acute reperfusion therapy; P = .0001).7 Development of a VSD correlates with delayed hospital admission after the infarction (> 24 hours) and may be triggered by undue physical activity in the early postinfarction (PI) period, as well as recurrent ischemia.8 Risk factors include age > 60 years, female gender, no history of previous MI, and hypertension. Patients with single-vessel disease, particularly of a wrap-around left anterior descending Figure 1. The Amplatzer PI muscular VSD occluder (AGA Medical Corporation, Plymouth, MN). Note the longer waist (10 mm) compared to the muscular VSD Amplatzer device. NOVEMBER 2009 I CARDIAC INTERVENTIONS TODAY I 43 COVER STORY VSDs tend to occur 3 to 8 days after the index AMI but may also occur within the first 24 hours, or as late as 2 weeks.2,5,13 Fibrinolysis may promote the breakdown of the necrosing septum, and reperfusion injury can result in hemorrhagic infarct leading to earlier VSD development. The median time from AMI symptoms to VSD diagnosis was just 1 day in the GUSTO-I thrombolysis trial6 and 16 hours in the Should We Emergently Revascularize Occluded Coronaries in Cardiogenic Shock (SHOCK) trial,14 with a tendency for earlier timing of rupture also noted in the more recent PPCI study.7 Transmural tissue necrosis causes loss of structural integrity with a dynamic perforation of the interventricular septum at the interface of necrotic and nonnecrotic myocardium. The defect is most often at the apical septum in anterior AMIs and the base of the heart after inferior AMIs, with the orifice varying from 1 to several centimeters in diameter.13 The architecture may be complex with serpiginous tunnels traversing the interventricular septum, particularly in ruptures involving the inferobasal septum, and multiple orifices can, less commonly, occur. Intramural extension with dissection of the interventricular septum or, rarely, the right ventricular free wall may occur.15-17 DIAGNOSIS AND IMAGING Diagnosis traditionally involved the passage of pulmonary artery balloon catheters to document the left-to-right shunt but is now achieved reliably and less invasively with Doppler transthoracic echocardiography (TTE). On TTE, VSD is suggested by a new regional wall motion abnormality suggestive of AMI and protrusion of the interventricular septum at this site toward the right ventricle. Doppler interrogation reveals a high-velocity, left-to-right ventricular shunt in almost all cases. Transesophageal echocardiography (TEE) may be occasionally necessary to establish the extent of the defect, particularly in the case of inferior infarction.18,19 Severity of the intraventricular shunt varies depending on the size of the defect, but most patients are clinically gravely ill with incipient or established cardiogenic shock. Even the minority of patients who are initially stable tend to develop rapid, progressive, or unexpected hemodynamic compromise. In addition to hypotension, patients have clinical evidence of biventricular (although predominantly right heart) failure and a loud, harsh, holosystolic parasternal murmur associated with a thrill in as many as 50% of cases. MANAGEMENT The prognosis of post-AMI VSD is very poor, with mortality rates as high as 50% at 1 week and 90% at 2 months with conservative medical treatment.13 Acute surgery is technically complicated by the myocardial tissue being soft and friable. Retrospective studies have suggested that better sur44 I CARDIAC INTERVENTIONS TODAY I NOVEMBER 2009 Figure 2. Transcatheter closure of PI VSD. Fluoroscopy shows the Amplatzer PI muscular VSD occluder device fully deployed and released. gical results were obtained in patients in whom surgery was delayed by 6 weeks until some myocardial fibrosis had occurred compared to operating during the acute phase.5,20,21 Although scarring at the tissue edges certainly permits better hold of the sutures and a more secure and long-lasting closure, the apparent favorable outcome of delayed surgery more likely reflects a selection bias, with hemodynamically stable patients with small defects selfselecting by surviving to a relatively lower-risk interim operation. Delaying surgery in hemodynamically stable patients engenders the risk of unpredictable and catastrophic deterioration, and multiple studies support rapid intervention.22-26 Coronary artery bypass grafting for underlying coronary disease at the time of VSD repair significantly improves longterm survival compared to VSD repair alone;27,28 consequently, evaluation of the coronary anatomy by cardiac catheterization is indicated before undertaking surgical repair of post-AMI VSD. The joint American Heart Association/American College of Cardiology (AHA/ACC) 2004 Guidelines recommend emergent repair of the VSD with concurrent coronary artery bypass grafting, as indicated, irrespective of hemodynamic status,29,30 with no change in this class I recommendation on the 2007 ACC/AHA focused guideline update.31 In-hospital mortality after surgery is significantly lower than with conservative management but remained as high as 47% in the GUSTO-I trial.6,32-34 A residual shunt persists in 10% to 37% of patients after surgery due to an overlooked additional defect or development of a new VSD such that up to 11% of patients may require a further surgical procedure.35 Patch dehiscence may COVER STORY Figure 3. Postmortem photograph of the heart showing an Amplatzer device in situ across an interventricular septal defect from a patient who died despite successful device implantation. also occur because the sutures may tear out of the friable, recently infracted myocardium. The long-term prognosis of patients who survive the acute 30-day postoperative period is, however, good.6 TR ANSCATHETER POST-AMI VSD CLOSURE Early surgery is considered the gold standard for postinfarction VSD, with the high surgical risk being acceptable in the face of the even higher risk of death without surgery. More recently, however, an additional option of percutaneous closure of the rupture has become available. Transcatheter closure of the VSD was initially reported in patients deemed to be at too high risk for surgical repair due to their recent post-AMI status, advanced age, severe coronary artery disease, hemodynamic instability, and added comorbidity (such as renal failure and diabetes mellitus). Transcatheter closure was also used in patients with residual leak after VSD repair surgery at excessive risk of a repeat surgical operation that ranges from 13% to 31%.35-37 Lately, the use of transcatheter VSD closure as primary therapy for post-AMI VSD has emerged. After the initial report by Lock et al in 1988 using the Rashkind double umbrella,38 various devices have been used, including the Clamshell occluder (USCI Angiographics, Tewksbury, MA),39 the CardioSeal (NMT Medical, Boston, MA),40 and the Amplatzer septal occluder (AGA Medical Corporation).37 Previous experience with congenital VSDs has found the Amplatzer system to have a higher success rate than other devices,41,42 and extrapolation of this experience has led to the tendency to also use this family of devices for the closure of acquired post-AMI ventricular septal ruptures. The Amplatzer muscular VSD occluder is a self- expanding, single-unit nitinol device with incorporated polyester fabric that comprises two discs connected by a 7mm-long waist portion, compared with a 4-mm waist in the atrial septal defect (ASD) device. The device is sized between 4 and 18 mm by the diameter of the central waist, with the discs being 8 mm larger than this segment. The device is secured onto a delivery cable and implanted via a 5- to 9-F diameter sheath. It is self-centering and permits several positioning attempts because it is retrievable before release. Specially designed devices for the closure of post-AMI VSDs have also become available. The Amplatzer PI muscular VSD device has larger disks and a longer waist (10 mm) than the muscular VSD Amplatzer device to accommodate the thicker adult interventricular septum. It is available in sizes of 16 to 24 mm in 2-mm increments, as determined by the diameter of the waist section (Figure 1). It requires a minimum 9- to 10-F sheath for delivery. The newer sheaths include wire braiding that obviates the previously troublesome risk of kinking. In some cases, the Amplatzer cribriform septal occluder and the CardioSeal septal occluder have been used to address multifenestrated defects.15,19 TECHNIQUES Antibiotic prophylaxis is administered periprocedure, and full heparinization is maintained for up to 24 hours. Antiplatelet therapy is administered for at least 6 months to protect the device but should probably be given to the patient lifelong in view of the AMI. Endocarditis prophylaxis is commonly recommended for 6 months or indefinitely for patients with residual shunts based on congenital ASD/VSD closure practice. The procedure is usually performed with fluoroscopic control under general anesthesia to permit intraoperative TEE. The use of real-time three-dimensional TEE to provide detailed assessment of the defect orifice and to guide the closure procedure has been recently reported.43 Procedure under conscious sedation is also possible for apical defects adequately visualized by TTE.19 Intracardiac echocardiography may prove a suitable alternative, but reports on its use in this setting are lacking. The defect anatomy and size are carefully evaluated using axial projection left ventriculography and multiple echocardiographic views. The orifice size measured on echocardiography forms the basis for the decision of what size of device to use. Intraoperative echocardiography also helps guide catheter manipulations, positioning, and deployment of the occluder device. Echocardiographic dropout due to the catheter may occasionally appear as a residual tissue defect, but careful assessment by color Doppler duplex echocardiography can help differentiate the two. NOVEMBER 2009 I CARDIAC INTERVENTIONS TODAY I 45 COVER STORY TABLE 1. TRANSCATHETER CLOSURE OF POSTMYOCARDIAL INFARCTION VSD WITH AMPLATZER OCCLUDER DEVICESa Total N Acute S/C Success of Patients (N Patients) (N Patients) Rate Chessa44 2002 12 Szkutnik45 7 2003 Goldstein46 4 2003 Holzer47, 48 18 2004 Demkow49 11 2005 Martinez50 5 2007 Bialkowski51 19 2007 Marinakis52 8 2007 Ahmed53 5 2008 Maltais24 12 2009 29 Thiele54 2009 Total N 130 Survival at 30 Days Residual Shunts Acute S/C Small/ Trivial Moderate/ Severe 3 9 11/12 0/3 8/9 0 0 0 7 5/7 - 4/5 3 1 0 4 3/4 - 3/3 2 2 5 13 16/18 2/5 9/13 8 2 3 8 10/11 0/2 8/8 4 0 3 2 5/5 2/3 2/2 3 1 1 18 14/19 0/1 9/13 9 3 6 2 7/8 0/6 1/2 0 0 2 3 4/5 0/1 3/3 3 1 12 0 11/12 7/11 - 10 1 29 0 25/29 10/29 - 6 4 64 66 111/130 21/61 47/58 48/111 15/111 85 34 81 43 14 Total % Abbreviations: N, number; S/C, subacute/chronic. aLiterature review for published series. Acute phase is considered the period within 14 days from the index infarction event, and the subacute/chronic phase is if closure was performed beyond this time period. The standard technique for muscular septum device implantation has been described in the literature.44,47,55-60 In brief, a Judkins right catheter is advanced retrogradely via the aortic valve to the left ventricle from a peripheral arterial access point. Access to the left ventricle via an atrial transseptal puncture has also been described when peripheral arterial access is not possible.61 The defect is then crossed from left to right using a soft wire that is advanced to the pulmonary artery or superior vena cava. The catheter may then be advanced to the right ventricle and the wire 46 I CARDIAC INTERVENTIONS TODAY I NOVEMBER 2009 exchanged for a more supportive 260-cm or 400-cm wire. Venous access is established via the right internal jugular vein, where a snare (such as an Amplatz Gooseneck, ev3 Inc., Plymouth, MN) is introduced to capture and exteriorize the transseptal wire creating an arteriovenous guidewire circuit. Balloon sizing of the defect may be performed by three principal methods. First, an OBW balloon may be placed in the left ventricle and expanded with dilute contrast to a volume that produces VSD occlusion on TEE when COVER STORY pulled gently against the defect and such that it can just be pulled through the defect. The diameter at this volume is then measured ex vivo and used to guide device size selection. Alternatively, the stop-flow technique may be used when a longer compliant balloon is placed across the defect and measured at the volume at which shunting is eliminated on Doppler echocardiography (not to the point of waist formation). Finally, an Amplatzer sizing balloon (AGA Medical Corporation) may be inflated across the defect and the stretched defect diameter measured as the balloon waist size. An occluder with a waist sized 1 to 7 mm larger than the maximal measured defect diameter is then selected.19,48 There are concerns regarding the use of these techniques in the setting of post-AMI VSD, because the tissue at the edges of the defect can be very friable, and application of pressure may easily lead to VSD enlargement, particularly with the last method. Some interventionists have, therefore, abandoned balloon sizing altogether (even in the non-AMI setting) and use two-dimensional TEE or even TTE measurements, oversizing the device by 2 to 8 mm and up to 50% above this reading to reduce the incidence of device embolization or residual shunt.44,49,54 The delivery sheath is then advanced from the venous side to the left ventricular cavity over the wire, and the dilator and wire are gently removed. The selected occluder device is then delivered to the left ventricle. The device is extruded from the sheath until the left ventricular disc is opened and then withdrawn toward the interventricular septum. After further satisfactory left ventriculography and echocardiographic evaluation of septal alignment, the proximal right ventricular disc is also deployed, and the device is released from the delivery cable (Figure 2). RESULTS AND COMPLICATIONS Outcomes using Amplatzer devices have been reported in multiple single-case reports but also in a number of case series studies, which are summarized in Table 1. Percutaneous device implantation was either the primary therapy or was used to treat a residual shunt after primary surgical VSD closure. The results of these series must be cautiously evaluated against surgical outcomes because the numbers in each series are small, and patients were not randomized, leading inevitably to a degree of patient selection bias. This bias may favor the percutaneous option—because larger, more complex defects are excluded due to lack of anatomical suitability—or favor surgery as higher-risk surgical candidates are referred for transcatheter device therapy. The largest series to date, including 29 consecutive unselected patients with VSD who underwent primary transcatheter closure, was reported earlier this year by Thiele et al.54 In total, 130 patients are reported in these 11 series, 64 of whom were treated in the acute phase after AMI. In the remaining 66 patients, the procedure was performed at least 14 days after the index infarction event. The overall device implantation success rate was 85% (95% confidence interval [CI] for mean, 81%–90%), with no significant difference between the acute and subacute/chronic phase patients. Despite successful device implantation, the morbidity and mortality remain very high when the procedure is performed in the acute phase, especially for patients in cardiogenic shock (Figure 3). The 30-day survival was 34% (95% CI, 10%–58%) in the acute phase patients, compared to an encouraging 81% (95% CI, 71%–91%) in the subacute/chronic group. In the recent large series, five of 29 patients died in the catheterization laboratory from procedure-related complications.54 Subsequent in-hospital death is attributed in the series to ventricular failure secondary to extensive infarction or associated comorbidity, such as renal failure, multiorgan failure, and sepsis.15,52 As for surgical repair, if a transcatheter procedure is technically feasible, it is prudent not to delay it, because secondary complications may ensue and impair subsequent prognosis even if the VSD is subsequently adequately corrected. Transient complete atrioventricular block is reported,15,49,51,54 but the long-term need for permanent pacing system implantation is unclear. Ventricular tachycardia or fibrillation, or atrial fibrillation requiring cardioversion may also arise.40,45 Contrast medium nephropathy may develop secondary to the implantation procedure, although the relative contribution of this to subsequent morbidity and mortality is difficult to dissect from preexisting renal impairment or nephropathy due to low cardiac output. Iatrogenic right or left ventricular free wall perforation and tamponade has also been reported.24,51,54,62 Device migration, although of primary concern in transcatheter device closure, is rare and associated with treatment of larger defects; it tends to be associated with incorrect device sizing, inaccurate deployment, and operator inexperience. Treatment of basal defects may lead to trapping of mitral or tricuspid chordae and interference with the aortic valve leading to valvular regurgitation. Although this is a concern stemming from treatment of perimembranous congenital VSDs, it does not appear to be a significant reported problem in the VSD literature. The rate of complete closure with no or small-volume residual shunting is reduced in the acute setting because the peri-VSD tissue may subsequently necrose and scar, resulting in retraction from the device causing an increasing shunt.47,52 Residual shunting after device implantation may need to be addressed by interval surgery or deployment of additional devices.44,45,48,63 On pooling the literature series data NOVEMBER 2009 I CARDIAC INTERVENTIONS TODAY I 47 COVER STORY (Table 1), small or trivial shunts remain in approximately 43% (95% CI, 27%–59%) of patients, and moderate-tosevere shunts remain in 15% (95% CI, 0%–34%), rates similar to surgical data. PATIENT SELECTION Not all patients are anatomically suitable for transcatheter closure. The exact position of the defect, its anatomy (simple vs complex), and its size affect the likelihood of successful deployment and subsequent stability of a percutaneously implanted device. Consequently, careful assessment by two-dimensional/three-dimensional TTE or TEE and (when hemodynamic stability permits) cardiac magnetic resonance imaging is important in patient selection.64 Maltais et al recently reported their single-center experience in which small or medium VSDs were preferentially treated with a transcatheter device, and defects larger than 15 mm (< 10 mm smaller than the largest available Amplatzer occluder) were considered for surgery, with no significant in-hospital or 30-day mortality outcome between the two groups. In the Amplatzer muscular VSD occluder US registry, exclusion criteria were more lenient, with defects up to 24 mm (maximum available device size) treated successfully with no reports of device embolization.48 In the more recent study by Thiele et al, patients with defects up to 35 mm were accepted, but the incidence of device dislocation was a relatively high 17% (five of 29 patients).54 Nonetheless, the paradigm may prove useful as the basis of a patient selection algorithm, with patients who have defects anatomically suitable for percutaneous closure being referred for primary transcatheter therapy and patients with larger, more complex or multiple defects preferentially referred for surgery. CONCLUSION Transcatheter device closure is an accepted alternative to medical therapy or surgery for congenital VSDs, and the application of the technology to the post-AMI VSD is expanding. Although cardiac surgery with concurrent coronary artery bypass grafting, as indicated, remains the gold standard, a significant proportion of patients are at too high risk for surgery due to their post-AMI status, cardiogenic shock, and comorbidities. Transcatheter device placement may provide a stabilization bridge to urgent surgery or even permit deferral of surgery until the peri-VSD tissue has strengthened.65 There is increasing evidence supporting the use of transcatheter device placement as a definitive primary treatment for anatomically suitable patients, and the procedure may also provide an alternative to repeat surgery for patients with residual shunts and patch dehiscence.37-39,66 Patients with large or multiple defects are best treated surgi48 I CARDIAC INTERVENTIONS TODAY I NOVEMBER 2009 cally when possible because the risk of transcatheter device embolization in this group may be greater.24 A multidisciplinary team, including interventional cardiologists and cardiac surgeons, should evaluate these high-risk patients to determine the optimal management strategy. Large series are needed in the future to further compare percutaneous with surgical options, as well as different occlusion devices, although the feasibility of randomized trials is likely to prove limited given the rarity, anatomic variability, and hemodynamic instability of these patients. Finally, the currently available devices do have significant shortcomings. They have been criticized for the rigid sheath that may traumatize and enlarge the VSD and for the requirement to remove the guidewire before device deployment such that the arteriovenous circuit is lost should the chosen device dislocate into the right ventricle. Furthermore, devices come in a limited range of sizes, and closure of the shunt in the acute period may be suboptimal because the polyester fabric requires time to thrombose and endothelialize before being efficient in preventing shunt across the high transventricular pressure gradient.54 Some of these shortcomings are being addressed,67 and newer devices are eagerly awaited. ■ Nikolaos Kakouros, BSc, MBBS, MRCP, is an interventional cardiology postdoctoral research fellow at the Johns Hopkins University in Baltimore, Maryland. He has disclosed that he holds no financial interest in any product or manufacturer mentioned herein. Dr. Kakouros may be reached at (410) 5026133; [email protected]. Stephen J.D. Brecker, MD, FRCP, FESC, FACC, is a consultant cardiologist at St George’s Hospital in London, United Kingdom. He has disclosed that he holds no financial interest in any product or manufacturer mentioned herein. Dr. Brecker may be reached at +44-(0)20-8725-3556; [email protected]. 1. Sager RV. Coronary thrombosis: perforation of the infarcted interventricular septum. Arch Intern Med. 1934;53:140-152. 2. Topaz O, Taylor AL. Interventricular septal rupture complicating acute myocardial infarction: from pathophysiologic features to the role of invasive and noninvasive diagnostic modalities in current management. Am J Med. 1992;93:683-688. 3. Heitmiller R, Jacobs ML, Daggett WM. Surgical management of postinfarction ventricular septal rupture. Ann Thorac Surg. 1986;41:683-691. 4. Pohjola-Sintonen S, Muller JE, Stone PH, et al. Ventricular septal and free wall rupture complicating acute myocardial infarction: experience in the Multicenter Investigation of Limitation of Infarct Size. Am Heart J. 1989;117:809-818. 5. Moore CA, Nygaard TW, Kaiser DL, et al. Postinfarction ventricular septal rupture: the importance of location of infarction and right ventricular function in determining survival. Circulation. 1986;74:45-55. 6. Crenshaw BS, Granger CB, Birnbaum Y, et al. Risk factors, angiographic patterns, and outcomes in patients with ventricular septal defect complicating acute myocardial infarction. GUSTO-I (Global Utilization of Streptokinase and TPA for Occluded Coronary Arteries) Trial Investigators. Circulation. 2000;101:27-32. 7. Yip HK, Fang CY, Tsai KT, et al. The potential impact of primary percutaneous coronary intervention on ventricular septal rupture complicating acute myocardial infarction. Chest. 2004;125:1622-1628. 8. Figueras J, Cortadellas J, Calvo F, et al. Relevance of delayed hospital admission on development of cardiac rupture during acute myocardial infarction: study in 225 patients with free wall, septal or papillary muscle rupture. J Am Coll Cardiol. 1998;32:135-139. COVER STORY 9. Radford MJ, Johnson RA, Daggett WM Jr, et al. Ventricular septal rupture: a review of clinical and physiologic features and an analysis of survival. Circulation. 1981;64:545-553. 10. Skehan JD, Carey C, Norrell MS, et al. Patterns of coronary artery disease in post-infarction ventricular septal rupture. Br Heart J. 1989;62:268-272. 11. Pretre R, Rickli H, Ye Q, et al. Frequency of collateral blood flow in the infarct-related coronary artery in rupture of the ventricular septum after acute myocardial infarction. Am J Cardiol. 2000;85:497-499, A10. 12. Birnbaum Y, Wagner GS, Gates KB, et al. Clinical and electrocardiographic variables associated with increased risk of ventricular septal defect in acute anterior myocardial infarction. Am J Cardiol. 2000;86:830-834. 13. Edwards BS, Edwards WD, Edwards JE. Ventricular septal rupture complicating acute myocardial infarction: identification of simple and complex types in 53 autopsied hearts. Am J Cardiol. 1984;54:1201-1205. 14. Menon V, Webb JG, Hillis LD, et al. Outcome and profile of ventricular septal rupture with cardiogenic shock after myocardial infarction: a report from the SHOCK Trial Registry. Should we emergently revascularize Occluded Coronaries in cardiogenic shock? J Am Coll Cardiol. 2000;36:1110-1116. 15. Giombolini C, Notaristefano S, Santucci S, et al. Transcatheter closure of postinfarction ventricular septal defect using the Amplatzer atrial septal defect occluder. J Cardiovasc Med. 2008;9:941-945. 16. Paul S, Mihaljevic T, Leacche M, et al. Postinfarction ventricular septal defect with pseudoaneurysm repair after failed percutaneous closure. Ann Thorac Surg. 2005;79:701-703. 17. Tighe DA, Paul JJ, Maniet AR, et al. Survival in infarct related intramyocardial dissection: importance of early echocardiography and prompt surgery. Echocardiography. 1997;14:403-408. 18. St John Sutton MG, Maniet AR. Atlas of multiplane transesophageal echocardiography. Evaluation of the cardiac chambers, and pericardium: structure and function. Vol. 2. London, England: Martin Dunitz; 2003: 487. 19. Szkutnik M, Kusa J, Bialkowski J. The use of two Amplatzer “cribriform” septal occluders to close multiple postinfarction ventricular septal defects. Tex Heart Inst J. 2008;35:362-364. 20. Deville C, Fontan F, Chevalier JM, et al. Surgery of post-infarction ventricular septal defect: risk factors for hospital death and long-term results. Eur J Cardiothorac Surg. 1991;5:167-174; discussion 75. 21. Held AC, Cole PL, Lipton B, et al. Rupture of the interventricular septum complicating acute myocardial infarction: a multicenter analysis of clinical findings and outcome. Am Heart J. 1988;116:1330-1336. 22. Pretre R, Ye Q, Grunenfelder J, et al. Operative results of “repair” of ventricular septal rupture after acute myocardial infraction. Am J Cardiol. 1999;84:785-788. 23. Scanlon PJ, Montoya A, Johnson SA, et al. Urgent surgery for ventricular septal rupture complicating acute myocardial infarction. Circulation. 1985;72:II185-II190. 24. Maltais S, Ibrahim R, Basmadjian AJ, et al. Postinfarction ventricular septal defects: towards a new treatment algorithm? Ann Thorac Surg. 2009;87:687-692. 25. David TE. Operative management of postinfarction ventricular septal defect. Semin Thorac Cardiovasc Surg. 1995;7:208-213. 26. Daggett WM. Postinfarction ventricular septal defect repair: retrospective thoughts and historical perspectives. Ann Thorac Surg. 1990;50:1006-1009. 27. Muehrcke DD, Daggett WM Jr, Buckley MJ, et al. Postinfarct ventricular septal defect repair: effect of coronary artery bypass grafting. Ann Thorac Surg. 1992;54:876-882; discussion 82-83. 28. Cox FF, Plokker HW, Morshuis WJ, et al. Importance of coronary revascularization for late survival after postinfarction ventricular septal rupture. A reason to perform coronary angiography prior to surgery. Eur Heart J. 1996;17:1841-1845. 29. Antman EM, Anbe DT, Armstrong PW, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction—executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1999 Guidelines for the Management of Patients With Acute Myocardial Infarction). Circulation. 2004;110:588-636. 30. Eagle KA, Guyton RA, Davidoff R, et al. ACC/AHA 2004 guideline update for coronary artery bypass graft surgery: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1999 Guidelines for Coronary Artery Bypass Graft Surgery). Circulation. 2004;110:e340-3437. 31. Antman EM, Hand M, Armstrong PW, et al. 2007 Focused Update of the ACC/AHA 2004 Guidelines for the Management of Patients With ST-Elevation Myocardial Infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines: developed in collaboration With the Canadian Cardiovascular Society endorsed by the American Academy of Family Physicians: 2007 Writing Group to Review New Evidence and Update the ACC/AHA 2004 Guidelines for the Management of Patients With ST-Elevation Myocardial Infarction, Writing on Behalf of the 2004 Writing Committee. Circulation. 2008;117:296-329. 32. Bolooki H. Emergency cardiac procedures in patients in cardiogenic shock due to complications of coronary artery disease. Circulation. 1989;79:I137-I148. 33. Davies RH, Dawkins KD, Skillington PD, et al. Late functional results after surgical closure of acquired ventricular septal defect. J Thorac Cardiovasc Surg. 1993;106:592-598. 34. Jones MT, Schofield PM, Dark JF, et al. Surgical repair of acquired ventricular septal defect. Determinants of early and late outcome. J Thorac Cardiovasc Surg. 1987;93:680-686. 35. Deja MA, Szostek J, Widenka K, et al. Post infarction ventricular septal defect - can we do better? Eur J Cardiothorac Surg. 2000;18:194-201. 36. Skillington PD, Davies RH, Luff AJ, et al. Surgical treatment for infarct-related ventricular septal defects. Improved early results combined with analysis of late functional status. J Thorac Cardiovasc Surg. 1990;99:798-808. 37. Lee EM, Roberts DH, Walsh KP. Transcatheter closure of a residual postmyocardial infarction ventricular septal defect with the Amplatzer septal occluder. Heart. 1998;80:522-524. 38. Lock JE, Block PC, McKay RG, et al. Transcatheter closure of ventricular septal defects. Circulation. 1988;78:361-368. 39. Landzberg MJ, Lock JE. Interventional catheter procedures used in congenital heart disease. Cardiol Clin. 1993;11:569-587. 40. Pienvichit P, Piemonte TC. Percutaneous closure of postmyocardial infarction ventricular septal defect with the CardioSeal septal occluder implant. Catheter Cardiovasc Interv. 2001;54:490494. 41. Arora R, Trehan V, Kumar A, et al. Transcatheter closure of congenital ventricular septal defects: experience with various devices. J Interv Cardiol. 2003;16:83-91. 42. Michel-Behnke I, Le TP, Waldecker B, et al. Percutaneous closure of congenital and acquired ventricular septal defects—considerations on selection of the occlusion device. J Interv Cardiol. 2005;18:89-99. 43. Halpern DG, Perk G, Ruiz C, et al. Percutaneous closure of a post-myocardial infarction ventricular septal defect guided by real-time three-dimensional echocardiography. Eur J Echocardiogr. 2009;10:569-571. 44. Chessa M, Carminati M, Cao QL, et al. Transcatheter closure of congenital and acquired muscular ventricular septal defects using the Amplatzer device. J Invasive Cardiol. 2002;14:322-327. 45. Szkutnik M, Bialkowski J, Kusa J, et al. Postinfarction ventricular septal defect closure with Amplatzer occluders. Eur J Cardiothorac Surg. 2003;23:323-327. 46. Goldstein JA, Casserly IP, Balzer DT, et al. Transcatheter closure of recurrent postmyocardial infarction ventricular septal defects utilizing the Amplatzer postinfarction VSD device: a case series. Catheter Cardiovasc Interv. 2003;59:238-243. 47. Holzer R, Balzer D, Cao QL, et al. Device closure of muscular ventricular septal defects using the Amplatzer muscular ventricular septal defect occluder: immediate and mid-term results of a U.S. registry. J Am Coll Cardiol. 2004;43:1257-1263. 48. Holzer R, Balzer D, Amin Z, et al. Transcatheter closure of postinfarction ventricular septal defects using the new Amplatzer muscular VSD occluder: results of a U.S. Registry. Catheter Cardiovasc Interv. 2004;61:196-201. 49. Demkow M, Ruzyllo W, Kepka C, et al. Primary transcatheter closure of postinfarction ventricular septal defects with the Amplatzer septal occluder- immediate results and up-to 5 years followup. EuroIntervention. 2005;1:43-47. 50. Martinez MW, Mookadam F, Sun Y, et al. Transcatheter closure of ischemic and post-traumatic ventricular septal ruptures. Catheter Cardiovasc Interv. 2007;69:403-407. 51. Bialkowski J, Szkutnik M, Kusa J, et al. Transcatheter closure of postinfarction ventricular septal defects using Amplatzer devices. Rev Esp Cardiol. 2007;60:548-551. 52. Marinakis A, Vydt T, Dens J, et al. Percutaneous transcatheter ventricular septal defect closure in adults with Amplatzer septal occluders. Acta Cardiol. 2007;62:391-395. 53. Ahmed J, Ruygrok PN, Wilson NJ, et al. Percutaneous closure of post-myocardial infarction ventricular septal defects: a single centre experience. Heart Lung Circ. 2008;17:119-123. 54. Thiele H, Kaulfersch C, Daehnert I, et al. Immediate primary transcatheter closure of postinfarction ventricular septal defects. Eur Heart J. 2009;30:81-88. 55. Amin Z, Gu X, Berry JM, et al. New device for closure of muscular ventricular septal defects in a canine model. Circulation. 1999;100:320-328. 56. Thanopoulos BD, Rigby ML. Outcome of transcatheter closure of muscular ventricular septal defects with the Amplatzer ventricular septal defect occluder. Heart. 2005;91:513-516. 57. Hijazi ZM, Hakim F, Al-Fadley F, et al. Transcatheter closure of single muscular ventricular septal defects using the Amplatzer muscular VSD occluder: initial results and technical considerations. Catheter Cardiovasc Interv. 2000;49:167-172. 58. Arora R, Trehan V, Thakur AK, et al. Transcatheter closure of congenital muscular ventricular septal defect. J Interv Cardiol. 2004;17:109-115. 59. Carminati M, Butera G, Chessa M, et al. Transcatheter closure of congenital ventricular septal defects: results of the European Registry. Eur Heart J. 2007;28:2361-2368. 60. Carminati M, Butera G, Chessa M, et al. Transcatheter closure of congenital ventricular septal defect with Amplatzer septal occluders. Am J Cardiol. 2005;96:52L-58L. 61. Perez-David E, Garcia Fernandez MA, Garcia E, et al. Successful transcatheter closure of a postmyocardial infarction ventricular septal rupture in a patient rejected for cardiac surgery: usefulness of transesophageal echocardiography. J Am Soc Echocardiogr. 2007;20:1417.e9-12. 62. Eshtehardi P, Garachemani A, Meier B. Percutaneous closure of a postinfarction ventricular septal defect and an iatrogenic left ventricular free-wall perforation using two Amplatzer muscular VSD occluders. Catheter Cardiovasc Interv. 2009;74:243-246. 63. Webb I, De Giovanni J, Hildick-Smith D. Multiple percutaneous VSD closures post-myocardial infarct. Eur Heart J. 2006;27:552. 64. Kaulfersch C, Daehnert I, Schuler G, et al. Transcatheter closure of postinfarction ventricular septal defects. Minerva Cardioangiol. 2007;55:693-701. 65. Costache VS, Chavanon O, Bouvaist H, et al. Early Amplatzer occluder closure of a postinfarct ventricular septal defect as a bridge to surgical procedure. Interact Cardiovasc Thorac Surg. 2007;6:503-504. 66. Hachida M, Nakano H, Hirai M, et al. Percutaneous transaortic closure of postinfarctional ventricular septal rupture. Ann Thorac Surg. 1991;51:655-657. 67. Majunke N, Sievert H. ASD/PFO devices: what is in the pipeline? J Interv Cardiol. 2007;20:517-523. NOVEMBER 2009 I CARDIAC INTERVENTIONS TODAY I 49