* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Heart Failure
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac surgery wikipedia , lookup
Electrocardiography wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Heart failure wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
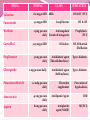
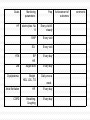
Heart Failure Done by : Taqwa shaban Amal razmak Aya hamad Amal al-jarrah Heart failure: HF is a complex clinical syndrome that results from any structural or functional impairment of ventricular filling or ejection of blood. Systolic HF (( systolic dysfunction)) : * Impaired ejection * Decreased contractility Signs and symptoms : - Low EF (<45%) - Cardiomegaly - S3 - Normal wall thickness - Hypokinesis - Symptoms primarily those of reduced cardiac output Chief Complaint “I’ve been more short of breath lately. I can’t seem to walk as far as I used to, and either my feet are growing or my shoes are shrinking!” History Of Present Illness (HPI) Rosemary Quincy is a 68 yo African-American female who presents to her family medicine physician for evaluation of her shortness of breath and increased swelling in her lower extremities. She reports that her shortness of breath has been gradually increasing over the past 4 days. She has noticed that her shortness of breath is particularly worse when she is lying in bed at night, and she has to prop her head up with three pillows in order to sleep. She also reports exertional dyspnea that is usual for her, but especially worse over the past couple of days. Past Medical History (PMH) -Hypertension × 20 years -CHD with history of MI in 2005 (PCI performed and bare metal stents placed in LAD and RCA) -Heart failure (NYHA FC III) -Type 2 DM × 25 years -Atrial fibrillation -COPD (stage 3) Family History (FH) Father died of lung cancer at age 71, mother died of MI at age 73 Social History (SH) Reports occasional alcohol intake. States she has been trying to follow her lowcholesterol and low-sodium diet. Former smoker (35 pack-year history; quit approximately 10 years ago). Medications ( Meds) : -Valsartan 160 mg po BID -Furosemide 40 mg po BID -Warfarin 2.5 mg po once daily -Carvedilol 3.125 mg po BID -Pioglitazone 30 mg po once daily -Glimepiride 2 mg po once daily -Potassium chloride 20 mEq po once daily -Atorvastatin 40 mg po once daily -Aspirin 81 mg po once daily -Albuterol MDI, two inhalations by mouth q 4–6 hours PRN shortness of breath -Tiotropium DPI 18 mcg, one inhalation by mouth daily -fluticasone/salmeterol DPI 250 mcg/50 mcg, one inhalation by mouth BID DRUGs Valsartan DOSING CLASS 160 mg po BID ARBs INDICATION HT & HF (PCI) Furosemide 40 mg po BID Loop Diuretic HT & HF Warfarin 2.5mg po once Anticoagulant daily Vitamin K Antagonist Prophylaxis (PCI) 3.125 mg po BID B-blocker HF, MI & Atrial fibrillation Pioglitazone 30 mg po once daily Antidiabetic agent (Thiazolidinedione) Type 2 diabetes Glimepiride 2 mg po once daily Antidiabetic agent (Sulfonylurea) Type 2 diabetes 20 mEq po once daily Electrolyte supplement Prevention of hypokalemia Atorvastatin 40 mg po once daily Antilipemic Agent CHD Aspirin 81 mg po once daily Antiplatelet agent(NSAID) MI (PCI) Carvedilol Potassium chloride DRUGs DOSING CLASS INDICATION Albuterol MDI 2 inhalations q 4_6 h PRN shortness of breath B2 Agonist Bronchospasm Tiotropium DPI 18 mcg 1 inhalations daily Anticholinergic Agent (long acting) COPD Fluticasone/ Salmeterol DPI 250 mcg/50mcg 1 inhalations BID B2 Agonist (long acting) COPD Review of symptoms (ROS) - Approximate 7-kg weight gain over the past week. - worsening shortness of breath with exertion and three-pillow orthopnea. - chronic, dry (nonproductive), hacking cough, which she describes as usual without recent worsening. Physical Examination General African-American female in moderate respiratory distress Vital sign (VS ( BP 134/76 mm hg (sitting; repeat 138/80), HR 65 (irreg irreg)=> normal 60-100 respiratory rate (RR) 24 => normal (16-20) , T 37°C, O2 sat 90% RA, Ht 5′5″ = 165.2 cm , Wt 79 kg (Wt 1 week ago: 72 kg) Skin Color pale and diaphoretic; no unusual lesions noted Head, Eyes, Ears, Nose and Throat (HEENT) PERRLA; Pupils,Equal,Round,Reactive to Light ,Accommodation lips mildly cyanotic; dentures Neck (+) JVD (Jugular Venous Distention) at 30° (7 cm) => normal <4 cm ; no lymphadenopathy or thyromegaly Lungs/Thorax Crackles bilaterally, 2/3 of the way up; no expiratory wheezing Heart Irregularly irregular; (+) S3; displaced PMI Abdomin Soft, mildly tender, nondistended; (+) HJR ( hepatojugular reflux); no masses, mild hepatosplenomegaly; normal BS Genit/Rect Guaiac (−), genital examination not performed MS/Ext 3+ pitting pedal edema bilaterally; radial and pedal pulses are of poor intensity bilaterally Neuro A & O × 3 (alert & oriented to person,place,time), CNs intact. No motor deficits ECG Atrial fibrillation, LVH Chest X-Ray evidence of congestive failure with cardiomegaly, interstitial edema, and some early alveolar edema. There is a small right pleural effusion. No evidence of infiltrates; evidence of pulmonary edema suggestive of congestive heart failure; enlarged cardiac silhouette Echocardiogram LVH, reduced global left ventricular systolic function, estimated EF 20%; evidence of impaired ventricular relaxation, Stage 1 diastolic dysfunction Labs Na 131 mEq/L (135-145) Hgb 13 g/dL (13-17) Mg 1.9 mEq/L (1.5-2) K 3.5 mEq/L (3.5-5) Hct 40% (37-52) Ca 9.3 mg/dL (8.4-10.2) HbA1C 6.1% (3.9-5.3) Cl 99 mEq/L (95-105) (50 -450) 3 3 Plt 192 × 10 /mm Phos 4.3 mg/dL (2.44.1) CO2 28 mEq/L (23-30) (4-10) AST 34 IU/L (8-46) 3 3 WBC 9.1 × 10 /mm ALT 27 IU/L (7-55) BUN 32 mg/dL (5-20) SCr 2.3 mg/dL (baseline SCr 2.1 mg/dL) (0.6-1.1) Glucose 124 mg/dL (70100) BNP 776 pg/mL (BNP drawn 2 months prior: 474 pg/mL) (<100) INR 2.3 (2-4) Labs Test Result Na 131 135-145 BUN 32 5-20 SCr 2.3 0.6-1.1 glucose 124 70-100 BNP 776 <100 Phos 4.3 2.4-4.1 HbA1c 6.1% 3.9-5.3 CCl = 24.2 Normal range Assessment Admit to hospital for acute exacerbation of heart failure. Clinical Pearl The presence of pitting edema is associated with a substantial increase in body weight; it typically takes a weight gain of 10 lb to result in the development of pitting edema. Questions 1.a. Create a list of this patient’s drug-related problems ? Drug-Drug Interactions Related issue Salmeterol with carvedilol B2 agonist with mixed B antagonist worsen dyspnea Warfarin with Aspirin May lead to bleeding Pioglitazone Exacerbate heart failure 1.b. What signs, symptoms, and other information indicate the presence and type of heart failure in this patient ? signs Shortness of breath over the past 4 days . Increased swelling in the lower extremities. Exertional dyspnea. symptoms HR 65 (irreg.irreg) Displaced PMI S3 sound present Cardiomegaly 3+ pitting pedal edema Interstitial edema Early alveolar edema Small right pleural effusion Skin color pale & diaphoretic. 1.c. What is the classification and staging of chronic heart failure for this patient stage 4 according to ( NYHA Functional Classification). She has acute exacerbation of heart failure with left systolic dysfunction. 1.d. Could any of this patient’s problems have been caused by drug therapy? Pioglitazone is a 1ST generation sulfonurea which exacerbate heart failure and cause pedal edema with weight gain. And intake of carvedilol with B2 agonist worsening of COPD by antagonism. There is also a glimepiride which increase CV mortality. 2.a. What are the goals for the pharmacologic management of heart failure in this patient? • Control the disease and prolonging survival by improving quality of life . • Relief symptoms of dyspnea & orthopnea . • Decrease edema & swelling. • Fluid restriction & Minimizing disability. • Manage the acute exacerbation of her HF. 3.a. What diuretic therapy should be recommended for this patient initially for acute treatment of her heart failure exacerbation? • Use the same diuretic which is furosemide but in IV/IM: 10 to 20 mg once over 1 to 2 minutes. A repeat dose similar to the initial dose may be given within 2 hours if there is an inadequate response. Following the repeat dose, if there is still an inadequate response the last IV dose may be raised by 20 to 40 mg until there is an effective diuresis. • Single doses NOT exceeding 200 mg. 3.b. How should this patient’s pharmacotherapy be adjusted for chronic management of her heart failure? • Change B blocker to metoprolol succinate to prevent interaction with b2 agonist which is salmeterol. • Titrate furosemide oral dose to 80 mg( max 600) • Warfarin dosage should adjusted according to results of International Normalized Ratio (INR) or prothrombin time (PT). • Increase the dose of glimepiride after stopping pioglitazone . Continue on Warfarin and Aspirin. For HTN management associated with heart faliure : Continue on valsartan& furosemide For atrial fibrillation: It managed by warfarin & carvedilol that replaced with metoprolol succinate. For Dyslipidemia: Continue on atorvastatin. For COPD management : Continue on albuterol ,tiotropium, Continue on fluticasone /salmetrol For hypokalemia : Continue on pottasium chloride supplements with monitoring 3.c. What non pharmacologic therapy should be recommended for this patient with respect to her heart failure? • Dietary modifications such as low sodium & cholesterol diet. • Risk factor reduction including stopping alcohol consumption and supervised regular physical activity. • O2 therapy to be >90% if the pt has hypoxia. • bed rest during exacerbation . • Fluid restriction. 4. What drugs, doses, schedules, and duration are best suited for the management of this patient? Drug Initial Daily Dose(s) Maximum Dose(s) Duration of action Metoprolol succinate extended release 12.5 to 25 mg once 200 mg once 24 hr Furosemide 20 to 40 mg once or twice 600 mg 6 to 8 h valsartan 40 mg twice daily 80 to 160 mg once daily 5. What clinical and laboratory parameters are needed to evaluate the therapy for achievement of the desired therapeutic outcome and to detect and prevent adverse events? • Initially monitor patient for rapid relief of symptoms related to the chief complaint of orthopnea, dyspnea , oxygenation & fatique. • Monitor for adequate perfusion of vital signs: • asses mental status , Cr Cl , stable HR btw 50-100 HR/min,BP. • Monitor kidney& liver function. • monitor blood glucose • Fluid intake – body weight (daily)- • Metoprolol succinate: • BP, HR baseline and after Carvedilol 3.125 mg twice 25 mg twice each dose titration, ECG • Furosemide : • monitor electrolyte ,hyperuricemia , nephrotoxicity & autotoxicity. • Valsartan : • Monitor potassium and serum creatinine 6. What information should be provided to the patient about the medications used to treat her heart failure? • Furosemide taking on empty stomach • Grapefruit juice can increase the blood levels of Atorvastatin. This can increase the risk of side effects such as liver damage • Take Metoprolol at the same time each day, preferably with or immediately following meals • Avoid taking potassium rich food. • Glimepiride should be administered with breakfast or the first main meal. Pharmacist Care Plan (PCP) Date Medical problem Tx issues Pharmacotherapy goals Recommendations 8/10 HF Acute exacerbation of systolic HF inadequately drug therapy Manage symptoms, Increase survival and QOL. Start on metoprolol succenate initial 12.5 mg BID Take Furosemide iv 40 mg with gradual increment, when stable back to po 80 mg BID continue on valsartan 160 mg po BID continue on warfarin 2.5 mg po once daily continue on aspirin 81 mg po once daily 8/10 HTN Bp above goal Bp<120/80 Increase Furosemide oral dose to 80 mg Continue on valsartan And metoprolol succenate as described above 8/10 DM Blood glucose above goal Decrease glucose to 100mg/ dl Stop pioglitazone and increase glimpiridine to 8 mg. 8/10 Dyslipidemia Increased lipids Decrease LDL and increase HDL Continue on Atorvastatin 40 mg po once daily 8/10 COPD management stable Decrease chronic cough and hacking cough (enhancing breathing) Continue on Albuterol MD2 inhalation q 4-6 hours continue on tiotropium DPI 18 mcg, continue on fluticasone/salmetrol DPI 250 mcg/ 50mcg, h inhalation BID. 8/10 Atrial fibrillation stable Continue to be managed Manage by warfarin 2.5 mg and carvedilol 3.125 mg( replaced with metoprolol succinate). Physician action Goals Monitoring parameters Freq HF electrolytes: Na K Every visit till steady BNP Every visit SCr Every visit HTN BP HR Every day DM Sugar level Every day Dyslipidemia Weight HDL, LDL, TG Daily once a Atrial fibrillation HR Every day COPD Breathing, Coughing Every day week Achievement of outcomes comments Goals Monitoring parameters Freq Valsartan Monitor pottasium and SCr Every visit Furosemide Monitor electrolytes ( Na/K, hyperuricemia, nephrotoxicity and autotoxicity) Every visit Metoprolol succinate BP, HR baseline and ECG Daily once a month Achievement of outcomes comments THE END