* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 5 dent inflammation and mucosal immunity
Survey
Document related concepts
DNA vaccination wikipedia , lookup
Rheumatic fever wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Inflammation wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Transcript
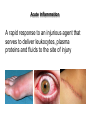
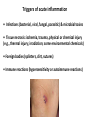
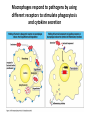
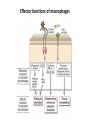
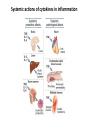
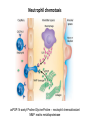
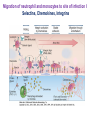
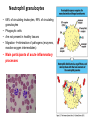
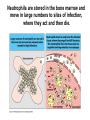
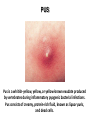
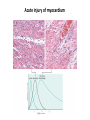
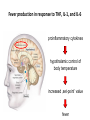
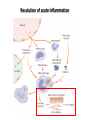
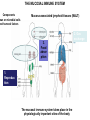
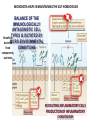
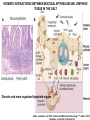
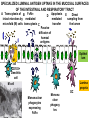
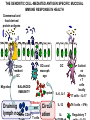
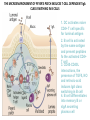
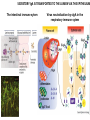
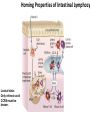
THE ACUTE INFLAMMATION AND ACUTE-PHASE RESPONSE Innate immune mechanisms establish a state of inflammation at sites of infection Acute inflammation A rapid response to an injurious agent that serves to deliver leukocytes, plasma proteins and fluids to the site of injury Triggers of acute inflammation • Infections (bacterial, viral, fungal, parasitic) & microbial toxins • Tissue necrosis: ischemia, trauma, physical or chemical injury (e.g., thermal injury; irradiation; some environmental chemicals) • Foreign bodies (splinters, dirt, sutures) • Immune reactions (hypersensitivity or autoimmune reactions) Major components of inflammation – Vascular changes • Vasodilation • Vascular permeability • Increased adhesion of white blood cells – Cellular events • Recruitment and activation of neutrophils (polymorphonuclear leukocytes) and monocytes Classical signs of acute inflammation • • • • • Redness (rubor) Swelling (tumor) Heat (calor) Pain (dolor) Loss of function (functio laesa) Macrophages respond to pathogens by using different receptors to stimulate phagocytosis and cytokine secretion Effector functions of macrophages Macrophages respond to infection by secreting inflammatory cytokines Systemic actions of cytokines in inflammation Neutrophils are directed to sites of infection through interactions between adhesion molecules Neutrophil chemotaxis acPGP: N-acetyl Proline-Glycine-Proline – neutrophil chemoattractant MMP: matrix metalloproteinase Migration of neutrophil and monocytes to site of infection I Selectins, Chemokines, Integrins Neutrophil granulocytes • 68% of circulating leukocytes, 99% of circulating granulocytes • Phagocytic cells • Are not present in healthy tissues • Migration elimination of pathogens (enzymes, reactive oxygen intermediates) • Main participants of acute inflammatory processes Neutrophils are stored in the bone marrow and move in large numbers to sites of infection, where they act and then die. PUS Pus is a whitish-yellow, yellow, or yellow-brown exudate produced by vertebrates during inflammatory pyogenic bacterial infections. Pus consists of creamy, protein-rich fluid, known as liquor puris, and dead cells. Acute injury of myocardium Fever production in response to TNF, IL-1, and IL-6 proinflammatory cytokines hypothalamic control of body temperature increased ‚set-point’ value fever ACUTE-PHASE REACTION IL-6 Liver Chemical mediators Vasodilation – Prostaglandins (PG), nitric oxide (NO) Increased vascular permeability – vasoactive amines (histamine, serotonin), C3a and C5a (complement system), bradykinin, leukotrienes (LT), PAF Chemotactic leukocyte activation – C3a, C5a, LTB4, chemokines (e.g. IL-8) Fever • IL-1, IL-6, TNFα, PGE2 Pain • Prostaglandins, bradykinin Tissue damage • Neutrophil and Macrophage products – lysosomal enzymes – Reactive oxygen species (ROS) – NO NSAIDs and Paracetamol: inhibiting COX-1 and COX-2 preventing the synthesis of prostaglandins Resolution of acute inflammation Septic shock Triggering factors : • systemic infection (bacteraemia) • microbial cell wall products and/or toxins released from the pathogens into blood circulation. Result: Systemic activation of neutrophils and macrophages High level of cytokine (TNF-alpha) production: „cytokine storm” Excessive inflammatory response Septic shock The key molecule of the process: TNF-alpha TNF-alpha and other inflammatory cytokines capillar permeability blood pressure high fever multiorgan failure DIC disseminated intravascular coagulation Therapy: anti-TNF-alpha antibody DIC Disseminated Intravascular Coagulation • pathologic activation of thrombotic process • distress of thrombotic process, bleeding Features of chronic inflammation • Prolonged host response to persistent stimulus • Caused by microbes that resist elimination, immune responses against self and environmental antigens, and some toxic substances (e.g., silica) • Characterized by persistent inflammation, tissue injury, attempted repair by scarring • Cellular infiltrate consisting of activated macrophages, lymphocytes, and plasma cells, often with prominent fibrosis • Mediated by cytokines produced by macrophages and lymphocytes (notably T lymphocytes), with a tendency to an amplified and prolonged inflammatory response owing to bidirectional interactions between these cells MUCOSAL IMMUNOLOGY THE VAST MAJORITY OF INFECTOUS AGENTS INVADE HUMAN BODY VIA MUCOSAL ROUTES Mucosal infections are one of the biggest health problems worldwide S. pneumonia, H. influenzae, influenza, RSV Cholera vibrio, rotaviruses B. pertussis The global murden of disease, WHO THE MUCOSAL IMMUNE SYSTEM Components man or microbial cells and humoral factors Mucosa-associated lymphoid tissues (MALT) 2. Gas exchange 3. Food absor ption 1. Reproduc tion The mucosal immune system takes place in the physiologically important sites of the body MICROBIOTA HELPS IN MAINTAINING THE GUT HOMEOSTASIS BALANCE OF THE IMMUNOLOGICALLY ANTAGONISTIC CELL TYPES IS DICTATED BY Beneficial MICRO-ENVIRONMENTAL bacteria Food CONDITIONS components, nutrients RECRUITING INFLAMMATORY CELLS PRODUCTION OF INFLAMMATORY CHAMOKINES INTIMATE INTERACTIONS BETWEEN MUCOSAL EPITHELIUM AND LYMPHOID TISSUE IN THE GALT A B Discrete and more organized lymphoid organs Abbas, Lichtman, and Pillai. Cellular and Mucosal Immunology, 7th edition. 2012 SPECIALIZED LUMINAL ANTIGEN UPTAKE IN THE MUCOSAL SURFACES OF THE INTESTINAL AND RESPIRATORY TRACT A Transcytosis of B FcRnintact microbes by mediated microfold (M) cells transcytosis C Apoptosis mediated transfer D E Direct sampling from the lumen Passive diffusion of humoal antigens Epithel ium Mcell CD103+ Dendritic cell M cell Lamina propria Mononuclear phagocytes expressing FcRn Mononu clear phagocy tes DC THE DENDRITIC CELL-MEDIATED ANTIGEN SPECIFIC MUCOSAL IMMUNE RESPONSE IN HEALTH Commensal and food derived protein antigens Msejt CD103+ resident DC Migration DCs and macroph age BALANCED IMMUNITY Effector Draining and lymph node Naive CD4+regulatory T cells DC Tropism! IL-6, IL-1 Circul ation Activat es effecto rT cells locally Th17 cells – IL-17 IL-12 Th1 cells – IFNγ IL- Regulatory T THE MICROENVIRONEMNT OF PEYER’S PATCH INDUCES T-CELL DEPENDENT IgA CLASS SWITHING IN B CELLS 1. DC activates naive CD4+ T cell specific for luminal antigen 1. 2. B cell is activated by the same antigen and present peptides fo the activated CD4+ T cell 3. CD40-CD40L interactions, the presence of TGFß, NO and retinoic-acid induces IgA class switching in B cell 4. B cell differentiates into memory B or sIgA secreting plasma cell SECRETORY IgA IS TRANSPORTED TO THE LUMEN VIA THE EPITHELIUM The intestinal immune sytem Virus neutralization by sIgA in the respiratory immune sytem Homing Properties of Intestinal Lymphocy Lexical data : Only retinoic-acid CCR9 must be known. Appendix- Non obligatory Immune priming and tolerance are different outcomes of intestinal exposure to antigen Oral/mucosal tolerance, as a form of peripheral tolerance BIDIRECTIONAL COMMUNICATION BETWEEN DIET, MICROBIOTA AND THE Interdependence of Diet, IMMUNE SYSTEM Immune, and Microbiota Interactions