* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download LACZIK_Pharmacology - 3.practice
Social immunity wikipedia , lookup
Periodontal disease wikipedia , lookup
DNA vaccination wikipedia , lookup
Infection control wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Acute pancreatitis wikipedia , lookup
Neonatal infection wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Adaptive immune system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Molecular mimicry wikipedia , lookup
Rheumatic fever wikipedia , lookup
Immune system wikipedia , lookup
Pathophysiology of multiple sclerosis wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
Complement system wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
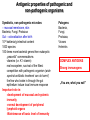
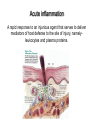
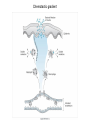
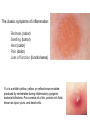
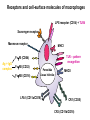
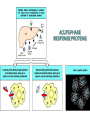
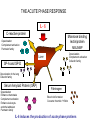
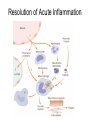
INTERACTION BETWEEN MICROORGANISMS AND THE IMMUNE SYSTEM INFLAMMATION Antigenic properties of pathogenic and non-pathogenic organisms Symbiotic, non-pathogenic microbes – mucosal membrane, skin Bacteria, Fungi, Protozoa Gut – colonalization after birth 1012 bakteria/g intestinal content 1000 species 100-times more bacterial genes then eukaryotic „peaceful” commensalisms vitamins (i.e. K1 vitamin) real ecosystem, survival of the fittest competition with pathogenic organism (wide spectral antibiotic treatment can do harm!) the few who brake in through the gut epithelium induce local immune response Important role in: -development of mucosal and systemic immunity -normal development of peripheral lymphoid organs -Maintenance of basic level of immunity Patogens Bacteria, Fungi, Protozoa, Viruses Helmints COMPLEX ANTIGENS Strong immunogens „You are, what you eat!” Gut normal flora play an important role in: - Development of mucosal and systemic immunity - Normal development of peripheral lymphoid organs - Maintenance of basic level of immunity THE GOOD, THE BAD & THE UGLY Some facts about gut flora: • • • • More than 500 microbial species live in a healthy adult gut, adding two pounds to its weight There are 1012 bacteria/g in the gut There are 100-times more bacterial genes than eukaryotic genes They produce a significant portion of vitamin K1 The challenge is to get an immune response that: 1. Eliminates pathogens 2. Limits commensal location and growth 3. Does not respond to harmless antigens in the food 4. Does not over-respond to harmful antigens in the food Immunesurveillance saves lives Under optimal conditions bacteria divide every 15-20 minutes. Physical conditions in the human body are amenable for bacterial growth MUCOSAL SURFACES AND THE SKIN ARE THE MOST COMMON ENTRY SITES FOR PATHOGENS Leading causes of death worldwide. About 15 million (>25%) of 57 million annual deaths worldwide are the direct result of infectious disease. Figures published by the World Health Organization (see http://www.who.int/whr/en and ref.7). Vaccine components Attenuated pathogen Killed pathogen Microbial extract / product Bacterial Diseases Typhoid fever (PO) BCG (M. bovis) Typhoid fever Cholera B. pertussis (DPT) Plague (Y. pestis) Anthrax B. pertussis (DTPa) Diphtheria (Tox.) Tetanus (Tox.) *Meningococcal *Pneumococcal *H. influenzae b Viral Diseases Measles Mumps Rubella Polio (Sabin - PO) Yellow fever Polio (Salk) Hep. A Influenza Rabies Japanese encephalitis Hepatitis B (HbSAg) ACUTE INFLAMMATION AND ACUTE-PHASE RESPONSE Acute inflammation A rapid response to an injurious agent that serves to deliver mediators of host defense to the site of injury, namelyleukocytes and plasma proteins. Triggers of acute inflammation: Infections (Bacterial, Viral, Parasitic and Microbial toxins) Trauma (Blunt or penetrating) Physical and Chemical agents (Thermal injury, irradiation, environmental chemicals) Tissue Necrosis Foreign bodies (Splinters, Dirt, Sutures) Immune reaction (Hypersensitivity or autoimmune reaction) MAJOR COMPONENTS OF INFLAMMATION (1) Increased vascular diameter Increased flood flow. (2) Structural changes in the microvasculature increased permeability. That permits plasma proteins and leukocytes to leave the circulation and enter the tissue. (3) Migration of the leukocytes from the micro-circulation, their accumulation in the focus of injury and their activation to eliminate the offending agent. Chemotactic gradient The classic symptoms of inflammation: Redness (rubor) Swelling (tumor) Heat (calor) Pain (dolor) Loss of function (functio laesa) Pus is a whitish-yellow, yellow, or yellow-brown exudate produced by vertebrates during inflammatory pyogenic bacterial infections. Pus consists of a thin, protein-rich fluid, known as liquor puris, and dead cells. MIGRATION OF NEUTROPHILS BLOOD TO INFLAMMED TISSUE Neutrophil granulocytes are the main cell types involved in inflammatory processes. Endothelial Adhesion Molecules during Inflammation Neutrophil Transendothelial Migration (Diapedesis) Migration of Neutrophils Extravasation Order of innate cells appearance in the inflamed site Initiation of inflammation Pathogens activate macrophages to release cytokines and are then phagocytized and digested in phagolysosomes Later… The binding of bacteria to these innate receptors causes activation of the phagocyte. This results in the synthesis and release of cytokines and the induction of lipid mediators of inflammation. Receptors and cell-surface molecules of macrophages LPS receptor (CD14) + TLR4 Scavenger receptor Mannose receptor MHCI TLR – pattern recognition FcRI (CD64) Ag + IgG complex FcRII (CD32) FcRIII (CD16) Peroxidáz Savas hidroláz LFA1 (CD11a/CD18) MHCII CR1 (CD35) CR3 (CD11b/CD18) CHEMICAL MEDIATORS • Vasodilation – Prostaglandins, Nitric Oxide • Increased Vascular Permeability – Vasoactive amines (histamine, serotonin), C3a and C5a, Bradykinin, Leukotrienes, PAF, • Chemotaxic Leukocyte Activation – C5a, LTB4, Chemokines CHEMICAL MEDIATORS OF INFLAMMATION The Basics • Fever – IL-1, IL-6, TNF, Prostaglandins • Pain – Prostaglandins, Bradykinin • Tissue Damage – Neutrophil and Macrophage products – Lysosomal enzymes – Oxygen metabolites – NO Consequences of macrophage activation Synthesis of cytokines ACUTE-PHASE RESPONSE PROTEINS During an APR their concentration increases up to x1000 THE ACUTE PHASE RESPONSE IL- 6 C-reactive protein Mannose binding lectin/protein Opsonization Complement activation Pentraxin family MBL/MBP Opsonization Complement activation Collectin family Liver SP-A and SP-D Opsonization in the lung Collectin family Serum Amyloid Protein (SAP) Opsonization Enhance chemotaxis Complement activation Enhance leukocyteendothel adhesion Pentraxin family Fibrinogen Blood clot formation Converts thrombin fibrin IL-6 induces the production of acute phase protiens Resolution of Acute Inflammation Septic shock Triggering factors: Systemic infection Microbial cell wall products and/or Toxins released from the site of infection Host factors: Neutrophils and macrophages mobilize to the site of infection „cytokine storm” release huge amounts of cytokines (TNF) Imbalance in the maintain of homeostatic cytokine production, coagulation, and vascular integrity The result……… shock, disseminated intravascular coagulation (DIC), multiple organ failure (MOF), and mortality Toxic Shock Syndrome caused by SAg Polyclonal extensive activation of T cells Over-production of INF-γ Activates Macrophages Over-production of IL-1, IL-6 and TNF-α Cytokine ‘storm’ The key molecule is TNF-α Capillary permeability Blood pressure Therapy includes: Fluids, organ support Anti-TNF-α antibody (in the very beginning) Antibiotics Corticosteroids NE FFP in DIC Fever, Rash Multi-organ failure Disseminated intravascular Coagulation (DIC) Coma, Death Similar findings found in Septic Shock caused by bacteremia/viremia NSAIDs (salicylates) ASA Mesalazine / Mesalamine Other NSAIDs Flurbiprofen Ibuprofen Naproxen Diclofenac