* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Ch 11- Cardiovascular System
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac surgery wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Ch 11- Cardiovascular System
A closed system of the heart and blood vessels
The ______________ pumps blood
__________ ___________ allow blood to circulated to all parts of the body
The function of the cardiovascular system is to deliver _______ and ____________ and remove
____________ ___________ and other __________ products
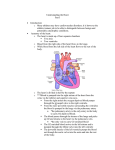
THE HEART (Fig 11.1)
Location
___________ between the lungs
Pointed apex directed toward left hip
About the size of your ________
Pericardium – a double serous membrane
_____________ pericardium – next to heart
_____________ pericardium – outside layer
_____________ fluid fills the space between the layers of pericardium
The Heart Wall
Three layers:
__________________
Outside layer – this layer is the parietal pericardium
__________________
Middle layer - mostly cardiac muscle
__________________
Inner layer - endothelium
External Heart Anatomy (Fig. 11.2a)
The Heart Chambers
Right and left sides act as separate pumps
Four Chambers:
_________ - Receiving chambers
Right Atrium
Left Atrium
_____________ - Discharging chambers
Right Ventricle
Left Ventricle
Congestive Heart Failure
In CHF, blood pumped to the lungs by the right ventricle does not keep pace with the blood pumped
around the system by the left ventricle
Fluid builds up in the lungs and causes difficulty breathing
___________ ____________ in lower legs
BLOOD CIRCULATION (Fig 11.3)
The Heart Valves
Allow blood to flow in only one direction
Four valves:
____________________ (AV) Valves – between atria and ventricles
Bicuspid (mitral) valve
Tricuspid valve
_________________ valves – between ventricle and artery
Pulmonary semilunar valve
Aortic semilunar valve
Valves open as blood is pumped through
Held in place by _____________ _______________ (“heart strings”)
Close to prevent backflow (type of murmur)
Operation of Heart Valves (Fig 11.4)
The Heart: Associated Great Vessels
____________- leaves left ventricle
Pulmonary arteries – leaves right ventricle
________ _________ (superior and inferior)– Enters right atrium
Pulmonary veins (four)
Enter left atrium
Coronary Circulation
Blood in the heart chambers does not nourish the myocardium
The heart has its own nourishing circulatory system
____________ arteries
____________ veins
Blood empties into the right atrium via the coronary sinus
Coronary Artery Disease (CAD)
CAD is a narrowing of coronary arteries due to plaque build up
Causes chest pain (_________), shortness of breath, and myocardial infarctions (MIs or heart attacks)
Risk factors include smoking, high cholestorol, high blood pressure, physical inactivity, obesity, and
diabetes
CABG pronounced “cabbage” (Coronary Artery Bypass Graft)
The Heart: Conduction System
Intrinsic conduction system (nodal system)
Heart muscle cells contract without nerve impulses in a regular, continuous way
Special tissue sets the pace
_______________ (SA) Node – Pacemaker
________________________ (AV) Node
Atrioventricular Bundle
Bundle branches
_______________ fibers
Heart Contractions (Fig. 11.5)
Contraction is initiated by the sinoatrial (SA) node
Sequential stimulation occurs at other autorhythmic cells
Electrocardiogram (ECG)
Each small box = 0.04 s, each large box = 0.20s; count # of boxes between R waves to determine HR
P wave = atrial depolarization
PR interval = pause before ventricular contraction (usually 0.12 to 0.2 s)
QRS Complex = ventricular depolarization (normally 0.04 to 0.10 s)
T wave = ventricles repolarization (refilling)
Heart Rythyms
Normal sinus rhythm
Sinus bradycardia (SR <_____bpm)
Sinus tachycardia (SR >______bpm)
Atrial fibrillation
Ventricular tachycardia
Ventricular fibrillation
Asystole – “flat line”, no electrical activity in heart
Cardiac Cycle (Fig. 11.6)
Atria contract simultaneously
Atria relax, then ventricles contract
____________ = contraction
____________ = relaxation
Cardiac Cycle – events of one complete heartbeat
Mid to late diastole – blood flows into ventricles
Ventricular systole – blood pressure builds before ventricle contracts, pushing out blood
Early diastole – atria finish re-filling, ventricular pressure is low
Cardiac Output (CO)
Amount of blood pumped by each side of the heart in one minute
CO = (heart rate{HR}) X (stroke volume {SV})
___________ _____________ = volume of blood pumped by each ventricle in one contraction
Cardiac Output Regulation (Fig. 11.7)
Regulation of Heart Rate
Stroke volume usually remains relatively constant
Starling’s law of the heart – the more that the cardiac muscle is stretched, the stronger the contraction
Changing the heart rate is the most common way to change cardiac output
Increased Heart Rate
_______________ Nervous System – Crisis or Low blood pressure
Hormones – Epinephrine and Thyroxine
Exercise
Decreased blood volume
Decreased Heart Rate
_____________________ Nervous System
High Blood Pressure
Decreased venous return
BLOOD VESSELS: THE VASCULAR SYSTEM (Fig. 11.8b)
Taking blood to the tissues
________________
________________
________________
________________
________________
Blood Vessels: Anatomy
Three layers (tunics)
Tunic __________ – endothelium
Tunic __________ – smooth muscle, controlled by sympathetic nervous system
Tunic __________ – mostly fibrous connective tissue
Differences between Blood Vessel Types
Walls of _____________ are the thickest
Lumens of ___________ are larger
Skeletal muscle “milks” blood in veins toward the heart
Walls of capillaries are only one cell layer thick to allow for exchanges between blood and tissue
Movement of Blood Through Vessels
Most arterial blood is pumped by the heart
Veins us the milking action of muscle to help move blood
Capillary Beds
Capillary beds consist of two types of vessels
Vascular shunt – directly connects an arteriole to a venule
True capillaries – exchange vessels
Oxygen and nutrients cross to cells
Carbon dioxide and metabolic waste products cross into blood
Capillary Exchange
Substances exchanged due to concentration gradients
Oxygen and nutrients leave the blood
Carbon dioxide and other wastes leave the cells
Capillary Exchange: Mechanisms
Direct diffusion across plasma membranes
Endocytosis or exocytosis
Some capillaries have gaps (intercellular clefts)
Plasma membrane not joined by tight junctions
_________________ (pores) of some capillaries
Diffusion at Capillary Beds (Fig. 11.20)
Major Arteries (Fig. 11.11)
Major Veins (Fig. 11.12)
Arterial Blood Supply to Brain (Fig. 11.13)
Hepatic Portal Circulation (Fig. 11.14)
Fetal Blood Circulation (Fig. 11.15)
Fetal Heart
Fetuses have _______ in their hearts which allow circulation to be routed around the non-inflated lungs
PDA (patent ductus arteriosis) results if these “holes” don’t close shortly after birth
Pulse – pressure wave of blood in vessels
Monitored at “pressure points” where pulse is easily palpated
(Fig. 11.16) Temporal artery, Facial artery, Carotid artery, Brachial artery, Radial artery, Femoral
artery, Popliteal artery, Posterior tibial artery, Dorsal pedis artery
Blood Pressure (Fig. 11.18)
Measurements by health professionals are made on the pressure in the arteries
____________ – pressure at the peak of ventricular contraction
____________ – pressure when ventricles relax
Pressure in blood vessels decreases as the distance away from the heart increases
Effects of Factors on Blood Pressure (Fig. 11.19)
Neural factors
Autonomic nervous system adjustments (sympathetic division)
Renal factors
Regulation by altering blood volume
__________ – hormonal control
Temperature
Heat has a vasodilating effect
Cold has a vasoconstricting effect
Chemicals
Various substances can cause increases or decreases
____________
Variations in Blood Pressure
Human normal range is variable
Normal
______________ mm Hg systolic
______________ mm Hg diastolic
Hypotension
Low systolic (below 110 mm Hg)
Often associated with illness
Hypertension
High systolic (above 140 mm Hg)
Can be dangerous if it is chronic
Major risk factor in stroke, CAD, CHF, and kidney failure
Developmental Aspects of the Cardiovascular System
A simple “tube heart” develops in the embryo and pumps by the fourth week
The heart becomes a four-chambered organ by the end of seven weeks