* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Movement Disorders
Survey
Document related concepts
Transcript
MOVEMENT
DISORDERS
Dayna Ryan, PT, DPT
Winter 2012
Summary
• Typically involve dysfunction to the basal ganglia and
cerebellum
• Both influences movement via the thalamus to motor
areas of the cerebral cortex
• UMNL or LMNL?
• It’s a Upper Lesion (chapter 10 Lundy-E)
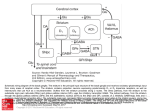
Basal Ganglia
The Role of the BG in Movement
Motor
Thalamus
Motor
Cortex
Corticospinal
tracts
LMNs
Voluntary
muscles
BG
Postural and
girdle
muscles
LMNs
Pedunculopontine
nucleus
Reticulospinal &
vestibulospinal
tracts
Basal Ganglia Circuitry
• DIRECT PATHWAY
• Striatum -> internal globus pallidus & substantia nigra parts retiulata
• These then project to the thalamus VA / VL
• Movement results when thalamic cells are released from tonic inhibition
• INCREASES excitatory thalamic drive to SMA
• TURNS UP motor activity
Normal Basal Ganglia Circuitry
• DIRECT PATHWAY
• Straitum -> internal
•
•
•
•
globus pallidus and
substantia nigra parts
retiulata
These then project to the
thalamus (inhibitory
signal)
Movement results when
thalamic cells released
from tonic inhibition
INCREASES excitatory
thalamic drive to SMA
TURNS UP motor activity
Normal Basal Ganglia Circuitry
• INDIRECT PATHWAY
• Striatum -> external
globus pallidus ->
subthalamic nucleus
• DECREASES excitatory
thalamic drive to SMA
• TURNS DOWN motor
activity
• Direct pathway TURNS UP motor activity
• Indirect pathway TURNS DOWN motor
activity
• Direct and indirect pathways counterbalance
each other to maintain normal movement
function.
• Basal Ganglia controls the motor
commands
Dopaminergic Modulation
Cholinergic (ACh) Modulation
• Excitatory effect on D1
receptors in direct pathway
• Inhibitory effect on D2
receptors in indirect pathway
• TURNS UP motor activity
• Cholinergic (ACh) interneuron:
Inhibits the direct pathway
and Excites the indirect
pathway
• TURNS DOWN motor activity
Parkinson’s Disease
• Parkinsonism: a group of rare diseases or
syndromes, with signs and symptoms similar to
Parkinson’s disease (PD)
• PD: the most common form of parkinsonism;
a.k.a. primary parkinsonism or idiopathic PD
• At least 500,000 people currently have
Parkinson's disease, ~ 50,000 new cases
annually
• Average age of onset = 60 years; Incidence
increases incrementally after age 50
• ~ 5-10 % diagnosed before age 50 ("early-onset“)
Parkinson’s Disease: Pathology
• Severe loss of substantia nigra (SN) dopaminergic neurons
• Most PD patients have lost 60-80% or more of the dopamine-
producing cells in the substantia nigra by the time symptoms
appear
Parkinson’s Disease: Histology
• Histology hallmark in PD is
Lewy bodies (abnormal
aggregates, clumps composed
principally of the protein alphasynuclein)
• Lewy bodies form primarily in
the substantia nigra and
brainstem, but can also be
elsewhere in the brain
• Researchers do not yet know
why Lewy bodies form or what
role they play in development
of the disease. They may
interfere with transmission of
nerve signals.
Abnormal Basal Ganglia Circuitry in PD
• Since dopamine cells are lost in PD…
• Direct pathway activity ↓ = LESS MOTOR ACTIVITY
• Indirect pathway activity ↑ = LESS MOTOR ACTIVITY
Causes of PD
• Genetic
• Environmental
• Toxins, e.g. MPTP (in heroin), DDT (in pesticides)
• Viruses, e.g. 1918 influenza, herpes virus infection
• Interaction of Genetic & Environmental Factors
• Even in familial cases, exposure to toxins or other
environmental factors may influence when symptoms of
the disease appear or how the disease progresses
• Mitochondrial Dysfunction
• Oxidative Stress
• Cerebral Inflammation
Parkinson’s Disease Symptoms
• Cardinal Symptoms:
• Resting Tremor
• “pill rolling”, back-and- forth motion
• Rate: 4-6 Hz
• Bradykinesia
• Slowing down; less consistent and slow force production
• Loss of spontaneous and automatic movements
• Rigidity
• Cogwheel
• Lead-pipe (when rigidity becomes severe)
• Postural Instability
• More likely to use hip instead of ankle strategies, due to
inappropriate scaling of sensory feedback
• Hypometric anticipatory postural adjustments
Parkinson’s Disease: Bradykinesia
• Slower and less consistent force production
Stelmach, GE 1989
Parkinson’s Disease Symptoms
• Other symptoms:
• Difficulty with swallowing and chewing
• Speech impairments: Speak too softly, monotone,
hesitant, slurred, repeating words
• “Masked” face/Expression-less
• Depressed, irritable, other emotional changes
• Fatigued-more muscle activity
• Sleep problems-when resting they shake
• Urinary problems or constipation
• Skin problems: very oily, very dry, excessive sweating
• Decreased strength in muscles of respiration
• Dementia or other cognitive problems
• Orthostatic hypotension
Parkinson’s Disease: Postural Changes
• Kyphotic posture with
forward-flexed trunk
• Forward head
• Crouched legs
• Mask-like face
(expression-less)
Parkinson’s Disease: Gait
• Difficulty INITIATING gait
• Freezing gait
• Patient will report that it feels like their feet are stuck on the
ground/heavy and they cannot move
• Festinating gait
• Steps too small
• Causes COM to get in front of BOS (upper body going faster than
lower body)
• Can’t always catch themselves so typically fall forward
• Decreased foot clearance
• Decreased or no trunk rotation
• No arm swing
Parkinsons’ Disease: Abnormal Postural
Control Strategies
• Abnormal combination of ankle and hip strategies
concurrently exhibited
Parkinson’s Disease: Micrographia
• Handwriting is slow and looks cramped or small.
Parkinson’s Disease Progression
• PD is not by itself a fatal disease but it does get
worse with time
• PD generally does not affect life expectancy
• In the later stages of the disease, PD-related
complications can lead to death, such as choking,
pneumonia, and falls
• Progression of symptoms may take 20 years or
more (In some, PD progresses more quickly)
Parkinson’s Disease Progression:
Hoehn & Yahr Staging
• Stage One
• Unilateral, one side of the body
• Symptoms mild, inconvenient
but not disabling
• Usually presents with tremor of
one limb
• Friends noticing change in
posture, gait, facial expression
• Stage Two
• Bilateral, both sides of the
body
• Minimal disability
• Posture and gait affected
• Stage Three
• Significant slowing of
movement
• Early impairment of equilibrium
on gait or standing
• Generalized dysfunction that is
moderately severe
• Stage Four
• Severe symptoms
• Can still walk to a limited
extent
• Rigidity and bradykinesia
• No longer able to live alone
• Tremor may be less than
earlier stages
• Stage five
• Cachectic stage
• Invalidism complete
• Cannot stand or walk
• Requires constant nursing
care
Parkinsons Disease:
UPDRS (United Parkinson Disease Rating Scale)
• Updated version in 2008
• Sections include:
• Mentation, Behavior, and Mood
• ADL
• Motor function
• 199 points total
• Higher score indicate increasing disability
UPDRS Example Items
Parkinson’s Disease Diagnosis
• No blood or laboratory tests
• Medical history & neurological exam
• Difficult to diagnose accurately
• early signs and symptoms may be dismissed as the effects of
normal aging
• Clinical signs and symptoms
• must have 2 or more cardinal signs
• Positive response to dopamine agonist
medication
• Unified Parkinson's Disease Rating Scale
(UPDRS)
• CT or MRI in PD usually appear normal but may
be needed to rule out other diseases
Parkinson’s Disease Medications
• Levodopa (L-dopa)
—A dopamine precursor that crosses the blood-brain barrier and then
converts to dopamine
—Side effects increase with continued usage, including
—Nausea, hypertension (due to activation of peripheral dopamine
receptors)
—Dyskinesias (involuntary movements, e.g. twitching, twisting)
—“tolerance” develops with continued usage
—Period of effectiveness after each does begins to shorten
—Larger doses may be needed to be effective
—“On-Off” effects
• Sinemet (a combination of Carbidopa and
Levodopa)
—Does not cross the blood brain barrier but prevents peripheral
conversion of levodopa to dopamine and thereby reduces the
unwanted peripheral side-effects of levodopa
Parkinson’s Disease Medications
• Dopamine agonists
—Mimics the effects of dopamine in the brain
—Given alone or in conjunction with L-dopa
—Can lengthen the duration of response to L-dopa in patients that are
developing “tolerance” and “on-off” effects
—Apomorphone, bromocriptin, pramipexole, ropinirole
• Anticholinergics
• Decrease the activity of ACh (Striatum has ACh interneurons, which
oppose the effect of D1 and D2 receptors in the striatum)
• Reduce tremors and muscle rigidity
• Trihexyphenidl, benztropine
Parkinson’s Disease Medications
• MAO-B inhibitors
—Inhibit the enzyme monoamine oxidase B (MAO-B), which breaks
down dopamine in the brain
—Delay the need for L-dopa by up to a year or more
—Azilect (Rasagiline)
• COMT inhibitors
—Inhibit the enzyme Catechol-O-Methyltransferase (COMT), which
breaks down dopamine
—Decrease the duration of “off” periods; make it possible to reduce Ldopa dosage
—Entacapone, tolcapone
• Other Medications for non-PD symptoms
Parkinson’s Disease: Surgery
• Used if medications no longer effective
• Ablation
— Selectively destroying specific cells that contribute to the
symptoms
— Pallidotomy (reduce tremor, rigidity, and bradykinesia)
— Thalamotomy (reduce tremor)
•
Deep brain stimulation (DBS)
—Electrodes implanted in thalamus, subthalamic nucleus,
and globus pallidus
—Electrodes connected to a pulse
generator
—The pulse generator and electrodes
painless stimulate the brain
—Blocks electrical signals from targeted areas
—Reduces the need for medications
•
Embryonic stem cell transplant
Recent Research Findings:
Implications for Interventions
• Paradoxical Kinesia (“motion”)
• A deficit to execute movements can be
overcome in the presence of external
sensory cues (e.g. visual, auditory,
proprioception)
• Rationale: distinct contribution of the corticostriatal (implicit) and cortico-cerebellar (explicit)
systems to motor learning and control
• Provide external sensory cues to bypass the
defected cortico-striatal system
Treatment for Freezing Gait in PD
• Visual cue on floor within one
• LaserCane™ projects
step length will stimulate a step a bright red line
across your path
• Can add hand triggered laser
light to a walker
Videos for PD
• Before and after L-dopa
• http://www.youtube.com/watch?v=sf1N0Zf5IqA&feature=related
• Michael J. Fox
• http://www.youtube.com/watch?v=ECkPVTZlfP8
• What you will likely see
• http://www.youtube.com/watch?v=29zHputMEQA&feature=related
• http://www.youtube.com/watch?v=oUDDRUtJcgM&feature=related
Huntington’s Disease (HD)
• Huntington’s chorea
• Involuntary choreoform movements
• Rapid, involuntary, purposeless jerks of irregular
and variable location on the body
• Hereditary (autosomal dominant)
• 50% inheritance rate in offspring
• No treatment to stop or reverse the progression
• Striatum affected.
Huntington’s Disease (HD)
• Pathology
• Primarily involved neuronal deaths in the Striatum (=
Caudate & Putamen)
• Enlarged ventricles, degenerative cortex & cerebellum
• Abnormal Basal Ganglia Circuitry
• Reduction of neurotransmitter, GABA, ACh,
metenkephalin due to loss of neurons in the striatum
• Causes relatively higher concentration of dopamine and
norepinepherine excessive excitation of
thalamocortical pathways choreoform movements
Huntington’s Disease
• Choreiform movements due to:
• Direct pathway activity ↑ = MOTOR ACTIVITY ↑
• Indirect pathway activity ↓ = MOTOR ACTIVITY ↑
http://www.youtube.com/watch?v=kINXIjs_V3M&fe
ature=related
http://www.youtube.com/watch?v=OveGZdZ_sVs
Abnormal Basal Ganglia Circuitry in HD
Huntington’s Chorea
Primary Characteristics
• Choreic Movements
• Brief
• Purposeless
• Involuntary
• Random
• Personality and Psychiatric
Disturbances
• Irritable, apathy, depression
• Explosive behaviors
• Dementia
• Decreased intellect
• Decreased memory, attention
Other Signs and Symptoms
• Dysarthria (speaking)
• Dysphagia (swallowing)
• Cachexia (muscle wasting)
• Sleep disorders
• Urinary incontinence
• Depression
• Apraxia
• May become severe
• Ideomotor form
Huntington’s Disease:
Motor and Sensory Signs
Motor
• DTRs = normal
• Strength = normal early in
disease
• Tone
• Normal initially
• Later become rigid
• Apraxia - ideomotor
• Cannot sustain long
muscle contractions
Sensory
• Abnormal eye movement
• Impaired saccade
• Impaired smooth pursuit
• Impaired gaze fixation
• Visuospatial deficits
• E.g. may not be able to see a
figure embedded in a picture
HD Movement Patterns
• Undershoot targets
• Decreased velocity of movement
• Latency in initiation (can develop freezing gait)
• Wide-based staggering gait
• Dysdiadochokinesia (pronate/supinate)
• Macrographia
Writing samples from Jan
21 and Nov 13 of same
year
HD Disease Progression
• Onset
• Juvenile: before age 20
• Adult: after age 50
• Juvenile – more severe
course
• Suicide
• 6% of deaths
• 25% attempt suicide
• As disease progresses
• More dystonic contractions
• May develop rigidity and
bradykinesia
• Less choreoform movement
(because more rigid)
• Death
• Typically from intercurrent
infection (usually in lungs)
• 15-20 years after onset
Huntington’s Disease:
Diagnosis and Treatment
Diagnosis
Medical Treatment
• DNA testing
• Anticonvulsants
• MRI to show atrophy of
• Antipsychotic agents
striatum in later stages
• Surgery to remove globus
pallidus
• Deep brain stimulation
Dystonia
• Etiology
• Unknown, idiopathic in most cases
• Defected DYT1 gene in early onset dystonia
• Secondary to some other neurologic
disorders
• Pathogenesis
• Lesions at Caudate, Putamen and Globus
pallidus
• Overactive direct pathway within the basal
ganglia circuitry increases motor activity
Characteristics of Dystonic Movements
•
•
•
•
•
•
•
Definition = abnormal tonicity of muscle with
simultaneous contraction of agonist and antagonist
Involuntary muscle spasms force affected parts of the
body into contorted or twisted postures
Rapid or slow; Rhythmic or un-patterned
Duration varies: < 1 s, a few sec or min, hours or
longer
May be increased with stress, during purposeful
movements, task-specific (Sx only present during
specific tasks, e.g. writing, playing instruments)
Decrease after relaxation and disappear during sleep
Often painful condition
Dystonia
• Focal and generalized forms
• Focal
• Pharyngeal
• Distorted speech; affect vocal cords
• Cervical dystonia
• Most common
• Hypertrophy of SCM muscle
• Rotation of neck with lateral flexion and flex/ext of
neck; typically painful
• Is NOT torticollis (a musculoskeletal disorder with muscle
fibrosis)
• Writer’s cramp (task-specific focal dystonia)
• Spasm affecting certain muscles of the hand and/or fingers
• Musician’s cramp (task-specific focal dystonia)
• Blepharospasm = uncontrollable blinking
• Can be considered legally blind
Dystonia: Disease Progression
• Onset
• Generalized ~ 8 y. o.
• Focal 30-50 y. o.
• Progression
• Dystonia is not fatal, but is chronic and often painful
and debilitating
• Generalized begins in legs and progresses to rest of
body
• Focal dystonia progresses for about 5 years then
plateau
• Spontaneous recovery in 30% of cases
Dystonia
• Medications
• BOTOX
• Effective for 3-4
months
• For focal dystonia
• Common medications for
Generalized Dystonia
• Baclofen (treats
spasticity)
• Artane
• Sinemet (parkinson)
• Klonopin
• Surgeries
• Deep brain stimulation of the
Globus pallidus
• Rhizotomy
• Resection of anterior (motor)
cervical spinal nerve roots
• Treatment in research
phase
• RNA interference (RNAi)
therapy
• Suppress the expression of
mutated DYT1 gene to
prevent further involvement
with cell replication
Videos on Dystonia
• Generalized Dystonia
• http://www.youtube.com/watch?v=b1yc6YnvrMs&feature=related
• Focal Dystonia
• http://www.youtube.com/watch?v=D8_98t74PnQ&feature=related
• http://www.youtube.com/watch?v=UzI_4IOw3_8&feature=related
Friedreich’s Ataxia
• Lesion:
• Cerebellum
• Dorsal root ganglia
• Dorsal columns
• Spinocerebellar tracts
• Some corticospinal tract
involvement
• Etiology: Hereditary
(Autosomal recessive)
• Onset
• Between 5 to 15 y. o.
(some later)
• 25% of offspring have FA
• Course (highly variable)
• Generally lose ability to
walk and confined to WC
within 10-20 years after
onset
• Prognosis
• Some survive into their
60’s & 70’s if no heart
attack
Friedreich’s Ataxia:
Signs and Symptoms
• Ataxia
• Most common Sx
• Gait ataxia is usually the first
•
•
•
•
•
•
Sx
• Ataxia gradually worsens and
spreads to the arms and the
trunk
Clumsiness and intention tremor
Muscle weakness and wasting
Loss of sensation in extremities
+ Babinski (esp. if corticospinal
tract involved)
Decreased DTRs
Tone is normal at rest
• May get flexor spasms
• Nystagmus (20% of cases)
• Impaired smooth pursuit
• Heart disease
• various forms (e.g.
cardiomyopathy,
dysrhythmia)
• 60% of population
• Easily fatigued
• Scoliosis
• Dysarthria/tongue and oral
motor issues
Videos of FA
• http://www.youtube.com/watch?v=CBlrp-Ok38E
• FYI – very long video
• http://www.youtube.com/watch?v=pfxPJVryhRE&feature=related
Dyskinesia
= a movement disorder that consists of decreased
voluntary movements and increased involuntary
movements
• Tic
• Chorea
• Tardive Dyskinesia = involuntary movements of the
tongue, lips, face, trunk, and extremities that occur in
patients treated with long-term dopaminergic antagonist
medications
• http://www.youtube.com/watch?v=UbBpt9uCXqc&feature=related
• http://www.youtube.com/watch?v=W_3bbpFjI68
• http://www.youtube.com/watch?v=R0EbgpyztCA&feature=fvwrel
Review