* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download No Slide Title
Survey
Document related concepts
Transcript
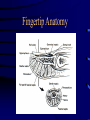
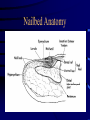
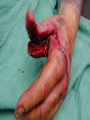
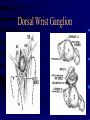
Tumors of the Hand Fingertip and Nail Injuries Injection Injuries Doug Humphreys BSc. MD Division of Plastic Surgery Dalhousie University Halifax, Nova Scotia Fingertip and Nail Injuries Fingertip Injury • • • • Most common hand injury Predisposed to injury Males > females Important for tactile, aesthetic function Types of Injury • • • • Simple Laceration Crush Avulsion Amputation Fingertip Anatomy Nailbed Anatomy Nailbed Injury • Remove nail plate to assess underlying injury – if necessary • Stabilize distal phalanx, if required • Repair nail bed • Replace sterile matrix with graft at the primary procedure • Replace nail / Stent Nailbed Injury • • • • Nailbed lacerations repaired 6-0 or 7-0 plain gut Loupe magnification Stenting of nail Nailbed Avulsion • • • • • Can replace as graft Leave small segments on nail Remove larger segments from nail Split thickness grafts Full thickness grafts Phalangeal Tuft Fractures • • • • Often associated with nailbed injury Displacement uncommon Support of nail and pulp Percutaneous K-wire occasionally Fingertip Amputation • • • • • Area Depth Location Orientation Bone exposure Fingertip Amputation Orientations Fingertip Amputation Goals • • • • • Achieve wound closure Maximize sensory return Preserve length Maintain joint function Obtain Satisfactory Appearance Conservative Treatment Advantages • • • • • Good for smaller defects ( < 1 cm2 ) Good in children Durable cover Sensation maintained No tender scars Conservative Treatment Disadvantages • • • • Requires patient compliance Longer time to wound closure Not preferred with bone exposure Hook nail deformity Skin Grafts Advantages • Quick coverage Skin Grafts Disadvantages • • • • • High rate of difficulties Instability Poor sensibility Hypersensitivity Donor site morbidity Lateral V-Y Advancement Kutler (1944) Lateral V-Y Advancement Kutler (1944) • • • • For vertical amputations Typical advancement 5mm Unreliable vascularity Places tender scars on fingertips Volar V-Y Advancement Tranquilli-Leali (1935) Volar V-Y Advancement Atasoy (1970) • • • • • For transverse midnail or dorsal oblique amputations Advances 10 mm Good vascularity, sensation Hyperesthesia, hypersensitvity, cold intolerance Hook nail deformity Volar Neurovascular Flap Moberg (1964) Volar Neurovascular Flap Moberg (1964) • • • • • • Entire palmar skin and neurovascular bundles Preserves sensation Digit must be flexed to close Joint contracture Tip necrosis Usefulness limited to thumb Cross-Finger Flaps Gurdin (1950) Cross-Finger Flaps Gurdin (1950) • Best for volar oblique amputations – Suitable for other types • • • • • • Uses uninjured digit Reliable vascularity Sensibility varies Requires multiple Procedures Requires skin grafting Flexion contractures, cold intolerance Thenar Flap Thenar Flap • • • • • • • • Alternative to cross-finger flap Uses thicker palmar skin Staged Proximally or distally based Donor site closed primarily Thenar scar can be painful Flexion contractures Used mainly in children Neurovascular Island Flap Littler (1960) Neurovascular Island Flap Littler (1960) • • • • • • Attempts to provide sensibility Used for thumb, index, ulnar fifth finger Donor site morbidity (ulnar fourth finger) Extensive surgery Results vary widely Pain, paresthesias, cold intolerance in donor and recipient digits Fingertip Replantation • Technically difficult • Questionable benefit Tumors of the Hand Tumors of the Hand • Overwhelming majority benign • Most amenable to surgical excision Tumors of the Hand Classification • Benign • Malignant Tumors of the Hand Classification • Skin • Soft Tissue • Bone • Metastatic Tumors Skin Tumors • Squamous cell carcinoma commonest • Basal cell carcinoma rare • Malignant Melanoma Malignant Skin Tumors Squamous Cell Carcinomas • Etiology – – – – – ionizing solar radiation previous irradiation burn scars exposure to arsenic compounds inherited genetic disorders Malignant Skin Tumors Squamous Cell Carcinomas • Dorsum of hand - common location • Treatment – wide excision • SCC of hand more aggressive – especially if tumor involves web space Malignant Skin Tumors Basal Cell Carcinomas • Rare on fingers • Gorlin’s Syndrome – Palmar variants • Treatment – local excision Malignant Skin Tumors Malignant Melanoma • Occur on palms or subungually • Tumor thickness prognostic indicator • Treatment – wide excision or amputation – appropriate level of amputation not determined Soft Tissue Tumors • • • • • • • Ganglions Giant Cell Tumor Of Tendon Sheath Glomus Tumor Peripheral Nerve Tumors Ulnar Artery Aneurysm Epidermal Inclusion Cysts Sarcomas Ganglions • 70 % of all hand tumors • Caused by mucoid degeneration of fibrous connective tissue in joint capsules or tendon sheaths • Women > Men (2-3X) • Presents as mass +/- pain Types of Ganglia I. Dorsal Wrist Ganglion II. Volar Wrist Ganglion III. Flexor Tendon Sheath Ganglion IV. Mucous Cysts V. Carpal Bosses Dorsal Wrist Ganglion • • • • 70% of all hand ganglia Over scapholunate ligament Possible periscaphoid ligamentous injury Can impinge on PIN Dorsal Wrist Ganglion Volar Wrist Ganglion • Most frequent site in children under 10 years • Arises from FCR tendon sheath, radioscaphoid or scaphotrapezial joints • Close proximity to radial artery – can be bilocular Volar Wrist Ganglion Flexor Tendon Sheath Ganglion • • • • Arise in vicinity of MP joint Lack of mobility with flexion Often through A1 pulley, or A1 - A2 region Pathophysiology – Pressure damage to fibrous sheath Flexor Tendon Sheath Ganglion Mucous Cysts • Arise in association with tendons and joints – dorsal aspect of fingers – from extensor tendon or joint capsule • Occur primarily in older women • Associated with osteoarthritis – arthritic joints must be debrided - decreases reoccurance Mucous Cyst Carpal Bosses • Painful masses on dorsal aspect second and third metacarpal bases • Bone lipping of the capitate, accessory ossicles often present – os styloideum • Strongly associated with osteoarthritis Carpal Bosses Ganglions Treatment • • • • • Observation Rupture Aspiration Injection Surgical Excision Giant Cell Tumor of Tendon Sheath • Pigmented Villonodular Sinovitis – considered benign • • • • Second commonest hand tumor 20 to 40 year olds slightly more common in men Lobulated mottled-yellow subcutaneous mass Giant Cell Tumor of Tendon Sheath • Polyhedral cells of a fibrous xanthoma, multinucleated giant cells, foam cells, reticulin • Can erode bone, skin by pressure • Complete local excision recommended • Recurrence common Glomus Tumor • Benign hamartomas of glomus apparatus – usually <1cm. In diameter • Pain, pinpoint tenderness, cold sensitivity – diagnostic triad • • • • Subungual Angiography, MRI, and Transillumination Excision recommended, recurrence common Remove nail and repair bed Peripheral Nerve Tumors • Rare in hand • All lesions arise from Schwann cells – Produce myelin and collagen • Difficult to diagnose and treat Peripheral Nerve Tumors • Types – – – – – Neurilemmomas Neurofibromas Neurofibromatosis (von Recklinghausen’s Disease) Neurofibrosarcomas Intraneural tumors of nonneural origin Peripheral Nerve Tumors Neurilemmoma • • • • Most common neural cell tumor Dumbbell shaped Extrinsic to nerve proper Treatment – Enucleation to preserve nerve fibres • Recurrences rare • Malignant degeneration not a feature Peripheral Nerve Tumors Neurofibromas • Can proliferate within the nerve fibres – produce functional abnormalities • Excision more difficult • Schwann cells associated with mast cells, lymphocytes, mucoid material, and xanthoma cells • Can cause gigantism of the affected part Peripheral Nerve Tumors Neurofibromatosis • Autosomal dominant • Multiple peripheral and central neurofibromas – acoustic neuromas, meningiomas, optic gliomas • Diagnosis – café au lait spots, greater than 6 • Sarcomatous degeneration reported – 10% - 15% of lesions Peripheral Nerve Tumors Neurofibrosarcomas • • • • • • Neurosarcomas or Malignant Schwannomas 2-3% of malignant hand tumors Usually associated with neurofibromatosis Local extension and metastasis are common Mortality - 90% Treatment – Wide excision or amputation Peripheral Nerve Tumors Intraneural Tumors of Nonneural Origin • Types – lipofibromatous hamartomas • seen if first decade of life • associated with median nerve • treatment - carpal tunnel release after excision of tumor – hemangiomas – ganglion cysts – lipomas Ulnar Artery Aneurysm • Hypothenar hammer syndrome – post traumatic • • • • More common in men Arteriography Aneurysm resection, ulnar artery ligation Regional thrombolysis may be considered if embolization present Ulnar Artery Aneurysm • Features – – – – Pulsatile mass Digital ischemic changes +/- distal emboli Tinel’s sign often present Epidermal Inclusion Cyst • Palmar surface • Traumatic etiology - penetrating hand injuries • Cyst wall consists of squamous epithelium with laminated keratin • Contents are protein, cholesterol, fat, fatty acids • Can become infected • Cyst wall removal recommended Sarcomas Malignant neoplasm arising in tissue of mesenchymal origin Sarcomas • Combination therapy – wide excision, radiotherapy, and chemotherapy • Amputation reserved for recurrences • Metastasis tend to occur at distant sites Ewing’s Sarcoma • • • • • 6- 10% of primary bone malignancies Rare in hand Young males Focal mass Poor prognosis – hand better - excellent local control and good function Osteosarcoma • • • • Rare in hand ( .18% of osteosarcomas) Increasing pain from rapidly growing mass Arise de novo or from other lesions Wide excision and adjuvant therapy Osteosarcoma • More frequent in – – – – – – – Irradiated bone Paget’s disease Fibrous dysplasia of bone Giant cell tumor Solitary enchondroma Multiple enchondromatosis Multiple osteochondromas Chondrosarcoma • • • • • Rare in the hand Typically in elderly Slow growing Progressively painful tumor near MP joint Treatment – Amputation / ray resection • Prognosis good Epithelioid Sarcoma • • • • Most common soft tissue sarcoma in hand Notoriously insidious Local recurrence, distant mets common Treatment – Radical excision • amputation – node dissection + /- adjuvant therapy Enchondromas • • • • • • Remain within substance of bone, cartilage Congenital cartilaginous rests Proximal, middle phalanges Well demarcated oval swellings Radiolucent diametaphyseal lesions Curettage +/- bone grafting Multiple Enchondromas • Ollier’s dyschondroplasia – disseminated involvement • Maffucci’s syndrome – multiple enchondromas associated with hemangiomas Osteochondromas • Most common cartilaginous neoplasm in body – not hand • Young patients • Radiographically – Bony protuberances from metaphyseal cortex • 1 % risk malignant transformation Chondroblastomas • • • • • • Rare Young patients Epiphysis of tubular bones Sclerotic rim on X-ray Malignant transformation unusual Treatment – curettage, +/- bone grafting Bone Cysts • Unicameral Bone Cyst – Common in children – Diaphyseal • abuts, but does not cross the epiphysis – Treatment • curettage and cancellous bone grafting Bone Cysts • Aneurysmal Bone Cyst – – – – – Second decade males = females Eccentric in metaphysis or diaphysis Expansile and lucent Treatment • resection or curettage with bone grafting Osteoid Osteoma • Benign osteoblastic tumor • Histology – Richly vascularized osteoblastic osteoid tissue • Uncommon in hand – distal phalynx most common site • Usually young males Osteoid Osteoma • Localized painful area over tubular bone • Pain worse at night, relieved by aspirin • Radiographically – Small central lucency, sclerotic surroundings • Treatment – complete excision – pack cavity with cancellous bone Osteoblastomas • Similar to osteoid osteomas • Benign with bone destruction • Entire bone removed for cure Giant Cell Tumor of Bone • • • • • • • • Uncommon anywhere in the body Ages 30 to 50 Solitary lesion Dull constant pain Epiphyseal end of bone affected Translucent, thin cortex Sarcomatous degeneration 10% Wide resection Metastatic Tumors • • • • Very uncommon Associated with primary lung, kidney Distal phalanges Amputation recommended if life expectancy compatible Injection Injuries Injection Injury • Extravasation – Medications – Intravenous agents • Industrial hydraulic devices – – – – Paints Lubricants Adhesives Organic solvents Extravasation • Inflammatory reaction – Tissue death, slough, ulceration • Most cases recognized promptly – Temporary erythema • Major injury – Surgical debridement – Amputation Drugs • Osmotically active agents – Potassium, Calcium, Urea, PPN • Ischemia- inducing agents – Catecholamines, vasopressors • Direct cellular toxicity – Antineoplastics, bicarbonate, digoxin, diazepam Management • • • • • • Removal of line Documentation of circumstances Photographs Cool vs. Warm compresses Elevation Waiting for demarcation Management • • • • Many recognized late Close observation May require serial debridement Watch for compartment syndrome Management • Hyaluronidase – reduces tissue injury • allows rapid diffusion of irritants – Advocated for • 10% dextrose, calcium, potassium, aminophylline, naficillin, radiocontrast media, and parenteral nutrition • Experimentally beneficial for vinca alkaloids High Pressure Injection • • • • • Industrial settings Can be severe if material injected Wide surgical opening Lavage and Debridement Possible fasciotomy THE END