* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download hormones
Survey
Document related concepts
Transcript
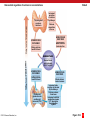
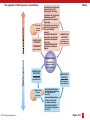
PowerPoint® Lecture Slides prepared by Betsy C. Brantley Valencia College CHAPTER 10 The Endocrine System © 2013 Pearson Education, Inc. Chapter 10 Learning Outcomes • Section 1: Hormones and Intercellular Communication • 10.1 • Explain the classification of hormones, identify key functions of hormones secreted by organs of the endocrine system, and list organs with secondary endocrine functions. • 10.2 • Compare the mechanism of action for nonsteroid and steroid hormones. • 10.3 • Describe how the hypothalamus controls other endocrine organs. © 2013 Pearson Education, Inc. Chapter 10 Learning Outcomes • Section 2: Endocrine Organs • 10.4 • Describe the location and structure of the pituitary gland, and identify pituitary hormones, their target tissues, and functions. • 10.5 • Describe the location and structure of the thyroid gland, identify the hormones it secretes, and list the effects of thyroid hormones on peripheral tissues. • 10.6 • Describe the location and structure of the parathyroid glands, identify the hormone they produce, and list the effects of parathyroid hormone on peripheral tissues. © 2013 Pearson Education, Inc. Chapter 10 Learning Outcomes • 10.7 • Describe the location, structure, and general functions of the adrenal glands, identify the hormones produced by the adrenal cortex and the adrenal medulla, and list the effects of each hormone. • 10.8 • Identify the location and structure of the pancreas, identify key pancreatic cells, and the hormones they produce, specify the functions of each hormone, and summarize blood glucose homeostasis. • 10.9 • Identify the location of the pineal gland, and identify the functions of melatonin. © 2013 Pearson Education, Inc. Chapter 10 Learning Outcomes • 10.10 • CLINICAL MODULE Define diabetes mellitus, explain Type 1 and Type 2 diabetes, list clinical problems caused by diabetes mellitus, and identify treatment for each type. • 10.11 • Define the stress response and summarize the events for each phase. © 2013 Pearson Education, Inc. Intercellular Communication (Section 1) • Coordination of cellular activity requires communication between cells • Most common type of communication uses chemical messengers • Messengers released into interstitial fluid and blood • Communication between neighboring cells by diffusion of messengers • Communication over greater distances coordinated by nervous and endocrine systems © 2013 Pearson Education, Inc. Intercellular Communication by the Endocrine and Nervous Systems Cell Type Endocrine glandular cells Neurons © 2013 Pearson Education, Inc. Transmission Through the bloodstream Across synaptic clefts Chemical Messengers Effects Hormones Long-term communication Neurotransmitters Short, quick communication Figure 10 Section 11 The Endocrine and Nervous Systems (Section 1) • Features in common • Release chemicals that bind to specific receptors • Share some of same chemical messengers (e.g., norepinephrine, epinephrine) • Regulate messenger activity by negative feedback • Common goal to preserve homeostasis © 2013 Pearson Education, Inc. Chemical Messengers (Section 1) • Endocrine – hormones • Transported in bloodstream to target cells • Target cells need appropriate receptors • Provides long-term communication (growth and development) • Nervous – neurotransmitters • Transported by diffusion across synaptic cleft • Limited to specific area • Target cells need appropriate receptors • Provides short, quick communication (reflexes) © 2013 Pearson Education, Inc. Chemical Categorization of Hormones (10.1) • Hormones divided into three groups based on chemical structure 1. Amino acid derivatives 2. Peptide hormones 3. Lipid derivatives © 2013 Pearson Education, Inc. Amino Acid Derivatives (10.1) • Small molecules related to amino acids 1. Derivatives of tyrosine • Thyroid hormone • Catecholamines (e.g., epinephrine) • Sources of tyrosine include meat, dairy, and fish 2. Derivatives of tryptophan • Melatonin • Sources of tryptophan include turkey, chocolate, oats, bananas, dried dates, milk, cottage cheese, and peanuts © 2013 Pearson Education, Inc. Peptide Hormones (10.1) • Chains of amino acids • Most synthesized as prohormones • Inactive molecules converted to active before or after secretion 1. Glycoproteins • More than 200 amino acids long with carbohydrate side chains 2. Short polypeptides/small proteins • Large and diverse group • Short chain polypeptides, 9 amino acids long • Small proteins up to 198 amino acids long © 2013 Pearson Education, Inc. Two Classes of Lipid Derivatives (10.1) 1. Eicosanoids • Derived from arachidonic acid • Coordinate cellular activities and affect enzymatic processes • Prostaglandins involved in coordinating local cellular activities 2. Steroid hormones • Derived from cholesterol • Released by reproductive organs • Androgens by testes • Estrogen and progesterone by ovaries • Released by adrenal cortex (corticosteroids) and kidneys (calcitriol) • Bound to specific transport proteins • Remain in circulation longer than peptide hormones © 2013 Pearson Education, Inc. Structural classification of hormones Amino Acid Derivatives Derivatives of Tyrosine Thyroid Hormones Thyroxine (T4) Catecholamines Epinephrine Peptide Hormones Glycoproteins Includes: Thyroid-stimulating hormone (TSH), Luteinizing hormone (LH), Follicle-stimulating hormone (FSH), and several other hormones Short Polypeptides/ Small Proteins Includes: Antidiuretic hormone (ADH), oxytocin (OXT), growth hormone (GH), prolactin (PRL), and several other hormones Lipid Derivatives Eicosanoids Prostaglandin E Aspirin suppresses the production of prostaglandins. Steroid Hormones Estrogen Sources of tyrosine include meat, dairy, and fish. Derivative of Tryptophan Melatonin Turkey is a well known source of tryptophan. Other sources include chocolate, oats, bananas, dried dates, milk, cottage cheese, and peanuts. © 2013 Pearson Education, Inc. Figure 10.1 11 Primary Endocrine System Organs (10.1) • Hypothalamus • Pituitary gland • Thyroid gland • Parathyroid glands • Adrenal glands • Pancreas (pancreatic islets) © 2013 Pearson Education, Inc. Secondary Endocrine Organs (10.1) • Contain tissues that secrete hormones, but endocrine functions are secondary • Heart hormones • Regulate blood volume • Thymus hormones • Stimulate and coordinate immune response • Digestive tract hormones • Coordinate digestive system functions, glucose metabolism, and appetite © 2013 Pearson Education, Inc. Secondary Endocrine Organs (10.1) • Adipose tissue hormones • Regulate appetite and fat metabolism • Kidney hormones • Regulate blood cell production and rates of calcium and phosphate absorption by intestinal tract • Gonadal hormones • Affect growth, metabolism, and sexual characteristics • Coordinate activities of organs in reproductive system © 2013 Pearson Education, Inc. Structural classification of hormones Pineal Gland Hypothalamus Organs with Secondary Endocrine Functions Pituitary Gland Thyroid Gland Heart Parathyroid Glands Thymus Adrenal Glands Digestive tract Pancreas (Pancreatic Islets) Adipose tissue Kidneys Testis Gonads Ovary © 2013 Pearson Education, Inc. Figure 10.1 22 Module 10.1 Review a. Define endocrine system. b. Describe the structural classification of hormones. c. Name the primary organs of the endocrine system and those organs and tissues with secondary endocrine functions. © 2013 Pearson Education, Inc. Nonsteroid Hormones Mechanism (10.2) • Bind to receptors on plasma membrane • Activate G proteins • Use second messenger • Intracellular intermediate alters enzyme activity in cell • Often high-energy compounds like cyclic-AMP (cAMP) • Nonsteroid hormones include: • Lipid soluble (eicosanoids) with receptors on inner surface of membrane • Not lipid soluble (catecholamines, peptide hormones) with receptors on outer surface of membrane © 2013 Pearson Education, Inc. Nonsteroid hormones and second messenger mechanism Nonsteroid hormone (first messenger) Plasma membrane 1 Binding of hormone to plasma membrane receptor 2 G protein activated 3 4 CYTOPLASM Second messenger system activated Cellular enzyme activity changed Target cell response NUCLEUS Nuclear envelope Nuclear pore © 2013 Pearson Education, Inc. DNA Figure 10.2 111 24 Steroid Hormones Mechanisms of Action (10.2) • Pass directly through target cell's plasma membrane • Lipid soluble • Bind to receptors in cytoplasm and nucleus • Affect gene activity and protein synthesis © 2013 Pearson Education, Inc. Steroid hormone mechanism 1 Steroid hormone Diffusion through membrane lipids Target cell response Alteration of cellular structure or activity 6 2 Receptor Translation and protein synthesis Binding of hormone to cytoplasmic or nuclear receptors creates a hormonereceptor complex. 5 4 Receptor Nuclear pore Nuclear envelope © 2013 Pearson Education, Inc. Transcription and mRNA production 3 Gene activation Binding of hormone-receptor complex to DNA Figure 10.2 221 24 Module 10.2 Review a. Describe two mechanisms of hormone action. b. Which type of hormone binds to a plasma membrane receptor and why? c. Which type of hormone diffuses across the plasma membrane and binds to receptors in the cytoplasm? © 2013 Pearson Education, Inc. Hypothalamus Control (10.3) • Integrates activities of nervous and endocrine systems through three mechanisms 1. Synthesis and transport of two hormones to posterior pituitary • Antidiuretic hormone (ADH) • Oxytocin (OXT) 2. Secretion of regulatory hormones to anterior pituitary • Releasing hormone (RH) • Inhibiting hormone (IH) 3. Autonomic centers © 2013 Pearson Education, Inc. Posterior Lobe of the Pituitary Gland (10.3) • ADH and oxytocin • Synthesized in hypothalamus • Released into circulation from posterior lobe of pituitary gland © 2013 Pearson Education, Inc. Anterior Lobe of the Pituitary Gland (10.3) • Regulatory hormones carried to anterior lobe by hypophyseal portal system • Releasing hormone stimulates secretion of hormone from anterior lobe • Inhibiting hormone prevents secretion of hormone from anterior lobe • Hormones from anterior lobe control: • Thyroid gland • Adrenal cortex • Reproductive organs © 2013 Pearson Education, Inc. Autonomic Centers (10.3) • Exert direct neural control over endocrine cells in adrenal medulla • Active when sympathetic division stimulated • Adrenal medulla responds by releasing epinephrine (E) and norepinephrine (NE) © 2013 Pearson Education, Inc. Three mechanisms of hypothalmic control over endocrine function 1 Antidiuretic hormone and oxytocin are synthesized by hypothalamic neurons. 2 Regulatory and inhibitory hormones target the anterior lobe of the pituitary gland. 3 Autonomic centers exert direct neural control over endocrine cells in the adrenal medullae. HYPOTHALAMUS Preganglionic motor fibers Hypophyseal portal system Anterior lobe of pituitary gland Hormones from anterior lobe of the pituitary gland target the thyroid, adrenal cortex, and reproductive organs. © 2013 Pearson Education, Inc. Adrenal cortex Adrenal medulla Posterior lobe of pituitary gland ADH and oxytocin are released into circulation from posterior lobe of the pituitary gland. Adrenal gland Upon direct neuronal stimulation, the adrenal medullae secrete epinephrine and norepinephrine into the circulation. Figure 10.3 11 Module 10.3 Review a. Identify the three mechanisms by which the hypothalamus integrates neural and endocrine function. b. Define regulatory hormone. c. Contrast releasing hormones with inhibiting hormones. © 2013 Pearson Education, Inc. Primary Endocrine Organs (Section 2) • Pituitary gland • Secretes multiple hormones regulating activities of adrenal cortex, thyroid gland, reproductive organs, and melatonin production • Thyroid gland • Affects metabolic rate and calcium levels in body fluids • Adrenal glands • Hormones involved with mineral balance, metabolic control, and resistance to stress • Adrenal medulla releases E and NE in response to sympathetic activation © 2013 Pearson Education, Inc. Primary Endocrine Organs (Section 2) • Pineal gland • Secretes melatonin • Affects reproductive function and circadian rhythm • Parathyroid glands • Secrete hormone important for regulating calcium ion concentration in body fluids • Pancreas (pancreatic islets) • Secrete hormones regulating glucose uptake and utilization © 2013 Pearson Education, Inc. Primary Endocrine Organs (Section 2) • Pituitary gland, parathyroid gland, pineal gland, pancreatic islets, some adrenal hormones • Exert effects through second messenger systems • Primarily impact enzyme activities • Thyroid hormones and other adrenal hormones • Primarily alter genetic activities • Effects take longer to appear © 2013 Pearson Education, Inc. Primary endocrine organs Pituitary Gland Pineal Gland Thyroid Gland Parathyroid Glands Adrenal Glands © 2013 Pearson Education, Inc. Pancreas (Pancreatic Islets) Figure 10 Section 2 The Pituitary Gland as a Master Gland (10.4) • Small, oval gland • Nestled within sella turcica, depression in sphenoid • Releases nine important peptide hormones • Seven secreted by the anterior pituitary • Two released from the posterior pituitary (made by the hypothalamus) • All bind to membrane receptors • All use same second messenger © 2013 Pearson Education, Inc. Pituitary hormones and their targets HYPOTHALAMUS Floor of hypothalamus Hormones of the Posterior Lobe of the Pituitary Gland Optic chiasm Fold of dura mater Anterior lobe of the pituitary gland ADH OXT Antidiuretic hormone (ADH), also known as vasopressin Oxytocin (okytokos, swift birth), or OXT Posterior lobe of the pituitary gland Kidney Hormones of the Anterior Lobe of the Pituitary Gland Gonadotropins (FSH and LH) TSH ACTH GH Adrenocorticotropic Thyroidhormone (ACTH) stimulating hormone (TSH) Thyroid gland © 2013 Pearson Education, Inc. Adrenal gland Folliclestimulating hormone (FSH) Ovary Luteinizing (LOO-tē-in-ī-zing) hormone (LH) Testis Growth hormone (GH) Uterus PRL MSH Prolactin (pro-, before + lac, milk) (PRL) Melanocytestimulating hormone (MSH) Muscular and skeletal systems Figure 10.4 Anterior Lobe of the Pituitary Gland (10.4) • Secretes seven hormones called tropic hormones • 1. 2. 3. 4. 5. 6. 7. "Turn on" other endocrine glands or support functions of other organs TSH ACTH FSH LH GH PRL MSH © 2013 Pearson Education, Inc. Anterior Pituitary Gland Hormones (10.4) 1. Thyroid-stimulating hormone (TSH) • Also called thyrotropin • Targets thyroid gland • Triggers release of thyroid hormones 2. Adrenocorticotropic hormone (ACTH) • Also called corticotropin • Targets cells of adrenal cortex • Triggers release of steroid hormones • © 2013 Pearson Education, Inc. Specifically hormones affecting glucose metabolism Anterior Pituitary Gland Hormones (10.4) • Gonadotropins regulate the activities of the gonads • • Gonads are organs (testes and ovaries) that produce reproductive cells and hormones Gonadotropins include FSH and LH 3. Follicle-stimulating hormone (FSH) • Females • • • Males • • Promotes ovarian follicle development Stimulates secretion of estrogen Promotes maturation of sperm Inhibited by inhibin, released by cells in testes and ovaries © 2013 Pearson Education, Inc. Anterior Pituitary Gland Hormones (10.4) 4. Luteinizing hormone (LH) • • Females • Induces ovulation • Promotes secretion of estrogen and progestins Males • Stimulates production of sex hormones (androgens) by interstitial cells • © 2013 Pearson Education, Inc. Testosterone most important androgen Anterior Pituitary Gland Hormones (10.4) 5. Growth hormone (GH) • • • Stimulates cell growth and reproduction Accelerates rate of protein synthesis Epithelia and connective tissues • • • Stimulates stem cell divisions and differentiations Adipose tissue • Stimulates break down of triglycerides into fatty acids • Glucose-sparing effect when tissues use fatty acids instead of glucose to generate ATP Liver • © 2013 Pearson Education, Inc. Stimulates breakdown of glycogen reserves Anterior Pituitary Gland Hormones (10.4) 6. Prolactin (PRL) • Stimulates mammary gland development • Stimulates milk production by mammary glands in pregnancy and nursing period 7. Melanocyte-stimulating hormone (MSH) • Stimulates melanocytes of skin to increase production of melanin • Portion of anterior lobe that produces this is virtually nonfunctional in adults © 2013 Pearson Education, Inc. Hormones of the anterior lobe of the pituitary gland Hormones of the Anterior Lobe of the Pituitary Gland Gonadotropins (FSH and LH) ACTH TSH GH Adrenocorticotropic FollicleThyroidLuteinizing hormone (ACTH) stimulating (LOO-tē-in-ī-zing) stimulating hormone hormone hormone (TSH) (FSH) (LH) Thyroid gland © 2013 Pearson Education, Inc. Adrenal gland Ovary Testis PRL Growth Prolactin hormone (GH) (pro-, before + lac, milk) (PRL) MSH Melanocytestimulating hormone (MSH) Muscular and skeletal systems Figure 10.4 Posterior Lobe of the Pituitary Gland (10.4) • Contains axons of hypothalamic neurons • Releases two hormones 1. Antidiuretic hormone (ADH) or vasopressin 2. Oxytocin (OXT) © 2013 Pearson Education, Inc. Posterior Pituitary Gland Hormones (10.4) 1. Antidiuretic Hormone (ADH) or vasopressin • Released in response to: • • • • • Neurosecretory neurons stimulated by osmoreceptors Primary function to decrease water loss at kidneys • • • Rise in solute concentration in blood Fall in blood volume Decreased blood pressure Resulting water retention reduces electrolyte concentration in extracellular fluid Also causes vasoconstriction, helping raise blood pressure Alcohol inhibits ADH release © 2013 Pearson Education, Inc. Posterior Pituitary Gland Hormones (10.4) 2. Oxytocin (OXT) • In women, stimulates smooth muscle contraction in wall of uterus • • Stimulates contraction of cells in mammary glands • • Promotes labor and delivery Promotes ejection of milk Find increased levels in both sexes during sexual arousal and orgasm © 2013 Pearson Education, Inc. Hormones of the posterior lobe of the pituitary gland Hormones of the Posterior Lobe of the Pituitary Gland ADH OXT Antidiuretic hormone (ADH), also known as vasopressin Oxytocin (okytokos, swift birth), or OXT Kidney © 2013 Pearson Education, Inc. Uterus Figure 10.4 Module 10.4 Review a. Name the two lobes of the pituitary gland and the cellular sources of their secreted hormones. b. Identify the nine pituitary hormones and their target tissues. c. In a dehydrated person, how would the amount of ADH released by the posterior pituitary change? © 2013 Pearson Education, Inc. Thyroid Gland (10.5) • On anterior surface of trachea • Inferior to thyroid cartilage • Two lobes connected by narrow isthmus • Variable size depending on: • Heredity • Environmental factors • Nutritional factors • Average weight 34 g • Deep red color from extensive blood supply © 2013 Pearson Education, Inc. The thyroid gland Thyroid cartilage Right lobe of thyroid gland Isthmus of thyroid gland Internal jugular vein Left lobe of thyroid gland Common carotid artery Simple cuboidal epithelium of follicle Thyroglobulin in colloid Trachea Outline of clavicle Outline of sternum Thyroid follicle C (clear) cells Section of thyroid gland LM x 260 © 2013 Pearson Education, Inc. Figure 10.5 1 – 2 Thyroid Follicles (10.5) • Thyroid gland filled with thyroid follicles • Hollow spheres lined with simple cuboidal epithelium • Colloid in cavity • Viscous fluid containing dissolved proteins • Follicular cells synthesize thyroglobulin • Contains amino acid tyrosine • Iodide ions added to form thyroid hormones • Thyroglobulin-hormone complex stored in follicle © 2013 Pearson Education, Inc. Parafollicular Cells (10.5) • In thyroid gland, cells outside follicles • Large, pale, clear cells called C (clear) cells or parafollicular cells • Produce calcitonin (CT) • Helps regulate calcium ion concentrations in body fluids © 2013 Pearson Education, Inc. Histological organization of thyroid gland Simple cuboidal epithelium of follicle Thyroglobulin in colloid Thyroid follicle C (clear) cells Section of thyroid gland LM x 260 © 2013 Pearson Education, Inc. Figure 10.5 2 Thyroglobulin (10.5) • Thyroglobulin broken down by follicular cells into two hormones released into bloodstream 1. T3 (triiodothyronine) with three iodide ions 2. T4 (thyroxine) with four iodide ions • About 75 percent thyroid hormones attached to transport proteins • Thyroid-binding globulins (TBGs) • Release thyroid hormones gradually • More than a week's supply of thyroid hormone in bloodstream bound to transport proteins © 2013 Pearson Education, Inc. Thyroid Hormone Transport (10.5) • Transported across plasma membrane • Primarily by carrier-mediated processes • Inside cell • Bind to receptors on mitochondria and within the nucleus • Increase rate of ATP production • In nucleus, activate specific genes or changes rate of transcription • Affect concentration of enzymes and so metabolic activities of cell © 2013 Pearson Education, Inc. Mechanism of thyroid hormone entry and action in a cell Thyroid-binding globulin Thyroid hormone (T3 and T4) 1 Carrier-mediated transport across the plasma membrane Target cell response Increased Receptor Alteration of cellular structure or enzymatic activity production 6 2 Binding to receptors at mitochondria and within the nucleus. Mitochondria respond by increasing ATP production. Translation and protein synthesis 5 Transcription and mRNA production Receptor 4 Gene activation 3 © 2013 Pearson Education, Inc. Binding of hormone-receptor complex to DNA Figure 10.5 4 Effects of Thyroid Hormones on Peripheral Tissues (10.5) • Raise metabolic rate • • In children, may raise body temperature, oxygen, and energy Increase heart rate and force of contraction • Generally raise blood pressure • Increase sensitivity to sympathetic stimulation • Maintain normal sensitivity of respiratory centers to changes in oxygen and carbon dioxide concentrations © 2013 Pearson Education, Inc. Effects of Thyroid Hormones on Peripheral Tissues (10.5) • Stimulate red blood cell formation • Enhancing oxygen concentration • Stimulate activity in other endocrine tissues • Accelerate turnover of minerals in bone © 2013 Pearson Education, Inc. Module 10.5 Review a. Name the three hormones secreted by the thyroid gland. b. List five effects that thyroid hormones have on peripheral tissues. c. After a thyroidectomy (surgical removal of the thyroid gland), symptoms of decreased thyroid hormone concentrations take about a week to appear. Why? © 2013 Pearson Education, Inc. Parathyroid Glands (10.6) • Four parathyroid glands • Embedded in posterior surface of thyroid gland • Shaped like small peas • Total weight 1.6 g • Covered by capsule of thyroid gland © 2013 Pearson Education, Inc. The parathyroid glands Thyroid gland Parathyroid glands Blood vessel Dense fibrous capsule Parathyroid gland © 2013 Pearson Education, Inc. LM x 94 Thyroid follicles Figure 10.6 1 – 2 Two Parts to the Parathyroid (10.6) 1. Parathyroid cells • Produce parathyroid hormone (PTH) • Secreted in response to low calcium concentrations in blood 2. Oxyphils • No known function © 2013 Pearson Education, Inc. Calcium Ion Balance (10.6) • Calcitonin lowers blood calcium; PTH raises blood calcium • PTH primary regulator of circulating calcium ion concentration • Increases calcium reabsorption in kidneys • Increases calcitriol production • Increases calcium absorption from digestive system • Causes release of calcium from bone • Elevated calcium levels are rare • Removal of thyroid gland (and calcitonin) seldom affects balance • Can give calcitonin if needed for disorders that raise calcium levels, causing excessive bone formation © 2013 Pearson Education, Inc. Slide 1 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations HOMEOSTASIS DISTURBED Rising calcium levels in blood HOMEOSTASIS © 2013 Pearson Education, Inc. Figure 10.6 3 Slide 2 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations Thyroid gland produces calcitonin HOMEOSTASIS DISTURBED Rising calcium levels in blood HOMEOSTASIS © 2013 Pearson Education, Inc. Figure 10.6 3 Slide 3 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations Thyroid gland produces calcitonin Increased excretion of calcium by kidneys Calcium deposition in bone HOMEOSTASIS DISTURBED Rising calcium levels in blood HOMEOSTASIS © 2013 Pearson Education, Inc. Figure 10.6 3 Slide 4 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations © 2013 Pearson Education, Inc. Thyroid gland produces calcitonin Increased excretion of calcium by kidneys Calcium deposition in bone HOMEOSTASIS RESTORED HOMEOSTASIS DISTURBED Blood calcium levels decline Rising calcium levels in blood HOMEOSTASIS Figure 10.6 3 Slide 5 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations Thyroid gland produces calcitonin Increased excretion of calcium by kidneys Calcium deposition in bone HOMEOSTASIS RESTORED HOMEOSTASIS DISTURBED Blood calcium levels decline Rising calcium levels in blood HOMEOSTASIS Normal blood calcium levels (8.5–11 mg/dL) HOMEOSTASIS DISTURBED Falling calcium levels in blood © 2013 Pearson Education, Inc. Figure 10.6 3 Slide 6 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations Thyroid gland produces calcitonin Increased excretion of calcium by kidneys Calcium deposition in bone HOMEOSTASIS RESTORED HOMEOSTASIS DISTURBED Blood calcium levels decline Rising calcium levels in blood HOMEOSTASIS Normal blood calcium levels (8.5–11 mg/dL) HOMEOSTASIS DISTURBED Falling calcium levels in blood Parathyroid glands secrete parathyroid hormone (PTH) © 2013 Pearson Education, Inc. Figure 10.6 3 Slide 7 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations Thyroid gland produces calcitonin Increased excretion of calcium by kidneys Calcium deposition in bone HOMEOSTASIS RESTORED HOMEOSTASIS DISTURBED Blood calcium levels decline Rising calcium levels in blood HOMEOSTASIS Normal blood calcium levels (8.5–11 mg/dL) HOMEOSTASIS DISTURBED Falling calcium levels in blood Parathyroid glands secrete parathyroid hormone (PTH) © 2013 Pearson Education, Inc. Increased reabsorption of calcium by the kidneys Calcium release from bone Increased calcitriol production causes Ca2+ absorption from digestive system Figure 10.6 3 Slide 8 Rising levels of blood calcium Homeostatic regulation of calcium ion concentrations Thyroid gland produces calcitonin Increased excretion of calcium by kidneys Calcium deposition in bone HOMEOSTASIS RESTORED HOMEOSTASIS DISTURBED Blood calcium levels decline Rising calcium levels in blood HOMEOSTASIS Normal blood calcium levels (8.5–11 mg/dL) HOMEOSTASIS DISTURBED Falling calcium levels in blood Parathyroid glands secrete parathyroid hormone (PTH) © 2013 Pearson Education, Inc. HOMEOSTASIS RESTORED Blood calcium levels increase Increased reabsorption of calcium by the kidneys Calcium release from bone Increased calcitriol production causes Ca2+ absorption from digestive system Figure 10.6 3 Effects of Parathyroid Hormone on Peripheral Tissues (10.6) • Mobilizes calcium from bone by affecting osteoblast and osteoclast activity • PTH inhibits osteoblasts • • • • • Reduces rate of calcium deposition in bone Osteoclast activity erodes bone matrix Plasma calcium levels rise Enhances reabsorption of calcium by kidneys Stimulates formation and secretion of calcitriol at kidneys • Calcitriol enhances calcium and phosphate absorption by the digestive system © 2013 Pearson Education, Inc. Module 10.6 Review a. Describe the locations of the parathyroid glands. b. Explain how parathyroid hormone raises blood calcium levels. c. Increased blood calcium levels would result in increased secretion of which hormone? © 2013 Pearson Education, Inc. Adrenal Glands (10.7) • Pyramid-shaped gland • On superior border of each kidney • Only anterior surface is covered with parietal peritoneum • Rich blood supply • Outer cortex region and inner medulla region • Cortex yellow from stored lipids © 2013 Pearson Education, Inc. The adrenal gland Capsule Adrenal cortex Adrenal medulla Right adrenal gland Adrenal arteries Left adrenal gland Right kidney Left kidney Abdominal aorta Inferior vena cava © 2013 Pearson Education, Inc. Figure 10.7 1 1– –24 2 Adrenal Hormones (10.7) • Adrenal cortex • Produces more than two dozen steroid hormones called corticosteroids • Affect genes in target cells, resulting in changes in enzymes and cellular metabolism • Adrenal medulla • Produces epinephrine and norepinephrine • Responds to sympathetic activation © 2013 Pearson Education, Inc. The adrenal gland and its hormones The Adrenal Hormones Region/ Zone Capsule Adrenal cortex Adrenal medulla Right adrenal Adrenal gland arteries Right kidney Left adrenal gland Left kidney Abdominal aorta Inferior vena cava Adrenal gland LM x 250 © 2013 Pearson Education, Inc. Hormones Primary Targets Hormonal Effects Regulatory Control Increased renal reabsorption of Na+ and water; accelerates urinary loss of K+ Stimulated by renin-angiotensin system; inhibited by opposing hormones Capsule ADRENAL CORTEX Outer zone of the adrenal cortex Mineralocorticoids (MCs), primarily aldosterone Kidneys Large, central zone of the adrenal cortex Glucocorticoids, primarily cortisol Increase glucose and glycogen formation and reduces inflammation Skin, bones, Adrenal androgens stimulate and other the development tissues, but of pubic hair in minimal boys and girls effects in normal adults before puberty. Most cells Narrow zone bordering each adrenal medulla Androgens ADRENAL MEDULLA Epinephrine Most cells (E) and norepinephrine (NE) Epinephrine and norepinephrine increase cardiac activity, blood pressure, glycogen breakdown, and blood glucose levels. Stimulated by ACTH Stimulated by ACTH Epinephrine and norepinephrine secretion is stimulated by sympathetic preganglionic fibers during sympathetic activation. Figure 10.7 Zones of the Adrenal Cortex (10.7) • Outer zone • Secretes mineralocorticoids (MCs), primarily aldosterone • Central zone • Secretes glucocorticoids (GCs), primarily cortisol • Involved in glucose-sparing effect and anti-inflammatory effect • Also secretes corticosterone, which liver converts to cortisone • Inner zone bordering adrenal medulla • Secretes androgens that can be converted to estrogens © 2013 Pearson Education, Inc. The Adrenal Hormones Region/ Zone Hormones Primary Targets Hormonal Effects Regulatory Control Capsule ADRENAL CORTEX Outer zone Mineraloof the adre- corticoids (MCs), nal cortex primarily aldosterone Adrenal gland © 2013 Pearson Education, Inc. Kidneys Increased renal reabsorption of Na+ and water; accelerates urinary loss of K+ Stimulated by reninangiotensin system; inhibited by opposing hormones Large, central zone of the adrenal cortex Glucocorticoids, primarily cortisol Most cells Increase glucose and glycogen formation and reduces inflammation Stimulated by ACTH Narrow zone bordering each adrenal medulla Androgens Skin, bones, and other tissues, but minimal effects in normal adults Adrenal androgens stimulate the development of pubic hair in boys and girls before puberty. Stimulated by ACTH ADRENAL MEDULLA Epinephrine (E) and norepinephrine (NE) Most cells Epinephrine and Epinephrine and norepinephrine norepinephrine secreincrease cardiac tion is stimulated by activity, blood pres- sympathetic preganglisure, glycogen break- onic fibers during down, and blood sympathetic glucose levels. activation. LM x 250 Figure 10.7 3 Module 10.7 Review a. Identify the two regions of an adrenal gland, and cite the hormones secreted by each. b. Identify the target tissue for aldosterone. c. How would elevated cortisol levels affect blood glucose levels? © 2013 Pearson Education, Inc. The Pancreas (10.8) • In abdominopelvic cavity between inferior border of stomach and proximal portion of small intestine • About 20–25 cm long • Weighs 80 g • Has both exocrine and endocrine functions • Exocrine pancreas is 99 percent of organ's volume • Forms clusters (pancreatic acini) around small ducts • Secretes enzymes through ducts to digestive tract © 2013 Pearson Education, Inc. Pancreatic structures Body of Small intestine (duodenum) Pancreatic pancreas duct © 2013 Pearson Education, Inc. Lobule Figure 10.8 11 24 The Endocrine Pancreas (10.8) • Pancreatic islets (or islets of Langerhans) • Small groups of cells among exocrine cells • Roughly 2 million pancreatic islets in pancreas • Alpha cells • Produce hormone glucagon • Raises blood glucose levels • Beta cells • Produce hormone insulin • Lowers blood glucose levels © 2013 Pearson Education, Inc. Pancreatic islet surrounded by pancreatic exocrine cells Alpha cells produce glucagon Pancreatic acini Capillaries Beta cells produce insulin Pancreatic islet © 2013 Pearson Education, Inc. Figure 10.8 21 24 Insulin and Glucagon (10.8) • Primary hormones regulating blood glucose levels • Rising blood glucose levels triggers beta cells • Insulin lowers blood glucose levels • Increases rate of glucose uptake and utilization by cells • Increases rate of glycogen synthesis in skeletal muscle and liver • Dropping blood glucose levels triggers alpha cells • Glucagon raises blood glucose levels • Increases rate of glycogen breakdown and glucose release by liver © 2013 Pearson Education, Inc. Slide 1 The regulation of blood glucose concentrations HOMEOSTASIS DISTURBED Rising blood glucose levels HOMEOSTASIS © 2013 Pearson Education, Inc. Figure 10.8 31 24 Slide 2 The regulation of blood glucose concentrations Beta cells secrete insulin. HOMEOSTASIS DISTURBED Rising blood glucose levels HOMEOSTASIS © 2013 Pearson Education, Inc. Figure 10.8 31 24 The regulation of blood glucose concentrations Beta cells secrete insulin. HOMEOSTASIS DISTURBED Rising blood glucose levels Slide 3 Increased rate of glucose transport into cells (throughout the body) Increased rate of glucose utilization and ATP generation (throughout the body) Increased conversion of glucose to glycogen (in liver and skeletal muscle) Increased amino acid absorption and protein synthesis (throughout the body) Increased triglyceride synthesis (in adipose tissue) HOMEOSTASIS © 2013 Pearson Education, Inc. Figure 10.8 31 24 The regulation of blood glucose concentrations Beta cells secrete insulin. HOMEOSTASIS DISTURBED Rising blood glucose levels Slide 4 Increased rate of glucose transport into cells (throughout the body) Increased rate of glucose utilization and ATP generation (throughout the body) Increased conversion of glucose to glycogen (in liver and skeletal muscle) HOMEOSTASIS Increased amino acid RESTORED absorption and protein synthesis (throughout Blood glucose the body) levels decrease Increased triglyceride synthesis (in adipose tissue) HOMEOSTASIS © 2013 Pearson Education, Inc. Figure 10.8 31 24 The regulation of blood glucose concentrations Beta cells secrete insulin. HOMEOSTASIS DISTURBED Rising blood glucose levels Slide 5 Increased rate of glucose transport into cells (throughout the body) Increased rate of glucose utilization and ATP generation (throughout the body) Increased conversion of glucose to glycogen (in liver and skeletal muscle) HOMEOSTASIS Increased amino acid RESTORED absorption and protein synthesis (throughout Blood glucose the body) levels decrease Increased triglyceride synthesis (in adipose tissue) HOMEOSTASIS Normal blood glucose levels (70–110 mg/dL) HOMEOSTASIS DISTURBED Falling blood glucose levels © 2013 Pearson Education, Inc. Figure 10.8 31 24 The regulation of blood glucose concentrations Beta cells secrete insulin. HOMEOSTASIS DISTURBED Rising blood glucose levels Slide 6 Increased rate of glucose transport into cells (throughout the body) Increased rate of glucose utilization and ATP generation (throughout the body) Increased conversion of glucose to glycogen (in liver and skeletal muscle) HOMEOSTASIS Increased amino acid RESTORED absorption and protein synthesis (throughout Blood glucose the body) levels decrease Increased triglyceride synthesis (in adipose tissue) HOMEOSTASIS Normal blood glucose levels (70–110 mg/dL) HOMEOSTASIS DISTURBED Falling blood glucose levels Alpha cells secrete glucagon © 2013 Pearson Education, Inc. Figure 10.8 31 24 The regulation of blood glucose concentrations Beta cells secrete insulin. HOMEOSTASIS DISTURBED Rising blood glucose levels Slide 7 Increased rate of glucose transport into cells (throughout the body) Increased rate of glucose utilization and ATP generation (throughout the body) Increased conversion of glucose to glycogen (in liver and skeletal muscle) HOMEOSTASIS Increased amino acid RESTORED absorption and protein synthesis (throughout Blood glucose the body) levels decrease Increased triglyceride synthesis (in adipose tissue) HOMEOSTASIS Normal blood glucose levels (70–110 mg/dL) HOMEOSTASIS DISTURBED Falling blood glucose levels Alpha cells secrete glucagon © 2013 Pearson Education, Inc. Increased breakdown of glycogen to glucose (in liver, skeletal muscle) Increased breakdown of fat to fatty acids (in adipose tissue) Increased synthesis and release of glucose (in liver) Figure 10.8 31 24 The regulation of blood glucose concentrations Beta cells secrete insulin. HOMEOSTASIS DISTURBED Rising blood glucose levels Slide 8 Increased rate of glucose transport into cells (throughout the body) Increased rate of glucose utilization and ATP generation (throughout the body) Increased conversion of glucose to glycogen (in liver and skeletal muscle) HOMEOSTASIS Increased amino acid RESTORED absorption and protein synthesis (throughout Blood glucose the body) levels decrease Increased triglyceride synthesis (in adipose tissue) HOMEOSTASIS Normal blood glucose levels (70–110 mg/dL) HOMEOSTASIS DISTURBED HOMEOSTASIS RESTORED Falling blood glucose levels Alpha cells secrete glucagon © 2013 Pearson Education, Inc. Blood glucose levels increase Increased breakdown of glycogen to glucose (in liver, skeletal muscle) Increased breakdown of fat to fatty acids (in adipose tissue) Increased synthesis and release of glucose (in liver) Figure 10.8 31 24 Module 10.8 Review a. Identify two important types of cells in the pancreatic islets and the hormones produced by each. b. The secretion of which hormone lowers blood glucose concentrations? c. How do rising glucagon levels affect the amount of glycogen stored in the liver? © 2013 Pearson Education, Inc. The Pineal Gland (10.9) • Part of epithalamus • In posterior portion of roof of third ventricle • Contains neurons, neuroglia, and secretory cells • Secretory cells produce melatonin • Rate of melatonin production influenced by visual pathway • Highest production at night • Lowest production during daylight hours © 2013 Pearson Education, Inc. The pineal gland Melatonin-secreting cells Pineal Gland © 2013 Pearson Education, Inc. LM x 450 Figure 10.9 11 24 Functions of Melatonin in Humans (10.9) • Inhibit reproductive functions • In some mammals, slows maturation of sperm, oocytes, and reproductive organs by reducing rate of GnRH secretion • May play role in timing human sexual maturation • Blood levels decline at puberty • Pineal tumors eliminating melatonin cause premature puberty © 2013 Pearson Education, Inc. Functions of Melatonin in Humans (10.9) • Effective antioxidant • • May protect CNS neurons from free radicals • Nitric oxide, hydrogen peroxide • Generated in active neural tissue Set circadian rhythms • Daily changes in physiological processes following a regular day-night pattern • Result of cyclical pineal activity © 2013 Pearson Education, Inc. Module 10.9 Review a. Describe the location of the pineal gland. b. How would longer hours of daylight, as during the summer, affect the production of melatonin? c. List the three functions of melatonin. © 2013 Pearson Education, Inc. Diabetes Mellitus (10.10) • Endocrine disorder characterized by high blood glucose levels (hyperglycemia) • Kidney reabsorption overwhelmed, so glucose in urine (glycosuria) • Urine volume increases (polyuria) • Disrupts metabolic activities throughout body • Cells shift to lipids and proteins as energy source • By-products (ketone bodies) can cause diabetic ketoacidosis © 2013 Pearson Education, Inc. Type 1 Diabetes Mellitus (10.10) • Type 1 (insulin dependent) diabetes • Pancreatic beta cells do not produce enough insulin • Patients must have daily injections or continuous infusions of insulin to live • 5–10 percent of diabetes cases • Often develops in childhood © 2013 Pearson Education, Inc. Type 2 Diabetes Mellitus (10.10) • Type 2 (non-insulin dependent) diabetes • Most common form of diabetes mellitus • May produce normal amounts of insulin • Body cells do not respond properly • Insulin resistance • Associated with obesity • Exercise and diet can be effective treatment • Medications can also alter rates of glucose synthesis and release by liver © 2013 Pearson Education, Inc. Diabetes Mellitus and related clinical problems Diabetes Mellitus Type 1 (insulin dependent) Diabetes © 2013 Pearson Education, Inc. Type 2 (non-insulin dependent) Diabetes Figure 10.10 Diabetes Mellitus – Clinical Problems (10.10) • Diabetic retinopathy • Partial or complete blindness from proliferation of capillaries and hemorrhaging at retina • Increased risk of heart attack • From increased blockages in cardiac circulation • Diabetic nephropathy • Degenerative changes in kidneys can lead to kidney failure • Diabetic neuropathy • Damage to nerves from abnormal blood flow to neural tissue • Damage to peripheral tissues (ulceration, infection) • From reduced blood flow to distal portions of limbs © 2013 Pearson Education, Inc. Diabetes Mellitus and related clinical problems Clinical Problems Caused by Diabetes Mellitus Diabetic retinopathy Increased risk of heart attack Diabetic nephropathy Diabetic neuropathy Reduced blood flow to distal portions of limbs, damaging peripheral tissues © 2013 Pearson Education, Inc. Figure 10.10 Module 10.10 Review a. Define diabetes mellitus. b. Identify and describe the two types of diabetes mellitus. c. Describe three clinical problems caused by diabetes mellitus. © 2013 Pearson Education, Inc. Stress Response (10.11) • Any condition that threatens homeostasis is a form of stress • May be physical or emotional • Several mechanisms in body to oppose specific disruption • Body also has general response to stress • Pattern of hormonal and physiological adjustments called stress response or general adaptation syndrome (GAS) © 2013 Pearson Education, Inc. Three Stages of Stress Response (10.11) 1. Alarm phase 2. Resistance phase 3. Exhaustion phase © 2013 Pearson Education, Inc. Alarm Phase (10.11) • "Fight or flight" • Immediate response directed by sympathetic nervous system 1. Energy reserves mobilized, primarily as glucose 2. Body prepares through "fight or flight" responses • Epinephrine dominant hormone • Causes generalized sympathetic activation © 2013 Pearson Education, Inc. Resistance Phase (10.11) • If stress is longer than a few hours, body moves into the second phase (resistance phase) • Glucocorticoids are the dominant hormones with help from epinephrine, GH, and thyroid hormone • Energy demands are still higher than normal • Neural tissue has high demand for energy • Glycogen reserves that were adequate in alarm phase are nearly exhausted • Body's metabolic reserves are mobilized and tissue metabolism is shifted away from glucose where possible © 2013 Pearson Education, Inc. Exhaustion Phase (10.11) • Lipid reserves can maintain resistance phase for weeks or months • When reserves are depleted, body enters third phase (exhaustion phase) • Mineral (Na+, K+) imbalances are involved causing neuron and muscle fiber malfunction • Without immediate corrective action, organ systems fail causing death © 2013 Pearson Education, Inc. Slide 1 General adaptation syndrome Alarm Phase (“Fight or Flight”) Brain Adrenal medulla Epinephrine, norepinephrine Sympathetic stimulation General sympathetic activation Immediate Short-Term Responses to Crises • Mobilize glycogen and lipid reserves to form glucose • Increase mental alertness • Increase energy use by all cells • Change circulation patterns • Reduce digestive activity and urine production • Increase sweat gland secretion • Increase heart rate and respiratory rate © 2013 Pearson Education, Inc. Figure 10.11 1 Slide 2 General adaptation syndrome Alarm Phase (“Fight or Flight”) Brain Resistance Phase Sympathetic stimulation Brain Adrenal medulla Epinephrine, norepinephrine General sympathetic activation Immediate Short-Term Responses to Crises • Mobilize glycogen and lipid reserves to form glucose • Increase mental alertness • Increase energy use by all cells • Change circulation patterns • Reduce digestive activity and urine production • Increase sweat gland secretion • Increase heart rate and respiratory rate © 2013 Pearson Education, Inc. Reninangiotensin system Sympathetic stimulation ACTH Pancreas Adrenal cortex Mineralocorticoids Glucagon Growth (with ADH) Glucocortichormone oids Long-Term Metabolic Adjustments • Mobilize remaining energy reserves: Adipose tissue releases lipids; skeletal muscle releases amino acids • Conserve glucose: Peripheral tissues (except neural) break down lipids to obtain energy • Raise blood glucose concentrations: Liver synthesizes glucose from other carbohydrates, amino acids, and lipids • Conserve salts and water; lose K+ and H+ Figure 10.11 1 Slide 3 General adaptation syndrome Alarm Phase (“Fight or Flight”) Brain Resistance Phase Sympathetic stimulation Brain Adrenal medulla Epinephrine, norepinephrine General sympathetic activation Immediate Short-Term Responses to Crises • Mobilize glycogen and lipid reserves to form glucose • Increase mental alertness • Increase energy use by all cells • Change circulation patterns • Reduce digestive activity and urine production • Increase sweat gland secretion • Increase heart rate and respiratory rate © 2013 Pearson Education, Inc. Reninangiotensin system Exhaustion Phase Sympathetic stimulation ACTH Pancreas Adrenal cortex Mineralocorticoids Glucagon Growth (with ADH) Glucocortichormone oids Long-Term Metabolic Adjustments • Mobilize remaining energy reserves: Adipose tissue releases lipids; skeletal muscle releases amino acids • Conserve glucose: Peripheral tissues (except neural) break down lipids to obtain energy • Raise blood glucose concentrations: Liver synthesizes glucose from other carbohydrates, amino acids, and lipids • Conserve salts and water; lose K+ and H+ Factors That Can Trigger the Exhaustion Phase • Exhaustion of lipid reserves and the breakdown of structural proteins as the body’s primary energy source, damaging vital organs • Infections that develop due to suppression of inflammation and the immune response, a secondary effect of the glucocorticoids that are essential to the metabolic activities of the resistance phase • Cardiovascular damage from the ADH and aldosterone- related elevations in blood pressure and blood volume • Inability of the adrenal cortex to continue producing glucocorticoids, which results in a failure to maintain acceptable blood glucose concentrations • Failure to maintain adequate fluid and electrolyte balance Figure 10.11 1 Module 10.11 Review a. List the three phases of the stress response. b. Describe the resistance phase. c. During which phase of the stress response is there a collapse of vital systems? © 2013 Pearson Education, Inc.