* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download PTSD - NDCRC
Spectrum disorder wikipedia , lookup
Depersonalization disorder wikipedia , lookup
History of mental disorders wikipedia , lookup
Abnormal psychology wikipedia , lookup
Substance dependence wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Asperger syndrome wikipedia , lookup
Child psychopathology wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Substance use disorder wikipedia , lookup
Effects of genocide on youth wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
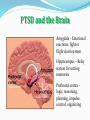
Brian L. Meyer, Ph.D. Interim Associate Chief, Mental Health Clinical Services McGuire VA Medical Center Richmond, VA October 28, 2014 Disclaimer The views expressed in this presentation are solely those of the presenter and do not represent those of the Veterans Health Administration, the Department of Defense, or the United States government. Co-Occurrence of PTSD and Substance Abuse Co-occurring disorders are the rule rather than the exception. (SAMHSA, 2002) PTSD Co-Morbidities Kessler et al., 1995 Co-Occurrence of PTSD and SUDs PTSD and substance abuse co-occur at a high rate 20-40% of people with PTSD also have SUDs (SAMHSA, 2007) 40-60% of people with SUDs have PTSD Substance use disorders are 3 times more prevalent in people with PTSD than those without PTSD The presence of either disorder alone increases the risk for the development of the other The combination results in poorer treatment outcomes Co-Occurring PTSD and SUDs Make Each Other Worse Substance abuse exacerbates PTSD symptoms, including sleep disturbance, nightmares, rage, depression, avoidance, numbing of feelings, social isolation, irritability, hypervigilance, paranoia, and suicidal ideation People who drink or use drugs are at risk for being retraumatized through accidents, injuries, and sexual trauma PTSD and Substance Abuse PTSD/SUD patients have significantly greater impairments Other Axis I disorders Increased psychiatric symptoms Increased inpatient admissions Interpersonal problems Medical problems Decreased motivation for treatment Decreased compliance with aftercare Maltreatment of children Custody battles Homelessness HIV risk Veterans in Prison By 1985, more that 1/5 prison inmates were Veterans (Daily Beast, 7/28/13) By 1988, more than half of all Vietnam Veterans with PTSD had been arrested More than 1/3 had been arrested multiple times (NCPTSD) 1/11 prison inmates are Veterans (DOJ, 2004) This is about 223,000 people 56,000 Veterans are released from state and federal prisons annually, and another 90,000 are released from city and county jails (Noonan, 2010) Veterans and Criminality We do not know how many Veterans of the Iraq and Afghanistan conflicts are in prison because the last Dept. of Justice survey was completed in 2004 The best estimate is 9% (Elbogen et al., 2012) This percentage is likely to rise, since the numbers and percentage of Veterans in prison rises after wars The primary reason Veterans are arrested is substance abuse (Beckerman, et al. 2009; Erickson, et al. 2008) The other major reason is PTSD When irritability and anger are high, 23% of OEF/OIF Veterans with PTSD have been arrested (Elbogen et al., 2012) Trauma and PTSD More men (61%) than women (51%) experience a trauma at some point in their lives, but women experience PTSD at twice the rate of men (10% vs. 5%) (Kessler et al., 1995; Tolin and Foa, 2006) Depending on the study, the type of trauma, and the group studied, 3%-58% get PTSD Therefore, not all trauma leads to PTSD Life-Threatening Events IMPERSONAL PERSONAL TRAUMATIC Who Gets PTSD? It depends on: Genetics Severity Duration Proximity PTSD is mitigated or worsened by: Childhood experience Personality characteristics Family history Social support PTSD and the Brain Amygdala – Emotional reactions, fight or flight alarm system (Overactive) (Underactive) (Smaller volume) Hippocampus – Relay station for sorting memories Prefrontal cortex – logic, reasoning, planning, impulse control, organizing Post-Traumatic Responses Occur on a Continuum Changes to PTSD Diagnosis in DSM 5* Trauma and Stressor-Related Disorders are placed in their own category Loss of loved one must be traumatic or accidental Elimination of B criterion of reaction of horror, terror, or helplessness Military and first responders do their job * Indicates material in packet Changes to PTSD Diagnosis in DSM 5 Addition of new criteria involving negative cognitions (negative beliefs about the world, blame of self or others for the trauma) and mood (depression, anger, guilt) Addition of a new arousal criterion: self-destructive or reckless behavior These changes result in approximately the same number of people who will meet criteria for a diagnosis of PTSD Post-Traumatic Stress Disorder in DSM 5 PTSD is characterized by: Exposure to a severe life-threatening event Repetitive re-experiencing of the event Avoidance of stimuli associated with trauma Negative moods and cognitions Increased arousal PTSD: Exposure to a LifeThreatening Event A. Exposure to a traumatic event Exposure to death, threatened death, actual or threatened serious injury, or actual or threatened sexual violence PTSD: Intrusion Symptoms B. Intrusion symptoms: Recurrent, involuntary and intrusive recollections Traumatic nightmares Dissociative reactions (e.g., flashbacks) Intense or prolonged distress after exposure to traumatic reminders Marked physiological reactivity to traumarelated stimuli PTSD: Avoidance of Stimuli Associated with Traumatic Event C. Persistent effortful Trauma-related avoidance of thoughts and feelings distressing trauma Trauma-related related stimuli after the external reminders event: PTSD: Negative Cognitions and Mood D. Negative alterations in cognitions and mood that began or worsened after the traumatic event: Inability to recall key features of the traumatic event Persistent negative beliefs and expectations about self or world Persistent distorted blame of self or others for causing the event or the resulting consequences PTSD: Negative Cognitions and Mood Persistent negative trauma- related emotions (e.g., fear, horror, anger, guilt, or shame) Markedly diminished interest in significant activities Feeling alienated from others Constricted affect: persistent inability to experience positive emotions PTSD: Increased Arousal and Reactivity E. Trauma-related alterations in arousal and reactivity that began or worsened after the traumatic event: Irritable or aggressive behavior Self-destructive or reckless behavior Hypervigilance Exaggerated startle response Problems in concentration Sleep disturbance PTSD: A New Subtype Dissociative Subtype of PTSD: Meets criteria for a diagnosis of PTSD Experiences high levels of depersonalization or derealization Dissociative symptoms are not related to substance abuse or other medical condition Implications of Changes to PTSD Diagnosis in DSM 5 Angry, depressive, and anxious affects now apply This is a rejoinder to the fear-based model of the past, recognizing greater complexity The existence of a dissociative subtype, combined with the new affective criteria and the new arousal criterion of self-destructive behavior, moves the description closer to that of Complex Trauma Some of the research on PTSD may no longer apply Implications of Changes to PTSD Diagnosis in DSM 5 Assessment instruments must change Different treatments may be needed for different phenotypes of PTSD (anger, depression/guilt, anxiety, dissociation) This may decrease the use of certain treatments, particularly Prolonged Exposure, which is fear-based Inside the Skin of PTSD Nerves on edge Jumpy Can’t sleep Nightmares Irritable all the time Explosive outbursts Wants to be left alone Depressed Can’t stand crowds Heart races/sweats Inside the Skin of PTSD Hates New Year’s Eve and July 4th Secretive Distrusts others Sees world as dangerous Constantly watching for danger Hates lines Overwhelmed by stimulation Feels responsible for trauma Inside the Skin of PTSD Copes by: Cutting off relationships Isolating Taking risks Self-harming behaviors Using drugs and alcohol Faces of PTSD Some Consequences of PTSD Damaged relationships Strain on families Domestic violence Multiple marriages Problems in parenting Children develop problems More Consequences of PTSD Lost productivity Poverty Homelessness Legal problems Reduced quality of life PTSD: A Case Example Mr. V: Vietnam Veteran; many battles; career Marine/Army man; married twice; automobile accident; became agoraphobic; startles easily; doesn’t trust others; nightmares; wife said she’s leaving; dissociated and shot up the house; arrested and jailed PTSD: A Case Example Mr. E: Army; guarded Tomb of the Unknown Soldier; engaged; apartment broken into; tortured; fiancée raped; fear of sleeping at night; triggered by sports games; became hypersexual; seven children by four women; became dependent on PCP; drove while high, arrested, and jailed for nine months PTSD: A Case Example Mr. G: Gulf War Veteran; sent woman out on convoy who was killed; significant guilt; isolated; began drinking and using crack cocaine; arrested and jailed; treated and stopped using crack; got comfortable and started drinking again; dissociated and arrested for drunk driving; jailed for a year Resources for PTSD Handbook of PTSD by Matthew Friedman, Terence Keane, and Patricia Resick Once a Warrior, Always a Warrior: Navigating the Transition from Combat to Home--Including Combat Stress, PTSD, and mTBI by Charles Hoge When Someone You Love Suffers from Posttraumatic Stress: What to Expect and What You Can Do by Claudia Zayfert and Jason Deviva Resources for PTSD National Center for PTSD: www.ptsd.va.gov International Society for Traumatic Stress Studies: www.istss.org International Society for the Study of Trauma and Dissociation: www.isst-d.org PTSD 101 courses: www.ptsd.va.gov/professional/ptsd101/coursemodules.asp Contact: Brian L. Meyer, Ph.D. [email protected]