* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Reactive Attachment Disorder
History of psychiatry wikipedia , lookup
Selective mutism wikipedia , lookup
Autism therapies wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Autism spectrum wikipedia , lookup
Conduct disorder wikipedia , lookup
Conversion disorder wikipedia , lookup
Spectrum disorder wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
Antisocial personality disorder wikipedia , lookup
History of mental disorders wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Maternal deprivation wikipedia , lookup
Abnormal psychology wikipedia , lookup
Asperger syndrome wikipedia , lookup
Attachment theory wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Attachment in adults wikipedia , lookup
Factitious disorder imposed on another wikipedia , lookup
Attachment measures wikipedia , lookup
History of attachment theory wikipedia , lookup
Child psychopathology wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Attachment in children wikipedia , lookup
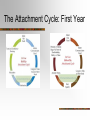
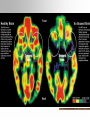
Reactive Attachment Disorder Causes Diagnosis Treatment Basic Trust vs. Mistrust (Erikson) Infants are totally helpless and dependent on parents/caregivers. If needs are met consistently, the child learns to trust others, and the foundation for a secure attachment is laid. If needs are not met consistently, the child becomes fearful and learns not to rely on others. The Attachment Cycle: First Year The Attachment Cycle: 2nd Year The 2nd year attachment cycle cannot be started until the first year secure attachment cycle has been met. Children with insecure attachment do not progress to this 2nd year cycle. www.attachmentdisorder.net. Unhealthy Attachment & the Brain Dr. Allan N. Schore’s 2001 article detailing the effects of traumatic attachment on the development of the right hemisphere changed the way RAD is conceptualized and treated. Traumatic attachment results in periods of “hyperarousal and dissociation,” which interferes with the developing autonomic nervous system & limbic system of the right brain. The structural changes in the brain lead to ineffective stress coping mechanisms in the child. What results is PTSD symptomatology. Early intervention with neurofeedback programs is crucial to altering the process. RAD as a diagnosis First talked about in 1980 as part of DSM- III Considered a controversial diagnosis at the time Some disagreement as to whether it is separate from Ainsworth’s disorganized attachment or basically the same thing. Current thinking is that it is a subcategory of disorganized attachment Disorganized attachment is also considered a risk factor for RAD. Changes from DSM IV to DSM 5 DSM-IV listed RAD as having two subtypes: --Emotionally withdrawn/inhibited --Indiscriminately social/disinhibited DSM 5 turned the two subtypes into separate disorders: --Reactive Attachment Disorder (RAD) --Disinhibited Social Engagement Disorder (DSED) Category placement of RAD/DSED DSM 5 places both disorders in the general category of trauma & stressrelated disorders. Included in this group (besides RAD and DSED) are PTSD Adjustment disorders Acute stress disorder RAD vs. DSED Same etiological pathway for both RAD has dampened positive affect (depressive symptoms) and is more internalized; equivalent to a lack of or improperly formed attachment to caregivers. DSED resembles ADHD more closely. Marked by externalized behavior and disinhibition. Social neglect during childhood is a diagnostic requirement for both conditions, but a child with DSED may have secure attachments. Diagnoses differ in correlates, causes, and responses to intervention and are therefore considered separate disorders in DSM 5. DSM 5 criteria for RAD A. Consistent pattern of inhibited, emotionally withdrawn behavior toward adult caregivers, manifested by both of the following: --Rarely/minimally seeks out comfort when distressed --Rarely/minimally responds to comfort when distressed B. A persistent social & emotional disturbance characterized by at least 2 of the following: --Minimal social & emotional responsiveness to others --Limited positive affect --Episodes of unexplained irritability, sadness, or fearfulness that are evident even during nonthreatening interactions with caregivers DSM Criteria (cont.) C. The child has experienced a pattern of extremes of insufficient care as evidenced by at least 1 of the following: 1. Social neglect or deprivation in the form of persistent lack of having basic emotional needs for comfort, stimulation, and affection by caregiving adults. 2. Repeated changes of primary caregivers that limit opportunities to form stable attachments (e.g., frequent changes in foster care). 3. Rearing in unusual settings that severely limit opportunities to form selective attachments (e.g., institutions with high child-tocaregiver ratios). DSM criteria (cont.) D. The care in Criterion C is presumed to be responsible for the disturbed behavior in Criterion A (e.g., the disturbances in Criterion A began following the lack of adequate care in Criterion C). E. The criteria are not met for autism spectrum disorder. F. The disturbance is evident before age 5. G. The child has a developmental age of at least 9 months. Specifications Specify if: Persistent: The disorder has been present for more than 12 months. Specify current severity: RAD is specified as severe when a child exhibits all symptoms of the disorder, with each symptom manifesting at relatively high levels. Key Diagnostic Features Absent or extremely underdeveloped attachments between the child and caregiving adults. No comfort-seeking behavior or responses to comfort when child is distressed. Diminished or absent positive emotions when interacting with caregivers Evidence that emotional regulation is compromised; negative emotions of fear, sadness, and irritability that are not easily explained. Older vs. Young Children It is unclear whether older children show the same symptoms as younger children do or if the disorder even presents in older children. Diagnosis should be made with caution in children older than age 5. Signs and Symptoms of RAD In Infants Withdrawn, sad, listless appearance Failure to smile Failure to follow others with eyes No interest in interactive games (peek-a-boo) or toys Won’t hold out arms to be picked up Self-soothing behavior Calm when left alone In Toddlers & Children Withdrawing from others Aggressive behavior Avoiding or dismissing comfort Watching others closely but not getting involved Obvious & consistent awkwardness or discomfort Failing to ask for assistance Masking feelings of anger or distress Treatment of RAD No standard treatment Individual and family counseling is typical. Behavior therapy is sometimes used. No pharmacological treatment exists. Neurofeedback is a promising new research & treatment area. Three Crucial Ingredients by Caregivers: Security Stability Sensitivity Beware of “Attachment Therapy” Based on the idea that the child must release pent-up rage in order to become emotionally healthy “Rebirthing”—has been linked to several deaths Holding therapy “Strong sitting” Forced eye contact Craniosacral therapy Some attachment therapists are quick to diagnose RAD based on vague symptoms; they do not follow the DSM’s diagnostic criteria and charge thousands of dollars for their “therapy.” http://www.youtube.com/watch?v=tNoIIwO3uIk BethThomas—original RAD kid (1989) http://www.youtube.com/watch?v=g2-Re_Fl_L4 HBO documentary Child of Rage.