* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Rippon JW. Medical Mycology: The Pathogenic Fungi and
Survey
Document related concepts
Sarcocystis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Orthohantavirus wikipedia , lookup
Tuberculosis wikipedia , lookup
Marburg virus disease wikipedia , lookup
Trichinosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Transcript
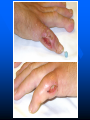
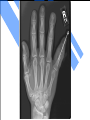
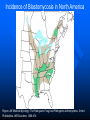
51 y.o. Man with Bilateral Osteomyelitis of the Hands David Feldstein, MD PCC 5/10/06 Patient 51 y.o. man with hx of pulmonary sarcoidosis – Osteomyelitis of bilateral 5th fingers 8 weeks (PTA) – Pain, erythema, swelling right 5th PIP joint – No trauma, injury, fevers chills – Urgent care – clinical dx fracture and splinted Patient 7 weeks (PTA) – Return UC increased swelling and pain – Xray with bony destruction head of 5th proximal phalynx – Ceftri x 1 and started on cephalexin 4 weeks (PTA) – Admitted to outside hospital – Progression of sx right 5th finger – Left 5th finger now with swelling and erythema Patient Outside Hospital – Xray »Almost complete destruction right 5th middle phalynx »Lucency left 5th proximal phalynx – Bone scan »Increased signal bilateral 5th fingers and right wrist Patient Outside Hospital Management – Incision and drainage right 5th finger – Pin placed for stabilization – Gram stain and cx of fluid negative – Vancomycin /Rifampin and discharged No clinical improvement and worsening xrays 3 weeks later Sent to UW (FINALLY!!) Why? Why did he fail treatment? At UW No constitutional sx or other skin findings PMH – Sarcoidosis SH – Machinist, lives on a farm PE – VSS, NAD – Lungs clear – Skin – see photos Objectives Recognize improper treatment of osteomyelitis Describe symptoms of blastomycosis infection Describe treatment of blastomycosis Blastomyces Dermatitidis Dimorphic fungus Mycelial phase in nature Converts to yeast at body temperature Warm moist soil in wooded areas rich in organic debris Endemic – See figure Incidence of Blastomycosis in North America Rippon JW. Medical Mycology: The Pathogenic Fungi and Pathogenic Actinomycetes. 3rd ed. Philadelphia: WB Saunders; 1988:474. Clinical Manifestations Very variable Infection caused by inhalation in almost all cases Most cases include symptomatic pulmonary infection Wisconsin 2 retrospective studies – Centers for Disease Control and Prevention (CDC). Blastomycosis-Wisconsin, 1986-1995. (1996) – Baumgardner DJ. Halsmer SE. Egan G. Symptoms of pulmonary blastomycosis: northern Wisconsin, United States. (2004) CDC All reported cases in WI 1986-1995 – 670 cases – 29 fatal Primary pulmonary disease without extrapulmonary manifestations – 76% Extrapulmonary disease only – 18% Pulmonary and Extrapulmonary – 6% Baumgardner Retrospective investigation of 170 reported cases in Vilas County – 1979-2001 – 91% pulmonary symptoms Pulmonary cases contacted and interviewed (118 of 154) Patients with Pulmonary Blasto Cough 90% Fever 75% Night Sweats 68% Weight Loss 68% Chest Pain 63% Dyspnea 54% Myalgias 50% Hemoptysis 18% Baumgardner, etal. Common Extrapulmonary Sx Skin – Verrucous or ulcerative Bone – Any bone – Xrays not specific GU – Prostatitis and epididymoorchitis CNS – Epidural or cranial abscesses Diagnosis Diagnosis – Histology – Culture »Easy to culture Serology – Not sensitive or specific – 95% cross reactivity with Histo – Also cross-reactive with paracoccidiodomycosis Treatment No good RCTs Guidelines based on small open label studies, case series and expert opinion Ampho for life threatening Itraconazole for mild to moderate At least 6 months IDSA Guidelines Pulmonary – Life threatening – Amphotericin B – Mild/Mod – Itraconazole Disseminated CNS – Ampho B Non-CNS – Life threatening – Ampho B – Mild/Mod - Itraconazole Clinical Follow-up Conclusions Treatment of osteomyelitis – Bone Culture – Reassess when not responding Manifestations of Blasto – Pulmonary most common – Can affect almost any organ Treatment – Ampho or Itraconazole – No good trials of efficacy References Centers for Disease Control and Prevention (CDC). Blastomycosis--Wisconsin, 1986-1995. MMWR - Morbidity & Mortality Weekly Report. 45(28):601-3, 1996 Jul 19. Baumgardner DJ. Halsmer SE. Egan G. Symptoms of pulmonary blastomycosis: northern Wisconsin, United States. Wilderness & Environmental Medicine. 15(4):250-6, 2004. Chapman SW. Bradsher RW Jr. Campbell GD Jr. Pappas PG. Kauffman CA. Practice guidelines for the management of patients with blastomycosis. Infectious Diseases Society of America. Clinical Infectious Diseases. 30(4):679-83, 2000 Apr.