* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Hypertrophic Cardiomyopathy
Remote ischemic conditioning wikipedia , lookup
Heart failure wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Jatene procedure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
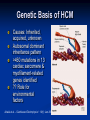
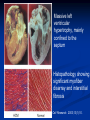
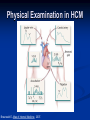
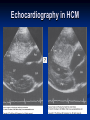
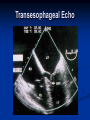
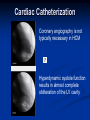
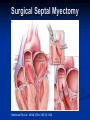
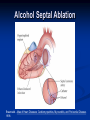
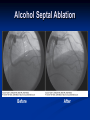
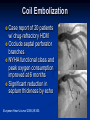
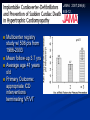
Hypertrophic Cardiomyopathy Learning Objectives Understand the prevalence of hypertrophic cardiomyopathy and the genetic basis for the disease Appreciate the pathophysiology of hypertrophic cardiomyopathy Be able to identify the various clinical presentations of the disease Learn how to diagnose hypertrophic cardiomyopathy using different modalities Understand the typical natural history of the disease Recognize the importance of implantable cardioverter defibrillators in the prevention of sudden cardiac death in this population Appreciate emerging therapeutic strategies and current research Case 17 yo male professional basketball player with no known PMH collapses on the playing floor during practice and subsequently arrests. He had been having some exertional dyspnea for a few months prior to this incident but it did not affect his activity level. He was told growing up that he had a “heart murmur” that was never formally investigated. He was taking no medications, and there was no family history of cardiac disease in his family. An autopsy later revealed that the patient had hypertrophic cardiomyopathy. Background Prevalence of HCM: 1:500 to 1:1000 individuals This occurrence is higher than previously thought, suggesting a large number of affected but undiagnosed people Men and African-Americans affected by almost 2:1 ratio over women and Caucasians Global disease with most cases reported from USA, Canada, Western Europe, Israel, & Asia Historical Perspective HCM was initially described by Teare in 1958 Found massive hypertrophy of ventricular septum in small cohort of young patients who died suddenly Braunwald was the first to diagnose HCM clinically in the 1960s Many names for the disease Idiopathic hypertrophic subaortic stenosis (IHSS) Muscle subaortic stenosis Hypertrophic obstructive cardiomyopathy (HOCM) Genetic Basis of HCM Causes: Inherited, acquired, unknown Autosomal dominant inheritance pattern >450 mutations in 13 cardiac sarcomere & myofilament-related genes identified ?? Role for environmental factors Alcalai et al. J Cardiovasc Electrophysiol. 19(1): Jan 2008. Genetics of HCM Alcalai et al. J Cardiovasc Electrophysiol 2008;19:105. Pathophysiology of HCM The pathophysiology of HCM involves 4 interrelated processes: Left ventricular outflow obstruction Diastolic dysfunction Myocardial ischemia Mitral regurgitation LV Outflow Obstruction in HCM Long-standing LV outflow obstruction is a major determinant for heart failure symptoms and death in HCM patients Subaortic outflow obstruction is caused by systolic anterior motion (SAM) of the mitral valve – leaflets move toward the septum LV Outflow Obstruction in HCM Physiological Consequences of Obstruction Elevated intraventricular pressures Prolongation of ventricular relaxation Increased myocardial wall stress Increased oxygen demand Decrease in forward cardiac output Massive left ventricular hypertrophy, mainly confined to the septum Histopathology showing significant myofiber disarray and interstitial fibrosis Cell Research. 2003;13(1):10. Maron MS et al. NEJM. 2003;348:295. Pathophysiology of HCM Diastolic Dysfunction Contributing factor in 80% of patients Impaired relaxation High systolic contraction load Ventricular contraction/relaxation not uniform Accounts for symptoms of exertional dyspnea Abnormal diastolic filling à increased pulmonary venous pressure Pathophysiology of HCM Myocardial Ischemia Often occurs without atherosclerotic coronary artery disease Postulated mechanisms Abnormally small and partially obliterated intramural coronary arteries as a result of hypertrophy Inadequate number of capillaries for the degree of LV mass Pathophysiology of HCM Mitral Regurgitation Results from the systolic anterior motion of the mitral valve Severity of MR directly proportional to LV outflow obstruction Results in symptoms of dyspnea, orthopnea in HCM patients Integrated Pathophysiology Braunwald. Atlas of Heart Diseases: Cardiomyopathies, Myocarditis, and Pericardial Disease. 1998. Clinical Presentation Dyspnea on exertion (90%), orthopnea, PND Angina (70-80%) Syncope (20%), Presyncope (50%) outflow obstruction worsens with increased contractility during exertional activities Sudden cardiac death HCM is most common cause of SCD in young people, including athletes Physical Examination Carotid Pulse Bifid – short upstroke & prolonged systolic ejection Jugular Venous Pulse a wave – decreased ventricular compliance Prominent Apical Impulse Double or triple Heart Sounds S4 usually present due to hypertrophy Physical Examination Murmur Medium-pitch crescendo-decrescendo systolic murmur along LLSB without radiation Dynamic maneuvers Murmur intensity increases with decreased preload (i.e. Valsalva) Murmur intensity decreases with increased preload (i.e. squatting, hand grip) Physical Examination in HCM Braunwald E. Atlas of Internal Medicine. 2007. Diagnostic Evaluation Electrocardiogram Echocardiogram Catheterization Electrocardiogram in HCM Echocardiography in HCM Transesophageal Echo Cardiac Catheterization Coronary angiography is not typically necessary in HCM Hyperdynamic systole function results in almost complete obliteration of the LV cavity Natural History of HCM Cumulative Survival After Initial Diagnostic Evaluation Among Patients Diagnosed as Having HCM at 20 Years or Older Maron, BJ et al. JAMA 1999;281:650-655 Disease Progression in HCM ACC Consensus Document. J Am Coll Cardiol. 2003;42(9):1693. Sudden Cardiac Death in HCM Most frequent in young adults <30-35 years old Primary VF/VT Tend to die during or just following vigorous physical activity Often is 1st clinical manifestation of disease HCM is most common cause of SCD among young competitive athletes J Am Coll Cardiol. 2003;42(9):1693. SCD in Competitive Athletes Maron B. Atlas of Heart Diseases. 1996 Natural History of HCM Heart Failure Only 10-15% progress to NYHA III-IV Only 3% will become truly end-stage with systolic dysfunction Endocarditis 4-5% of HCM patients Usually mitral valve affected Atrial Fibrillation Prevalent in up to 30% of older patients Dependent on atrial kick – CO decreases by 40% if AF present Autonomic Dysfunction 25% of HCM patients Associated with poor prognosis Influence of Gender & Race Women often remain underdiagnosed and are clinical recognized after they develop 1 more pronounced symptoms HCM clinically underrecognized in AfricanAmericans Most athletes with SCD due to HCM are undiagnosed African-Americans2 1 Olivotto I et al. J Am Coll Cardiol 2005;46:480. 2 Maron BJ et al. J Am Coll Cardiol 2003;41:974. Treatment of HCM Medical therapy Device therapy Surgical septal myectomy Alcohol septal ablation ACC Consensus Document. J Am Coll Cardiol. 2003;42(9):1693. Medical Therapy Beta-blockers Increase ventricular diastolic filling/relaxation Decrease myocardial oxygen consumption Have not been shown to reduce the incidence of SCD Verapamil Augments ventricular diastolic filling/relaxation Disopyramide Used in combination with beta-blocker Negative inotrope Diuretics Dual-Chamber Pacing Proposed benefit: pacing the RV apex will decrease the outflow tract gradient Several RCTs have found that the improvement in subjective measures provided by dual-chamber pacing is likely a placebo effect Objective measures such as exercise capacity and oxygen consumption are not improved No correlation has been found between pacing and reduction of LVOT gradient Surgical Septal Myectomy Nishimura RA et al. NEJM. 2004. 350(13):1320. Alcohol Septal Ablation Braunwald. Atlas of Heart Diseases: Cardiomyopathies, Myocarditis, and Pericardial Disease. 1998. Alcohol Septal Ablation Before After Alcohol Septal Ablation Successful short-term outcomes LVOT gradient reduced from a mean of 60-70 mmHg to <20 mmHg Symptomatic improvements, increased exercise tolerance Long-term data not available yet Complications Complete heart block Large myocardial infarctions No randomized efficacy trials yet for alcohol septal ablation vs. surgical myectomy Circulation. 2008; 18(2): 131-9. Efficacy of Therapeutic Strategies Nishimura et al. NEJM. 2004. 350(13):1323. Coil Embolization Case report of 20 patients w/ drug-refractory HCM Occlude septal perforator branches NYHA functional class and peak oxygen consumption improved at 6 months Significant reduction in septum thickness by echo European Heart Journal 2008;29:350. Implantable Cardioverter Defibrillators in HCM Primary & Secondary Prevention Maron BJ et al. NEJM 2000;342: 365-73. Appropriate discharges in 23% of patients Rate of appropriate discharges of 7% per year Of 21 patients for which intracardiac electrograms were available, 10 shocks for VT, 9 shocks for VF Suggested role for ICDs in primary & secondary prevention of SCD Risk Stratification – ICDs Primary Prevention Risk Factors for SCD Premature HCM-related sudden death in more than 1 relative History of unexplained syncope Multiple or prolonged NSVT on Holter Hypotensive blood pressure response to exercise Massive LVH How many risk factors warrant ICD placement? JAMA. 2007;298(4): 405-12. Multicenter registry study w/ 506 pts from 1986-2003 Mean follow-up 3.7 yrs Average age 41 years old Primary Outcome: appropriate ICD interventions terminating VF/VT JAMA. 2007;298(4): 405-12. J Cardiovasc Electrophysiol 2008;19(10). J Am Coll Cardiol 2008;51(10):103 3-9. 3500 asymptomatic elite athletes (75% male), mean age 20.5 +/- 5.8 years, no family hx of HCM 12-lead ECG, 2D-Echo 53 athletes (1.5%) had LVH 3 athletes (0.08%) had ECG and echo features of HCM HCM vs. Athlete’s Heart Circulation 1995;91. Future Directions Identification of additional causative mutations Risk stratification tools Determining more precise indications for ICDs Defining most appropriate role for alcohol septal ablation ?Gene therapy