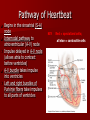
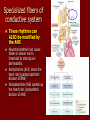
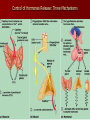
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 23 Comp Review 2
Survey
Document related concepts
Transcript
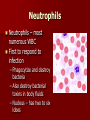
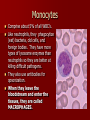
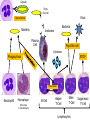
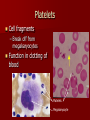
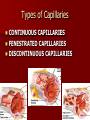
LEUKOCYTES (White blood cells) all fight infection BASOPHILS – MAST CELL EOSINOPHILS NEUTROPHILS MONOCYTES – MACROPHAGES LYMPHOCYTES – B CELLS – T CELLS BASOPHILS Basophils – only about 0.5% of all leukocytes – Granules secrete histamines (vasodilation; more WBCs can get to the infection site) – Antihistamines interfere with the function of basophils. – Mast Cell: a basophil that leaves the blood vessel and enters the tissues. Eosinophils Eosinophils – compose 1-4% of all WBCs – Play roles in: Ending allergic reactions, parasitic infections During these conditions they increase in numbers Neutrophils Neutrophils – most numerous WBC First to respond to infection – Phagocytize and destroy bacteria – Also destroy bacterial toxins in body fluids – Nucleus – has two to six lobes Monocytes Comprise about 5% of all WBC’s. Like neutrophils, they phagocytize (eat) bacteria, old cells, and foreign bodies. They have more types of lysosome enzymes than neutrophils so they are better at killing difficult pathogens. They also use antibodies for opsonization. When they leave the bloodstream and enter the tissues, they are called MACROPHAGES. Lymphocytes 20–45% of WBCs – The most important cells of the immune system – There are two types of lymphocytes; one type is effective in fighting infectious organisms like body cells infected with viruses – Both types of lymphocytes act against a specific foreign molecule (antigen) Lymphocytes Two main classes of lymphocyte – – B cells – Originate in the bone marrow, mature into plasma cells. A mature plasma cell fights infection by producing antibodies T cells – Originate in the thymus gland. They attack foreign cells directly (including organ transplants!). They can also kill viruses. Lymphocytes B cells – mature into plasma cells Plasma cells secrete antibodies; the plasma cell’s antibodies are what kills the attacking cell. Antibodies attack in two ways: – – They attach to bacteria and pop the cell membrane They attach to encapsulated bacteria to help neutrophils and macrophages to phagocytize them. T-cell Lymphocytes T cells are the cells that attack organ transplants! Immunosuppression drugs are designed to inhibit the action of T cells. T cells are attacked by the HIV (AIDS) virus. The thymus gland secrets certain hormones which can cause T cells to become immunocompetent (makes the cells mature and start to work) T Cells There are several types of T cells. The main types are Cytotoxic (Killer) T cells – Go out and directly kill bacteria or infected host cells Helper T cells – Release chemicals called “cytokines” to call in more white blood cells of all types to join in the war. They also present the macrophage’s antigen to a plasma cell, which causes the plasma cell to produce antibodies against that particular bacteria. Suppressor T cells – Stop the immune process when it is over, and also "tell" some plasma cells to "remember" how to destroy that specific pathogen. Those plasma B-cells are then called Memory B-Cells. They can react to the same pathogen faster, the next time it invades because Memory B-cells already have the proper antibodies stored up for that pathogen. Capsule Pops the cell Virus Opsonization Bacteria Bacteria Antibodies Plasma Cell Pops the cell Cytokines Phagocytosis STOP Presentation Neutrophil Macrophage (Monocyte in bloodstream) B-Cell Helper T-Cell Killer T-Cell Lymphocytes Suppressor T-Cell Platelets Cell fragments – Break off from megakaryocytes Function in clotting of blood Platelets Megakaryocyte RBC Development A mature RBC is called an ERYTHROCYTE, which circulates in the blood. If the body makes too few erythrocytes it can lead to one form of ANEMIA. ERYTHROBLASTS These mature into RETICULOCYTES, a RBC with bits of nucleus material, which later dissolves to make room for more Hgb. It is now called an ERYTHROCYTE. Anemia Characteristic sign of anemia: see reticulocytes in the blood (immature red blood cells). Remnants of the nucleus are still in the cell. Disorders of RBCs Polycythemia Anemia – – – – – – Too few RBC’s Iron deficiency Hemorrhagic anemia (person lost blood) Pernicious anemia (lack of vitamin B12 or intrinsic factor) Excess RBC destruction (immune disorder or infection) Hemoglobin abnormalities Thalassemia Sickle cell disease Megaloblastic anemia (pernicious anemia) More Causes of Anemia Hemorrhagic anemia: loss of blood Pernicious anemia: lack of vitamin B12 or intrinsic factor, which is needed to make the hemoglobin in a RBC Excess RBC destruction (from an autoimmune disease, infection, etc) Genetic defect in Hemoglobin (deforms the cell) Thalassemia A form of anemia where the RBCs have abnormal hemoglobin that deforms the cells TEAR DROP TARGET CELLS SPHEROCYTE Sickle Cell Disease Present in African Americans more than in other groups, and is always characterized by sickled erythrocytes. Megaloblastic Anemia (Large RBCs: Note that the lymphocyte is the same size as the huge RBCs) Hematocrit A quick screening test for anemia is the hematocrit. A drop of blood is drawn up a small glass capillary tube and the tube is centrifuged to pack the red blood cells at the bottom with the plasma on top. Hematocrit measures the percentage of blood volume that consists of erythrocytes. The hematocrit is the ratio of packed red blood cells to total blood volume. Normal is about 45% (46% for men and 38% for women.) Disorders of WBCs Disorders of leukocytes – Leukemia – too few mature WBC’s (may see increase in immature forms); a form of cancer – Classified as lymphoblastic (too many immature lymphocytes) or myeloblastic (too many immature neutrophils) Disorders of Platelets – Thrombocytopenia Abnormally low concentration of platelets Blood does not clot properly HEMOPHILIA A hereditary disease of males, where they are unable to clot properly because they are missing some clotting factors. When they get even a slight bump or bruise they have to have an intravenous infusion of clotting factors or they will bleed to death. This is probably the disease that was in the genes of Henry VIII, which caused all of his male children to become weak and die in infancy. Blood Clots Thrombus – A clot in a vessel Embolism – a thrombus that broke away and travels in the blood stream. – It usually lodges in a smaller blood vessel and blocks circulation distal to that point. BLOOD TYPING These proteins are called antigens (something that causes an allergic reaction). There are two types of blood antigens: Type A and Type B. A person with Type A antigens on their blood cells have Type A blood. A person with Type B antigens have Type B blood. A person with both types has type AB blood. A person with neither antigen has type O blood. RH FACTOR The reason this is so important is that if an Rh- mother has an Rh+ fetus in her womb (from an Rh+ father), her antibodies will attack the red blood cells of the fetus because her body detects the Rh protein on the baby’s red blood cells and thinks they are foreign objects. This is called Hemolytic Disease of the Newborn (HDN). IMMUNE SYSTEM INFLAMMATORY REACTION: When you get stuck by a thorn or have an infected cut, the body goes through a series of events called an inflammatory reaction. Four outward signs: – – – – Redness (erythema or rubor) Heat (calor) Swelling (edema) Pain (dolor) ADAPTIVE IMMUNITY Two types of Adaptive Immunity – ACTIVE immunity Naturally Acquired Artificially Acquired You can also think of it this way – PASSIVE immunity Naturally Acquired Artificially Acquired ALLERGIES From a hypersensitivity to substances such as pollen or animal hair that would not ordinarily cause a reaction. There are two types of allergic responses: Immediate Delayed AUTOIMMUNE DISEASE A hereditary problem where the body thinks its own tissues are foreign bodies, and it constantly tries to kill off its own tissues. Tunica intima Endothelium Subendothelium Tunica media Smooth muscles Elastic fibers Tunica adventitia Vasa vasorum Types of Blood Vessels Arteries – carry blood away from the heart – It does not matter if it is oxygenated or deoxy blood. If it is leaving the heart, it is an artery. Capillaries – smallest blood vessels – The site of exchange of molecules between blood and tissue fluid Veins – carry blood toward the heart It does not matter if it is oxygenated or deoxy blood. If it is entering the heart, it is a vein. Arteries ARTERIES carry blood away from the heart. Arteries have a smaller lumen than veins of similar size. Arterial walls are thicker than venous walls. Arteries have more elastin than veins. Arteries have no valves because the blood pressure in arteries is high enough that there is no backflow of blood. ARTERIOLES These are microscopic; they are the smallest type of artery. Large ones look like muscular arteries. Small ones only have two layers: endothelium and tunica media. One of the characteristics of an arteriole is that when it contracts, the lumen closes completely. A sac-like outpouching of an artery – Can rupture at any time; in aorta or brain can cause death within a few seconds. – Symptoms: Swelling or throbbing (asymptomatic in brain) Some common locations for aneurysms include: – Aorta – Brain – Leg – Intestine (mesenteric artery aneurysm) – Splenic artery aneurysm (can form during pregnancy) Aneurysm Aneurysm Causes of an aneurysm: – Defect in part of the artery wall – High blood pressure (abdominal aortic aneurysms) – Congenital (present at birth) Usually not detected except by an angiogram or ultrasound. Treatment: surgical repair Some clinically significant arteries Femoral artery: easy to find pulse, but susceptible to injury. Circle of Willis: loop of arteries around pituitary and optic chiasma. Common area for stroke to cause blindness. Types of Capillaries CONTINUOUS CAPILLARIES FENESTRATED CAPILLARIES DISCONTINUOUS CAPILLARIES PRE-CAPILLARY SPHINCTER A small muscle in front of each capillary, controls the flow of blood to individual capillaries. ARTERIOLES direct the blood flow to the specific tissue. PRE-CAPILLARY SPHINCTERS direct the blood flow to specific cells. If one cell is starving, the capillary next to it will open. The sphincter opens and closes depending on the needs of individual cells. Veins Veins take blood TO the heart. Two types: – Venuole: from the capillary to the vein – Vein: takes blood to the heart. Thinner walls (less pressure here) Larger lumen (blood moves more slowly) Skeletal muscle pushes on the vein to move the blood uphill. Need valves in veins Valves in Veins How does blood get uphill back to the heart? Veins need valves. Veins are the only BLOOD vessels that have valves (although LYMPH vessels also have valves). Valves in veins allow blood to move in only one direction. What pushes the blood? The muscles of the body constrict, squeezing the vessels. This is a type of blood pump. Clinically Significant Veins Greater Saphenous vein: used for coronary bypass; most likely becomes varicose. Facial vein: “Danger triangle” infection spreads to meninges in brain. Renal vein: oxygen poor, and contains the lowest concentration of nitrogen waste. Veins that are rich in oxygen and nutrients Umbilical vein Hepatic Portal vein Pulmonary vein Varicose Veins The valves become incompetent: They can’t close all the way because too much fluid has built up in them and the lumen has stretched too wide. They might be asymptomatic or they may be painful (phlebitis). Edema If the veins are varicose for a long time, plasma may leak out into the tissues, causing edema. Edema means swelling anywhere in the body (including from an injury or from hanging your legs down too long like when on an airplane), but it frequently occurs from incompetent veins in the legs. There are two types of edema: – Pitting – Non-pitting PHLEBITIS Inflammation of a vein Usually in the legs. When phlebitis is associated with the formation of blood clots (thrombosis), usually in the deep veins of the legs, the condition is called Deep Vein Thrombophlebitis (DVT). DEEP VEIN THROMBOPHLEBITIS Signs and Symptoms Redness (erythema) and warmth with a temperature elevation of a degree or more above the baseline Pain or burning along the length of the vein Swelling (edema) Vein being hard, and cordlike Need ER if all symptoms are present Spider Veins Small superficial veins become varicose and do not function properly. Cause an unsightly appearance but are not dangerous. Injections of alcohol or saline into the vein will sclerose them (scar them shut). A laser can also be used to do the same. After treatment, macrophages will eventually phagocytize them and they will disappear. Tissue Necrosis Necrosis = dead Caused by infection, toxins, or trauma Almost always detrimental and can be fatal Peripheral Vascular Disease (PVD) Refers to the obstruction of large arteries, frequently in the lower extremity. Usually caused from atherosclerosis (fatty plaques). Symptoms – Claudication: pain, weakness, numbness, or cramping in muscles due to decreased blood flow – Sores, wounds, or ulcers that heal slowly or not at all – Change in color (blueness or paleness) or temperature (coolness) when compared to the other limb – Diminished hair and nail growth on affected limb and digits (shiny, hairless skin) Lymph System The lymph system retrieves excess tissue fluid (plasma that leaks out of the blood vessels) and filters it and cleans it and returns it to the blood. This plasma is now called lymphatic fluid. It is sent through the lymph nodes throughout the body. There are hundreds of lymph nodes in the body, occurring in clusters. Each lymph node filters the lymph fluid to get rid of bacteria and viruses, and returns the fluid back into the blood. How does lymph move? All of the following mechanisms help move lymph through the lymphatic vessels Body movements during exercise Contraction of skeletal muscles Contractions of smooth muscle in the wall of the lymph vessels. Network of lymph vessels Lymph vessels drain into the right thoracic duct near the clavicle. Lymph Node Figure 20.4a GIANT LYMPH NODES Considered as lymph organs 1. TONSILS and ADENOIDS 2. THYMUS 3. PAYER’S PATCHES 4. APPENDIX 5. SPLEEN Lymph Disorders Hodgkin’s Disease: cancer of lymph node; does NOT feel tender Lymphangitis: inflammation of lymph vessels, usually from infection Mononucleosis: Epstein-Barr virus attacks Blymphocytes; characterized by inflammation of lymph vessels (lymphangitis). Edema: accumulation of fluid in connective tissue Bubo: infected node with trapped pathogens that are not destroyed Layers of tissues around the heart: PERICARDIUM 1) Parietal pericardium 2) Pericardial cavity 3) Visceral pericardium HEART 1) Epicardium (same as visceral pericardium) 2) Myocardium 3) Endocardium Parietal pericardium Visceral pericardium PERICARDITIS Inflamed outer layer of heart. Fluid accumulates in pericardial cavity, putting pressure on heart improper beat Pericarditis can be caused by damage to the blood vessels blood leaks into pericardial cavity pressure improper beat. Pericarditis can lead to pericardial friction rub, adhesions, and additional excess fluid in the pericardial cavity. PERICARDITIS CARDIAC TAPENADE: In severe cases of pericarditis, or if there is a stab wound to the heart wall that causes fluid to exude into the pericardial cavity. The excess fluid compresses the heart and diminishes the heart’s ability to pump. Don’t get this confused with arrhythmia that is caused from a problem with the SA or AV node. The irregular heart beat from cardiac tapenade is caused from fluid entering the pericardial cavity and putting pressure on the heart. Treatment is to stick a needle in the cavity and drain the fluid. ENDOCARDITIS More serious: Bacteria enter bloodstream (dental procedures, IV drug abuse, catheter) damage to lining and valves blood clots. Those who already have damaged heart valves need prophylactic antibiotics. Don’t get endocarditis (bacterial infection) mixed up with pericarditis, which can lead to cardiac tapenade. Blood Flow When the ventricles relax, the PULMONARY SEMILUNAR VALVE closes to prevent blood from going from the pulmonary artery back into the right ventricle. Do the semilunar valves have a chordae tendonae? No; the blood is not being forced back (with a contraction), it just falls back with gravity, so there’s not as much pressure. • Therefore, the left ventricle is the chamber which is responsible for generating the largest pressure upon contraction. SVC IVC RA RV Tricuspid valve Pulmonary artery Pulmonary vein LA LV Pulmonary semilunar valve Bicuspid valve (Mitral) Aorta • The blood then goes past the AORTIC SEMILUNAR VALVE, into the AORTA, and back to the body. The semilunar valves are located between the ventricles and the great arteries. IVC SVC RA RV Tricuspid valve Pulmonary artery Pulmonary vein LA LV Pulmonary semilunar valve Bicuspid valve (Mitral) Aorta Aortic semilunar valve Body SUMMARY OF BLOOD FLOW Deoxy blood sup/inf vena cava R atrium tricuspid valve R ventricle pulmonary semilunar valve pulmonary artery lungs pulmonary veins Left atrium mitral (bicuspid) valve Left ventricle aortic semilunar valve aorta rest of body. Mitral Valve Stenosis • If there is stenosis (blockage) of the mitral valve, where will the blood back up into? • Answer: the pulmonary circulation. SVC IVC RA RV Tricuspid valve Lungs Pulmonary artery Pulmonary vein LA LV Pulmonary semilunar valve Bicuspid valve (Mitral) Aorta Aortic semilunar valve Body HEART BEATS The pressure of blood against blood vessel walls is called blood pressure. Blood pressure is recorded systole over diastole. Normal resting blood pressure is said to be 120/80. When blood pressure is too high, it is called HYPERTENSION. The sound your heart makes when it is beating is the sound of the blood hitting the valves after they are closed. The heart normally beats at a rate of 60-80 beats per minute. A faster (tachycardia) or slower (bradycardia) heart rate is an indication of a problem. HEART BEATS SYSTOLE: – Ventricles contract – Atria relax DIASTOLE: – Ventricles relax – Atria contract Valve Problems HEART MURMUR – If the valve leaks, it doesn’t close all the way – “Lub-squirt” – Most murmurs are benign; fairly common, esp. in babies and some adults. Valve Problems PROLAPSED VALVE is more serious. Mitral valve is most likely to prolapse because it pumped the hardest. See how much thicker the left ventricle is? Mitral Valve Prolapse is the most common heart valve disorder. Might need artificial valve. What controls the heart beat? There is a small region in the right atrium = SA NODE (Sino-atrium node) = pacemaker of the heart. Its job is to speed up or slow down the heart rate as needed. SA node sends an electrical signal (action potential) to the AV NODE (atrio-ventricular node) atrium contraction then the signal pauses while the signal is transmitted to both ventricles (atria are now relaxing) sends the action potential to all parts of the heart so it can contract. Conducting System Heart Beats The heart does not need a nerve to stimulate it to contract; rather, specialized heart cells can spontaneously start an action potential that spreads to depolarize the rest of the cardiac muscle cells. These are the specialized cells: – A. SA node – B. AV node – C. Bundle of His (AV bundle) – D. left and right bundle branches – E. Purkinje fibers Heart Beats This is the order in which these specialized cells function: First the Sinoatrial (SA) node starts an action potential which causes the atria to depolarize. This depolarization will then reach the AV node at the bottom portion of the right atrium and there is a delay here because these cells are so small in diameter. Another delay in the transmission of the depolarization at the bundle of His (AV bundle) because these special heart cells travel through the atrioventricular septum which is non-conductive fibrous connective tissue. The Bundle of His slows down the electrical pathway to give the atria a chance to finish contacting. Next, the depolarizing event travels through the left and right bundle branches, found in the interventricular septum, to finally arrive at the Purkinje fibers in the lateral walls of the myocardium of the ventricles. Problems ARRHYTHMIA Problem with the SA or AV node improper heart beat. Treatment is medicines or a pacemaker. Ventricular Fibrillation FIBRILLATION is when the heart beat is not really present…it just vibrates. A heart in fibrillation does not contract rhythmically; it just quivers without pumping blood. The ventricles are unable to pump blood efficiently due to rapid, random contraction of cardiac muscle fibers. The muscle doesn’t contract as a unit. Treatment is defibrillate with electric shock closes down heart maybe it will restart. Coronary Vessels 1) Right coronary artery The left one is too short to be counted 2) Circumflex artery 3) Anterior Interventricular artery 4) Posterior Interventricular artery The coronary sinus is a collection of veins joined together to form a large vessel that collects blood from the myocardium of the heart and delivers it into the right atrium. THE HEART NEEDS ITS OWN BLOOD/O2 If one of the four coronary arteries becomes clogged, ISCHEMIA (lack of oxygen) to part of the heart muscle will result. This is a painful condition, and the pain of it is called ANGINA (heart pain). If nothing is done immediately to increase the blood flow, the myocardial tissue can die; this condition is called a HEART ATTACK. Coronary Bypass People who have an angina attack can take nitroglycerine as a tablet under the tongue that dissolves quickly. This medicine will dilate the blood vessels. Coronary Bypass When a person has their first angina attack, the doctor will order an ANGIOGRAM to look for a narrowing in an artery, especially in one of the coronary arteries. Coronary Bypass If a coronary artery is found to have a severe blockage, they can do a CORONARY BYPASS. In this procedure, the doctor takes another blood vessel graft (from the greater saphenous vein in the thigh) and sews it in around the blockage. For double or triple bypasses, that’s how many vessels are affected. TERMS ANGINA: heart pain, usually caused from not enough oxygen to the myocardium (ischemia) ISCHEMIA: lack of blood/oxygen MYOCARDIAL INFARCTION: heart attack from blood clot in coronary artery, causing ischemia, which causes angina HEART ATTACK Not enough blood to the heart’s myocardium layer MILD ISCHEMIA severe pain: ANGINA (angina pectoris) – Treatment is nitroglycerine to open arteries Complete blockage not enough O2 to that area = SEVERE ISCHEMIA that part of heart muscle dies = MYOCARDIAL INFARCTION. Heart muscle never regenerates. If a large area dies, person will die. Heart Medicines t-PA (dissolves blood clots) Beta-blockers (slows heart rate) Aspirin (prevents blood clots) Nitroglycerine (dilates coronary arteries) Causes of High Blood Pressure ARTERIOSCLEROSIS (hardening of the arteries): caused by a build-up of calcium deposits in the artery wall; artery cannot expand with blood surges. Tends to be hereditary. The blood vessel becomes hard like a rock; it can’t expand or contract, causes increase in blood pressure. Diet and exercise don’t help this much. Both arteriosclerosis and atherosclerosis cause high blood pressure. Causes of High Blood Pressure ATHEROSCLEROSIS (a build-up of fat in the arteries): caused from eating fatty food narrowing of artery Spasm shut or blood clot. EMBOLISM When fat builds up in a lump in one place, it is called a PLAQUE. It causes the lumen to narrow, restricting blood flow. If this fatty plaque breaks off and travels in the bloodstream, it is now called an EMBOLISM. An embolism can also be made of blood instead of fat. How a thrombus becomes embolism If a platelet catches on a piece of this fat, it can start a blood clot (thrombus). If a piece of the clot (thrombus) breaks off and enters the circulation, it is now called an embolism, it can lodge in a smaller blood vessel and block the oxygen to all the tissue past that point, and the tissue dies. Blockage of blood vessel If the embolism lodges in the coronary arteries myocardial infarct (Heart attack). If the embolism lodges in an artery in the brain stroke If the embolism lodges in the lungs pulmonary embolism ANGIOGRAM An ANGIOGRAM is a procedure to inject dye into the arteries and x-ray to see if there is narrowing (sclerosis) of a vessel. This can be done anywhere in the body that is of interest, but frequently it is done to check the coronary arteries. ANGIOGRAM If an artery is too narrow, an ANGIOPLASTY can be performed to open it up. This involves sticking a balloon into the artery and inflating it, causing the vessel to enlarge a little to increase blood flow. This can be done anywhere in the body, but is frequently done in coronary arteries. CORONARY BYPASS For a coronary artery that has become extremely narrow from plaques, you can do a CORONARY BYPASS. People who exercise have the same number of heart attacks as those who don’t, but they tend to survive them. VENTRICULAR FIBRILLATION Even a small clot can be a problem. If it happens to enter the interior of the heart and lodge in the wall of the atrium, it can block the conduction of the signal of the AV node VENTRICULAR FIBRILLATION. ANEURYSM High blood pressure is due to high pressure of blood against the walls of the blood vessels; the blood vessels compensate by developing a thicker wall. The vessels can no longer expand during systole, so the vessel gets thicker and thicker, and the blood pressure goes up more. If the blood pressure gets too high, an ANEURYSM can form, which is a weakening in the wall of the blood vessel, causing it to expand like a balloon. Coronary artery disease terms Coronary artery disease – Atherosclerosis – fatty deposits – Angina pectoris – chest pain – Myocardial infarction – blocked coronary artery – Silent ischemia – lack of blood flow that happens to not cause any pain or other symptoms; leads to an unexpected heart attack. – Stroke – ruptured blood vessel in the brain. Also called Cerebral Vascular Accident (CVA) Other Heart Conditions Congestive Heart failure – Progressive weakening of the heart – Blood backs up into lungs (may cough up blood) – Cannot meet the body’s demands for oxygenated blood Hypertrophic cardiomyopathy – Congenital condition where the walls of the left ventricle are so thick that the lumen is too small to hold much blood. Disorders of Conduction Ventricular fibrillation – Rapid, random firing of electrical impulses in the ventricles of the AV node Atrial fibrillation – Rapid, random firing of electrical impulses of the SA node Most Common Heart Problems ATHEROSCLEROSIS VENTRICULAR FIBRILLATION Congestive heart failure Hypertrophic cardiomyopathy FORAMEN OVALE The lung tissue needs some oxygenated blood, but only a little. Therefore, there is an opening from the right to the left atrium called the FORAMEN OVALE which shunts blood from the right to the left side of the heart to bypass the lungs. There is a foramen ovale in the skull and another one in the heart. The foramen ovale in the heart normally closes shortly after birth, and is then called the FOSSA OVALIS. A ‘blue baby” has low oxygen levels in the blood that may be due to failure of the foramen ovale to close at birth: Patent foramen ovale. DUCTUS ARTERIOSIS Another shunt: between the pulmonary artery and the aortic arch so that most of the blood bypasses the immature lungs Therefore, there are two shunts to take blood away from the lungs. If the electrical signals from the atria were conducted directly into the ventricles across the AV septum, the ventricles would start to contract at the top (base). Then the blood would be squeezed downward and trapped at the bottom of the ventricle. The apex to base contraction squeezes blood toward the arterial opening at the base of the heart. The AV node also delays the transmission of action potentials slightly, allowing the atria to complete their contraction before the ventricles begin their contraction. This AV nodal delay is accomplished by the naturally slow conduction through the AV node cells. (Why are they slow conductors? Small diameter cells, fewer channels) Fibers within the heart Specialized Fibers – are the fibers that can spontaneously initiate an AP all by themselves! – The AP will spread to all other fibers via gap junctions – AKA “leading cells” – But they are also muscle, so they do contract, albeit feebly! – They are not nerves!!!! Contractile Fibers – These maintain their RMP forever, unless brought to threshold by some other cell – They cannot generate an AP by themselves – AKA “following cells” – But they do have gap junctions, so once they’re triggered, they will help spread the AP to neighbors. Pathway of Heartbeat Begins in the sinoatrial (S-A) node Internodal pathway to atrioventricular (A-V) node Impulse delayed in A-V node (allows atria to contract before ventricles) A-V bundle takes impulse into ventricles Left and right bundles of Purkinje fibers take impulses to all parts of ventricles KEY Red = specialized cells; all else = contractile cells How can these Specialized fibers spontaneously “fire?” Can’t hold stable resting membrane potential Potentials drift (gradual depolarization) During this time, they have a gradually increasing perm to Na+ and less leaky to K+ (more “+” inside causes cell to depolarize, remember?). Only specialized fibers of the heart can depolarize on their own. This is what gives the heart it’s rhythm. Na+ Specialized fibers of conductive system These rhythms can ALSO be modified by the ANS Neurotransmitters can cause faster or slower rise to threshold by altering ion permeability. Acetylcholine (ACh) slows the heart rate (parasympathetic division of ANS) Norepinephrine (NE) speeds up the heart rate (sympathetic division of ANS) K+ efflux Sympathetic and Parasympathetic Sympathetic – speeds heart rate by Ca++ & Na+ channel influx and K+ permeability/efflux (increases sodium and calcium permeability) Parasympathetic – slows rate by K+ efflux & Ca++ influx (decreases sodium and calcium permeability) Which neurotransmitter will cause your heart to pound rapidly? – Norepinephrine Blood Flow (L/min) Blood flow is the quantity of Overall flow in the circulation of an adult is 5 liters/min which is the cardiac output. HR = heart rate SV = stroke volume CO= HR X SV 70 b/min x 70 ml/beat =4900ml/min blood that passes a given point in the circulation in a given period of time. 108 Ventricular Ejection Volume = Stroke Volume Stroke Volume (SV) – amount ejected, ~ 70 ml End Diastolic Volume (EDV) SV/EDV= ejection fraction, – at rest ~ 60% – during vigorous exercise as high as 90% – diseased heart < 50% End-systolic volume: amount left in heart (50ml) Cardiac Output (CO) Amount ejected by a ventricle in 1 minute CO = HR x SV Resting values, 4- 6 L/min Vigorous exercise, 21 L/min Cardiac reserve: difference between maximum and resting CO If resting CO = 6 L/min and after exercise increases to 21 L/min, what is the cardiac reserve? CR = 21 – 6 CR = 15 L/min Volumes and Fraction End diastolic volume = 120 ml End systolic volume = 50 ml Ejection volume (stroke volume) = 70 ml Ejection fraction = 70ml/120ml = 58% (normally 60%) • If heart rate (HR) is 70 beats/minute, what is cardiac output? • Cardiac output = HR * stroke volume = 70/min. * 70 ml = 4900ml/min. • • • • Questions • If EDV = 120 ml and ESV = 50 ml: • What is the SV? • 120-50 = 70 ml • What is the EF? • 70/120 = 58% • What is the CO if HR is 70 bpm? • 70/bpm * 70 ml = 4900ml/min. Ohm’s Law: Q=P/R Flow (Q) through a blood vessel which is the same thing as saying Cardiac Output (CO). It is usually 5. The pressure difference (P) is normally 100. Resistance (R) of the vessel needs to be calculated. Therefore, applying Ohm’s Law (Q=P/R) to a normal person, we get this: 5 = 100/R Solving for R: R = 100/5 R = 20 PRU That means that the normal amount of resistance in the blood vessels is 20 PRU (peripheral resistance units). Overall, the values for a normal person are: 5 = 100/20 Factors Affecting CO Blood viscosity (decreases CO) Total vessel length (longer decreases CO) Vessel diameter (larger increases CO) Regulation of Blood Flow Vasodilators increase blood flow Vasoconstrictors decrease blood flow Vasomotor control: Sympathetic Innervation of Blood Vessels Sympathetic nerve fibers innervate all vessels except capillaries and precapillary sphincters (precapillary sphincters follow local control) Innervation of small arteries and arterioles allow sympathetic nerves to increase vascular resistance. Large veins and the heart are also Figure 18-2; Guyton and Hall sympathetically innervated. 116 Baroreceptors respond to changes in arterial pressure. As blood pressure increases the number of impulses from carotid sinus increases which results in: 1) inhibition of vasoconstricton (so the blood vessels dilate, which lowers blood pressure) 2) activation of the vagal center (lowers blood pressure) As blood pressure decreases the number of impulses from carotid sinus decreases which results in: 1) Increased sympathetic activity (which causes blood vessels to constrict) 2) vasoconstricton (which raises blood pressure) 117 Drugs Affecting CO Atropine- blocks parasympathetic system (increase in sympathetic responses) Pilocarpine- drug that causes skeletal muscle neurons to release ACH, which decreases heart rate. Propranalol- blocks sympathetic effect of heart. This causes decreased heart rate and force of contraction, and lowers blood pressure. Drugs Affecting CO (2) Digoxin (shorter ½ life) or Digitoxin- come from group of drugs derived from digitalis. Digitalis derived from foxglove plant. Slows heart rate but increases force of contraction. Is only drug with this effect on heart. – Disadvantage of using digitalis is that it’s extremely toxic. The optimal dose is very close to lethal dose- stops heart Causes of Edema Excessive accumulation of tissue fluid. Edema may result from: – High arterial blood pressure. – Venous obstruction. – Leakage of plasma proteins into interstitial fluid. – Valve problems – Cardiac failure – Decreased plasma protein. – Obstruction of lymphatic drainage. – Elephantiasis 120 Control of Hormones Release: Three Mechanisms Figure 25.2a-c The Pituitary Gland Secretes nine major hormones Attached to the hypothalamus by the infundibulum Two basic divisions of the pituitary gland – Adenohypophysis (anterior lobe) – Neurohypophysis (posterior lobe) The Adenhypophysis Growth hormone (GH) – Causes the body to grow Prolactin (PRL) – Stimulates lactation (milk production) in females – Produces desire to cry – Decreased in adolescent males so it decreases desire to cry Thyroid Stimulating Hormone (TSH) – Causes the thyroid gland to release thyroid hormone The Adenhypophysis Adrenocorticotropic hormone (ACTH) – Acts on adrenal cortex to stimulate the release of cortisol – Helps people cope with stress Melanocyte-stimulating hormone (MSH) – Darkens skin pigmentation – Increases during pregnancy – Also has effects on appetite and sexual arousal Follicle-stimulating hormone (FSH) – Present in males and females, affects both – Stimulates maturation of sex cells Luteinizing hormone (LH) – Induces ovulation Study Tip to remember the hormones secreted by the pituitary gland “Melons grow and produce through late fall” stands for the hormones made in the anterior pituitary. Melanocyte stimulating hormone (MSH) Growth Hormone (GH) Adrenal corticotropic Hormone (ACTH) Prolactin (stimulates the production of breast milk) Thyroid stimulating hormone (TSH) Luteinizing Hormone (LH) Follicle stimulating Hormone (FSH) 125 The Neurohypophysis This is a continuation of the brain; cell bodies of special neurons in the hypothalamus have axons which go to the neurohypophysis and synapse on capillaries there. Instead of releasing neurotransmitter, they release hormones. Oxytocin – Childbirth contractions Antidiuretic hormone (ADH) – Signals kidneys to increase water reabsorption Figure 25.6 Hypothalamus Regulation The hypothalamus produces hormones which affect the pituitary, for example: Thyroid Stimulating Hormone Releasing Hormone (TSHRH) – Causes adenohypophysis to secrete TSH – TSH affects thyroid gland to secrete TH Thyroid Stimulating Hormone Inhibiting Hormone (TSHIH) – Causes adenohypophysis to stop secreting TSH so thyroid gland stops secreting thyroid hormone The hypothalamus affects the adenohypophysis, and that’s about it. Pituitary Disorders Gigantism and Acromegaly – Hypersecretion of GH in children – Gigantism is overall growth – Acromegaly is enlarged hands and feet Pituitary dwarfism – Hyposecretion of GH – Proportions are normal, overall size is small Diabetes insipidus – Not enough ADH (anti-diuretic hormone; a diuretic takes out excess fluid from the body) The Thyroid Gland Thyroid hormone (TH) – – – – Acts on most cells of the body Increases metabolic rate Controlled by humeral (blood) elements Iodine is needed to make TH Calcitonin – Lowers blood calcium levels in children – Slows osteoclasts to allow for bone deposition (Vitamin D is synthesized and secreted by bone cells) Thyroid Hormone The major stimulus for the release of thyroid hormone is humeral (blood elements tell the body it needs more thyroid hormone). Thyroid hormone is partly made of iodine. Iodine is essential for the formation of thyroxin. If a person doesn’t eat enough iodine, they can’t make thyroid hormone. The hypothalamus responds by putting out more TSHRH. The pituitary will respond by releasing TSH. But the thyroid can’t respond by releasing TH if it does not have the iodine to make the hormone, so it the size of the follicle grows gland grows GOITER. Problems with Thyroid Goiter – Too little iodine in the diet Hyperthyroidism (Graves’ Disease) – Caused by autoimmune disorder – Leads to nervousness, weight loss, sweating, and rapid heart rate Hypothyroidism – Decreases metabolism, causes obesity Hypothyroidism Hashimodo’s Thyroiditis – Antibodies attack and destroy thyroid tissue – Low metabolic rate and weight gain are common symptoms Cretinism – hypothyroidism in children – Short, disproportionate body, thick tongue and mental retardation Parathyroid Glands Parathyroid hormone (PTH) Increases blood concentration of Ca2+ Tells osteoclasts to release calcium from bone Tells kidneys to decrease secretion of calcium Activates vitamin D which increases calcium uptake by intestines Does NOT metabolize calcium THYMUS GLAND Hormones produced by this organ stimulate the production of T cells. The Adrenal Glands Located on the superior surface of the kidneys Two endocrine glands in one – Adrenal cortex – bulk of the adrenal gland – Adrenal medulla – a knot of nervous tissue within the gland The Adrenal Cortex Secretes a variety of hormones; All are steroids CORTISONE reduces inflammation CORTISOL helps the body deal with stressful situations like fasting, anxiety, trauma, and infection. It keeps the blood protein and glucose levels high enough to support the brain’s activities and affects the metabolic rate. When the brain perceives a stressful situation, the hypothalamus tells the pituitary to secrete ACTH, which travels to the adrenal gland and signals it to release cortisol to most of the cells of the body. ALDOSTERONE increases blood volume during hemorrhage or drop in blood pressure. It causes kidney to reabsorb more sodium; water follows with it, so the blood volume increases. SEX HORMONES for the opposite sex: Males produce estrogen here, and females produce testosterone. The Adrenal Medulla Secretes catecholamines: ADRENALIN (AKA epinephrine “above the kidney”; Greek). This is the neurotransmitter for the sympathetic nervous system. The adrenal medulla also has sympathetic neurons which synapse on it, so when you are spooked, the neurons fire and stimulates the adrenal medulla to release more epinephrine to increase the effects of the sympathetic nervous system. Adrenal Gland Disorders Cushing’s syndrome – hypersecretion of cortisol – Round “moon” face and “buffalo hump” Addison’s disease – Hyposecretion of cortisol – Low blood pressure results – Also get hyperpigmentation The Pineal Gland Pinealocytes secrete melatonin – A hormone that regulates circadian rhythms (sense of daytime and night; it regulates sleep cycle) Endocrine Hormones of the Pancreas Glucagon Signals liver to break down glycogen into glucose Raises blood sugar Insulin Signals most body cells to take up glucose from the blood Promotes storage of glucose as glycogen in liver Lowers blood sugar Diabetes DIABETES INSIPIDUS – pituitary gland does not secrete antidiuretic hormone, or the kidney does not respond to the hormone. DIABETES MELLITUS – hereditary lack of insulin secretion in the pancreas, or resistance to insulin by the body’s cells. Type I diabetes (insulin dependent, develops in children) – Destruction of pancreatic islets by autoimmune disorders. – Need insulin injections daily throughout life. Type II diabetes (not insulin dependent, develops in adults) – Consequence of obesity: cells are less sensitive to insulin. – Initially treated with diet and exercise. – Oral medicines or injected insulin may be needed. The Gonads Ovaries – Secrete progesterone Prepares uterus for pregnancy – Secrete estrogen Female secondary characteristics Stores enough for several months Testes – Secrete androgens (e.g. testosterone) Promotes the formation of sperm Maintains secondary sex characteristics Testes are the primary sex organs in the male, NOT the penis This is what happens in the body: Hypothalamus (the boss) makes TSH-RH (thyroid stimulating hormone releasing hormone) Pituitary (the manager) makes TSH (thyroid stimulating hormone) Thyroid gland (the worker) makes TH (thyroid hormone) 143 Thyroid Hormone The hypothalamus releases its hormone (TSH-RH) to the pituitary, telling the pituitary to release its hormone (TSH), which tells the thyroid gland to release thyroid hormone (TH). When thyroid hormone is released, it will circulate throughout the body, causing an increase in metabolism in all of those cells. Some of the TH will bind to receptors in the hypothalamus, and then the hypothalamus knows there is enough TH, and it will stop releasing TSH-RH. Until the receptors in the hypothalamus are bound with the resulting thyroid hormone, the hypothalamus is not satisfied that there is enough thyroid hormone present. 144 What if the hypothalamus released its signal and the thyroid released too much hormone? The hypothalamus will stop secreting its releasing hormone. This is a negative feedback signal. When very few TH receptors are bound on the hypothalamus, it will keep releasing its hormone. When its thyroid receptors are saturated, will stop. 145 What if a gland disobeys the negative feedback? Example: Thyroid gland is impaired by a tumor. A thyroid tumor might cause it to over-secrete or under-secrete TH. Under-secreting thyroid tumor: what happens to the other hormone levels? Start with the problem area (in this case, the thyroid is the place with the tumor), and then evaluate the other glands. (Start with the problem area, the thyroid gland) – TH will be low (hypothyroidism) – TSH-RH will be high, since only a few hypothalamus receptors are bound – TSH levels will be high. Over-secreting thyroid tumor: – TH will be high (hyperthyroidism) – TSH-RH will be low – TSH levels will be low. This combination tells you the source of the problem is the thyroid. 146 Another Example: Pituitary tumor Under-secreting pituitary tumor (Start with the problem area, the pituitary) – TSH is low – TH is low (hypothyroidism) – TSH-RH is high Over-secreting pituitary tumor – TSH is high – TH is high (hyperthyroidism) – TSH-RH is low NOTE: If the problem is the TSH, we don’t bother injecting TSH, we just give the hormone that is lacking: Thyroid hormone. 147 Example: Hypothalamic Tumor Under-secreting hypothalamic tumor (Start with the problem area, the hypothalamus) – TSH-RH is low – TSH is low – TH is low (hypothyroidism) Over-secreting hypothalamic tumor – TSH-RH is high – TSH is high – TH is high (hyperthyroidism) 148 Other Hormone Cycles The adrenal cortex has the same cycle as thyroid hormone; it needs ACTH-RH (adrenocorticotropic releasing hormone), ACTH, CH (cortisol hormone). 149 Hormone Levels Know what would happen to the three hormone levels (TSH-RH, TSH, TH) in the following conditions: Antibodies attacking thyroid gland, destroying the gland Antibodies binding to the TSH receptor, stimulating it Graves’ Disease Hashimoto’s Thyroiditis 150 Regulation of Blood Glucose Levels When blood glucose is high, the pancreas secretes insulin, which tells the cells to take in the sugar from the bloodstream. If the blood sugar levels remain high, the excess sugar is taken to the liver and converted to glycogen for storage. When blood glucose is low, the pancreas secretes glucagon, which tells the liver to take the glycogen and break it back down into glucose and release it into the bloodstream. Gluconeogenesis is when the liver takes fatty acids (leftover from fat metabolism) and joins them to amino acids (from broken down proteins), and makes new glucose molecules that you did not get from eating glucose. These new glucose molecules are then released into the bloodstream to elevate blood glucose levels. Summary: – When blood glucose is high, insulin lowers blood glucose levels. – When blood glucose is low, glucagon causes glycogen breakdown and gluconeogenesis to raise blood glucose levels. 151 Hyperthyroidism (Most commonly caused by Graves Disease) Signs include thinness, eyes that stick out like a bug (exophthalmoses). Graves Disease is a person who has antibodies that bind to thyroid gland, tricks it into making excess TH, while TSH-RH and TSH levels are decreased. You can also get hyperthyroidism from over-secreting thyroid tumors. 152 Disorders of the thyroid-- hyperthyroidism •Graves disease •Tumor (of the hypothalamus, pituitary, or thyroid) Hypothalamus _ TRH + Pituitary Figure 76-8 Patient with exophthalmic hyperthyroidism. Note protrusion of the eyes and retraction of the superior eyelids. The basal metabolic rate was +40. (Courtesy Dr. Leonard Posey.) _ Abs Draw the disrupted pathways! TSH + + Thyroid T3, T4 153 Hypothyroidism This can be caused by Hashimoto’s thyroiditis Iodine deficiency Tumor 154 Cretinism (diminished mental ability) This term describes babies whose MOTHER had the lack of iodine. Baby now cannot get iodine, and the baby will have reduced growth and intellectual ability. Once it is born and gets a healthy diet, it still won’t go back to normal because TH is necessary for proper myelination and synaptic formation. 155 Congenital Hypothyroidism Congenital hypothyroidism is the term for a baby whose thyroid gland is not working correctly (not secreting enough TH). The problem is only with baby, not with the mom. Congenital hypothyroidism and cretin babies have similar symptoms. Child will stay tiny because GH does not work without TH. 156 Hashimoto’s thyroiditis Hashimoto’s thyroiditis is an autoimmune disorder, where antibodies attack and destroy the thyroid gland, and TH goes down while TSH-RH and TSH are elevated. The healthy remaining thyroid tissue will enlarge. Myxedema is non-pitting edema. Touch it, feels solid, and does not leave a fingerprint when you push on it. It is a common symptom in Hashimoto’s thyroiditis. A few people (4%) with Graves’ Disease get myxedema also. People with Hashimoto’s thyroiditis have depressed mental and emotional activity, may have psychosis, not in touch with reality, detached. They gain weight easily, are tired and sleep a lot. 157 The Adrenal Glands Located on the superior surface of the kidneys Two endocrine glands in one (different embryological origin) – ADRENAL MEDULLA – a knot of sympathetic nervous tissue Secretes catecholamines (mostly epinephrine) – Active in “fight, flight, and fright” response – ADRENAL CORTEX – bulk of the adrenal gland Secretes aldosterone (salt and water balance for blood pressure) Secretes androgens and estrogens (sex hormones) Secretes cortisol (anti-stress and anti-inflammation hormone) 158 Adrenal Medulla The adrenal medulla releases catecholamines (epinephrine and norepinephrine). These catecholamines are released when the sympathetic nervous system is activated (“fight or flight”). When you run from a predator, is that when you want insulin to take glucose from blood? No, you want to keep it there so the brain can get the glucose. The brain needs to think of a way to escape, and thinking burns glucose. Therefore, epinephrine is antagonistic to insulin Cells that don’t get the glucose during fight or flight break down fatty acids to get their ATP. These fatty acids will be taken to the liver for gluconeogenesis to elevate the depleted blood glucose levels. Glycogen will also be broken down to glucose to elevate the depleted blood glucose levels. Epinephrine has the same effect as the sympathetic nervous system: – Heart rate and force increases. – Digestion slows – respiratory passages open (bronchiole dilation) – BP goes up (from vasoconstriction in less-needed organs). 159 Adrenal Cortex Secretes a variety of hormones- all are steroids (steroids are made from cholesterol) and are grouped into three main categories: – Mineralocorticoids Aldosterone -Sodium/water reabsorbed – Androgens and Estrogens Male sex hormones (Androgens) Female sex hormones (estrogen) – Glucocorticoids Cortisol – secreted in response to ACTH from the pituitary gland. Cortisol stimulates fat and protein catabolism to use for gluconeogenesis. 160 Adrenal Cortex Hormones Aldosterone Testosterone and Estrogen Cortisol 161 Aldosterone Aldosterone (a mineralocorticoid) targets the cells of kidney, increases the amount of salt and water that is reabsorbed, and that increases blood volume, which elevates blood pressure. 162 How Low BP is Raised When baroreceptors detect low blood pressure, the kidney releases an enzyme called renin, which cuts Angiotensinogen into angiotensin-1 (A1), which travels through blood to the pulmonary capillary bed, where cells have angiotensin converting enzyme that cuts A1 into A2 (the active form). – Any word that ends in –ogen means it is a longer, inactive protein, called a zymogen. – To become activated, they need to be cut by an enzyme into a smaller segment. These high levels of A2 stimulates the adrenal cortex to make more aldosterone, and also stimulates the hypothalamus to release ADH. This will raise the blood pressure. 163 Prednisone, cortisone, cortisol, and aldosterone are all similar in structure. One can be used to make the others. If ACTH is demanding more cortisol, but the body cannot make enough, it may start making androgens instead. 164 Androgens Androgens are called male sex hormones because they cause male secondary sexual characteristics to develop, such as facial hair and low voice. The main androgen secreted by the adrenal gland is called DHEA. DHEA can be converted into testosterone or estrogen. A large amount of testosterone is made in the testes in males. A small amount of testosterone is made in adrenal cortex in males and females. If the adrenal cortex hyper-secretes testosterone and other androgens, it won’t impact a male, because the testes make more than that already. However, in females, hypersecretion causes masculinization (such as facial hair and low voice). 165 Estrogen Estrogens are one of the female sex hormones because they cause female secondary sexual characteristics to develop, such as breasts. A large amount of estrogen is made in the ovaries in females. A small amount of estrogen is made in adrenal cortex in males and females. The androgen, DHEA, can be converted into estrogen. If the adrenal cortex hypersecretes estrogen, it won’t impact a female’s sex characteristics, because the ovaries make more than that already. However, in males, hypersecretion causes feminization (such as breast development). 166 Cortisol: Hormonal Mechanism ACTH-RH is released by the hypothalamus. ACTH is released by pituitary. Cortisol (also called corticotropic hormone or CT). Cortisol affects almost all cells in body. Note: When ACTH plus cholesterol is present, you can take cortisol and turn it into aldosterone if you need to. – It does not do this unless the blood pressure is too low, because aldosterone is under a humeral mechanism (turned on by high blood levels of potassium or A2). 167 Glucocorticoids (cortisol) Glucocorticoids (GC) are a class of steroid hormones that bind to the glucocorticoid receptor (GR), which is present in almost every cell in the body. The name glucocorticoid (glucose + cortex + steroid) derives from their role in the regulation of the metabolism of glucose, their synthesis in the adrenal cortex, and their steroidal structure. They suppress the immune system (they are anti-inflammatory). Cortisol (also known as hydrocortisone) is one of the most important glucocorticoids. Others are prednisone, prednisolone, dexamethasone, and triamcinolone, which are also commonly used medicines for anti-inflammation. 168 Effects of Increased Glucocorticoids Cortisol is called an anti-stress hormone because it does several things: Stimulates protein and fat catabolism (breakdown) – The breakdown products are then taken to the liver for gluconeogenesis in the liver Inhibits glucose uptake by the body but not the brain It elevates blood glucose (diabetogenic effect) It inhibits non essential functions like reproduction and growth It suppresses the immune response – That means it is an anti-inflammatory agent It is prescribed as a medicine to suppress inflammation and the immune system. 169 Cortisol Cortisol (also known as corticosterol and also known as hydrocortisone) The hypothalamus releases ACTH-RH, pituitary releases ACTH, adrenal gland releases cortisol. The adrenal gland also can release androgens. When there is an intense need to make cortisol in response to stress, and if the body cannot keep up with the demand for cortisol, excess ACTH might be shunted into the androgen production pathway, so that androgens are secreted instead of cortisol. Excess androgens do not affect males, but females might develop more masculine features. 170 Prednisone If a person has a lot of cortisol or prednisone in their body, blood sugar levels rise too much, and sugar spills out in the urine. They have symptoms of diabetes, although that is not their disease. You have some cortisol in you now to help maintain normally elevated blood glucose levels between meals, and glucocorticoids stimulate smooth muscle in the vasculature to maintain BP. In high doses only, prednisone may be given for asthma because it suppresses smooth muscle from constricting, and bronchioles cannot close up. What would you predict their natural prednisone hormone levels to be, without the inhaler? high 171 ADDISON’S DISEASE Also called Primary Adrenal Insufficiency and hypoadrenalism; mainly see effects in the hands, fingers, and gums. Addison’s disease may be caused by anything that disturbs the production of adrenal hormones (for some reason, Tuberculosis attacks the adrenal glands as well as the lungs, and can cause hypoadrenalism). In Addison’s disease, the adrenal cortex does not respond to pituitary orders. Cortisol levels are low, but pituitary ACTH and hypothalamus ACTH-RH hormones are high. Symptoms of Addison’s disease are decreased glucose levels, a drop in blood pressure from water and salt imbalance, and darkening of the skin. 172 CUSHING’S DISEASE Excess ACTH caused only by a pituitary tumor. Patient has excess cortisol, high blood pressure, high blood glucose, and too much aldosterone is produced. More salt and water is reabsorbed by the kidney, so the blood volume increases. In this disorder, the hypothalamus (ACTH-RH) levels are low, the other hormone levels (ACTH, cortisol, androgens, and aldosterone) are high. 173 Symptoms of Cushing’s Disease and Cushing’s Syndrome Fat deposition around waist, scapula (buffalo hump), and “moon” shaped face. There is muscle loss and weakness (cortisol tells muscles to break down), thin skin with striae, (High levels of cortisol leads to destruction of collagen, get thin and striae on skin), hyperglycemia, immune suppression. Excessive amounts of adrenal stimulation causes release of male steroids, causing male secondary characteristics, but only in females. Adult onset disease in females causes masculinization, including facial hair, thicker jaw and skull. 174 GROWTH HORMONE (SOMATOTROPIN) GH needs TH to be present. GH stimulates all cells to increase protein synthesis, fat utilization, and gluconeogenesis. Gigantism is the result of excess GH during pre-puberty and acromegaly is the result of excess GH after growth plates closed. The genetic determination of a person’s height has multiple genes involved, so parents might be tall and have smaller children. There are no rules to predict it. A child may also be small due to a defect in the placenta, blocking nutrients during development. 175 PARATHYROID GLANDS There are several of these glands, embedded in the thyroid gland on the posterior surface. The parathyroid glands are the ones that are the most responsible for maintaining blood calcium levels. They accomplish this by releasing parathyroid hormone, which stimulates osteoclasts to chew away bone, releasing the bone’s calcium into the bloodstream. 176 PARATHYROID GLANDS The antagonist of parathyroid hormone is calcitonin, which is produced in the thyroid gland, and stimulates osteoblasts to take calcium from the blood and deposit it in bone. Parathyroid levels are released by a humeral mechanism. If blood calcium levels are low, parathyroid hormone is released. If blood calcium levels are high, parathyroid levels are low. NOTE: Parathyroid glands are do not actually metabolize (use up) calcium. 177 PARATHYROID GLANDS There are three ways that the parathyroid gland raises blood calcium levels Stimulates osteoclasts to move bone calcium into the bloodstream Stimulates the intestines to absorb more calcium from diet Stimulates the kidneys to stop excreting calcium 178 Other Endocrine Glands Many of the glands we talked about have no other function than to make hormones. But almost all organs are endocrine glands in addition to their other functions. Heart pumps blood and produces hormones GI tract digests food and produces hormones. Liver makes enzymes, produces hormones, is involved in calcium metabolism Kidney: excretes wastes, makes hormones, is involved in calcium metabolism and RBC production Dermis Involved in calcium metabolism, vitamin D synthesis – Epithelial glands that have ducts are NOT endocrine glands Lungs oxygenates and produces hormones. Bones synthesize and secrete Vitamin D. Placenta oxygenates and produces hormones. The only thing that does NOT make hormones are epithelial glands that have ducts (hormone glands are by definition without ducts).