* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Heart Failure
Cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Electrocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Rheumatic fever wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
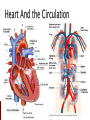
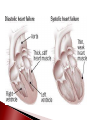
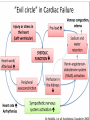
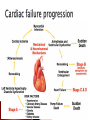
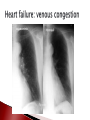
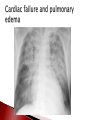
Anna Jaatinen MD Rotary Doctor Bank Finland Ilembula Hospital Heart failure patophysiology and reasons for heart failure Clinical presentation How to treat ◦ Acute cardiac failure ◦ Chronic cardiac failure Patient education Heart failure is a clinical syndrome in which the heart impair its ability to meet the metabolic demands of the body = heart function is not enough to provide blood to the body There is always reason for heart failure! Heart failure is NOT a disease by itself! Prevalence ◦ In Europe and USA 2-3% of adult population, mean age 75 years Leading cause of the hospitalization in people over than 65 years ◦ In developing countries 2-3% of population 20-30 % in people over 70 years Prognosis is poor if not treated ◦ Even when treated 1-year mortality is 30%, and 5year mortality 50% Systolic dysfuntion ◦ Abnormal myocardial contraction Coronary artery disease, dilated cardiomyopathy Diastolic dysfuntion ◦ Abnormal realaxation and filling Hypertension, hypertrofic cardiomyopathy, infiltrative cardiomyopathies, constictive pericarditis Systolic + diastolic dysfuntion Left side cardiac failure Right side cardiac failure ◦ Pulmonary hypertension, pulmonar stenosis, pulmonary embolism Acute Chronic > 80% Coronary artery disease Hypertension Valvular heart disease < 20% Myocarditis ◦ Infectious, Autoimmune Familial cardiomyopathy Infiltrative disease ◦ Amyloidosis, Sarcoidosis ◦ Hemochromatosis Hypertrofic cardiomyopathy Constrictive pericardial disease High-output states; arteriovenous malformation Tacycardia-induced cardiomyopathy Idiopathic cardiomyopathy Toxins; alkohol, cocaine, chemotherapy Heart Myocardial ischemia Hypertension Arrythmias ◦ Atrial fibrillation! Other Infection Volume overload Anemia Alkohol/toxins Thyroid disease Drugs ◦ NSAID! Pulmonary embolism Medication noncompliance Dietary noncompliance ◦ Salt overload, water overload Alcohol Heart failure begins with injury or stress on the heart Remodelling Increase in left ventricular size or/and mass (dilatation or hypertrophy) Stress on the heart, function of the heart Compensatory adaptation Reduction in cardiac output results organ hypoperfusion and pulmonary and systemic venous congestion Symptoms ◦ Dyspnea First on exertion, later also on rest ◦ ◦ ◦ ◦ ◦ ◦ ◦ Exercise intolerance Fatique Ortopnea, paroxyxmal nocturnal dyspnea Cough, wheezing Lower extremity swelling Presyncope, palpitation Angina pectoris (chest pain) can be present Physical examination and findings ◦ ◦ ◦ ◦ ◦ ◦ ◦ ◦ Lower extremity edema Pulmonary cracles Jugular venous distension Diminished carotic upstrokes Pleural and pericardial effusions Hepatic congestion Ascites Third or fourth heart sound may be present as well as holosystolic murmur (tricuspic or mitral regurgitation) Extreme decompensation ◦ Cardiogenic shock ◦ Renal failure, decreased urine output ◦ Confusion, lethargy Laboratories ◦ Reason for heart failure? ◦ Hb (anemia?) ◦ B/S, WBC, Urinalysis if you suspect infection ◦ Also when possible: metabolic panel (electrolytes, creatinine, liver function tests, calcium, fasting glucose), lipid profile, urinalysis, thyroid function tests ◦ If new oncet and clinically suspected: test for HIV, hepatitis, hemochromatosis, rheumatologic diseases Electrocardiogram ECG ◦ Iscemia? Arrhytmias? Conduction delays? Imaging ◦ Chest X-ray Pulmonary edema? Cardiomegaly? Rule out other etiologies of dyspnea (pneumonia, pneumothorax) ◦ Echocardiogram LV funtion and structure? Valvular heart disease? Exclude cardiac tamponade NYHA I No symptoms or limitation while performing ordinary physical activity NYHA II Mild symptoms and slight limitation when performing ordinary physical activity NYHA III Marked limitation in activity due to symptoms, even durin less-than – ordinary activities. Comfortable only at rest. NYHA IV Severe limitations with symptoms even while at rest. Goal: blocking the neurohormonal pathways that contribute to the progression of heart failure ◦ Reducing symptoms ◦ Reducing hospitalization ◦ Reducing mortality Most patients reguire multidrug regimen Treatment shoud be maintained even the clinical status improves! Β-blockers Angiotensin-converting enzyme inhibitors (eg ACEinhibitors) ◦ Carvedilol, bisoprolol, metoprolol, (propranolol, atenolol) ◦ Captopril, enalapril, perindopril, lisinopril…. Vasodilators ◦ Isosorbide mononitrate, Isosorbide dinitrate, Glyceryl trinitrate ◦ Hydralazine Diuretic therapy Digoxin ◦ Furosemide (loop-diuretic) ◦ Thiazide diuretics: Hydrochlorothiazide, chlortialidone ◦ Spironolactone (potassium-sparing diuretic, aldosterone receptor antagonist) (Angiotensin receptore blockers: Valsartan, Candesartan) Spironolactone with ACE-inhibitor: Potential risk for life-threatening hyperkalemia ◦ Renal insufficiency and NSAIDs increase the risk ◦ Serum potasium-level should be monitored Β-blockers are contraindicated patients with ◦ Symptomatic bradycardia or hypotension ◦ Bronchial Asthma Digoxin ◦ Increaces myocardial contractility, may attenate neurohormonal activation of HF ◦ Dose 0.125 to 0.25 mg/day Even lower dose: renal insufficiency, women, elderly, low body weight Narrow therapeutic range! ◦ Drug interactions! Eryhromycin and tetracycline may increase digoxin levels up to 40% Verapamil, flecainide, amiodarone also increace levels Clinical manifestation on CPE can occur rapidly ◦ Dyspnea, anxiety, restlessness, coughing pink foam ◦ Psysical signs: decreased peripheral perfusion, pulmonary congestion, use of accessory respiratory muscels, wheesing ◦ Chest-X-ray: cardiomegaly, interstitial and perihilar vascular engorgement, pleural effusions Radiographic abnormalities may follow the development of symptoms by several hours Cardiac failure and pulmonary edema Acute treatment Supplemental oxygen (Keep oxygen saturation >90%, even >95%) Patient in a sitting position; improves pulmonal function Bed rest, pain control and relief of anxiety can decrease cardiac work load Precipitating factors should be indetificated and corrected ◦ Hypertension? Acute iscemia? Tachyarrythmias? Volume overload? Severe anemia? Infection? Acute Medications Morphine 2-5 mg i.v. (4-8 mg s.c., 5-10 mg p.o.) can be repeated 10-25 min until the effect is seen Furesemide 20 (-80)mg i.v. may be repeated in 10-15 min Nitroglyseride i.v. (or p.o.) if systolic blood pressure is >100 (If rapid arrythmia and possible iscemia consider β-blocker with small dose) Sometimes also fluid-resuscitation is needed when cardiogenic shock and decreased preload Treatment after acute phase Β-blocker, ACE-inhibitor ◦ If patient has the medication before acute oncet pulmonary edema, treatment should not be stopped ◦ When starting as a new medication be careful and start when the condition is stabilized ◦ If myocardial ischemia, start as soon as possible (in 48 h) Treat possible anemia: Blood transfusion if needed (slowly!) In the ward ◦ Monitor BP, pulse, ventilation rate, temperature ◦ Weight every day! Or monitor diuresis and calculate the balance (remember also evaporation) Weight should go down 0.5-1 kg/day ◦ Is breathing easier? Are swellings decreasing? ◦ Physiotherapy after the acute phase if needed ◦ Patient education before going home Medications wich has been shown to reduce morbidity and re-hospitalization ◦ Β-blocker, ACE-inhibitor, Digoxin, spironolactone Medications wich reduce symptoms ◦ Diuretics, Vasodilators (Nitrates+hydralazine) NYHA 1-2: ACE-inhibitor, B-blocker, furosemide (+spironolactone) NYHA 3-4: Add vasodilator, spironolactone, Digoxin Consider anti-thrombotic agents And remember to take care of the cause of the HF, hypertension, diabetes… Explain ◦ What heart failure is and why symptoms occurs ◦ Cause of heart failure ◦ How to recognize symptoms and what to do when they occur ◦ Daily self-weighting and what to do if weight gains Drugs ◦ Encourage to maintain the medication, give information about the dose and effect Dietary treatment and social habit ◦ Control sodium intake, avoid excessive fluid intake (in severe cases limit fluid intake 1-1.5 l/day) ◦ No excessive alcohol, no smoking! Regular exercise within limits of symptoms NSAIDs (also Coxibs): Ibuprofein, Diclofenac Trisyclic anti-depressants: Amitriptylin Some anti-arrythmic drugs: Verapamil Systemic corticosteroids Lithium Nature medications? Heart failure is a sydrome, not a isolated disease! Cause of the heart failure should be considered! Ask and examine: dyspnea, swellings, heart and pulm auskultation, chest-x-ray Treatment is usually multidrug treatment and it should be mantained even the patient is improving Patient education is crucial!