* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Lutembacher's syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Coronary artery disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Atrial fibrillation wikipedia , lookup
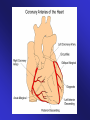
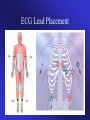
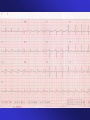
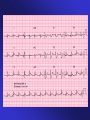
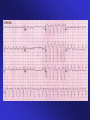
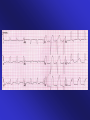
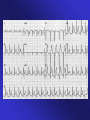
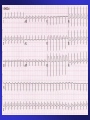
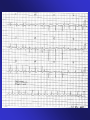
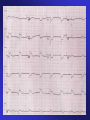
ECGs and Acute Cardiac Events Workshop Dr. Stewart McMorran Consultant in Accident and Emergency MB, BCh, MRCS, FFAEM Objectives • Emergency management of common cardiac events • ST elevation MIs • Tachyarrhythmias • Bradyarrhythmias • Overview of management • Interactive case discussions National Service Framework • NSF for coronary artery disease established 2000 • Relevant to emergency medicine – need for timely reperfusion therapy • Door to needle time of 30 mins • Call to needle time of 60 mins • Results … – 75% eligible patients thrombolysed within 30 minutes of hospital arrival Impact of NSF • Emphasis on timely delivery of reperfusion therapy • Thrombolysis – most places • Percutaneous Coronary Intervention: – Primary – limited availability – Rescue – local policy; if less than 50% resolution in ST segment elevation after 90 minutes • Coronary artery bypass graft Impact on first line services • Timely assessment of chest pain in A&E • Extended skills of paramedics • Availability of Air Ambulances ECG Lead Placement Wall affected Leads Artery involved Reciprocal changes Anterior V2-4 LAD II, III, aVF LAD, circumflex LAD II, III, aVF Anterolateral I, aVL, V3-6 Anteroseptal V1-4 Inferior II, III, aVF RCA I, aVL Lateral I, aVL, V5-6 circumflex II, III, aVF Posterior V7-9 RCA V1-3 Right ventricular RV4-6 RCA Criteria for thrombolysis • Chest pain, onset within last 12 hours plus any of: • ST elevation 2 mm or more in two contiguous chest leads • ST elevation 1 mm or more in two contiguous limb leads • Dominant R wave and ST depression in V1-3 • New LBBB Posterior MI • Dominant R wave chest leads V1-3 • ST depression chest leads V1-3 • Turn ECG upside down and back to front – see typical changes of STEMI • Alternatively … – Posterior leads V7-9 Left Bundle Branch Block and MI • ST segment elevation more than 1 mm concordant (same direction) as QRS complex • ST segment depression more than 1 mm in V1,2,3 • ST segment elevation more than 5 mm discordant (opposite direction) from QRS complex • Sgarbossa E et al. NEJM 1996 Feb 22:334(8) 481-7 Pericarditis • Widespread ST elevation (in leads looking at inflamed epicardium) • Reciprocal depression in aVR and V1 • ST segment saddle shaped (concave upwards) • No Q waves ST segment high take off • Normal variant • High take off or early repolarisation or J point elevation • Younger patients • Usually follows an S wave • T wave maintains independent wave form • No reciprocal ST segment depression • If in doubt, compare with earlier ECGs Arrhythmias - principles of treatment • Choice of intervention - drugs vs. electricity • How symptomatic is patient – How urgent is need for action Choice of intervention • Drugs: – Not always reliable – Side effects – Every anti-arrhythmic is potentially pro-arrhythmic • Electricity: – Reliable – Patient considerations – Environmental considerations How symptomatic is patient • Signs of poor cardiac output – Heart rate • Too fast – depends on rhythm • Too slow – depends on patient – – – – Systolic blood pressure < 90 mm Hg Chest pain Breathlessness Altered level of consciousness • Support ABCs: give oxygen; cannulate a vein • Monitor ECG, BP, SpO2 • Record 12-lead if possible, if not record rhythm strip • Identify and treat reversible causes (e.g. electrolyte abnormalities) Tachycardia Algorithm Is patient stable? Synchronised DC Shock* Up to 3 attempts Unstable Signs of instability include: 1. Reduced conscious level 2. Chest pain 3. Systolic BP < 90 mmHg 4. Heart failure (Rate related symptoms uncommon at less than 150 beats min-1) • Amiodarone 300 mg IV over 10-20 min and repeat shock; followed by: • Amiodarone 900 mg over 24 h Stable Broad Is QRS narrow (< 0.12 sec)? Narrow Narrow QRS Broad QRS Is rhythm regular? Is QRS regular? Irregular Regular Regular Seek expert help Possibilities include: • AF with bundle branch block treat as for narrow complex • Pre-excited AF consider amiodarone • Polymorphic VT (e.g. torsade de pointes - give magnesium 2 g over 10 min) *Attempted electrical cardioversion is always undertaken under sedation or general anaesthesia (with pulse) If Ventricular Tachycardia (or uncertain rhythm): • Amiodarone 300 mg IV over 20-60 min; then 900 mg over 24 h If previously confirmed SVT with bundle branch block: • Give adenosine as for regular narrow complex tachycardia • Use vagal manoeuvres • Adenosine 6 mg rapid IV bolus; if unsuccessful give 12 mg; if unsuccessful give further 12 mg. • Monitor ECG continuously Irregular Irregular Narrow Complex Tachycardia Probable atrial fibrillation Control rate with: • -Blocker IV or digoxin IV If onset < 48 h consider: • Amiodarone 300 mg IV 20-60 min; then 900 mg over 24 h Normal sinus rhythm restored? Yes No Seek expert help Probable re-entry PSVT: • Record 12-lead ECG in sinus rhythm • If recurs, give adenosine again & consider choice of anti-arrhythmic prophylaxis Possible atrial flutter • Control rate (e.g. -Blocker) Example • • • • • • 65 year old male Presents to A&E Palpitations /chest pain MI 3 months ago Sa02 95% on high flow oxygen PR 190 BP 90/70 How do you know it is VT ? • May be difficult to distinguish ventricular tachycardia from atrial tachycardia with aberrant conduction e.g. LBBB • Default position – assume ventricular • Look for confirmatory features: – capture beats – fusion beats – concordance – extreme axis deviation Main learning points • VT is a malignant arrhythmia • DC cardioversion in presence of adverse signs • Check electrolytes especially K+ and Mg2+ • Amiodarone anti-arrhythmic of choice Example • • • • • 25 year old female Presents to A&E Palpitations Sa02 97% on high flow oxygen PR 200 BP 110/70 • Support ABCs: give oxygen; cannulate a vein • Monitor ECG, BP, SpO2 • Record 12-lead if possible, if not record rhythm strip • Identify and treat reversible causes (e.g. electrolyte abnormalities) Tachycardia Algorithm Is patient stable? Synchronised DC Shock* Up to 3 attempts Unstable Signs of instability include: 1. Reduced conscious level 2. Chest pain 3. Systolic BP < 90 mmHg 4. Heart failure (Rate related symptoms uncommon at less than 150 beats min-1) • Amiodarone 300 mg IV over 10-20 min and repeat shock; followed by: • Amiodarone 900 mg over 24 h Stable Broad Is QRS narrow (< 0.12 sec)? Narrow Narrow QRS Broad QRS Is rhythm regular? Is QRS regular? Irregular Regular Regular Seek expert help Possibilities include: • AF with bundle branch block treat as for narrow complex • Pre-excited AF consider amiodarone • Polymorphic VT (e.g. torsade de pointes - give magnesium 2 g over 10 min) *Attempted electrical cardioversion is always undertaken under sedation or general anaesthesia (with pulse) If Ventricular Tachycardia (or uncertain rhythm): • Amiodarone 300 mg IV over 20-60 min; then 900 mg over 24 h If previously confirmed SVT with bundle branch block: • Give adenosine as for regular narrow complex tachycardia • Use vagal manoeuvres • Adenosine 6 mg rapid IV bolus; if unsuccessful give 12 mg; if unsuccessful give further 12 mg. • Monitor ECG continuously Irregular Irregular Narrow Complex Tachycardia Probable atrial fibrillation Control rate with: • -Blocker IV or digoxin IV If onset < 48 h consider: • Amiodarone 300 mg IV 20-60 min; then 900 mg over 24 h Normal sinus rhythm restored? Yes No Seek expert help Probable re-entry PSVT: • Record 12-lead ECG in sinus rhythm • If recurs, give adenosine again & consider choice of anti-arrhythmic prophylaxis Possible atrial flutter • Control rate (e.g. -Blocker) Main learning points • Supraventricular tachycardias are often well tolerated • Usually younger patients • Vagal manoeuvres may be successful • Adenosine is an effective anti-arrhythmic Wolf Parkinson White Wolf Parkinson White syndrome • Uncommon cause of SVT • Presence of accessory pathway (bundle of Kent) • Characteristic ECG features – Short PR interval (<120 ms) – Wide QRS (>120 ms) – Delta wave (slurred upstroke) • Unpredictable response to adenosine Example • • • • • 55 year old man Presents to A&E 1 hour history of central chest pain Sa02 97% on high flow oxygen PR 45 BP 80/50 BRADYCARDIA ALGORITHM (includes rates inappropriately slow for haemodynamic state) Adverse signs? Yes Atropine 500 mcg IV Satisfactory Response? • Systolic BP < 90 mmHg • Heart rate < 40 beats min-1 • Ventricular arrhythmias compromising BP • Heart failure No Yes No Interim measures: • Atropine 500 mcg IV repeat to maximum of 3 mg • Adrenaline 2-10 mcg min-1 • Alternative drugs OR • Transcutaneous pacing Seek expert help Arrange transvenous pacing Risk of asystole? Yes • Recent asystole • Möbitz II AV block • Complete heart block with broad QRS • Ventricular pause > 3s Observe Main learning points • Bradyarrhythmias may complicate inferior myocardial infarction (RCA supplies AVN) • Atropine may be effective • Pacing for symptomatic bradycardias resistant to atropine Example • • • • • 75 year old female Presents to A&E Palpitations Sa02 95% on high flow oxygen PR 175 irreg BP 80/50 Atrial fibrillation Treatment based on risk to patient from the arrhythmia • High risk – Rate > 150 beats min-1 – Chest pain – Critical perfusion • Intermediate risk – Rate 100-150 beats min-1 – Breathlessness – Poor perfusion • Low risk – Rate < 100 beats min-1 – Mild or no symptoms – Good perfusion Main learning points • Management of AF is complex • Universal agreement on high risk patients • Anticoagulation essential to prevent thromboembolic complications Example • • • • • 35 year old male Presents to A&E Palpitations Sa02 97% on high flow oxygen PR 200 BP 110/70 Any Questions? Summary • Chest pain is a common cause of attendance to hospital • Important to recognise STEMI • Arrhythmias may precede or complicate MI • Standardised treatment algorithms for initial management