* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Myocardial infarction wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Jatene procedure wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
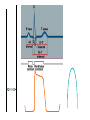
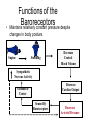
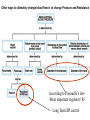
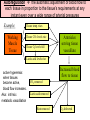
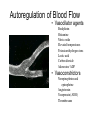
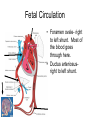
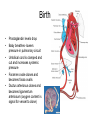
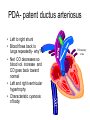
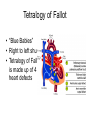
---------------------++++++++++++++++ ++++++++++++++----------------------++++++++++++++-------------------------------------------++++++++++++++++++ • • • • • • • • With a vector, demonstrate the depolarization of the atria. With a vector, demonstrate the repolarization of the atria With a vector, demonstrate the depolarization of the ventricles With a vector, demonstrate the repolarization of the ventricles. What does a vector show? If there is a negative surface charge, what does that mean? If there is a positive surface charge what does that mean? What causes the P, QRS, T wave, exactly? Rhythmical Discharge of Sinus Nodal Fiber Slow Ca++ Channels Open Membrane Potential (mV) Sinus Nodal Fiber K+ Channels Open more +20 Ventricular Muscle fiber Threshold 0 -20 -40 -60 -80 -100 Na+ Leak And less leaky to potassium 0 1 2 Seconds 3 4 Ventricular Muscle Action Potential Fast Na+ close Slow Ca++ Channels open and decreased K+ permeability K+ Channels Open 1 Membrane Potential (mV) +20 2 0 -20 3 -40 -60 -80 -100 Na+ 0 4 Fast Na+ Channels Open 0 1 phase 0- Fast channels open phase 1- Fast Na+ channels close phase 2- slow Ca++ open and decreased K+ permeability phase 3- K+ channels open phase 4- Resting membrane potential Copyright © 2006 by Elsevier, Inc. 2 3 Seconds 4 Sympathetic and Parasympathetic • Sympathetic – speeds heart rate by Ca++ & Na+ channel influx and K+ permeability/efflux • Parasympathetic – slows rate by K+ efflux & Ca++ influx Figure 14-17: Modulation of heart rate by the nervous system Regulators of the Heart: Reflex Controls of Rate Positive or negative chronotropy? K+ efflux Figure 14-28: Reflex control of heart rate Regulators of the Heart: Reflex Controls of Rate • Your HR at any moment is the balance between symp and parasym discharge rates. (“tone”/ reserve) • Tonic discharge • How to speed up? Two ways (faucet analogy) • How to slow down? Two ways • Range: about 50 – near 200 • Typical resting HR: near 70 -SA would normally beat at 80 bpm- but vagal tone slows it down. Parasympathetic slowsdown (20bpm or even stop)• Sympathetic speeds-speed up (230bpm) K+ Drugs Affecting CO • Atropine- parasympathetic blocking (blocks muscarinic AchR) agent, (+,+) • Pilocarpine- drug that causes cholinergic neurons to release ACH. Since Ach decreases heart rate, it causes (-, ) effect on heart. • Propranalol- Reversible, competitive blocker of Beta1 receptor. So blocks sympathetics effect of heart (-,-) Decrease heart rate and force of contraction, and lowers blood pressure. Drugs Affecting CO (2) • Digoxin (shorter ½ life) or Digitoxin- come from group of drugs derived from digitalis. Digitalis derived from foxglove plant. It has a (-,+) effect, neg chronotropic and positive inotropic effect; slows heart rate but increases force of contraction. Is only drug with this effect on heart. – increases intracellular concentration of Ca. – increase force of contraction by inhibiting Na+/K+ pump. So cells start to accumulate Na. – Disadvantage of using digitalis is that it’s extremely toxic. The optimal dose is very close to lethal dose- stops heart Cardiac Cycle (cont’d) 4th Heart sounds are from turbulent blood! Figure 9-5; Guyton & Hall Important things to consider • Cardiac muscle cells have a long absolute refractory period • Twitches can not summate • Tetany not possible (this is good!) • If average heart beats 72bpm; what does the heart do for the rest of the time? • Answer : It “rests” and fills Factors Influencing CO Figure 14-31: Factors that affect cardiac output Arterial PulseCardiac output Systolic Pressure } Pulse Pressure Mean Pressure Peripheral resistance Stroke volume Diastolic Pressure Time HR x SV = CO = MAP/ TPR Arterial compliance Frank-Starling Mechanism • Within physiological limits the heart pumps all the blood that comes to it without excessive damming in the veins. • Length-tension relationship of cardiocytes. • Extra stretch on cardiac myocytes makes actin and myosin filaments interdigitate to a more optimal degree for force generation. Factors that Affect Stroke volume • EDV- dependent on filling time (diastole) and venous return – Skeletal pumping – Respiratory pumping • ESV– Preload- degree of stretching (EDV) • Frank-Starling Principle: more in, more out – Contractility of the ventricle • Availability of calcium; positive and negative inotropy – Afterload- amount of tension ventricle must exert to eject; affected by peripheral vasculature; if greater ESV then there was less stroke volume If a patient has hypertension (MAP greater than 110mmHg) • • • • • What happens to his/her SV? What happens to ESV? What is happening in the arterioles? What would the ventricles have to do? What could happen to the patient’s MEA? Considering the F/S mechanism • • • • • What happens to ejection fraction? What happens to SV? What happens to EDV? What do the ventricles do? What would happen to SV if the F/S mechanism occurs plus increased sympathetic stimulation? • When might the above occur? • Functions of the Baroreceptors Maintains relatively constant pressure despite changes in body posture. Supine Standing Decrease Central Blood Volume Sympathetic Nervous Activity Decrease Cardiac Output Vasomotor Center Sensed By Baroreceptors Decrease Arterial Pressure Baroreceptor activity • If there is an increase in pressure – What will the rate of baroreceptor “firing” be – What will happen to the vasomotor center? – What will happen to the cardioacceleratory center? – What will happen to the cardio-inhibitory center? • If there is a decrease in pressure.... – Answer same above questions. Other ways to ultimately change blood flow is to change Pressure and Resistance Arterial Pressure = Cardiac Output x Total Peripheral Resistance According to Poiseuille’s law-Most important regulator! R4 Long Term BP control Factors of Resistance Poiseuille’s Law = • Blood viscosity • Total vessel length • Vessel diameter • Resistance (length)(viscosity) – (radius)4 Q =_Pr4 8l Blood Pressure Profile in the Circulatory System 20 0 Systemic Pulmonary Circulatory pressure- averages 100mmHg Arterial blood pressure-100-35mmHg Capillary pressure- 35mmHg at beginning and 10-15mmHg at end Venous pressure-15-0mmHg •Large pressure drop across the arteriolar-capillary junction Pulmonary viens Capillaries Large viens 40 Small viens 60 Venules 80 Capillaries Pressure (mmHg) 100 Pulmonary arteries 120 Autoregulation the automatic adjustment of blood flow to each tissue in proportion to the tissue’s requirements at any instant even over a wide range of arterial pressures Example: Working Muscle Tissue Tissue temp. rises Tissue CO2 levels rise Tissue O2 levels fall Arterioles serving tissue vasodilate Lactic acid levels rise active hyperemia: when tissues become active, blood flow increases. Aka: intrinsic metabolic vasodilation Increased blood flow to tissue CO2 removed Lactic acid removed Heat removed O2 delivered Autoregulation of Blood Flow • Vasodilator agents Bradykinin Histamine Nitric oxide Elevated temperatures Potassium/hydrogen ions Lactic acid Carbon dioxide Adenosine/ ADP • Vasoconstrictors Norepinephrine and epinephrine Angiotensin Vasopressin (ADH) Thromboxane Fetal Circulation • Foramen ovale- right to left shunt. Most of the blood goes through here. • Ductus arteriosusright to left shunt. Blood Flow within the Fetal Heart Right atrium Foramen ovale Left atrium (Most of the blood) Right ventricle Pulmonary trunk Pulmonary circuit Left ventricle Ductus arteriosus Aorta Systemic circuit Birth • Prostaglandin levels drop • Baby breathes- lowers pressure in pulmonary circuit • Umbilical cord is clamped and cut and increases systemic pressure • Foramen ovale closes and becomes fossa ovalis • Ductus arteriosus closes and becomes ligamentum arteriosum (oxygen content is signal for vessel to close) PDA- patent ductus arteriosus • Left to right shunt • Blood flows back to lungs repeatedly- why? • Net CO decreases so blood vol. increase and CO goes back toward normal • Left and right ventricular hypertrophy • Characteristic cyanosis of baby Pulmonary veins Tetralogy of Fallot • “Blue Babies” • Right to left shunt • Tetralogy of Fallot is made up of 4 heart defects Determinants of Net Fluid Movement across Capillaries-Starling forces=(Pc + Pif)out - (Pif + Pp)in Figure 16-5; Guyton and Hall • Capillary hydrostatic pressure (Pc)-tends to force fluid outward through the capillary membrane. (30 mmHg arterial; 10mmHg venous- average 17.3mmHg) • Interstitial fluid hydrostatic pressure (Pif)- opposes filtration when value is positive (but it’s not due to lymphatic drainage! – 3mmHg). Determinants of Net Fluid Movement across Capillaries-Starling forces=(Pc + Pif)out - (Pif + Pp)in Figure 16-5; Guyton and Hall • Plasma colloid osmotic pressure ( c)- opposes filtration causing osmosis of water inward through the membrane – Colloid osmotic pressure of the blood plasma. (28mmHg) – 75% from albumin; 25% from globulins • Interstitial fluid colloid pressure ( if) promotes filtration by causing osmosis of fluid outward through the membrane – Colloid osmotic pressure of the interstitial fluid. (8mmHg) – 3gm% Net Starting Forces in Capillaries mmHg Mean forces tending to move fluid outward: Mean Capillary pressure Negative interstitial free fluid pressure Interstitial fluid colloid osmotic pressure TOTAL OUTWARD FORCE 17.3 3.0 8.0 28.3 Mean force tending to move fluid inward: Plasma colloid osmotic pressure TOTAL INWARD FORCE 28.0 28.0 Summation of mean forces: Outward Inward NET OUTWARD FORCE 28.3 28.0 0.3 Net filtration pressure of .3 mmHg which causes a net filtration rate of 2ml/min for entire body (2-4 liters/day!) If capillary BP is greater than capillary OP, there will be net movement of fluid out of the capillary. Capillary BP Filtration Pressure Capillary OP Reabsorption If capillary BP is less than capillary OP, there will be net movement of fluid into the capillary. Arterial end Venous end Distance along the capillary