* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 毒物与吸毒Poisons and drug abuse Department of Forenxic
Survey
Document related concepts
Blood–brain barrier wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Toxicodynamics wikipedia , lookup
Pharmacognosy wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Theralizumab wikipedia , lookup
Urban legends about drugs wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Neuropharmacology wikipedia , lookup
Psychopharmacology wikipedia , lookup
Transcript
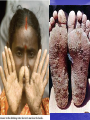
毒物与吸毒 Poisons and drug abuse Department of Forenxic Toxicology SHIZHONG BIAN Intentional Poisoning* Advantages Gender Silent Precise targeting Depersonalized Safe for attacker Male Female Unknown Profile Background Caucasian Male Average or above intelligence Underachiever Personality defect Cowardly, nonconfrontational Nonathletic Neat and orderly, meticulous Careful planner Loner Public Physician Political Nurse Other Unknown 46% 39% 16% 71% 8% 4% 4% 5% 9% *Source: Criminal Poisoning (2000) J. H. Trestrail, Humana Press Properties of Ideal Poison Undetectable by senses Soluble Delayed effect Easily obtained Not traceable Symptoms mimic actual disease Chemically stable (?) Undetectable by instrumentation Potent “The dose makes the poison” Potencies of Poisons Agent Lethal dose Botulinum toxin 0.05 mg Ricin 0.5 mg Strychnine 100 mg Sodium arsenite 200 mg Sodium cyanide 250 mg Thallium 1000 mg NB: A dime is 2300 mg Sources of Poisons Commercial Laboratories Underground catalogs Antique drug collections Hobbies/natural sources (e.g., plants) Pesticide Poisons of Note Synthetic – Organophosphates Carbamates Paraquat Fluroacetate (1080 bait) Plant-derived – Oleander Poison hemlock Mushroom Ricin Atropine/belladonna Nicotine Strychnine Cyanogenic glycosides • 毒物与中毒的概念:某种物质进入机体后,通过化 • • • 学或物理化学作用,使组织细胞结构发生改变、代 谢或功能遭受损害,从而引起健康障碍、疾病或死 亡者,称为中毒。凡在一定剂量时能引起中毒的各 种物质,就称为毒物。 毒物与药物不能机械地划分。 毒物广泛分布于人的周围环境中。 毒物的概念只是相对的,没有在任何条件下都可产 生毒性作用的毒物。食盐一次服用15~60克即有碍 于健康,一次用至200~250克,可因其吸水作用和 所致的离子平衡障碍引起死亡。 • 毒物的分类:毒物的种类繁多,目前尚无 一个完善的分类法。为了法医学鉴定中毒 的需要,在分析中毒症状病理变化时,宜 采用按毒理作用分类;在作法医化学分析 时则采用按毒物的化学性质分类;为追溯 毒物来源,则可采用按毒物用途、来源和 作用混合分类。 • 按毒物的化学性质分类 1.挥发性毒物 氰化物、醇、有机磷农药 2.非挥发性毒物 巴比妥类催眠药、吗啡 3.金属毒物 砷、汞、钡、铬、锌 4.阴离子毒物 强酸、强碱、亚硝酸盐 5.其他毒物 煎毒碱、CO、硫化氢 • 按毒理作用分类 1、腐蚀毒 强酸、强碱、酚类 2、实质毒 砷、汞 3、酶系毒 有机磷、氰化物 4、血液毒 CO、亚硝酸盐及某些蛇毒等 5、神经毒 醇类、麻醉药、催眠药、士的 宁、烟碱等抑制或兴奋中枢神经的药物。 • 混合分类法 1、腐蚀性毒物 2、毁坏性毒物(即实质毒) 3、障碍功能的毒物 4、农药 5、杀鼠剂 敌鼠钠、安妥等 6、有毒植物 乌头、钩吻等 7、有毒动物 蛇毒、河豚、斑蝥等 • 中毒发生的条件 1、毒物的量。中毒量;致死量(g/kg体重) 2、毒物的性状。气态;液态;固态。 3、毒物进入机体的途径。心脏或血管内注射>呼吸 道吸入>腹腔注射>肌肉注射>皮下注射>口服>直肠灌注。 4、毒物的协同作用与拮抗作用。 5、机体状态。体重;年龄;性别;健康状态;习惯性或成 瘾性;过敏性;体内蓄积。 6、其他。 • 毒物的转运、转化及其法医学意义 1、吸收。消化道;呼吸道;皮肤吸收;注 射吸收。 2、分布。毒物在体内的分布并非均匀。 3、代谢。氧化;还原;水解;结合。 4、排泄。肾;胆道;其他(上皮、皮脂腺、 唾液腺、乳腺、消化液)。 中毒的法医学鉴定 • • • • • • • 案情调查 症状分析 现场勘验 尸体检查 检材采取 毒物分析结果的评价 中毒尸体挖掘取材的 价值 Poison plants readily available from nurseries, arboreta, backyards, wild areas Foxglove purpurea Datura digitalis atropine Not visible: Lupine (lupanine) Oleander Autumn Poison Lantana crocus hemlock cardiac colchicine coniine glycosides Ricinus communis (Castor bean) lantadene ricin Top 5 Homicidal Poisons Agent Frequency Target Arsenic 31% Cyanide 9% Strychnine 6% Morphine 3% “ Chloroform 2% “ Energy generation “ Nervous system Analysis Evidence in vicinity of victim Pill bottle, drug paraphernalia Food, beverage leftovers Symptoms Acute Chronic Sampling Organs, fluids Accessory material Detection Analytical instrumentation HPLC, GC, Mass Spec Motivation Love, money, power Disguised as random Poison Symptoms Constricted/dilated pupils (opioids, organophosphates) Breath odor (arsenic – garlic) Hair loss (thallium) Convulsions (strychnine) Paralysis (botulism) Coma (depressants, hypnotics) Skin color (CO – cherry red; nitrites – blue) Skin appearance (arsenic – hyperkeratosis, warts) (dioxin – chloracne) TCDD (dioxin) – Chloracne Poisoning of Victor Yushchenko just before Ukraine presidential election Dioxin (TCDD) Sensitivities Species LD50 (µg/kg) Guinea pig Rat Monkey Human Mouse Rabbit Hamster 2 40 50 ? 130 200 4000 Autopsy samples Organs (brain, liver, kidney, muscle) Blood (heart, peripheral) Vitreous humor Bile (insoluble metabolites) Urine (soluble) Gastric contents (alkaloids) Hair Bone Maggots Environmental/Accidental Contamination Differential diagnosis Accidental death or homicide? Compensable injury or carelessness? Background that could confound interpretation Verify authenticity/natural source or show adulteration How did the mass poisoning occur? Substitution of inferior/contaminated component? Track source of environmental contamination Environmental justice for underserved? Safeguards not enforced Children often victims Which companies are breaking the law? Marine Toxins in Food Pufferfish Delicacy in Japanese restaurants Gives tingling of lips when properly prepared Tetrodotoxin concentrated in liver and ovary (removed) Blocks sodium channel in nerves Fatal in excess (lethal dose 1 mg) Shellfish Tainted by Red Tide (3 examples) Saxitoxin – Paralytic shellfish poison (blocks sodium channel), potentially fatal Domoic acid – Amnesic shellfish poison (glutamate neurotransmitter analog) Disorientation, loss of short term memory at moderate doses Fatal excitotoxin activity at higher doses Okadaic acid – Diarrhetic shellfish poison (phosphatase inhibitor), nonfatal Harmful Algal Blooms Thought increasing due to coastal pollution, ocean warming Of 4,400 known algal species, >1% produce toxins Known causes of wildlife epidemics Marine mammal mortality off California coast from domoic acid Accidental Food Contamination Iraq 1972: 5-6,000 people hospitalized, 10% died. Seed grain donated with methyl mercury antifungal agent. Distributed 100,000 tons to farmers, improperly identified. Grain (wheat, barley) mistakenly used to make bread. Michigan 1973: Nearly 2 million livestock destroyed. Several hundred pounds PBBs mixed with dairy feed. Coverup by company and state officials compounded problem. Spain 1981: 11,000 people hospitalized, >500 died. Industrial rapeseed oil from France containing aniline refined. Refining process produced toxic components. Resold fraudulently as cooking oil (59 tons) after mixing olive oil. Adulturation of vegetable oils (soybean/canola in olive) frequent. Biochemical components becoming available for detection. Commercial Activity - Mercury A woman holds a victim of "Minamata Disease", or mercury poisoning, in Minamata, Japan, in 1973. The girl has a malformed hand, like many victims of the disease who suffer from physical deformities and mental retardation. Chisso Corporation, a Japanese fertilizer, petrochemical and plastics company, dumped an estimated 27 tons of mercury compounds into Minamata Bay between 1932 and 1968. Up to 10,000 people were affected by eating seafood from the bay. Many sources of mercury exist, either natural (fish) or associated with human activity (chloralkali plants, gold mines, effluent from power plants). Elemental form is methylated by micro-organisms in the environment. Commercial Activity - Lead Targets: Blood cells (anemia), kidney (gout), sperm (infertility) Nervous system most sensitive target Adults: Occupational exposures Lead smelters, battery factories, lead additives Painters got peripheral neuropathy (wrist drop) Children: Colic (acute) and mental retardation (chronic) Legacy of leaded paint and gasoline • Eating peeling paint (many inner cities) • Playing in contaminated yards (e.g., Oakland) Commercial activity – Acrylamide Sweden 1997: Hallandsas tunnel construction halted. Acrylamide used in grouting to prevent water seepage. 20 workers experienced neurological symptoms (reversible). Several cows grazing nearby showed severe neural effects. Dead fish found in hatchery supplied by water from tunnel. Acrylamide found in ground water near tunnel. Sensitive methods developed to detect acrylamide showed high background levels in humans. Surprisingly high levels found in fried foods (potato chips). Potential exposures in typical labs using acrylamide gels (including DNA identification labs). Intracellular Targets of Neurotoxins Ion channels – Signal conduction Sodium Potassium Calcium Chloride Synaptic region – Neurotransmitter processing Release Reuptake of excess Receptor response (stimulate, block) Channels and receptors - multigene families Located in different parts of the nervous system Responsible for differential effects Uses of Amphetamines and Derivatives Treatment for narcolepsy - 1930’s Maintaining military alertness - 1940’s Occupational alertness (students, truckers) – 1950’s Appetite suppressant Suppress childhood attention deficit disorder Dietary supplement (ephedrine) as “natural energizer” Opioid Analgesics • • • • • • Background Pharmacokinetics Pharmacodynamics Tolerance and Dependence Side Effects and Toxicity Pharmacotherapy Opioids: Background • Poppy (Papaver • somniferum) Morphine isolated in 1803 (“Morpheus”) – German chemist, Serturner • Codeine isolated by accident in 1830s – French chemist, Robiquet Opioids: Background • Heroin – made from morphine, 1898, Bayer Co. – advertised as having all benefits, none of liabilities of morphine and codeine Opioids: Background • Harrison Narcotics Act • • of 1914 1924, Heroin added Current Use levels: illicit Morphine/Heroin: Pharmacokinetics • Absorption – routes of administration – physical properties: base; poor lipid solubility (except heroin) – peak absorption rapid via IV and inhalation Morphine/Heroin: Pharmacokinetics • Distribution – – – – lungs, liver, spleen blood protein binding pass placental barrier difficulty passing blood/brain barrier – active system pumps opiates out of brain – Heroin is very lipid soluable--exception Morphine/Heroin: Pharmacokinetics • Inactivation – Metabolism • Heroin metabolized to monoacetylmorphine, then to morphine in brain • Morphine metabolized by conjugation; P450 enzymes in liver • Morphine 1/2 life is 2 hours – Elimination • 4 hours 1/2 life Morphine/Heroin: Pharmacodynamics • Cellular sites and mechanism(s) of action – 1973, opioid receptors discovered – Mu, Epsilon, Delta, Kappa – Mu receptors are metabotropic: • activation enhances flow of K+ out of cell and/or decreases activity of voltage-sensitive Ca++ Morphine/Heroin: Pharmacodynamics • Brain sites of action – Medulla – Basal ganglia – Hippocampus – Amygdala – hypothalamus Morphine/Heroin: Pharmacodynamics • Brain sites of action (cont.) – Periaqueductal grey – locus coeruleus – Frontal cortex – Inhibitory interneurons in VTA (GABAr) Morphine/Heroin: Tolerance and Dependence • Tolerance – Fastest to euphoric and analgesic effects • 40-50x non-tolerant dose – Cellular/Pharmacodynamic (not metabolic) • decreased receptor sensitivity Morphine/Heroin: Tolerance and Dependence • Dependence – Withdrawal peaks at 23 days – Naloxone test for dependence – Seldom lifethreatening, “flu-like” – Methadone treatment of withdrawal Morphine/Heroin: Side Effects and Toxicity • Lethality – lowers seizure threshold – tolerance to desired v. lethal effects – life style v. direct effect of drug Morphine/Heroin: Pharmacological Treatment • Methadone • • • maintenance Naltrexone/Naloxone Buprenorphine Rapid detoxification