* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Blood–brain barrier wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Prescription costs wikipedia , lookup
Pharmacognosy wikipedia , lookup
Psychopharmacology wikipedia , lookup
Plateau principle wikipedia , lookup
Intravenous therapy wikipedia , lookup
Drug design wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Drug discovery wikipedia , lookup
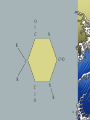
Drug interaction wikipedia , lookup
Neuropharmacology wikipedia , lookup
Theralizumab wikipedia , lookup
Intavenous Anaesthetic Agents Dr.C.N.Chandra Sekhar 1 Intravenous Anaesthetic Agents Induction with IV Anaesthetic agents is smoother and rapid than inhalational agents 2 Intravenous Anaesthetic Agents Properties of the Ideal IV Anaesthetic Agent: Rapid onset – mainly unionized at blood pH - highly lipid soluble Rapid recovery –Rapid redistribution Analgesic at subanaesthetic Concentration Minimal CV and Resp. depression No emetic effects No emergence phenomena No Interaction with NMBD 3 Intravenous Anaesthetic Agents Properties of the Ideal IV Anaesthetic Agent: No pain on injection No venous sequelae Safe if injected inadvertantly into an artery No toxic effects on other organs No release of Histamine No hypersensitivity reactions Water soluble formulation Long shelf-life No stimulation of Porphyrias. 4 Intravenous Anaesthetic Agents Pharmacokinetics of IV Anaesthetic Agents: After IV rapid in plasma conc. slower decline Anaesthesia is produced by diffusion of drug from arterial blood across BBB into the brain 5 Intravenous Anaesthetic Agents Rate of transfer into the brain and anaesthetic effect is regulated by: 1.Protein binding 2.Blood flow to the brain 3.Extracellular pH & pKa of the drug 4.The relative solubilities of the drug in lipid and water 5.Speed of Injection 6 Intravenous Anaesthetic Agents 1.Protein Binding: Only unbound drug is free to cross the BBB Low plasma protein Displacement from proteins by other drugs increase free drug conc. Hyperventilation decreases protein binding and increases anaesthetic effect 7 Intravenous Anaesthetic Agents 2.Blood Flow to the Brain: Reduced blood flow reduced delivery of the drug. If CBF is decreased due to low Cardiac output---initial blood conc. Higher than N, i.e Anaesthetic effect may be delayed but enhanced. 8 Intravenous Anaesthetic Agents 3.Extracellular pH & pKa of the drug: Only non-ionized fraction of the drug penetrates the lipid BBB The potency of the drug depends on the degree of ionization at the pH of extracellular fluid & pKa of the drug. 9 Intravenous Anaesthetic Agents 4.The relative solubilities of the drug in lipid and Water: High lipid solubility enhances transfer into brain. 5.Speed of Injection: Rapid IV adminstration high initial conc. increases speed of induction and extent of CV and Resp.side effects 10 Pool Lean % of Dose Viscera Fat 0.06 0.125 025 0.5 1 2 4 8 16 32 11 128 mts Classification of Intravenous Anaesthetics Rapidly acting agents: Barbiturates Methohexital Thiobarbiturates- thiopental, thiamylal Imidazole compounds: eg.etomidate Sterically hindered alkyl phenols: eg. Propofol Steroids: eg. Eltanalone, Althesin, Minaxolone Eugenol: eg. Propanidid 12 Classification of Intravenous Anaesthetics Slower- acting agents: Ketamine Benzodiazepines:- Diazepam, flunitrazepam, midazolam Large-dose opioids:- Fentanyl, Alfentanil, Sufentanil, remifentanil Neurolept combinations:- Opioid + Neuroleptic 13 O ‖ C N R C=O C R C ‖ O N R 14 Thiopental Sodium Chemical Structure:Sodium 5-ethyl – 5(1-methylbutyl) – 2 thiobarbiturate Physical properties & Presentation:Sulphur analogue of pentobarbital Taste = bitter Colour = yellowish State = powder Smell = garlic 15 Thiopental Stored in Nitrogen to prevent chemical reaction with atmospheric CO2 6% anhydrous sodium carbonate to increase solubility in water 2.5% solution pH : 10.8 Solution is hypotonic Prepared solution can be kept for 24 hrs. Oil/water partition coefficient 4.7 pKa is 7.6 16 Thiopental Central Nervous System:Onset <30sec after IV injection delayed if CO is low Progressive depression of CNS and spinal cord reflexes Hypnotic action – potent Analgesic effect – poor CMR CBF CBV ICP 17 Thiopental - CNS Recovery of consciousness occurs at high blood concentrations if a large dose is given or if the drug is injected rapidly (acute tolerance) Consciousness regained in 5-10mts. At subanaesthetic conc. Antanalgesic effect Reduces pain threshold Potent anticonvulsant Sympathetic effect depressed more than parasympathetic. Tachycardia 18 Thiopentone Cardiovascular System:Myocardial contractility depressed Peripheral vasodilation Hypotension HR 19 Thiopentone Respiratory System:Ventilatory drive In spont.Vent. Vf & Vt in bronchial muscle tone Laryngospasm 20 Thiopentone Skeletal muscle: tone at high blood concentrations No direct effect on NMJ Uterus & Placenta:Contractions suppressed at high doses Crosses the placenta rapidly Foetal blood conc. Not reach upto mother’s Eye:IOP by 40% Pupils = dilates first and then constricts Light reflex present until surgical anaesthesia is reached Corneal,conjunctival,eyelash and eyelid reflexes21 Thiopentone Hepatorenal Function:Transient impairement of liver and kidney functions. Hepatic microsomal enzymes are induced metabolism & elimination of other drugs. 22 Thiopentone Pharmacokinetics:75-85% drug is protein bound (mostly albumin) Protein binding affected by pH I.e by alkalemia Conc. Of free drug in hyperventilation Diffuses readily into CNS because of high lipid solubility. Predominantly unionized (61%) at body pH Consciousness returns when the brain concentration returns to a threshold value( vary from patient to patient) 23 Thiopentone Pharmacokinetics:- (contd….) Metabolism occurs in Liver Metabolites excreted in Urine Terminal elimination half-life 11.5 hrs. Metabolism is a Zero order process 30% of original drug remain after 24 hrs. Hangover effect common Elimination impaired in elderly In obese dose should be based on lean body mass as distribution to fat is slow. 24 Thiopentone Dosage & adminstration:Adminstered as 2.5% solution Initially 1-2 ml injected Healthy adults: 4 mg/kg administered over 15-20 sec. Loss of eye reflex within 30sec Supplementary dose 50-100mg slowly Children 6 mg/kg Elderly patients 2.5 – 3 mg/kg Induction smooth, preceded by the taste of garlic No other drugs should be mixed with Thiopentone 25 Thiopentone Adverse Effects:Hypotension Respiratory depression Tissue necrosis Intra-arterial injection Laryngospasm Bronchospasm Allergic reactions Thombophlebitis 26 Thiopentone Indications:Induction of Anaesthesia Maintenance of Anaestheisa Treatment of Status epilepticus Reduce intracranial pressure 27 Thiopentone Absolute Contraindications: Airway Obstruction Porphyria Hypersensitivity reaction to Baribiturates 28 Thiopentone Precautions:Cardiovascular disease Severe hepatic disease Renal disease Muscle disease Reduced metabolic rate Obstetrics Outpatient anaesthesia Adrenocortical insufficiency Extremes of age asthma 29 Thiopentone 30 Propofol Indications: For induction and Maintenance of General anaesthesia Sedation in Intensive Care Unit and during Regional anaesthesia techniques For treatment of refractory nausea and vomiting in patients receiving chemotherapy Treatment of status epilepticus 31 Propofol Mode of Action:- transmitters and GABA Unclear. Potentiates the inhibitory glycine 32 Propofol Routes of Adminstration and Dose: Intravenous bolus dose 1.5 – 2.5 mg/kg for induction Maintenance 4-12mg/kg/hour For children induction dose should be increased by 50% and Manintenance infusion by 25-50% 33 Propofol Consciousness lost in 30 sec. Recovery about 10mts after a single dose Plasma concentration of 2-6mcg/ml associated with hypnosis. Plasma conc. of 0.5 – 1.5 mcg/ml associated with sedation. 34 Propofol- pharmacodynamics CVS: - -15-25% drop in Blood pressure and SVR without comp. Increase in HR -20% decrease in Cardiac output -attenuates laryngoscopic response -Vasodilatation due to NO release 35 Propofol- pharmacodynamics Respiratory System: Apnea for variable duration Decreased laryngeal reflexes Infusion decreases the TV and RR Depresses ventilatory response to CO2 Bronchodilatation due to direct effect Preserves the mechanism of hypoxic pulm.vaso constriction 36 Propofol- pharmacodynamics Central Nervous System:Smooth,rapid induction with rapid and clear headed recovery Intracranial pressure,cerebral perfusion pressure, cerebral oxygen consumption reduced GIT:Propofol has got intrinsic antiemetic properties, mediated by antagonism of dopamine D2 receptors. 37 Propofol- Pharmacodynamics Renal:Causes reduction in excretion of Na+ ions Metabolic:Longterm use causes hypertriglyceridemia 38 Propofol Toxicity and side effects:Pain on injection seen in 28% subjects Epileptiform movements Facial parasthesias Bradycardia Neurological sequelae in children after longterm use of propofol for sedation Quinol metabolites give green colour to urine 39 Propofol-Pharmacokinetics Distribution:97% protein bound in plasma VD is 700 – 1500 L Distribution half-life is 1.3 – 4.1minutes. Metabolism:Rapidly metabolised in the liver Primarily to inactive glucuronide and sulphate conjugates and the corresponding quinol. Renal and hepatic disease have no significant effect on the metabolism. 40 Propofol Chemical:- 2,6 – diisopropylphenol Presentation:- White oil in water emulsion containing 1 to 2% propofol in soyabean oil and purified egg phosphatide Main Action:- Hypnotic 41 Ketamine Hydrochloride 1965 Phencyclidine derivative Dissociative anaesthesia Chemical structure:2(o-chlorophenyl)-2(methylamino)cyclohexanone hydrochloride 42 Ketamine Physical characteristics & presentation:Soluble in water 1% with NaCl for istonicity 5 & 10% with benzothonium chloride 0.1mg/kg as preservative pH of the solution 3.5 – 5.5 pKa of Ketamine 7.5 43 Ketamine Central Nervous System:Extremely lipid soluble After IV Onset: 30-60 sec Duration: 10-15 min After IM Onset: 3-4 mts. Duration: 15-25mts Potent analgesic at subanaesthetic doses 44 Ketamine Central Nervous System:- (contd…) Amnesia persists 1 hr. after recovery of consciousness Induction smooth Emergence delirium,restlessness,disorientation & agitation EEG changes – loss of alpha activity & predominant theta activity CMR CBF CBV ICP 45 Ketamine Cardiovascular System:Arterial pressure by 25% HR by 20% CO may increase Myocardial O2 consumption Myocardial sensitivity to Epinephrine Vasodilatation in tissues innervated by -adrenergic receptors & vasoconstriction in those with receptors 46 Ketamine Respiratory System:Transient apnoea Pharyngeal & laryngeal reflexes, patent airway maintained Bronchial muscle is dilated 47 Ketamine Skeletal Muscle:Muscle tone GI system:Salivation is increased Uterus & Placenta:Crosses placenta readily Eye:IOP 48 Ketamine Pharmacokinetics:12% is bound to protein Initial peak conc.after IV injection decreases after drug distributes Metabolism is by liver demethylation & hydroxylation of cyclohexanone ring (norketamine is the active metabolite) 80% of injected drug excreted as glucuronides 49 Ketamine Pharmacokinetics:- contd…… 2.5% excreted unchanged in urine Elimination half-life 2.5hrs. Peak conc. Achieved after 20 mts. After IM inj. 50 Ketamine Dosage & administration:Induction of Anaesthesia:2mg/kg IV, 1-1.5mg/kg required every 5-10mts. 8-10mg/kg IM. 0.25-0.5mg/kg or 50g/kg/min infusion for analgesia without loss of consciousness 51 Ketamine Adverse effects: Emergence delirium,nightmares & hallucinations Hypertension & tachycardia Prolonged recovery Increased salivation Increased ICP Allergic reactions 52 Ketamine Indications:High risk patients:- (shocked patients) Paediatric anaesthesia Difficult locations Analgesia & sedation Developing countries 53 Ketamine Absolute contraindications:Airway obstruction Raised ICP Precautions:Cardiovascular diseases Repeated administration Visceral stimulation Outpatient anaesthesia (not suitable for adults) 54 Total Intravenous Anaesthesia Indications: Rapid recovery and minimal hangover Minimal cardiovascular depression To deliver High oxygen concentration To avoid nitrous oxide 55 Methohexital Sodium Chemical Structure:Sodium-α-dl-5-allyl-1-methyl-5(1-methyl-2pentynyl) barbiturate Physical Properties & Presentation:Two asymmetrical carbon atoms White powder Mixed with 6% anhydrous Na2CO3 1% solution pH 11.1 , pKa 7.9 Single dose vial 100mg & multidose vials.5&2.5gm. Stable in solution for about 6 wks.(allowed only 56 24hrs) Methohexital Sodium Pharmacodynamics:Central Nervous System:Induction 15-30sec. Recovery more rapid than thio (2-3mts.) Drowsiness persists for several hours Epileptiform activity in EEG seen in epileptic patients. In sufficient doses acts as anticonvulsant 57 Mthohexital Sodium CVS:Hypotension less than thio HR increases RESP:Moderate hypoventilation Pharmacokinetics:More is unionized at body pH( 75%) than thio Elmination half life is shorter( appx. 4hrs) 58 Methohexital Sodium Dose & Administration:1- 1.5mg/kg Adverse effects:CVS and Resp. depression Excitatory phenomena during induction Epileptiform activity Pain on injection Tissue damage Intraarterial injection Allergic reaction Thrombophlebitis 59 Etomidate Chemical Structure:D-Ethyl-1-(α-methylbenzyl)-imidazole-5-carboxylate Physical characteristics and presentation:Soluble but unstable in water Contains 35% propylene glycol 10ml ampoule contains 20mg pH is 8.1 60 Etomidate Pharmacology:Rapidly acting Duration of action 2-3 mts. Less cardiovascular depression Large doses may produce tachycardia Respiratory depression is less Impairs synthesis of cortisol from adrenal gland. Longterm infusion in ICU leads to increased infection and Mortality. 61 Etomidate Pharmacodynamics:76% bound to protein Metabolised in liver mainly by esterase hydrolysis Terminal elimination half life 75mts. 62 Etomidate Dose & administration:0.3mg/kg Adverse effects:Suppression of synthesis of cortisol Excitatory phenomenon Pain on injection Nausea and vomiting Emergence phenomena Venous thrombosis 63 Incidence of Adverse reactions: Thiopentone Methohexital Althesin Propanidid Etomidate Propofol : 1:14000-1:20000 : 1:1600- 1:7000 : 1:400- 1:11000 : 1:500- 1:1700 :1: 450000 :1:50000- 100000 64