* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download let`s see if you can swallow this…
Surgical management of fecal incontinence wikipedia , lookup
Liver cancer wikipedia , lookup
Schistosomiasis wikipedia , lookup
Ascending cholangitis wikipedia , lookup
Fecal incontinence wikipedia , lookup
Bariatric surgery wikipedia , lookup
Colonoscopy wikipedia , lookup
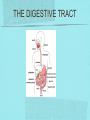
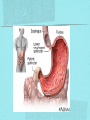
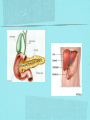
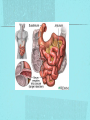
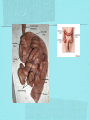
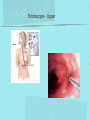
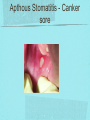
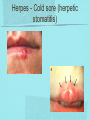
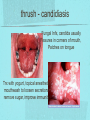
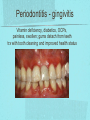
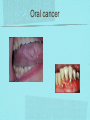
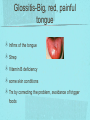
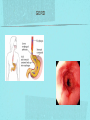
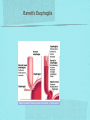
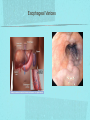
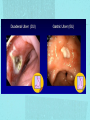
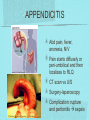
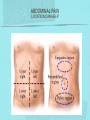
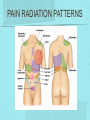
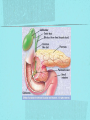
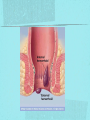
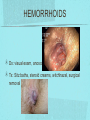
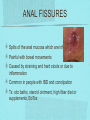
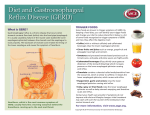
Gastrointestinal DisordersChapter 4 The End of The DigestiveSystem THE DIGESTIVE TRACT THE DIGESTIVE TRACT Basically a long tube for passage and processing of food 28 feet long Mouth Pharynx Esophagus Stomach Duodenum Jejunum Ileum (sm int) Large intestine (colon) THE DIGESTIVE TRACT Mouth: teeth grind food, salivary glands lubricate and begin enzyme processing, tongue coordinates swallowing and allows taste Pharynx: Aids swallowing, epiglottis prevents choking Esophagus: Coordinated peristaltic contractions. lower sphincter competence important Stomach: Villi (like velvet), mixes and stores food and secretes enzymes for digestion (pepsin and hydrochloric acid digest protein, amylase digests starch, intrinsic factor allows absorption of vitamin B12) THE DIGESTIVE TRACT Pyloric sphincter Duodenum Duodenum secretes alkaline mucus fluid + bile from gallbladder + enzymes from the pancreas Pancreas secretes digestive enzymes into duodenum, also secretes insulin into blood stream drives glucose into cells, and secretes glucagon into blood stream stimulates liver to release glucose Liver receives blood via portal circulation and purifies toxins (meds, alcohol), manufactures cholesterol, and produces bile. Bile absorbs and digests fats and fat-soluble vitamins, eliminates excess cholesterol by binding with it and passes thru GI tract. Gallbladder stores bile. If cholesterol level is high cholesterol rich bile in the gallbladder stones. THE DIGESTIVE TRACT Small intestine: 20 feet long, vast surface area (2300 sq ft!) Digests nutrients and absorb them into the portal circulation liver for processing and detoxifying. The lining secretes water, mucus, enzymes (amylase, pepsin, lipase, trypsin, bile, sucrase, lactase etc). Some of these enzymes are also responsible for the feeling of hunger and satiety, and peristalsis stimulation or suppression. Rapid turnover of cells that line the small intestine. 50 million cells/minute (!) are sloughed off into the lumen and are part of our stool. THE DIGESTIVE TRACT Large Intestine: NOT a digestive organ 4-5 feet long Secretes mucus, absorbs water and electrolytes, solidifies feces Cecum Ascending colon Transverse colon Descending colon Sigmoid Rectum Anus Filled with bacteria that help absorb nutrients/vitamins. ½ the weight of dry stool is bacteria! WHAT ARE SOME SYMPTOMS OF DIGESTIVE TRACT DISEASE? Abdominal pain Nausea Vomiting Diarrhea Constipation Dyspepsia Gas Belching SYMPTOMS OF GI DISORDERS • • • • • • • • Melena Hematochezia Hematemesis Dysphagia Bloating Anorexia Ascites Fatigue PHYSICAL EXAM Inspect Auscultate bowel tones Percussion Palpation DIAGNOSTIC TESTS Endoscopy Upper endoscopy: mouth, pharynx, esophagus, stomach, duodenum Lower endoscopy (colonoscopy): rectum, sigmoid, descending, transverse, ascending colon Ability to not only view and diagnose conditions, but also take biopsies, cauterize, sew, grab stones or foreign bodies, remove polyps, dilate strictures… Endoscope - Upper Endoscope: Lower DIAGNOSTIC TESTS X-ray Ultrasound CT MRI Chemistry tests: blood, urine, feces, gastric contens Imaging Studies Organization of Chapter Mouth and Esophagus (- tracheoesophageal fistula section) Stomach, Intestine, pancreas Anorectum DISORDERS OF THE MOUTH Canker sores (Apthous ulcers/stomatitis) Oral herpes (HSV I) (Cold sores) Thrush Gingivitis TMJ (temporomandibular joint syndrome) Cancer of the tongue and mouth Cigarettes, chew, snuff, alcohol, long term gingivitis Disorders of the Esophagus GERD Tracheoesophageal fistula and esophageal atresia Corrosive esophagitis and stricture Mallory-Weiss Syndrome Esophageal diverticula Hiatal hernia Apthous Stomatitis - Canker sore Herpes - Cold sore (herpetic stomatitis) Stomatitis Inflammation of oral mucosa (cheeks, lips, palate) Acute herpetic and apthous Self-limiting, 10 -14 days Severe or fatal in neonates Viral and Unknown etiology Tzanck smear thrush - candidiasis Fungal Infx, candida usually Fissures in corners of mouth, Patches on tongue Trx with yogurt, topical anesthetic mouthwash to loosen secretions remove sugar, improve immunity Periodontitis - gingivitis Vitamin deficiency, diabetics, OCPs, painless, swollen; gums detach from teeth trx with tooth cleaning and improved health status Oral cancer Glossitis-Big, red, painful tongue Inflmx of the tongue Strep Vitamin B deficiency some skin conditions Trx by correcting the problem, avoidance of trigger foods DISORDERS OF THE ESOPHAGUS Dysphagia = trouble swallowing, sensation of food being “stuck” Half the time it is psychological Also due to: Acid reflux damage esophageal mucosa Bacterial, viral, fungal infections Tumors of the throat, thyroid, parathyroid Chemical injury Neuromuscular disease (Parkinson’s, MD, ALS) Achalasia (lower 2/3 lacks normal innervation) Congenital narrowing DISORDERS OF THE ESOPHAGUS Gastroesophageal Reflux Disease (GERD) = heartburn 10% of adults in the US have daily GERD Peristaltic abnormality, malfunction of the lower esophageal sphincter, widening of the esophageal-gastric junction (hiatal hernia) Risks: obesity, alcohol, coffee, tobacco, caffeine, fats, chocolate, NSAIDs, pregnancy, hiatal hernia GERD GERD (continued) Intensity of symptoms DOES NOT correlate with extent of disease Sx’s: heartburn, pain, burping, acid in mouth Complications: narrowing of the esophagus due to scarring, ulcers, Barrett’s esophagus (cell changes that make cancer 40x more likely; 10% of people with GERD sx’s have Barrett’s) Barrett’s Esophagitis GERD (continued) Treatment: No lying down for 3 hrs after eating Elevate head of bed Avoid citrus, tomato prdts, spicy foods, coffee, alcohol, NSAIDs Antacids (Gaviscon, Tums, Rolaids, Maalox) H2 receptor antagonists reduce acid production (Tagamet, Pepcid, Zantac) Proton pump inhibitors reduce acid secretion (Nexium, Prevacid, Prilosec) Surgery **GERD RED FLAGS** Wakes someone up from sleep Occurs every day Trouble swallowing Persistent despite medical treatment Changes in or loss of voice Weight loss Wheezing ESOPHAGEAL VARICES Varicose veins of the upper GI tract Due to liver problems Cirrhosis causes scarring of liver Blood flow thru the liver is constricted due to scar tissue portal hypertension increased pressure in the veins of the lower esophagus and upper stomach can rupture and bleed heavily and sometimes fatally Esophageal Varices ESOPHAGEAL VARICES Causes upper GI bleed (hematemesis) Diagnose by medical history (liver disease, alcoholism, hepatitis), symptoms, and upper endoscopy Treat with cautery or ligature at the time of endoscopy, compression with balloon, surgery to redirect blood flow bypassing the liver ESOPHAGEAL CANCER History of heavy alcohol use, smoking, or chronic GERD Usually 50-70 years old Poor prognosis: 5 year survival is < 15% Surgery to remove esophagus, but recurrence is common Mallory-Weiss Syndrome Mild to Massive bleeding after forceful and prolonged vomiting Tear in cardia or Lower Esophagus Mentioning because though rare, is fatal Esophageal Diverticula Hollow outpouchings in the esophageal wall Mostly older men Throat irritation--> dysphasia--> regurg after eating--> aspiration pneumonia Sx/Sxs: hoarseness, asthma, pneumonitis in elderly, usually have bad breath, chronic cough Hiatal Hernia Defective diaphragm Portion of stomach passes into opening to chest sliding and paraesophageal hernia Strangulation of herniated portion can happen Hiatal Hernias Visceral Manipulation MOVING ALONG THE GI TRACT…WE REACH THE STOMACH Gastritis = stomach inflammation Most often caused by NSAIDs (ibuprofen) The risk of having gastritis with regular NSAID use is close to 10% 25,000 people out of every 100,000 hospitalized due to NSAID gastritis die of massive bleeding Also caused by alcohol and stress (such as severe illness, particularly when treated with steroids, such as shock, respiratory failure, anaphylaxis) GASTRITIS Sx’s: loss of appetite, abdominal pain, bloating, upper GI bleed Dx: endoscopy for those at risk and with sx’s Tx: Proton pump inhibitors and sucralfate (liquid that adheres to damaged mucosa and protects it from acid by forming a barrier) Gastroenteritis Self-limiting Nausea, vomiting, diarrhea intestinal flu, traveler’s diarrhea, viral enteritis, food poisoning 2nd to common cold in lost work and 5th in mortality of kids life threatening in old people too Bacteria, virus, toxins, drug reactions, food allerens Supportive care, hydration, rest GASTROENTERITIS Caused by both virus and bacteria, but both usually resolve without specific treatment. Need to think twice if lasts > 10 days, bloody diarrhea. Supportive care: HYDRATION, help with the nausea/vomiting. Diarrhea usually happens for a reason. Probiotics. Signs of dehydration: dry mouth/tongue, no tears, dough-y feeling skin, fast heart rate, low blood pressure, lightheadedness esp with a position change Peptic Ulcers circumscribed lesions in the mucosa- LE, stomach, pylorus, duodenum, jejunum (80% are duodenal) Gastric ulcers affect stomach, mostly elder men who use NSAIDs, tobacco and alcohol H. pylori, NSAIDs and hypersecretory disorders like Zolinger Ellison Syndrome are etiological Type A blood gets gastric ulcers and Type O get duodenal Acid secretion exceeds buffering capacity Ulcer Disease - Duodenal Duodenal ulcers are relieved by eating weight gain then ensues a strange sensation of hot water bubbling in the back of the throat Attacks are 2 hrs after meals and with trigger foods Bleeding can be fatal. Remember Jessie story Dumping Syndrome Associated with bolus of food stretching duodenum and rapid gastric emptying nausea, diaphoresis, weakness, flatulence, explosive diarrhea, distention and palpitations about 30 minutes after a meal Avoid by having patient drink fluids between meal, lie down after meals, don’t eat large meals and eat 6 small meals a day INFLAMMATORY BOWEL DISEASE (IBD) Ulcerative colitis and Crohn’s Disease Both are autoimmune, chronic lifelong illnesses Ulcerative colitis affects only the large intestine where it causes ulcerations and bleeding of the mucosal lining. Crohn’s affects the whole GI system from mouth to anus and causes swelling, infection, narrowing of the bowel with obstruction, and fibrosis of the entire bowel wall. IBD Both UC and Crohn’s can cause abdominal pain, cramping, bloody diarrhea, fecal urgency, weight loss, anemia, fever, malaise/fatigue. Crohn’s can cause fistulae (small tracts into the surrounding tissue that contain pus and infection, common at the anus pain in the butt) UC can cause other problems such as arthritis, eye inflammation, and dermatitis. It also greatly increases the risk of colon cancer. Folic acid supplements can reduce this risk somewhat. IBD Dx: Sigmoidoscopy with biopsy of the mucosa to diagnose UC. X-ray with barium can show ulcerations, strictures, and fistulae associated with Crohn’s. Endoscopy less helpful as it can’t look at the small bowel. IBD Tx: UC: high fiber diet, anti-diarrhea medications, steroids (oral, rectal suppositories and rectal foam), probiotics Crohn’s: low lactose, low fiber, multivitamins, mineral supplements, probiotics, steroids, antibiotics, immunosuppressant drugs, surgery for obstruction, abscess, fistulae Celiac Disease Gluten Enteropathy Poor food absorption and intolerance to gluten Intramucosal enzyme defect Can cause anemia, heart problems, bleeding disorders Biopsy and Endomysial IgG and IgA DIVERTICULOSIS Common in Western countries due to low fiber diets. Seen more in the elderly. (50% of people age 80 and up) The colon has to work too hard to move along small, hard stools causing blow-outs in weakened, older colonic tissue which has already lost its normal elasticity due to age. Most diverticulae are in the sigmoid colon. DIVERTICULOSIS Sx’s: Most people with diverticulae have no symptoms (2/3). Some have bleeding due to stretching and breaking blood vessels in the bowel wall. (this is the cause of HALF of all lower GI bleeds) Diverticulitis is when infection begins inside the out-pouching, and can cause perforation, abscess, peritonitis with severe abdominal pain, fever, LLQ tenderness (“reverse appendicitis”) DIVERTICULOSIS Dx: colonoscopy Tx: Antibiotics for diverticulitis, high fiber diet to bulk the stools, avoid small seeds (debatable point), surgery if peritonitis or abscess, if recurrent diverticulitis remove the sigmoid colon APPENDICITIS Abd pain, fever, anorexia, N/V Pain starts diffusely or peri-umbilical and then localizes to RLQ CT scan vs U/S Surgery-laparoscopy Complication: rupture and peritonitis sepsis ABDOMINAL PAIN LOCATION CAN HELP ABDOMINAL PAIN (DON’T FORGET NON-GI CAUSES) RIGHT UPPER QUADRANT: RIGHT LOWER QUADRANT: LEFT UPPER QUADRANT: LEFT LOWER QUADRANT: ABDOMINAL PAIN DIFFUSE: PERI-UMBILICAL: EPIGASTRIC: WOMEN: ELDERLY: PAIN RADIATION PATTERNS LOWER GI BLEED Hemorrhoid Fissure Infection Colon cancer/polyp Diverticuli/diverticulitis Ischemic gut Inflammatory bowel disease UPPER GI BLEED Esophagitis Gastritis Esophageal cancer Gastric cancer Esophageal, stomach, or duodenal ulcer Esophageal tear Esophageal varices Peritonitis Acute Abdomen Inflammation of the lining of the stomach 10% mortality Other GI issues cause this Intestinal Obstruction Usually from adhesions and strangulated hernias Simple, strangulated and closed-looped Colicky pain, nausea, vomiting, constipation, abdominal distention, Intussusception Telescoping bowel Fatal if not treated Most common in children Volvulus Twisted bowel 40-50% fatal Can feel palpable mass with severe pain and vomiting WHEN THE PANCREAS IS UPSET... Pancreatitis causes sudden, severe pain in the epigastrium radiating to the back Fever, altered consciousness, pain worse with lying down and improved with sitting up or leaning forward, nausea, vomiting, weak, anxious, sweaty Who gets pancreatitis? People with gallstones, alcoholics, trauma, viral infections including mumps, reaction to medications, peptic ulcer PANCREATITIS Dx: Acute mid-epigastric tenderness, silent bowel sounds. Amylase and lipase (on blood work) are very high. The pancreas can dissolve itself due to the release of its own enzymes and can hemorrhage, and can cause shock Tx: nothing by mouth to quiet the GI system and prevent stimulus to secrete enzymes, IV fluid and food. Occasionally surgical removal of the pancreas. CHRONIC PANCREATITIS Usually caused by alcoholism, but also CF Chronic pain, malabsorption, nutritional deficiencies STOMACH CANCER The 2nd most common cancer worldwide (2nd to skin cancer) Less common in the US where spoiled food is less common. 5 year survival is 10% Strongly associated with H.pylori gastritis STOMACH CANCER Sx’s: severe epigastric pain, weight loss, weakness, gastric obstruction with projectile vomiting after meals Dx: endoscopy and biopsy Tx: surgical removal of the stomach + chemotherapy. Often when it is diagnosed it has spread (metastasized) and surgery is palliative (to help symptoms only, not to cure) ANORECTUM Hemorrhoids Anorectal abscess and fistula- infections Rectal Polyps Pilonidal Abscess Rectal Prolapse - not covering Anal Fissure Pruritis Ani Proctitis ANORECTUM Hemorrhoids: engorged veins due to straining or inflammation Internal: nonpainful, can prolapse from the anus, can cause blood streaking the stool, in the toilet bowl, or seen when wiping External: commonly seen in pregnancy, obesity, constipation; blood clots can form inside them and are VERY painful HEMORRHOIDS Dx: visual exam, anoscopy Tx: Sitz baths, steroid creams, witchhazel, surgical removal or banding ANAL FISSURES Splits of the anal mucosa which are inflamed. Painful with bowel movements Caused by straining and hard stools or due to inflammation Common in people with IBD and constipation Tx: sitz baths, steroid ointment, high fiber diet or supplements, BoTox PRURITIS ANI (ITCHY BUTT) Can be quite intense Very common The itch you should not scratch Allergy to soap or foods (chocolate, nuts, citrus, fruits, berries, seafood, beer, coffee, vitamin C) Too little or too much anal hygiene Pinworms Rectal Polyps Masses of tissue that rise above mucosal membrane and protrude into GI tract asymptomatic look for other conditions like familial polyposis Proctitis STD from anal intercourse is mostly the cause Other factors are chronic constipation, laxative use, emotional upset, endocrine issues, etc. gonorrhea, herpes, chlamydia, anal-oral sex causes amebiasis symptoms are tenesmus, constipation, rectal fullness, abd cramps on left side, intense sense of needing to defecate and only small amount of fecal matter with blood and mucous is produced. Supportive treatment and antibiotics Ulcerating proctitis with perirectal fistulas and abscess Wow. A PRETTIER END