* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Four Shunts in Fetal Circulation
Survey
Document related concepts
Transcript
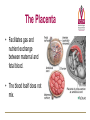
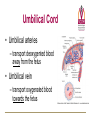
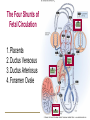
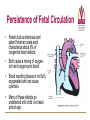
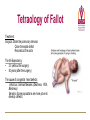
Fetal and Neonatal Circulation Dr. Carol Brenner Ph.D Gentleman’s Review Daniel Martingano OMS I Fetal Circulation • By the third month of development, all major blood vessels are present and functioning. • Fetus must have blood flow to placenta. • Resistance to blood flow is high in lungs. Fetal Circulation • The First Heart beat – Heart rate – Prior to delivery 4th week 65 beats/min 140 beats/min Fetal Circulation The fetal circulatory system is adapted to: • Maximize : gas and nutrient exchange between the mother and the fetus • Provide : a higher supply of oxygen to developing organs with high metabolic demand Bypasses the organs with low metabolic demand • High metabolic demand: Heart, Brain, Upper body • Low metabolic demand: Liver, Lungs, Lower body Four Shunts in Fetal Circulation The main features of the fetal circulation are: • • • 3 Non functioning lungs Course of the blood from the placenta to the heart Four shunts permitting the blood to bypass the liver and lungs: 1. 2. 3. 4. 4 Placenta Ductus Venosus Foramen Ovale Ductus Arterios 2 1 The Placenta • Facilitates gas and nutrient exchange between maternal and fetal blood. • The blood itself does not mix. First Shunt - Placenta • It replaces 4 separate organs – Lungs, GI system, Liver, and Kidneys – Participates in gas exhange, nutrition, fluid regulation, waste removal, fluid excretion and ion regulation • The Fetal Heart pumps blood primarily though the placenta (40%) • Placenta recieves most of the combined cardiac output Umbilical Cord • Umbilical arteries – transport deoxygented blood away from the fetus • Umbilical vein – transport oxygenated blood towards the fetus Umbilical Vein to Portal Circulation • Some blood from the umbilical vein enters the portal circulation allowing the liver to process nutrients. • The majority of the blood enters the ductus venosus, a shunt which bypasses the liver and puts blood into the hepatic veins. Second Shunt – Ductus Venosus • In the fetus, the ductus venosus shunts approximately half of the blood flow of the umbilical vein directly to the inferior vena cava – Thus, it allows oxygenated blood from the placenta to bypass the liver. – Plays a critical role in preferentially shunting oxygenated blood to the fetal brain. Second Shunt – Ductus Venosus • The second shunt bypasses the liver which is nonfunctional. • Oxygenated blood from the umbilical vein enters the Inferior vena cava bypassing the liver • Inferior vena cava drains the lower body (deoxygenated) • IVC deoxygenated blood mixes with the Ductus Venosus oxygenated blood Third Shunt – Foramen Ovale • The third major shunt is the blood entering the right atrium and then crossing the foramen ovale to enter the left atrium. • The oval hole in the septum which divides the right and the left atria – Shunts highly oxygenated blood from right atrium to left atrium • Right to Left shunt: – O2 from the IVC is send in to the left ventricle (foramen ovale) and in to the aorta Fourth Shunt – Ductus Arteriosus • The fourth shunt directs the blood from the pulmonary artery to the aorta through the ductus arteriosus. • Collapsed Right to Left Shunt – lungs- Vascular resistance – Aorta- Vascular resistance • Blood: Pulmonary artery Aorta • Aorta: – Proximally to the DA, the oxygenated blood is shuttled in to the upper parts of the fetus (Aorta) – Distally to the DA blood is mixed and transported to the systemic circulation • Aorta Umbilical arteries Placenta Maternal circulation The Four Shunts of Fetal Circulation 1. Placenta 2. Ductus Vensosus 3. Ductus Arteriosus 4. Foramen Ovale Fetal Hemoglobin • • Fetal Hb can carry 20-30% more O2 than the adult Hb Fetal hemoglobin 2 and 2 – – The γ chains of the fetal hemoglobin the higher affinity for the oxygen than its adult form. (shift to the left) • High Hb concentration (Hct 4060%) • High cardiac output Transition to Neonatal Circulation • The infants lungs begin to function – The lungs inflate which tends to draw blood from the right ventricle • Oxygenated blood from the lung passes through the pulmonary veins to the left atrium – Results in closure of the foramen ovale effectively separating the two atria – This also increases blood flow to the lungs as blood entering the right atrium can no longer bypass the right ventricle Transition to Neonatal Circulation The mechanisms that trigger the shift from the fetal to the adult circulation are: • Newborn breathing – pulmonary resistance • Removal of the placenta – systemic vascular resistance Transition to Neonatal Circulation • The placental circulation ceases – Umbilical vessels are no longer needed. They become obliterated – Occlusion of the placental circulation causes fall of blood pressure in the inferior vena cava and right atrium • The shunts stop to function – Within a day or two of birth, the ductus arteriosus closes off, preventing blood from the aorta from entering the pulmonary artery – The ductus venosus closes off so that all blood entering the liver passes through the hepatic sinusoids. Adult Derivatives of Vascular Structures Foramen ovale Closes shortly after birth, fuses completely in first year. Ductus arteriousus Ductus venosus Closes soon after birth, becomes ligamentum arteriousum in about 3 months. Ligamentum venosum Umbilical arteries Medial umbilical ligaments Umbilical vein Ligamentum teres Closure of the Ductus Venosus • Cessation of blood flow due to the clipping and cutting of the umbilical vein (pressure rises) • Blood backs up from the portal vein • 1-3 hrs after the birth- the strong contraction of DV smooth muscle • The closure of the DV causes an increase in the portal vein pressure-increased perfusion of liver Closure of the Ductus Arteriosus • pulmonary pressure + systemic pressure • Change of flow-from the aorta in to the pulmonary system – • reversal of the flow Increased O2/ prostanglandin E2 levels cause the progressive closure and formation of the fibrous tissue – 4-6 days; forms ligamentum arteriosum • The role of prostaglandin E2 (keeps the duct open) – The usage of PE2 blocker drug Indometacin (closes the duct) Persistence of Fetal Circulation • Patent ductus arteriosus and patent foramen ovale each characterize about 8% of congenital heart defects. • Both cause a mixing of oxygenrich and oxygen-poor blood • Blood reaching tissues is not fully oxygenated and can cause cyanosis. • Many of these defects go undetected until child is at least school age. Patent Ductus Arteriosus • Left to right shunt • Failure of ductus arteriosus to close – Leads to increased aortic pressure – Decreased blood flow through the PDA in to the pulmonary circulation • No problems in early life – no cyanosis • As patient grows – aortic pressure increases – cyanosis dude to increased diameter of PDA Patent Ductus Arteriosus • Cyanosis usually occurs late in life • Prolonged left to right shunting -> pulmonary hypertensions -> rightsided heart pressures that exceed the left -> reversal of blood flow through the shunt • This shunting of unoxygenated blood to the systemic circulation is called Eisenmenger syndrome (irreversible pulmonary vascular sclerosis) – Eisenmenger syndrome indicates that the defect is non-operable Patent Ductus Arteriosus • • ½ to 2/3 of blood from the aorta passes through the pulmonary system (recirculation) Cyanosis occurs latter in life as heart and/or lungs fail Diminished cardiac and respiratory reserve – Diminished physical activity (fainting) The life span: 20-40 years (MCCD: pulmonary edema and CHF) • • • • Treatment : Indometacin Heart surgery-historical Watch for prematures !!! Machinery murmur (S2 diminished) • • Tetralogy of Fallot • Blue Baby- EARLY CYANOSIS • Group of anomalies: • • • • Stenosis of pulmonary artery (bypass lungs) Right ventricle enlargement Aorta-originates from the right ventricle riding on the septum Blood from the Right ventricle passes trough the ventricular septal defect in to the L Ventricle and in to the overriding aorta Tetraology of Fallot Treatment: Surgical: Dilate the pulmonary stenosis Close the septal defect Reconstruct the aorta The life Expectancy: • 2-3 (without the surgery) • 50 years (after the surgery) The cause of congenital heart defects: Infectious: German Measles (Deafness, PDA , Blindness) Genetics: Some populations are more prone to develop defects