* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download General characteristic of intestinal infections. Typhoid fever
Sexually transmitted infection wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Meningococcal disease wikipedia , lookup
Trichinosis wikipedia , lookup
Yellow fever wikipedia , lookup
Brucellosis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Gastroenteritis wikipedia , lookup
Chagas disease wikipedia , lookup
Yellow fever in Buenos Aires wikipedia , lookup
Leishmaniasis wikipedia , lookup
Marburg virus disease wikipedia , lookup
1793 Philadelphia yellow fever epidemic wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Oesophagostomum wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Multiple sclerosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
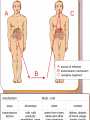
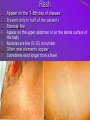
General characteristic of intestinal infections. Typhoid fever, paratyphoids A and B Intestinal infections are characterized by location of causative agents in intestine and their distribution in the environment with excrement's. As a microbe is released into the environment with feces, urine, vomits (cholera), it can cause disease in a healthy person only after ingestion with food or water. In other words, i.i. are characterized by faecal-oral mechanism of transmission. On a global scale, intestinal infections are second only to cardiovascular diseases as a cause of death, they are the leading cause of childhood death, and in some populous, developing areas, they are responsible for many years of potential life loss then all other causes combined. Estimates are that 4.6-6 mln children die each year (more than 12,600/day) in Asia, Africa and Latin America and that over 10,000 die from diarrhea each year in the USA. Typhoid fever Typhoid fever is an acute disease from the group of intestinal infections. Characterized by cyclic course, bacteremia, intoxication, rash on the skin, lesions of the lymphatic apparatus of the small intestine. Salmonella typhi Antigens О Н Vi ІІІ І ІІ 1 2 3 Scheme of infection’s transmission: Source: 1. Patient 2. Carrier Mechanism of transmission – fecal-oral Susceptibility – up to 40 – 50 % Water epidemy characterized by: 1. Sudden beginning 2. Most of the patients were used the same water-supply 3. Mild forms of disease mainly 4. Fast decreasing of epidemy after disinfection of water Food epidemy : 1. Acute or gradual begining after consuming of contaminated food (milk) 2. Most patients fall ill after consuming of unboiled milk (family outbreaks) from the same source 3. Biggest part of sick contigent are children 4. Severe forms of disease mainly, because microorganisms replicates in milk and create massive infectious dose Phases of pathogenesis: 1. Penetration of the causative agent into the organism 2. Invasion of the small intestine through Peyer’s patches and multiplication within macrophages 3. Spreading by bacteremia to the reticuloendothelia system (liver, spleen, bone marrow) where furthe multiplication occurs 4. Discharging of the agent from the organism (excretory phase) 5. Re-invasion of the bloodstream and infection of othe organs including the kidney and Peyer’s patches again causing apparent relapse in the third week 6. Formation of immunity A chronic asymptomatic carrier state persist in 1-2 %. Prodromal period fever malaise anorexia headache myalgias Climax period Constipation or diarrhea Respiratory symptoms, including cough and sore throat Neuropsychiatries manifestations, including confusion, dizziness, seizures Hepatosplenmegaly Violation of cardiovascular system Status typhosus is observed in serious course of the disease Rash 1. 2. 3. 4. Appear on the 7-8th day of disease Present only in half of the patients Roseola-like 5. Appear on the upper abdomen or on the lateral surface of the body Roseolas are few (5-15) in number 7. Sometimes exist longer than a fever 6. Often new elements appear Specific complications: 1. Intestinal bleeding 2. Intestinal perforation 3. Infectious-toxic shock Signs of bleeding 1. Increase of pulse rate and decrease of body temperature - “devil’s cross” 1. Clarification of consciousness 2. Other signs of posthaemorrhagic anemia Clinical signs of perforation 1. Mostly weak abdominal pain, sudden acute pain occur rarely 2. Important symptom of peritonitis – local tension of abdominal muscles 3. Signs of peritoneal irritation are weak or absent Factors, provoking relapses: 1. Violation of diet 2. Advanced cancellation of bed regime 3. Emotional stress 4. Intercurrent diseases 5. Avitaminosis, immunodeficiency state etc Signs preceeding relapses 1. 2. 3. 4. 5. Subfebrile temperature Increasing of pulse rate Presence of rash Splenomegalia Aneozynophylia Clinical peculiarities of paratyphoid A 1. In paratyphoid A incubation period is shorter than in typhoid fever. It's duration is 8-10 days. 2. The onset of the disease is an acute. Sometimes, the onset of the disease is accompanied by cough, catarrh. 3. Facial hyperemia, blood injection of the sclera’s vessels, herpes on the lips are observed during examination. 4. The temperature is wave-like or remittent. The fever is accompanied by chills and than by diaphoreses. Clinical peculiarities of paratyphoid A 5. In paratyphoid A the rash appears more early than in typhoid fever. The rash is polymorphic. Roseolas, petechias and measles-like rash may be observed. The intoxication is temperate. 6. There is no status typhosus. 7. There is normal quantity of leukocytes in peripheral blood. But leukocytosis and lymphocytosis may occur too. 8. In majority of the patients the disease has a moderate course. The relapses are frequently observed in case of paratyphoid A. Clinical peculiarities of paratyphoid B • • • • • Paratyphoid B incubation period is 5-10 days. The onset of the disease is acute, with expressive chill, myalgia and weakness At the initial period of the disease the intoxication may be combined with symptoms of acute gastroenteritis The temperature is not prolonged. Status typhosus is absent in majority of the patients. The symptoms of intoxication disappears very quickly The rash is polymorphic, plenty. It appears at the earlier period. In some cases the course of paratyphoid B may be severe with septic manifestations Diagnostics Positive blood culture during first two weeks From the third week positive faecal, bile and urine cultures are obtained Widal serology test is most helpful in non-endemic areas RIHA with erythrocyte diagnostics (O-, H-, Vi-antigens) Treatment 1. Etiotropic: Ciprofloxacin, Ceftriaxone, Ampicillin, Co-Trimoxazole or Chloramphenicol, Levomycetin, Bactrim, Azitromicin, Ofloxacin , Cefotaxim (depending on sensitivity tests) Vi – antigen 2. Pathogenetic: diet № 2, bed regime, desintoxication remedies, inhibitors of proteases, probiotics, desensibilizing remedies, vitamins Treatment of infectious-toxic shock: Rheopolyglukin Quartasault (Lactosault) Dopamine Prednisolone Treatment of intestinal bleeding: Precise bed regime, laying on the back during 24 h Water-tea diet 10 -12 h Cooling of abdominal area during first hours after bleeding detection Medicinal treatment (Vicasol, Calcium chloride, blood transfusion, amynobutyrum acid etc) Ant epidemic measures: Examination on typhoid fever and paratyphoids all patient with fever, which last more than 5 days (once on hemoculture, and if fever continue more than 10 days - Widal’s hemaglutination reaction or RIHA) Examination of all persons, who are working at the industried dealing with food for detection of bacteriocarriers Obligatory hospitalization of patients and carriers into infectious hospital Obzervation of contact persons during 25 days and their isolation from other people Every day thermometry, interrogation and medical examination One test of feces on coproculture and blood on Vi-antigene Reconvalescents are discharged from the hospital after clinical recovering and three-times analysis of feces and urine with 5-days interval, and bile after 10 days of disappearing of clinical signs three-month observation and 2-years registration in sanitary-epidemic department with several times bacterial examination during a year Current and final disinfection Control and prevention Depends on personal hygiene, safe food and water, and good sewage disposal facilities to control endemic disease. Carrier detection and treatment help to control outbreaks, and killed or live v accine will protect travellers.