* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Imaging Post-Fontan: Why I Do It
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial septal defect wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
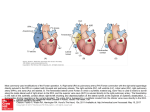
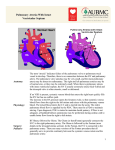
Imaging Post-Fontan: Why I Do It Cynthia K. Rigsby, MD Department of Medical Imaging Post-Fontan Imaging ! Fontan circuit palliative ! Good result for patients with ideal hemodynamic profile ! Most patients are NYHA class I or II ! Can be early and late morbidity and mortality ! Complications include exercise intolerance, desaturation, ventricular dysfunction, rhythm disturbances, hepatomegaly, lymphatic dysfunction, systemic venous thrombi/pulmonary embolism, ascites, and peripheral edema ! Absence of symptoms does not mean ideal hemodynamic profile ! Potential complications should be pursued and treated prior to becoming clinically apparent Gewillig. Heart 2005;91:839–846. Post-Fontan Imaging ! Cross-sectional imaging complimentary to echocardiography ! Echo windows limited as patients grow ! Fontan pathway can be completely delineated ! Driving force for Fontan cardiac output is pulmonary vascular resistance ! Non-obstructive flow to/from lungs essential ! Functional ventricular, valvular, and flow assessment ! Lung, liver evaluation Brown DW. Progress in Pediatric Cardiology 28 (2010) 45–58. Fontan Anatomy ! Determine Fontan type ! RA to PA or variants ! Generally older patients ! Stasis secondary to swirling of flow in dilated RA ! Poor flow to lungs ! Arrhythmia ! Coronary sinus dilation; coronary stasis ! Lateral tunnel prosthetic baffle and portion of right atrial wall ! Can grow with patient ! Can be performed under 3 years ! RA tissue exposed to high pressure; RA sutures; can lead to arrhythmia ! Extracardiac baffle ! ! ! ! PTFE graft Does not grow Older than 3 years Adequate size for adult IVC blood flow Fontan Anatomy ! Determine Fontan type ! RA to PA or variants ! Generally older patients ! Stasis secondary to swirling of flow in dilated RA ! Poor flow to lungs ! Arrhythmia ! Coronary sinus dilation; coronary stasis ! Lateral tunnel prosthetic baffle and portion of right atrial wall ! Can grow with patient ! Can be performed under 3 years ! RA tissue exposed to high pressure; RA sutures; can lead to arrhythmia ! Extracardiac baffle; PTFE graft ! Does not grow ! Older than 3 years ! Adequate size for adult IVC blood flow Fontan Anatomy ! Determine Fontan type ! RA to PA or variants ! Generally older patients ! Stasis secondary to swirling of flow in dilated RA ! Poor flow to lungs ! Arrhythmia ! Coronary sinus dilation; coronary stasis ! Lateral tunnel = prosthetic baffle and portion of right atrial wall ! Can grow with patient ! Can be performed under 3 years ! RA tissue exposed to high pressure; RA sutures; can lead to arrhythmia ! Extracardiac baffle ! ! ! ! PTFE graft Does not grow Older than 3 years Adequate size for adult IVC blood flow Fontan Anatomy ! Fenestration ! Allow for decompression of initial higher pressures in venae cavae ! Prevent rapid lung volume overload ! Increase systemic ventricle preload/ increase cardiac output ! Can cause desaturation ! Can be closed percutaneously ! Venovenous collaterals ! Decompress from higher pressure venae cavae to lower pressure pulmonary or systemic veins that drain to the common atrium ! Systemic desaturation ! Plan for cath treatment ! Thrombus ! Massive PE most common cause of out of hospital death Gewillig M. Heart 2005; 91(6):839–846. Fontan Anatomy ! Fenestration ! Allow for decompression of initial higher pressures in venae cavae ! Prevent rapid lung volume overload ! Increase systemic ventricle preload/ increase cardiac output ! Can cause desaturation ! Can be closed percutaneously ! Venovenous collaterals ! Decompress from higher pressure venae cavae to lower pressure pulmonary or systemic veins that drain to the common atrium ! Systemic desaturation ! Plan for cath treatment ! Thrombus ! Massive PE most common cause of out of hospital death Gewillig M. Heart 2005; 91(6):839–846. Fontan Anatomy ! Fenestration ! Allow for decompression of initial higher pressures in venae cavae ! Prevent rapid lung volume overload ! Increase systemic ventricle preload/ increase cardiac output ! Can cause desaturation ! Can be closed percutaneously ! Venovenous collaterals ! Decompress from higher pressure venae cavae to lower pressure pulmonary or systemic veins that drain to the common atrium ! Systemic desaturation ! Plan for cath treatment ! Thrombus ! Massive PE most common cause of out of hospital death Gewillig M. Heart 2005; 91(6):839–846. Pulmonary Arteries ! Stenosis ! Anastomosis/prior shunt ! Compression ! Differential pulmonary blood flow ! IVC/SVC blood flow distribution ! Pulmonary arteriovenous malformations ! Absence of pulsatile flow ! Absence of “hepatic factor” ! Desaturation Pulmonary Arteries ! Stenosis ! Anastomosis/prior shunt ! Differential pulmonary blood flow ! IVC/SVC blood flow distribution ! Pulmonary arteriovenous malformations ! Absence of pulsatile flow ! Absence of “hepatic factor” ! Desaturation Pulmonary Arteries ! Stenosis ! Anastomosis/prior shunt ! Differential pulmonary blood flow ! IVC/SVC blood flow distribution ! Pulmonary arteriovenous malformations ! Absence of pulsatile flow ! Absence of “hepatic factor” ! Desaturation IVC to LPA 64%; IVC to RPA 36% SVC to LPA 0%; SVC to RPA 100% Pulmonary Veins ! Stenosis Atrioventricular Valves ! Left, right, common ! Stenosis ! Regurgitation ! Valvular regurgitation can be estimated using ventricular volumetrics and AV valve/great artery flow analysis Single Ventricle Function/Scar ! Single right or left ventricle ! Morphologic right ventricle and systemic afterload ! Multicenter study showed abnormal ventricular function in 27% patient ! Associated with older age/ systemic RV morphology ! Association between myocardial fibrosis/LGE and higher ventricular volumes, global and regional FSV function, and nonsustained VT Anderson PA. JACC. 2008 July 8;52(2):85–98. Rathod RH. JACC. 2009;53:A3. Aortic/Neoaortic Valve ! Stenosis/Regurgitation ! Volume load from regurgitation can be assessed with phase contrast Aorta ! Aortopulmonary collaterals ! Volume load systemic ventricle ! Detrimental volume/ pressure load on pulmonary circulation ! Collateral flow as a percentage of aortic flow 26±9% ! Significant contribution of collateral flow to pulmonary flow ! No correlation with hemodynamic findings at cath Grosse-Wortmann L.Circ Cardiovasc Imaging 2009. May;2:219–25. Liver ! Venous hypertension ! Increased sinusoidal pressure ! Cirrhosis ! Coagulation abnormalities ! Risk for thromboembolism ! Portal hypertension ! Risk for hepatocellular carcinoma Lymphatic System ! Early lymphedema/ pulmonary edema and chylothorax ! Elevated SVC pressure ! Protein losing enteropathy ! Intestinal lymphangiectasia ! Chyle leak into gut/abdomen ! Ascites, immunodeficiency, coagulopathy ! Poor prognosis ! Plastic bronchitis ! Secretion of mucoid material into airways ! Airway obstruction, respiratory distress Fredenberg T. RadioGraphics 2011; 31:453–463. Lymphatic System ! Early lymphedema/pulmonary edema and chylothorax ! Elevated SVC pressure ! Protein losing enteropathy ! Intestinal lymphangiectasia ! Chyle leak into gut/abdomen ! Ascites, immunodeficiency, coagulopathy ! Poor prognosis ! Plastic bronchitis ! Secretion of mucoid material into airways ! Airway obstruction, respiratory distress Fredenberg T. RadioGraphics 2011; 31:453–463.