* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The Expanding Role of Microsomal Enzyme Induction, and Its
Psychopharmacology wikipedia , lookup
Discovery and development of neuraminidase inhibitors wikipedia , lookup
Discovery and development of non-nucleoside reverse-transcriptase inhibitors wikipedia , lookup
Drug design wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Discovery and development of ACE inhibitors wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Pharmacognosy wikipedia , lookup
Neuropharmacology wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
Theralizumab wikipedia , lookup
Drug discovery wikipedia , lookup
Prescription costs wikipedia , lookup
Pharmacokinetics wikipedia , lookup
CLIN.CHEM. 26/6,691-699 (1980)
The Expanding Role of Microsomal Enzyme Induction, and Its Implications
for Clinical Chemistry
David M. Goldberg
Microsomal enzyme induction, a term denoting the ability
of the substrate for a microsomal enzyme to enhance the
activity of that enzyme and frequently of related enzymes,
has been demonstratQd in a wide range of tissues, notably
the liver, placenta, small intestinal mucosa, and peripheral
lymphocytes. The major agents that cause microsomal
enzyme induction are drugs and xenobiotics. Factors
modulating the extent of enzyme induction by a given agent
include age and nutrition, and wide species variations are
encountered with different inducing agents. Markers for
microsomal enzyme induction include determination of the
plasma half-life for conveniently measured drugs, and the
measurement of endogenous metabolites such as 6flhydroxycortisol and D.glucaric acid in 24-h urine collections. While these are valuable for monitoring enzyme
induction in healthy patients, they are altered in certain
forms of liver disease, and results must then be interpreted
with caution.
Microsomal enzyme induction may interfere with reference values, particularly for membrane-bound enzymes,
in otherwise healthy populations, and may play a role in
metabolic bone disease, drug interactions, carcinogenesis,
and hypertriglyceridemia. Drug therapy of the neonatal and
congenital hyperbilirubinemias has been inspired by the
mechanism of hepatic microsomal enzyme induction, and
“markers” for enzyme induction can be used to monitor
drug compliance. The activity of serum y-glutamyltransferase seems to be especially valuable for this purpose.
Additional Keyphrases: aminopyrine
anticonvulsants
antipyrine half-life
aryl hydrocarbon hydroxylase
‘
3,4benzpyrene
‘
carcinogenesis
cigarette smoking
‘
cytochrome P450 - phenytoin
.
drug interaction
epilepsy
epoxide hydrase
‘
ethanol
D-glucaric acid #{149} y -glutamyltransferase
63-hydroxycortisoI
hyperbilirubinemia
hypertriglyceridemia
.
metabolic bone disease
phenobarbital
.
polycyclic
hydrocarbons
theophylline
tricyclic antidepressants
What Is “Microsomal
Enzyme Induction”?
The term “microsomal
enzyme induction”
denotes
the
ability of a substrate for a microsomal
enzyme to enhance the
activity
of that enzyme-and
frequently
of related
enzymes-by
promoting
their de novo synthesis
(J_3),1
This,
The Department
of Biochemistry,
The Hospital for Sick Children,
555 University
Ave., Toronto;
and the Department
of Clinical Biochemistry, The University
of Toronto,
Toronto,
Ontario,
Canada.
1 Ed. note: History repeats
itself. There was a large flurry of interest, some 150 papers, in “induced”
enzymes in the first half of this
century (cf, e.g., the reviews by Abderhalden:
Abwehrfermente,
Verlag
Steinkopff,
Dresden,
1944, and Ergeb. Enzymforsch.
11: 1, 1950).
Then it died away, although
there w,as later work on “adaptive”
enzymes, principally
in microbiology.
Received and accepted
Feb. 12, 1980.
in turn, may lead to a dramatic
increase in the endoplasmic
reticulum
of the affected cells, classically
seen in the liver of
the phenobarbital-treated
rodent
(4), although
extensive
morphological
changes
accompanying
microsomal
enzyme
induction
are the exception rather than the rule. Most of the
agents recognized
as inducers
of microsomal
enzymes
are
foreign to the body and are knowingly ingested as drugs or are
fortuitously
ingested
as environmental
and food contaminants. The number
of compounds
in both categories
is increasing at an alarming rate as our society proliferates
the use
of therapeutic
and abused drugs and of chemical substances
in industrial
processes
and agriculture
that can enter the
human food chain. Current
research
is uncovering
the enzyme-inducing
properties
of these agents as awareness
of the
problem
by government
authorities
and the scientific
community expands. Some representative
examples are shown in
Table 1.
Where Does It Occur?
Although
most of our knowledge
of microsomal
enzyme
induction
has come from recognition
of its effects upon the
liver, other tissues such as placenta,
small intestinal
mucosa,
and peripheral
lymphocytes
may show similar responses
to
environmental
agents. The availability
of the latter cells for
study without
the need for invasive biopsy procedures
has
stimulated
interest in their diagnostic
potential
as “markers”
of the body’s exposure
and response to carcinogenic
hydrocarbons.
The clinical chemist is being challenged
on many
fronts to an awareness
of the phenomenon
and its scope. He
should understand
the subtle as well as the more obvious
implications
this has for his interpretation
of laboratory
data
and his role in developing
new test procedures
to evaluate
enzyme induction
where this is of help in the diagnosis and
management
of patients.
The Microsomal
“Drug Hydroxylation
System”
For an understanding
of microsomal
enzyme induction,
it
is necessary to describe the hepatic drug hydroxylation
system
as a prototype.
This is shown schematically
in Figure 1. The
reaction involves molecular oxygen, one atom of which is used
to hydroxylate
the drug, while the other atom is used to generate water from reduced pyridine nucleotides.
The electrons
required
to reduce the free atom of oxygen generally
come
from NADPH,
but under certain circumstances
NADH can
also provide the necessary reducing equivalents.
Where NADP
is the source of electrons,
the flow is through the enzyme cytochrome
c reductase
(EC 1.6.99.3) to a group of cytochromes
that are characterized
by their spectral properties
and that
also differ in enzyme specificity.
The best characterized
are
cytochrome
P450, the terminal
electron-transport
system for
barbiturate hydroxylation,
and cytochrome
P448, the terminal
electron-transport
protein for hydroxylation
of aromatic
hydrocarbons,
especially those that have carcinogenic
properties.
The function
of this system in general terms is to detoxify
drugs and foreign
compounds
and to render
them more
water-soluble,
to facilitate
their excretion
by the kidney. A
CLINICAL CHEMISTRY, Vol. 26, No. 6, 1980
691
NADPH
NADH
-
Cytochrome
reductase
c
Cytochrome
reductase
b5
Lipid
e.-Cytochrome
Cytochrome
P-450
P-448
_____
b5 --CN-
sensitive
factor
-.02
Fig. 1. Pathwaysand components of hepatic microsomal electron-transport system utilized in drug hydroxylation reactions
From ret. 1 with kind permission of the authors and publishers (Karger, Basel)
number of qualifications
must be made, to put this statement
into proper perspective:
(a) The chemical reactions of which this system is capable
go far beyond simple hydroxylation
and include demethylation, de-ethylation,
epoxidation,
deamination,
and dehalogenation,
although
all these reactions
can be generically
regarded as catabolic.
(b) Metabolism
of a drug or carcinogen
by this system may
actually enhance its biological potency.
(c) Other chemical
reactions that do not primarily
involve
the hepatic cytochrome
P450 drug-hydroxylation
system,
such
as sulfation
and glucuronidation,
may be used by the liver to
detoxify foreign compounds.
(d) The cytochrome
P450 system and its congener hemoproteins are found in tissues other than the liver, in organelles
other than the microsomes,
and are involved in the hydroxylation of important
endogenous
compounds
such as cholesterol and the steroid hormones (for example, by adrenal mitochondria),
and of heme itself by the heme oxygenase system
of macrophages,
which converts
heme to biliverdin
and has
been shown to be substrate-inducible.
Drugs and Enzyme Induction
Compounds
metabolized
ylation system are capable
system,
and thereby
the
by the microsomal
drug-hydroxof inducing the components
of the
metabolism
of many other com-
Table 1. Range of Microsomal Enzyme-Inducing
Agents Demonstrated in Man
pounds that act as substrates
for the same metabolic pathway.
Administration
of phenobarbital
induces the enzyme hexobarbital oxidase and cytochrome
P450, as well as many other
enzymes
that feed into the cytochrome
P450 system. The
carcinogen
3,4-benzpyrene
induces the enzyme aryl hydrocarbon hydroxylase
and cytochrome
P448, as well as the activity of many other enzymes which feed into the cytochrome
P448 pathway.
Compounds
that are strong inducers of cytochrome P450-related
enzymes
are weak inducers-or
even
inhibitors-of
cytochrome
P448-related
enzymes. However,
many of these interactions
vary with the agent and show
marked differences
among animal species. The mechanism
of this induction is not known in detail. It seems to depend
upon de novo protein synthesis,
because it can be blocked by
agents such as actinomycin
D, cycloheximide,
and puromycin
(1), which inhibit one or other of the steps in transcription
or
translation
of the genetic code. One proposal
is that the inducing agent acts to relieve repression
of enzyme synthesis;
another suggestion
is that binding of the exogenous
inducer
at the active site blocks the binding of an endogenous
inducer
(possibly
a lipid peroxide),
which thus accumulates
and
stimulates
synthesis
of the enzyme until a new steady-state
is reached (3). It is even more difficult to explain the increase
in non-heme
microsomal
enzymes such as glucuronyl
transferases, and in plasma membrane
enzymes
such as y-glutamyltransferase
(EC 2.3.2.2), as well as the generalized
increase in microsomal
protein that occurs with some inducing
agents, notably phenobarbital.
How Specific
Are the Microsomal
Hemoproteins?
Relaxant (muscle)
Sedatives
Phenylbutazone
‘iseofuIvin
Rifampicin
Warfarin
Alcohol
Marijuana
Polychlorinated and
polybrominated biphenyls
Dioxane
Progesterone
DDT
Tobacco smoke
Coal tar paste
Barbecued foods
Meprobamate
Barbiturates
The relationship
between the number of cytochrome
P450
enzyme proteins and the wide range of activities catalyzed by
the microsomal drug-hydroxylation
system is not yet resolved.
It is inherently
unlikely that there is a specific hemoprotein
enzyme available
for each metabolizable
drug or chemical
substance,
because
most of these are compounds
to which the
body has not previously
been exposed. Although the number
of individually
recognized
cytochrome
P450 congeners
is approaching
double figures, this still falls considerably
short of
the number required to support the known specific reactions
of the drug hydroxylation
system. An alternative
possibility
is that there are different binding proteins for each compound
or class of compound,
and that these binding proteins in turn
react with only one of the known
forms of cytochrome
P450.
Many fascinating
reconstitution
experiments
have been
performed
with animal materials to obtain deeper insight into
this issue. Studies of this type are now becoming feasible with
human liver. Cytochrome
P450 from adult (5, 6) and from
fetal (7) human liver was purified by using chromatography
on Octyl-Sepharose
4B as the initial step. The fetal hemoprotein differed from the adult form in that it alone catalyzed
hydroxylation
of aniline in a reconstituted
system. A com-
Methaqualone
ponent
Stimulants
Glutethimide
Nikethamide
(P450) reductase
(EC 1.6.2.4) from human liver; this enzyme
proved capable of using cytochrome
P450 and cytochrome
P448 for different
catalytic reactions
(5), and it therefore
Class of compounds
Anticonvulsants
Some Individual agents
Phenobarbital
Anti-inflammatory
Phenytoin
Aminopyrine
Antifungal
Ant!biotlcs
Anticoagulants
Agents of addiction
Industrial products
Oral contraceptives
Pesticides
Polycyclic hydrocarbons
692
CLINICAL CHEMISTRY, Vol. 26, No. 6, 1980
of this
system
was
purified
NADPH-cytochrome
c
seems that substrate
specificity
and hemoprotein
specificity
are not mediated
through
different
reductase
enzymes. Another achievement
has been the purification
of epoxide hydratase (EC 3.3.2.3) from human liver microsomes,
although
some minor contaminants
were still present (8). The enzyme
preparation
was active with a wide range of alkene and arene
oxides.
What Factors Affect Enzyme Induction?
Enzyme inducibility
shows marked species-related
differences and, in man, genetic factors exercise a paramount
influence
(9). Dependency
upon age has also been clearly
demonstrated.
Pregnancy
and seasonal factors modulate
the
response to enzyme-inducing
agents. So do nutritional
factors,
with fat (10), protein
(11), and carbohydrate
(12) all being
important
and relatively independent
of each other or of their
caloric equivalents.
Of those vitamins
so far examined,
only
vitamin
E has been shown to exercise-a
role in enzyme induction in the experimental
animal (13).
How Can We Recognize
Induction?
Microsomal
Enzyme
Recognition
of hepatic microsomal
enzyme induction stems
from the availability
of some analytical
tools for studying this
process. The activity of drug hydroxylation
reactions
can be
indirectly
assessed by measuring
the plasma half-life of the
drug after its injection. After equilibration
in the appropriate
distribution
space, its concentration
in the plasma decays
according to first-order
kinetics. Although several factors such
as renal and biliary excretion
contribute
to this clearance,
in
most instances
it is the activity of the liver drug-metabolizing
system that is rate limiting. Measurement
of drug half-lives
involves the semi-invasive
technique
of injection followed by
frequent
blood sampling,
although
in the case of some drugs,
such as aminopyrine,
the availability
of a 14C-labeled form of
the drug enables an index of its metabolism
to be obtained by
measuring
the excretion
of labeled
carbon dioxide
in the
breath (14, 15). Discrepancies
are seen between disappearance
rate of 14cJO2 from the breath and aminopyrine
clearance from
plasma
because the aminopyrine
is labeled at two methyl
groups, which are demethylated
at different
rates (16). For
this reason, [14C-methoxy]glycodiazine
(glymidine)
has been
proposed
as a more reliable compound
because its plasma
clearance correlates well with terminal disappearance
of ‘4C02
from the breath. With antipyrine
and with some other drugs,
salivary
measurements
can be used instead
of blood measurements
to follow drug clearance
(17). This has been validated by comparison
of the clearance rates of the drug and its
three major metabolites
in plasma,
saliva, and urine (18).
However,
for drugs in general, the pKa and the extent of
protein binding must be considered
in deciding the suitability
of substituting
salivary
for plasma
clearance
measurements.
Endogenous
factors that can be measured
are the urinary
excretion
of 6$-hydroxycortisol
and D-glucaric acid. Cortisol
is mainly metabolized
to 17-hydroxy-corticoids,
but a small
fraction
is converted
in liver microsomes
to the alternative
excretory
product,
6f3-hydroxycortisol,
and this fraction
is
greatly increased
during enzyme induction.
There is growing
interest
in this compound
as an index to steroid hormone
metabolism
as well as a marker of microsomal
enzyme induction (19), and its study has been greatly facilitated
by the
development
of radioimmunoassays
for its measurement
in
urine and plasma (20,21).
D-Glucaric acid is the main excretory product of the glucuronic
acid pathway,
which in mammals other than primates
and guinea pigs goes on to ascorbic
acid. This pathway,
and therefore
formation
of its terminal
product
D-glucaric
acid, is greatly stimulated
in situations
where microsomal
enzyme induction
occurs, for reasons that
are not entirely clear, aside from its known location
in the
endoplasmic
reticulum.
There is a need for better methods
than those currently used and which are predominantly
based
upon the ability of the lactone formed from D-glucaric
acid
(by heating the urine after acidification)
to inhibit the enzyme
/3-D-glucuronidase
(EC 3.2.1.31) (22). A method
based on
gas-liquid
chromatography
suffers the disadvantage
of converting D-glucaric acid into a series of different lactones, which
then have to be individually
quantitated
(23); thus the procedure is inherently
a complicated
one.
As Table 2 demonstrates,
the normal ranges for these tests
are not very reproducible
and are based on small numbers.
Closest agreement
among different
laboratories
exists for
antipyrine
half-life, which currently
has to be #{235}onsideredas
the reference
procedure
for demonstrating
microsomal
enzyme induction.
However,
the increases
in excretion
of 6/3hydroxycortisol
and D-glucaric
acid usually exceed the decreases in drug half-lives. Although reference ranges for these
chemical
markers
of enzyme induction
are not very useful,
important
information
can be obtained
by sequentially
measuring these constituents
in the same individual. The most
direct and unequivocal
evidence
of microsomal
enzyme induction is afforded by demonstrating
increased activity of the
enzyme responsible
for metabolizing
the inducing agent or the
appropriate
form of cytochrome
P450 to which it is related.
This is seldom possible in human patients.
It is important
to
Table 2. Values for Indicators of Hepatic
Microsomal Enzyme Induction Reported In
Healthy Untreated Control Subjects (mean ± SD)
Antipyrine
Indicator8
half-life (h)”
Reference no.
11.5 ± 2.1 (n = 15)
14.1 ± 2.7 (n = 7)
18
24
11.4± 3.0(n
=
10.9 ± 1.5 (n
=
25
26
27
8)
16)
14)
15)
31)
6)
12.1 ± 3.9 (n =
11.3 ± 3.1 (n =
12.0 ± 4.3 (n =
10.8 ±1.1 (n =
Paracetamol
half-life
28
29
30
(h)
2.5 ± 0.7 (n = 31)
Phenylbutazone
29
half-life
(h)
81 ± 16 (n = 18)
64 ± 12 (n = 12)
6/3-Hydroxycortisol
185 ± 72 (n
excretion
(t
9/ 24 h)
32
18)
=
320 ± 160 (n
32
33
=
34
20
14)
286 ± 54 (n = 10 males)
233 ± 80 (n = 8 females)
487 ± 145 (n = 6)
o-Glucaric
acid excretion
20
21
(mol/24
34.3 ± 16.0 (n = 18)
53.0 ± 10.0 (n = 16 males)
41.0±8.0(n=
l4females)
56.1 ± 15.6 (n = 38 males)
32.5 ± 4.9 (n = 19 males)
9.9 ± 3.7 (n = 17)
a
b
h)C
35
36
36
37
38
39
Based on mixed male and female populations unless otherwise stated.
All resultsbased on serum clearance except first, which Is based on salivary
clearance.
C
Some discrepancies due to difterences arising from standardization with
D-glucaric
acid or with its lactone.
CLINICAL CHEMISTRY, Vol. 26. No. 6, 1980
693
Table 3. Influence of Alcohol on t1/ Clearance of,
Drugs from the Plasma (mean ± SD, in hours;
from refs. 60 and 61)
Alcoholics
Tolbutamide
2.8 ± 0.5
(n31)
Non-alcoholics
5.8 ± 2.2
(n13)
Warfarin
26.5 ± 13.3
(n = 15)
41.4 ± 19.2
(n = 11)
Phenytoin
16.3 ± 6.8
(n = 15)
23.5±11
(n = 76)
note that the procedures
listed in Table 2 do not always show
a close correlation
with induction
of the specific enzyme in
animal experiments,
or amongst each other in human studies.
This is due to several factors:
(a) Each procedure
probably is subject to a different
dose
relationship.
(b) Each is subject to a different time course and may show
increase early, late, or only for a relatively limited period after
exposure
to the inducing agent.
(c) All are indirect and therefore
are subject to influences
of the inducing agent other than that of microsomal
enzyme
induction
alone.
(d) They may be differentially
affected
by disease,
or
physiological
states such as age or pregnancy.
What Are the Effects of Disease on Enzyme
Induction?
This point has received much attention
recently because
clinicians
have become interested
in examining
drug metabolism as an index of hepatic function.
By use of antipyrine
clearance, hepatic drug metabolism
was shown to be impaired
in cholestatic
patients, but the impairment
was reversible and
the liver remained
sensitive to microsomal
enzyme inducers
(27). Patients
with advanced
cirrhosis
and chronic active
hepatitis
(but not compensated
cirrhosis or acute hepatitis)
manifested
reduced
antipyrine
clearance,
which correlated
with and frequently
appeared
earlier than abnormalities
in
prothrombin
time (28, 40). However, in line with a study on
malnourished
children
(41), antipyrine
clearance
in these
patients was found to be greatly prolonged
if the diet was inadequate.
Although the authors failed to find an effect exercised by other environmental
factors such as use of alcohol and
cigarette
smoking,
this is contradicted
by another
report in
which the [t4Claminopyrine
breath
test was used, where
clearance was found to be faster in cirrhotic patients who were
consuming
alcohol or enzyme-inducing
drugs (42). By contrast, oral contraceptives
and therapeutic
doses of propranolol
seem to slow the clearance
rate of antipyrine
(30, 31), while
the delayed clearance
of three model analgesics
in a group of
cirrhotic
patients
was shown to be associated
with portalsystemic shunting of blood, although this was not established
as the sole contributing
factor (43). Again, ethanol enhances
acetylation
of sulfamethazine
in man and may obfuscate
the
patient’s
true “acetylator
status” (44).
With the above complexities
in mind, microsomal
enzyme
induction
clearly is one of several phenomena
that may prevent accurate
assessment
of the intrinsic
ability of the liver
to metabolize
drugs in health and disease. Because hepatic
disease alters drug metabolism,
this in turn may lead to erroneous conclusions when drug clearances are used to monitor
enzyme induction rather than to test hepatic function. In both
endeavors, the need for a detailed nutritional,
social, and drug
694
CLINICAL CHEMISTRY,
Vol. 26, No. 6, 1980
history of each patient hardly requires emphasis.
Nevertheless, an experimental
study recently reported
in this journal
(45) claimed that antipyrine
half-life was a more sensitive
index of hepatic damage caused by cytotoxic drugs than were
several serum enzyme assays, including alkaline phosphatase
(EC 3.1.3.1), y-glutamyltransferase,
aspartate
aminotransferase
(EC 2.6.1.1),
and glutamate
dehydrogenase
(EC
1.4.1.3).
Not only drug metabolism
but also the excretion
of D-glucane acid is affected by disease. Apart from the obvious errors
of interpretation
likely in patients with renal disease, significantly increased excretion has been reported in all jaundiced
patients, most notably where this is obstructive
(39), and also
in patients
with certain forms of porphyria
(46).
What Are the Consequences
Enzyme Induction?
of Microsomal
(a) Interference
with reference
values. Microsomal
enzyme induction
increases the activities
in serum of some enzymes commonly
used in diagnosis, especially in diagnosis of
liver disease (46-52). Gamma-glutamyltransferase
is the enzyme in serum that is most frequently
and dramatically
affected, and this poses problems
in defining reference
ranges
for this enzyme because even moderate drinking of alcohol can
increase its activity (53). Other membrane-associated
enzymes
such as alkaline phosphatase
and 5’-nucleotidase
(EC 3.1.3.5)
may be more active in the serum of patients
who are taking
such drugs (47). It is important
to recognize this relationship
and to avoid the over-investigation
of such abnormalities
in
the absence of clinical corroboration
of liver disease.
Serum ‘y-glutamyltransferase
activity can serve as a convenient marker of microsomal
enzyme induction
(51, 54-56).
It is simpler to measure than the urinary constituents
and the
results are promptly
available.
It is the most convenient
and
cheapest
index of microsomal
enzyme induction
currently
available, although
it will become more abnormal
in hepatobiliary disease than will the other indices described
above.
(b) Metabolic
bone disease.
The relationship
between
metabolic
bone disease and anticonvulsant
therapy has been
recognized for the past decade. It may depend upon the rapid
metabolism
of vitamin D by hepatic hydroxylating
enzymes
to inactive metabolites.
Patients
receiving
anticonvulsants
show a much faster half-life of vitamin
D3 than do normal
subjects (57) and their serum calcium concentrations
are lower
(58). In such patients,
there is significant
inverse correlation
between serum calcium concentration
and serum y-glutamyltransferase
activity (59), convincing
evidence that the enzyme induction
and the hypocalcemia
are directly
connected.
(c) Drug interactions.
This is well illustrated
by the effects
of chronic alcohol consumption
on drug metabolism.
Table
3 shows that the clearance
of three drugs known to be metabolized
by the hepatic drug-hydroxylation
system is enhanced because of the powerful enzyme-inducing
effect exercised by ethanol (60, 61). The data were obtained when the
patients were not actively drinking alcohol. When alcohol and
the drug are given simultaneously,
drug clearance is prolonged
because the alcohol acts as a competitive
substrate
inhibitor
of the drug-metabolizing
system. This explains
why it is
dangerous
to take barbiturates
along with alcohol, although
the chronic alcoholic is resistant
to barbiturate
as long as he
is not drinking
alcohol at the same time.
Plasma warfarin half-life is dramatically
lowered by various
enzyme-inducing
drugs (62). Patients
receiving such drugs
will require larger doses of warfarmn to achieve the desired
change in prothrombin
time. If the enzyme-inducing
drug is
withdrawn
while the warfarin is continued
at the same dosage,
the increase in half-life that follows will lead to the dose being
inappropriately
high, with risk of fatal hemorrhage.
j
11l.T.J
2000
%..:.I9RI1Qtct
LHNo8ARBITONE180mDAfl.,Y1
30
F.
25
15
10
5
0
0
2
4
6
8 10121416
1820
TIME (DAYS)
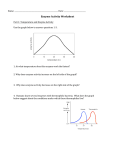
Fig. 2. Response to calorie restriction and to phenobarbital
(phenobarbitone)of serum bilirubin concentration in patient with
Criggler-Naj jar disease Type II
From ref. 91 with kind permission of the authors andof the publishersof Gas-
troenterology
(d) Cigarette
smoking.
It has been known for some time
that cigarette smoking affects the disposition
of certain drugs
by enhancing
their clearance
through
microsomal
enzyme
induction
(9, 63), theophylline
being a striking example (64).
Smoking halves the mean plasma concentration
of propanolol
for a constant
drug dose, but this effect diminishes
with age
due to an age-dependent
resistance
to enzyme inducibility
(65). A similar age-dependent
resistance
to the enzyme-inducing properties
of cigarette smoke has been observed with
antipyrine
clearance
(66).
The enzyme-inducing
properties
of tobacco
smoke are
predominantly
ascribable
to its content
of 3,4-benzpyrene,
and because this compound
is also generated
by the charcoal
broiling of meat, persons eating such food also have faster
rates of drug clearance (67). Moreover, it is present in coal tar,
and when this is applied to human skin in usual therapeutic
doses, it increases
by two- to five-fold the activity of the enzyme aryl hydrocarbon
hydroxylase
(AHH; EC 1.14.14.1),
which catalyzes
the initial step in benzpyrene
metabolism
(68). This enzyme is present in the epidermis
rather than the
dermis, and it increases
with age in healthy humans (69).
Activities
of this enzyme in the placentas
of women who
smoked during pregnancy
were more than 25-fold those of
non-smokers,
and the effect seemed to be dose-dependent
in
that activities
were greatest among mothers who smoked the
most (70, 71). Indeed, placental
AHH can be used as a measure of fetal exposure
to maternal
cigarette
smoking
(72).
Much effort is being expended
in measuring the AHH activity
of peripheral
blood lymphocytes,
monocytes,
and macrophages, directly as well s in cultured and mitogen-stimulated
preparations
of these cells (73, 74). A good correlation
with
cigarette
consumption
is revealed by these studies. AHH activity in lymphoblasts
showed high absolute induction
in 39%
of patients
with untreated
lung cancer but in only 15% of
normal subjects,
and the frequency
in patients
with other
malignancies
was not different
from that of controls
(75).
Indices of enzyme induction are thus being used as a measure
of cancer risk among smokers,
although
the current
procedures need to be greatly refined to achieve acceptable
predictive value.
(e) Carcinogenesis.
The relationship
between
carcinogenesis and enzyme induction is very complex. Many aromatic
hydrocarbons
that can induce experimental
cancer in animals
are metabolized
by the microsomal
hydroxylating
system to
inactive compounds.
If the hydroxylating
system has already
been activated
by enzyme-inducing
drugs, conversion
to inactive metabolites
will be faster and tumor development
will
be slower (76, 77). The opposite
situation
may also apply.
Compounds
such as polycyclic hydrocarbons
are metabolized
by microsomal
enzymes to active carcinogens
(78), and this
conversion
will be accelerated
where microsomal
enzyme induction has occurred.
Environmental
agents may be responsible for as many as 90% of human cancers (79), and because
the metabolism
of these agents is highly dependent
upon
microsomal
enzymes, the interaction
between carcinogenesis
and microsomal
enzyme induction
could be the most fruitful
area of cancer research in the next decade.
(I) Hypertriglyceridemia.
A relationship
between microsomal enzyme induction
and hypertniglyceridemia
has been
proposed
in several clinical states, including
hypertension
(80), diabetes
mellitus
(81), and use of oral contraceptives
(82). Support has been provided by other authors (83,84) and
has been extended
by the original authors (85, 86). Because
hypertniglycenidemia
is a risk factor for ischemic heart disease,
this association
could represent
an unfavorable
influence
of
microsomal
enzyme induction
upon survival in human populations.
What Are the Uses of Microsomal
Induction?
Enzyme
(a) Treatment
of hyperbilirubinemia.
Enzyme induction
has been used in the treatment
of subjects with unconjugated
hyperbilirubinemia.
These included
neonates
(87), patients
with Gilbert’s disease (88), and patients with Criggler-Naj
jar
Type II disease (89). Enzyme-inducing
drugs increase not only
the cytochrome
P450 content of human liver (90), but also its
ability to conjugate bilirubin (since this is an enzymic function
of the microsomes),
which leads to a dramatic
decrease
in
serum bilirubin
concentration
(91). This was valuable
in
treating
neonatal
hyperbilirubinemia
before phototherapy
was introduced
for this condition.
It still has a role in the
treatment
of Cniggler-Najjar
Type II patients.
Microsomal
enzyme induction
has been used prophylactically
in mothers
whose infants are expected to suffer from hyperbilirubinemia.
Phenobarbital
(92) and ethanol
(93) have been given to
mothers for this purpose, and lead to lower bilirubin concentrations
in the serum of their offspring than those in control
infants. When the carbohydrate
content of the diet is drastically decreased,
the concentration
of unconjugated
bilirubin
in serum increases.
The increase is greater in patients
with
Gilbert’s
disease,
readily
distinguishable
from the much
smaller increase in normal subjects
(Figure 2), and this provides a useful diagnostic test for Gilbert’s disease, particularly
when the patient is anictenic (94). Recent experimental
work
has shown that fasting diminishes
the supply of UDP-glucuronic acid available
for bilirubin
conjugation
(95) and this
stresses the already compromised
bilirubin
UDPglucuronosyltransferase
system
of patients
with Gilbert’s
disease,
whereas the normal subject is better able to cope with this
unfavorable
situation.
(b) Monitoring
of drug compliance.
Enzyme induction
as
an index of compliance
with prescribed
therapy has been well
defined in the treatment
of alcoholism.
This is related to the
very high serum y-glutamyltransferase
activity occurring
in
CLINICAL CHEMISTRY,
Vol. 26, No. 6, 1980
695
100
100S
.
2
90-
S
90
0
.
S
E
S
.
N
0
60-
0
E
a
S
0
.
‘in
0
30S
S
a
C
S
a
>
a
2
30-
:
:.
bDEQUAT
Too
ioo
DOSAGE
MUCH
LITTLE I
(CONTROLS) (EPILEPTICSON ANTICONVULSANTS)
I
:
Fig. 3. Urinary o-glucaric acid excretion in control subjects and
in epileptic patients short’y after starting anticonvulsant therapy
on a standard dose In relation to control of seizures and presence
of side effects
From ref. 102,with kind permissionof Masson Publishing Co
chronic alcoholics,
which declines towards normal on withdrawal from alcohol. Thus programs
for the rehabilitation
of
alcoholic patients can be devised in which these measurements
are used as a valuable aid in judging the effectiveness
of the
regime (96-98). However, recent reports have emphasized
the
need for caution in using such protocols,
because the decline
in serum ‘y-glutamyltransferase
activity on withdrawal
from
alcohol may not be as consistent
or as prompt as the earlier
authors suggested (99, 100). The role of y-glutainyltransferase
as an index of microsomal
enzyme induction
has been emphasized in many recent publications
(38-42,54-56),
and, as
I indicated earlier, this strongly limits its utility asa diagnostic
test in hepatobiliary
disease (101).
By measuring
drug concentrations
in blood or urine, one
cannot invariably assess a patient’s compliance
with therapy.
I have therefore
examined
the role of enzyme-induction
parameters
in this context. Epileptic
patients
given a standard
dose of anticonvulsants
on a body-weight
basis had extremely
variable serum drug concentrations
when measured
shortly
after therapy was begun (102). Those with lower values were
mcre poorly controlled clinically than those with higher serum
values. High D-glucaric acid excretion was observed in patients
whose therapy did not seem to control seizures, suggesting that
these patients had responded
to the drug by rapidly inducing
microsomal
enzymes, leading to rapid drug metabolism,
and
that they required a higher drug dose (Figure 3). Patients who
displayed
side effects from the standard
dose had lower Dglucaric
acid excretion,
presumably
because
their enzyme
systems were not induced sufficiently
to prevent accumulation
of the drug to higher concentrations
than were therapeutically
desirable. This information
can be obtained by measurements
of drug metabolism
and clearance,
but these are more complicated than measurement
of some acceptable
index to microsomal enzyme induction-which
therefore can serve as the
initial step in evaluating
such patients.
Epileptic
patients
stabilized
after three to six months on
a suitable dosage of phenytoin,
individualized
for each subject,
demonstrated
an apparent
correlation
between the dose required for stabilization
and the urinary D-glucaric
acid excretion (Figure 4). The extent of enzyme induction as reflected
696
A
Daily phenytoin
CLINICAL CHEMISTRY, Vol.26,No. 6,1980
8
6
dosage, mg/kg
Fig. 4. Relationship between urinary D-glucaric acid excretion
and daily dose of phenytoin (diphenylhydantoin) in patients after
several months of stabilization with control of seizures and absence of side effects
From ref. 102,with kind permission of MassonPublishingCo
by D-glucaric acid seemed to determine
the dose of phenytoin
required
to suppress
seizures reliably. Similar observations
have been made with other enzyme-induction
indices and
other enzyme-inducing
drugs; in general, patients who demonstrate a sharp enzyme-induction
response can be expected
to require more drug to attain a therapeutic
response.
It is
more meaningful
to evaluate
the change in the measured
variable above the basal value before initiating
therapy,
because the variance in reference values makes it essential to use
each subject as his own reference.
Urinary excretion
of D-glucaric acid and ‘y-glutamyltrans-
U
#{149}
100-
U
.
#{149}
U
.
.
U
U
4
E
-j
0
E
#{149}
90-
U
0
U
U
#{149} .
#{149}
N
0
E
.
0
a
#{149}
.
.
60.
U
U
.
U
9)
0
>
.
a
#{149}
.
#{149} .2
.
C
J
#{149}
301
2.
3.
.1
4#{149}
.3
POOR
RESPONDERS
GOOD
RESPONDERS
Fig. 5. Urinary D-glucaric acid excretion and serum ‘y-glutamyltransferase activity in psychiatric patients receiving tricyclic
antidepressants, graded according to response to therapy
From ref. 102, with kind permission of Masson Publishing Co
ferase activity in serum were measured in psychiatric
patients
receiving
tricyclic antidepressant
drugs who were classified
as poor responders
and good responders
(Figure 5). Both
indices of microsomal
enzyme induction
were higher in good
responders
than in poor responders.
Among poor responders,
enhanced
drug metabolism
was unlikely to be a factor since
the response to microsomal
enzyme induction
was also poor.
Patients
labeled 1, 2, 3, and 4 in Figure 5 finally admitted
to
taking the drugs irregularly.
Monitoring
indices of microsomal
enzyme induction
can therefore
provide guidance concerning
decisions
about increasing
the dose of a drug, switching
to a
different
drug, or, in the event of total noncompliance,
changing
to some therapy
other than one requiring
drugs
(102).
Concluding
Remarks
Microsomal
enzyme induction
is a phenomenon
that has
excited widespread
interest since its existence
was first recognized. Its impact upon biochemical
pharmacology
and environmental
medicine
has been explosive,
and it is now beginning to have important
implications
for clinical medicine
of which the clinical chemist should be aware. This review has
attempted
to focus attention
on these latter aspects,
with
special emphasis upon the more recent literature.
References
to fundamental
biochemical
mechanisms
will be found in
earlier reviews (1-3). It is reasonable
to assume that clinical
laboratories
will be increasingly
required
to implement
and
develop analytical
procedures,
stimulated
by the need to gain
a keener insight into drug metabolism
by individual
patients.
This process will accelerate
as the function of clinical chemistry changes from a diagnostic
role to one primarily
devoted
to the monitoring
of therapy. Chemical indices of microsomal
enzyme induction
will then assume prominence
in the laboratory armamentarium
of the future.
References
1. Lu, A. Y. H., Kuntzman, R., and Conney, A. H., The liver microsomal hydroxylation enzyme system. Induction and properties of the
functional components. In Frontiers of Gastrointestinal
Research,
2, L. Van der Reis, Ed., S. Karger, Basel, 1976, pp 1-31.
2. Hunter, J., and Chasseaud, L. F., Clinical aspects of microsomal
enzyme induction. In Progress in Drug Metabolism, 1, J. W. Bridges
and L. F. Chasseaud, Eds., J. Wiley, London, 1978, pp 129-191.
3. Marshall, W. J., Enzyme induction by drugs. Its relevance to
clinical biochemistry. Ann. Clin. Biochem. 15, 55 (1978).
4. Fouts, J. R., and Rogers, L. A., Morphological changes in the liver
accompanying stimulation of microsomal drug metabolizing enzyme
activity by phenobarbital,
chlordane, benzpyrene or methyl-cholanthrene in rats. J. Pharmacol.
Exp. Ther. 147, 112 (1965).
5. Kamataki, T., Sugiura, M., Yamazoe, Y., and Kato, R., Purification
and properties of cytochrome P-450 and NADPH-cytochrome
c
(P-450) reductase from human liver microsomes. Biochem. Pharmacol. 28, 1993 (1979).
6. Beaune, Ph., Dansette,
P., Flinois, J. P., Columelli, S., Mansuy,
D., and Leroux, J. P., Partial purification of human liver cytochrome
P450. Biochem.
Biophys.
Res. Commun. 88, 826 (1979).
7. Kitada, M., and Kamataki, T., Partial purification and properties
of cytochrome P450 from homogenates of human fetal livers. Biochem. Pharmacol. 28, 793 (1979).
8. Lu, A. Y. H., Thomas, P. E., Ryan, D., Jerina, D. M., and Levin, W.,
Purification of human liver microsomal epoxide hydrase. Differences
in the properties of the human and rat enzymes. J. Biol. Chem. 254,
5878 (1979).
9. Vesell, E. S., Disease as one of many variables affecting drug disposition and response: Alterations of drug disposition in liver disease.
Drug Metab. Rev. 8, 265 (1978).
10. Wade, A. E., and Norred, W. P., Effect of dietary lipid on drugmetabolizing enzymes. Fed. Proc. Fed. Am. Soc. Exp. Biol. 35,2475
(1976).
11. Alvares, A. P., Anderson, K. E., Conney, A. H., and Kappas, A.,
Interactions between nutritional factors and drug biotransformations
in man. Proc. NatI. Acad. Sci. USA 73, 2501 (1976).
12. Gollan, J. L., Bateman,
composition
syndrome.
C., and Billing, B. H., Effect of dietary
on the unconjugated
hyperbilirubinaemia
of Gilbert’s
Gut 17, 335 (1976).
13. Aftergood,
L., and Alfin-Slater,
copherol interrelationships.
Lipids
R. B., Oral contraceptive-a-to-
9, 91(1974).
14. Lewis, 0., Nicholson,
G., Lance, P., and Paton, A., Aminopyrine
breath test in alcoholic
liver disease and in patients
on enzyme-inducing drugs. J. Clin. Pat hot. 30, 1040 (1977).
15. Scherrer,
S., Haldemann,
B., K#{252}pfer,
A., Reubi,
F., and Bircher,
J., Hepatic metabolism
of aminopyrine
in patients
with chronic renal
failure. Clin. Sci. Mol. Med. 54, 133 (1978).
16. Platzer, R., Galeazzi, R. L., Karlaganis, G., and Bircher, J., Rate
of drug metabolism
in man measured
by ‘4C02-breath
analysis. Eur.
J. Clin. Pharmacol. 14, 293 (1978).
17. Hart, P., Farrel, G. C., Cooksley, W. G. E., and Powell, L. W.,
Enhanced drug metabolism in cigarette smokers. Br. Med. J. iii, 147
(1976).
18. Kellermann,
G. H., and Luyten-Kellermann,
M., Antipyrine
metabolism in man. Life Sci. 23, 2485 (1978).
19. Pal, S. B., Progress in endocrinology
and metabolism.
6-Hydroxylation of cortisol and urinary 63-hydroxycortisol.
Metabolism
27, 1003 (1978).
20. Park, B. K., A direct radioimmunoassay
for 6/3-hydroxycortisol
in human urine. J. Steroid Biochem. 9, 963 (1978).
21. Kishida, S., and Fukushima, D. K., Radioimmunoassay
of 63hydroxycortisol
in human plasma and urine. Steroids
30, 741
(1977).
22. Marsh, C. A., Metabolism of D-glucuronolactone
in mammalian
systems. 2. Conversion of D-glucuronolactone
into D-glucaric acid by
tissue preparations.
Biochem.
J. 87,82 (1963).
23. Gangolli, S. D., Longland, R. C., and Shilling, W. H., A gas-liquid
chromatographic
method for the determination
of D-glucaric acid in
urine. Clin. Chim. Acta 50, 237 (1974).
24. Vesell, E. S., Passananti, G. T., and Lee, C. H., Impairment of drug
metabolism by disulfiram in man. Clin. Pharmacol. Ther. 12, 785
(197 1).
25. Huffman, D. H., Shoeman, D. W., and Azarnoti, D. L., Correlation
of the plasma elimination
of antipyrine
and the appearance of 4hydroxy antipyrine in the urine of man. Biochem. Pharnuzcol. 23, 197
(1974).
26. Lindgren, S., Collate, P., Norlander, B., and Sjoqvist, F., Gas
chromatographic
assessment of the reproducibility
of phenazone
plasma half-life in young healthy volunteers. Eur. J. Clin. Pharmacol.
7,381
(1974).
27. Deschamps,J.-P.,Miguet,J.-P.,Vuitton,D.,Joanne,C.,Allemand, H., Carayon,
P., Bechtel, P., and Gisselbrecht,
H., Le m#{233}tabolisme h#{233}patique
des m#{233}dicaments
au cours des cholestases intrah#{233}patiques chez l’homme.
Gastroenterol. Clin. Biol. 3,439 (1979).
28. Miguet, J.-P., Allemand,
H., Joanne, C., and Dhumeaux,
D., La
clairance de l’antipyrine:
Un test pour appr#{233}cier
Ia fonction hepatique
d’oxydation
des m#{233}dicaments.Etude au cours de La cirrhose.
Nouv.
Presse Med. 7,4209 (1978).
29. Dollery, C. T., Fraser, H. S., Mucklow, J. C., and Bulpitt, C. J.,
Contribution
of environmental
factors to variability in human drug
metabolism. Drug Metab. Rev. 9, 207 (1979).
30. Greenblatt, D. J., Franke, K., and Huffman, D. H., Impairment
of antipyrine clearance in humans by propranolol. Circulation 57,
1161 (1978).
31. Herz, R., Koelz, H. R., Haemmerli, U. P., Benes, I., and Blum, A.
L., Inhibition
of hepatic demethylation
of aminopyrine by oral contraceptive steroids in humans. Eur. J. Clin. Invest. 8, 27 (1978).
32. Poland, A., Smith, D., Kuntzman,
R., Jacobson, M., and Conney,
A. H., Effect of intensive occupational
exposure to DDT on phenylbutazone
and cortisol metabolism
in human subjects.
Clin. Pharmacol. Ther. 11,724 (1970).
33. Kolmodin-Hedman,
B., Decreased
plasma half-life of phenylbutazone
in workers exposed to chlorinated
pesticides.
Eur. J. Clin.
Pharmacol.
5, 195 (1973).
34. Ballinger, B., Browning, M., O’Malley, K., and Stevenson, I. H.,
Drug metabolizing
capacity
in states of drug dependence
and withdrawal. Br. J. Pharmacol.
45,638 (1972).
35. Davis, M., Simmons, C. J., Dordoni, B., and Williams, R., Urinary
D-glucaric acid excretion and plasma antipyrine kinetics during enzyme induction.
36. Marsh,
Br. J. Clin. Pharmacol.
C. A., and Carr, A. J., Changes
1, 253 (1974).
in enzyme
activity
related
CLINICAL CHEMISTRY, Vol.26,No. 6, 1980
697
to D-glucaric acid synthesis with age, pregnancy
Sci. 28, 209 (1965).
and malignancy.
Clin.
37. March, J., Turner,
W. J., Shanley, J., and Field, J., Values for
urinary excretion of D-glucaric acid by normal individuals. Clin.
Chem. 20, 1155(1974).
38. Hildebrandt,
A. G., Roots, I., Speck, M., Saalfrank, K., and
Kewitz, H., Evaluation
of in vivo parameters
of drug metabolising
enzyme
barbital
activity in man, after administration
or placebo. Eur. J. Clin. Pharmacol.
of clemastine,
8, 327 (1975).
pheno-
39. Herzberg, M., and Wiener, M. H., Increased D-glucaric acid excretion by jaundiced patients. Clin. Chem. 24, 1759 (1978).
40. Farrell, G. C., Cooksley, W. G. E., Hart, P., and Powell, L. W.,
Drug metabolism in liver disease. Identification of patients with impaired hepatic drug metabolism. Gastroenterology
75, 580 (1978).
41. Homeida, M., Karrar, Z. A., and Roberts, C. J. C., Drug metabolism in malnourished
children:
A study with antipyrine.
Arch. Dis.
Child. 54, 299 (1979).
42. Lewis, K. 0., Nicholson,
G., Lance, P., and Paton, A., Aminopyrine breath test in alcoholic liver disease and in patients
on enzymeinducing drugs. J. Clin. Pathol. 30, 1040 (1977).
43. Neal, E. A., Meffin, P. J., Gregory,
Enhanced
bioavailability
and decreased
patients
with cirrhosis.
Gastroenterology
44. Olsen,
acetylation
(1978).
P. B., and Blaschke,
T. F.,
clearance
of analgesics
in
77, 96 (1979).
H., and M#{248}rland,J., Ethanol-induced
increase in drug
in man and isolated rat liver cells. Br. Med. J. ii, 1260
45. Capel, I. D., Jenner,
M., Dorrell,
H. M., and Williams,
D. C., He-
patic function assessed (in rats) during chemotherapy
with some
anti-cancer drugs. Clin. Chem. 25, 1381 (1979).
46. Budillon,
G., Ayala, F., Carrella,
M., and Mazzacca, G., Urinary
excretion of D-glucaric acid, total glucuronic acid and total porphyrms
in porphyria cutanea tarda. Acta Hepato-Gastroenterol.
25, 267
(1978).
47. Greenwood,
R. H., Prunty, F. T. G., and Silver, J., Osteomalacia
after prolonged glutethimide
administration.
Br. Med. J. i, 643
(1973).
48. Whitfield, J. B., Moss, D. W., Neale, G., Orme, M., and Breckenridge, A., Changes in plasma-glutamyL transpeptidase
activity associated with alterations in drug metabolism in man. Br. Med. J. i,
316 (1973).
49. Bartels, H., Evert, W., Hauck, W., Petersen,
C., Putzki, H., and
Schulze, W., Significance
of increased serum gamma-glutamyl
transferase
activity during long-term anticonvulsive
treatment.
Clinical and experimental studies. Neuropaediatrie
6, 77 (1975).
50. Rosalki, S. B., Gamma-glutamyl
transpeptidase. Adv. Clin. Chem.
17,53
(1975).
51. Goldberg, D. M., and Martin, J. V., Role of y-glutamyl transpeptidase activity in the diagnosis of hepatobiliary disease. Digestion
12, 232 (1975).
52. Rosalki, S. B., Plasma enzyme changes and their interpretation
in patients receiving anticonvulsant
and enzyme-inducing
drugs. In
Anticonvulsant
Drugs and Enzyme
Induction,
A. Richens and F. P.
Woodford, Eds., Elsevier, Amsterdam, 1976, pp 27-35.
53. Martin, J. V., Gray, P. B., and Goldberg, D. M., Pitfalls in assay
and interpretation of serum gammaglutamyl transpeptidase
activity.
Clin.
Chim.
Acta
61,99
(1975).
54. Siest, G., Batt, A. M., and Galteau, M. M., Los examens biologiques t#{233}moins
indirects de l’activit#{233}
des enzymes du m#{233}tabolisme
des
m#{233}dicaments.
Ann. Biol. Clin. 35, 425 (1977).
55. Goldberg, D. M., Functional
tamyl
transpeptidase
progress. In Clinical
and clinical aspects of gamma-glu-
and its isoenzymes:
A critical review of recent
Enzymology,
J. C. Griffiths, Ed., Masson, New
York, NY, 1979, pp 123-154.
56. Goldberg, D. M., Structural, functional and clinical aspects of
‘y-glutamyl-transferase,
CRC Crit. Rev. Med. Lab. Sci. In press.
57. Hunter, J., Effects of enzyme induction on Vitamin D3 metabolism in man. In ref. 52, pp 77-85.
58. Latham, A. N., Millbank, L, Richens, A., and Rowe, D. J. F., Liver
enzyme inductlan by anticonvulsant
drugs and its relationship to
disturbed calcium and folic acid metabolism. J. Clin. Pharmacol.
13,
337 (1973).
59. Stamp, T. C. B., Round, J. M., Dupr#{233},
P., Flanagan, R. J., and
Twigg, C. A., Enzyme induction and calcium and Vitamin D metabolism during chronic anticonvulsant
therapy. In ref. 52, pp 87-97.
60. Kater, R. M. H., Tobon, F., and Iber, F. L., Increased rate of tol698
CLINICAL CHEMISTRY, Vol. 26, No. 6, 1980
butamide metabolism in alcoholic patients. J. Am. Med. Assoc. 207,
363 (1969).
61. Kater, R. M. H., Roggin, G., Tobon, F., Zieve, P., and Iber, F. L.,
Increased rate of clearance of drugs from the circulation of alcoholics.
Am. J. Med. Sci. 258, 35 (1969).
62. MacDonald, M. G., Robinson, D. S., Sylwester, D., and Jaffe, J.
J., The effects of phenobarbital,
chloral betaine, and glutethimide
administration
on warfarin plasma levels and hypoprothrombinemic
response in man. Clin. Pharmacol.
Ther. 10,80 (1969).
63. Jick, H., Smoking and clinical drug effects. Med. Clin. North Am.
58, 1143 (1974).
64. Jusko, W. J., Influence of cigarette smoking on drug metabolism
in man. Drug Metab. Rev. 9, 221 (1979).
65. Vestal, R. E., Wood, A. J. J., Branch, R. A., Shand, D.G., and
Wilkinson, G. R., Effects of age and cigarette smoking on propranolol
disposition. Clin. Pharmacol.
Ther. 26, 8 (1979).
66. Wood, A. J. J., Vestal, R. E., Wilkinson, G. R., Branch, R. A., and
Shand, D. G., Effect of aging and cigarette smoking on antipyrine and
indocyanine
green elimination.
Clin. Pharmacol.
Ther.
26, 16
(1979).
67. Alvares, A. P., Pantuck,
E. J., Anderson,
K. E., Kappas, A., and
Conney, A. H., Regulation
of drug metabolism
in man
mental factors. Drug Metab. Rev. 9, 185 (1979).
by environ-
68. Bickers, D. R., and Kappas, A., Human skin aryl hydrocarbon
hydroxylase. Induction by coal tar. J. Clin. Invest. 62, 1061 (1978).
69. Chapman, P. H., Rawlins, M. D., and Shuster, S., The activity of
aryl hydrocarbon
hydroxylase in adult human skin. Br. J. Clin.
Pharmacol.
7, 499 (1979).
70. Welch, R. M., Harrison, Y. E., Gommi, B. W., Poppers, P. J.,
Finster, M., and Conney, A. H., Stimulatory
effect of cigarette
smoking on the hydroxylation
of 3,4-benzpyrene
and the N-demethylation of 3-methyl-4-mono-methyl-amino-azo-benzene.
Clin.
Pharmacol.
Ther. 10, 100 (1969).
71. Vaught, J. B., Gurtoo, H. L., Parker, N. B., LeBoeuf, R., and
Doctor, G., Effects of smoking on benzo(a)pyrene
metabolism by
human placental microsomes. Cancer Res. 39, 3177 (1979).
72. Pelkonen, 0., Karki, N. T., Koivisto, M., Tuimala, R., and
Kauppila, A., Maternal cigarette smoking, placental aryl hydrocarbon
hydroxylase and neonatal size. Toxicol. Lett. 3, 331 (1979).
73. McLemore, T. L., Marton, R. R., Pickard, L. R., Springer, R. R.,
Wray, N. P., Toppell, K. L., Mattox, K. L., Guinn, G. A., Cantrell, E.
T., and Busbee, D. L., Analyses of aryl hydrocarbon
hydroxylase
activity in human
lung tissue, pulmonary
macrophages,
and blood
lymphocytes.
Cancer 41,2292 (1978).
74. Vaught, J. B., Gurtoo, H. L., Paigen, B., Minowada, J., and Sartori,
P., Comparison of benzo[a]pyrene metabolism by human peripheral
blood lymphocytes and monocytes. Cancer Lett. 5, 261(1978).
75. Gahmberg,
C. G., Sekki, A., Kosunen,
T. U., Holsti, L. R., and
M#{225}kelS,
0., Induction
of aryl hydrocarbon
hydroxylase
activity
and
pulmonary carcinoma. Int. J. Cancer 23, 302 (1979).
76. Schlede, E., Kuntzman, R., Haber, S., and Conney, A. H., Effect
of enzyme induction on the metabolism and tissue distribution
of
benzo[a]pyrene.
Cancer Res. 30, 2893 (1970).
77. Gelboin, H. V., Kinoshita, N., and Wiebel, F. J., Microsomal hydroxyl.ases: Induction and role in polycyclic hydrocarbon carcinogenesis and toxicity. Fed. Proc. Fed. Am. Soc. Exp. Biol. 31, 1298
(1972).
78. Garner, R. C., The role of epoxides in bioactivation and carcinogenesis. In Progress in Drug Metabolism,
1, J. W. Bridges and L. F.
Chasseaud, Eds., Wiley, London, 1976, pp 77-128.
79. Ames, B. N., Identifying
environmental
chemicals causing
mutations and cancer. Science 204, 587 (1979).
80. Martin, P. J., Martin, J. V., and Goldberg, D. M., ‘y-Glutamyl
transpeptidase,
triglycerides, and enzyme induction. Br. Med J. i, 17
(1975).
81. Martin, J. V., Hague, R. V., Martin, P. J., Cullen, D. R., and
Goldberg, D. M., The association between serum triglycerides and
gamma glutamyl transpeptidase
activity in diabetes mellitus. Clin.
Biochem. 9, 208 (1976).
82. Martin, J. V., Martin, P. J., and Goldberg, D. M., Enzyme induction as a possible cause of increased serum-triglycerides
after oral
contraceptives.
Lancet i, 1107 (1976).
83. Annoni, G., Barbi, G. L., and Ideo, G., Enzyme induction and
increased serum-triglyceride.
Lancet
i, 1414 (1976).
84. Cucuiani, M., Zdrenghea,
D., Pop, M., and Opincaru, A., Increased
serum gamma-glutamyltransferase
in hypertriglyceridemia:
Comparison with serum pseudocholinesterase.
Clin. Chim. Acta 71,419
(1976).
85. Goldberg,
D. M., Martin, J. V., and Martin, P. J., The association
between
serum gamma
glutamyl
transpeptidase
activity
and triglyceride concentration
in a constellation of clinical situations. In
Clinical
Enzymology,
J. C. Griffiths, Ed., Masson Publishing Inc.,
New York,
86. Goldberg,
transpeptidase
1979, pp 187-198.
D. M., Martin,
J. V., and Martin,
and enzyme induction:
A possible
synthesis. In Clinical
Enzymology
P. ,J., ‘y-Glutaniyl
relationship
with
Symposia,
2, A.
triglyceride
Burlina and L. Galzigna, Eds., Piccin Medical Books. Padua. In
press.
87. Yeung, C. Y., and Field, C. E., Phenobarbitone
therapy in neonatal hyperbilirubinaemia.
Lancet
ii, 135 (1969).
88. Wheiton, M. J., Krustev, L. P., and Billing, B. H., Reduction in
serum bilirubin by phenobarbital
in adult unconjugated
hyperbilirubinaemia. Is enzyme induction responsible? Am. J. Med. 45, 160
(1968).
89. Arias, I. M., Gartner, L. M., Cohen, M., Ben-Ezzer, J., and Levi,
A. J., Chronic
nonhemolytic
unconjugated
hyperbilirubinemia
with
glucuronyl transferase deficiency. Clinical, biochemical, pharmacologic and genetic evidence for heterogeneityl.
Am. J. Med. 47, 395
(1969).
90. Billing, B. H., and Black, M., The action of drugs on bilirubin
metabolism in man. Ann. N.Y. Acad. Sci. 179, 403 (1971).
91. Gollan, J. L., Huang, S. N., Billing, B., and Sherlock, S., Prolonged
survival in three brothers with severe type 2 Criggler-Najjar syndrome.
Ultrastructural
and metabolic studies. Gastroenterology
68, 1543
(1975).
92. Maurer, H. M., Wolff, J. A., Finster, M., Poppers, P. J., Pantuck,
E., Kuntzman, R., and Conney, A. H., Reduction in concentration of
total
serum-bilirubin
in offspring
of women
treated
with phenobar-
bitone during pregnancy. Lancet ii, 122 (1968).
93. Waltman, R., Bonura, F., Nigrin, G., and Pipat, C., Ethanol in
prevention of hyperbilirubinaemia
in the newborn. A controlled trial.
Lancet
ii, 1265 (1969).
94. Owens, D., and Sherlock, S., Diagnosis of Gilbert’s syndrome: role
of reduced caloric intake test. Br. Med. J. ii, 559 (1973).
95. Felsher, B. F., Carpio, N. M., and VanCouvering,
K., Effect of
fasting and phenobarbital on hepatic UDP-glucuronic acid formation
in the rat. J. Lab. Clin. Med. 93,414 (1979).
96. Lamy, J., Baglin, M. C., Ferrant, J. P., and Weill, J., Emploi de
Ia mesure de Ia ‘y-glutamyltranspeptidase
sSrique pour controler le
succes des cures de desintoxication anti-alcoolique. Clin. Chim. Acta
60, 102 (1975).
97. Lamy, J., Baglin, M. C., Weill, J., and Aron, E., Gamma glutamyl
transpeptidase
sSrique et alcoolisme. Diagnostic et contrSle du 8evrage. Nouv. Presse Med. 4, 487 (1975).
98. Wietholtz, H., and Colombo, J. P., Das Verhalten der ‘y-Glutamyl-transpeptidase
und anderer Leberenzyme,
im Plasma wahrend
der Alkohol-Entziehungskur.
Schweiz. Med. Wochenschr.
106, 981
(1976).
99. Homer, F., Kellen, J. A., Kingstone, B., Maharaj, N., and Malkin,
A., Dynamic changes of serum gamma-glutamyl transferase in chronic
alcoholism. Enzyme
24, 217 (1979).
100. Wadstein, J., and Skude, G., Changes in amylase, hepatic enzymes and bilirubin in serum upon initiation of alcohol abstinence.
Acta Med. Scand. 205 313 (1979).
101. Ellis, G., Worthy, E., and Goldberg, D. M., Lack of value of serum
y-glutamyl transferase in the diagnosis of hepatobiliary disease. Clin.
Biochem.
12, 142 (1979).
102. Goldberg, D. M., Selected aspects of microsomal enzyme induction. In Progress in Clinical Enzymology,
D. M. Goldberg and M.
Werner, Eds., Masson, New York, NY, 1980. In press.
CLINICAL CHEMISTRY, Vol.26,No. 6, 1980
699