* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Ticagrelor Protects the Heart Against Reperfusion Injury and
Survey
Document related concepts
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Transcript
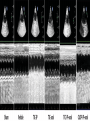
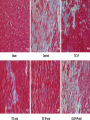
Ticagrelor Protects the Heart Against Reperfusion Injury and Improves Remodeling After Myocardial Infarction Yumei Ye, Gilad D. Birnbaum, Jose R. Perez-Polo, Manjyot K. Nanhwan, Sven Nylander, Yochai Birnbaum Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 Objective—In addition to P2Y12 receptor antagonism, ticagrelor inhibits adenosine cell uptake. Prior data show that 7-day pretreatment with ticagrelor limits infarct size. We explored the acute effects of ticagrelor and clopidogrel on infarct size and potential long-term effects on heart function. Approach and Results—Rats underwent 30-minute ischemia per 24-hour reperfusion. (1) Ticagrelor (10 or 30 mg/kg) or clopidogrel (12.5 mg/kg) was given via intraperitoneal injection 5 minutes before reperfusion. (2) Rats received ticagrelor acute (intraperitoneal; 30 mg/kg), chronic (oral; 300 mg/kg per day) for 4 weeks starting 1 day after reperfusion or the combination (acute+chronic). Another group received clopidogrel (intraperitoneal [12.5 mg/kg]+oral [62.5 mg/kg per day]) for 4 weeks. (1) Ticagrelor dose-dependently reduced infarct size, 10 mg/kg (31.5%±1.8%; P<0.001) and 30 mg/ kg (21.4%±2.6%; P<0.001) versus control (45.3±1.7%), whereas clopidogrel had no effect (42.4%±2.6%). Ticagrelor, but not clopidogrel, increased myocardial adenosine levels, increased phosphorylation of Akt, endothelial NO synthase, and extracellular-signal-regulated kinase 1/2 4 hours after reperfusion and decreased apoptosis. (2) After 4 weeks, left ventricular ejection fraction was reduced in the vehicle-treated group (44.8%±3.5%) versus sham (77.6%±0.9%). All ticagrelor treatments improved left ventricular ejection fraction, acute (69.5%±1.6%), chronic (69.2%±1.0%), and acute+chronic (76.3%±1.2%), whereas clopidogrel had no effect (37.4%±3.7%). Ticagrelor, but not clopidogrel, attenuated fibrosis and decreased collagen-III mRNA levels 4 weeks after ischemia/reperfusion. Ticagrelor, but not clopidogrel, attenuated the increase in proinflammatory tumor necrosis factor-α, interleukin-1β, and interleukin-18, and increased anti-inflammatory 15-epi-lipoxin-A4 levels. Conclusions—Ticagrelor, but not clopidogrel, administered just before reperfusion protects against reperfusion injury. This acute treatment or chronic ticagrelor for 4 weeks or their combination improved heart function, whereas clopidogrel, despite achieving a similar degree of platelet inhibition, had no effect. (Arterioscler Thromb Vasc Biol. 2015;35: 1805-1814. DOI: 10.1161/ATVBAHA.115.305655.) Key Words: adenosine ◼ aspirin ◼ platelet inhibitors ◼ prostaglandin-endoperoxide synthases ◼ reperfusion injury I n patients with acute coronary syndromes (ACSs), P2Y12 receptor antagonists reduce the incidence of cardiovascular events.1 A combination of aspirin with P2Y12 receptor antagonists is recommended by the guidelines for patients with ACS, including ST-segment–elevation myocardial infarction (STEMI).2–6 P2Y12 receptor antagonists block ADP-induced platelet aggregation, which is one of the main amplification pathways of platelet activation.1 The multicenter, randomized, placebo-controlled Platelet inhibition and patient Outcomes (PLATO) trial showed that added to aspirin, ticagrelor is associated with lower incidence of cardiovascular mortality, myocardial infarction, or stroke compared with clopidogrel in patients with ACS.7,8 Although the increased benefit was originally ascribed to better and more consistent platelet inhibition, ticagrelor, in addition to its P2Y12 receptor–blocking properties, inhibits interstitial adenosine cell reuptake, via inhibition of the equilibrative nucleoside transporter 1, thereby increasing extracellular adenosine levels.9–12 Adenosine is a major mediator of myocardial protection against ischemia–reperfusion injury and is essential for the myocardial protection by ischemic preconditioning and various pharmacological preconditioning.13,14 We have recently shown that 7-day oral pretreatment with ticagrelor, but not clopidogrel, limits myocardial infarct size (IS) in rats subjected to 30-minute coronary artery ligation followed by 24-hour reperfusion.15 Importantly, the degree of platelet inhibition was comparable between the clopidogrel and ticagrelor arms indicating a P2Y12- and platelet-independent cardioprotective effect of ticagrelor. Indeed, the protective effect was mediated by adenosine receptor activation with downstream phosphorylation of protein kinase B (Akt), endothelial NO synthase, and activation of cyclooxygenase-2 (COX2).15 Thus, the data support that in Received on: April 1, 2015; final version accepted on: May 18, 2015. From the Department of Biochemistry and Molecular Biology, University of Texas Medical Branch, Galveston (Y.Y., J.R.P.-P., M.K.N., Y.B.); Section of Cardiology, Baylor College of Medicine, Houston, TX (G.D.B., Y.B.); and AstraZeneca R&D, Mölndal, Sweden (S.N.). The online-only Data Supplement is available with this article at http://atvb.ahajournals.org/lookup/suppl/doi:10.1161/ATVBAHA.115.305655/-/DC1. Correspondence to Yochai Birnbaum, MD, One Baylor Plaza, MS: BCM620, Houston, TX 77030. E-mail [email protected] © 2015 American Heart Association, Inc. Arterioscler Thromb Vasc Biol is available at http://atvb.ahajournals.org 1805 DOI: 10.1161/ATVBAHA.115.305655 1806 Arterioscler Thromb Vasc Biol August 2015 Nonstandard Abbreviations and Acronyms ACS COX2 FGF-2 IL IS MIP-2 pPCI STEMI TNFα acute coronary syndrome cyclooxygenase-2 fibroblast growth factor-2 interleukin infarct size macrophage inflammatory protein-2 primary percutaneous coronary intervention ST-segment–elevation myocardial infarction tumor necrosis factor-α Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 addition to platelet inhibition, ticagrelor, but not clopidogrel, has protective effects against ischemia–reperfusion that may help explain the differences in clinical benefit in the PLATO trial.7,8 However, a recent multicenter, randomized, double-blind clinical trial did not show a clear clinical benefit in patients with STEMI receiving ticagrelor en route to the hospital versus in the catheterization laboratory.16 As the study was not powered for benefit on cardiovascular events, it is inconclusive about the hypothesis that administration of ticagrelor after onset of ischemia (in contrast to pretreatment just before reperfusion) can ameliorate reperfusion injury. In addition, as the median time difference between the prehospital and the in-hospital ticagrelor administration groups was only 31 minutes,16 it is plausible that ticagrelor absorption was insufficient and therefore, blood levels at the time of primary percutaneous coronary intervention (pPCI) were too low to protect the heart against reperfusion injury. Here, we asked (1) whether ticagrelor, administered intraperitoneal just before reperfusion, could limit IS in the rat and (2) whether ticagrelor can ameliorate adverse remodeling after infarction dependently or independently of its IS-limiting effect, and, thereby, improve heart function. Materials and Methods Materials and methods are available in the online-only Data Supplement. Results Ticagrelor, but Not Clopidogrel, Attenuates Reperfusion Injury Rats underwent 30-minute coronary artery ligation followed by reperfusion. Ticagrelor (10 or 30 mg/kg), clopidogrel (12.5 mg/kg), or vehicle was given intraperitoneally 5 minutes before reperfusion. Area at risk was assessed by blue dye and IS by 2,3,5-triphenyltetrazolium chloride staining 24 hours after reperfusion. One rat in the ticagrelor 30 mg/kg and 1 in the clopidogrel group died during surgery (before administration of the study drugs). Hemodynamic data are presented in Figure IA in the online-only Data Supplement (heart rate) and Figure IB (mean blood pressure). Body weight and the size of the area at risk were comparable among groups (Table). Ticagrelor dose-dependently reduced IS, expressed as percentage of the left ventricular weight (Table) or percentage of the area at risk (Figure 1A), whereas clopidogrel had no effect. IS (percentage of the area at risk) was significantly smaller in the ticagrelor 30 mg/kg than in the ticagrelor 10 mg/kg group (P=0.019). Ticagrelor plasma exposure 2 hours after reperfusion was 1.12±0.03 μmol/L in the ticagrelor 30 mg/kg group. Both ticagrelor (10 and 30 mg/kg) and clopidogrel significantly inhibited ADP-induced platelet aggregation compared with the control group (Figure 1B). The effect of ticagrelor 30 mg/kg was significantly greater than that of ticagrelor 10 mg/ kg. The difference in level of inhibition between the clopidogrel (64.2%) and ticagrelor 30 mg/kg (61.5%) groups was not significant, suggesting that both drugs were equally effective in inhibiting P2Y12 and platelet aggregation at these doses. In addition, 2 hours after reperfusion, tail vein bleeding time was equally prolonged by ticagrelor 30 mg/kg and clopidogrel (Figure 1C). Ticagrelor 30 mg/kg, but not clopidogrel, increased myocardial adenosine levels, a pharmacological marker of equilibrative nucleoside transporter 1 inhibition (Figure 1D). The reperfusion injury induced an increased phosphorylation (enzyme activity) of the prosurvival mediators Akt (P-Akt), endothelial NO synthase (P-eNOS), and extracellular-signal-regulated kinase (ERK) 1/2 (P-ERK 1/2) 2 hours after reperfusion in the border zone, whereas the total enzyme levels remained constant (Figure 2). Ticagrelor, but not clopidogrel, further increased the levels of P-Akt, P-endothelial NO synthase, and P-ERK 1/2 compared with the vehicle group (Figure 2). The reperfusion injury also induced an increase in the COX2 mRNA levels 2 hours after reperfusion, which remained unaffected by both ticagrelor and clopidogrel (Figure 3A). However, ticagrelor significantly increased, whereas clopidogrel tended to decrease (P=0.05) COX2-dependent 6-keto-PGF1α production compared with the vehicle group (Figure 3B). Twenty-four hours after reperfusion, apoptosis in the previously ischemic zone increased compared with the shamoperated animals (Figure 3C). Ticagrelor, but not clopidogrel, significantly decreased the number of apoptotic cells. Ticagrelor, but Not Clopidogrel, Improved Remodeling After Ischemia–Reperfusion Injury Next, we asked whether ticagrelor ameliorates adverse remodeling after infarction dependently or independently of Table. Body Weight, the Size of the Ischemic Area at Risk, and Infarct Size in the Control, TIC-Treated and CLOP-Treated Groups Control (n=8) P Value for the Differences TIC 10 mg/ TIC 30 mg/ CLOP 12.5 Among kg (n=8) kg (n=8) mg/kg (n=8) Groups Body weight, g 268±15 265±13 271±12 281±20 0.901 AR (percentage 31.6±0.6 of LV) 30.6±0.7 31.0±0.7 32.1±2.1 0.813 IS (percentage 14.3±0.6† of LV) 9.6±0.5* 6.6±0.8* 13.5±1.1† <0.001 AR indicates area at risk; CLOP, clopidogrel; IS, infarct size; LV, left ventricular; and TIC, ticagrelor. *P<0.002 vs control and †P<0.001 vs TIC 30 mg/kg. The P value for the difference in IS between TIC10 and TIC30 is 0.061. Ye et al Ticagrelor Protects Against Reperfusion Injury 1807 Figure 1. Acute intraperitoneal (IP) treatment with ticagrelor ([TIC] 10 and 30 mg/ kg) and clopidogrel ([CLOP] 12.5 mg/kg) 5 minutes before reperfusion. A, Infarct size (% of the ischemic area at risk 24 hours after reperfusion). *P<0.002 vs control; †P<0.02 vs TIC30. B, Platelet aggregation, induced by 15 µmol/L ADP in platelet-rich plasma 2 hours after reperfusion (n=4 per group). *P<0.001 vs control; †P<0.002 vs TIC30. C, Tail vein bleeding time (seconds) 2 hours after reperfusion (n=6 per group). *P<0.001 vs control. D, Myocardial adenosine levels 2 hours after reperfusion (n=6 per group). *P<0.001 vs control; †P<0.001 vs TIC30. Control; vehicle-treated, TIC10, TIC30, and CLOP12.5; Acute TIC (10 and 30 mg/kg) or CLOP (12.5 mg/kg) IP 5 minutes before reperfusion. P values shown in the graphs are for the overall differences among groups (ANOVA). Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 its IS-limiting effect. This question was addressed by comparing the effect of acute treatment with chronic treatment initiated the day after reperfusion on heart function 4 weeks after reperfusion. We also evaluated whether the combined acute+chronic treatment would be additive. At the end of the 4-week treatment period there were no significant differences in heart rate, body weight, and heart weight among the treatment groups (Table II in the Data Supplement). Echocardiographic data are presented in Figure 4 and Figure II in the online-only Data Supplement. Left ventricular internal diameter in diastole and systole significantly increased in the rats subjected to ischemia–reperfusion, whereas fractional shortening and left ventricular ejection fraction decreased. Acute or chronic (initiated the day after reperfusion) ticagrelor treatment normalized left ventricular internal diameter in diastole (Figure 4A). The effect of the combined acute+chronic ticagrelor treatment was comparable with that of acute and chronic alone. In contrast, clopidogrel (acute+chronic) had no effect at all. Ticagrelor, but not clopidogrel, also attenuated the increase in left ventricular internal diameter in systole but unlike data for left ventricular internal diameter in diastole with a significant additive effect of the combination (Figure 4B). Ticagrelor, but not clopidogrel, also improved the calculated parameters: left ventricular ejection fraction and fractional shortening (Figure 4C and 4D). For left ventricular ejection fraction and fractional shortening, there was a numeric additive effect of the combination that did not reach statistical significance. Ticagrelor plasma exposure after 7-day oral therapy was 1.43±0.05 and 4.21±0.09 μmol/L in the 150 and 300 mg/kg per day group, respectively. In parallel, ticagrelor significantly inhibited ADP-induced platelet aggregation by 53.5% and 69.7%, respectively. The level of inhibition, at 300 mg/kg per day, was equal to that of clopidogrel (70.9%; Figure 5A). Myocardial fibrosis increased in the rats that underwent ischemia–reperfusion injury when evaluated 4 weeks after reperfusion. All 3 ticagrelor regimes, but not clopidogrel, reduced fibrosis with significantly greater reduction with chronic versus acute treatment (P=0.002), and there was no additional effect of the combination (Figure 5B; Figure III in the online-only Data Supplement). Collagen III mRNA levels increased significantly in the group exposed to ischemia–reperfusion. All 3 ticagrelor regimes significantly decreased collagen III mRNA levels with no significant difference between treatments, whereas clopidogrel had no effect (Figure 5C). The mRNA levels of the proinflammatory mediators, tumor necrosis factor-α (TNFα), interleukin (IL)-1β, and IL-18, increased in the myocardial border zone 4 weeks after reperfusion (Figure 6A–6C). All 3 ticagrelor regimens significantly reduced the levels of all these mediators with no significant difference among treatments, whereas clopidogrel had no effect. Myocardial levels of the anti-inflammatory eicosanoid 15-epi-lipoxin A4 remained unchanged 4 weeks after reperfusion (7.3±0.7 versus 7.6±0.3 pg/µg). Chronic (17.2±0.5 pg/µg; P<0.001) or combined acute+chronic ticagrelor treatment (17.4±0.7 pg/µg; P<0.001) significantly increased 15-epilipoxin A4 levels, whereas clopidogrel (7.3±0.6 pg/µg; P=1.0) and acute ticagrelor (8.3±0.7 pg/µg) had no effect. Myocardial macrophage inflammatory protein-2 (MIP-2; Figure 6D) and fibroblast growth factor-2 (FGF-2; Figure 6E) levels increased 4 weeks after reperfusion. Acute ticagrelor treatment tended to reduce MIP-2 levels (P=0.93) and significantly reduced FGF-2 levels (P=0.02). Chronic ticagrelor significantly reduced MIP-2 and FGF-2 levels, with no significant additional effect of the combination. Clopidogrel had no effect on MIP-2 levels (P=1.00 versus vehicle), but completely normalized FGF-2 levels (P=1.0 versus the sham group). Discussion The main findings of the present study are that acute ticagrelor treatment just before reperfusion increased myocardial adenosine levels, augmented the phosphorylation of the prosurvival kinases Akt and ERK 1/2 and endothelial NO synthase, and limited myocardial IS. This cardioprotective effect 1808 Arterioscler Thromb Vasc Biol August 2015 Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 Figure 2. Ischemic zone heart tissue enzyme protein expression 2 hours after reperfusion. A, Samples of immunoblots and densitometric analysis of P-Akt (B), total Akt (C), P-endothelial NO synthase (eNOS; D), total eNOS (E), P-extracellular-signal-regulated kinase (ERK) 1/2 (F), and total ERK 1/2 (G; n=4 per group). *P<0.022 vs control; †P<0.001 vs ticagrelor (TIC) 30. Sham, sham-operated; control, vehicletreated; TIC30; and clopidogrel (CLOP) 12.5; acute TIC (30 mg/kg) or CLOP (12.5 mg/kg) intraperitoneal 5 minutes before reperfusion. P values shown in the graphs are for the overall differences among groups (ANOVA). of a single acute dose of ticagrelor translated into an improved heart function and reduced fibrosis and collagen III expression 4 weeks later. Similar effects on heart function fibrosis and collagen III, along with attenuation of the increase in proinflammatory mediators, was seen with chronic oral ticagrelor therapy, started the day after reperfusion, and with the combination of acute and chronic oral treatment. In contrast, clopidogrel, despite achieving similar degree of inhibition of platelet aggregation, did not display any acute cardioprotective effect or improved long-term heart function. The mean maximal ticagrelor plasma exposure (Cmax) reported in patients after 4 weeks of treatment with the standard dose of 90 mg BID is 1.4 μmol/L with a SD of 0.7 μmol/L.15,17 Thus, the experiments reported here were conducted at clinically relevant ticagrelor plasma exposure levels (1.12 and 1.43 μmol/L in 30 mg/kg IP and 150 mg/kg per day oral), except for a slightly supratherapeutic exposure after 300 mg/kg per day oral (4.21 μmol/L). Considering the lack of effect seen for clopidogrel, dosed to a similar platelet inhibition, suggests that the protective effects seen with ticagrelor are independent of platelet and P2Y12 inhibition. The current data confirm our previous findings that ticagrelor, but not clopidogrel, increases myocardial adenosine levels.15 Higher plasma adenosine levels have also been documented in patients with ACS treated with ticagrelor than in those receiving clopidogrel.10 Adenosine mediates myocardial Ye et al Ticagrelor Protects Against Reperfusion Injury 1809 Figure 3. Acute intraperitoneal (IP) treatment with ticagrelor ([TIC] 30 mg/kg) and clopidogrel ([CLOP] 12.5 mg/kg) 5 minutes before reperfusion. A, Ischemic zone heart tissue cyclooxygenase-2 (COX2) mRNA levels 2 hours after reperfusion (n=4 per group). *P<0.002 vs vehicle; †P<0.001 vs TIC30. B, Ischemic zone heart tissue COX2 activity 2 hours after reperfusion (n=4 per group). *P<0.05 vs vehicle; †P<0.002 vs TIC30. C, Ischemic zone heart tissue apoptosis 24 hours after reperfusion (n=5 per group). *P<0.001 vs control; †P<0.001 vs TIC30. Sham, sham-operated; control, vehicle-treated; TIC30; and CLOP12.5; acute TIC (30 mg/kg) or CLOP (12.5 mg/kg) IP 5 minutes before reperfusion. P values shown in the graphs are for the overall differences among groups (ANOVA). Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 protection by ischemic preconditioning and various pharmacological preconditioning.13,14 We have recently shown that the protective effects of ticagrelor pretreatment against ischemia– reperfusion injury are dependent on adenosine receptor activation.15 In addition to its role in preconditioning, adenosine is also essential for the cardioprotective effect of postconditioning.14 Two large multicenter studies (the Acute Myocardial Infarction Study of Adenosine [AMISTAD] I and AMISTAD II) demonstrated that high-dose intravenous infusion of adenosine, started before reperfusion, significantly reduced IS in patients with anterior wall STEMI.18,19 However, the primary end point of new congestive heart failure beginning >24 hours after randomization, the first rehospitalization for heart failure, or death from any cause within 6 months was not reduced by adenosine therapy in the AMISTAD-II trial,19 whereas there was a trend toward increasing adverse clinical end points with adenosine in the smaller AMISTAD-I trial.18 In AMISTAD-II intravenous administration of adenosine was associated with an increased rate of hypotension19 that may explain the dissociation between the favorable effect on IS and the lack of Figure 4. Heart function 4 weeks after reperfusion. A, Left ventricular internal diameter in diastole (LVIDd). B, LV internal diameter in systole (LVIDs). C, Fractional shortening (FS). D, LV ejection fraction (LVEF; n=7–8 per group; Table II in the online-only Data Supplement). *P<0.001 vs control with ischemia–reperfusion; †P<0.04 vs ticagrelor (TIC)-intraperitoneal (IP)+oral. Sham, sham-operated; control, vehicletreated; TIC-IP, acute TIC (30 mg/kg) IP 5 minutes before reperfusion; TIC-oral, oral TIC (300 mg/kg per day) for 4 weeks, initiated the day after reperfusion; TIC-IP+oral, TIC-acute+TIC-chronic; clopidogrel (CLOP)-IP+oral, CLOP acute+chronic for 4 weeks (12.5 mg/kg IP+62.5 mg/kg per day oral). P values shown in the graphs are for the overall differences among groups (ANOVA). 1810 Arterioscler Thromb Vasc Biol August 2015 Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 Figure 5. A, Platelet aggregation, induced by 15 µmol/L ADP in platelet-rich plasma. *P<0.001 vs control (n=4 per group). Control; vehicle, ticagrelor (TIC) 300, and clopidogrel (CLOP) 62.5; oral TIC (300 mg/kg per day) or CLOP (62.5 mg/kg per day) for 7 days. B, Myocardial fibrosis 4 weeks after reperfusion. *P<0.001 vs control; †P<0.002 vs TIC intraperitoneal (IP)+oral (n=7 per group; Table II in the online-only Data Supplement). C, Myocardial collagen III mRNA expression 4 weeks after reperfusion. *P<0.001 vs vehicle; †P<0.001 vs TIC IP+oral (n=4–5 per group). P values shown in the graphs are for the overall differences among groups (ANOVA). benefit concerning clinical outcomes. Nevertheless, in a retrospective analysis of patients who achieved reperfusion within 3.17 hours of onset of symptoms, adenosine, compared with placebo, significantly reduced mortality.20 Two recent clinical trials did not show to demonstrate beneficial effects of intracoronary adenosine before reperfusion on myocardial IS.21,22 A likely explanation is that the short half-life of adenosine in the circulation makes intracoronary bolus injections ineffective.14 In contrast to intravenous adenosine, ticagrelor increases adenosine levels at sites with increased production by preventing its reuptake. The effect should be sustained as long as sufficient ticagrelor exposure is present.9–12 In a previous study we showed that 7-day pretreatment with ticagrelor upregulated COX2 expression and activity.15 The protective effect of ticagrelor pretreatment was blocked with specific COX2 inhibitors, as well as aspirin.15 In the present study, acute ticagrelor treatment just before reperfusion did not increase COX2 mRNA levels 2 hours after reperfusion. The role of COX2 in mediating the second window of protection by ischemic preconditioning and various pharmacological agents is well established.23 Yet, the significance of COX2 in mediating the protective effects of postconditioning against reperfusion injury is less certain.23,24 Here, we show that although COX2 mRNA levels were not changed by ticagrelor and clopidogrel 2 hours after reperfusion, ticagrelor significantly increased COX2 activity. Statins induce adenosine receptor–dependent COX2 activation via S-nitrosylation.25,26 This mode of COX2 activation is probably a prompt response, before COX2 mRNA and protein expression are increased. It remains to be explored whether ticagrelor-induced COX2 activation, described here, works via the same or similar mechanism. Unlike ticagrelor, acute clopidogrel treatment failed to limit IS, which further supports the lack of cardioprotective effect of clopidogrel in our previous study evaluating 7-day pretreatment.15 Yang et al27 reported that 2-day pretreatment with clopidogrel and intravenous cangrelor, started before reperfusion, reduced IS in rabbits subjected to 30 minutes of ischemia per 3 hours of reperfusion. However, clopidogrel had no effect when administered only 24 hours before ischemia. They report that the protective effect was independent of the antiplatelet effects of the drugs, but was attenuated by adenosine receptor blockers and phosphoinositide 3-kinase/ Akt inhibitors.27 The differences between the study by Yang et al and our studies are unclear. Cangrelor and clopidogrel, in contrast to ticagrelor, do not inhibit cellular adenosine uptake via equilibrative nucleoside transporter 1.9 Differences between species (rats versus rabbits), dose, or the length of reperfusion (3 versus 24 hours) may be the explanation. Wang et al,28 however, compared the effect of intravenous ticagrelor and clopidogrel, added to intravenous thrombolytic therapy with tissue-type plasminogen activator in dogs with electrolytic injury–induced intracoronary thrombus. They found that ticagrelor, but not clopidogrel, limits myocardial IS. As both ticagrelor and clopidogrel were dosed to complete inhibition of ex vivo ADP-induced aggregation, as in our study, they also raised the possibility that the beneficial effect could be mediated by mechanisms independent of platelet inhibition, including inhibition of vascular P2Y12 receptors or via adenosine uptake inhibition.28 Patti et al29 compared the effect of a 600- versus a 300-mg loading dose of clopidogrel on IS in patients who underwent pPCI for STEMI. The high dose of clopidogrel was associated with lower levels of creatine kinase MB and troponin-I, better TIMI (thrombolysis in myocardial infarction) flow grade, and improved left ventricular ejection fraction at discharge. However, these results may be attributed to better and more rapid platelet inhibition. In our model, myocardial infarction is induced by mechanical ligation of the coronary artery; and hence, the role of platelet inhibition is probably less significant. Importantly, we found that the acute cardioprotective effect against reperfusion injury mediated by ticagrelor translated into improved heart function 4 weeks later. Surprisingly, Ye et al Ticagrelor Protects Against Reperfusion Injury 1811 Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 Figure 6. Acute intraperitoneal (IP) treatment with ticagrelor ([TIC] 30 mg/kg) 5 minutes before reperfusion, oral TIC (300 mg/kg per day) for 4 weeks initiated the day after reperfusion, TIC IP+oral or clopidogrel (CLOP) IP+oral (12.5 mg/kg+62.5 mg/kg per day). Myocardial mRNA levels of tumor necrosis factor (TNF)-α (A), interleukin (IL)-1β (B), and IL-18 (C), myocardial protein levels of macrophage inflammatory protein 2 (MIP-2; D), and fibroblast growth factor-2 (FGF-2; E) 4 weeks after reperfusion. *P<0.015 vs control; †P<0.002 vs TIC IP+oral (n=4 per group). Sham, sham-operated; control, vehicle-treated; TIC-IP, acute TIC (30 mg/kg) IP 5 minutes before reperfusion; TIC-oral, chronic oral TIC (300 mg/kg per day) for 4 weeks, initiated the day after reperfusion; TIC-IP+oral, TIC-acute+TIC-chronic; CLOPIP+oral, CLOP IP+oral for 4 weeks (12.5 mg/kg+62.5 mg/kg per day). P values shown in the graphs are for the overall differences among groups (ANOVA). a similar beneficial effect on heart function was seen with chronic treatment initiated 1 day after reperfusion, thus independent of its IS-limiting effect, with minor additive effect when acute and chronic treatments were combined. In contrast, Yang et al27 reported that the protective effect of cangrelor was lost when the drug infusion started 10 minutes after reperfusion compared with drug infusion before reperfusion. As differences in angiographic findings, secondary to greater platelet inhibition, cannot explain the differences in clinical outcomes between ticagrelor and clopidogrel in the PLATO trial,30,31 our study may provide an alternative explanation. In addition to its antiplatelet effects, ticagrelor provides cardioprotection against ischemia–reperfusion injury and improve long-term remodeling after infarction. The recent Administration of Ticagrelor in the Cath Laboratory or in the Ambulance for New ST-Elevation Myocardial Infarction to Open the Coronary Artery (ATLANTIC) trial failed to show a clear clinical benefit in patients with STEMI undergoing pPCI and receiving ticagrelor en route to the hospital versus in the catheterization laboratory.16 The myocardial reperfusion in angioplasty of patients with STEMI loaded with ticagrelor or clopidogrel (MICAMI-TICLO) trial31 showed that ticagrelor loading before pPCI for STEMI did not improve angiographic findings or ST-segment elevation resolution, as compared with clopidogrel loading. In both trials, the time from drug loading to intervention was short (31–43 minutes).16,31 It is plausible that the time between dose and pPCI in the in-ambulance study arm was insufficient to allow significant ticagrelor exposure at the time of pPCI to induce adenosine-dependent protection against the acute reperfusion injury, as shown in the current rat study. The MICAMI-TICLO trial was relatively small and did not follow the patients for clinical outcomes.31 However, both groups in the ATLANTIC trial received chronic ticagrelor treatment; hence, both groups benefited from the long-term effects of the drug. Therefore, no between-group difference could be seen.16 Considering our data, which show a benefit of both acute and chronic treatments, and these clinical data, which have not been able to make the comparison, the relative benefit from acute and chronic ticagrelor treatments in patients remains to be defined. A single dose of ticagrelor, administered intraperitoneally before reperfusion, reduced IS, and as a consequence, inflammation, fibrosis, and remodeling 4 weeks after infarction. In contrast, the effect of the 4-week chronic treatment cannot be attributed to direct protection against reperfusion injury, as at the time therapy started, cell death because of ischemia and reperfusion was completed. It is thus plausible that ticagrelor, via its adenosine augmentation effects, ameliorated inflammation and attenuated adverse remodeling. It is clear that these favorable effects are independent of the antiplatelet properties 1812 Arterioscler Thromb Vasc Biol August 2015 Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 of ticagrelor, as clopidogrel had no effect on inflammation, fibrosis, and remodeling despite achieving a similar degree of platelet aggregation inhibition. TNFα,32,33 IL-1β,33,34 and IL-1834–36 are involved in myocardial ischemia–reperfusion injury and remodeling. Thus, the reduction of these proinflammatory mediators induced by ticagrelor may explain the favorable effects on fibrosis and remodeling. It has been reported that activation of the adenosine A1 receptors attenuates the prohypertrophic effects of TNFα on cardiomyocytes,37 and that adenosine suppresses TNFα expression.38 Ticagrelor increased myocardial levels of 15-epi-lipoxin A4, an eicosanoid mediator with potent anti-inflammation effects,15 that has been shown to inhibit TNFα and IL1β secretion and to attenuate the effects of TNFα.39–41 Future studies are needed to explore whether the effects of ticagrelor on the expression of the proinflammatory mediators are dependent on the upregulation of 15-epi-lipoxin A4 levels. As the synthesis of 15-epilipoxin A4 is dependent on COX2, these anti-inflammatory effects of ticagrelor might be COX2 dependent and could be potentially inhibited by high-dose aspirin.15 MIP-2 is a proinflammatory chemokine that increases after ischemia–reperfusion injury and infarction and may be involved in adverse cardiac remodeling.42,43 Here, we show that ticagrelor, but not clopidogrel, attenuates the increase in MIP-2 4 weeks after myocardial infarction. However, FGF-2 induces cardioprotection,44 has a role as a chemotactic factor for stem cell homing after myocardial injury,45 induces angiogenesis,46,47 and improves remodeling after myocardial infarction in the rat.48–50 The significance of the ticagrelorinduced attenuation and clopidogrel-induced normalization of the increase in FGF-2 levels 4 weeks after infarction is unclear. Although ticagrelor attenuated adverse remodeling after infarction, clopidogrel had no effect. It is possible that 4 weeks after infarction, healing was better in the ticagrelortreated animals and therefore, the stimulus for FGF-2 release was decreased. In contrast, as clopidogrel had no effect on adverse remodeling, its normalization of the FGF-2 levels may have adverse effects. Further studies are needed to clarify the effects of these drugs on FGF-2 release over time after infarction and their pathophysiologic significance. Here, we are showing that acute administration of ticagrelor before reperfusion reduces myocardial IS. The challenge in the clinical setting is how to get sufficient drug exposure before pPCI, as the average time between first medical encounter and reperfusion is relatively short. Parenteral (intravenous) or chewable formulation should probably be developed for this purpose. This may be less a problem in non–ST elevation ACSs, as the time from first medical encounter to PCI is longer. One may question the role of chronic treatment if the initial acute effects could be achieved by reaching adequate drug exposure at the time of reperfusion. In our models, the only parameter that showed greater improvement with the acute and chronic ticagrelor treatments as compared with acute treatment alone or chronic treatment alone was left ventricular internal diameter in systole. However, the animals in our models do not have atherosclerosis and coronary occlusion was induced by mechanical ligation of the artery. Thus, the role of platelet aggregation in mediating acute reperfusion injury, and over the long run, new coronary lesions, including acute thrombotic occlusion of coronary arteries, is much less important in our model than in the clinical setting. Thus, in the current model, we do not compare the effects of outcomes of chronic antiplatelet inhibition with ticagrelor versus clopidogrel, but only study acute cardioprotection and subsequent effects on remodeling. Importantly, our experiments indicate that even if optimal ticagrelor exposure cannot be achieved at the time of pPCI, oral therapy started after reperfusion could still improve heart function. This effect on remodeling after infarction should be further studied. It is plausible that the effects of chronic exposure on remodeling after infarction (along with better and more reliable antiplatelet effects) are the explanation of the superiority of ticagrelor over clopidogrel in the PLATO trial. Based on the results of the current study, we have initiated a clinical trial comparing the effects of ticagrelor and another P2Y12 receptor antagonist on myocardial IS in patients with first anterior STEMI undergoing pPCI. Further studies are probably needed to search for alternative mode of administration (chewable, intravenous, or even higher loading dose) to achieve effective ticagrelor blood levels by the time reperfusion occurs. Additional studies are needed to evaluate the effects of ticagrelor treatment on cardiac remodeling and heart function after myocardial infarction. In addition to ticagrelor, 2 other antiplatelet agents, dipyridamole51,52 and cilostazol,53 also prevent the reuptake of adenosine and have been shown to limit myocardial IS. However, both also inhibit phosphodiesterase-III, increasing intracellular levels of cAMP making comparisons difficult. Also in addition to ticagrelor, the other P2Y12 antagonists, clopidogrel and prasugrel, can attenuate platelet–leukocyte interactions and modulate inflammatory response.54 Yet, in our model, ticagrelor, but not clopidogrel, limited IS and improved postinfarction remodeling, despite similar platelet inhibition by both drugs. No data are available for prasugrel in this regard. Limitations The number of animals in each group is small (especially when compared with the number of patients in each group in clinical trials). However, these sample sizes are commonly used in animal studies and are based on experience and sample size calculation. The animals used in bench research are more homogeneous (age, sex, weight, and genetic background) than the typical patient populations and they are exposed to exactly same insult (ischemic time, reperfusion time, etc). The results of the current study should be verified in other animal models and in clinical trials before they are implemented for patient care. In conclusion, ticagrelor, administered just before reperfusion, provided acute cardioprotection and limited IS. This acute cardioprotective effect translates into long-term improved heart function. In addition, also chronic ticagrelor treatment initiated the day after reperfusion improved heart function independently of the acute IS-limiting effect. Clopidogrel, despite achieving similar degree of platelet inhibition, had no acute or chronic cardioprotective effects. The results should be confirmed in appropriate clinical studies, as Ye et al Ticagrelor Protects Against Reperfusion Injury 1813 frequently, positive findings from animal models are not translated to clinical benefits in patients.55 Sources of Funding This study was supported by an Investigator Initiated grant from AstraZeneca. Partial support was provided by the John S. Dunn Foundation. Disclosures Y. Ye and Dr Birnbaum received research grants from Astra Zeneca, BMS, Boehringer Ingelheim. S. Nylander is an employee of Astra Zeneca. The other authors report no conflicts. References Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 1. Eikelboom JW, Hirsh J, Spencer FA, Baglin TP, Weitz JI. Antiplatelet drugs: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;141(2 Suppl):e89S–119S. doi: 10.1378/ chest.11-2293. 2. Hamm CW, Bassand JP, Agewall S, et al; ESC Committee for Practice Guidelines. ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: The Task Force for the management of acute coronary syndromes (ACS) in patients presenting without persistent ST-segment elevation of the European Society of Cardiology (ESC). Eur Heart J. 2011;32:2999–3054. doi: 10.1093/eurheartj/ehr236. 3. Jneid H, Anderson JL, Wright RS, et al. 2012 ACCF/AHA focused update of the guideline for the management of patients with unstable angina/ non-ST-elevation myocardial infarction (updating the 2007 guideline and replacing the 2011 focused update): a report of the American College Of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2012;126:875–910 4. Steg PG, James SK, Atar D, et al. ESC guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur Heart J. 2012;33:2569–2619. 5.Thygesen K, Alpert JS, Jaffe AS, et al; Joint ESC/ACCF/AHA/WHF Task Force for Universal Definition of Myocardial Infarction; Authors/ Task Force Members Chairpersons; Biomarker Subcommittee; ECG Subcommittee; Imaging Subcommittee; Classification Subcommittee; Intervention Subcommittee; Trials & Registries Subcommittee; Trials & Registries Subcommittee; Trials & Registries Subcommittee; Trials & Registries Subcommittee; ESC Committee for Practice Guidelines (CPG); Document Reviewers. Third universal definition of myocardial infarction. J Am Coll Cardiol. 2012;60:1581–1598. doi: 10.1016/j.jacc.2012.08.001. 6.Vandvik PO, Lincoff AM, Gore JM, Gutterman DD, Sonnenberg FA, Alonso-Coello P, Akl EA, Lansberg MG, Guyatt GH, Spencer FA; American College of Chest Physicians. Primary and secondary prevention of cardiovascular disease: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians EvidenceBased Clinical Practice Guidelines. Chest. 2012;141(2 Suppl):e637S– e668S. doi: 10.1378/chest.11-2306. 7. Wallentin L, Becker RC, Budaj A, et al; PLATO Investigators. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N Engl J Med. 2009;361:1045–1057. doi: 10.1056/NEJMoa0904327. 8.Cannon CP, Harrington RA, James S, et al; PLATelet inhibition and patient Outcomes Investigators. Comparison of ticagrelor with clopidogrel in patients with a planned invasive strategy for acute coronary syndromes (PLATO): a randomised double-blind study. Lancet. 2010;375:283–293. doi: 10.1016/S0140-6736(09)62191-7. 9.Armstrong D, Summers C, Ewart L, Nylander S, Sidaway JE, van Giezen JJ. Characterization of the adenosine pharmacology of ticagrelor reveals therapeutically relevant inhibition of equilibrative nucleoside transporter 1. J Cardiovasc Pharmacol Ther. 2014;19:209–219. doi: 10.1177/1074248413511693. 10. Bonello L, Laine M, Kipson N, Mancini J, Helal O, Fromonot J, Gariboldi V, Condo J, Thuny F, Frere C, Camoin-Jau L, Paganelli F, Dignat-George F, Guieu R. Ticagrelor increases adenosine plasma concentration in patients with an acute coronary syndrome. J Am Coll Cardiol. 2014;63:872–877. doi: 10.1016/j.jacc.2013.09.067. 11. van Giezen JJ, Sidaway J, Glaves P, Kirk I, Björkman JA. Ticagrelor inhibits adenosine uptake in vitro and enhances adenosine-mediated hyperemia responses in a canine model. J Cardiovasc Pharmacol Ther. 2012;17:164– 172. doi: 10.1177/1074248411410883. 12.Cattaneo M, Schulz R, Nylander S. Adenosine-mediated effects of ticagrelor: evidence and potential clinical relevance. J Am Coll Cardiol. 2014;63:2503–2509. doi: 10.1016/j.jacc.2014.03.031. 13. Kitakaze M, Minamino T, Node K, Takashima S, Funaya H, Kuzuya T, Hori M. Adenosine and cardioprotection in the diseased heart. Jpn Circ J. 1999;63:231–243. 14.Kloner RA. Current state of clinical translation of cardioprotective agents for acute myocardial infarction. Circ Res. 2013;113:451–463. doi: 10.1161/CIRCRESAHA.112.300627. 15. Nanhwan MK, Ling S, Kodakandla M, Nylander S, Ye Y, Birnbaum Y. Chronic treatment with ticagrelor limits myocardial infarct size: an adenosine and cyclooxygenase-2-dependent effect. Arterioscler Thromb Vasc Biol. 2014;34:2078–2085. doi: 10.1161/ATVBAHA.114.304002. 16. Montalescot G, van ‘t Hof AW. Prehospital ticagrelor in ST-segment elevation myocardial infarction. N Engl J Med. 2014;371:2339. doi: 10.1056/ NEJMc1412729. 17. Storey RF, Husted S, Harrington RA, Heptinstall S, Wilcox RG, Peters G, Wickens M, Emanuelsson H, Gurbel P, Grande P, Cannon CP. Inhibition of platelet aggregation by AZD6140, a reversible oral P2Y12 receptor antagonist, compared with clopidogrel in patients with acute coronary syndromes. J Am Coll Cardiol. 2007;50:1852–1856. doi: 10.1016/j. jacc.2007.07.058. 18.Mahaffey KW, Puma JA, Barbagelata NA, DiCarli MF, Leesar MA, Browne KF, Eisenberg PR, Bolli R, Casas AC, Molina-Viamonte V, Orlandi C, Blevins R, Gibbons RJ, Califf RM, Granger CB. Adenosine as an adjunct to thrombolytic therapy for acute myocardial infarction: results of a multicenter, randomized, placebo-controlled trial: the Acute Myocardial Infarction STudy of ADenosine (AMISTAD) trial. J Am Coll Cardiol. 1999;34:1711–1720. 19.Ross AM, Gibbons RJ, Stone GW, Kloner RA, Alexander RW; AMISTAD-II Investigators. A randomized, double-blinded, placebocontrolled multicenter trial of adenosine as an adjunct to reperfusion in the treatment of acute myocardial infarction (AMISTAD-II). J Am Coll Cardiol. 2005;45:1775–1780. doi: 10.1016/j.jacc.2005.02.061. 20. Kloner RA, Forman MB, Gibbons RJ, Ross AM, Alexander RW, Stone GW. Impact of time to therapy and reperfusion modality on the efficacy of adenosine in acute myocardial infarction: the AMISTAD-2 trial. Eur Heart J. 2006;27:2400–2405. doi: 10.1093/eurheartj/ehl094. 21. Desmet W, Bogaert J, Dubois C, Sinnaeve P, Adriaenssens T, Pappas C, Ganame J, Dymarkowski S, Janssens S, Belmans A, Van de Werf F. Highdose intracoronary adenosine for myocardial salvage in patients with acute ST-segment elevation myocardial infarction. Eur Heart J. 2011;32:867– 877. doi: 10.1093/eurheartj/ehq492. 22. Fokkema ML, Vlaar PJ, Vogelzang M, Gu YL, Kampinga MA, de Smet BJ, Jessurun GA, Anthonio RL, van den Heuvel AF, Tan ES, Zijlstra F. Effect of high-dose intracoronary adenosine administration during primary percutaneous coronary intervention in acute myocardial infarction: a randomized controlled trial. Circ Cardiovasc Interv. 2009;2:323–329. doi: 10.1161/CIRCINTERVENTIONS.109.858977.109.858977. 23. Hausenloy DJ, Yellon DM. Survival kinases in ischemic preconditioning and postconditioning. Cardiovasc Res. 2006;70:240–253. doi: 10.1016/j. cardiores.2006.01.017. 24. Penna C, Mancardi D, Tullio F, Pagliaro P. Postconditioning and intermittent bradykinin induced cardioprotection require cyclooxygenase activation and prostacyclin release during reperfusion. Basic Res Cardiol. 2008;103:368–377. doi: 10.1007/s00395-007-0695-7. 25.Kim SF, Huri DA, Snyder SH. Inducible nitric oxide synthase binds, S-nitrosylates, and activates cyclooxygenase-2. Science. 2005;310:1966– 1970. doi: 10.1126/science.1119407. 26. Atar S, Ye Y, Lin Y, Freeberg SY, Nishi SP, Rosanio S, Huang MH, Uretsky BF, Perez-Polo JR, Birnbaum Y. Atorvastatin-induced cardioprotection is mediated by increasing inducible nitric oxide synthase and consequent S-nitrosylation of cyclooxygenase-2. Am J Physiol Heart Circ Physiol. 2006;290:H1960–H1968. doi: 10.1152/ajpheart.01137.2005. 27. Yang XM, Liu Y, Cui L, Yang X, Liu Y, Tandon N, Kambayashi J, Downey JM, Cohen MV. Platelet P2Y₁₂ blockers confer direct postconditioninglike protection in reperfused rabbit hearts. J Cardiovasc Pharmacol Ther. 2013;18:251–262. doi: 10.1177/1074248412467692. 28. Wang K, Zhou X, Huang Y, Khalil M, Wiktor D, van Giezen JJ, Penn MS. Adjunctive treatment with ticagrelor, but not clopidogrel, added to tPA enables sustained coronary artery recanalisation with recovery of myocardium perfusion in a canine coronary thrombosis model. Thromb Haemost. 2010;104:609–617. doi: 10.1160/TH09-12-0823. 1814 Arterioscler Thromb Vasc Biol August 2015 Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 29.Patti G, Bárczi G, Orlic D, Mangiacapra F, Colonna G, Pasceri V, Barbato E, Merkely B, Edes I, Ostojic M, Wijns W, Di Sciascio G. Outcome comparison of 600- and 300-mg loading doses of clopidogrel in patients undergoing primary percutaneous coronary intervention for ST-segment elevation myocardial infarction: results from the ARMYDA-6 MI (Antiplatelet therapy for Reduction of MYocardial Damage during Angioplasty-Myocardial Infarction) randomized study. J Am Coll Cardiol. 2011;58:1592–1599. doi: 10.1016/j.jacc.2011.06.044. 30. Kunadian V, James SK, Wojdyla DM, Zorkun C, Wu J, Storey RF, Steg PG, Katus H, Emanuelsson H, Horrow J, Maya J, Wallentin L, Harrington RA, Gibson CM. Angiographic outcomes in the PLATO Trial (Platelet Inhibition and Patient Outcomes). JACC Cardiovasc Interv. 2013;6:671– 683. doi: 10.1016/j.jcin.2013.03.014. 31.Winter JL, Lindefjeld DS, Veas N, Guarda E, Valdebenito M, Méndez M, Pérez O, Zuanic K, Mestas M, Martínez A. Angiographic and electrocardiographic parameters of myocardial reperfusion in angioplasty of patients with ST elevation acute myocardial infarction loaded with ticagrelor or clopidogrel (MICAMI-TICLO trial). Cardiovasc Revasc Med. 2014;15:284–288. doi: 10.1016/j.carrev.2014.07.001. 32. Berthonneche C, Sulpice T, Boucher F, Gouraud L, de Leiris J, O’Connor SE, Herbert JM, Janiak P. New insights into the pathological role of TNFalpha in early cardiac dysfunction and subsequent heart failure after infarction in rats. Am J Physiol Heart Circ Physiol. 2004;287:H340–H350. doi: 10.1152/ajpheart.01210.2003. 33. Gurantz D, Cowling RT, Varki N, Frikovsky E, Moore CD, Greenberg BH. IL-1beta and TNF-alpha upregulate angiotensin II type 1 (AT1) receptors on cardiac fibroblasts and are associated with increased AT1 density in the post-MI heart. J Mol Cell Cardiol. 2005;38:505–515. doi: 10.1016/j. yjmcc.2004.12.015. 34. Sandanger Ø, Ranheim T, Vinge LE, et al. The NLRP3 inflammasome is up-regulated in cardiac fibroblasts and mediates myocardial ischaemiareperfusion injury. Cardiovasc Res. 2013;99:164–174. doi: 10.1093/cvr/ cvt091. 35.O’Brien LC, Mezzaroma E, Van Tassell BW, Marchetti C, Carbone S, Abbate A, Toldo S. Interleukin-18 as a therapeutic target in acute myocardial infarction and heart failure. Mol Med. 2014;20:221–229. doi: 10.2119/molmed.2014.00034. 36. LaFramboise WA, Bombach KL, Dhir RJ, Muha N, Cullen RF, Pogozelski AR, Turk D, George JD, Guthrie RD, Magovern JA. Molecular dynamics of the compensatory response to myocardial infarct. J Mol Cell Cardiol. 2005;38:103–117. doi: 10.1016/j.yjmcc.2004.09.011. 37. Liao Y, Lin L, Lu D, Fu Y, Bin J, Xu D, Kitakaze M. Activation of adenosine A1 receptor attenuates tumor necrosis factor-α induced hypertrophy of cardiomyocytes. Biomed Pharmacother. 2011;65:491–495. doi: 10.1016/j.biopha.2011.06.008. 38. Wagner DR, Combes A, McTiernan C, Sanders VJ, Lemster B, Feldman AM. Adenosine inhibits lipopolysaccharide-induced cardiac expression of tumor necrosis factor-alpha. Circ Res. 1998;82:47–56. 39. Hu S, Mao-Ying QL, Wang J, Wang ZF, Mi WL, Wang XW, Jiang JW, Huang YL, Wu GC, Wang YQ. Lipoxins and aspirin-triggered lipoxin alleviate bone cancer pain in association with suppressing expression of spinal proinflammatory cytokines. J Neuroinflammation. 2012;9:278. doi: 10.1186/1742-2094-9-278. 40. Ariel A, Chiang N, Arita M, Petasis NA, Serhan CN. Aspirin-triggered lipoxin A4 and B4 analogs block extracellular signal-regulated kinasedependent TNF-alpha secretion from human T cells. J Immunol. 2003;170:6266–6272. 41.Hachicha M, Pouliot M, Petasis NA, Serhan CN. Lipoxin (LX)A4 and aspirin-triggered 15-epi-LXA4 inhibit tumor necrosis factor 1alpha-initiated neutrophil responses and trafficking: regulators of a cytokine-chemokine axis. J Exp Med. 1999;189:1923–1930. 42. Natarajan R, Salloum FN, Fisher BJ, Ownby ED, Kukreja RC, Fowler AA 3rd. Activation of hypoxia-inducible factor-1 via prolyl-4 hydoxylase-2 gene silencing attenuates acute inflammatory responses in postischemic myocardium. Am J Physiol Heart Circ Physiol. 2007;293:H1571–H1580. doi: 10.1152/ajpheart.00291.2007. 43. Göser S, Andrassy M, Buss SJ, Leuschner F, Volz CH, Ottl R, Zittrich S, Blaudeck N, Hardt SE, Pfitzer G, Rose NR, Katus HA, Kaya Z. Cardiac troponin I but not cardiac troponin T induces severe autoimmune inflammation in the myocardium. Circulation. 2006;114:1693–1702. doi: 10.1161/CIRCULATIONAHA.106.635664. 44. Manning JR, Carpenter G, Porter DR, House SL, Pietras DA, Doetschman T, Schultz Jel J. Fibroblast growth factor-2-induced cardioprotection against myocardial infarction occurs via the interplay between nitric oxide, protein kinase signaling, and ATP-sensitive potassium channels. Growth Factors. 2012;30:124–139. doi: 10.3109/08977194.2012.656759. 45. Di Scipio F, Sprio AE, Folino A, Carere ME, Salamone P, Yang Z, Berrone M, Prat M, Losano G, Rastaldo R, Berta GN. Injured cardiomyocytes promote dental pulp mesenchymal stem cell homing. Biochim Biophys Acta. 2014;1840:2152–2161. doi: 10.1016/j.bbagen.2014.03.005. 46.Fathi E, Nassiri SM, Atyabi N, Ahmadi SH, Imani M, Farahzadi R, Rabbani S, Akhlaghpour S, Sahebjam M, Taheri M. Induction of angiogenesis via topical delivery of basic-fibroblast growth factor from polyvinyl alcohol-dextran blend hydrogel in an ovine model of acute myocardial infarction. J Tissue Eng Regen Med. 2013;7:697–707. doi: 10.1002/ term.1460. 47. Zhao T, Zhao W, Chen Y, Ahokas RA, Sun Y. Acidic and basic fibroblast growth factors involved in cardiac angiogenesis following infarction. Int J Cardiol. 2011;152:307–313. doi: 10.1016/j.ijcard.2010.07.024. 48. Mewhort HE, Turnbull JD, Meijndert HC, Ngu JM, Fedak PW. Epicardial infarct repair with basic fibroblast growth factor-enhanced CorMatrixECM biomaterial attenuates postischemic cardiac remodeling. J Thorac Cardiovasc Surg. 2014;147:1650–1659. doi: 10.1016/j.jtcvs.2013.08.005. 49. Virag JA, Rolle ML, Reece J, Hardouin S, Feigl EO, Murry CE. Fibroblast growth factor-2 regulates myocardial infarct repair: effects on cell proliferation, scar contraction, and ventricular function. Am J Pathol. 2007;171:1431–1440. doi: 10.2353/ajpath.2007.070003. 50. Yao HC, Liu T, Meng XY, Han QF, Zhang M, Wang LX. Effect of basic fibroblast growth factor on the myocardial expression of hypoxia-inducible factor-1α and vascular endothelial growth factor following acute myocardial infarction. Heart Lung Circ. 2013;22:946–951. doi: 10.1016/j. hlc.2013.04.111. 51.Ye Y, Lin Y, Perez-Polo R, Huang MH, Hughes MG, McAdoo DJ, Manickavasagam S, Uretsky BF, Birnbaum Y. Enhanced cardioprotection against ischemia-reperfusion injury with a dipyridamole and low-dose atorvastatin combination. Am J Physiol Heart Circ Physiol. 2007;293:H813–H818. doi: 10.1152/ajpheart.00210.2007. 52.Ye Y, Long B, Qian J, Perez-Polo JR, Birnbaum Y. Dipyridamole with low-dose aspirin augments the infarct size-limiting effects of simvastatin. Cardiovasc Drugs Ther. 2010;24:391–399. doi: 10.1007/ s10557-010-6252-x. 53.Manickavasagam S, Ye Y, Lin Y, Perez-Polo RJ, Huang MH, Lui CY, Hughes MG, McAdoo DJ, Uretsky BF, Birnbaum Y. The cardioprotective effect of a statin and cilostazol combination: relationship to Akt and endothelial nitric oxide synthase activation. Cardiovasc Drugs Ther. 2007;21:321–330. doi: 10.1007/s10557-007-6036-0. 54. Schrottmaier WC, Kral JB, Badrnya S, Assinger A. Aspirin and P2Y12 Inhibitors in platelet-mediated activation of neutrophils and monocytes. Thromb Haemost. 2015;114:. doi: 10.1160/TH14-11-0943. 55.Hausenloy DJ, Baxter G, Bell R, et al. Translating novel strategies for cardioprotection: the Hatter Workshop Recommendations. Basic Res Cardiol. 2010;105:677–686. doi: 10.1007/s00395-010-0121-4. Significance This study shows that in addition to its antiplatelet effects, ticagrelor reduces myocardial infarct size when administered before reperfusion. Moreover, even if started 1 day after infarction, ticagrelor, but not clopidogrel, improves remodeling and attenuates inflammation and fibrosis. Downloaded from http://atvb.ahajournals.org/ by guest on May 11, 2017 Ticagrelor Protects the Heart Against Reperfusion Injury and Improves Remodeling After Myocardial Infarction Yumei Ye, Gilad D. Birnbaum, Jose R. Perez-Polo, Manjyot K. Nanhwan, Sven Nylander and Yochai Birnbaum Arterioscler Thromb Vasc Biol. 2015;35:1805-1814; originally published online June 4, 2015; doi: 10.1161/ATVBAHA.115.305655 Arteriosclerosis, Thrombosis, and Vascular Biology is published by the American Heart Association, 7272 Greenville Avenue, Dallas, TX 75231 Copyright © 2015 American Heart Association, Inc. All rights reserved. Print ISSN: 1079-5642. Online ISSN: 1524-4636 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://atvb.ahajournals.org/content/35/8/1805 Data Supplement (unedited) at: http://atvb.ahajournals.org/content/suppl/2015/06/04/ATVBAHA.115.305655.DC1 Permissions: Requests for permissions to reproduce figures, tables, or portions of articles originally published in Arteriosclerosis, Thrombosis, and Vascular Biology can be obtained via RightsLink, a service of the Copyright Clearance Center, not the Editorial Office. Once the online version of the published article for which permission is being requested is located, click Request Permissions in the middle column of the Web page under Services. Further information about this process is available in the Permissions and Rights Question and Answer document. Reprints: Information about reprints can be found online at: http://www.lww.com/reprints Subscriptions: Information about subscribing to Arteriosclerosis, Thrombosis, and Vascular Biology is online at: http://atvb.ahajournals.org//subscriptions/ Ticagrelor Protects the Heart Against Reperfusion Injury and Improves Remodeling After Myocardial Infarction Running title: Ticagrelor Protects Against Reperfusion Injury Yumei Ye, MD1; Gilad D. Birnbaum2; Jose R Perez-Polo, PhD1; Manjyot K Nanhwan, MD1; Sven Nylander, PhD3; Yochai Birnbaum, MD1,2 Materials and Methods: Animal care This study was approved by The University of Texas Medical Branch IACUC and conducted in accordance with ‘The Guide for the Care and Use of Laboratory Animals’ published by the US National Institutes of Health (NIH Publication No. 85-23, revised 1996). Male Sprague-Dawley rats were used in the study. Materials Ticagrelor was provided by AstraZeneca and clopidogrel was purchased from Bristol-Myers Squibb/ Sanofi Pharmaceuticals. Anti-β-actin antibodies were from Sigma (St Louis, MO). ELISA kits for 6-keto-PGF1α and cPLA2 activity, immunoassay kit for 15-epi-LXA4 was from Oxford Biomedical Research (Rochester Hills, MI), FGF-2 (Fibroblastic growth factor-2, basic fibroblastic growth factor) EIA kit from R&D (Minneapolis, MN), and EIA kit for MIP-2 (macrophage inflammatory protein-2) ELISA kit from Invitrogen (Grand Island, NY). Anti-AKT and anti-phospho-AKT antibodies were from R&D Systems (Minneapolis, MN). Anti-Ser1177 Phospho-eNOS, anti-total ERK and P-ERK and anti- eNOS antibodies were from Cell Signaling (Beverly, MA). TUNEL staining for apoptosis was performed using Cardio-TACS kit (Trevigen; Gaithersburg, MD). Treatment Experiment 1: Does Ticagrelor limit reperfusion injury? Rats were subjected to 30 min coronary artery ligation followed by reperfusion. Ticagrelor (10 or 30mg/kg), clopidogrel (12.5mg/kg) or vehicle was given via intraperitoneal (IP) injection 5min before reperfusion (acute treatment). Experiment 2: Does TIC affect adverse remodeling after myocardial infarction? Rats were subjected to 30 min coronary artery ligation followed by reperfusion. Ticagrelor (30mg/kg), clopidogrel (12.5mg/kg) or vehicle was given via intraperitoneal (IP) injection 5min before reperfusion (acute treatment). The next day oral Ticagrelor (300 mg/kg/d), Oral clopidogrel (62.5 mg/kg/d) or placebo was started and continued for 4W (chronic treatment). Ticagrelor and Clopidogrel were mixed with normal chow (Ticagrelor: 4mg/g chow, Clopidogrel: 0.83mg/g chow). The following groups were included: sham- sham surgery + vehicle IP and oral placebo; control- ischemia-reperfusion surgery + vehicle IP + oral placebo; Ticagrelor acute- ischemiareperfusion surgery + Ticagrelor 30 mg/kg IP + oral placebo; Ticagrelor chronic- ischemiareperfusion surgery + vehicle IP + oral Ticagrelor 300 mg/kg/d; Ticagrelor acute + chronic ischemia-reperfusion surgery + Ticagrelor 30 mg/kg IP + oral Ticagrelor 300 mg/kg/d; and Clopidogrel (12.5mg/kg IP + oral 62.5mg/kg/d). IS surgical protocol The rat model of myocardial ischemia-reperfusion injury has been described in detail.1-4 Rats were anesthetized with intraperitoneal injection of xylazine (6 mg/kg) and ketamine (60 mg/kg), intubated and ventilated (FIO2=30%). The rectal temperature was monitored and body temperature was maintained between 36.7 and 37.3o C throughout the experiment. The left carotid artery was cannulated. The chest was opened and the left coronary artery was encircled with a suture and ligated for 30min. Isofluorane (1-2.5% titrated to effect) was added after the beginning of ischemia to maintain anesthesia. After 30min of coronary occlusion, the snare was released and myocardial reperfusion was verified by change in the color of the myocardium. Subcutaneous buprenorphine (0.1 mg/kg) was administered, the chest was closed and the rats were recovered from anesthesia. Twenty-four hours after reperfusion, the rats were re- anesthetized, the coronary artery was reoccluded, 1.5 ml of Evan's blue dye 3% was injected into the right ventricle and the rats euthanized under deep anesthesia. Heart rate and mean blood pressure were noted at baseline (10min after completion of surgery), immediately before coronary artery occlusion, after 25min of ischemia, and following 20min of reperfusion. The pre-specified exclusion criteria were lack of signs of ischemia during coronary artery ligation, lack of signs of reperfusion after release of the snare, prolonged ventricular arrhythmia with hypotension, and area at risk ≤ 10% of the LV weight. 1-4 Determination of area at risk (AR) and IS Hearts were excised and the left ventricle was sliced transversely into 6 sections. Slices were incubated for 10 minutes at 37C in 1% buffered (pH=7.4) 2,3,5-triphenyl-tetrazolium-chloride (TTC), fixed in a 10% formaldehyde and photographed in order to identify the AR (unstained by Evan’s blue dye), the IS (unstained by TTC), and the non-ischemic zones (stained by Evan’s blue). The AR and IS area in each slice were determined by planimetry, converted into percentages of the total area, multiplied by the weight of the slice and finally data for all 6 sections were combined to obtain the weight of the myocardial AR and IS 1, 3-6. Echocardiogram Echocardiogram was performed 4 weeks after infarction using a fully digitized Vevo 770 highresolution ultrasound system (VisualSonics, Inc.) with a 25 MHz transducer-710B (VisualsonicsToronto, Canada), designed for the examination of small animals. Animals were anesthetized with ketamine-xylazine. 7 Standard M-mode images were taken in the long axis and short axis position at the level of the papillary muscles for each animal. Key cardiac parameters, such as left ventricle internal diameters at end diastole (LVIDd) and systole (LVIDs), and left ventricular fractional shortening (FS) were measured. Ejection fraction was measured by a single-plane area length using 2D parasternal long axis images. 7 Myocardial fibrosis Samples from the left ventricular border zone of the infarction were fixed in 10% buffered formaldehyde for 24 h and embedded in paraffin. Serial sections of 4μm were incubated for 1h in 0.2% picrosirius red in aqueous saturated picric acid. The images were analyzed under a microscope at magnification ×200. The area of the myocardial collagen network was determined using the image-processing program Image-Pro Plus v. 4.5 and expressed as the percentage of picrosirius red–positive pixels among the total pixels in each image stack. Apoptosis TUNEL (terminal transferase dUTP nick end labeling) staining was used. Rats underwent 30 min coronary artery occlusion and 24h reperfusion, as above. At 5 min of coronary artery occlusion rats received IP vehicle, Clopidogrel 12.5 mg/kg or Ticagrelor 30 mg/kg. Additional group undergoing sham surgery and receiving vehicle IP. At 4h of reperfusion, rats were euthanized and 2-mm section of myocardial tissue from the border of the ischemic zone was fixed in 4% formalin solution and embedded in paraffin. Immunohistochemical procedures for detecting apoptotic cardiomyocytes was performed by using Cardio-TACS kit according to the manufacturer’s instructions. Apoptotic-positive myocytes were determined by randomly counting 10 fields. The percentage of apoptoic cells was then determined (i.e., the number of apoptotic myocytes/total number of myocytes counted × 100). 15-epi-LXA4 Myocardial samples of the anterior wall of the left ventricle were harvested and snap-frozen in liquid nitrogen and stored at −80°C. Samples were rinsed in cold PBS solution (pH 7.4) containing 0.16mg/mL heparin to remove red blood cells and clots, homogenized in cold PBS (pH 7.4) and centrifuged at 10,000 x g for 15 min at 40C. The supernatant was diluted with water and acidified to pH 3.5 with 1M HCl. The sample was loaded into C-18 Sep-Pak light column (Waters Corporation, Milford, MA) and washed with 1 mL of water followed by 1 mL of petroleum ether. The sample was eluted with 2 mL of methyl formate and evaporated with N2 and the residue was dissolved in extraction buffer. We followed the manufacturer instruction of the immunoassay kits for measuring 15-epi-LXA4.8 COX2 activity Myocardial samples were sectioned into three segments (20 mg each), homogenized in cold PBS (pH 7.4), and centrifuged. The supernatants were collected and stored on ice. The segments were placed into test vials with 500µL Hanks’ HEPES solution. Fifty µM arachidonic acid (AA) were added to the first tube (for overcoming the potential rate limiting effects of cPLA2 that generates AA); AA + 200µM of SC58125 (a specific COX2 inhibitor) to the second tube; and AA + 100µM of SC560 (a specific COX1 inhibitor) to the third tube. After 15minute incubation at room temperature, the supernatant in each vial was aspirated and stored at -70°C. The samples (25µL each) were analyzed for 6-keto-PGF1. 5, 8 by an ELISA kit according to the manufacturer instruction. The first tube represents 6-keto-PGF1 generated by both COX1 and COX2. COX2 activity was calculated as 6-Keto-PGF1α levels in the first minus the second tube and COX1 activity as 6-Keto-PGF1α levels in the first minus the third tube.5, 8 FGF2 and MIP2 Myocardial tissue was harvested and snap-frozen in liquid nitrogen and stored at −80°C. Samples were rinsed with PBS and homogenized with a tissue homogenizer. Levels of FGF2 or MIP2 in the samples were quantified with a FGF2 EIA kit (R&D) or a MIP-2 ELISA kit (Invitrogen). All samples were prepared and analyzed in triplicate, and absorbance at 405 nm was read in a microplate reader. Immunoblotting Myocardial samples from the left ventricle of animals not exposed to ischemia (sham) and from the border zone of the previously ischemic area of animals exposed to ischemia-reperfusion and treated with vehicle, TIC 30 or CLOP12.5 were homogenized in lysis buffer (in mM): 25 Tris·HCl (pH 7.4), 0.5 EDTA, 0.5 EGTA, 1 phenylmethylsulfonyl fluoride, 1 dithiothreitol, 25 NaF, 1 Na3VO4, 1% Triton X-100, 2% SDS and 1% protease inhibitor cocktail. The lysate was centrifuged at 10,000g for 15min at 4°C and supernatants were collected. Protein (50µg) was fractionated by SDS-PAGE (4%-20% polyacrylamide gels) and transferred to PVDF membranes (Millipore, Bedford, MA). The membranes were incubated overnight at 40C with primary antibodies (see ”Materials”). Bound antibodies were detected using the chemiluminescent substrate (NEN Life Science Products, Boston, MA). The protein signals were quantified with an image-scanning densitometer, and the strength of each protein signal was normalized to the corresponding β-actin signal. Data are expressed as percent relative the expression in the control group. Plasma Ticagrelor levels Blood was collected from the tail-vein into EDTA anti-coagulated tubes. All blood samples were gently mixed, and immediately placed on ice. Plasma was prepared within 30 minutes of blood sampling by centrifugation at 1500 x g for 10 min at approximately 4°C. The plasma was transferred into tubes stored at or below -20°C within 1 hour of sample collection and plasma concentration of ticargelor was determined by protein precipitation and liquid chromatography mass spectrometry as described previously.9 Platelet aggregation Platelet rich plasma (PRP) was prepared from blood sampled from rats in experiment 1 by centrifugation of whole blood anticoagulated with citrate dextrose at 800 rpm for 10 minutes at room temperature. Platelet aggregation were recorded after activation with 15 µM ADP using a platelet aggregation profiler (PAP-8; BioData). Data are expressed as the final percent aggreagation response after 6 min. 4 Myocardial adenosine levels Myocardial samples were immediately shock-frozen with liquid nitrogen. Adenosine levels in myocardial tissue samples were analyzed by high performance liquid chromatography (HPLC) based on the procedure of Wojcik and Neff. 10 Samples were homogenized in 10 volumes of 0.25 M ZnSO4, and protein concentrations were examined by the Lowry assay. After adding ten volumes of 0.25 M Ba(OH)2, the samples were centrifuged at 30,000 x g for 10 minutes. The supernatants were collected and 5 µL of chloroacetaldehyde was added to 20 µL of supernatant. The tubes were capped, mixed and submerged in a boiling water bath for 10 min. Samples were analyzed by HPLC using a Waters C18 reversed phase 150 mm X 4.6 mm column. The mobile phase was a 50 mM acetate buffer (pH 4.5) and 6.5% aqueous acetonitrile (volume/volume) containing 2 mM sodium octyl sulfonate, flow rate was 1.1 mL/min, the excitation monochromator was set to a wavelength of 270 nm and the cutoff wavelength of the emission filter was 389 nm.4 Tail Vein Bleeding time Rats were anesthetized and placed on a 370C heating pad. The tail was transected 0.5 cm from the tip using a 21-G syringe needle. Then the tail was immediately immersed in a 50-mL falcon tube filled with 37 °C saline. Bleeding time will be recorded as the time at which bleeding stopped. Animal will also be observed for 6 hours and examined on the next morning for signs of delayed bleeding. Real-Time PCR Total RNA from heart tissue was extracted using TRIzol reagent (Invitrogen, Carlsbad, CA), per the manufacturer instructions. 2μg total RNA from each sample was reverse-transcribed into cDNA and equal amounts of transcriptional products were subjected to PCR amplification. The mRNA expression of IL-1β IL-18 TNF-α, Collagen III or COX2 was performed by using the primers designed in Supplement Table II. The Ct (threshold cycle) is defined as the number of cycles required for the fluorescence signal to exceed the detection threshold. Expression of the gene relative to the GAPDH expression was calculated as the difference between the threshold values of these two genes (2-Δct). Melting curve analysis was performed during real-time PCR to analyze and verify the specificity of the reaction. The values are given as the means ± standard error of four independent experiments. Statistical Analysis Data are presented as means ± SE. Analysis of variance (ANOVA) with Sidak correction for multiple comparisons was applied to compare the different groups. The differences in HR and MBP were compared using two-way repeated measures ANOVA with Holm-Sidak multiple comparison procedures. Values of P <0.05 were considered statistically significant. References: 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Atar S, Ye Y, Lin Y, Freeberg SY, Nishi SP, Rosanio S, Huang MH, Uretsky BF, PerezPolo JR, Birnbaum Y. Atorvastatin-induced cardioprotection is mediated by increasing inducible nitric oxide synthase and consequent s-nitrosylation of cyclooxygenase-2. Am J Physiol Heart Circ Physiol. 2006;290:H1960-1968 Birnbaum Y, Lin Y, Ye Y, Martinez JD, Huang MH, Lui CY, Perez-Polo JR, Uretsky BF. Aspirin before reperfusion blunts the infarct size limiting effect of atorvastatin. Am J Physiol Heart Circ Physiol. 2007;292:H2891-2897 Birnbaum Y, Ye Y, Rosanio S, Tavackoli S, Hu ZY, Schwarz ER, Uretsky BF. Prostaglandins mediate the cardioprotective effects of atorvastatin against ischemiareperfusion injury. Cardiovasc Res. 2005;65:345-355 Nanhwan MK, Ling S, Kodakandla M, Nylander S, Ye Y, Birnbaum Y. Chronic treatment with ticagrelor limits myocardial infarct size: An adenosine and cyclooxygenase-2dependent effect. Arterioscler Thromb Vasc Biol. 2014;34:2078-2085 Birnbaum Y, Ye Y, Lin Y, Freeberg SY, Huang MH, Perez-Polo JR, Uretsky BF. Aspirin augments 15-epi-lipoxin a4 production by lipopolysaccharide, but blocks the pioglitazone and atorvastatin induction of 15-epi-lipoxin a4 in the rat heart. Prostaglandins Other Lipid Mediat. 2007;83:89-98 Ye Y, Lin Y, Atar S, Huang MH, Perez-Polo JR, Uretsky BF, Birnbaum Y. Myocardial protection by pioglitazone, atorvastatin, and their combination: Mechanisms and possible interactions. Am J Physiol Heart Circ Physiol. 2006;291:H1158-1169 Keyes KT, Xu J, Long B, Zhang C, Hu Z, Ye Y. Pharmacological inhibition of pten limits myocardial infarct size and improves left ventricular function postinfarction. Am J Physiol Heart Circ Physiol. 2010;298:H1198-1208 Birnbaum Y, Ye Y, Lin Y, Freeberg SY, Nishi SP, Martinez JD, Huang MH, Uretsky BF, Perez-Polo JR. Augmentation of myocardial production of 15-epi-lipoxin-a4 by pioglitazone and atorvastatin in the rat. Circulation. 2006;114:929-935 Sillen H, Cook M, Davis P. Determination of ticagrelor and two metabolites in plasma samples by liquid chromatography and mass spectrometry. J Chromatogr B Analyt Technol Biomed Life Sci. 2010;878:2299-2306 Wojcik WJ, Neff NH. Adenosine measurement by a rapid hplc-fluorometric method: Induced changes of adenosine content in regions of rat brain. J Neurochem. 1982;39:280-282 Ticagrelor Protects the Heart Against Reperfusion Injury and Improves Remodeling After Myocardial Infarction Running title: Ticagrelor Protects Against Reperfusion Injury Yumei Ye, MD1; Gilad D. Birnbaum2; Jose R Perez-Polo, PhD1; Manjyot K Nanhwan, MD1; Sven Nylander, PhD3; Yochai Birnbaum, MD1,2 Supplement Material Supplement Table I: Primers used for the rt-PCR Target mRNA Forward primer Reverse primer IL-1β IL-18 TNF-α Collagen III COX2 GAPDH TGCTGTCTGACCCATGTGAG GTCGTTGCTTGTCTCTCCTTG CAGACCACTTTGGCAGACTTCACT GACCCTCACACTCAGATCATCTTCT GACAGATGCTGGTGCTGAGAAG TGCGATGCTCTTCCGAGCTGTGCT ATGATTCTACCCACGGCAAG GGATTCGTTGGCTGTTCGGTCG TGCTACGACGTGGGCTACG TCTGAGGAAGGCCAGCTGTAC TCAGGAAGTTCCTTATTTCCTTTC CTGGAAGATGGTGATGGGTT Supplement Table II: Heart rate (HR), body weight (BW) and heart weight (HW) of the rats at the end of the 4W treatment (Experiment 2). Sham HR Control TIC IP TIC oral TIC CLOP IP + oral IP + oral P value n=8 n=7 n=8 n=8 n=8 n=8 295±5 288±5 290±5 301±4 298±6 287±6 0.291 268±14 267±11 266±12 283±12 259±16 259±16 0.824 (bpm) BW (g) HW (g) 1.22±0.05 1.19±0.05 1.15±0.04 1.25±0.05 1.19±0.04 1.19±0.03 0.641 Supplement Figure I: a. Heart rate (HR, BPM). There was a significant time effect (p<0.001), but not treatment effect (p=0.511) on HR (p=0.012 for the treatment X time interaction). b. Mean blood pressure (MBP, mmHg). There was a significant time effect (p<0.001), but not treatment effect (p=0.842) on MBP (p<0.001 for the treatment X time interaction). Supplement Figure 2: Two-dimensional and M-mode echocardiographic samples at 4W of rats that underwent sham surgery (sham), or ischemia-reperfusion injury and treated with vehicle (control), ticagrelor IP only (TIC-IP), ticagrelor oral only (TIC-oral), ticagrelor IP + oral (TIC IP + oral), or clopidogrel IP + oral (Clop IP + oral). Supplement Figure 3: Picrosirius red staining of myocardial samples from the left ventricle of sham- operated rats and rats exposed to ischemia-reperfusion injury and treated with vehicle, ticagrelor IP only (TIC-IP), ticagrelor oral only (TIC-oral), ticagrelor IP + oral (TIC IP + oral), or clopidogrel IP + oral (Clop IP + oral).