* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Case
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Jatene procedure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Myocardial infarction wikipedia , lookup
Electrocardiography wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
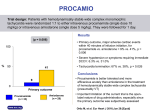
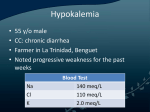
Case Report: Amiodarone Administration in a Patient with Ventricular Bigeminy and Hypokalemia Jerry Marisi Hasiholan Marbun1, Raden Syarif Hidayat Soeriasaputra2, Cekli Wahyuwidowati3, Eka Dharma Sastra3 1 General Practitioner at Berkah General Hospital, Pandeglang, Banten, Indonesia 2 Cardiologist at Berkah General Hospital, Pandeglang, Banten, Indonesia 3 Internist at Berkah General Hospital, Pandeglang, Banten, Indonesia Introduction Ventricular bigeminy refers to alternating normal sinus and premature ventricular complexes. Amiodarone is a potent antiarrhythmic agent to treat ventricular arrhythmias. Amiodarone administration in hypokalemia may increase the risk of adverse effect of amiodarone. Case report A 51-year old woman was admitted to the emergency with complaints of palpitations. She had a history of hypertension and heart failure, but didn’t remember the medications. Upon admission, 12-lead electrocardiogram (ECG) revealed ventricular bigeminy, with heart rate of 72 times/minute. Amiodarone bolus was given 150 mg intravenous (IV), continued with dosage of 900 mg (IV) for 24 hours, and continued 3x200 mg oral daily. After amiodarone bolus, ECG showed sinus rhythm with ventricular quadrigeminy. On the 3th day hospitalized, ECG showed sinus rhythm with ventricular quadrigeminy; laboratory results showed marked hypokalemia (2,4 mmol/L). Intravenous potassium chloride and oral potassium aspartate was added. On the 5th day, ECG showed sinus bradycardia; potassium level was 2,2 mmol/L. On the 6th day, the patient asked to be discharged. Discussion Amiodarone is the most effective antiarrhythmic drugs for the treatment of supraventricular and ventricular tachyarrhythmias. Despite that, amiodarone has numerous adverse effects. Amiodarone may prolong QT interval, although polymorphic ventricular tachycardia (torsades de pointes) is rare. Prolongation of QT interval increases the risk for torsade the pointes. In this case, ECG showed QT prolongation (QTc 570 ms) after amiodarone administration. Hypokalemia in this case was troubling. Hypokalemia could itself had been the arrhythmogenic factor in this case, although the arrhythmia was reverted to sinus rhythm while potassium level was still low. Furthermore, hypokalemia could also be the concomitant factor for QT prolongation. The cause of hypokalemia isn’t entirely clear; it most probably was attributed to the renal loss from chronic diuretic therapy. But the fact that potassium level decreased on hospitalization, while there’s no diuretic therapy and potassium supplement was administered, raises suspicion that there probably were other factors. Conclusion Amiodarone should be used carefully in hypokalemia, because the increased risk of QT prolongation. Although hypokalemia should be corrected before amiodarone administration, it’s still a challenge in a remote area with limited resources. Keywords: Amiodarone, arrhythmia, hypokalemia, QT prolongation, ventricular bigeminy