* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download clinical problems in cardiopulmonary disease
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Transcript
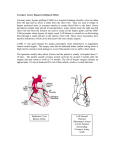
clinical problems in cardiopulmonary disease Management of a Patient With Angina Pectoris* Rabih R. Azar, MD, MSc; and David D. Waters, MD (CHEST 2001; 119:287–289) Key words: angina; angioplasty; coronary artery disease Abbreviations: CAD ⫽ coronary artery disease; LDL ⫽ lowdensity lipoprotein Case Presentation 56-year-old man consulted his physician comA plaining of “pressure” in the central chest with radiation into both arms. This symptom had been present for approximately 1 year, was induced primarily by exertion, and was relieved promptly by rest. It was nonprogressive in nature and did not alter his lifestyle to any significant degree. In the past, he had always enjoyed good health. He had given up cigarette smoking 10 years previously after having smoked one pack daily for 25 years. In an evaluation 3 years ago, he was told that his cholesterol was “slightly high.” He was overweight with little recent change and considered his lifestyle sedentary, seldom engaging in active exercise. He was never told of hypertension or diabetes mellitus. A physical examination disclosed a well-developed, mildly obese man with a BP of 140/86 mm Hg, heart rate of 82 beats/min and regular, height of 5 feet 8 inches, and a weight of 192 lb. The results of an examination of the heart and lung were normal, and the remainder of the general examination was also normal. The results of laboratory testing disclosed a normal CBC count and fasting blood glucose level. The patient’s lipid profile disclosed the following levels: total cholesterol, 232 mg/dL; high-density lipopro*From the University of California at San Francisco, CA. Manuscript received May 4, 2000; revision accepted June 1, 2000. Correspondence to: David D. Waters, MD, Division of Cardiology, San Francisco General Hospital, 1001 Potrero Ave, Room 5G1, San Francisco, CA 94110; e-mail: dwaters@ medsfgh.ucsf.edu tein, 40 mg/dL; low-density lipoprotein (LDL), 166 mg/dL; and triglycerides, 170 mg/dL. A treadmill examination then was performed. The patient was able to achieve an exertional level of approximately 7 metabolic equivalents (ie, 2.5 miles per hour with a 12% grade). During the test, 1.5 mm of horizontal ST-segment depression occurred at a heart rate of 125 beats/min (76% of the expected maximum heart rate). Shortly thereafter, chest pain was noted, and the test was discontinued at a heart rate of 130 beats/min. The patient then was subjected to cardiac catheterization with coronary cineangiography, which provided the following information: the left ventriculogram showed a normally contracting chamber with normal systolic and diastolic pressures. The left anterior descending coronary artery disclosed a short, high-grade lesion (90% narrowing) in an area proximal to the first septal perforator branch. The remainder of the left coronary system displayed scattered luminal irregularities with an area of modest narrowing (30%) in the proximal portion of the obtuse marginal branch of the left circumflex artery. The right coronary artery harbored an area of 80% narrowing (1 cm distal to the ostium). Distally, this artery appeared free of significant disease. The two high-grade lesions were considered to be amenable to angioplasty procedures. Questions for Consultants 1. What would be your overall management of this patient? 2. Assuming that one chooses medical therapy with rigorous lipid control, what circumstances would you require in order to recommend an alternate approach, such as angioplasty or coronary bypass surgery? 3. Would the severity of angina or the presence of reduced left ventricular function influence your therapeutic approach? CHEST / 119 / 1 / JANUARY, 2001 Downloaded From: http://publications.chestnet.org/pdfaccess.ashx?url=/data/journals/chest/21956/ on 05/11/2017 287 Comments by Consultants Rabih R. Azar, MD, MSc, and David D. Waters, MD The patient is a 56-year-old man who presented with chronic stable angina and a stress test suggesting at least moderate impairment in his exercise tolerance due to ischemia. The fact that angina has not limited his daily activity is related to his sedentary lifestyle. The other important elements to consider in the management of his condition are his risk factors for coronary artery disease (CAD), the underlying left ventricular function, and the anatomy of coronary atherosclerosis. Our first step in managing this patient is to start aspirin therapy (81 to 325 mg/d) and lipid-lowering therapy, preferably with administration of a statin agent. By inhibiting platelet aggregation, aspirin decreases the incidence of future coronary events by ⬎ 50%, and this agent is a well-tolerated drug. Cholesterol lowering improves endothelial function, delays the progression of CAD, and, most importantly, leads to the stabilization of the atherosclerotic plaques preventing future acute coronary syndromes. Our goal in lipid management would be to lower the patient’s LDL levels to ⬍ 100 mg/dL. Lipid lowering was shown to decrease significantly the incidence of death and nonfatal myocardial infarction in both primary and secondary prevention trials with no significant serious side effects compared to placebo. Furthermore, in a recent prospective trial, aggressive LDL lowering (mean level, 77 mg/dL) with atorvastatin, 80 mg/d, was at least as effective as angioplasty and usual care in reducing ischemic cardiac events in patients with one- or two-vessel CAD and normal left ventricular function. In addition to medical therapy, we would recommend revascularization of the left anterior descending artery and the right coronary artery. We recommend this because the patient has at least a moderately limited exercise capacity and a large amount of myocardium at risk. Studies comparing bypass surgery to medical therapy alone have shown a survival benefit for surgery in patients with twovessel CAD involving the proximal left anterior descending artery. For this patient, we would favor angioplasty with stenting over bypass surgery. In patients without diabetes mellitus and with a preserved left ventricular function, the Bypass Angioplasty Revascularization Investigation trial has shown that both revascularization strategies are equally effective in terms of survival and freedom from myocardial infarction. The two coronary lesions seen in this patient seem easily amendable to percutaneous revascularization. Angioplasty is much less aggressive than bypass surgery, but the likelihood for repeat interventions is higher because of restenosis. However, coronary stenting has significantly decreased this complication. Angioplasty is not superior to medical therapy for the prevention of myocardial infarction and death, but it is better in angina control and in improving exercise capacity. This is important for our patient who is mildly obese, has a sedentary lifestyle, and is still relatively young. We would recommend that he starts a progressive exercise program and loses weight following angioplasty. If the patient refuses revascularization, we would start him on a -blocker (in addition to aspirin and aggressive lipid lowering) with careful monitoring of his underlying symptoms. Any evidence of the progression of symptoms or further deterioration in exercise capacity should urge reconsideration of coronary revascularization. Should he develop left ventricular dysfunction, our recommendation for revascularization would be even stronger. In the absence of myocardial infarction, left ventricular dysfunction suggests a severe reduction in coronary blood flow resulting in myocardial hibernation. This condition usually improves after revascularization. Left ventricular dysfunction is also an independent predictor of reduced survival. While multivessel angioplasty was shown to be equal to bypass surgery in terms of improving survival and the incidence of nonfatal myocardial infarctions, patients with impaired left ventricular function were excluded from these trials. This would lead us to recommend bypass surgery as a first choice in a revascularization strategy in a patient with left ventricular dysfunction. Editor’s Comment This case exemplifies the various options presently available to the clinician for the management of stable CAD. In comparison with earlier standard medical management, several trials have demonstrated the efficacy of vigorous cholesterol reduction in reducing atheroscleric events and prolonging survival in patients who already have manifested ischemic cardiac or cerebrovascular disease. As Dr. Waters’ group has demonstrated,1 aggressive lipid lowering with atorvastatin in patients with stable coronary disease who have one or two major coronary vessels involved is at least as effective as the traditional mechanical interventions (ie, angioplasty or bypass operations) in the prevention of subsequent ischemic events and in prolonging survival. These findings apply at the least to patients who are asymptomatic or have mild to moderate angina pectoris and who have normal or only mildly decreased resting left-ventricular systolic function (ejection fraction, ⱖ 40%). In comparison with med- 288 Downloaded From: http://publications.chestnet.org/pdfaccess.ashx?url=/data/journals/chest/21956/ on 05/11/2017 Clinical Problems in Cardiopulmonary Disease ical therapy, mechanical interventions result in more immediate and complete relief of anginal symptoms in this group of patients, despite providing no survival benefit. In past comparisons with medical therapy, coronary bypass surgery has been found to prolong survival in patients who have triple-vessel coronary artery disease combined with impaired left ventricular function, as well as in such patients who have involvement of the proximal left anterior descending coronary artery, even with normal left ventricular function or an absence of triple-vessel disease.2,3 Equivalent outcomes have been reported when surgery is compared with angioplasty in such groups of nondiabetic patients.4 In the light of the aggressive lipid lowering produced by modern drugs, singly or in combination, time-honored indications for surgery or angioplasty are in a state of flux and may no longer be valid. Thus, in a patient such as this, one could make a strong case for initial therapy with a statin-type cholesterol-lowering drug combined with vigorous risk factor control, reserving mechanical interventions for patients who fail to respond or who show further progression of cardiac symptoms. How contemporary medical therapy would compare with mechanical interventions (an- gioplasty or surgery) in the presence of left-ventricular dysfunction, triple-vessel coronary disease, or more severe symptoms is largely unknown and awaits the results of long-term trials. In the meantime, however, one might anticipate that the aggressive lowering of lipid levels would at least complement angioplasty or surgery in such patients, presumably by stabilizing untreated atherosclerotic lesions. References 1 Pitt B, Waters D, Brown WV, et al. Aggressive lipid-lowering therapy compared with angioplasty in stable coronary artery disease. N Engl J Med 1991; 341:70 –76 2 Yusuf S, Zucker D, Peduzzi P, et al. Effect of coronary artery bypass graft surgery on survival: overview of 10 year results from randomized trials by the Coronary Artery Bypass Graft Surgery Trialists Collaboration. Lancet 1994; 344:563–570 3 American College of Cardiology/American Heart Association Task Force on Assessment of Diagnostic and Therapeutic Cardiovascular Procedures (Subcommittee on Coronary Artery Bypass Graft Surgery). Guidelines and indications for coronary artery bypass graft surgery. J Am Coll Cardiol 1991; 17:543–589 4 Lincoff AM, Topol EJ. Interventional catheterization techniques. In: Braunwald, E, ed. Heart disease. 5th ed. Philadelphia, PA: WB Saunders, 1997; 1366 –1403 CHEST / 119 / 1 / JANUARY, 2001 Downloaded From: http://publications.chestnet.org/pdfaccess.ashx?url=/data/journals/chest/21956/ on 05/11/2017 289