* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Tuberculosis
Brucellosis wikipedia , lookup
Hepatitis B wikipedia , lookup
Sarcocystis wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Marburg virus disease wikipedia , lookup
Meningococcal disease wikipedia , lookup
Oesophagostomum wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Onchocerciasis wikipedia , lookup
Chagas disease wikipedia , lookup
Leishmaniasis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Leptospirosis wikipedia , lookup
History of tuberculosis wikipedia , lookup
Neonatal infection wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Tuberculosis wikipedia , lookup
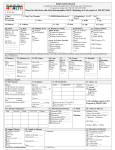
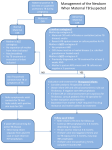
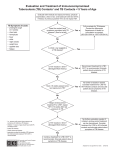
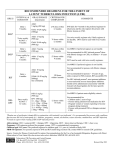
Tuberculosis August 17, 2010 Tuberculosis • Mycobacterium tuberculosis – Fastidious, aerobic, acid-fast bacillus • Tremendous increase in incidence over 25 yrs • On average, adult pts infect 8 to 15 individuals prior to being diagnosed • Increased risk – HIV, diabetes, renal failure – 9% of pts in US coinfected with HIV Three Groups • Exposed, but status unknown – Insufficient period of time to rely on TST • Latent TB Infection – Positive TST but no signs or symptoms, nl CXR – 30% global population – 5-10% progress to disease • TB Disease – Clinical or radiographic findings – Reportable Resistance • Drug-resistant TB (DR-TB) – Relapse after tx – Positive sputum smear after 2mos tx • Multidrug-resistant TB (MDR-TB) – Resistance to at least 2 first line abx (1% in US) • Extensively drug-resistant TB – Resistance to INH, rifampin, any fluoroquinolone, and any second line IV agent Pathogenesis • Lymphadenitis • Ghon complex – Focus of infection with enlarged regional nodes • Contained • Spread rapidly • Reactivated later in life • Most clinical manifestations in children 1-2 yrs from initial infection Clinical Manifestations • Lung is most common site of infxn (80%) • Tuberculous LAD (67%) • Meningitis (13%) – Most commonly infants and toddlers • Pleural, miliary, skeletal account for <6% Pulmonary Disease • Primary Parenchymal – Most common, Infants most likely to be symptomatic • Cough, low-grade fever, wt loss – CXR: hilar or mediastinal adenopathy • Collapse-consolidation pattern • Progressive Primary Disease – Lung tissue destruction and cavitary lesion • Reactivation disease – Immunocompromised adolescents or adults Lymphatic Disease • Most common extrapulmonary form of TB • Usually cervical nodes • Slightly older than pts with nontuberculous mycobacterial LAD • 2-4cm, may have overlying violaceous skin color – Lack classic findings of pyogenic nodes • CXR abnl in 33% • Tx: 6 mos multidrug tx, +/- excision CNS Disease • 50% are <2y/o • May include CNS vasculitis or increased ICP – Consider in cases of childhood stroke • Tuberculomas in 5% of CNS TB – Single rim-enhancing lesion • • • • CSF: lymphocytes, low glucose, high protein TST in only 33% CXR in 90% Highest morbidity/mortality Diagnosis • TST, epidemiologic info, clinical/radiographic findings • Children: vigorous response to few organisms – 30% with positive cx (AFB) • TST (purified protein derivative or Mantoux) – Read at 48-72hrs – Delayed hypersensitivity rxn in those exposed – Negative in 15% of cases • Interferon-gamma release assay (IGRA) • Use CXR, CT not routine Treatment • TB Exposure – Contact with index case, but asymptomatic, neg TST and CXR – If < 4y/o or immunocompromised • INH pending results of repeat TST (2-3 mos) • LTBI – INH for 9mos – If intermittently dosed, used Directly Observed Tx Treatment • TB Disease – 4 drug Directly Observed Therapy – INH, rifampin, pyrazinamide, ethambutol – 6 months – If CNS involvement, 9-12 mos What about infant of TB mom? • Maternal LTBI… no workup or isolation for infant • Maternal positive TST and CXR abnl but not consistent with TB – Maternal AFB sputum smear neg – No isolation or workup for infant – Tx maternal LTBI What about infant of TB mom? • Mom with CXR consistent with TB – Evaluate infant for TB • CXR and PE – If infant is normal • Separate from mother until she is being treated and infant starts INH • Once on INH, separation unnecessary and may breastfeed Health Care Workers • Positive TST with normal CXR – Offer therapy for LTBI – Repeat screening should be done with CXR, not TST Prevention • Negative pressure and N95 use in children – Cavitary or extensive pulmonary involvement – AFB positive TB – Procedures such as intubation/bronchoscopy • BCG vaccine in US – Children continually exposed to MDR-TB – Continually exposed to adults who have infectious TB who cannot be removed from setting