* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
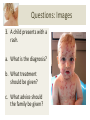
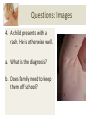
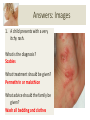
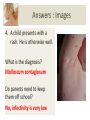
Download The Child with a Rash
Dirofilaria immitis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Orthohantavirus wikipedia , lookup
Trichinosis wikipedia , lookup
Yellow fever wikipedia , lookup
Typhoid fever wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Leptospirosis wikipedia , lookup
West Nile fever wikipedia , lookup
Hepatitis C wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Rotaviral gastroenteritis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Herpes simplex wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Oesophagostomum wikipedia , lookup
Neonatal infection wikipedia , lookup
Henipavirus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Hepatitis B wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Lymphocytic choriomeningitis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Infectious mononucleosis wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Schistosomiasis wikipedia , lookup
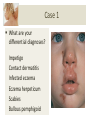
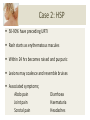
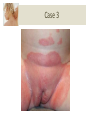
The Child with a Rash Lydia Burland Learning Outcomes By the end of the session students should; Be able to recognise common rashes presenting in childhood Know about common associations and red flag symptoms Be able to discuss initial management options and explain to parents Be able to answer questions on common infectious diseases and rashes Case 1 A 3 year old presents with a 2 day history of a pustular rash on his face and hands He is otherwise well, but keeps picking the scabs causing them to bleed 3 other children at nursery have a similar rash He is usually fit and well, with no PMH or allergies Case 1 What are your differential diagnoses? Impetigo Contact dermatitis Infected eczema Eczema herpeticum Scabies Bullous pemphigoid Case 1: Impetigo Very common superficial skin infection Usually due to staph. aureus or beta-haemolytic strep. Two forms: bullous or non-bullous (70%) Most common in pre-school children and warm (sweaty) environments Risk factors: poor hygiene and skin conditions Case 1: Impetigo Non-bullous: – – – – Initial vesicles, developing into honey-crusted plaques Minimal surrounding erythema Spreads rapidly Often regional lymphadenopathy Bullous: – Thin membranes that rupture spontaneously – More common with underlying eczema Diagnosis is clinical, though you can swab vesicular fluid for MC+S Case 1: Impetigo Conservative measures: – Avoid itching/touching – Avoid towel sharing Topical treatments: – Fusidic acid – Mupirocin (for MRSA carriers) Systemic treatment: – Flucloxacillin – Clarithromycin (for penicillin allergy) Case 1: Impetigo Complications include: – Cellulitis – Lymphadenitis – Staphlococcal scalded skin syndrome – Scarlet fever – Post-streptococcal glomerulonephritis Re-infection may occur in household contacts Case 2 A 9 year old presents with a 3 day history of cough, coryza and mild pyrexia In the last 24 hours a non-blanching macular rash has developed on his buttocks/legs He also has non-specific abdominal pain, and pain/swelling of his knees and ankles He has a PMH of asthma, and is allergic to nuts Case 2 Obs: HR 123, RR 32, T37 OE: Alert, but crying Coryzal, pink left TM HS I + II + 0, chest clear Abdo soft, generally tender, no masses Case 2 Florid, non-blanching purpuric rash on LL Pain and swelling of ankles bilaterally, with limited ROM What’s the diagnosis? Case 2: HSP Henoch-Schonlein purpura IgA mediated hypersensitivity vasculitis 90% of cases in childhood, peak 4-6 years Risk factors; Recent infection Environmental exposure Vaccinations Case 2: HSP 50-90% have preceding URTI Rash starts as erythematous macules Within 24 hrs becomes raised and purpuric Lesions may coalesce and resemble bruises Associated symptoms; Abdo pain Joint pain Scrotal pain Diarrhoea Haematuria Headaches Case 2: HSP HSP is self-limiting Management includes NSAIDs +/- steroids Complications; Renal involvement GI bleeding Intussusception Pulmonary haemorrhage Prognosis is excellent, however 25% may have recurrent symptoms Case 3 A 17 year old mum brings her 3 month old daughter in with ‘nappy rash’ It’s been present for ‘weeks’ and is getting worse She has been putting on regular sudocrem What are the differentials for nappy rash? Case 3 Case 3: Nappy Rash Very common under 18 months Risk factors include; Immunodeficiency Irritant soaps/detergents Poor nappy hygiene Diarrhoea Atopy Causes include; 1. Contact dermatitis 2. Candida infection 3. Superimposed bacterial infection Case 3: Nappy Rash 1. Contact dermatitis Erythema sparing skin folds Borders not well defined 2. Candida infection Erythema with well defined, raised borders No sparing of skin folds Satellite lesions 3. Superimposed bacterial infection Increased erythema and purulent discharge Case 3: Nappy Rash Management includes; Regular nappy changes (6-12/day) Thorough cleaning with water/baby wipes ‘Naked’, nappy-free time Barrier creams (zinc, metanium) Topical anti-fungals for candida infection (e.g. Clotrimazole, Miconazole) Topical antibiotics for bacterial infection (e.g. Fusidic acid) Topical steroids may also be used in severe cases (e.g. 0.5% hydrocortisone) Case 4 A 3 year old presents with 24 hrs of D+V Initially vomiting 4-5x day, mostly post feeds Now watery, offensive stools 12x day Low grade pyrexia 37.9, but otherwise well in himself What investigations are needed? Does he need admitting? Case 4 Obs: HR 105, RR 43, Sat 99%, T 37.8 OE: Alert and playing Moist mucous membranes, CRT <2s HS I + II + 0, chest clear Abdo soft but diffuse discomfort No masses or guarding Is he dehydrated? What should we do with him next? Case 4 NICE fluid challenge = 50mls/kg over 4 hours He manages to drink 22mls every 10 minutes without vomiting over the next 2 hrs His obs remain stable throughout and he is discharged home with safety netting advice Stool culture has been sent Case 4: Gastroenteritis Diarrhoea +/- vomiting is very common in childhood Risk factors include; Poor hygiene Immunodeficiency Lack of sanitation Undercooked meat Causes include; Rotavirus (>50%) Salmonella Shigella Campylobacter Norovirus E. coli Case 4: Gastroenteritis Investigation depends on presenting features, but may include; Stool MC+S FBC/U+E/cultures Management involves; Appropriate hand hygiene Oral rehydration where appropriate Abx only in septicaemia, salmonella + C Diff Avoid anti-diarrhoeals Safety netting advice Majority resolve within 5-7 days Breastfeeding and rotarix vaccine are preventative Summary Infectious diseases and rashes are common in childhood For your exams; Recognise key rashes (google/patient.co.uk) Know about causative organisms Be able to recommend treatment Be able to advise families re: infectivity Know about important complications Questions Questions: MCQs 1. The most common cause of gastroenteritis is...? a. E. Coli c. Salmonella b. Adenovirus d. Rotavirus 2. The most common cause of opthalmia neonatorum is...? a. Chlamydia T. b. N. gonorrhoeae c. Haemophilus inf. d. Staph. aureus Questions: MCQs 3. Bullous impetigo is most commonly caused by...? a. Group A strep. c. Staph aureus b. Β-haemolytic strep. d. Haemophilus inf. 4. HSP is...? a. IgA mediated b. IgG mediated c. Common in adults d. Secondary to staph. aureus Questions: EMQ 1 a. b. c. d. Erythema toxicum Kawasaki disease Measles Rubella e. Chicken pox f. Glandular fever g. Mumps h. Milia 1. A 2 day old baby has erythematous macules and occasional pustules on his trunk. He is otherwise well. 2. An unimmunised 3 year old presents with a rash that started on her head, and has since spread down her body. She also has a cough and bilateral conjunctivitis. There are white ‘spots’ seen inside her mouth. Questions: EMQ 1 a. b. c. d. Erythema toxicum Kawasaki disease Measles Rubella e. Chicken pox f. Glandular fever g. Mumps h. Milia 3. A 7 year old presents with fever and rash. The rash was initially vesicular but has now crusted over. 4. An unimmunised 3 year old presents with a pink rash and lymphadenopathy. The rash started behind her ears and has spread to her trunk. Questions: EMQ 1 a. b. c. d. Erythema toxicum Kawasaki disease Measles Rubella e. Chicken pox f. Glandular fever g. Mumps h. Milia 5. A newborn has several tiny raised, pearly-white papules on either side of his nose. 6. A 15 year old boy presents with several weeks of lethargy and low fever. He has a sort throat and did have a fine macular rash that has now gone. Questions: EMQ 2 a. b. c. d. Staph. Aureus Epstein-Barr virus Herpes simplex Strep. Pyogenes e. Varicella zoster f. E. Coli 0157 g. Pox virus h. Campylobacter 1. A 15 year old presents with an itchy maculopapular rash. He has just started antibiotics for tonsillitis. 2. A 7 year old with known eczema presents with rapidly worsening eczema that is painful. On examination you see multiple vesicles. Questions: EMQ 2 a. b. c. d. Staph. aureus Epstein-Barr virus Herpes simplex Strep. pyogenes e. Varicella zoster f. E. Coli 0157 g. Pox virus h. Campylobacter 3. A 4 year old presents with firm, circular papules on his torso. They are painless and have an umbilicated centre. 4. A 4 year presents with haematuria. He has had 7 days of diarrhoea, which has contained blood for the last 3 days. Questions: EMQ 2 a. b. c. d. Staph. aureus Epstein-Barr virus Herpes simplex Strep. pyogenes e. Varicella zoster f. E. Coli 0157 g. Pox virus h. Campylobacter 5. A 2 year old comes back from nursery with 2 peri-oral vesicles. The next day they have burst and left a honey-coloured scab. 6. A 12 year presents with 24 hrs of D+V. He is concerned as he has passed fresh blood per rectum. Questions: Images 1. A child presents with a very itchy rash. a. What is the diagnosis? b. What treatment should be given? c. What advice should the family be given? Questions: Images 2. Mum notices the following in her babies mouth. a. What is the diagnosis? b. What treatment should be given? Questions: Images 3. A child presents with a rash. a. What is the diagnosis? b. What treatment should be given? c. What advice should the family be given? Questions: Images 4. A child presents with a rash. He is otherwise well. a. What is the diagnosis? b. Does family need to keep them off school? Answers Answers: MCQs 1. The most common cause of gastroenteritis is...? a. E. Coli c. Salmonella b. Adenovirus d. Rotavirus Rotavirus is responsible for >50% of all cases of gastroenteritis. It is self-limiting and no treatment is required. Answers : MCQs 2. The most common cause of opthalmia neonatorum is...? a. Chlamydia T. c. Haemophilus inf. b. N. gonorrhoeae d. Staph. Aureus Opthalmia neonatorum is conjunctivitis in the first 28 days of life. Chlamydia is the most common causative organism, usually presenting 5-14 days after birth. Answers : MCQs 3. Bullous impetigo is most commonly caused by...? a. Group A strep. c. Staph aureus b. Β-haemolytic strep. d. Haemophilus inf. The majority of impetigo is non-bullous and is caused by beta haemolytic strep or staph aureus. If impetigo is bullous, it is almost always due to staph aureus infection. Answers : MCQs 4. HSP is...? a. IgA mediated b. IgG mediated c. Common in adults d. Secondary to staph. Aureus HSP is an IgA mediated vasculitis most common in children. The underlying cause is unknown but it may follow recent infection or vaccinations. When it does occur in older children or adolescents the disease tends to be more severe and associated with more renal complications. Answers: EMQ 1 1. A 2 day old baby has erythematous macules and occasional pustules on his trunk. He is otherwise well. a. Erythema toxicum Erythema toxicum neonatorum is a noninfective rash occurring in the first 28 days of life. It is self limiting. Questions: EMQs 2. An unimmunised 3 year old presents with a rash that started on her head, and has since spread down her body. She also has a cough and bilateral conjunctivitis. There are white ‘spots’ seen inside her mouth. c. Measles Measles is due to morbillivirus infection transmitted by airbourne respiratory droplets. It presents with a rash, most commonly starting on the head and spreading downwards, coryza, conjunctivitis and koplik spots.Measles is usually self-limiting, but may be complicated by pneumonia and encephalitis. It is a notifiable disease. Answers: EMQ 1 3. A 7 year old presents with fever and rash. The rash was initially vesicular but has now crusted over. e. Chicken pox Chicken pox is very common and due to varicella zoster virus. It enters via the upper respiratory tract, and presents with fever and malaise, before vesicles appear around day 3-5. They are infective prior to the rash appearing until all the vesicles have scabbed over. Patients should be advised against itching, and given antipyretics/analgesia as required. Answers: EMQ 1 4. An unimmunised 3 year old presents with a pink rash and lymphadenopathy. The rash started behind her ears and has spread to her trunk. d. Rubella Rubella is usually and mild and self-limiting illness, and presents with a rash starting behind the ears and spreading down the trunk. The main concern regarding rubella is its effect on the growing foetus. Answers: EMQ 1 5. A newborn has several tiny raised, pearlywhite papules on either side of his nose. h. Milia Answers: EMQ 1 6. A 15 year old boy presents with several weeks of lethargy and low fever. He has a sort throat and did have a fine macular rash that has now gone. f. Glandular fever Infectious mononucleosis, or glandular fever, is a self limiting infection usually caused by Epstein Barr virus. It presents with fever and malaise over a few weeks to months, sore throat and enlarged tonsils and a transient fine macular rash. Patients may later develop transient splenomegaly and should be advised against contact sports for the next month to avoid splenic rupture. Answers: EMQ 2 1. A 15 year old presents with an itchy maculopapular rash. He has just started antibiotics for tonsillitis. b. Epstein-Barr virus This is a common presentation of infectious mononucleosis – the child is treated for presumed tonsillitis with amoxicillin, resulting in a florid maculopapular rash. Answers: EMQ 2 2. A 7 year old with known eczema presents with rapidly worsening eczema that is painful. On examination you see multiple vesicles. c. Herpes simplex This describes eczema herpeticum – herpes simplex infection complicating known eczema. It is characterised by fever, painful rash and clusters of vesicles. Answers: EMQ 2 3. A 4 year old presents with firm, circular papules on his torso. They are painless and have an umbilicated centre. g. Pox virus This describes molloscum contagiosum – firm painless papules appearing in crops with an punctate centre. They are caused by pox virus and are self-limiting though may take months to resolve. Answers: EMQ 2 4. A 4 year presents with haematuria. He has had 7 days of diarrhoea, which has contained blood for the last 3 days. f. E. Coli 0157 This describes a likely cause of haemolytic uraemic syndrome which most commonly follows e.coli 0157 infection. It tends to occur 6-8 post diarrhoea and presents with haematuria, fever and lethargy. Blood tests show haemolytic anaemia, thrombocytopenia and renal impairment. Answers: EMQ 2 5. A 2 year old comes back from nursery with 2 peri-oral vesicles. The next day they have burst and left a honey-coloured scab. a. Staph. Aureus/d. Strep. Pyogenes This describes impetigo which may be due to beta haemolytic strep, such as strep pyogenes or staph aureus. Answers: EMQ 2 6. A 12 year presents with 24 hrs of D+V. He is concerned as he has passed fresh blood per rectum. h. Campylobacter Campylobacter is the most common cause of bloody diarrhoea secondary to food poisoning, and is due to eating under meat, especially chicken. Answers: Images 1. A child presents with a very itchy rash. What is the diagnosis? Scabies What treatment should be given? Permethrin or malathion What advice should the family be given? Wash all bedding and clothes Answers : Images 2. Mum notices the following in her babies mouth. What is the diagnosis? Oral candidiasis What treatment should be given? Oral antifungal, i.e. Nystatin or daktarin Answers : Images 3. A child presents with a rash. What is the diagnosis? Chicken pox What treatment should be given? Supportive (unless immunosupressed) What advice should the family be given? Contagious until all vesicles scab over Avoid pregnant women Answers : Images 4. A child presents with a rash. He is otherwise well. What is the diagnosis? Molloscum contagiosum Do parents need to keep them off school? No, infectivity is very low Any questions? Thanks for listening