* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download What comes after Ancef? A guide to antimicrobial
Antimicrobial surface wikipedia , lookup
Bacterial cell structure wikipedia , lookup
Human microbiota wikipedia , lookup
Gastroenteritis wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Infection control wikipedia , lookup
Neonatal infection wikipedia , lookup
Triclocarban wikipedia , lookup
Antibiotics wikipedia , lookup
Urinary tract infection wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Bacterial morphological plasticity wikipedia , lookup
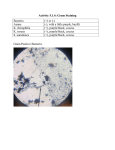
What comes after Ancef? A guide to antimicrobial prophylaxis in the surgical patient Course Objectives 1. Identify commonly used antibiotics in the surgical setting 2. Describe the mechanism of action of commonly used antibiotics 3. Identify common surgical pathogens 4. Discuss current guidelines for antimicrobial prophylaxis during surgery EVERYONE JOIN THE FUN! pollev.com/meaghanmcclo717 Before we figure out what weapons we need to use we first need to know who the enemies are Gram staining By Graevemoore at English Wikipedia, CC BY-SA 3.0 https://commons.wikimedia.org/w/index.php?curid=8477969 Meet Staph Aureus › Aerobic gram positive cocci › Is the primary cause of the majority SSI (up to 30 %) › Staph aureus is ubiquitous. Part of the natural flora of the skin and mucous membranes. › Colonization occurs in about 1 in 4 patients and increases the risk of SSI by up to 14 fold › Harmless until it penetrates deeper tissues Enzymes secreted by staph A. › Coagulase: Converts fibrinogen into fibrin to form clots. Prevents phagocytosis. › Staphylokinase: dissolves fibrin, spreads the bacteria › Deoxyrobonuclease: breaks down DNA › Beta-lactamase – degrades the beta lactam ring and causes drug resistance. Other gram positive organisms › Staph epidermis known for its bio slime and occurs in sternal wounds and prosthesis › Streptococcus, commonly found in mouth throat skin and intestine are commonly found SSI bacteria and can cause hemolysis. Common subtypes include Streptococcus pyogenes and Enterococcus. › Streptococcus pyogenes: Group A streptococcus is responsible for type II necrotizing fasciitis › Enterococcus: present in the adult GI tract and account for a large amount of clean contaminated SSI › All of these bacteria can be either aerobic or anaerobic Anaerobic Gram positive bacilli › Members of the clostridium species › Cause tetanus and botulism, but are not common in surgical site infection › Clostridium perfringens causes the surgical site infection known as “gas gangrene” › C difficile occurs when the normal flora of the intestine are eliminated by prolonged antibiotic therapy- may lead to toxic megacolon Gram positive cocci account for nearly 50% of all surgical site infections Gram negative bacilli › Primarily found in the intestines › Account for about 20 % Of surgical site infections › . Enterobacter spp, › Escherichia coli (E coli ) › Klebsiella pneumoniae Anaerobic gram negative organisms: BACTEROIDES FRAGILIS › Most common anaerobe in intraabdominal infections › Has the tendency to form capsules and are notorious for the formation of appendicitic abscess Now that we know what we are fighting, let’s see what tools we have to use Beta Lactam Antibiotics › Are the most commonly prescribed antibiotic for surgical site infection › They work by inactivating a set of enzymes that are necessary for cell wall synthesis › These enzymes are called penicillin binding proteins (PBP) and different bacteria have anywhere between 4 and 8 of them › Each PBP has a different function depending on the bacteria and each of the beta lactam drugs impact cell wall synthesis diffently › Cover a broad spectrum of microorganisms and we will look at them more closely later in the lecture › Anaphylaxis is the primary concern Beta Lactam Antibiotics Penicillins Narrow spectrum Not commonly used perioperatively Cephalosporins Broad Spectrum Ampicillin 1st Generation Cefazolin 2nd Generation 3rd Generation Cefuroxime Cefotaxime Cefoxitin Ceftriaxone Cefotetan 4th and 5th Generation Not commonly used perioperatively Carbapenems Monobactams Ertapenem Aztreonam Beta lactamase inhibitors Sulbactam Tazocactam Selection of antimicrobial agent Appropriate spectrum of activity Inexpensive Cefazolin Desirable side effect profile Appropriate duration of action Beta lactam allergy › Patients who have a penicillin allergy generally react to either the beta lactam ring or the R group side chain › 2% of patients who are skin test positive for penicillin have a cross sensitivity to cephalosporins › There is a 1% chance of cross sensitivity with carbapenems › There is no evidence of cross sensitivity with aztreonam › All of these drugs are safe to use if the allergy is not IgE mediated Quinolones › Levofloxacin › Ciprofloxacin › Bind to the enzymes that are involved with DNA synthesis leading to cell death › Largest degree of activity is against gram negative bacilli and gram negative rods. Limited activity against staph and enterococcus › Adverse effects include C-Diff colitis, peripheral neuropathy and tendon rupture Aminoglycosides › Gentamycin › Works by inhibiting translocation of DNA to RNA › Activity primarily against aerobic gram negative bacteria › Nephrotoxic › Ototoxic › Neuromuscular blockade and is contraindicated in myasthenia gravis Clindamycin (lincosamide antibiotic) › Inhibits bacterial protein synthesis, and is bacteriostatic ( as opposed to bactericidal) › Activity against MRSA, Gram positive bacteria and Anaerobes › Adverse reactions: C-diff colitis Metronidazole › Mainstay of treatment for obligate anaerobic bacteria (C-Diff) › Its low molecular weight allows it to pass easily into the cell and destabilize the DNA helix › Can turn urine into a red brown color › Can cause flushing and tachycardia and nausea on vomiting if given to patients who have had alcohol Vancomycin › A glycopeptide antibiotic › Spectrum of activity include gram positive bacteria including MRSA › Routine prophylaxis with vancomycin is not recommended for any surgical procedure in an effort to control vancomycin resistance › Should be reserved for patients that are MRSA positive of institution that are experiencing clusters of MRSA. › Adverse reaction includes red man syndrome › Ototoxic › nephrotoxic Now lets put it all together Recommendations Orthopedic procedures › Procedures with implantation, the recommendation is cefazolin which covers gram positive staph and e-coli › 2nd generation cephalosporin are equally as effective in preventing surgical site infection, but are more costly, and have a broader spectrum which may contribute to resistance and C-Diff › Vancomycin and clindamycin are alternatives for patients with a beta lactam allergy Orthopedic procedures not involving implantation › Arthroscopy of the knee hand and foot have low infection rates › These guidelines do not recommend antibiotics Cardiac procedures › Recommendation: cefazolin or a 2nd generation cephalosporin (cefuroxime) › Vancomycin or clindamycin is acceptable in a beta lactam allergy Thoracic Procedures › Thoracic procedures can also carry the risk of pneumonia. Some studies indicate that ampicillin-sulbactam is more effective than cephalosporins › The recommendation is cefazolin or ampicillin-sulbactam Urologic procedures › The primary concern for urologic procedures entering the urinary tract is bacteriuria cased by E. Coli and other gram negative bacilli › The recommendation is Fluoroquinolones. › Procedures that enter the urinary tract through the skin will require cefazolin plus a strong gram negative like gentamicin or a fluoroquinolone Surgeries of the bowel › The natural flora of the bowel changes as you travel down the intestine › Patients with a small bowel obstruction or appendicitis get treated the same way as patients undergoing bowel surgery Biliary Tract • E. Coli (G-) • Klebiella (G-) • Enterococci (G+) Small Intestine • E. Coli (G-) • Klebiella (G-) • Enterococci (G+) Colon • B fragilis (anaerobe) • E coli Surgeries of the Gastrointestinal tract › Biliary tract recommendations: › Cefazolin. Studies show that there is no difference between 1st 2nd and 3rd generations cephalosporins › Small Bowel recommendations: › Cefazolin Unless there is small bowel obstruction then the recommendation is for a 2nd generation cephalosporin or cefazolin and metronidazole. › Colorectal recommendations (including Appendectomy) › 2nd generation cephalosporins or cefazolin and metronidazole Head and Neck procedures › Clean head and neck procedures, as well as tonsillectomy and endoscopic sinus surgeries have a very low rate of infection, and do not require antibiotic prophylaxis › Clean-contaminated, commonly head in neck cancer, are very complex do to the flora of the mouth, › Recommendations for clean contaminated procedures › 1st or 2nd generation cephalosporin with the addition of metronidazole › For patients with a beta lactam allergy, clindamycin plus gentamycin covers the gamut. Reference 1. CDC. New York activities to prevent HAIs. http://www.cdc.gov/HAI/stateplans/state-hai-plans/ny.html. Accessed September 24, 2016. 2. Qadan M, Cheadle WG. Common microbial Pathogens in surgical practice. Surgical Clinics of North America. 2009;89(2):295–310. doi:10.1016/j.suc.2008.09.002. 3. Calderwood, SB. Beta-lactam antibiotics: Mechanisms of action and resistance and adverse effects. In: Up to Date, Hooper, DC. (Ed), UpToDate.Waltham, MA. (Accessed on August 28, 2016.) 4. Solenski, R, SB. Penicillin-allergic patients: Use of cephalosporins, carbapenems, and monobactams. In: Up to Date, Adkinsen, NF. (Ed), UpToDate.Waltham, MA. (Accessed on Sept 02, 2016.) 5. Bratzler DW, Dellinger EP, Olsen KM, et al. Clinical practice guidelines for antimicrobial prophylaxis in surgery. American Journal of Health-System Pharmacy. 2013;70(3):195–283. doi:10.2146/ajhp120568. 6. Hooper DC. Fluoroquinolones . In: Up to Date, Calderwood SB. (Ed), UpToDate.Waltham, MA. (Accessed on Sept 01, 2016.) 7. Johnson M. Clindamycin: An overview In: Up to Date,Hooper DC. (Ed), UpToDate.Waltham, MA. (Accessed on August 21, 2016.) 8. Johnson M. Metronidazole: An overview In: Up to Date,Hooper DC. (Ed), UpToDate.Waltham, MA. (Accessed on August 21, 2016.) 9. Drew, R. Clindamycin: Vancomycin dosing and serum concentration monitoring in adults ,Hooper DC. (Ed), UpToDate.Waltham, MA. (Accessed on August 24, 2016.)