* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download COMA AND BRAIN DEATH
Survey
Document related concepts
Transcript
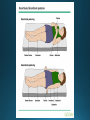
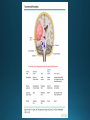
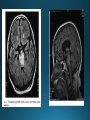
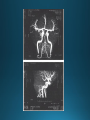
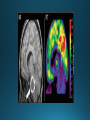
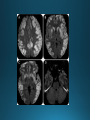
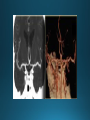
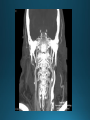
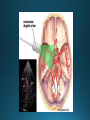
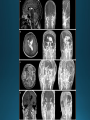
COMA AND BRAIN DEATH Introduction Coma – clinical state in which patients have impaired responsiveness (or are unresponsive) to external stimulation and are either difficult to arouse or are unarousable. Stupor, lethargy and obtundation – states between alertness and coma. An alteration in arousal – acute, life treating emergency Etiologies and pathophysiology • ARAS (ascending reticular activating system) • Tegmentum (upper pons and midbrain) –diencephalon (thalamus & hypothalamus) – cerebral cortex • Cerebral hemispheres – must be bilateral/or large unilateral • Toxic, metabolic, infection, hypothermia • Multiple medical conditions • ER presentation: TBI, stroke, intoxications, infections, metabolic disturbance History • History from witnesses, friends, family members • The patient’s personal belongings (bracelet, wallet, list of medications) • Old hospital chart General examination • • • • • • • • • Vital signs (HTN-PRES, ICH, hypotension-sepsis, cardiac failure) Ventilatory pattern Hyperthermia (infection, heat stroke, anticholinergic) Hypothermia (accidental, primary-hypothalamic dysfunction-Wernicke, secondary-adrenal failure, hypothyroidism, sepsis, EtOH, drugs) Cutaneous and mucosal abnormalities, bullous lesions- barbiturate Perspiration (fevers, hypoglycemia, pheochromocytoma) Jaundice, cherry red color-CO, pallor – uremia, anemia, myxedema Needle tracks CSF rhinorrhea Neurologic examination • Level of consciousness • Motor responses • Cranial nerves • Brainstem reflexes: pupillary light, extraocular and corneal • Coma syndromes • Herniation syndromes • Brainstem lesions • Metabolic coma • Toxic syndromes Coma syndromes Herniation syndromes • Transtentorial herniation (expanding mass lesions) • Horizontal shifts- pineal body >8mm (some impairment of consciousness), >11 mm = usually comatose • Papilledema • Cushing’s triad: HTN, bradycardia, irregular respiration • CENTRAL HERNIATION • UNCAL HERNIATION (ipsilateral III -mydriasis, downward and outward eye deviation. Loss of contralateral pupil reactivity=brainstem lesion Brainstem lesions • Infarction or hemorrhage of the upper pons and/or midbrain • Osmotic demyelination syndrome (CPM) • Brainstem encephalitis • Asymmetric eye movements, small pupils Metabolic coma • Symmetrical nature of neurologic deficits • Exceptions: hypo or hyperglycemia-lateralized motor findings • Tremor, asterixis, multifocal myoclonus • Decreased muscle tone • Less common cerebrate posturing • Pupils abnormal, symmetric, constrict with light Toxic syndromes Conditions mistaken for coma • Locked-in syndrome • Akinetic mutism • Psychogenic unresponsiveness Locked-in syndrome • Focal injury to the base of the pons (BA embolic occlusion) • Consciousness is preserved • Can voluntary blink and vertical eye movements Akinetic mutism • A lack of motor response in an awake individual • Prefrontal or premotor (supplementary motor) areas –executive problem • The patient follows with the eyes but does not initiate other movements or obey commands • Muscle tone, reflexes and postural reflexes usually intact Psychogenic unresponsiveness • Resist passive eye opening • Roll over when tickled • Turn the eyes towards the floor • Nonepileptic seizures • Catatonia-preserved ability to maintain posture (sitting or standing) Diagnosis • Laboratory tests • Neuroimaging • Lumbar puncture • EEG Management Prognosis • Coma – transitional state that rarely lasts > several weeks (except in cases of ongoing sedative therapies or protracted sepsis) • Recovery of brain death/persistent vegetative or minimally conscious state • Depends on the underlying etiology, severity of the insult and other premorbid factors, including age Brain death Death is an irreversible, biological event that consists of permanent cessation of the critical functions of the organism as a whole. Brain death qualifies as death, as the brain is essential for integrating critical functions of the body. Permanent absence of cerebral and brainstem functions. 1959 – the first concept of irreversible coma or brain death TBI and SAH, ICH, hypoxic ischemic encephalopathy, ischemic stroke Clinical criteria • Clinical setting • Neurological examination • Apnea test • Observation period • Examiner(s) Clinical setting • Clinical or neuroimaging evidence of an acute CNS catastrophe • Exclusion of complicating medical conditions (no severe electrolyte, acid-base, endocrine or circulatory disturbance) • No drug intoxication or poisoning • Core temperature >36C (97F) • Normal SBP>100 mm Hg (vasopressors may be required) Neurologic examination It must demonstrate absent cerebral or brainstem function with all of the following findings: • Coma • Absent brain-originating motor response, including response to pain above the neck or other brain-originating movements (seizures, decerebrate or decorticate posturing) • Absent pupillary light reflex (midposition or dilated (4-9 mm) • Absent corneal reflexes • Absent oculovestibular reflexes (caloric responses) • Absent jaw reflex • Absent gag, sucking or rooting reflex • Absent cough with tracheal suctioning Neurologic examination Movements originating from the spinal cord or peripheral nerve may occur in brain death – common- 33-75% • Semi-rhythmic facial movements • Finger flexor movements • Tonic neck reflexes – “Lazarus sign” • Triple flexion response – plantar response • Asymmetrical opisthotonic posturing of the trunk • Alternating flexion-extension of the toes • Upper limb pronation extension reflex • Widespread fasciculations of trunk and extremities Apnea test • Performed after all other criteria for brain deathhave been met • Core temperature >36C • SBP>100 mm Hg • Absence of hypoxia • Euvolemia Not valid in patients with chronic >PaCO2, neuromuscular paralysis or high cervical spinal cord lesion. Preoxygenation POSITIVE TEST: no respiratory response to a PaCO2>60 mm HG or 20 mm Hg greater than baseline values and a final arterial pH<7.28. 8-10 min Observation period • Varies extensively • 24 hours for adults • 48 hours for children Examiner(s) • Varies by the state and country Ancillary tests Brain blood flow • Cerebral angiography • TCD • MRA • CTA • Nuclear medicine Electrophysiology • EEG • EP Other tests • Atropine test (3mg IV, >HR<3%) Brain death mimics • Locked-in syndrome • Neuromuscular paralysis (acute, severe PN or with neuromuscular blocking agents) • Hypothermia • Drug intoxication • Guillain-Barre syndrome