* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download neuroassess
Cortical stimulation mapping wikipedia , lookup
Craniometry wikipedia , lookup
History of anthropometry wikipedia , lookup
History of neuroimaging wikipedia , lookup
Hemiparesis wikipedia , lookup
Auditory system wikipedia , lookup
Lumbar puncture wikipedia , lookup
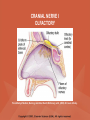
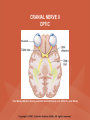
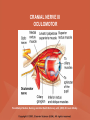
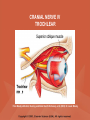
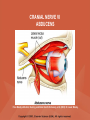
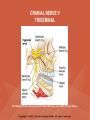
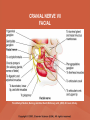
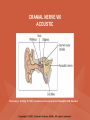
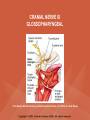
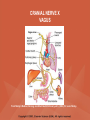
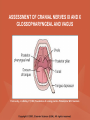
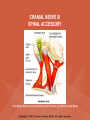
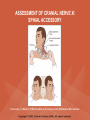
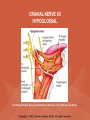
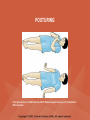
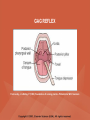
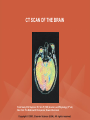
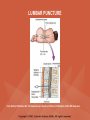
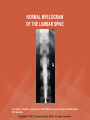
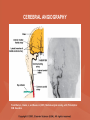
NEUROLOGICAL SYSTEM ASSESSMENT PYRAMID POINTS • Risk factors associated with neurological disorders • Neurological assessment • Cranial nerve assessment • Glasgow coma scale • Preprocedure and postprocedure nursing care and client education • Positioning a client following a diagnostic procedure ASSESSMENT OF RISK FACTORS • • • • • • Trauma Hemorrhage Tumors Infection Toxicity Metabolic disorders ASSESSMENT OF RISK FACTORS • • • • • Hypoxic conditions Deficiency conditions Hypertension Cigarette smoking Stress ASSESSMENT OF CRANIAL NERVE I OLFACTORY • Cranial nerve I: (olfactory) sensory, smell • Have the client close eyes and occlude one nostril with finger • Ask the client to identify nonirritating odors such as coffee, tea, cloves, soap, chewing gum, and peppermint • Repeat the test on the other nostril CRANIAL NERVE I OLFACTORY From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF CRANIAL NERVE II OPTIC • Cranial nerve II: (optic) sensory, vision • Assess visual acuity with a Snellen chart or newspaper or ask the client to count how many fingers the examiner is holding up • Check visual fields by confrontation • Have the client sit directly in front of examiner and stare at examiner's nose • Examiner slowly moves his or her finger from the periphery towards the center until the client says it can be seen • Check color vision by asking the client to name the color of several nearby objects CRANIAL NERVE II OPTIC From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. CRANIAL NERVE II: OPTIC ASSESSING VISUAL FIELDS From Leahy, J. & Kizilay, P. (1998). Foundations of nursing practice. Philadelphia: W.B. Saunders ASSESSMENT OF CRANIAL NERVES III, IV, VI OCULOMOTOR, TROCHLEAR, ABDUCENS • • • • Cranial nerve III (oculomotor) Cranial nerve IV (trochlear) Cranial nerve VI (abducens) The motor functions of these nerves overlap; therefore, they need to be tested together • First, inspect the eyelids for ptosis (drooping), then assess ocular movements and note any eye deviation • Test accommodation and direct and consensual light reflexes ASSESSMENT OF CRANIAL NERVES III, IV, VI OCULOMOTOR, TROCHLEAR, ABDUCENS • Cranial nerve III: (oculomotor) motor – Assesses pupillary constriction, upper eyelid elevation, and most eye movement • Cranial nerve IV: (trochlear) motor – Assesses downward and inward eye movement • Cranial nerve VI: (abducens) – Assesses lateral eye movement CRANIAL NERVE III OCULOMOTOR From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. CRANIAL NERVE IV TROCHLEAR From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. CRANIAL NERVE VI ABDUCENS From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF CRANIAL NERVE V TRIGEMINAL • Cranial nerve V: (trigeminal) sensory and motor • Assesses sensation to the cornea, nasal and oral mucosa, facial skin, and mastication • To test motor function, ask the client to close jaws tightly then try to separate the clenched jaw • Test the corneal reflex by lightly touching the client's cornea with a cotton wisp • Check sensory function by asking the client to close the eyes, then lightly touch the forehead, cheeks, and chin noting if the touch can be felt equally on both sides CRANIAL NERVE V TRIGEMINAL From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF THE CORNEAL REFLEX From Lemmi FO, Lemmi CAE: Physical assessment findings CD-ROM, Philadelphia, 2000, W.B. Saunders. ASSESSMENT OF CRANIAL NERVE VII FACIAL • Cranial nerve VII: (facial) sensory and motor • Tests taste perception on the anterior two-thirds of the tongue • Have the client show the teeth • Attempt to close the client's eyes against resistance and ask the client to puff out his or her cheeks • Place sugar, salt, or vinegar on the front of the tongue and have the client identify these substances by their tastes CRANIAL NERVE VII FACIAL From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF CRANIAL NERVE VIII ACOUSTIC • Cranial nerve VIII: (acoustic) sensory • The ability to hear tests the cochlear portion • The sense of equilibrium tests the vestibular portion • Check the client's ability to hear a watch ticking or a whisper • Observe the client's balance and observe for swaying when walking or standing CRANIAL NERVE VIII ACOUSTIC From Leahy, J. & Kizilay, P. (1998). Foundations of nursing practice. Philadelphia: W.B. Saunders ASSESSMENT OF CRANIAL NERVE IX GLOSSOPHARYNGEAL • Cranial nerve IX: (glossopharyngeal) sensory and motor • Assesses swallowing ability • Assesses sensation to the pharyngeal soft palate and tonsillar mucosa, and taste perception on the posterior third of the tongue and salivation CRANIAL NERVE IX GLOSSOPHARYNGEAL From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF CRANIAL NERVE X VAGUS • Cranial nerve X: (vagus) sensory and motor • Assesses swallowing and phonation, sensation to the exterior ear's posterior wall, and sensation behind the ear • Assesses sensation to the thoracic and abdominal viscera CRANIAL NERVE X VAGUS From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF CRANIAL NERVES IX AND X GLOSSOPHARYNGEAL AND VAGUS • Cranial nerve IX: (glossopharyngeal) • Cranial nerve X: (vagus) • Have the client identify a taste at the back of the tongue • Inspect the soft palate and observe for symmetrical elevation when the client says "aah" • Touch the posterior pharyngeal wall with a tongue depressor to elicit a gag reflex ASSESSMENT OF CRANIAL NERVES IX AND X GLOSSOPHARYNGEAL AND VAGUS From Leahy, J. & Kizilay, P. (1998). Foundations of nursing practice. Philadelphia: W.B. Saunders ASSESSMENT OF CRANIAL NERVE XI SPINAL ACCESSORY • Cranial nerve XI: (spinal accessory) motor • Assesses uvula and soft palate movement, sternocleidomastoid, and trapezius muscle • Assesses upper portion of the trapezius muscle, which governs shoulder movement and neck rotation • Palpate and inspect the sternocleidomastoid muscle as the client pushes the chin against the examiner’s hand • Palpate and inspect the trapezius muscle as the client shrugs the shoulders against the examiner’s resistance CRANIAL NERVE XI SPINAL ACCESSORY From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF CRANIAL NERVE XI SPINAL ACCESSORY From Leahy, J. & Kizilay, P. (1998). Foundations of nursing practice. Philadelphia: W.B. Saunders ASSESSMENT OF CRANIAL NERVE XII HYPOGLOSSAL • Cranial nerve XII: (hypoglossal) motor • Assesses tongue movements involved in swallowing and speech • Observe the tongue for asymmetry, atrophy, deviation to one side, and fasciculations • Ask the client to push the tongue against a tongue depressor, then have the client move the tongue rapidly in and out and from side to side CRANIAL NERVE XII HYPOGLOSSAL From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. ASSESSMENT OF LEVEL OF CONSCIOUSNESS • Assesses cerebral function • Assess client behavior to determine level of consciousness such as confusion, delirium, unconsciousness, stupor, and coma ASSESSMENT OF RESPIRATIONS • CHEYNE-STOKES – Rhythmical with periods of apnea – Can indicate a metabolic dysfunction or dysfunction in the cerebral hemisphere or basal ganglia • NEUROGENIC HYPERVENTILATION – Regular, rapid, deep, sustained respirations – Indicates a dysfunction to the low midbrain and middle pons ASSESSMENT OF RESPIRATIONS • APNEUSTIC – Irregular respirations with pauses at the end of inspiration and expiration – Indicates a dysfunction to the middle or caudal pons • ATAXIC – Totally irregular in rhythm and depth – Indicates a dysfunction in the medulla ASSESSMENT OF RESPIRATIONS • CLUSTER – Clusters of breaths with irregularly spaced pauses – Indicates a dysfunction in the medulla and pons ASSESSMENT OF PUPILS • Size • Equality • Reactions to light described as brisk, slow, or fixed • Unusual eye movements • Unilateral pupil dilation indicates compression of the third cranial nerve • Mid-position, fixed pupil indicates midbrain injury • Pinpoint, fixed pupil indicates pontine damage RESPIRATORY PATTERNS AND PUPIL APPEARANCES From Black, J., Hawks, J., and Keene, A. (2001). Medical-surgical nursing, ed 6, Philadelphia: W.B. Saunders. ASSESSMENT OF TEMPERATURE • An elevated temperature increases the brain's metabolic rate • A rapid rise in temperature indicates a dysfunction of the hypothalamus or brain stem • A slow rise in temperature may indicate infection ASSESSMENT OF MOTOR FUNCTION • Muscle tone including strength and equality • Voluntary and involuntary movements • Purposeful and nonpurposeful movements ASSESSMENT FOR POSTURING • POSTURING – Indicates a deterioration of the condition • FLEXION (DECORTICATE POSTURING) – Client flexes one or both arms on the chest and may stiffly extend the legs – Indicates a nonfunctioning cortex ASSESSMENT FOR POSTURING • EXTENSOR (DECEREBRATE POSTURING) – Client stiffly extends one or both arms and possibly the legs – Indicates a brain stem lesion • FLACCID POSTURING – Client displays no motor response in any extremity POSTURING From Ignatavicius, D. & Workman, M. (2001). Medical-surgical nursing, ed 6, Philadelphia: W.B. Saunders. ASSESSMENT OF REFLEXES • BABINSKI’S REFLEX – Dorsiflexion of the ankle and great toe with fanning of the other toes – Indicates a disruption of the pyramidal tract • CORNEAL REFLEX – Loss of the blink reflex – Indicates a dysfunction of cranial nerve V • GAG REFLEX – Loss of the gag reflex – Indicates a dysfunction of cranial nerves IX and X BABINSKI’S REFLEX IN AN ADULT From Mosby’s Medical, Nursing, and Allied Health Dictionary, ed 6, (2002). St. Louis: Mosby. CORNEAL REFLEX From Lemmi FO, Lemmi CAE: Physical assessment findings CD-ROM, Philadelphia, 2000, W.B. Saunders. GAG REFLEX From Leahy, J. & Kizilay, P. (1998). Foundations of nursing practice. Philadelphia: W.B. Saunders ASSESSMENT OF MENINGEAL IRRITATION • Nuchal rigidity • Irritability • Fever ASSESSMENT OF MENINGEAL IRRITATION • KERNIG’S SIGN – Flexion of the thigh and knee to right angles, and when extended, causes spasm of hamstring and pain • BRUDZINSKI’S SIGN – Flexion of the head causes flexion of both thighs at the hips, and knee flexion NUCHAL RIGIDITY KERNIG’S AND BRUDZINSKI’S SIGNS From Monahan, F. & Neighbors, M. (1998). Medical-surgical nursing: Foundations for clinical practice, ed 2, Philadelphia: W.B. Saunders. ASSESSMENT OF THE AUTONOMIC SYSTEM • SYMPATHETIC FUNCTIONS/ADRENERGIC RESPONSES – Increased pulse and blood pressure – Dilated pupils – Decreased peristalsis – Increased perspiration ASSESSMENT OF THE AUTONOMIC SYSTEM • PARASYMPATHETIC FUNCTION/CHOLINERGIC RESPONSES – Decreased pulse and blood pressure – Constricted pupils – Increased salivation – Increased peristalsis – Dilated blood vessels – Bladder contraction ASSESSMENT OF SENSORY FUNCTION • • • • • Touch Pressure Pain Bladder control Bowel control GLASGOW COMA SCALE • A method of assessing a client's neurological condition • A scoring system based on a scale of 1 to 15 points • A score below 8 indicates coma is present • Eye opening is the most important indicator SKULL AND SPINAL X-RAY • DESCRIPTION – X-rays of the skull reveal the size and shape of the skull bones, suture separation in infants, fractures or bony defects, erosion, or calcification – Spinal x-rays identify fractures, dislocation, compression, curvature, erosion, narrowed spinal cord, and degenerative processes SKULL AND SPINAL X-RAY • PREPROCEDURE – Provide support for the confused, combative, or ventilator-dependent client – Maintain immobilization of the neck if a spinal fracture is suspected – Remove metal items from body parts – If the client has thick and heavy hair, this should be documented, because it may affect interpretation of the x-ray film • POSTPROCEDURE – Maintain immobilization until results are known COMPUTED TOMOGRAPHY (CT) SCAN • DESCRIPTION – A type of brain scanning that may or may not require an injection of a dye – Used to detect intracranial bleeding, spaceoccupying lesions, cerebral edema, infarctions, hydrocephalus, cerebral atrophy, and shifts of brain structures POSITIONING FOR CT SCAN From Perkin GD et al (1986) Atlas of clinical neurology. London: Gower Medical Publishing. CT SCAN OF THE BRAIN From Seeley RS, Stephens TD, Tate P (1995) Anatomy and Physiology (3rd ed.) New York: The McGraw-Hill Companies; Howard Sochurek. COMPUTED TOMOGRAPHY (CT) SCAN • PREPROCEDURE – Obtain a consent if a dye is used – Assess for allergies to iodine, contrast dyes, or shellfish if a dye is used – Instruct the client in the need to lie still and flat during the test – Instruct the client to hold his or her breath when requested – Initiate an IV if prescribed COMPUTED TOMOGRAPHY (CT) SCAN • PREPROCEDURE – Remove objects from the head such as wigs, barrettes, earrings, and hairpins – Assess for claustrophobia – Inform the client of possible mechanical noises as the scanning occurs and that there may be a hot, flushed sensation and a metallic taste in the mouth when the dye is injected – Note that some clients may be given the dye even if they report an allergy, and are pretreated with an antihistamine and corticosteroids prior to the injection, to reduce the severity of a reaction COMPUTED TOMOGRAPHY (CT) SCAN • POSTPROCEDURE – Provide replacement fluids because diuresis from the dye is expected – Monitor for an allergic reaction to dye – Assess dye injection site for bleeding or hematoma, and monitor extremity for color, warmth, and the presence of distal pulses MAGNETIC RESONANCE IMAGING (MRI) • DESCRIPTION – A noninvasive procedure that identifies types of tissues, tumors, and vascular abnormalities – Similar to the CT scan but provides more detailed pictures and does not expose the client to ionizing radiation CLINICAL SETTING FOR AN MRI From Mourad LA (1991) Orthopedic disorders. St. Louis: Mosby. MAGNETIC RESONANCE IMAGE From Crossman AR, Neary D (1995). Neuroanatomy: an illustrated color text. Edinburgh: Churchill Livingstone. MAGNETIC RESONANCE IMAGING (MRI) • PREPROCEDURE – Remove all metal objects from the client – Determine if the client has a pacemaker, implanted defibrillator, or metal implants such as a hip prosthesis or vascular clips because these clients cannot have this test performed – Remove IV fluid pumps during the test MAGNETIC RESONANCE IMAGING (MRI) • PREPROCEDURE – Provide precautions for the client attached to a pulse oximetry because it can cause a burn during testing if coiled around the body or a body part – Provide an assessment of the client with claustrophobia – Administer medication as prescribed for the client with claustrophobia MAGNETIC RESONANCE IMAGING (MRI) • PREPROCEDURE – Determine if a contrast agent is to be used and follow the prescription related to the administration of food, fluids, and medications – Instruct the client that he or she will need to remain still during the procedure • POSTPROCEDURE – Client may resume normal activities – Expect diuresis if a contrast agent was used LUMBAR PUNCTURE • DESCRIPTION – Insertion of a spinal needle through L3-L4 interspace into the lumbar subarachnoid space to obtain cerebrospinal fluid (CSF); measure CSF fluid or pressure; or to instill air, dye, or medications – Contraindicated in clients with increased intracranial pressure, because the procedure will cause a rapid decrease in pressure within the CSF around the spinal cord, leading to brain herniation LUMBAR PUNCTURE • PREPROCEDURE – Obtain a consent – Have the client empty his or her bladder LUMBAR PUNCTURE • DURING THE PROCEDURE – Position the client in a lateral recumbent position and have the client draw knees up to the abdomen and chin onto the chest – Assist with the collection of specimens (label the specimens in sequence) – Maintain strict asepsis LUMBAR PUNCTURE From Herlihy B, Maebius NK: The human body in health and illness, Philadelphia, 2000, W.B. Saunders. LUMBAR PUNCTURE • POSTPROCEDURE – Monitor vital signs and neurological signs – Position the client flat as prescribed – Force fluids – Monitor I&O MYELOGRAM • DESCRIPTION – Injection of dye or air into the subarachnoid space to detect abnormalities of the spinal cord and vertebrae POSITIONING FOR A MYELOGRAM From Chipps EM, Clanin NJ, Campbell VG (1992) Neurologic disorders. St. Louis: Mosby. Courtesy of Doctors Hospital, Columbus, OH. NORMAL MYELOGRAM OF THE LUMBAR SPINE From Black, J., Hawks, J., and Keene, A. (2001). Medical-surgical nursing, ed 6, Philadelphia: W.B. Saunders. MYELOGRAM • PREPROCEDURE – Obtain a signed consent form – Provide hydration for at least 12 hours before the test – Assess for allergies to iodine – If the client is taking a phenothiazine, hold the medication because this medication lowers the seizure threshold – Premedicate for sedation as prescribed MYELOGRAM • POSTPROCEDURE – Vital signs and neurological assessment frequently as prescribed – If a water-based dye is used, elevate the head 15 to 30 degrees for 8 hours as prescribed – If an oil-based dye is used, keep the client flat 6 to 8 hours as prescribed – If air is used, keep the head lower than the trunk as prescribed MYELOGRAM • POSTPROCEDURE – Administer analgesics for headache or backache as prescribed – Force fluids – Monitor I&O – Assess for bladder distention and voiding CEREBRAL ANGIOGRAPHY • DESCRIPTION – Injection of a contrast through the femoral artery into the carotid arteries to visualize the cerebral arteries and assess for lesions CEREBRAL ANGIOGRAPHY From Black, J., Hawks, J., and Keene, A. (2001). Medical-surgical nursing, ed 6, Philadelphia: W.B. Saunders. CEREBRAL ANGIOGRAPHY • PREPROCEDURE – Obtain a consent – Assess the client for allergies to iodine and shellfish – Encourage hydration for 2 days before the test – NPO 4 to 6 hours prior to the test as prescribed – Obtain a baseline neurological assessment – Mark the peripheral pulses CEREBRAL ANGIOGRAPHY • PREPROCEDURE – Remove metal items from the hair – Administer premedication as prescribed CEREBRAL ANGIOGRAPHY • POSTPROCEDURE – Monitor neurological status and vital signs frequently until stable – Monitor for swelling in the neck and for difficulty swallowing and notify the physician if these symptoms occur – Maintain bed rest for 12 hours as prescribed – Elevate the head of the bed 15 to 30 degrees only if prescribed CEREBRAL ANGIOGRAPHY • POSTPROCEDURE – Keep the bed flat if the femoral artery is used as prescribed – Assess peripheral pulses – Immobilize the puncture site for 12 hours as prescribed – Apply sandbags and a pressure dressing to the injection site as prescribed – Place ice to the puncture site as prescribed – Force fluids ELECTROENCEPHALOGRAPHY (EEG) • DESCRIPTION – A graphic recording of the electrical activity of the superficial layers of the cerebral cortex ELECTROENCEPHALOGRAPHY From Chipps EM, Clanin NJ, Campbell VG (1992) Neurologic disorders. St. Louis: Mosby. ELECTROENCEPHALOGRAPHY NORMAL AND INTRACRANIAL TUMOR Thompson JM et al. Mosby’s Clinical Nursing, ed. 4, St. Louis, 1997, Mosby. ELECTROENCEPHALOGRAPHY (EEG) • PREPROCEDURE – Wash the client's hair – Inform the client that electrodes are attached to the head and that electricity does not enter the head – Withhold stimulants, antidepressants, tranquilizers, and anticonvulsants for 24 to 48 hours prior to the test as prescribed – Allow the client to have breakfast if prescribed – Premedicate for sedation as prescribed ELECTROENCEPHALOGRAPHY (EEG) • POSTPROCEDURE – Wash the client's hair – Maintain siderails and safety precautions if the client was sedated CALORIC TESTING (OCULOVESTIBULAR TESTING) • DESCRIPTION – Provides information about the function of the vestibular portion of cranial nerve VIII and aids in the diagnosis of cerebellum and brain stem lesions CALORIC TESTING (OCULOVESTIBULAR TESTING) • PROCEDURE – Patency of the external canal is confirmed – Cold or warm water is introduced into the external auditory canal – Stimulation of the auditory canal with warm water produces a horizontal nystagmus toward the side of the irrigated ear when the vestibular cranial nerve VIII is normal – Stimulation of the auditory canal with cold water produces a horizontal nystagmus away from the side of the irrigated ear if the brain stem is intact