* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download General approach to hyperproolactinaemia
Sex reassignment therapy wikipedia , lookup
Hormone replacement therapy (menopause) wikipedia , lookup
Osteoporosis wikipedia , lookup
Growth hormone therapy wikipedia , lookup
Neuroendocrine tumor wikipedia , lookup
Hypothalamus wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
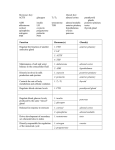
General approach to management of hyperprolactinaemia Dr. But Wai Man Prolactin Polypeptide hormone consisted of 199 aminoacids with 3 intramolecular disulfide bonds Encoded by a single gene on chromosome 6, 5 coding exons Secreted by lactotrophic cells in anterior pituitary gland Prolactin receptor Identified as a member of the cytokine receptor superfamily Single –chain transmembrane receptor Functions by binding a single prolactin molecule and then dimerizing with a second receptor molecule Functions of prolactin Important role in a variety of reproductive functions Essential factor for normal production of breast milk following child birth Hyperprolactinaemia disrupts normal pulsatile secretion of gonadotrophic-releasing hormone, altered LH and FSH secretion and impaired gonadal steroidogenesis, leads to infertility and gonadal dysfunction Control of prolactin secretion Secretion is mainly under inhibitory control by hypothalamic dopamine Circadian variation. Levels rise after the onset of sleep, nocturnal peak of 2x daytime concentration Hyperprolactinaemia Clinical manifestations Galactorrhoea 90%: affect mammary gland development Amenorrhoea/Oligomenorrhoea: In women, prolactin-secreting tumors is usually small, headache and neurological deficits are rare In men, tend to be large, and may cause cranial-nerve dysfunction, visual loss and panhypopituitarism loss of libido and erection dysfunction Galactorrhea and gynaecomastia are uncommon N Engl J Med 78; 299: 847-52 In both men and women Low bone density Weight gain Mood and behaviour changes Causes Pregnancy 10X Dopamine antagonist drug therapy ( phenothiazines and metoclopramide, TCA, monamine oxidase inhibitors, oestrogen, verapamil, methyldopa Stress eg venepuncture/ exercise Polycystic ovarian syndrome Pituitary-secreting microadenomas/macroadenomas Pituitary stalk disruption by interfering with the normal suppression of prolactin by hypothalamic dopamine Chronic renal failure Evaluation Biological evaluation of related hormonal axes: Careful drug history and physical examination TFT, RFT PCO and exclusion of pregnancy Levels of prolactin <1000 m U/L <5000 m U/L stress Micro-prolactinoma hypothyroidism Pituitary stalk disconnection PCOS > 10,000 m U/L Macroprolactinoma Macroprolactinaemia High molecular-weight prolactinimmunoglobulin complexes Polyethylene glycol precipitation of complexes allows the measurement of free monmeric prolactin Not thought to have pathological significance Evaluation for hypothalamicpituitary pathology Clinical examination: assessment of visual fields Imaging : MRI /CT Pituitary microadenoma < 10mm Pituitary macroadenoma > 10 mm Pituitary stalk lesions Hypothalamic tumours, granulomas Pituitary microadenoma 20% of the normal population at autopsy 50% of MRI imaging No lesion suggesting microadenoma < 2mm, lactotroph hyperplasia Hypopituitarism in structural lesion Prolactin secreting pituitary tumors Benign tumors Commonest pituitary tumors, 40% >90% are small, intrasellar tumors that rarely increase in size JCEM 89; 68: 412-8 Treatment of prolactinsecreting pituitary adenoma Medical Surgical Radiotherapy Indication To suppressive abnormal lactation To restore ovarian function Protection against development of osteoporosis Rx may not be required in a few women with modest elevations of prolactin, may retain normal ovarian function and have few symptoms Dopamine agonist Primary treatment of choice Normalise prolactin levels, restoration of pituitary function and tumor shinkage in 8090% over several weeks JCEM 1997 82 996-1000 Tumour shinkage by at least 25% of volume in 80% of patients with large macroadenoma Improvement in pressure symptoms within 48 hrs In men, 50% may require testosterone replacement, withhold until prolactin levels are normalised Bromocriptine Cabergoline Quinagolide 1st dopamine agonist since early New, high affinity for lactotroph 1970 dopamine receptors 2-3 x/day 5-30mg/day (7.5mg/d) 1-2x/week 0.5-2 mg/wk Nausea, postural hypotension, dizziness, headache, depression Improved efficacy and few side effects NEJM 94; 331: 904-909 Start with low dose and increase Most effective dosage gradually. Start 0.625 in reducing mg Nocte tumor size JCEM 2000 85 2247-2252 Duration 2-6 years? Once daily 0.05-0.25 mg Duration of treatment Early studies showed remission is rare after interruption of therapy, life long treatment Clin Endo 1991; 34: 173-174 Recent studies showed increase in remission and therapeutic withdrawal is recommended J Royal College of Physicians 1997; 31: 628-636 List of studies assessing dopamine agonist withdrawal Authors No Agent Duration (month) Type Remission FU (month) Zarate 83 16 BRC 24 Micro 37.5% 24 Moriondo 84 36 BRC 12 Macro 11% 30 Wang 87 24 BRC 24 Micro 21% 12-48 Rasmussen 87 75 BRC 24 All 44% >6 Ferari 92 127 CAB 14 All 31% 3-24 Muratori 97 26 CAB 12 Micro 19% 38-60 Colao 03 105 CAB 48 Micro 73% 24-60 Biswas 05 89 67- CAB 22- BRC 37 Micro 31% >12 Remission Long term follow up studies of untreated patients have shown that prolactinomas are very indolent Short term therapy appears to induce cytostatic effects including reduction in organelle size and reduction in the volume of prolactin cells JCEM 55, 117981183 Long-term therapy induces cytocidal effects such as necrosis, fibrosis and inflammatory cell infiltration JCEM 58, 1179-1183 Pregnancy Warned that restoration of ovulatory menstral cycle within weeks Advised to use mechanical form of contraception until 2 regular menstrual flow Stop dopamine agonist as soon as pregnancy is confirmed for microadenoma, risk of pituitary enlargement is low <2% Bromocriptine can cross placenta and suppress pituitary prolactin secretion, but no apparent risk of congenital abnormality or misscarriage JCEM 97 82 996-1000 For macroadenoma, bromocriptine is advised during pregnancy to avoid significant tumor expansion as risk of enlargement is 15-30% (J Reprod Med 99; 44: 1121-6) Some recommend debulking for macroadenoma which have extended beyond the sella before pregnancy and bromocriptime prescribed throughout pregnancy (Am J O&G 83; 146:935-8) Cabergoline should not be used as a therapy for infertility until more information is available Surgery Not first line option as outcomes reported are variable Experienced center cure rate 85-90%, recurrence and complication <10% and hypopituitarism <1% JCEM 1995 81 1711-1719 Prolactin decrease to very low values immediately after surgery and gradually to low-normal over wks, recurrence rate is very low Meta 1986 35 905-912 Success is less likely (<50%) in macroadenoma which has extended beyond the sella JCEM 1995 81 1711-1719 Indications for pituitary surgery Resistance or intolerance to optimal medical therapy For patients with intrasellar tumor for whom long-term drug treatment is not acceptable Surgical decompression may be required for tumors pressing on optic chiasm Avoid in cases o f extrasellar expanding tumors without optic chiasm compression because of low success rate Hormonal therapy Fertility is not a concern For hypogonadism Prevent progressive bone loss Macroadenomas Tend to grow, absolute indication for therapy Managed with dopamine agonist Confined to the sella should be managed as micraoadenoma as unlikely enlarged sufficiently to cause serious complications Higher doses Decrease in prolactin levels within 2-3 wks and precedes a decrease in the size of the tumor and restoration of anterior pituitary function Visual field assessment 1 month after the initiation of therapy MRI repeated 6 months later Prolactin measured yearly Hyperprolactinaemia and antipsychotic drugs Hyperprolactinaemia and antipsychotic drugs 34% of men and 75% of women showed hyperprolactinaemia (Curr Med Res Opin 2004;20:(2) 18997) Hypogonadism is common. Mean levels were in the hypogonadal range for women and 6.4% of men were hypogonadal (Br J Psy 2004;184:503-8) Sexual dysfunction in 45% compared with 17% of GP clinic control (Br J Psy 2004;184:503-8) Effects of long term prolactin raising antipsychotic medication on bone mineral density in patients with schizophrenia Male and post-menopausal female patients with schizophrenia on longterm prolactin –raising antipsychotic drugs (>10yr) British J of Psychiatry 2004; 184; 503-508 Results Hyperprolactinaemia was present in 62% of the overall group (60% in male and 64% in female) 57% of the men and 32% of the women had reduced bone mineral density Antipsychotic drugs A new risk factor for osteoporosis in young women with schizophrenia To study the effect of prolactin-raising and prolactin-sparing antipsychotic drugs (olanzapine) on bone density of premenopausal females J of clinical psychopharmacology 2005; 25 (1):26-31 Results Low BMD in 65% of prolactin-raising group, compared with 17% in prolactinsparing group Hyperprolactinaemia was associated with low BMD; 95% with low BMD had hyperprolactinemia and only 11% of the group with normal prolactin had abnormal BMD Relative percentage distribution of low BMD in prolactin-sparing and prolactin – raising groups Relative percentage distribution of bone loss in normal prolactin and hyperprolactinemia Thanks you