* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Section A: Introduction - University of Arkansas
Epidemiology of metabolic syndrome wikipedia , lookup
Herd immunity wikipedia , lookup
Infection control wikipedia , lookup
Race and health wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Diseases of poverty wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Compartmental models in epidemiology wikipedia , lookup
Seven Countries Study wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Preventive healthcare wikipedia , lookup
Alzheimer's disease research wikipedia , lookup
Public health genomics wikipedia , lookup
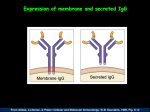
Section A: Introduction Dr. Jones University of Arkansas Human Disease History of Disease 4 Theories of Disease Causation Evil spirits and supernatural beings Contagion Germ Multiple causation (agent-environment-host) 30 00 B 25 C 00 B 20 C 00 B 15 C 00 B 10 C 00 B C 50 0B C 50 0A D 10 00 A 17 D 00 A 18 D 00 A 19 D 00 A 20 D 00 A 20 D 03 A D Years in Age Life Expectancy 90 80 70 60 50 40 30 20 10 0 Years Wow! Bad graph, huh? Why? LE Data pre-1750 are not solid. Much from special populations (wealthy landowners, popes, etc) – not representative. Jonker, 2003; Wilmoth, 2000 Evil Spirits and Gods 4000 to1000 BC Egyptians used medicine and magic Treatment used drugs such as Castor oil Olive oil Opium Some treatment methods still used today Evil Spirits and Gods Chinese Medicine Herbal remedies Opium as a narcotic Iron to treat anemia Invented acupuncture Contagion Theory 460BC to 1790AD World Events Effecting Disease Religion Travel (spread of disease) Lack of scientific study War (The Crusades) Plagues Control methods included isolation/quarantine The Islamic World in Medicine 8th century AD (CE) – 1st Bimaristan, specialty hospital female nurses, first to employ female physicians (separate wards made necessary) 865 to 930 - Al-Razi Three treatises; most influential, on smallpox and measles, was translated into Latin in 1700s Wakeel, n.d. The Islamic World in Medicine Retaining/translating texts when knowledge was being lost ~1012 AD (CE) – Ibn Sina, Book of Healing and Canon of Medicine Espoused mind-body connection, mental health, selfesteem; emphasized understanding causes of disease 13th century - Ibn an-Nafis, physician Challenged Galen’s view of the heart, discovered pulmonary circulation Mondalou, 2008; Stephenson, 2000; Wakeel, n.d. Contagion Theory Natural and humanistic causes Hippocrates (Father of Medicine-430 BC) Developed belief of 4 humors (fluids) Blood, Phlegm, Yellow & Black Bile Disease caused by imbalance Bloodletting was preferred treatment Galileo (1609 AD) discovered first microscope Contagion Theory Major Diseases Plague Typhoid Typhus Diphtheria Streptococcal Small pox Dysenteries Syphilis Cholera Anthrax Leprosy-Hansen’s Disease Contagion Theory Major Discoveries Galen (168 AD (CE))-Imperial physician for Roman empire provided the best knowledge of the human anatomy. Leonardo da Vinci/Andreas Vesalius (1540 AD) showed that Galen’s work was incorrect and based on animals. Antonie Van Leeuwenhoek (1683) was the first to use a microscope to identify bacteria. Germ Theory (1800 to 1940) Specific Cause – Specific Disease Girolamo Fracastoro (1550) Edward Jenner (smallpox vaccination)-1796 Louis Pasteur (pasteurization) Robert Koch (4 postulates of disease causation) Koch’s 4 Postulates 1. 2. 3. 4. Always be present in the disease Capable of growth in the lab Cause disease when injected in an animal Can be recovered from the animal Germ Theory (1800 to 1940) Claude Bernard (digestion/endocrine system) Joseph Lister (developed antiseptic) Marie & Pierre Curie (discovered Radium) Roentgen (X-rays) Electron Microscope (1930) Multiple Causation (1850 - Present) One Disease – Multiple Causes Cancer & Heart Disease Emergence of non-infectious disease Medical technology and new medicines Epidemiology Public health movement Multiple Causation (1850 - Present) Major Discoveries Vitamins and deficiency diseases (Beriberi Pellagra, Rickets, Scurvy) Paul Ehrlich (specific chemical agent – Syphilis) Alexander Fleming (Penicillin) Jonas Salk/Albert Sabin (vaccine for Poliomyelitis) Multiple Causation (1850 - Present) Major Disease Investigation Framingham heart Study (identified risk factors of heart disease) Nurses Health Study Tuskegee Study (Human Subject Review Boards) ACS Cancer Prevention Study (largest cohort study) 1 million people from 1959 – 1972 in 25 states Non-Infectious Disease Deaths 400 300 200 Infectious Disease Deaths 100 1920 1930 1940 1950 1960 1970 1980 Pneumonia Tuberculosis Diarhhea Heart Disease Stroke Liver Disease Injuries Cancer Senility Diptheria Heart Disease Cancer Stroke Chronic Lung Disease Unintentional Injuries Pneumonia and Flu Diabetes Suicide HIV Infection Suicide Liver Disease History of Public Health Roman Civilization (100 BC-300 AD) Developed concept of public health Built aqueducts Built sewers Street cleaning Physicians tended to the poor History of Public Health Modern (1850 to Present) British Public Health Act of 1848 (Edwin Chaddick) John Snow investigates Cholera 1850 – American Lemuel Shattuck publishes recommendations for public health American Public Health Association Focus on school health Distribution of cholera cases, Golden Square area of London, Aug/Sept 1854 Recommendations for Public Health Lemuel Shattuck Establishment of state & local health dept. Hiring sanitary inspectors Keeping vital statistics Establishment of school health Studies of tuberculosis Supervision of the mentally ill Study of immigrants’ problems Building of model tenements Recommendations for Public Health Establishment of public restrooms Control of smoke nuisances Control of food adulteration Exposure of quack medicines Preaching of health in the churches Training schools for nurses Teaching of sanitary science in medical school Include preventive medicine in clinical practice Public Health What is it? Activities that a society undertakes to assure the conditions which people live are healthy and safe. Included are community efforts to prevent, identify, and counter threats to the health of the public. Examples: Public Health vs. Medical Care Medical Care Treatment Individual Health care Unlimited $ Individual supported Public Health Prevention Community Multidiscipline Limited $ Taxpayer supported Section B: Epidemiology Dr. Jones University of Arkansas Human Disease Epidemiology The study of the distribution and determinants of disease frequency in human populations Distribution Determinants Populations Frequency Key Terms Epidemic – excessive occurrence of disease Pandemic – epidemic over a large area, such as a country, continent, or the world Endemic – constant presence of a disease, specific to a region or population; usual or expected frequency of a disease Main Concepts of Epidemiology 1. An analytic, descriptive component termed classical epidemiology, and 2. A diagnosis, management of illness, and critical review of literature termed clinical epidemiology. 3 Levels of Prevention Primary – prevention of the development of disease Secondary – early detection and treatment of disease Tertiary – rehabilitation and/or restoration of effective functioning after the treatment of disease Epidemiologic Surveillance Definition The ongoing process and systematic collection, analysis, and interpretation of health data in the process of describing and investigating the health status of a population. Current Uses of Epidemiology Identifying the etiology and cause of a new epidemic or syndrome Example: Carpal Tunnel Syndrome Ebola Virus Epidemic Post Traumatic Stress Syndrome Current Uses of Epidemiology Investigating the risk associated with a harmful exposure Example: Radon exposure Lead Environmental tobacco smoke (ETS) Dioxin Current Uses of Epidemiology Determine if a treatment is effective Example: Comparison of survival rates after segmental and total mastectomies Study/identify health service utilization needs and trends Examples: Effect of health insurance coverage on health services used by poor and near poor populations Impact of youth violence on ER services and utilization Current Uses of Epidemiology To provide rationalization and justification for health policy planning Example: Smoking bans Gun-control laws Drunk-driving laws Hazardous waste regulations Epidemiological Models Chain of Infection Traditional Model Health Field Concept Acute vs. Chronic Disease Chain of Infection Chain of Transmission Direct or Indirect Host Susceptibility Portal of Entry Vector (animate, inanimate) Pathogenic Agent Reservoir (human, animal, or inanimate) Portal of Exit Transmission Direct Direct Contact Kissing Skin-to-skin Sexual intercourse Droplet Spread Sneezing Coughing Talking Transmission Indirect Airborne (dust, droplet nuclei) Vehicleborne (food, water, etc.) Vectorborne (ticks, mosquitoes, etc.) Traditional Model Environment Agent Host Health Field Concept Biology Heredity Environment Lifestyle Health Care System Health Field Concept Lifestyle Leisure Consumption patterns Employment/occupational risks Environment Physical Social and psychological Health Field Concept Human biology Genetic Inheritance Maturation and aging Medical Care System Preventative Restorative Curative Infectious Disease Cause – Diagnosis – Treatment – Severity Disease of short duration Affects mainly the young Chronic Disease Cause – Diagnosis – Treatment (cure) Disease of long induction period Time allows multiple causes to develop Affects mainly the old Concept of Risk With multiple causes and chronic diseases, epidemiologists like to refer to the concept of causality based on the odds (risks, chances) of the occurrence of disease or health status as associated with the occurrence of another (risk factor) Limitations of Epidemiology It is difficult to assess risk from epidemiological data because: 1. Research studies on humans are sometimes unethical, expensive, and difficult to obtain 2. Chronic disease situations often find very low risks Limitations of Epidemiology 3. The number of persons with the disease or exposure is very small 4. Latency period between exposure and disease status are sometimes many years apart 5. Humans may be exposed to multiple chemical, biological , and physical hazards Types of Epi Strategies Used 1. 2. 3. Descriptive Analytic (retrospective – case-control, prospective – longitudinal/cohort, & cross-sectional) Experimental (cause & effect) Descriptive & Analytic Epidemiology Descriptive Epidemiology – amount and distribution of disease within a population by person, place, and time Analytic Epidemiology – more focused study on the determinants of the disease or reason for relatively high or low frequency in specific groups Ask These Questions Who (person) – D What (type of disease, illness, disability) – D When (time) – D Where (place) – D How (etiology or cause of event) – A A = analytic D = descriptive Descriptive Person 3 main characteristics: Age Gender Ethnic group/race Age It is the most important determinant among the person variables Mortality and morbidity rates of most conditions show some relation to age Infectious diseases – younger Chronic diseases – older Gender Mortality is higher among males Morbidity is higher among females Why? Gender Mortality – linked with inheritance, hormonal balance, environment, or habit pattern Morbidity – women have higher rates of illness and more physician contacts than men. Possible reasons: 1. 2. Women seek medical care more freely & perhaps at an earlier stage of disease. The same disease will tend to have a less lethal dose in women than men. Ethnic Group Classifying people by ethnic group is difficult but important in the field of epidemiology. Why? 1. 2. Many diseases differ in frequency, severity, or both in different racial groups and Statistically by race are helpful for identifying health problems Other Person Variables Social class Occupation Marital Status Family Variables Family Size Birth Order Personality traits Maternal Age Parental Deprivation Blood Type Environmental Exposure Place Considerations Frequency of disease can be related to place of occurrence by: Natural boundaries (these are more useful & include things like rivers, deserts, mountains) Political subdivisions (these are more convenient) Place Considerations Mapping environmental factors Urban-Rural differences International comparisons Time Considerations 3 major time measurements: 1. Secular trends (long-term variations) 2. Cyclic (recurrent alterations in the frequency of disease) 3. Short-term fluctuations Study Design Definitions Confounding – illusory association between two variables. The association is caused by a 3rd factor, “confounder.” major confounders are age, gender, and smoking Bias – subjects chosen for the study are unrepresentative of the population. Types of bias include: (over 57 types) Healthy worker bias Information Volunteer Study Design Definitions Chance – making assumptions and inferences of the measure of disease frequency concerning the experience of a population based on an evaluation of only a sample. Because of chance variation, for any two samples in a population to be identical is highly unlikely. Chance-example via checkerboard Types of Study Designs Case Report or Case Series Descriptive (Population-based) *Follow-up (Population-based) *Case-Control Follow-Up Studies Retrospective Prospective Retrospective People diagnosed as having a disease are studied to determine past exposure to various risk factors Past Present Look for past exposure to factor in diseased people Select individuals with the disease Retrospective Strengths Less expensive Faster to do study Limitations Impossible to control for confounding factors Bias prone Prospective Study starts with a group (cohort ) of people who are free of disease, but who vary according to exposure to probable disease factor Present Future Select cohort & classify as to exposure to factor Follow-up to see frequency with which disease develops Prospective Strengths Temporal sequence is clear Bias and confounding are relatively easy to control Absolute measures of occurrence are available (incidence, mortality, etc.) Provides information on many factors Prospective Limitations Very expensive and time consuming May not provide significant findings until after 5-10 years Inappropriate for rare diseases Problems with following up on new subjects Extremely inefficient Case Control Study People are diagnosed as having a disease (cases) are compared with persons who do not have the disease (controls) with relation to various risk factors Past Present Look for past exposure to factor in cases & controls Select people with the disease (cases) Select people with out the disease (controls) Case Control Study Dominant form of epidemiologic study (> 80%) Difficult but rewarding design to use Case-control studies have been used in other areas besides causation-preventive services and health services research Case Control Study Strengths Appropriate for rare diseases Appropriate for diseases with long induction time Economical & done rapidly Allow evaluation of multiple hypotheses Extremely efficient Large amount of information on small amount of subjects Case Control Study Limitations People don’t understand it (abused) Study is poor when exposure of interest is rare Only relative measures are available Bias prone Epidemiological Measurements General Formula Number of events (cases, deaths, services) in a specified time period Population at risk of Experiencing the event X 10n Using Rates & Risks Ecological fallacy (generalizing) Variations in base (what base is used) Variance in rates (differences based on rates) Measures of Mortality Crude Mortality Rate Infant Mortality Rate Case Fatality Rate Measures of Morbidity Incidence Rate Prevalence Rate Crude Mortality Rate General Formula All deaths during a calendar year Total population X 1,000 = deaths per 1,000 Crude Mortality Rate This rate expresses the actual observed mortality rate in a population under study and is considered the starting point for the adjustment of rates Infant Mortality Rate Most widely accepted measure for estimating the health status of a population # of infant deaths* (less than 1 year of age) Total live births *excludes fetal deaths X 1,000 Case Fatality Rate General Formula # of deaths due to the disease in a specific time period # of cases of the disease in the same time period Expressed as a percentage (%) X 100 Case Fatality Rate This measure represents the probability of death among diagnosed cases, or the killing power of a disease Example: In Sudan Africa, 34 people were infected with the Ebola virus in 1979. Of those infected, 31 eventually died from the disease 31 X 100 = 91% 34 Incidence & Prevalence The two main measures of disease frequency (morbidity) Incidence – new cases of a certain disease Prevalence – ALL cases of a certain disease Incidence & Prevalence Incidence (new cases) Death Recovery Prevalence Pot Incidence Incidence rates are designed to measure the rate at which people without a disease develop the disease during a specific period of time. Incidence rate = # of new cases of a disease over a period of time population at risk of the disease in the time period Incidence Example Gonorrhea in Arkansas 1987 I = 8898 new cases of Gonorrhea 2,342,699 population =381/100,000 1996 I = 5027 new cases of Gonorrhea 2,509,793 population =200/100,000 Prevalence Prevalence rates measure the number of people in a population who have the disease at a given point in time Prevalence rate = total # of cases of a disease at a given time total population at a given time AIDS in Arkansas - 1996 County Benton Carroll Pulaski Wash Pop’n 105,588 19,505 353,394 120,146 AIDS 4 1 24 2 46 18 499 124 6/949/94 AIDS Total Section C: Infectious Disease Dr. Jones University of Arkansas Human Disease The Immune System Natural Nonspecific Immunity Acquired Immunity Immune Disorders Natural Nonspecific Immunity 3 types External Barriers Inflammation Natural Specific Immunity Natural Nonspecific Immunity External Barriers Body’s first line of defense Defense Mechanisms Skin protection Mucus secretion Body fluid secretion External protection by bacteria Natural Nonspecific Immunity Inflammation A non-specific response to any foreign agent that causes cell injury. Body’s first line of defense upon penetration of a foreign organism. Acute Inflammation Response Pathogen Physical Agent Chemical Agent Tissue Injury Mediators of inflammation Capillary Increased Dilation capillary permeability Increased Extravasation Blood Flow of fluid Heat Redness Attraction of Systemic leukocytes response WBC go to site of injury Fever Leukocytes Tenderness Swelling Pain Inflammation Healing Process Two outcomes Recovery Chronic inflammation Inflammation Healing Process Regeneration – replacing of lost tissue by the same type of tissue (primary healing) Cells incapable of regeneration: Nerve Heart muscle Skeletal Repair – replacing of lost tissue by connective scar tissue (secondary healing) Inflammation Factors Effecting the Process Age? Diet/Nutrition Blood Supply Previous Infection Foreign Organisms Natural Nonspecific Immunity Natural Specific Immmunity 2 types Humoral immunity Cell-mediated immunity Humoral Immunity Production of antibodies (immunoglobulins) that combine with and eliminate foreign material. Main defense mechanism against bacteria Cell-Mediated Immunity Formation of lymphocytes that attack and destroy foreign material. Main defense against viruses, fungi, parasites, and some bacteria Types of Leukocytes (White Blood Cells) Neutrophils 50-70% Lymphocytes 20-40% Eosinophils 1-3% Basophils (release histamine) -1% Monocytes (Macrophage) 1-6% Natural Nonspecific Immunity Immune Response Types of Lymphocytes Thymus-dependent (T cells) Development of cell-mediated immunity Bone marrow (B cells) Development of humoral defense reaction T lymphocyte Sensitized lymphocyte Cell-Mediated Immunity Macrophage Processed Antigen Interaction Antigen interaction B lymphocyte "Memory Cells" Humoral Immunity Plasma cell Immune Response 3 types of T cells Helper T Cells – help make antibody forming cells from B cells (AIDS attacks these cells) Killer T Cells – interact with antigens and kill foreign material Regulatory (Suppressor) T Cells – suppress formation of antibody forming cells from B cells Natural Killer T Cells – involved in innate immune system Acquired Immunity 4 types Active Natural Immunity Active Artificial Immunity Passive Natural Immunity Passive Artificial Immunity Acquired Immunity Active Natural Immunity The individual is exposed to pathogen and the body produces antibodies to destroy it Acquired Immunity Active Artificial Immunity Vaccination with form (dead, weakened, or attenuated) of the disease causing pathogen thus enabling the body to produce antibodies Acquired Immunity Passive Natural Immunity Results from the transfer of antibodies from a mother to her child through the placenta. Acquired Immunity Passive Artificial Immunity Inoculation of antibodies to destroy foreign pathogen. Usually given to individuals effected by rabies or tetanus Acquired Immunity Antibodies-Immunoglobulins 5 types IgM IgG IgA IgD IgE * Picture of an IgM Immunoglobulins IgM – large antibody that is very effective in combining with large antigens such as fungi. IgG – smaller antibody that is formed in response to the majority of the infectious agents. Immunoglobulins IgA – produced by antibody-forming cells in the respiratory and gastrointestinal mucosa. Protects against harmful ingested or inhaled antigens. IgD – surrounds surfaces of lymphocytes IgE – present in small amounts in blood but higher concentrations can be found in individuals with allergies. Immune Disorders An individual form antibodies to his/her own cells or tissues 2 types Hypersensitivity Autoimmunity Hypersensitivity 4 major types Allergic Rhinitis Urticaria Angioedema Asthma Allergic Rhinitis (Hay Fever) Reaction to airborne allergen. May be seasonal or year round condition. Cause – pollen, mold spores, house dust, cat dander, cigarette smoke Symptoms – histamine and other chemicals released by the body Prevention – avoid allergens Treatment – antihistamines reduce symptoms, desensitization Urticaria (Hives) & Angioedema Skin condition characterized by itchy, raised white lumps surrounded by red, inflamed area. Cause – reaction to chemical substance or toxin Symptoms – rash Prevention – avoid allergen Treatment – antihistamines and skin lotions Urticaria (Hives) & Angioedema Asthma Immediate or subdued spasms of the bronchial tubes, increase mucous secretion, and swelling of the mucous membrane, and preceded by respiratory infection Cause – genetics, exposure to allergens, stress Prevention – avoid allergens, predisposing factors Treatment – adrenocortical drugs Anaphylaxis Anaphylactic Shock A life-threatening rapid and serious allergic reaction due to increase in IgE antibody resulting in a narrowed airway. Cause: foods (nuts), vaccinations, antibiotics (penicillin), other medicines, latex, insect stings/bites, exercise. Treatment requires: Adrenaline (epinephrine) injection to stabilize. Asthma Prevalence, United States Asthma Mortality Autoimmunity Rheumatoid Arthritis Lupus Erythematosus Immune-mediated Diabetes Rheumatoid Arthritis Inflammation of joints, muscles, tendons, ligaments, and blood vessels Cause – unknown, possibly genetic Prevention – none known Treatment – aspirin, anti-inflammatory drugs Lupus Erythematosus Inflammatory disorder effecting the connective tissue 2 types Cutaneous: affects skin Systemic: affects body organ systems Cause – stress, bacterial & viral infections, sun exposure Prevention – none known Treatment – corticosteroids for systemic lupus, avoid sun exposure Lupus Erythematosus Immune-mediated Diabetes The body destroys the cells in the pancreas that produce insulin, leading to a total failure to produce insulin and the way the body uses food Cause – unknown, possibly genetic Prevention – none known Treatment – monitor insulin, food, & blood. Exercise is beneficial Stages of Disease 1. 2. 3. 4. 5. Incubation – agent enters body (latent) Prodrome – first symptoms appear (communicable) Clinical – peak for symptoms (communicable) Decline – signs of recovery (carrier) Convalescent – return to full health (carrier) Disease Causing Organisms Prions Bacteria Rickettsiae Chlamydiae Mycoplasma Viruses Fungi Protozoa Metazoa Prions An infective group of complex organic compounds (proteins) suggested as the causative agents of several infectious diseases Examples: Creutzfeldt-Jakob Kuru Disease (Mad Cow Disease) Bacteria Small, single-celled microorganisms that are the most common cause of disease. Diseases: Cholera Diphtheria Most STDs Most Foodborne diseases Tuberculosis Septicemia-bacterial blood infection Nosocomial disease-Hospital acquired Bacteria Common Foodborne Diseases: E. Coli Listeriosis Campylobacter Salmonella Botulism Bacteria Common STDs: Chlamydia Syphilis Gonnorhea Herpes (virus) HPV (Human Papillomavirus) Genital warts Treatment for Bacterial Infections Use of Antibiotics Inhibition of cell-wall synthesis Inhibition of cell-membrane function Inhibition of metabolic functions Competitive inhibition Adverse Effects of Antibiotics Toxicity Hypersensitivity Alteration of “friendly” bacteria Development of antibiotic-resistant bacteria: MRSA (and CA-MRSA) VRE MDTB Rickettsiae Microorganisms that resemble viruses and bacteria Diseases include: Typhus (body lice, ticks) Rocky Mountain Spotted Fever Tick-borne diseases Rocky Mountain Spotted Fever (Rickettsiae) Tularemia (Bacteria) Babesiosis (Protozoa) Lyme Disease (Bacteria) Ehrlichiosis (Bacteria) Chlamydiae Very small, nonmotile bacteria Diseases include: Nongonococcal urethritis Inclusion conjunctivitis Picture of inclusion conjunctivitis Mycoplasmas Very small bacteria that lack a cell wall Diseases include: Primary atypical pneumonia Electron micrograph of thin-sectioned mycoplasma cells Viruses Small infectious pathogen that relies on other living cells to complete life cycle. Three main type of viruses exist: DNA, RNA, and incomplete or defective Diseases include: Cold/Flu Chicken Pox AIDS Measles Small Pox (eradicated) Hemorrhagic Fevers -Ebola -Lassa Fever Small Pox and Chicken Pox Human Defense Mechanisms Against Viruses Formation of Interferon Interferon is a nonspecific antiviral agent induced by viruses. Produced mainly by monocytes and lymphocytes Humoral Cell Response Cell-Mediated Response Diseases Targeted for Eradication World Health Organization (WHO) Small pox (since 1973) Polio Drancunculiasis (Guinea Worm) Leprosy Fungi Plantlike organism that vary in size and number of cells Two types of fungal diseases: Athlete’s foot fungus Superficial (skin) infections Athlete’s feet Ringworm Systematic infections Ringworm fungus Fungi Systematic Infections Histoplasmosis Blastomycosis Coccidiodomycosis These diseases can infect a persons heart, lung, and central nervous system Protozoa Single-celled microscopic animal forms that release toxins and enzymes that interfere with bodily functions. Diseases include: Dysentery (vehicle-water) Malaria (vector-mosquito) African Sleeping Sickness (tsetse fly) Chagas (reduviid bug) Giardiasis (vehicle-water) Toxoplasmosis (reservoir-cat) Leishmaniasis (vector-sand fly) Metazoa Multicellular organisms such as tapeworms, ringworms, and flukes. Diseases include: Trichinosis Pinworm Tapeworm Lymphatic Filiarisis (Elephantiasis) vectormosquito Drancunculiasis (Guinea Worm) vehicle-water Tapeworm & Elephantiasis Bioterrorism Diseases Small pox Tuleremia Anthrax Plague Botulism (Toxin) Current World Health Problems Morbidity 1. 2. 3. 4. 5. Diarrhea Respiratory infections Occupational injuries Chlamydia Trichomoniasis Number 1821 million 248 million 120 million 97 million 94 million Current World Health Problems Morbidity (2nd top 5) 6. 7. 8. 9. 10. Gonococcal Infections Occupational Diseases Measles Whooping Cough Genital Warts Number 78 million 69 million 45 million 43 million 32 million Current World Health Problems Disability 1. 2. 3. 4. 5. Mood Disorders Lymphatic Filariasis Hearing Loss Mental Retardation Cataract-related Blindness Number 59 million 43 million 42 million 41 million 16 million Current World Health Problems Disability (2nd top 5) 6. 7. 8. 9. 10. Epilepsy Dementia Poliomyelitis Schizophrenia Obstructed Labor Number 15 million 11 million 10 million 8 million 7 million Section D: Chronic Diseases Dr. Jones University of Arkansas Human Disease Chronic Diseases Definition Illnesses that are prolonged, do not resolve spontaneously, & are rarely cured completely Chronic diseases that are a focus of prevention efforts are those that are preventable & pose a significant burden in mortality, morbidity, & cost Chronic Diseases & Conditions Major Diseases Alzheimer’s Disease = 4 million Arthritis = 69 million Cancer = 8 million Cardiovascular Disease = 58 million Chronic Obstructive Pulmonary Disease = 30 million Chronic Diseases & Conditions Major Diseases Diabetes =20 million Epilepsy = 2.3 million Iron Overload = 1 million Oral Diseases & Conditions = ?? Osteoporosis = 28 million Age-adjusted death rates for selected leading causes of death: United States,1958-2005 ICD-7 ICD-8 ICD-9 ICD-10 1-diseases of the heart 1000.0 2-malignant neoplasms 3-cerebrovascular diseases 100.0 5-unintentional injuries 9-nephritis, nephrotic syndrome and nephrosis 10.0 13-Hypertension 14-Parkinson’s 1.0 7- Alzheimer’s 0.1 1958 1960 1965 1970 1975 1980 1985 1990 1995 2000 2005 Numbers indicate ranking of conditions as leading causes of death in 2005. (ICD stands for International Classification of Diseases) NOTE: Age-adjusted rates per 100,000 U.S. standard population, see “Technical Notes.” SOURCE: CDC/NCHS, National Vital Statistics System, Mortality. Cardiovascular Disease A general term to describe many heart disorders, including high blood pressure, coronary artery disease, & clogging of the arteries (arthrosclerosis). Number one cause of death in the United States (CDC) and worldwide (WHO) Cardiovascular Disease Congenital Valvular Coronary Hypertension (high blood pressure) Primary Myocardial Congenital Heart Disease The heart fails to develop normally from the prenatal to 1 year period of a person’s life. Causes: virus, chromosomal abnormalities, or unknown Prevention: protection of fetus from interuterine injury Congenital Heart Disease Primary Types: Septal defects Obstruction defects (stenosis) Cyanotic defects Hypoplastic Valvular Heart Disease Scarring or malfunction of heart valves (mainly mitral & aortic) Causes: bacterial infections, degenerative processes, IV drug abusers Treatment: prevention of Rheumatic Fever & other bacterial infections Valvular Heart Disease Dysfunctions of valves Stenosis-hardening or calcification of valves that prevents valves from fully closing. Prolapse (floppy valve)-valves are enlarged and attached cords become long and allows blood to flow in the opposite direction back into the chamber. Valvular Heart Disease Valves can become damaged by: Pregnancy Fever, infection Changes due to aging Coronary Heart Disease Diseases resulting from the arteriosclerosis of the large coronary arteries. Arteries become: Narrowed due to the accumulation of lipids (fat & cholesterol) & 2) Weak & brittle due to degeneration 1) Another view Coronary Heart Disease Possible causes Elevated blood lipids High blood pressure Smoking Diabetes Personality Obesity Results of Myocardial Ischemia (Loss of Blood Flow) Coronary Thrombosis Hemorrhage in plaque Coronary arterial spasm Increased myocardial oxygen requirements Cardiac Arrest Myocardial Infarction Myocardial Infarction 1. 2. 3. 4. 5. 6. 7. Disturbance of cardiac rhythm Heart failure Cardiac rupture Intracardial thrombi Pericarditis Papillary muscle dysfunction Ventricular aneurysm More realistic view As in prior picture, heart muscle death would be taking place in area of thrombosis Coronary Heart Disease Treatment Procedures Medical Treatment Medication Smoking cessation Control of Hypertension Surgical Treatment Coronary Angioplasty/Catheterization Cost for Treatment Cardiac Catheterization - $20,000 Angioplasty - $20,370 Open Heart - $253,000 Bypass - $44,000 Transmyocardial Revascularization - ? Hypertensive Heart Disease Excessive vasoconstriction of the small arterioles throughout the body, thus raising diastolic blood pressure. Measured by taking the systolic blood pressure (arteries) over the diastolic blood pressure (ventricles). Hypertensive Heart Disease Effects Cardiac Vascular Renal Causes In most cases it is unknown Treatment medication Primary Myocardial Disease Disease of the heart muscle Two types: Myocarditis Cardiomyopathy Primary Myocardial Disease Myocarditis Inflammation of the heart muscle associated with injury and necrosis of the muscle fibers. Cause: viruses, parasites, fungi, hypersensitivity Treatment: bed rest, treat the cause This is your pericardium. This is your pericardium with myocarditis. Heart Disease as Compared with Mechanical Pump Dysfunction Mechanical Abnormality Faulty pump construction Faulty unidirectional valves Dirty or clogged fuel line Overloaded pump Malfunctioning pump Heart Disease Congenital Valvular Coronary Hypertensive Primary myocardial Cerebrovascular Disease (Stroke) Injury to the brain tissue resulting from disturbance of blood supply to the brain Cerebrovascular Disease (Stroke) Three Classifications Thrombosis (clot forms in the brain; most common) Embolus (clot forms elsewhere, moves to brain) Hemorrhage (most fatal) Causes: Same as for CVD (cardiovascular disease) Treatment: Rehabilitation -Anti-clot busting drugs(TPA) Prevalence of stroke by age* and sex Percent of Population 16 14.8 14 12.4 12 10 8 6.5 6.2 6 4 2 0.5 0.5 1.2 2.3 0 20-39 40-59 Men 60-79 Women *Note age categories are different than prior slide. (NHANES: 1999-2004). Source: NCHS and NHLBI. 80+ Diabetes Definition The inability of the body to produce or respond properly to the hormone insulin. The body needs insulin to convert glucose (“blood sugar”) to energy. Diabetes is defined as a fasting plasma glucose level of 126 mg/dL or more measured on 2 different occasions. Diabetes Types Type I – insulin dependent (3 mil) Type II – non-insulin dependent (17 mil) Pre-diabetes (15 mil) Gestational Other causes Diabetes Complications Heart Disease Kidney Failure Blindness Lower/Upper Extremity Amputations Diabetes Treatment Changes in eating habits Weight management Exercise programs Medication Regular check-ups Diabetes Possible Cures Pancreas transplantation Islet cell transplantation Artificial pancreas development Genetic manipulation Cancer A group of diseases characterized by uncontrolled growth and spread of abnormal cells Induction time of cancer (exposure + incubation) can be from 30 years or more to less than 1 year Second leading cause of death in the United States The good news – Estimated cancer survivors, 1971-2004 2008 Estimated US Cancer Cases* Men 745,180 Women 692,000 Prostate 25% 26% Breast Lung & bronchus 15% 14% Lung & bronchus Colon & rectum 10% 10% Colon & rectum Urinary bladder 7% 6% Uterine corpus Non-Hodgkin lymphoma 5% 4% Non-Hodgkin lymphoma Melanoma of skin 5% 4% Thyroid Kidney & renal pelvis 4% 4% Melanoma of skin Oral cavity 3% 3% Ovary Leukemia 3% 3% Kidney & renal pelvis Pancreas 3% 3% Leukemia 20% 23% All Other Sites All Other Sites *Excludes basal and squamous cell skin cancers and in situ carcinomas except urinary bladder. Source: American Cancer Society, 2008. 2008 Estimated US Cancer Deaths* Lung & bronchus 31% Prostate 10% Men 294,120 Women 26% 271,530 15% Lung & bronchus Breast Colon & rectum 8% 9% Colon & rectum Pancreas 6% 6% Pancreas Liver & intrahepatic bile duct 4% 6% Ovary 3% Leukemia 4% Non-Hodgkin lymphoma Esophagus 4% 3% Leukemia Urinary bladder 3% 3% Uterine corpus Non-Hodgkin lymphoma 3% 2% Liver & intrahepatic bile duct Kidney & renal pelvis 3% 2% Brain/ONS 24% 25% All other sites ONS=Other nervous system. Source: American Cancer Society, 2008. All other sites Lifetime Probability of Developing Cancer, Men, 2002-2004* Site Risk All sites† Prostate 1 in 2 1 in 6 Lung and bronchus 1 in 13 Colon and rectum 1 in 18 Urinary bladder‡ 1 in 27 Melanoma 1 in 41 Non-Hodgkin lymphoma 1 in 46 Kidney 1 in 59 Leukemia 1 in 67 Oral Cavity 1 in 71 Stomach 1 in 88 * For those free of cancer at beginning of age interval. † All Sites exclude basal and squamous cell skin cancers and in situ cancers except urinary bladder. ‡ Includes invasive and in situ cancer cases Source: DevCan: Probability of Developing or Dying of Cancer Software, Version 6.2.1 Statistical Research and Applications Branch, NCI, 2007. http://srab.cancer.gov/devcan Lifetime Probability of Developing Cancer, Women, US, 2002-2004* Site Risk All sites† Breast 1 in 3 1 in 8 Lung & bronchus 1 in 16 Colon & rectum 1 in 19 Uterine corpus 1 in 41 Non-Hodgkin lymphoma 1 in 53 Melanoma 1 in 61 Ovary 1 in 71 Pancreas 1 in 76 Urinary bladder‡ 1 in 85 Uterine cervix 1 in 142 * For those free of cancer at beginning of age interval. † All Sites exclude basal and squamous cell skin cancers and in situ cancers except urinary bladder. ‡ Includes invasive and in situ cancer cases Source: DevCan: Probability of Developing or Dying of Cancer Software, Version 6.2.1 Statistical Research and Applications Branch, NCI, 2007. http://srab.cancer.gov/devcan Cancer Survival*(%) by Race,1996-2003 Site African WhiteAmerican Absolute Difference All Sites 67 57 10 Breast (female) 90 78 12 Colon 66 55 11 Esophagus 18 11 7 Leukemia 51 40 11 Non-Hodgkin lymphoma 65 56 9 Oral cavity 62 41 21 Prostate 99 95 4 Rectum 66 58 8 Urinary bladder 81 65 16 Uterine cervix 74 66 8 Uterine corpus 86 61 25 *5-year relative survival rates based on cancer patients diagnosed from 1996 to 2003 and followed through 2004. Source: Surveillance, Epidemiology, and End Results Program, 1975-2004, Division of Cancer Control and Population Sciences, National Cancer Institute, 2007. Trends in Five-year Relative Survival (%)* Rates, US, 1975-2003 Site 1975-1977 1984-1986 1996-2003 All sites 50 54 66 Breast (female) 75 79 89 Colon 51 59 65 Leukemia 35 42 50 Lung and bronchus 13 13 16 Melanoma 82 87 92 Non-Hodgkin lymphoma 48 53 64 Ovary 37 40 45 Pancreas 2 3 5 Prostate 69 76 99 Rectum 49 57 66 Urinary bladder 74 78 81 *5-year relative survival rates based on follow up of patients through 2004. Source: Surveillance, Epidemiology, and End Results Program, 1975-2004, Division of Cancer Control and Population Sciences, National Cancer Institute, 2007. http://statecancerprofiles.cancer.gov/map/map.noimage.php http://statecancerprofiles.cancer.gov/map/map.noimage.php Causes of Cancer Exact cause is unknown Multiple causes associated with cancer may include life-style, and external and internal factors Causes of Cancer Life-style factors include: External factors include: Nutrition, smoking, stress, and activity levels Chemicals, radiation, viruses Internal factors include: Hormones, immune system, and inherited mutations Cancer Tumors (Neoplasms) Two types: 1. Benign (non-cancerous) 2. Malignant (harmful growth) Which is which? How Cancer Spreads Infiltration-effecting nearby organ Metastases – spreads through blood vessels or lymphatic system Colon cancer infiltration The Metastasis Process Cancer Tissue By Type Lung adenocarcinoma Carcinoma – Epithelium Sarcoma – Connective tissue Soft tissue sarcoma Cancer Tissue By Type Melanoma – Skin cells Neuroblastoma – Central Nervous System Large neuroblastoma behind liver Types of Skin Cancer Basal Cell (90%) Squamous Cell Melanoma (most serious) Cancer Tissue By Type Adenocarcinoma – Epithelium & Endocrine gland tissue Hepatoma – liver Leukemia – blood cells Lymphoma – immune system and lymphatic tissue Grading and Staging of Cancer Grading Based on grades of I through IV, depending on degree of difference from normal cells Grading and Staging of Cancer The American Joint Commission on Cancer has recommended the following guidelines for grading tumors: GX – grade cannot be assessed G1 – well differentiated G2 – moderately well differentiated G3 – poorly differentiated G4 - undifferentiated Grading and Staging of Cancer Staging Use of the TNM system T = primary tumor N = nodal involvement M = metastases Grading and Staging of Cancer Example for Rectal Cancer Primary tumor (T) TX: Minimum requirements to assess the primary tumor cannot be met TO: No evidence of primary tumor Tis: Carcinoma in situ: intraepithelial or invasion of the lamina propria* T1: Tumor invades submucosa T2: Tumor invades muscularis propria T3: Tumor invades through the muscularis propria into the subserosa or into the nonperitonealized pericolic or perirectal tissues T4: Tumor perforates the visceral peritoneum, or directly invades other organs or structures** Grading and Staging of Cancer Example for Rectal Cancer Regional lymph nodes (N) NX: Minimum requirements to assess the regional nodes can be met NO: No regional lymph node metastasis N1: Metastasis in 1 to 3 pericolic or perirectal lymph nodes N2: Metastasis in 4 or more pericolic or perirectal lymph nodes N3: Metastasis in any lymph node along the course of a named vascular trunk and/or metastasis to apical node(s) (when marked by the surgeon) Grading and Staging of Cancer Example for Rectal Cancer Distant metastasis (M) MX: Minimum requirements to assess the presence of distant metastasis cannot be met MO: No distant metastasis M1: Distant metastasis 7 Warning Signs of Cancer Change in bowel or bladder habits A sore that does not heal Unusual bleeding or discharge Thickening or lump in breast or elsewhere Indigestion or difficulty swallowing Obvious change in a wart or mole Nagging cough or hoarseness Cancer Treatment Surgery Radiation Chemotherapy Anti-cancer drugs Any combination of the above Promising Cancer Treatments Immunotherapy Vaccines Gene/hormone Therapy Bone Marrow Transplantation Drug Delivery Systems Disease Screening Purpose To identify people who have an enhanced probability of receiving a disease and have no signs or symptoms of the disease. A screening test is not intended to be diagnostic. Disease Screening Outcomes True-Positive – individual has the disease & is screened with the disease True-Negative – individual does not have disease & is screened without the disease False-Positive – individual does not have disease but is screened positive False-Negative – individual has the disease but is screened negative Disease Screening Definitions Sensitivity – the ability of a screening tool to detect individuals with the disease Specificity – the ability of a screening tool to detect individuals without the disease Sensitivity vs. Specificity A B C Non-diseased Diseased Disease Screening Types of Screening Tools Mammography Pap Smear PSA Cholesterol Blood Pressure Blood Sugar