* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PGD - Center for Research on End-of-Life Care
Schizoaffective disorder wikipedia , lookup
Antisocial personality disorder wikipedia , lookup
Mental disorder wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Conduct disorder wikipedia , lookup
Child psychopathology wikipedia , lookup
Conversion disorder wikipedia , lookup
Emergency psychiatry wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Abnormal psychology wikipedia , lookup
Autism spectrum wikipedia , lookup
History of mental disorders wikipedia , lookup
Asperger syndrome wikipedia , lookup
Separation anxiety disorder wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Posttraumatic stress disorder wikipedia , lookup
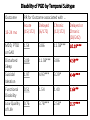
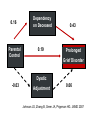
Time Will Tell: Pathways to Prolonged Grief, Pathways to Acceptance Holly G. Prigerson, PhD Irving Sherwood Wright Professor of Geriatrics Professor of Sociology in Medicine Weill Cornell Medical College Director, Center for Research on End-of-Life Care Cornell University Presentation Overview “Is this grief reaction normal?” “Am I going crazy?” “Will I feel better and, if so, when?” “Is this grief a problem, and if yes, What can be done about it?” Presentation Overview These are common questions that: bereaved people ask themselves their family members wonder clinicians often struggle to answer and address They are also the questions you should be able to answer after this talk At the end of this talk you should know how to: 1. Distinguish normal grief from PGD, & specifically how to a. diagnose PGD 2 Know who is at risk for PGD 3. Know outcomes of PGD – why clinicians should care 4. Understand core therapeutic issues in PGD Putting Bereavement in Context Bereavement is a normal, common life event ~ 52 million people die/year (or 142,000/day) worldwide • That is, almost as many people die per year as the entire population of France 100% of us will die; risk increases with age Not a rare or typically unnatural event! What is the normative circumstance of bereavement? Despite disproportionate media attention, most deaths do NOT involve younger people dying traumatic deaths Most US deaths occur in later life 75% deaths occur in people over 65 yrs 50% women over age 65 are widows Only 6% US deaths from unnatural causes (1.5% motor vehicle; 1.2% firearms); 94% natural causes Epidemiology of bereavement in France 66 million is population of France; 8.5/1000 death rate= 561,000 deaths/yr in France ± 3 survivors ±1.7 million bereaved survivors/yr in France Most will come to accept the loss over time (90%); ± 10% will not ± 170,000 bereaved people/year in France with PGD Question: How do you know if a grief reaction is normal? Answer: Time will tell. Time … Heals most wounds path of acceptance ~90% of bereavement reactions are “normal” Most people gradually adjust/accommodate to the loss But time …doesn’t heal all wounds path to Prolonged Grief Disorder (PGD) ~10% will follow an unending path of sorrow These are the people who may benefit from help For typical bereavement (e.g., late-life widowhood after natural death) … Most bereaved people accept death, even initially Acceptance increases with time from loss On scale where: 1= < 1/mo; 2= monthly; 3= weekly; 4=daily; 5= > 1X/day Maciejewski, Zhang, Block, Prigerson JAMA 2007 Maciejewski, Zhang, Block, Prigerson JAMA 2007 Indicator Rating 5.0 Acceptance 4.0 Yearning 3.0 Grief Disbelief Sadness 2.0 Anger 1.0 0 2 4 6 8 10 12 14 16 18 20 22 24 Time From Loss (months) Prigerson, Maciejewski BJP 2010 Grief is wanting something you love but can’t have Acceptance is letting go of wanting/craving, is associated with declining emotional distress over the loss Grief Resolution for those who do and do not meet criteria for PGD Grief score 50 Prolonged Grief 1 40 1 1 1 1 1 11 1 11 1 1 11 1 11 1 1 1 30 1 1 11 1 00 0 0 0 00 0 0 00 00 000 0 0 0 0 0 0 0 0 0 0000 000 0 0 00 0 0 0 0 0 0 0 0 00 0 0 000 0 0 0 00 0 0 0 0 0 10 1 1 1 1 1 20 1 1 1 0 Not Prolonged Grief 0 0 0 0 0 0 0 0 0 0 0 0 0 00 0 0 0 0 0 0 0 10 20 30 40 Months from the death 50 60 PGD reflects chronic distress, but is it a psychiatric disorder? Phenomenology: Symptoms distinct from other DSM-5 and ICD-11 disorders (MDD, PTSD) Risk Factors: Distinctive risk factors/etiology Outcomes: PGD independently associated with distress & disability Response to Treatment: PGD unresponsive to certain antidepressant treatments Prolonged Grief Disorder Differs from Other Psychiatric Disorders . . . Phenomenologically a. Forms separate, unidimensional symptom set b. Relatively low rate of diagnostic overlap with competing diagnoses (e.g., MDD, GAD, PTSD) Symptoms PGD Dep Anx depressed .10 .71 -.31 blues .07 .66 -.16 anxious -.18 -.22 .52 nervous -.13 -.22 .88 Yearn .62 .21 .02 Intrusive thoughts .68 .26 -.10 ID symptoms .77 -.03 .02 Drawn->reminders .71 .15 -.12 Feel presence .82 -.02 -.08 __________________________________________ Egs: Prigerson et al. AJP, 1996, replication of AJP 1995; Boelen 2003, 2005; Phillip Dodd Ireland learning disabled; Kiely caregivers 2008; Jacobsen advanced cancer patients 2008 ROC Analysis of Alternative Diagnostic Algorithms for PGD N=5, k=3 1.00 N=6, k=3 N=6, k=4 0.80 Sensitivity N=7, k=3 N=7, k=4 N=7, k=5 0.60 N=8, k=3 N=8, k=4 0.40 N=8, k=5 N=9, k=4 N=9, k=5 0.20 N=9, k=6 Optimal 0.00 0.80 0.85 0.90 Specificity 0.95 1.00 Diagnostic accuracy absent other mental disorders (MDD, PTSD and GAD) (N=234) 100.0% DSM-5 (2013) TG (1999) ICD-11 (2013) PGD (2009) 90.0% Specificity CGD (1997) CG (2011) 80.0% 70.0% 60.0% 60.0% 70.0% 80.0% Sensitivity 90.0% 100.0% Diagnostic accuracy in the context of other mental disorders (MDD, PTSD and GAD) (N=34) 100.0% 90.0% PGD (2009) ICD-11 (2013) 80.0% Specificity DSM-5 (2013) TG (1999) 70.0% 60.0% 50.0% CGD (1997) 40.0% CG (2011) 30.0% 30.0% 40.0% 50.0% 60.0% 70.0% Sensitivity 80.0% 90.0% 100.0% Criteria for Prolonged Grief Disorder Proposed for DSM-5 & ICD-11 (PG-13 Scale maps onto these criteria) A. Loss: Loss of something loved B. Separation Distress: to a daily, distressing, or disruptive degree: 1. Yearning, pining longing for the lost person 2. Intense feelings of emotional pain, sorrow, or pangs of grief C. Cognitive, Emotional, Behavioral Symptoms: (5+/9 daily or to distressing or disruptive degree) 1. 2. 3. 4. 5. 6. 7. 8. 9. Confusion about one’s identity ( role in life or diminished sense of self; feeling that a part of oneself has died) Difficulty accepting the loss Avoidance of reminders of the reality of the loss Inability to trust others since the loss Bitterness or anger related to the loss Difficulty moving on with life (eg, making new friends, pursuing interests); feeling stuck in grief Numbness (absence of emotion) since the loss Feeling that life is unfulfilling, empty, and meaningless since the loss Feeling stunned, dazed or shocked by the loss Diagnostic Criteria for PGD D. Duration: At least 6 months elapsed since the loss E. Impairment: The above symptomatic disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning (e.g., domestic responsibilities) Reliability & Discriminant Validity (N=291) PGD Dx Cronbach’s alpha Internal Consistency 0.94 PGD Phi Depression 0.36 PTSD 0.31 GAD 0.17 PGD Dx MDD, PTSD, GAD w/ PGD 15/34 (44%) MDD, PTSD, GAD w/o PGD 19/34 (56%) PGD w/o MDD, PTSD, GAD 7/22 (32%) Specific Risk Factors/Clinical Correlates for PGD Sociodemographics: • Kinship relationships -- parents/spouses * (*= not MDD) • African Americans * Biomarkers: • No shortened REM latency * (EEG) • Brain imaging * (f/MRI) –nucleus accumbens; smaller brain volume Psychosocial Factors: • • • • • • • • • Pre-loss PGD symptomatology Dependency on deceased * Parental loss, abuse or serious neglect in childhood Parental control Separation anxiety in childhood * Preoccupation with relationships; need for approval*(insecure attachments) Preference for lifestyle regularity * - averse to change Lack of preparation for the death * Hospitalized (compared with home hospice) deaths* Cognition, Structural Brain Changes and Complicated Grief. A Population-Based Study • Study: Rotterdam Study “no grief” (control group, N=4731), “normal grief” (N=615), “complicated grief” (N=155) • Result: CG participants had lower scores for Letter-digit test, Word fluency test, and smaller brain volumes than controls • Conclusion: CG participants performed poorly on cognitive tests and had a smaller total brain volume. This suggests there is a neurological correlate of complicated but not of normal grief in the elderly Saavedra Pérez …Tiemeier Psychological Medicine 2014 Craving love? Enduring grief activates brain's reward center • Study: Bereaved women (11 CG, 12 NCG) fMRI scan of pictures of deceased • Result: Only those with PGD showed reward-related activity in nucleus accumbens (NA). This NA cluster was positively correlated with self-reported yearning, but not with time since death, participant age, or positive/negative affect • Conclusion: Shows attachment activates reward pathways. For those with PGD, reminders of the deceased still activate neural reward activity, which may interfere adapting to the loss in the present Something pleasurable that may make grief resolution akin to withdrawal of addiction. What creates this craving? O’Connor MF et al. Neuroimage 2008 Dependent Relationships Poor Bereavement Adjustment Close, dependent, harmonious relationships PGD (vanDoorn, Johnson, Carr, Lai) Caregiver’s Relationship to Dying Patient and Risk for PGD vs. MDD Marital Quality • feelings of security • dependency on partner • confiding in partner • active emotional support • combo security, confiding, support • Overall Quality of Marriage MDD PGD r .47 .43 .43 .60 .69 p .005 .001 .001 .0001 .0001 .39 .01 r .15 .06 .02 .18 .23 p ns ns ns ns ns .03 ns Van Doorn et al. 1998 Security-increasing marriages and insecure attachment styles put spouses at risk for PGD Childhood Separation Anxiety & Psychiatric Disorders in Bereaved Persons Dx PGD MDD PTSD GAD OR a 95% CI_______ 4.20 (1.42-12.42)** 1.42 (0.49-4.16) 1.20 (0.29-5.01) 2.18 (0.43-11.19)___ a Controlling for age, sex, race, childhood abuse or neglect, prior psych diagnosis; N=290 Vanderwerker, Jacobs, Parkes, Prigerson JNMD 2006 0.16 Dependency on Deceased Bereavement 0.43 Dependency Parental Control 0.19 Prolonged Grief Disorder Dyadic -0.03 Adjustment 0.06 Johnson JG, Zhang B, Greer JA, Prigerson HG. JNMD 2007 Preparedness for the Death Reduces PGD Risk Retrospectively • Prepared caregivers 2.4 times less likely to have PGD (Barry 2003) ; • 2.9 times among bereaved Alzheimer’s patient caregivers (Hebert, 2006) Prospectively Does preparation for the death promote bereavement adjustment? •longer time from dx to death less grief (Maciejewski et al. JAMA 2007) • EOL discussionacceptancehospital deathPGD (Wright et al. JAMA; JCO 2010) Health Consequences of Prolonged Grief Disorder (PGD) or Why should clinicians care about PGD? PGD at 6 months Predicts Impairment at 13 Months Family Health Project PGD at 6 Months 13 months Outcome a OR Hospitalizationb Major Health Event 1.32 1.16 (heart attack, cancer, stroke) Accidents 1.27 Altered Sleep 8.39 Smoking c 16.7 Eating 7.02 High Blood pressure 1.11 Controlling for pre-loss outcome measure, depression, anxiety, age and sex. At 25 mos: cancer, cardiac probs, alcohol probs, suicidality Yale Bereavement Study Disability associated with 6-12 mo PGD for those w/o MDD, PTSD, GAD 13-24 months post-loss MDD, PTSD or GAD Suicidal Ideation Functional Disability Low Quality of Life PGD Yes PGD No 55.9% 30.8% 72.7 50.0 44.1% 10.0 35.0 14.7 RR 8.86*** 5.61*** 2.01** 5.70*** Disability of PGD by Temporal Subtype Outcome 13-24 mo MDD, PTSD or GAD Disturbed Sleep Suicidal Ideation Functional Disability Low Quality of Life RR for Outcome associated with … Acute Delayed Chronic (15/172) (6/172) (12/172) Delayed or Chronic (28/242) 1.54 3.86 11.58*** 10.19*** 3.09 11.58*** 3.86 4.59** 1.97 4.93*** 3.29* 4.44*** 0.51 1.54 1.40 1.64** 0.76 3.78*** 2.58* 3.17*** Mean Sick leave (months in last 5yrs, Adjusted for gender) 1.4 Mean sick leave (months) 1.2 1 0.8 0.6 0.4 0.2 0 Controls A lot/completely No/Little* Worked trough grief Population-based sample of 449 Swedish parents who lost a child to cancer 4 to 9 years earlier (Kreicbergs et al.JCO, 2008) Evidence-based Recommendations for Bereavement Interventions: Why, Who, When, & What • Why: do benefits of intervening outweigh the costs? • What: what interventions are most effective, for whom? • Who: which bereaved should be targeted for intervention? • When: how soon to intervene after loss? Why Intervene? On Whom to Intervene? • Vast majority fine and gradually . . . • Move from very upset, disturbed to diminished distress, eventual adjustment • Questionable whether would benefit from intervention • Significant minority not fine and time won’t heal; • At risk for enduring distress and dysfunction (“eternal path of sorrow”) • Interventions improve their quality of life; potentially reduce adverse outcomes: • Social withdrawal, suicidality, alcohol abuse, high blood pressure, functional disability, loss of productivity When to intervene? Really Early Intervention: • Pre-loss in caregivers who are very dependent and have high levels of pre-loss grief (PG-12) • Benefits of preparation for the death: • Promotes accept of death, reduces grief • Opportunity to say goodbye • Fewer regrets • Result in better quality of death better bereavement outcomes Litz’ Healing Experiences After Loss (HEAL) •Litz suggests early post-loss period a time of re-establishing healthy routines •Online, CBT-based preventive intervention •Early intervention speedier rate of recovery HEAL (Healthy Experiences After Loss) • PI: Litz; NIMH R-34 indicated prevention • Internet-based, professional-assisted • Online, CBT-based preventive intervention • Wait-list controlled RCT • Targeting bereaved at the Dana-Farber Cancer Institute HEAL’s Approach to Prevention • 18 logons 6-weeks • Modules: promote self-care, accommodation of loss, enhanced self-efficacy, pleasurable activities, reattachment • Web interface text-driven but interactive • Homework-based approach • Professional oversight HEAL Outcome Data Time 1 Waitlist M SD Time 2 Immediate M Waitlist SD M SD Immediate M SD Time X Condition d PG-13 34.99 7.46 34.39 8.11 32.84 9.11 24.70 8.33 F(1, 74.10) = 29.04** 1.19 BDI 37.65 8.01 38.08 8.20 36.15 8.67 30.80 7.60 F(1, 72.63) = 14.19** .79 PCL 38.33 11.28 39.73 11.99 37.31 12.74 28.11 10.06 F(1,71.87) = 27.68** 1.02 BAI 31.52 7.52 35.22 11.16 30.31 6.78 29.18 9.39 F(1,73.99) = 10.68* .53 Note. *p<.01. **p<.001. Means over time for Prolonged Grief PGD Caseness Findings n χ2 Pre-test 25 ----- Post-test 6 10.129 0.001 6-week follow-up 5 11.621 0.001 3-month follow-up* 2 8.142 0.004 *comparison for the immediate group Mean PG-13 Score p 40.00 38.00 36.00 34.00 32.00 30.00 28.00 26.00 24.00 22.00 20.00 Pre-test Post-test 6-week follow-up Effective Approaches • Cognitive restructuring techniques help the griever to identify problematic aspects of the loss and to revise their understanding of them • Exposure techniques typically involve imaginal components, such as talking with deceased, and in-vivo components, such as confronting avoidance of places or people associated with the loss, and reliving the moment when witness or learned of the death – tapping “hot” emotions What Interventions Work? CBT-based Psychotherapies • Complicated Grief Therapy (Shear, 2005, 2014) • Psycho-ed about normal and CG • Dual process of adaptive coping – adjust to loss & restoration of satisfying life (goals defined with motivational enhancement) • Model: Grief is a trauma, people avoid trauma; exposure-based therapy reduces/desensitizes distress re: trauma • Exposure for traumatic avoidance – imagined conversation with deceased; retelling the death scene • Prolonged Grief Therapy (Bryant, 2014) CBT with exposure therapy where patients relive the experience of a death of a loved one, resulted in greater reductions in measures of prolonged grief disorder (PGD) than CBT alone • Boelen 2007; O’Donnell Tanzanian orphans 2014; Rosner German outpatients 2014 “optimal gains with PGD patients are achieved when the emotions associated with the memories of the death and the sequelae of the loss are fully accessed. ... Despite the distress elicited by engaging with memories of the death, this strategy does not lead to aversive responses. In light of evidence that many interventions provided to grieving people are not empirically supported, the challenge is to foster better education of clinicians through evidence-supported interventions to optimize adaptation to the loss as effectively as possible," Bryant “Treating PGD: A Randomized Clinical Trial” JAMA Psychiatry 2014 Conclusions Now (I hope) you know: • • • • • How to distinguish normal grief from PGD Diagnose PGD Tell if someone is at risk for PGD Know outcomes of PGD Understand core therapeutic issues in PGD Our time together has come to a close. Should you wish to contact me, my email address is: [email protected]